Midterm outcomes after percutaneous interventions in coronary bifurcations

Mid-term outcomes after percutaneous interventions in coronary bifurcations Alaide Chieffo MD Reaserch director Interventional Cardiology Unit IRCCS San Raffaele Scientific Institute Milan, Italy

I have the following potentially relevant disclosures: Consulting, speaker honorarium: • • • Abiomed Abbott Biosensor Cardinal Health GADA Magenta • Coinventor and cofounder Cephea Valve Technology
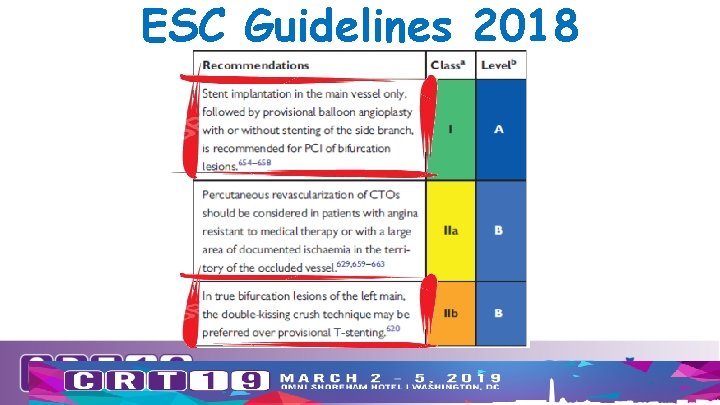

ESC Guidelines 2018
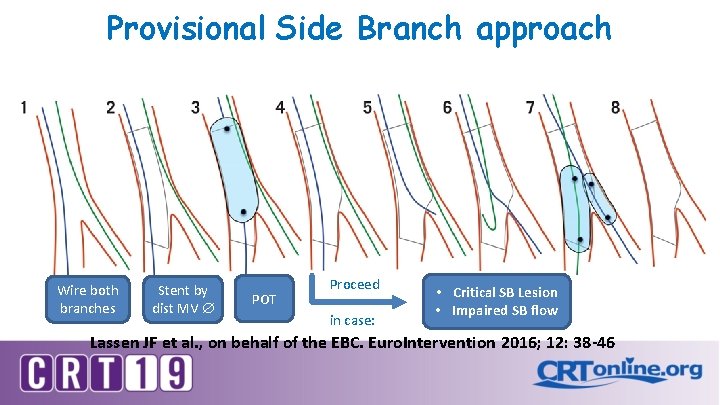
Provisional Side Branch approach Wire both branches Stent by dist MV POT Proceed in case: • Critical SB Lesion • Impaired SB flow Lassen JF et al. , on behalf of the EBC. Euro. Intervention 2016; 12: 38 -46
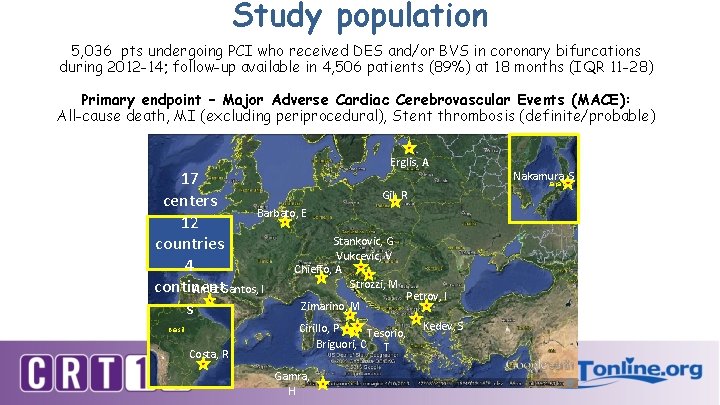
Study population 5, 036 pts undergoing PCI who received DES and/or BVS in coronary bifurcations during 2012 -14; follow-up available in 4, 506 patients (89%) at 18 months (IQR 11 -28) Primary endpoint – Major Adverse Cardiac Cerebrovascular Events (MACE): All-cause death, MI (excluding periprocedural), Stent thrombosis (definite/probable) Erglis, A 17 Gil, R centers Barbato, E 12 Stankovic, G countries Vukcevic, V 4 Chieffo, A Strozzi, M continent Amat-Santos, I Petrov, I Zimarino, M s Brasil Costa, R Cirillo, P Tesorio, Briguori, C T Gamra, H Kedev, S Nakamura, S Japan

Methods • • The choice of DES or BVS and the treatment strategy were left to the individual operator’s discretion. Stent Strategy: – Single-stenting: MB or SB – Double-stenting: both MB and SB. – Bail-out stenting: any stent deployed beyond the planned strategy, with either one or double stenting. True bifurcation = Medina 1. 1. 1/1. 0. 1/0. 1. 1 After PCI, aspirin was continued indefinitely, and the duration of P 2 Y 12 inhibitors was recommended at physician’s judgement.
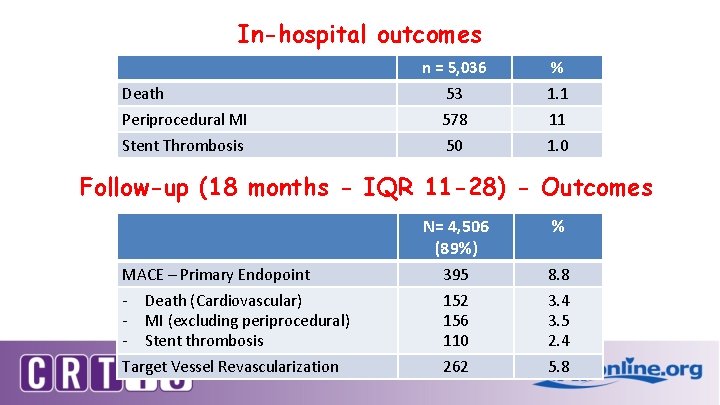
In-hospital outcomes n = 5, 036 % Death 53 1. 1 Periprocedural MI 578 11 Stent Thrombosis 50 1. 0 Follow-up (18 months - IQR 11 -28) - Outcomes N= 4, 506 (89%) % MACE – Primary Endopoint 395 8. 8 - Death (Cardiovascular) - MI (excluding periprocedural) - Stent thrombosis Target Vessel Revascularization 152 156 110 3. 4 3. 5 2. 4 262 5. 8
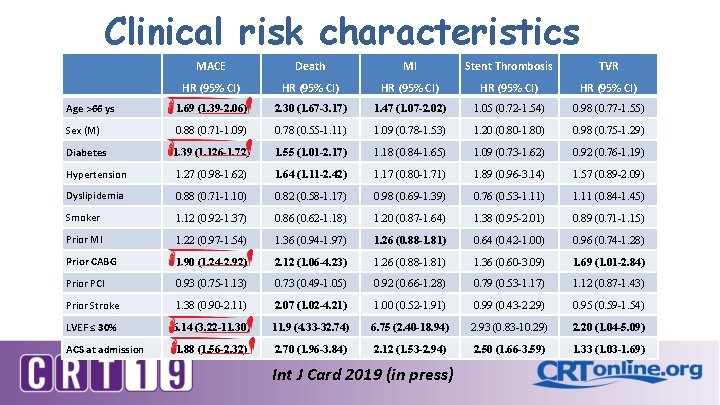
Clinical risk characteristics MACE Death MI Stent Thrombosis TVR HR (95% CI) HR (95% CI) Age >66 ys 1. 69 (1. 39 -2. 06) 2. 30 (1. 67 -3. 17) 1. 47 (1. 07 -2. 02) 1. 05 (0. 72 -1. 54) 0. 98 (0. 77 -1. 55) Sex (M) 0. 88 (0. 71 -1. 09) 0. 78 (0. 55 -1. 11) 1. 09 (0. 78 -1. 53) 1. 20 (0. 80 -1. 80) 0. 98 (0. 75 -1. 29) Diabetes 1. 39 (1. 126 -1. 72) 1. 55 (1. 01 -2. 17) 1. 18 (0. 84 -1. 65) 1. 09 (0. 73 -1. 62) 0. 92 (0. 76 -1. 19) Hypertension 1. 27 (0. 98 -1. 62) 1. 64 (1. 11 -2. 42) 1. 17 (0. 80 -1. 71) 1. 89 (0. 96 -3. 14) 1. 57 (0. 89 -2. 09) Dyslipidemia 0. 88 (0. 71 -1. 10) 0. 82 (0. 58 -1. 17) 0. 98 (0. 69 -1. 39) 0. 76 (0. 53 -1. 11) 1. 11 (0. 84 -1. 45) Smoker 1. 12 (0. 92 -1. 37) 0. 86 (0. 62 -1. 18) 1. 20 (0. 87 -1. 64) 1. 38 (0. 95 -2. 01) 0. 89 (0. 71 -1. 15) Prior MI 1. 22 (0. 97 -1. 54) 1. 36 (0. 94 -1. 97) 1. 26 (0. 88 -1. 81) 0. 64 (0. 42 -1. 00) 0. 96 (0. 74 -1. 28) Prior CABG 1. 90 (1. 24 -2. 92) 2. 12 (1. 06 -4. 23) 1. 26 (0. 88 -1. 81) 1. 36 (0. 60 -3. 09) 1. 69 (1. 01 -2. 84) Prior PCI 0. 93 (0. 75 -1. 13) 0. 73 (0. 49 -1. 05) 0. 92 (0. 66 -1. 28) 0. 79 (0. 53 -1. 17) 1. 12 (0. 87 -1. 43) Prior Stroke 1. 38 (0. 90 -2. 11) 2. 07 (1. 02 -4. 21) 1. 00 (0. 52 -1. 91) 0. 99 (0. 43 -2. 29) 0. 95 (0. 59 -1. 54) LVEF ≤ 30% 6. 14 (3. 22 -11. 30) 11. 9 (4. 33 -32. 74) 6. 75 (2. 40 -18. 94) 2. 93 (0. 83 -10. 29) 2. 20 (1. 04 -5. 09) ACS at admission 1. 88 (1. 56 -2. 32) 2. 70 (1. 96 -3. 84) 2. 12 (1. 53 -2. 94) 2. 50 (1. 66 -3. 59) 1. 33 (1. 03 -1. 69) Int J Card 2019 (in press)
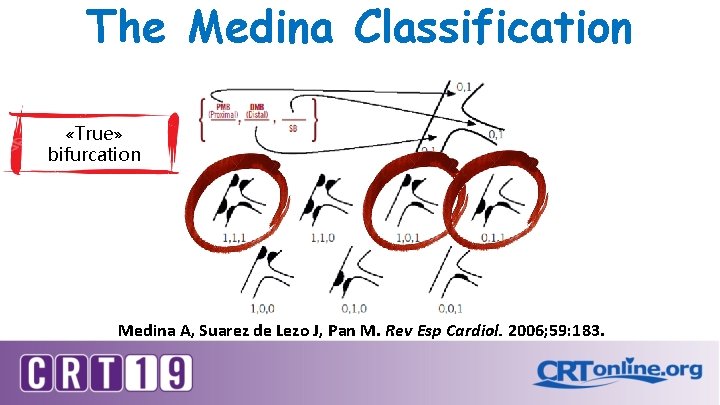
The Medina Classification «True» bifurcation Medina A, Suarez de Lezo J, Pan M. Rev Esp Cardiol. 2006; 59: 183.
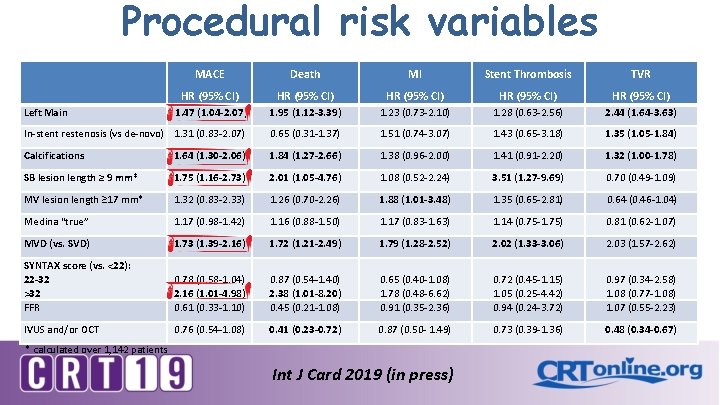
Procedural risk variables MACE Death MI Stent Thrombosis TVR HR (95% CI) HR (95% CI) 1. 47 (1. 04 -2. 07) 1. 95 (1. 12 -3. 39) 1. 23 (0. 73 -2. 10) 1. 28 (0. 63 -2. 56) 2. 44 (1. 64 -3. 63) In-stent restenosis (vs de-novo) 1. 31 (0. 83 -2. 07) 0. 65 (0. 31 -1. 37) 1. 51 (0. 74 -3. 07) 1. 43 (0. 65 -3. 18) 1. 35 (1. 05 -1. 84) Calcifications 1. 64 (1. 30 -2. 06) 1. 84 (1. 27 -2. 66) 1. 38 (0. 96 -2. 00) 1. 41 (0. 91 -2. 20) 1. 32 (1. 00 -1. 78) SB lesion length ≥ 9 mm* 1. 75 (1. 16 -2. 73) 2. 01 (1. 05 -4. 76) 1. 08 (0. 52 -2. 24) 3. 51 (1. 27 -9. 69) 0. 70 (0. 49 -1. 09) MV lesion length ≥ 17 mm* 1. 32 (0. 83 -2. 33) 1. 26 (0. 70 -2. 26) 1. 88 (1. 01 -3. 48) 1. 35 (0. 65 -2. 81) 0. 64 (0. 46 -1. 04) Medina “true” 1. 17 (0. 98 -1. 42) 1. 16 (0. 88 -1. 50) 1. 17 (0. 83 -1. 63) 1. 14 (0. 75 -1. 75) 0. 81 (0. 62 -1. 07) MVD (vs. SVD) 1. 73 (1. 39 -2. 16) 1. 72 (1. 21 -2. 49) 1. 79 (1. 28 -2. 52) 2. 02 (1. 33 -3. 06) 2. 03 (1. 57 -2. 62) SYNTAX score (vs. <22): 22 -32 >32 FFR 0. 78 (0. 58 -1. 04) 2. 16 (1. 01 -4. 98) 0. 61 (0. 33 -1. 10) 0. 87 (0. 54 -1. 40) 2. 38 (1. 01 -8. 20) 0. 45 (0. 21 -1. 08) 0. 65 (0. 40 -1. 08) 1. 78 (0. 48 -6. 62) 0. 91 (0. 35 -2. 36) 0. 72 (0. 45 -1. 15) 1. 05 (0. 25 -4. 42) 0. 94 (0. 24 -3. 72) 0. 97 (0. 34 -2. 58) 1. 08 (0. 77 -1. 08) 1. 07 (0. 55 -2. 23) IVUS and/or OCT 0. 76 (0. 54 -1. 08) 0. 41 (0. 23 -0. 72) 0. 87 (0. 50 - 1. 49) 0. 73 (0. 39 -1. 36) 0. 48 (0. 34 -0. 67) Left Main * calculated over 1, 142 patients Int J Card 2019 (in press)
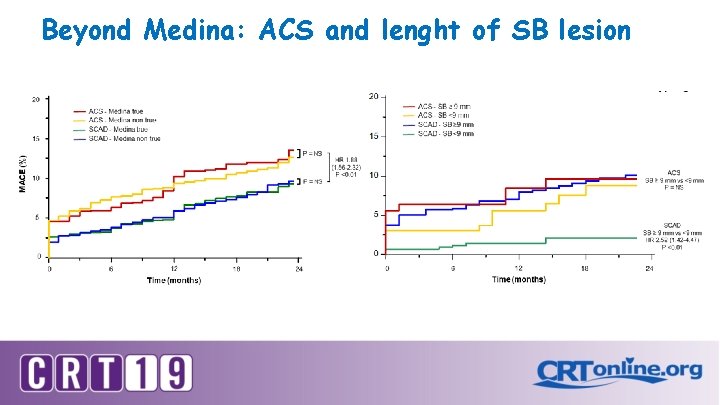
Beyond Medina: ACS and lenght of SB lesion
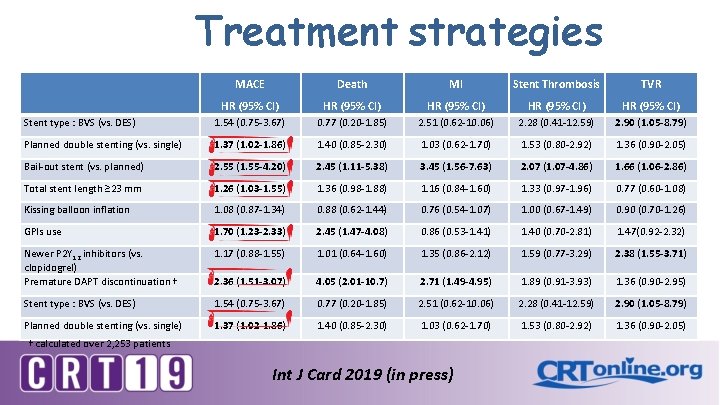
Treatment strategies MACE Death MI Stent Thrombosis TVR HR (95% CI) HR (95% CI) Stent type : BVS (vs. DES) 1. 54 (0. 75 -3. 67) 0. 77 (0. 20 -1. 85) 2. 51 (0. 62 -10. 06) 2. 28 (0. 41 -12. 59) 2. 90 (1. 05 -8. 79) Planned double stenting (vs. single) 1. 37 (1. 02 -1. 86) 1. 40 (0. 85 -2. 30) 1. 03 (0. 62 -1. 70) 1. 53 (0. 80 -2. 92) 1. 36 (0. 90 -2. 05) Bail-out stent (vs. planned) 2. 55 (1. 55 -4. 20) 2. 45 (1. 11 -5. 38) 3. 45 (1. 56 -7. 63) 2. 07 (1. 07 -4. 86) 1. 66 (1. 06 -2. 86) Total stent length ≥ 23 mm 1. 26 (1. 03 -1. 55) 1. 36 (0. 98 -1. 88) 1. 16 (0. 84 -1. 60) 1. 33 (0. 97 -1. 96) 0. 77 (0. 60 -1. 08) Kissing balloon inflation 1. 08 (0. 87 -1. 34) 0. 88 (0. 62 -1. 44) 0. 76 (0. 54 -1. 07) 1. 00 (0. 67 -1. 49) 0. 90 (0. 70 -1. 26) GPIs use 1. 70 (1. 23 -2. 33) 2. 45 (1. 47 -4. 08) 0. 86 (0. 53 -1. 41) 1. 40 (0. 70 -2. 81) 1. 47(0. 92 -2. 32) Newer P 2 Y 12 inhibitors (vs. clopidogrel) Premature DAPT discontinuation † 1. 17 (0. 88 -1. 55) 1. 01 (0. 64 -1. 60) 1. 35 (0. 86 -2. 12) 1. 59 (0. 77 -3. 29) 2. 38 (1. 55 -3. 71) 2. 36 (1. 51 -3. 07) 4. 05 (2. 01 -10. 7) 2. 71 (1. 49 -4. 95) 1. 89 (0. 91 -3. 93) 1. 36 (0. 90 -2. 95) Stent type : BVS (vs. DES) 1. 54 (0. 75 -3. 67) 0. 77 (0. 20 -1. 85) 2. 51 (0. 62 -10. 06) 2. 28 (0. 41 -12. 59) 2. 90 (1. 05 -8. 79) Planned double stenting (vs. single) 1. 37 (1. 02 -1. 86) 1. 40 (0. 85 -2. 30) 1. 03 (0. 62 -1. 70) 1. 53 (0. 80 -2. 92) 1. 36 (0. 90 -2. 05) † calculated over 2, 253 patients Int J Card 2019 (in press)
Treatment strategy in “true” Medina strongly depends on SB lesion
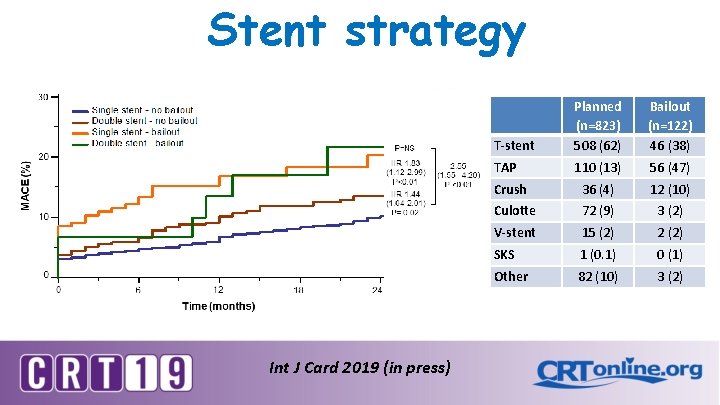
Stent strategy Int J Card 2019 (in press) T-stent Planned (n=823) 508 (62) Bailout (n=122) 46 (38) TAP 110 (13) 56 (47) Crush 36 (4) 12 (10) Culotte 72 (9) 3 (2) V-stent 15 (2) 2 (2) SKS 1 (0. 1) 0 (1) Other 82 (10) 3 (2)
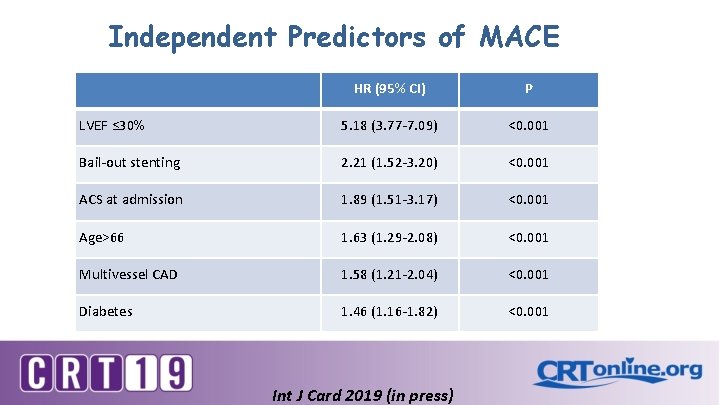
Independent Predictors of MACE HR (95% CI) P LVEF ≤ 30% 5. 18 (3. 77 -7. 09) <0. 001 Bail-out stenting 2. 21 (1. 52 -3. 20) <0. 001 ACS at admission 1. 89 (1. 51 -3. 17) <0. 001 Age>66 1. 63 (1. 29 -2. 08) <0. 001 Multivessel CAD 1. 58 (1. 21 -2. 04) <0. 001 Diabetes 1. 46 (1. 16 -1. 82) <0. 001 Int J Card 2019 (in press)
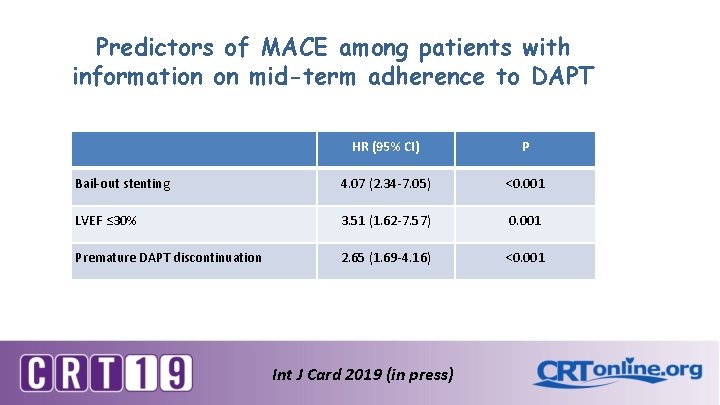
Predictors of MACE among patients with information on mid-term adherence to DAPT HR (95% CI) P Bail-out stenting 4. 07 (2. 34 -7. 05) <0. 001 LVEF ≤ 30% 3. 51 (1. 62 -7. 57) 0. 001 Premature DAPT discontinuation 2. 65 (1. 69 -4. 16) <0. 001 Int J Card 2019 (in press)
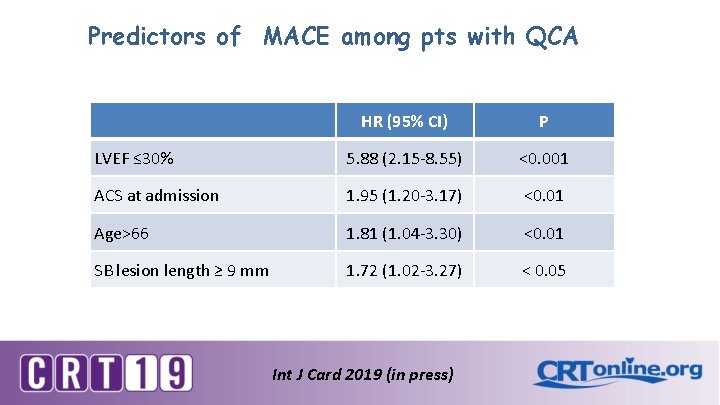
Predictors of MACE among pts with QCA HR (95% CI) P LVEF ≤ 30% 5. 88 (2. 15 -8. 55) <0. 001 ACS at admission 1. 95 (1. 20 -3. 17) <0. 01 Age>66 1. 81 (1. 04 -3. 30) <0. 01 SB lesion length ≥ 9 mm 1. 72 (1. 02 -3. 27) < 0. 05 Int J Card 2019 (in press)
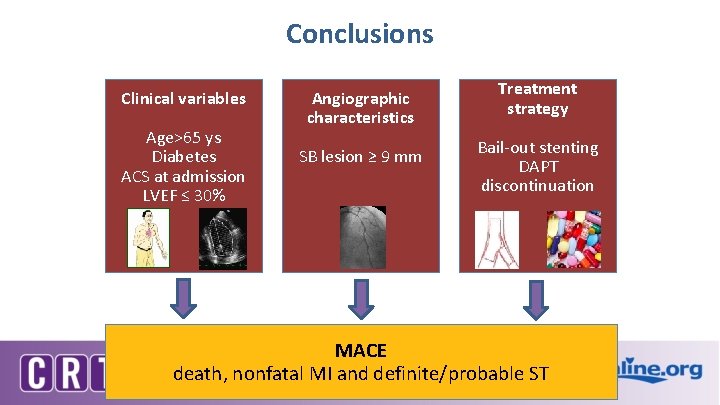
Conclusions Clinical variables Age>65 ys Diabetes ACS at admission LVEF ≤ 30% Angiographic characteristics SB lesion ≥ 9 mm Treatment strategy Bail-out stenting DAPT discontinuation MACE death, nonfatal MI and definite/probable ST
- Slides: 18