Microcytic Anemias Submitted February 2019 TOPIC Overview SLIDE

Microcytic Anemias Submitted: February, 2019
TOPIC Overview SLIDE 4 -6 Iron Deficiency - Overview 11 -14 Iron Deficiency - Overview 16 Iron Deficiency - Diagnosis 18 Iron Deficiency - Treatment 20 -22 Thalassemias - Reproduction 33 -36 When in presentation mode, click this button to advance to each sex and gender difference slide. Sex & Gender Difference Slides

Overview Microcytic Anemias

• Anemia is defined as: • hemoglobin <12 g/d. L in females and <13 g/d. L in males 1 • Anemias based on morphology: 2 • Microcytic- MCV <80 f. L • Normocytic- MCV 80 -100 f. L • Macrocytic- MCV >100 f. L • Anemia is more prevalent in females 3 Anemia Overview

Most Common Causes of Anemias in Females Worldwide: 1 • Iron deficiency anemia due to: menstrual blood loss and childbirth, uterine bleeding disorders • Hemoglobinopathies • GI losses • Gynecological conditions • Other nutritional deficiencies • Anemia second to chronic disease • Aplastic anemia • Anemia secondary to infiltrative disorder Anemias in Females

Most Common Causes of Anemias in Males Worldwide: 1 • • Iron deficiency anemia Hemoglobinopathies GI losses Tropical diseases bleeding from duodenal ulcer Anemias in Males
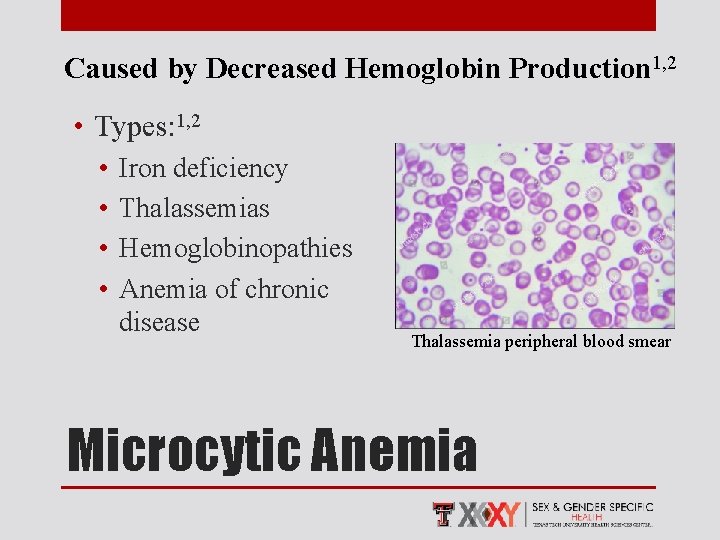
Caused by Decreased Hemoglobin Production 1, 2 • Types: 1, 2 • • Iron deficiency Thalassemias Hemoglobinopathies Anemia of chronic disease Thalassemia peripheral blood smear Microcytic Anemia
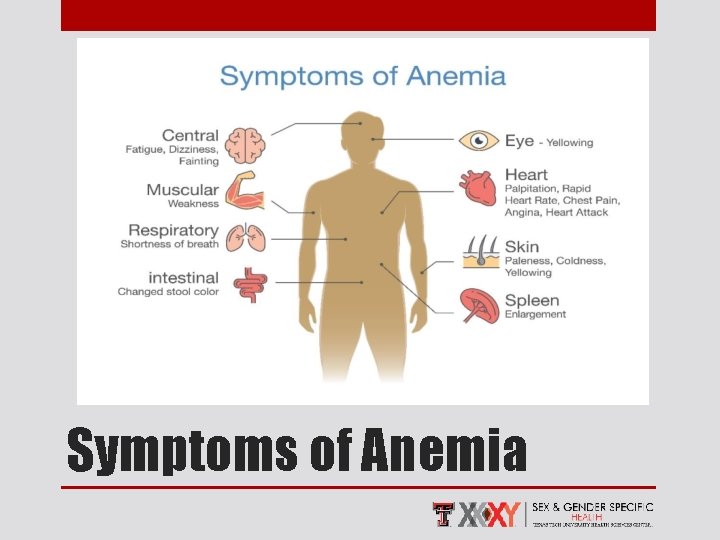
Symptoms of Anemia

Microcytic Anemia Workup

Iron Deficiency Anemia

• Affects >20% of • Global prevalence reproductive aged 38% in pregnant females 2 women 2 • 40% prevalence in • Affects <1% of preschool aged males in the same children 3 age group 4 Epidemiology

• Adolescent/adult females of childbearing age every 5 -10 years 1 • No screening needed for males or post-menopausal females 1, 2 • First prenatal visit 1, 2 Screening
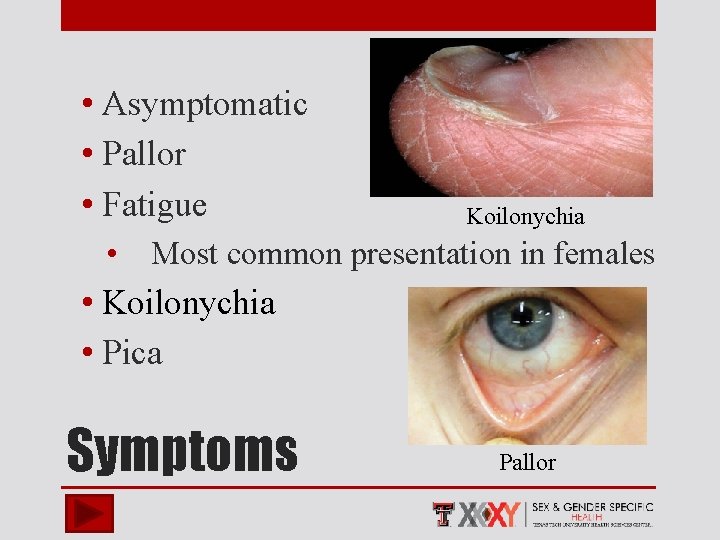
• Asymptomatic • Pallor • Fatigue Koilonychia • Most common presentation in females • Koilonychia • Pica Symptoms Pallor

• Occult blood loss • Insufficient oral intake of iron • Poor gastrointestinal absorption of iron • Pregnancy and delivery Causes
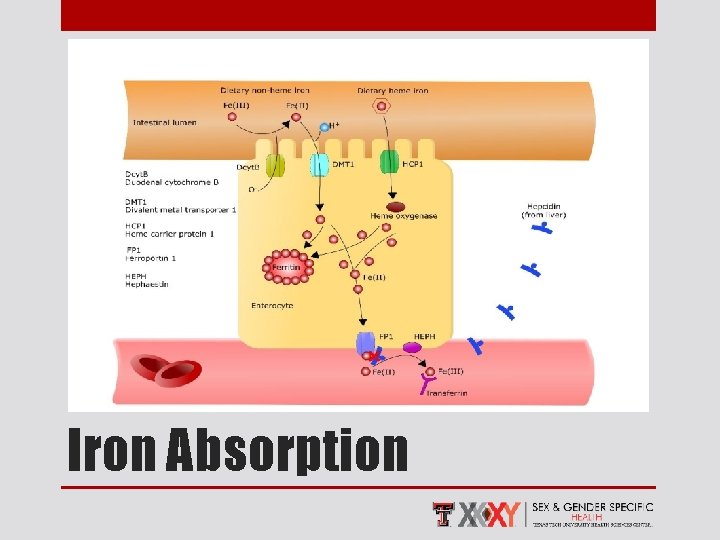
Iron Absorption

• Decreased in premenopausal and menstruating females 1, 2 • Postmenopausal females and males exhibit similar levels 1, 2 Hepcidin

Diagnosis Anemia
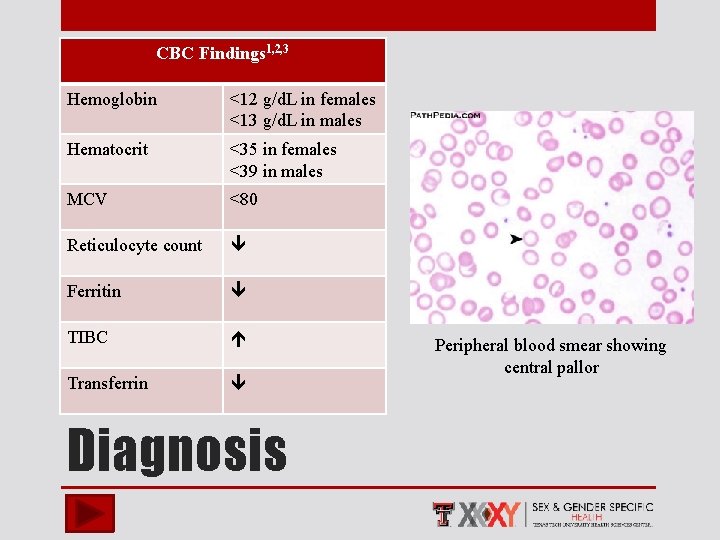
CBC Findings 1, 2, 3 Hemoglobin <12 g/d. L in females <13 g/d. L in males Hematocrit <35 in females <39 in males MCV <80 Reticulocyte count Ferritin TIBC Transferrin Diagnosis Peripheral blood smear showing central pallor

Treatment Anemia

• Oral iron supplementation 1, 2 • Increase dietary iron intake 1, 2 Daily Recommendations 1 Men 8 mg Women 18 mg Pregnant 27 mg Women Treatment

• Impaired cognitive function 1 • Perinatal complications 1 • Increased falls in the elderly 1 • Strong predictor of GI cancer in males and postmenopausal females 2 Complications Colon cancer

• Associated with increased maternal and neonatal morbidity and mortality 1 • Increased risk of: 1 • Prematurity • Low birth weight • Peripartum blood loss Pregnancy and Anemia

Thalassemias Anemia

Absent or Defective α chain Production 1, 2 α-Thalassemia Pathogenesis

Absent or Defective β chain Production 1, 2 Clinical Classification Genotype Normal β/β Minor β/β 0 β/β+ Intermedia β 0/β+ Major β 0/β 0 or β+/β+ β-Thalassemia Pathogenesis

Diagnosis Anemia

Silent Carrier α-thalassemia Hemoglobin H Hydrops fetalis/ αtrait thalassemia major Hemoglobin Normal 7 -10 g/d. L Reticulocyte count Normal 5 -10% MCV 75 -85 f. L 65 -75 f. L 55 -65 f. L MCH 26 pg 22 pg 20 pg Peripheral smear - - Target cells 4 -10 g/d. L 110 -120 f. L Severe anisopoikilo -cytosis and nucleated RBCs α-Thalassemia Diagnosis
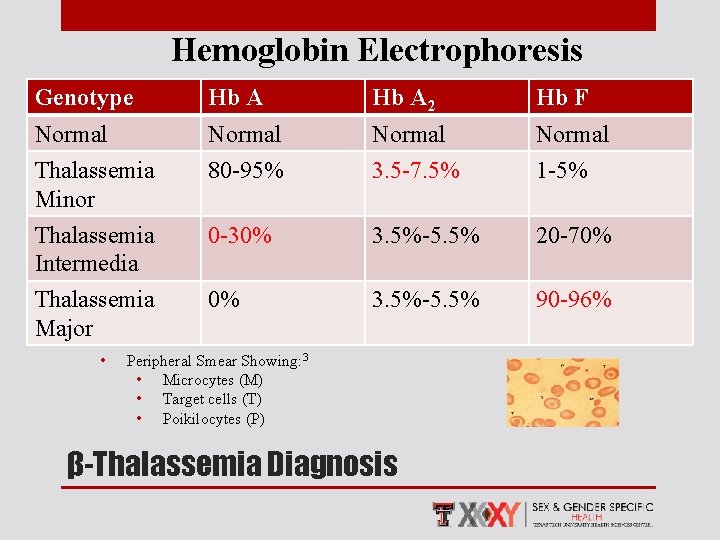
Hemoglobin Electrophoresis Genotype Hb A 2 Hb F Normal Thalassemia Minor 80 -95% 3. 5 -7. 5% 1 -5% Thalassemia Intermedia 0 -30% 3. 5%-5. 5% 20 -70% Thalassemia Major 0% 3. 5%-5. 5% 90 -96% • Peripheral Smear Showing: 3 • Microcytes (M) • Target cells (T) • Poikilocytes (P) β-Thalassemia Diagnosis
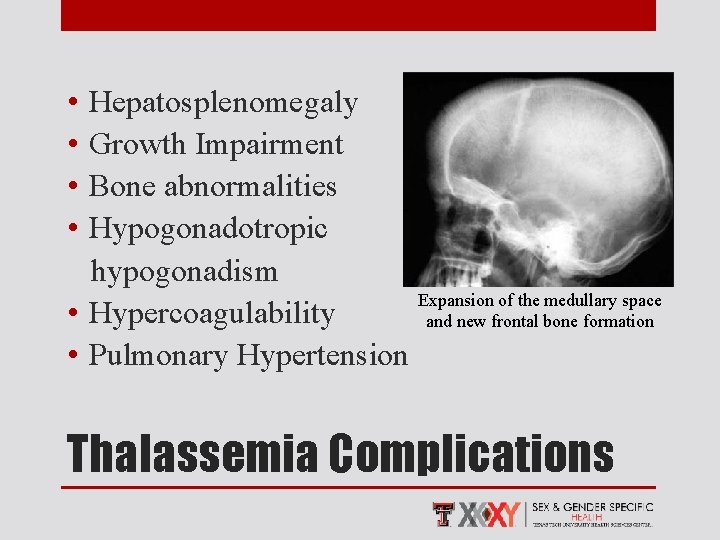
• • Hepatosplenomegaly Growth Impairment Bone abnormalities Hypogonadotropic hypogonadism Expansion of the medullary space • Hypercoagulability and new frontal bone formation • Pulmonary Hypertension Thalassemia Complications

Treatment Anemia
• • Transfusion Splenectomy Iron Chelation Fetal Hemoglobin Inducers • Stem Cell Transplant Thalassemia Treatment

Reproduction Anemia

α-thalassemia retardation (X-linked): 1, 2, 3 • • • Occurs only in males Severe mental retardation Developmental abnormalities Genital abnormalities Classic facies ATR-X

• Caused by iron overload secondary to transfusions and gut absorption 1, 2 • Iron deposition in the pituitary 1, 2 • Iron chelation therapy 1 • Ovulation induction 1 Hypogonadotropic Hypogonadism and Fertility

If undiagnosed in mom: 1, 2, 3 • CBC in prenatal labs • Hemoglobin electrophoresis If undiagnosed in both parents: 1, 3 • Prenatal ultrasound If mutations have been identified in both parents: 2, 3 • Preimplantation genetic diagnosis with IVF • Chorionic villus sampling or amniocentesis Prenatal Diagnosis Hydrops fetalis

• Cardiac impairment • Anticoagulation • Vertical transmission of viruses • Alloimmunization • Fetal Loss Thalassemia and Pregnancy
- Slides: 36