MIPS AND MOHSAIQ 2021 OVERVIEW A MIPS OVERVIEW




















- Slides: 22

MIPS AND MOHSAIQ 2021

OVERVIEW A. MIPS OVERVIEW B. MOHSAIQ C. MIPS CATEGORY UPDATES A. QUALITY PERFORMANCE B. COST PERFORMANCE C. PROMOTING INTEROPERABILITY D. IMPROVEMENT ACTIVITIES

QUALITY PAYMENT PROGRAM ■ The Medicare Access and CHIP Reauthorization Act (MACRA) was signed into law April 2015 – MACRA established a two-track Medicare physician payment system that emphasizes the transition to value-based payment and delivery ■ The Quality Payment Program (QPP) rewards value and outcomes in two ways: – Merit-based incentive payment system (MIPS) ■ Primary track for Mohs Surgeons – Advanced Alternative Payment Model (APMs)

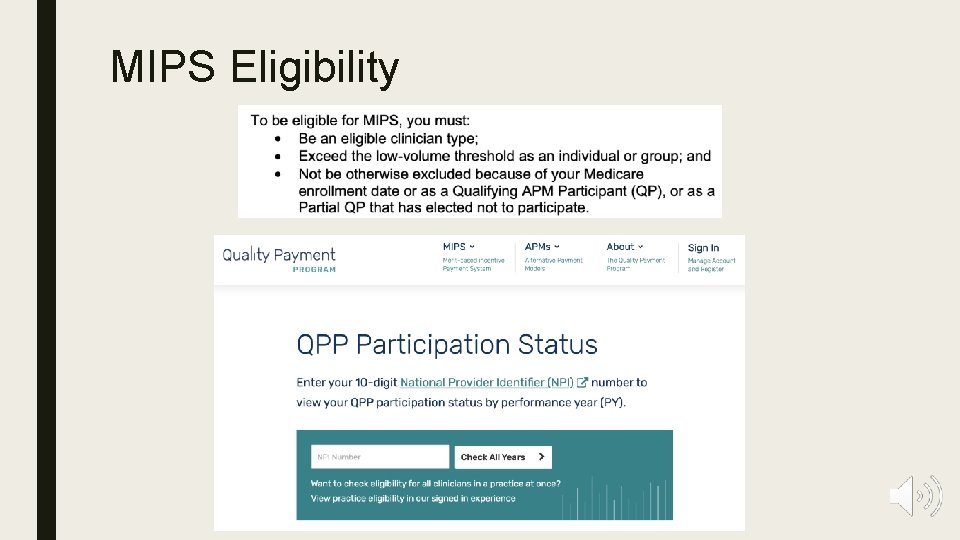
MIPS Eligibility

Performance ■ Performance is measured through data clinicians report in four areas: 40% 60% 20% 15% 25%

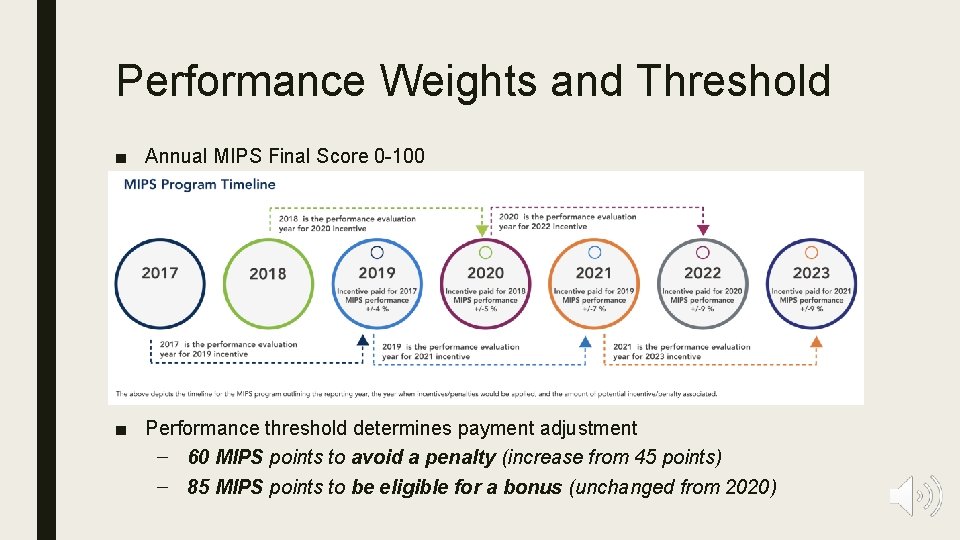
Performance Weights and Threshold ■ Annual MIPS Final Score 0 -100 – Final score is the sum of the weighted score of each category ■ MIPS is a budget neutral program: Payment adjustments are made on a sliding scale. – Payment adjustments are applied to Part B payments for Medicare physician fee schedule services two years after the performance period ■ Performance threshold determines payment adjustment – 60 MIPS points to avoid a penalty (increase from 45 points) – 85 MIPS points to be eligible for a bonus (unchanged from 2020)

COVID-19 ■ CMS anticipates that the national public health emergency (PHE) for COVID-19 will continue into and through 2021 ■ Extreme and Uncontrollable Circumstances Policy – Allows clinicians, groups and virtual groups significantly impacted by COVID-19 PHE to request reweighting for any or all MIPS performance categories

Reporting Mechanisms ■ Claims ■ Registry (Mohs. AIQ) ■ Certified Electronic Health Record ■ Web-Based Attestation ACMS members are strongly encouraged to report quality data using Mohs. AIQ

Mohs. AIQ ■ The American College of Mohs Surgery (ACMS) created Mohs. AIQ, a CMSrecognized Qualified Clinical Data Registry (QCDR) that allows Mohs surgeons to participate in the MIPS track of QPP by reporting quality measures relevant to their practice.

QUALITY PERFORMANCE CATEGORY

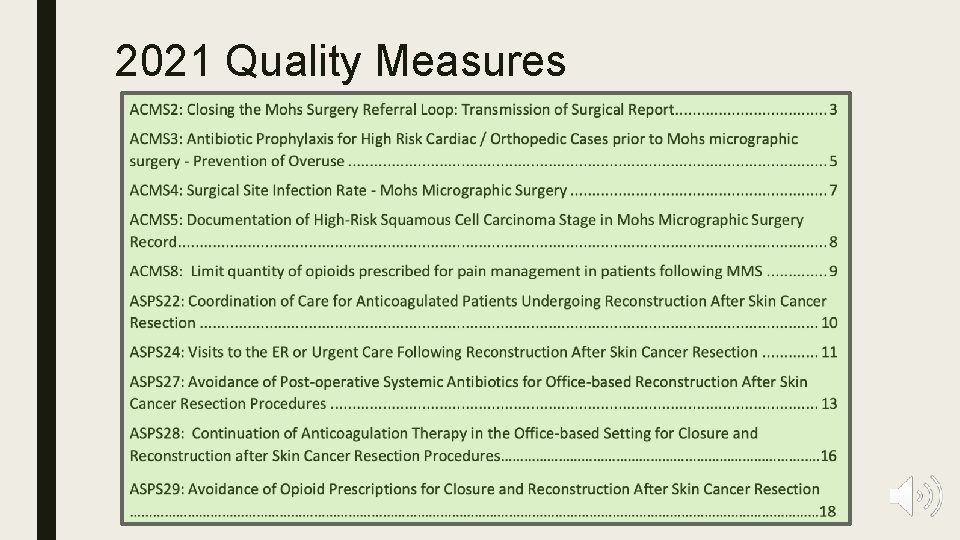
Quality Performance Category (60%) ■ For 2021: 1. Clinicians and groups must report at least six measures 2. Including one outcome or high-priority measure 3. For at least 70 percent of all patients eligible for the measure ■ Each measure is worth anywhere between 1 -10 points – Points are awarded based on comparisons to national benchmarks – Points are not assigned to a measure until post-submission ■ CMS has organized available MIPS quality measures into specialty measure sets to assist clinicians with selecting relevant measures. – A specialty measure set is available for Dermatology – For Mohs surgeons reporting through the Mohs. AIQ registry is strongly recommended since it includes even more specific measures developed by ACMS.

2021 Quality Measures

COST PERFORMANCE CATEGORY

Cost Performance Category (20%) ■ For 2021, there is no specific episode based measure for skin cancer care. ■ No reporting is required by the clinician in this category. ■ Mohs surgeons and dermatologists not reporting through a larger health care system or ACO would have the 20% attributed to this category reassigned to the quality measure category which can make the quality score up to 60% of the total ■ ACMS leaders are working with CMS on episode based measures that may be included in future years ■ Login to https: //qpp. cms. gov/ for further information and to see any cost score attributed to you.

IMPROVEMENT PERFORMANCE CATEGORY

Improvement Category (15%) ■ This performance category measures participation in activities that improve clinical practice. ■ To earn full credit in this performance category, you must generally submit one of the following combinations of activities: – 2 high-weighted activities – 1 high-weighted and 2 medium-weighted activities or – 4 medium-weighted activities ■ Physicians must report on an activity for a 90 day continuous period ■ Improvement activities can be selected and submitted through Mohs. AIQ – *Webinar available on ACMS Website

PROMOTING INTEROPERABILITY PERFORMANCE CATEGORY

2021 Promoting Interoperability Category (25%) ■ To report for this measure for 2021: – login to https: //qpp. cms. gov/ – Submit QRDA III form through Mohs. AIQ ■ Clinicians must attest “yes” to the following attestation statements: – The Prevention of Information Blocking Attestation, – The ONC Direct Review Attestation, and; – The security risk analysis measure. ■ Hardship exceptions are available in this category for clinicians and groups who are deemed as a small practice, use decertified EHR technology, have insufficient internet connectivity, face extreme and uncontrollable circumstances, or lack of control over the availability of CEHRT. Clinicians with a special status (e. g. , hospital-based) will have their PI performance category score automatically reweighted to the Quality performance category and will not need to submit a hardship exception application.

2021 Promoting Interoperability Category (25%) ■ There are 4 main categories to garner scoring in this category – 1) Eprescribing – 2) Health Information Exchange-sending and receiving patient health information electronically with other providers – 3) Provide patients electronic access to their health information – 4) Public Health and Clinical Data Exchange-e. g. public health registry reporting

2021 Promoting Interoperability Category (25%) ■ 5 bonus points are awarded for making a query of the PDMP, Prescription Drug Monitoring Database which can be accessed when prescribing opioids

Avoiding MIPS Penalty ■ The maximum downward payment adjustment in 2023 is -9 percent based on 2021 performance ■ Example of how to reach the 2021 performance threshold include: – Achieving a perfect score of (60/60) points, in the Quality category, which – when reweighted – will yield 60 total points (60/60) x (60%) toward the MIPS final score (with category reweighting). Total MIPS Final Score = 60.

MIPS and Mohs. AIQ SUMMARY ■ MACRA established a two-track Medicare physician payment system that emphasizes the transition to value-based payment and delivery ■ Merit-based incentive payment system (MIPS) is the primary QPP track for Mohs surgeons. ■ Mohs. AIQ, a CMS-recognized Qualified Clinical Data Registry (QCDR) that allows Mohs surgeons to participate in the MIPS track of QPP by reporting quality measures relevant to their practice. ■ Performance threshold determines payment adjustment – 60 MIPS points to avoid a penalty (increase from 45 points) – 85 MIPS points to be eligible for a bonus