Migraine Essentials in Primary Care Britt Schloemer APRN

Migraine Essentials in Primary Care Britt Schloemer, APRN 2018 KY NAPNAP Annual Update

Describe what a migraine is Present an update on acute migraine treatment recommendations Objectives Discuss treatment options for migraine prevention Discuss treatment and management priorities when caring for a child with migraines Present resources that can be utilized by both patients and PCPs when treating and managing migraines

Migraine What is a migraine?

Migraine without aura: International Headache Society (IHS) Diagnostic Criteria (Patients < 15 years of age) At least 5 attacks Duration 4 -72 hours At least 2 of the following: o Unilateral o Pulsating quality o Moderate to severe intensity o Exacerbation by activity At least one of the following: o Nausea, vomiting, or both o Photophobia or phonophobia Migraine with aura: At least 2 attacks At least 3 of the following: o At least one fully reversible aura symptoms indicating focal, cerebral, cortical or brainstem dysfunction o At least one aura symptoms developing gradually for 4 minutes or ≥ 2 symptoms in succession o No aura > 60 minutes o Headache begins before, simultaneously, or within 60 minutes of aura

Listed among the top 5 youth health problems 3 rd most common referral to the ED Migraine Statistics (Alfonzo & Chen, 2015) The most common cause of headache (HA) in children Incidence and prevalence increases with age: 3 – 7 years: 2% 7 - 11 years: 7% 11 – 15 years: 20% Prepubertal males: females – 3: 2 Adolescent females: postpubescent males – 3: 1

What do parents do?

What do they think is happening?

But, what if… Lee, 2017

Red flags could indicate: Increase in intracranial pressure Focal irritation Stroke Infection Red flag may indicate an emergency: Refer to ED Head CT
Can act like strokes Rare migraine variants Hemiplegic migraine Basilar artery migraine Opthalmoplegic migraine Alice in Wonderland Syndrome Confusional migraine May not be associated with headache Cyclic vomiting Abdominal migraine Benign paroxysmal vertigo Benign paroxysmal torticollis


U. S. Headache Consortium Guidelines for Neuroimaging in Patients Presenting With Headaches Imaging is recommended: Lets talk imaging In patients with non-acute headache and unexplained findings on neurologic examination In patients with neurologic symptoms (headache that is worsened with use of Valsalva’s maneuver, awakens the patient from sleep, is newly onset in an older person, or is progressively worsening), the evidence is insufficient to make specific recommendations In patients with a normal neurological examination if they have atypical features to their headache An MRI is preferred to a CT scan for the above situations, unless it is contraindicated or emergent neuroimaging is needed.
Back to the tumor question… 0. 0056% of children exhibiting a typical migraine or headache will have a tumor 56 children out of 100, 000 (personal communication, Elizabeth Doll, MD, 2018) Your examination and history taking skills are vital

Do not overlook the simple treatments requiring no Rx Acute/ Abortive Treatment Hydration Sleep Decrease stimulation Dim lights Medications Non-steroidal anti-inflammatories Triptans Steroids Over the counter combination therapies

1. Last dose of a triptan within 2 hours 2. More than 2 doses of a triptan within a 24 hour period 3. Last dose of triptan within 24 hours prior DHE 4. Last dose of NSAID within 6 hours 5. Pregnancy 6. Breastfeeding Some Contraindications 7. Angina 8. Ischemic heart disease 9. Perivascular disease 10. HTN 11. CAD 12. Concurrent MAO inhibitors or serotonin agonists 13. Concurrent potent 3 A 4 inhibitors 14. Concurrent peripheral and central vasoconstrictors 15. Hemiplegic or Basilar migraine 16. Severe hepatic and renal disease

Naproxen > Ibuprofen > Acetaminophen Naproxen NSAIDS Approved for pain in ages >12 5 mg/kg or 500 mg PO initially, then 250 mg PO q 6 -8 hr or 500 mg PO q 12 hr PRN; not to exceed 1250 mg/day on day 1; subsequent daily doses should not exceed 1000 mg NSAID precautions and contraindications At least 6 hours between doses GI caution Bleeding caution More efficacious if given with a triptan

Naproxen > Ibuprofen > Acetaminophen Ibuprofen NSAIDS 10 mg/kg/dose every 6 hours Not to exceed 600 mg/dose or 40 mg/kg/day Approved for children > 6 months of age NSAID precautions Twice as efficacious as acetaminophen Acetaminophen 15 mg/kg/dose max 1000 mg every 4 hours Max daily dose of 75 mg/kg or 4000 mg

NSAIDS Age Recommendation if Initial Dose at no contraindications onset of HA > 12 years Naproxen 6 months – 12 Ibuprofen years <6 months Acetaminophen 5 mg/kg; MAX 500 mg at onset 10 mg/kg; max 600 mg 15 mg/kg; max 1000 mg

Produce vasoconstriction Best if used early May repeat, x 1, 2 hours after initial dose if migraine persists Triptans Many contraindications, including, but not limited to: Stoke CV disease, HTN Pregnancy Pay attention to ages
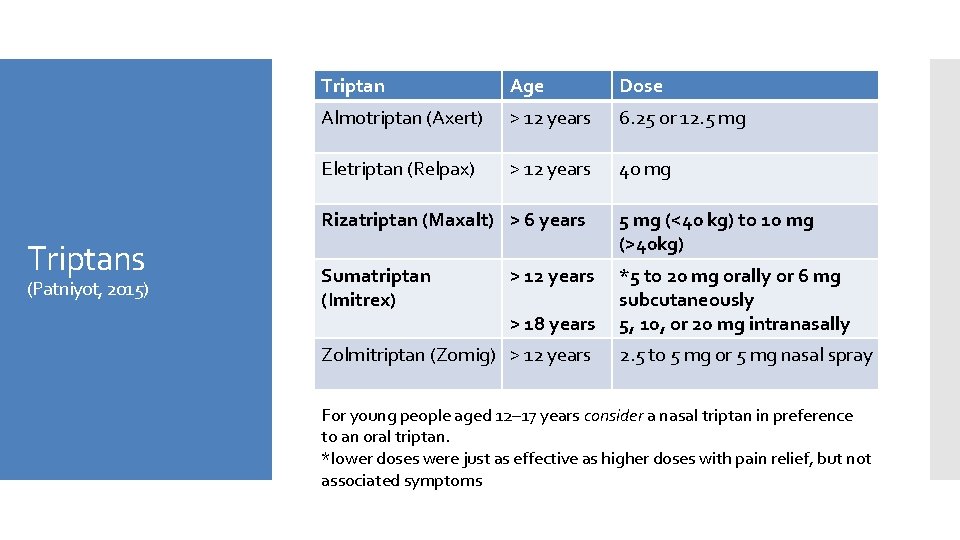
Triptans (Patniyot, 2015) Triptan Age Dose Almotriptan (Axert) > 12 years 6. 25 or 12. 5 mg Eletriptan (Relpax) > 12 years 40 mg Rizatriptan (Maxalt) > 6 years 5 mg (<40 kg) to 10 mg (>40 kg) Sumatriptan (Imitrex) *5 to 20 mg orally or 6 mg subcutaneously 5, 10, or 20 mg intranasally > 12 years > 18 years Zolmitriptan (Zomig) > 12 years 2. 5 to 5 mg or 5 mg nasal spray For young people aged 12– 17 years consider a nasal triptan in preference to an oral triptan. *lower doses were just as effective as higher doses with pain relief, but not associated symptoms
Triptans (Patniyot, 2015) Recommendation: At onset of headache, administer Naproxen AND Triptan For older children, intranasal triptan is preferred over oral Always consider indications and contraindications of medications

Sumatriptan/Naproxen oral tablets (Treximet) 10/60 mg up to 85/500 mg; MAX x 1 85/500 mg tab/day > 12 years of age Other Treatments (Alfonzo & Chen, 2015) & (National Guideline Clearinghouse, 2012) Nausea and vomiting: Ondansetron (Zofran) 0. 1 mg/kg; MAX 8 mg every 8 hours PRN Dopamine Receptor Antagonists: Promethazine (Phernergan): 0. 25— 1 mg/kg/dose; MAX 25 mg/dose Metoclopramide: 0. 1 – 0. 2 mg/kg/dose; MAX 10 mg Consider diphenhydramine (benadryl) DO NOT GIVE OPIOIDS No research supports use of steroids Abortive medications should not be used more than 2 -3 x/week or 10 x/month Mind and Body
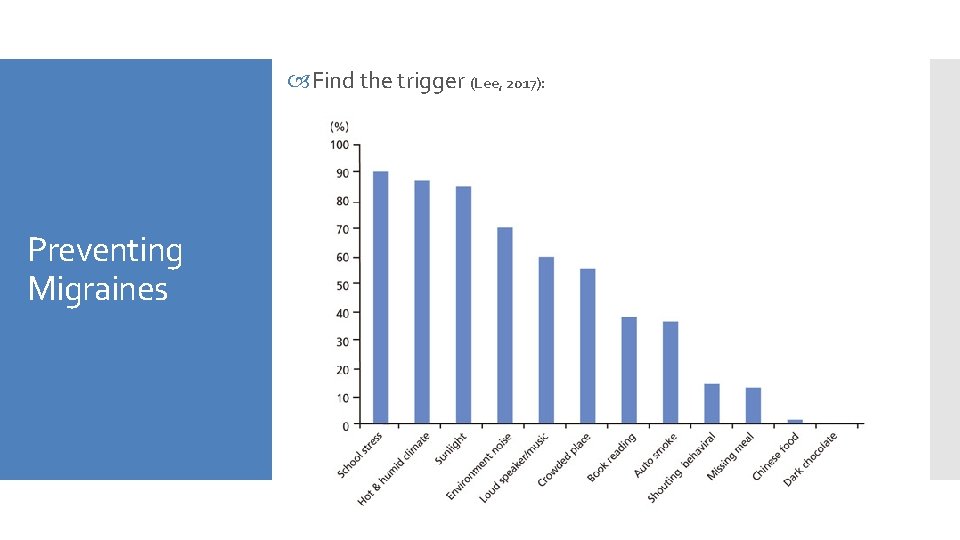
Find the trigger (Lee, 2017): Preventing Migraines

Consider: Quality of life (QOL) Degree of disability HA characteristics: frequency, severity, duration When to prevent… Generally, 1. If the patient has two (2) or more headaches per week that are associated with disability or 2. > 3 incapacitating headaches per month or 3. If the headache is predictable (ex. premenstrual migraine) Prophylaxis takes up to 4 -6 months to reduce HA frequency

Preventative treatments Antidepressants Antihypertensives Antiepileptics Antihistamines Other

BLACK BOX WARNING Antidepressants Tricyclic Antidepressants (TCAs) Amitriptyline 0. 25 - 1 mg/kg/day; dose at bedtime; start low and increase to max of 75 mg/day Nortriptyline similar dosing to above; not as sedating Antidepressants & Antihypertensives (Hickman, Lewis, Little, Rastogi, & Yonker, 2015) SSRIs more beneficial in adults than children Antihypertensives Beta Blockers: Propranolol 0. 5 -1 mg/kg/day divided BID (Initial MAX 80 mg/day) or Atenolol 0. 5 -1 mg/kg/day divided BID (Initial MAX 50 mg/day) Calcium Channel Blockers: Verapamil 2 -3 mg/kg/day divided BID (Initial MAX 240 mg/day)

Antieplieptics Topiramate – approved in children >12 for migraine; 2 -3 mg/kg/day; MAX 200 mg/day Antiepileptics CAUTION in girls of child bearing age Kidney stones, word finding difficulties Increase dose slowly Valproic Acid – used in adults for migraine prevention; 10 -20 mg/kg/day; MAX 1000 mg CAUTION in girls of child bearing age Thrombocytopenia Weight gain! BLACK BOX WARNING

Cyproheptadine: Antihistamines Used since the 1970’s in children to prevent headaches Usually for younger children 0. 2 -0. 4 mg/kg/day dosed at night SEDATION Appetite stimulant

Botulinum toxin Fluid Drink at least 6 cups (1. 5 L) of water daily Remover or reduce caffeine from the diet Other Treatments Sleep Maintain a regular sleep pattern every day Diet and exercise Eat 3 meals a day, do NOT skip meals Eat a protein source for breakfast Mind and body Accupuncture Biobehavior techniques are beneficial Relaxation training Biofeedback Cognitive behavior therapy Stress management Supplements Magnesium Oxide 9 mg/kg/day BID (MAX 600 mg/day) Maintain a healthy body weight Coenzyme Q 10 1 -3 mg/kg/day daily (MAX 150 mg/day) Exercise for 30 minutes daily Vitamin B 2 200 -400 mg/day daily

Abnormal brain imaging Migraines with unusual neurological symptoms Chronic migraines 15 or more headaches a month for three months or longer, often as a result of medication overuse When to refer Intractable migraines Migraines not helped by medications Any headache outside the clinical criteria for migraine or tensiontype headache There are more than 200 different types of headache disorders in the International Classification of Headache Disorders. Although migraines and tension-type headaches are most common, there a myriad of other headache disorders.

Do not be afraid to start approved or recommended treatments, both acute and preventative… But… It may take months for preventative medications to take effect!

Lee, K. H. (2017). Recent updates on treatment for pediatric migraine. J Korean Med Association. Feb; 60(2): 118 -125. https: //doi. org/10. 5124/jkma. 2017. 60. 2. 118 National Guideline Clearinghouse (NGC). Guideline summary: Headaches: diagnosis and management of headaches in young people and adults. In: National Guideline Clearinghouse (NGC) [Web site]. Rockville (MD): Agency for Healthcare Research and Quality (AHRQ); 2012 Sep 01. [cited 2018 Jan 20]. Available: https: //www. guideline. gov
- Slides: 32