Milton Ontario Health Team Dr Arieg Badawi Milton

Milton Ontario Health Team Dr. Arieg Badawi Milton District Hospital Presentation – 10/10/2019

Ontario Health Teams (OHT) In his letter to the Premier and Minister of Health Dr. Rueben Devlin wrote, “The concern is that on any given day in the province, there at least 1000 patients receiving health care in the hallways of our hospitals. At the same time, the wait time to access a bed in a long-term care home is 146 days, and this can vary significantly depending on where you happen to reside in Ontario. ” (Devlin, 2019)

Ontario Health Teams (OHT) § He identified a few challenges: 1. The patients and their care givers are facing a lot of challenges “navigating” our healthcare system. 2. The wait times are long. “Ontarians cannot always see their primary care provider when they need to, wait times for some procedures and access to specialists and community care too long, and emergency department use is increasing. ” 3. Our healthcare system has capacity pressures. 4. A need has been identified for effective, seamless coordination at the “system level and point of care” 5. Everyone is feeling the strain “Health care providers, patients and their family members” 6. “Responsibility for coordinating high-quality health care is spread across many government agencies, organizations, and the Ministry with no clear point of accountability. ” (Devlin, 2019)
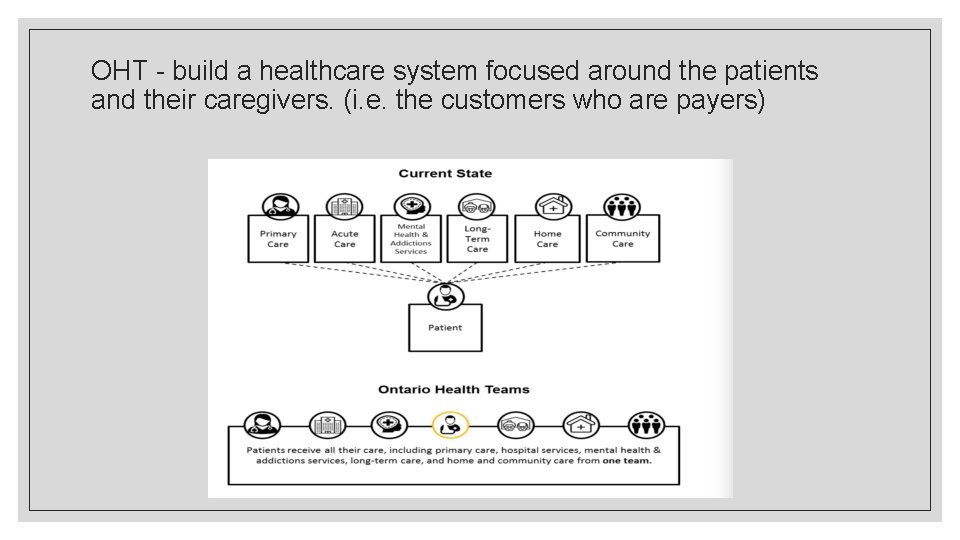
OHT - build a healthcare system focused around the patients and their caregivers. (i. e. the customers who are payers)

Providers and organizations eligible to become an OHT. 1) primary care (including inter-professional primary care and physicians) 2) secondary care (e. g. , in-patient and ambulatory medical and surgical services (includes specialist services) 3) home care, community support services 4) mental health and addictions services 5) health promotion and disease prevention services 6) rehabilitation and complex care 7) palliative care (e. g. , hospice) 8) residential care and short-term transitional care (e. g. , in supportive housing, long-term care homes, retirement homes) 9) long-term care home placement 10) emergency health services 11) laboratory and diagnostic services 12) midwifery services, and other social and community services and other services, as needed by the population. (Ontario Ministry of Health, Ministry of Long-Term Care, 2019)
OHT Stages: 1. Self-Assessment. 2. Validating the provider Readiness: There are 3 categories: • Proceed to Full Application. • In Development- Milton OHT • In Discovery. 3. In-person Community Visits. 4. Designated Ontario Health Teams: “receive an integrated funding envelope and enter into an OHT accountability agreement. ” (Ontario Ministry of Health, Ministry of Long-Term Care, 2019)

Milton OHT – Quadruple Aim (population health, patient experience, provider experience and reducing the per capita cost. ) 1. Family Physicians (practices) Integrated Practice Unit (IPU) – The Primary care clinic is the centre of the healthcare cell; It is where all of the patient information originates, received and is transferred. 2. Mental health IPU – includes community-based mental health organizations (7 organizations). Mental health is a community challenge and it requires a community solution. 3. Palliative care IPU – The community palliative care will be supported by scale. 4. Elderly and Community IPU – a smooth transition of the patient from the hospital to the community. Goal is to keep patients out of the hospital by maximizing the home and community supports.

Patient Care & Experience ◦ Accessible & practice in interdisciplinary teams. (Wen & Tucker, 2015) ◦ An organic team approach. ◦ Leverage technology to help our patients increase access and communication, like the use of “practical apps” in an attempt to transform the healthcare experience to one shared between the patient and the healthcare team. ◦ Competitive advantage to approach and deliver results that align with the strategic goal of providing value - based care by increasing access, connectivity and coordinated care.

Defined Patient Population ◦ Patients rostered in the primary care practices of the 54 physicians in this team, living in Milton, ON. ◦ According to Statistics Canada the population of Milton in 2016 was 110, 128. (Focus on Geography Series, 2016 Census, 2016) ▪ 25. 8 % of the population is between 0 & 14. ▪ 65 % between the ages of 15 & 64. ▪ > 65 were 9. 2%. ▪ The Aboriginal people are 1 % of the population, 57. 4% First Nations, 31. 1%Métis and 1. 4% Inuit. ▪ 35. 9 % of immigrants compared with 29. 1 % for Ontario and 21. 9 % to Canada. ▪ The median household income in Milton was $104, 730 in 2015. ▪ Highly educated 93. 5 % compared to 86. 3 % for the rest of Canada.

Leadership, Accountability and Governance ◦ Vision: a comprehensive cycle of value-based care. ◦ Strategic theme: Quadruple Aim of population health, patient and provider experience and cost reduction. ◦ Goal: a seamless, integrated, efficient and innovative healthcare system. ◦ Brand: “One Team, One Outcome. ” ◦ Governance: Community and patient advocacy leaders, leaders from the Primary care IPU, Mental health IPU, Palliative & Community care IPU, a Chief Health Information Officer and a hospital representative. ◦ Accountability: “Must be tied to the strategy” (Brian Golden) § Measuring performance and experience metrics which is reliable, easy to obtain and cost effective. § Rewards: to motivate team members to perform and achieve target goals. § Performance metrics: 1. Avoidable hospital utilizations: readmission rates, emergency department visits & length of stay. 2. Measure access to services like primary care, mental health, long term and home care. 3. Dr. Kaiser’s Value equation= Access+ Technical Quality+ Service Satisfaction+ Functional status/ Cost (Edmondson, Golden, & Young, 2008) 4. Patient experience metrics. 5. Provider experience metrics.

Digital Health ◦ Bhatia and Falk, 2018, “Ontario’s Digital Health by Design - goal is to advance the modernization of a patient-centred health system by making digital health an integral and routine part of patients’ experience. . . It is a “digital first” philosophy. ” (Bhatia & Falk, 2018) ◦ Choose the technology that will fit our business model and the digital intervention must support the strategic goal of the OHT. ◦ Leveraged technological use in primary care, e. g. the use of i. Pads in waiting rooms, E-portals, OTN “e. Visit”, “practical apps” and telehealth services for psychotherapy in addition to: ◦ The Hospital Report Manager (HRM). ◦ e-Referral for diabetes, footcare, and mental health and addiction. ◦ e-Consults allowing timely access to specialist. ◦ The Chief Health Information Officer will have a team composed of a data manager for data collection, an analyst who would report important trends and a data architect reporting to her. (IT Transformation Health care Needs)

The End…Thank you for your patience! This Photo by Unknown Author is licensed under CC BY
- Slides: 12