Minimally Invasive Surgery rtPA for ICH Evacuation SURGICAL































- Slides: 47

Minimally Invasive Surgery + rt-PA for ICH Evacuation SURGICAL PERSPECTIVES ISSAM AWAD, MD MARIO ZUCCARELLO, MD CO-STUDY CHAIRS 10 July 15

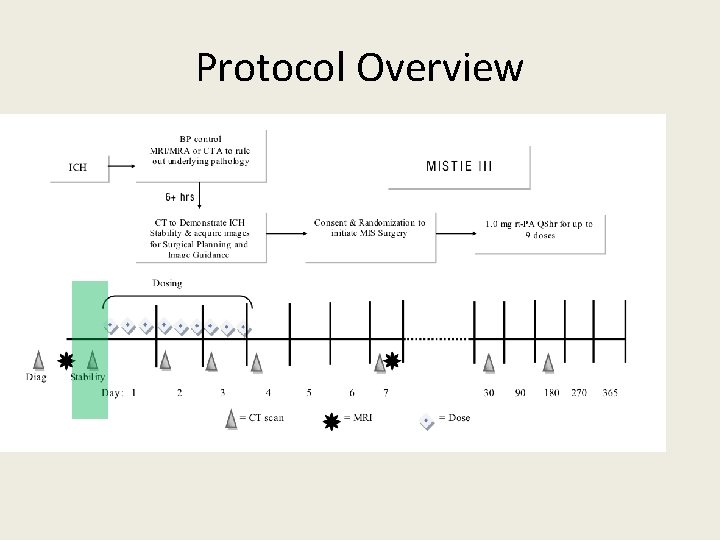
Protocol Overview

Objectives • • • About MISTIE 2 Lessons Learned from MISTIE 2 8 Essential Elements of MISTIE 3 Minimally Invasive Procedure Considerations

M 2 Results 1. The MIS procedure can reduce clot size safely without increased mortality or morbidity 2. The reduction is associated with an estimate between 10% - 14% improved outcome across multiple modified Rankin cut points 3. The intervention is associated with shorter (39 -day) hospital stay and a $45, 000 savings/patient 4. An estimate of 14% fewer patients reside in long-term nursing facilities at 180 and 365 days post procedure.

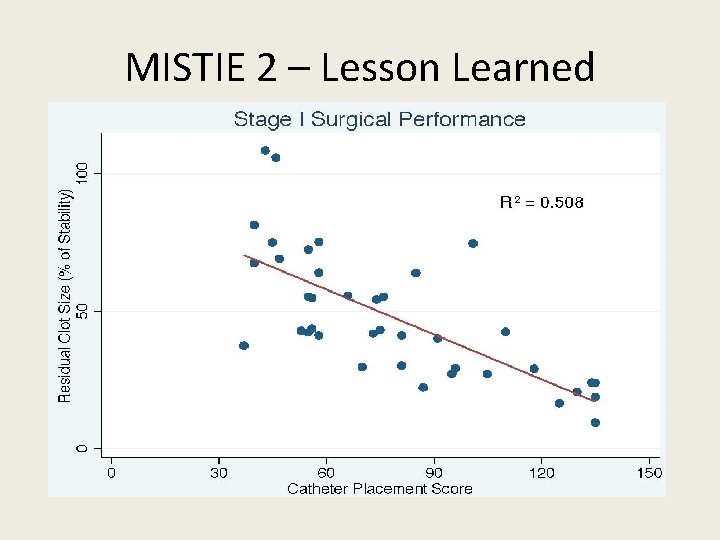
M 2 Surgical Results • Optimal catheter placement within the clot is critical to successful outcome – Achieved by catheter trajectory planning – Surgical Review Required • Not required to follow Surgical Review Recommendation • If disagreement, site NS must demonstrate rationale of his/her plan

MISTIE 2 – Lesson Learned

Overview • Performed by certified neurosurgeon • Performed in OR (preferred) – Also in procedural CT/MRI scanner or ICU • Use introducer and catheter (commercially suitable kit is available) • Gentle Aspiration with 10 ml syringe • Antibiotic coverage

Site Neurosurgeon Qualification Requirements • Pre-qualification – Each surgeon applying to participate in M 3 must attest that they have performed at least 3 prior image guided or stereotactic catheter aspiration or placement procedures – Each surgeon must attest that they have current privileges to perform these procedures at their institution • Qualification with probation – One MISTIE procedure for ICH must have been performed prior to the start of the trial - SC will review images – If surgeon hasn’t done a MISTIE procedure, surgeon will need to be proctored on site or teleproctored with their first case – The proctoring or tele-proctoring of a first case MISTIE procedure may only be performed by a fully qualified MISTIE surgeon • Full Qualification – Review of 3 MISTIE procedures prior to or during the trial. – Also a requirement for proctoring each site’s new surgeons

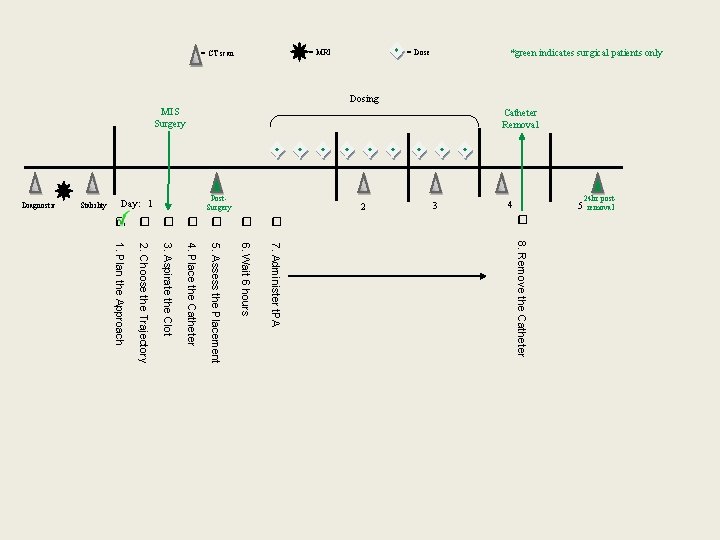
Standardization • Precision, Accuracy, Safety are NOT Negotiable • Standardization of 8 Essential Elements: – Plan the Approach – Choose the Trajectory – Aspirate the Clot – Place the Catheter – Assess catheter placement – Stabilization = Wait 6 hours – Administer TPA – Remove the Catheter • Will later discuss where there is latitude

Catheter Removal MIS Surgery 24 hr postremoval 5 4 3 2 Post. Surgery Day: 1 Stability Diagnostic *green indicates surgical patients only = Dose = MRI = CT scan Dosing q q q q 1. Plan the Approach 2. Choose the Trajectory 3. Aspirate the Clot 4. Place the Catheter 5. Assess the Placement 6. Wait 6 hours 7. Administer t. PA 8. Remove the Catheter

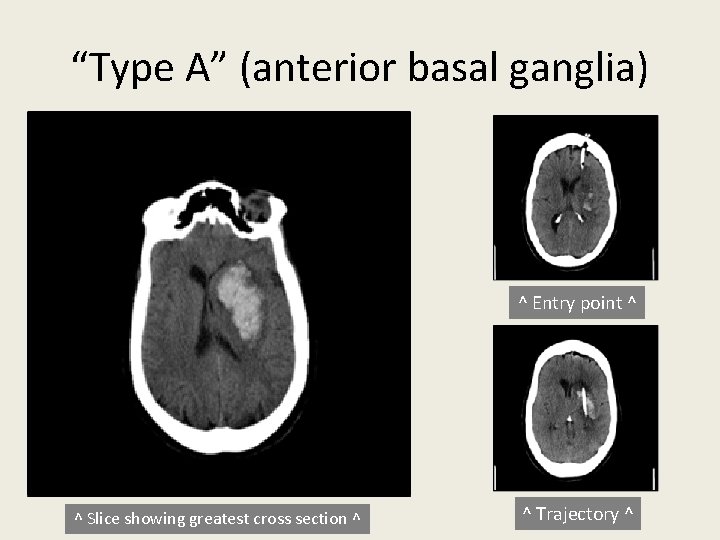
Trajectory Planning ICH Categories 1. Type A = Deep-seated occupying the anterior third of the basal ganglia with typical “oval” shape (“American” football shape) 2. Type B = Deep-seated occupying the posterior third of the basal ganglia; the shape can range from more roundish to elliptical 3. Type C = Superficial (lobar) with variable shape, but often more spherical

“Type A” (anterior basal ganglia) ^ Entry point ^ ^ Slice showing greatest cross section ^ ^ Trajectory ^

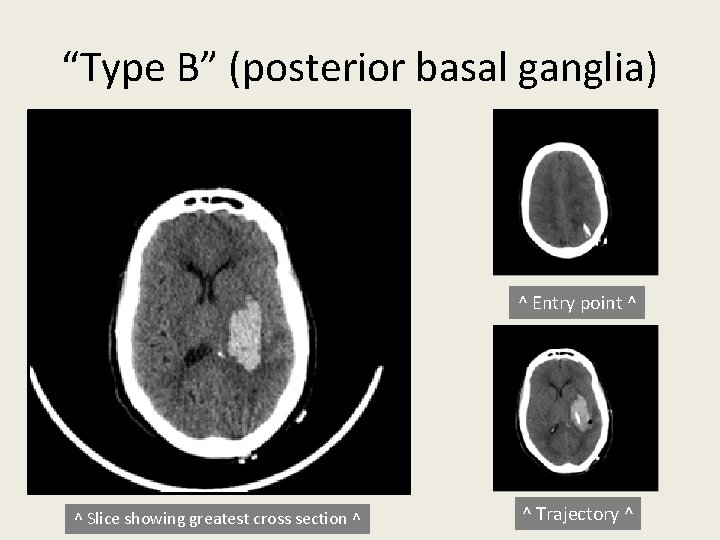
“Type B” (posterior basal ganglia) ^ Entry point ^ ^ Slice showing greatest cross section ^ ^ Trajectory ^

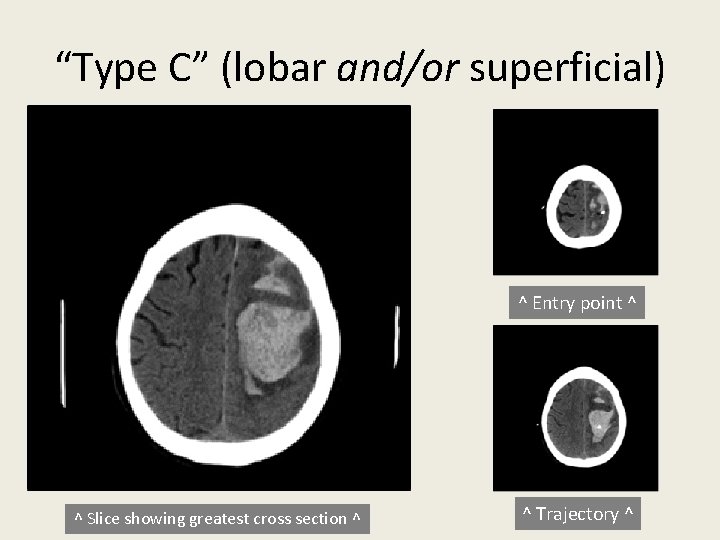
“Type C” (lobar and/or superficial) ^ Entry point ^ ^ Slice showing greatest cross section ^ ^ Trajectory ^

Instructional Surgical Presentation Minimally Invasive Surgery (MIS) for Intracerebral Clot Removal

Antibiotics • Protocol states it is up to local hospital protocol or 1 to 2 G Ancef IV – To be given pre-operatively and every 8 hours following until catheter is removed

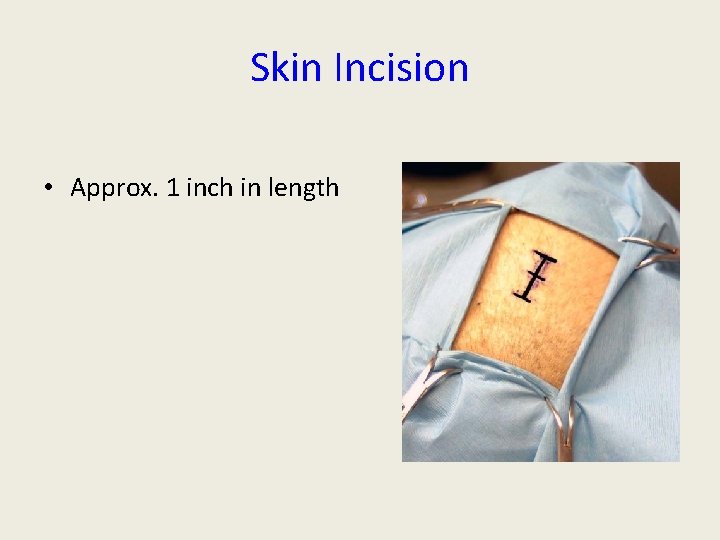
Skin Incision • Approx. 1 inch in length

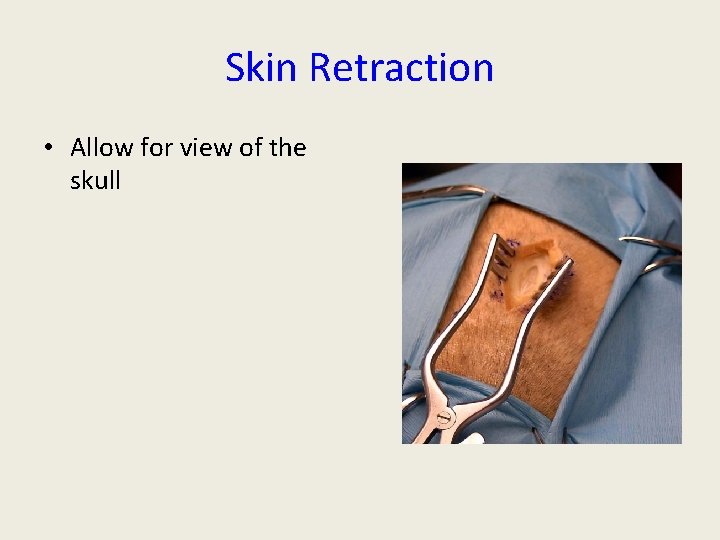
Skin Retraction • Allow for view of the skull

Burr Hole Drilling • Burr hole is made at the appropriate site for the planned trajectory according to ICH Type (A, B, or C) • Large burr hole as needed for angle of approach

Cannula Introduction • Dura is opened with a small incision • 14 French Cannula illustrated • It is placed with a single pass into central core (2/3 of overall hematoma diameter)

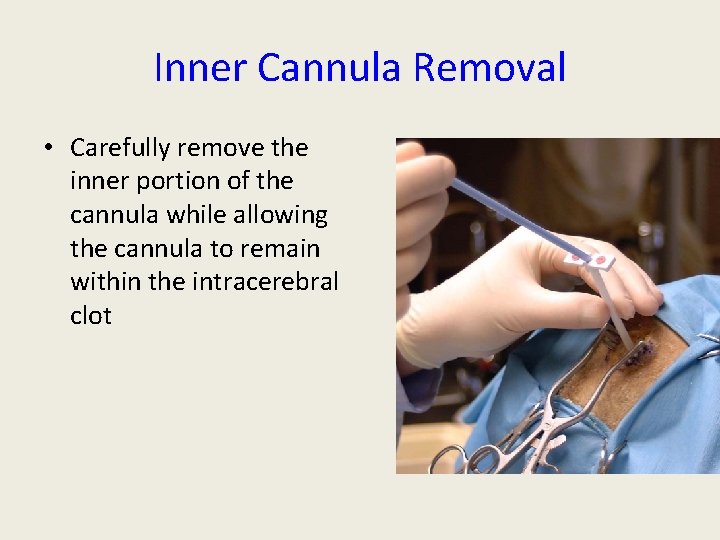
Inner Cannula Removal • Carefully remove the inner portion of the cannula while allowing the cannula to remain within the intracerebral clot

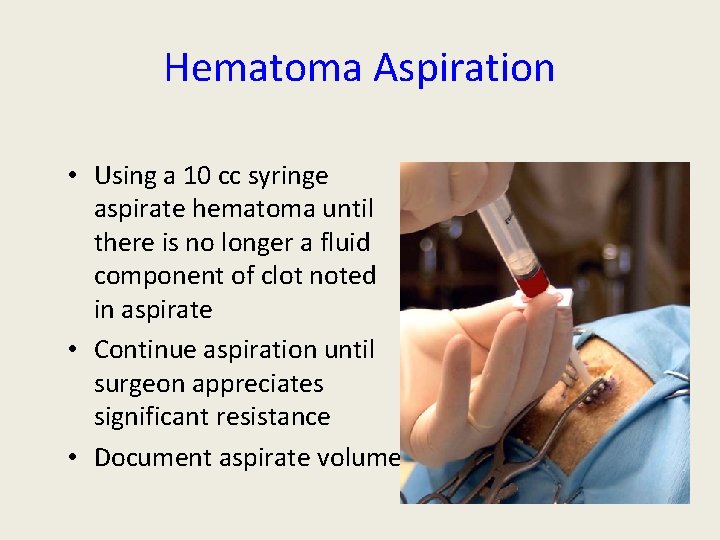
Hematoma Aspiration • Using a 10 cc syringe aspirate hematoma until there is no longer a fluid component of clot noted in aspirate • Continue aspiration until surgeon appreciates significant resistance • Document aspirate volume

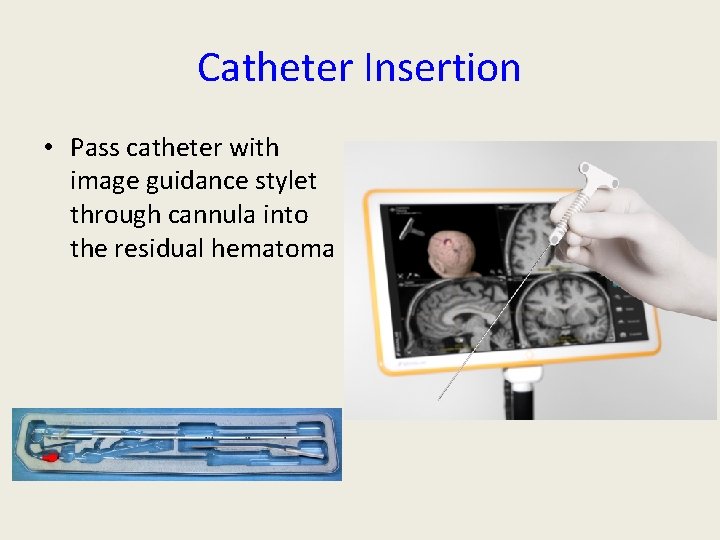
Catheter Insertion • Pass catheter with image guidance stylet through cannula into the residual hematoma

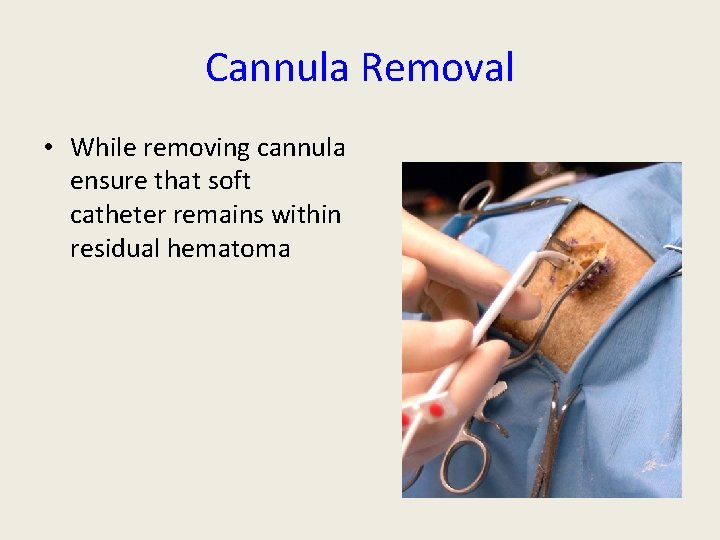
Cannula Removal • While removing cannula ensure that soft catheter remains within residual hematoma

Catheter Tunneling • Tunnel catheter subcutaneously away from the incision as is standard practice • Suture catheter before skin closure

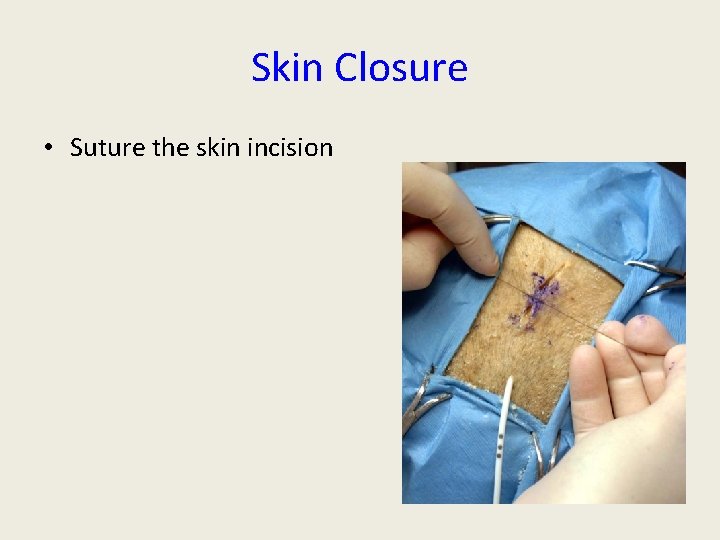
Skin Closure • Suture the skin incision

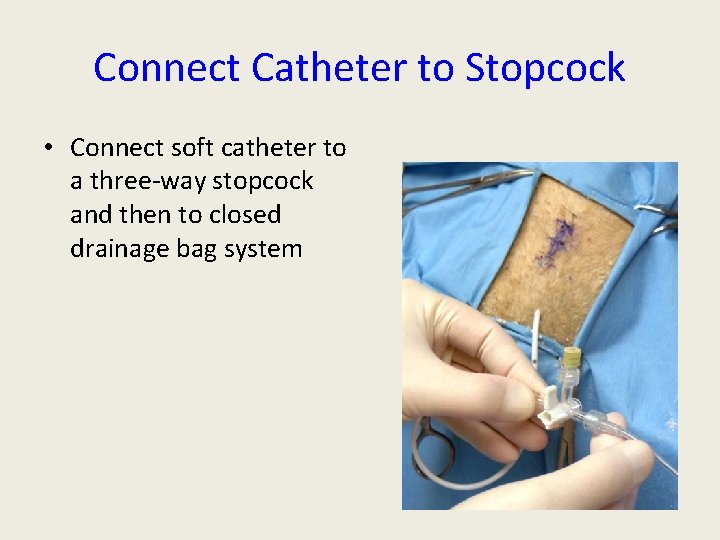
Connect Catheter to Stopcock • Connect soft catheter to a three-way stopcock and then to closed drainage bag system

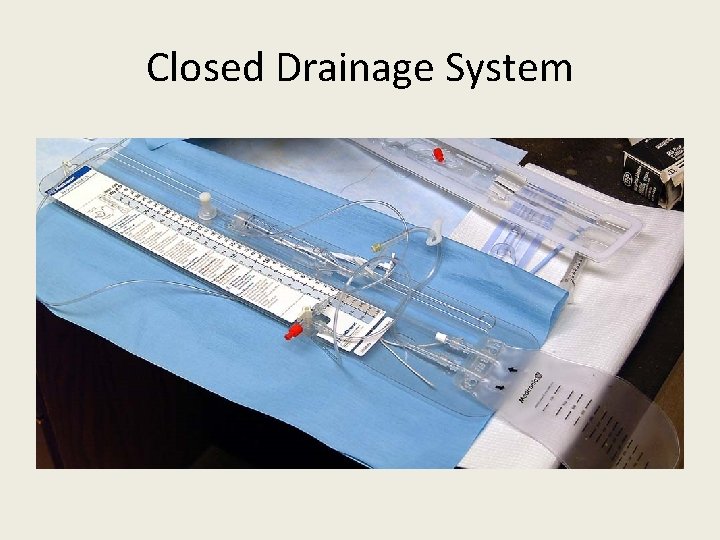
Closed Drainage System

Considerations for the Surgeon

Autonomy vs Standardization of Surgical Elements • We don’t want to restrict the procedure and how it’s done – Each veteran MISTIE surgeon has their own technique, have to allow for variation – Variability could cause fewer complications but also may take away generalizability • Technical variations OK if goal is met – Standardization of key elements – Optimal catheter placement within the clot, for example, as we have discussed

Feb 7, 2013 ISC 2013 Late Breaking News 31 Image Guidance is Mandatory For both cannula (if used) and catheter Stereotactic CT Guided Navigation (passive catheter introducer or equivalent device) Real Time Image Guidance (Procedural CT, intraop imaging, etc)

Acceptable Image Guidance Modalities • Image guidance restrictive in M 2, now can have procedural CT in OR, even in CT, with real -time guidance – Must be flexible with image guidance issues • There are 2 algorithms for catheter placement – Stereotactic Image Guided using passive catheter introducer – Real Time Image Guidance using CT

Stereotactic Image Guidance • Create Burr Hole w/Drill • Use cannula large enough to pass final catheter through (14 F, 16 F) • Catheter inserted passively inside cannula which is then removed • To Reposition, must re-target clot with new cannula/catheter • Variation: Larger, soft catheter with stylet

Real Time CT • May use twist hole • May use Dandy needle, brain needle or other suitable hard cannula to aspirate clot, then • Insert soft catheter using planned trajectory – More than 2 passes discouraged, would need further stabilization • To reposition – Correct on the spot – Check placement at completion of procedure

Accuracy of Trajectory Influenced By: • Image guidance protocol – Use modality that yields greater # slices (MRI vs CT) – Improves accuracy – 1 mm Slices • Place fiducials both anteriorly and posteriorly – Typically done on 6 facial landmarks – Critical for Type B clots: 3 posterior landmarks – Per MOP, highly recommend obtaining fiducials at 6 hour stabilization scan - or at least early once pt appears to be good potential candidate

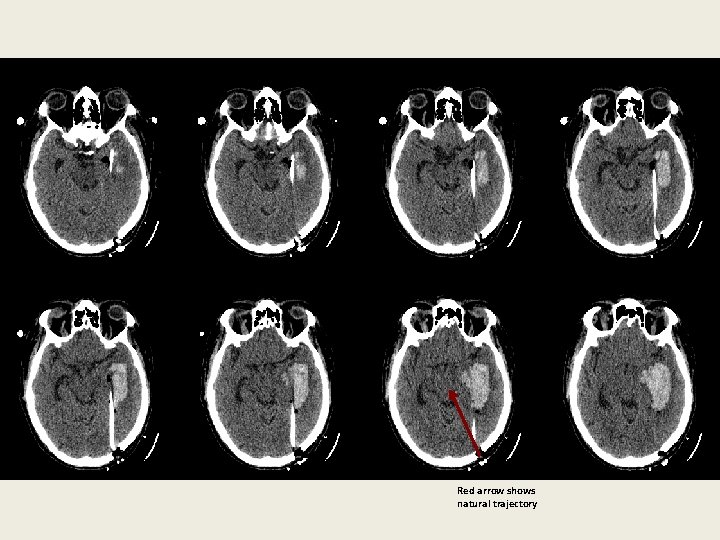
SC Analysis – Trajectory B Clots Greater Proportion of Sub-Optimal Placements • Most difficult often end up w/catheter medial to clot – Location burr hole relative to Angles of Freedom – Cannula/Catheter will take path of least resistance • If on edge of clot, the clot will move to the side • If going through center of clot, it won’t move away • Traj B must factor in Angles of Freedom – Move burr hole more lateral – Enlarge burr hole, particularly inner table of skull

Red arrow shows natural trajectory

Repositioning or replacement before dosing • Reposition defined as: – Partial removal or “pull back” – Remove non-optimally placed catheter/replace using second MIS procedure using same or different trajectory • Complete replacement of the catheter is allowed if there is disturbance by inadvertent catheter movement or partial clot reduction • In any subject, complete replacement to occur only once • Never have > 2 passes with a rigid cannula

Repositioning or replacement before dosing (cont) • If after placement and subsequent CT you decide to reposition, you do not need Surgical Center confirmation for your decision • Only after you have your final placement do you need to submit images for Surgical Center review (important to remember, you need to submit images to the Surgical Center when you feel you have the final position) • Eventually must upload all CT images into EDC

Repositioning or replacement after dosing begun • If dosing has begun, there is a different procedure for repositioning/replacement • You must wait at least 24 hours after the most recent dose before manipulating the catheter • You must repeat all stability protocols as if it were the original catheter placement – Post placement, must upload DICOMs showing final placement – Obtain SC approval – Wait 6 hours for stability before resuming dosing

Large Difficult Shapes • Consider 2 catheters from the beginning – Each using a different trajectory • Consult SC for issues regarding – Catheter management – Dosing considerations • SC and CC will adjudicate such matters on a case by case basis

IVH • IVH, even when EVD placed, does not necessarily represent an exclusion unless casting/mass effect – Proceed with evaluation – Send CT scans – Case will be adjudicated by SC and CC • Cases with IVH and more than one EVD cannot be included • If your patient has more than one catheter, they should be clearly labeled to ensure the study rt. PA is injected only into the ICH – To promote ICH catheter drainage, also clamp EVD drain for one hour after dosing if ICP will allow

Helpful CPT Codes • • 61781: Stereotactic image guidance 61156: Burr hole for ICH 61210: Placement of brain catheter 61070: Aspiration or injection through brain tubing – Injection is standard – Drug is research • 61795: PI as Surgeon • 76355: CT guidance of stereotactic localization = PI management of stereotaxis = PRO-FEE

Consideration of Surgical Endpoint • We confirm we wish to leave the primary surgical endpoints unchanged from the MISTIE Phase II study – The goal is to decrease clot volume to 10 -15 cc – May ideally achieve <10 if possible

Consideration of Surgical Endpoint The MISTIE II multivariable outcome prediction model demonstrates that the greater the removal of clot the greater the benefit. Animal models are consistent but have not been performed with detailed dose injury studies. Epidemiologic models of human outcome after ICH have however confirmed volume severity relationships. Thus our surgical endpoint is to decrease to 10 -15 cc.

Consideration of Surgical Endpoint The failure to reach 10 -15 cc is a practical matter. As removal is limited when the catheter does not contact the clot, the surgeon must be allowed to individualize the goal for each patient's specific catheter situation.

WELCOME to