Microbiology of Respiratory Infection II Dr Michael Lockhart

Microbiology of Respiratory Infection II Dr Michael Lockhart

Respiratory Infections of throat and pharynx n Infections of middle ear and sinuses n Infections of trachea and bronchi n Infections of the lungs n

Infections of throat and pharynx Sore throat n Diphtheria n Candida/thrush n Vincent’s angina n

Infections of throat and pharynx n Diagnosis: – Well taken throat swab
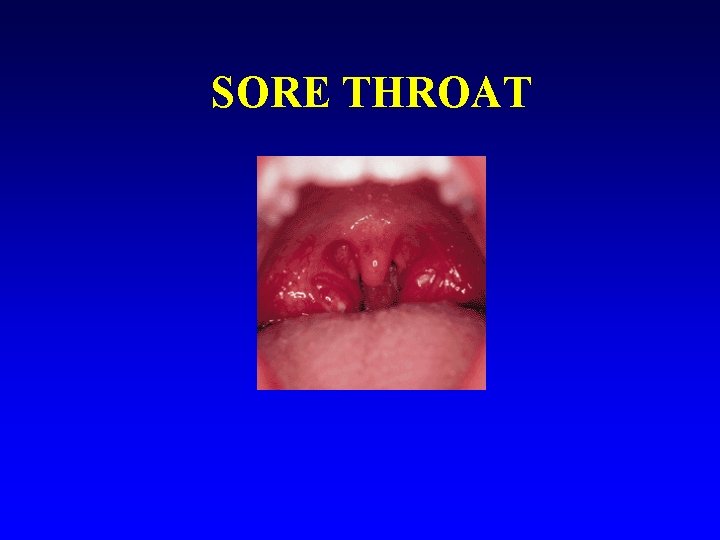
SORE THROAT

Sore throat n VAST MAJORITY (OVER TWO THIRDS) - VIRAL – DO NOT NEED ANTIBIOTICS

Bacterial sore throat n The most common BACTERIAL cause is Streptococcus pyogenes (also known as Group A streptococci) n Clinical: Acute follicular tonsillitis n Treatment: Penicillin
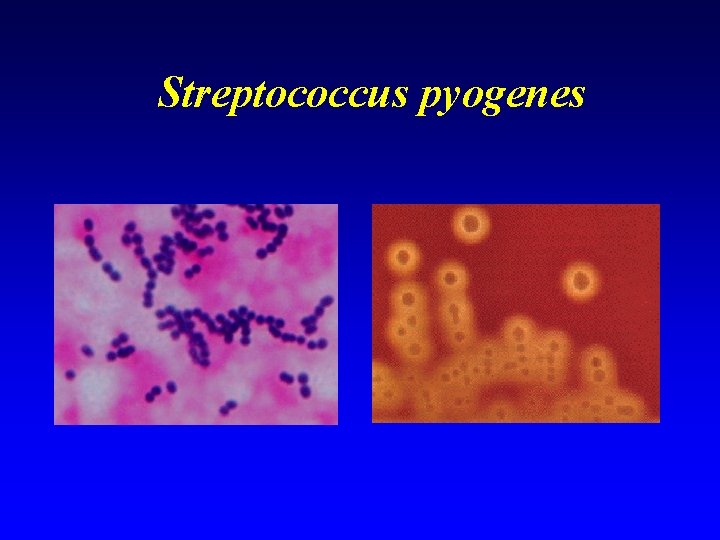
Streptococcus pyogenes

Streptococcal sore throat n Acute complications: – – – Peritonsillar abscess (quinsy) Sinusitis/ otitis media Scarlet fever
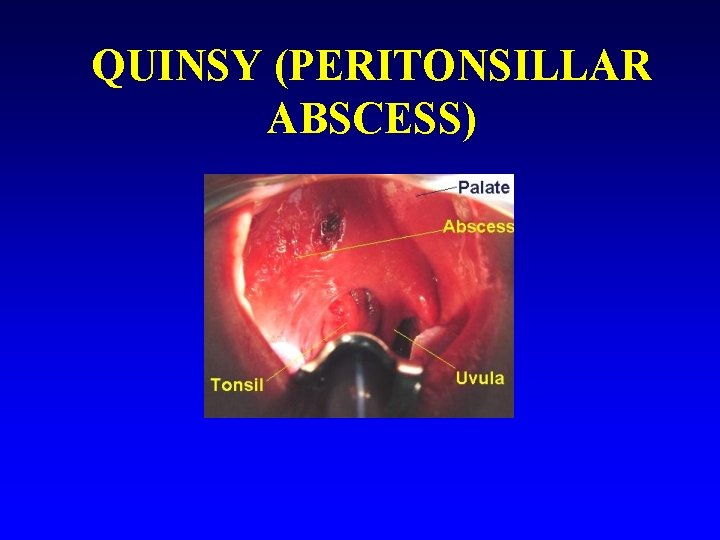
QUINSY (PERITONSILLAR ABSCESS)

Streptococcal sore throat n Late complications – Rheumatic fever n 3 weeks post sore throat n fever, arthritis and pancarditis – Glomerulonephritis n 1 -3 weeks post sore throat n haematuria, albuminuria and oedema

Diphtheria n Corynebacterium diphtheriae n Clinical: Severe sore throat with a grey white membrane across the pharynx. The organism produces a potent exotoxin which is cardiotoxic and neurotoxic.

DIPHTHERIA
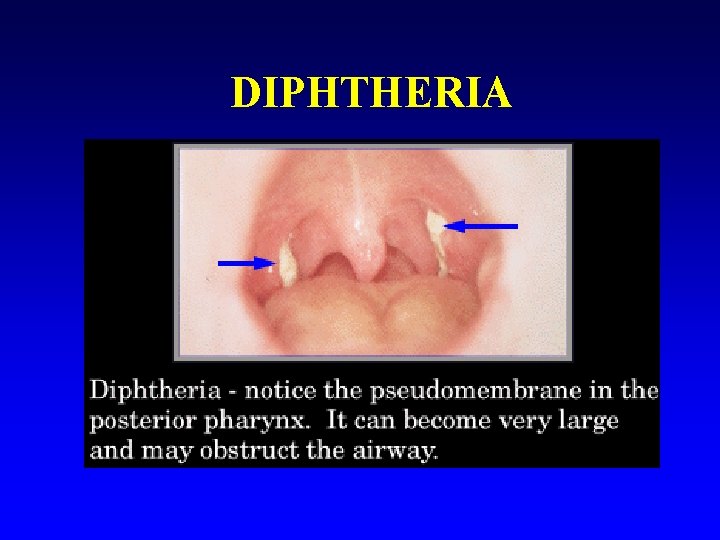
DIPHTHERIA

Diphtheria n Epidemiology : Rare, but increased in certain parts of the world eg Russia n Treatment: Antitoxin and Supportive and Penicillin/erythromycin

Candida/Thrush n Candida albicans n Clinical: White patches on red, raw mucous membranes in throat/ mouth n Cause: endogenous n Treatment: Nystatin
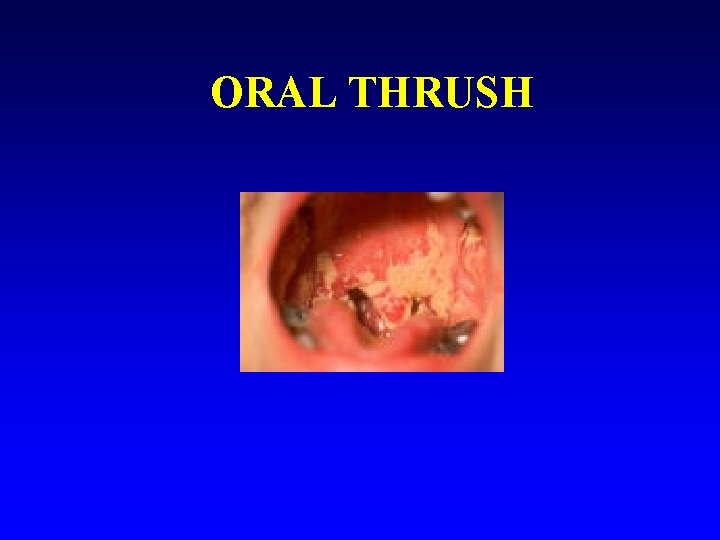
ORAL THRUSH

Vincent’s angina n Mixture of organisms (Borrelia vincenti and Fusobacterium sp. ) n Clinical: Foul smelling mouth and throat ulcers n Treatment: penicillin
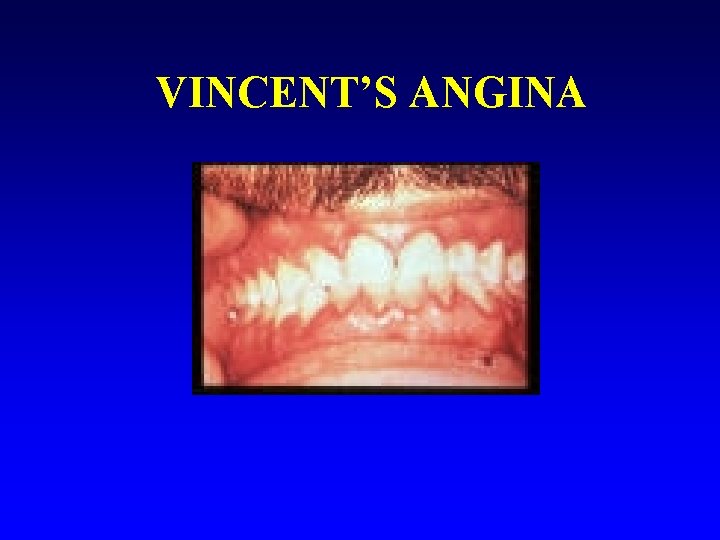
VINCENT’S ANGINA

Respiratory Infections of throat and pharynx n Infections of middle ear and sinuses n Infections of trachea and bronchi n Infections of the lungs n
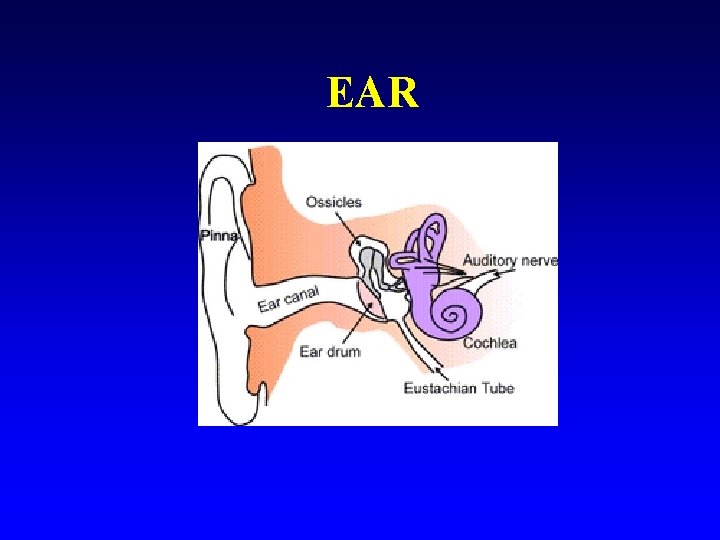
EAR
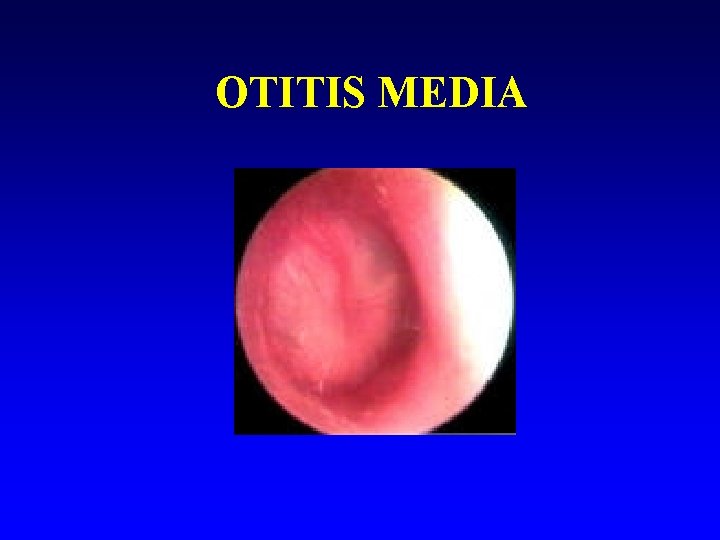
OTITIS MEDIA

Infections of middle ear and sinuses Often viral with bacterial secondary infection n Most common bacteria: Haemophilus influenzae, Streptococcus pneumoniae and Streptococcus pyogenes. n Treat: Amoxycillin n

Respiratory Infections of throat and pharynx n Infections of middle ear and sinuses n Infections of trachea and bronchi n Infections of the lungs n

Infections of trachea and bronchi Acute epiglottitis n Acute exacerbations of COPD n Cystic fibrosis n Pertussis (whooping cough) n

Acute epiglottitis Haemophilus influenzae n Clinical: severe croup in children aged 2 -7 years, may progress to respiratory obstruction and death. n
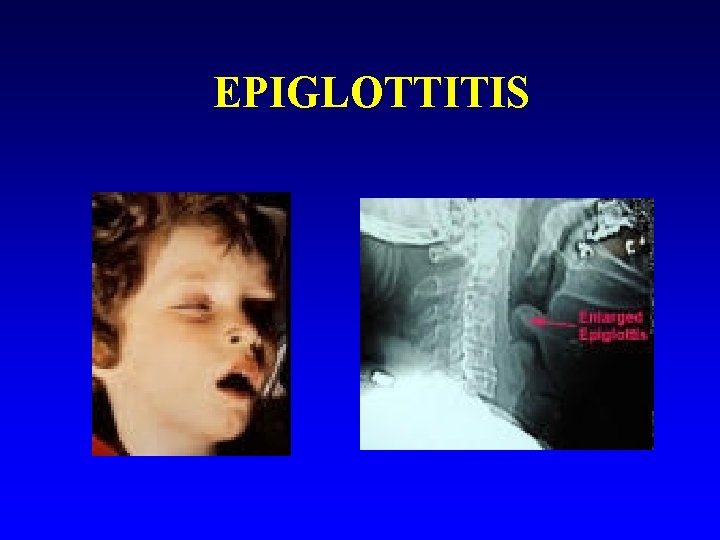
EPIGLOTTITIS
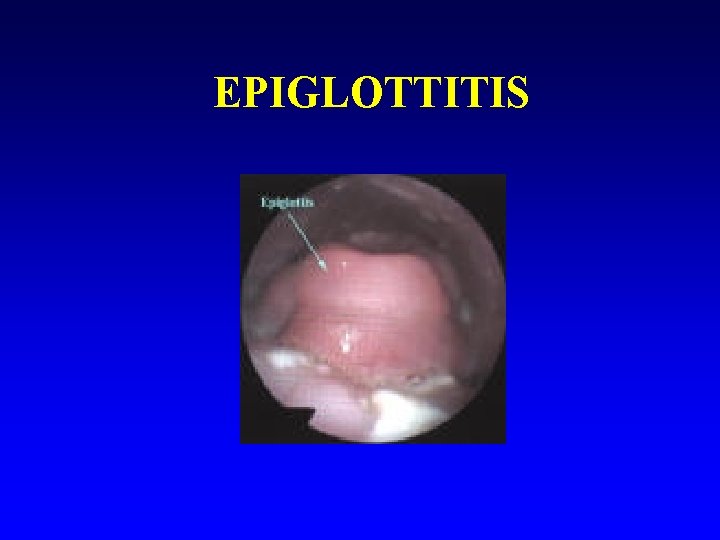
EPIGLOTTITIS

Acute epiglottitis n Microbiology of Haemophilus influenzae – – Habitat - upper respiratory tract Microscopy- small gram negative bacillus Culture - Chocolate agar -small translucent colonies Identify - “X and V test”; H influenzae requires both factors X and V to grow.
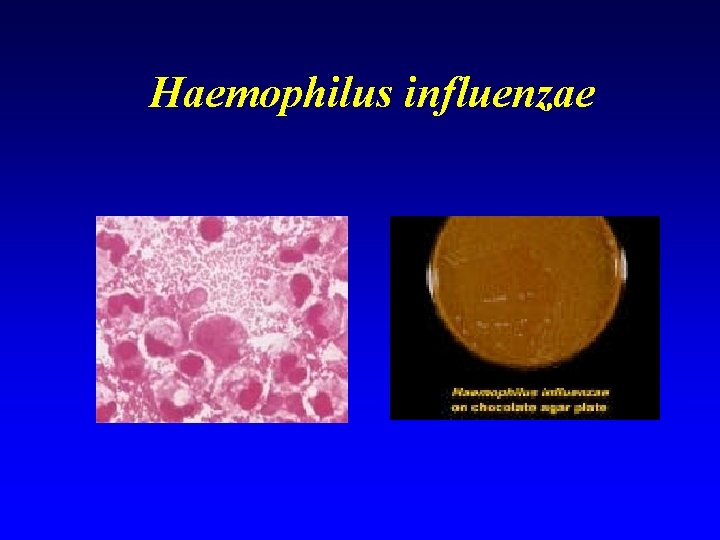
Haemophilus influenzae

Acute epiglottitis n Diagnosis: blood culture (? throat swab) n Treatment: ITU and ceftriaxone

COPD n Acute exacerbations of COPD. – Exacerbations of this chronic condition are often associated with bacterial infection.

Acute exacerbations of COPD Often follow viral infection, or fall in atmospheric temperature with increase in humidity (often in winter) n Clinical: Patients present with increased breathlessness. The volume and purulence of sputum is increased. n

Acute exacerbations of COPD n The most common organisms associated are: – – – n Haemophilus influenzae Streptococcus pneumoniae Moraxella catarrhalis NB All three organisms are present in normal upper respiratory tract flora.

Acute exacerbations of COPD n n Treatment: Give antibiotics if ↑sputum purulence. If no ↑sputum purulence then antibiotics not needed unless consolidation on CXR or signs of pneumonia. 1 ST LINE Amoxicillin 500 mg tds 2 ND LINE Doxycycline 200 mg on day 1 then 100 mg daily (5 days) With time becomes increasingly difficult to treat, due to acquisition of more resistant organisms.

Cystic fibrosis n Inherited defect – leads to abnormally viscid mucus which blocks tubular structures in many different organs including the lungs.

Cystic fibrosis Chronic respiratory infection is a major problem. n Causal bacteria: n – – – Staphylococcus aureus and Haemophilus influenzae Pseudomonas aeruginosa Burkholderia cepacia

Pertussis (whooping cough) Bordetella pertussis n Clinical: Acute tracheobronchitis n – – cold like symptoms for two weeks paroxysmal coughing (2 weeks) n repeated violent exhalations with severe inspiratory whoop, vomiting common – residual cough for month or more

Pertussis (whooping cough) n Diagnosis: – – – n n pernasal swab (charcoal blood agar/ Bordet-Gengou medium) serology clinical ( by the stage of paroxysmal coughing organism numbers much reduced) Treatment: most effective in the first 10 days of illness, also reduces spread to susceptible contacts Vaccination
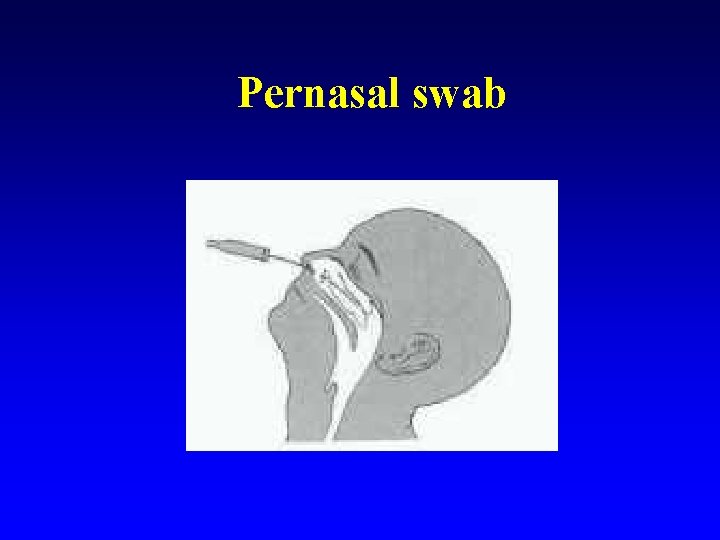
Pernasal swab

Respiratory Infections of throat and pharynx n Infections of middle ear and sinuses n Infections of trachea and bronchi n Infections of the lungs n

Infections of the lungs Community acquired pneumonia n Nosocomial pneumonia n Legionnaires disease n Pneumocysitis carinii pneumonia (PCP) n Fungal chest infection n Tuberculosis n

Community acquired pneumonia Clinical: cough, sputum production, dyspnoea, fever. n Chest x-ray with infiltrates. n Acquired in the community n

Community acquired pneumonia n Causative organisms: – – – Streptococcus pneumoniae Atypicals/viruses Staphylococcus aureus Other bacteria Haemophilus influenzae 70% 20% 4% 1% 5%

Community acquired pneumonia n Streptococcus pneumoniae – Microbiology: n Microscopy - gram positive cocci n Culture - Alpha haemolytic colonies, typically “draughtsmen” ie with sunken centre. n Identify - “Optochin” sensitive – Treatment - generally penicillin sensitive
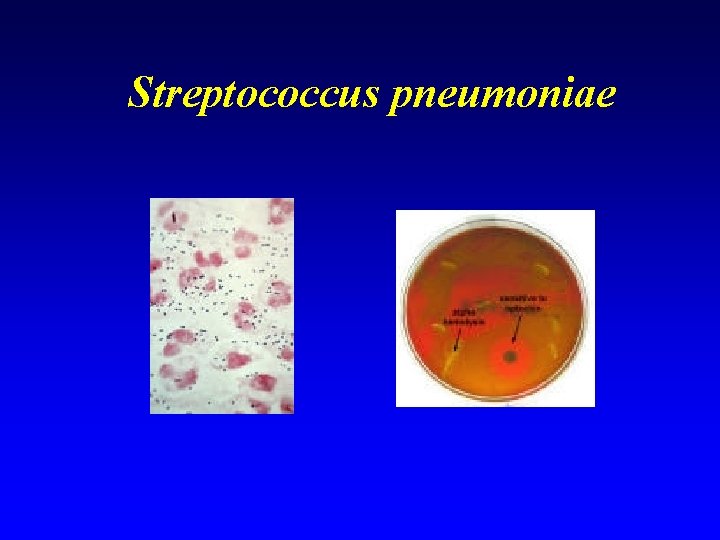
Streptococcus pneumoniae
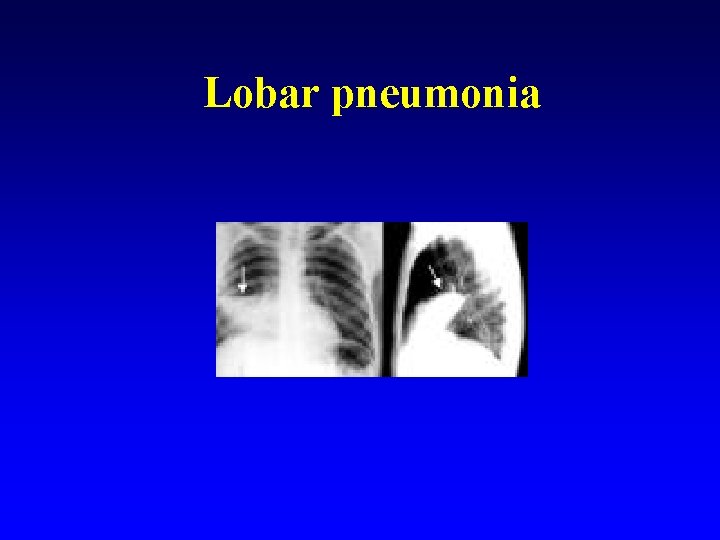
Lobar pneumonia

Community acquired pneumonia “Atypicals” - old term for pneumonias not attributable to any of the common bacterial causes of pneumonia. n Refer to Dr Mc. Intyre’s talk n

Community acquired pneumonia n Treatment , follow the Tayside Critical Care Pathway for the Management of Community-Acquired Pneumonia


CURB 65 SCORE 3 OR MORE (SEVERE) ANTIBIOTICS: SEVERE ·ALL SHOULD INITIALLY RECEIVE: IV CO-AMOXICLAV 1. 2 g x 3/day PLUS IV CLARITHROMYCIN 500 mg x 2/day or PO DOXYCYCLINE 100 mg x 2/day (PENICILLIN ALLERGY: IV Levofloxacin 500 mg 2/day) · Step down to oral doxycycline 100 mg x 2/day in all patients ·ALL SHOULD HAVE: Paired serology, throat swab/gargle for virology PCR, urinary legionella antigen tests ·Treat for at least 10 days (IV/oral)

Nosocomial pneumonia = hospital acquired pneumonia n Predisposing factors: n – – – Intubation Intensive care unit Antibiotics Surgery Immunosuppression

Nosocomial pneumonia n Organisms -60% gram negative organisms : – – n includes Pseudomonas aeruginosa, and Coliforms (such as E. coli, Klebsiella sp) If aspiration pneumonia anaerobes may be involved Treatment – Severe IV Amoxicillin + Metronidazole + Gentamicin n – Step down to Coamoxiclav PO 7 -10 days total Non severe Amoxicillin + Metronidazole for 7 days

Legionnaires disease Legionella pneumophila n Clinical: n – n flu like illness which may progress to a severe pneumonia, with mental confusion, acute renal failure and GI symptoms. Epidemiology – often associated with travel, usually associated with water.

Legionnaires disease Diagnosis: Legionella urinary antigen/ Serology n Treatment: n – – Erythromycin/clarythromycin Fluoroquinolones

Pneumocysitis carinii pneumonia (PCP) A cause of pneumonia in patients with AIDS n Diagnosis: Bronchioalvelar lavage (BAL) or induced sputum and identification of cysts. n Treatment: Cotrimoxazole, pentamidine. n

Fungal chest infection n n Aspergillus fumigatus Clinical: Causes severe pneumonia/systemic infection in the severely immunocompromised. – n n Or aspergilloma Diagnosis : Culture Treatment : iv Amphotereicin B
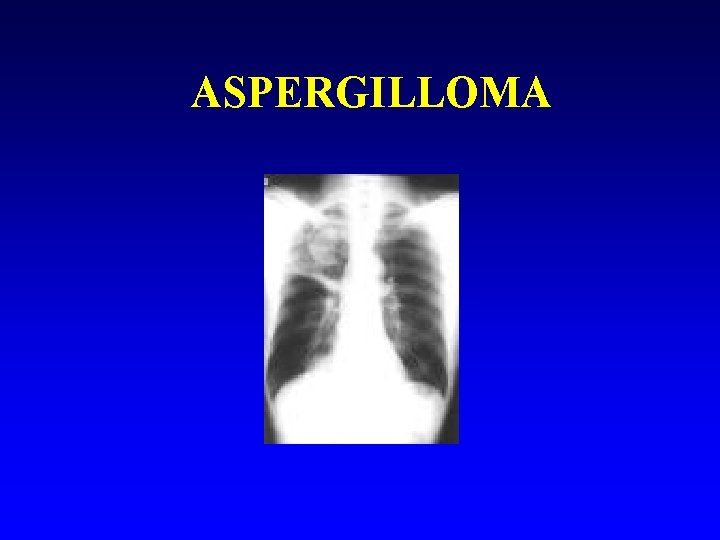
ASPERGILLOMA

TUBERCULOSIS Mycobacterium tuberculosis n Acid Alcohol Fast Bacilli n Bread crumb like growth on special medium, after prolonged (up to 3 months) incubation n

Acid and Alcohol Fast Bacilli (AAFB)

Growing Tuberculosis

Tuberculosis n For more detailed information see Dr Winters Lecture

Infections in lungs General diagnostic points

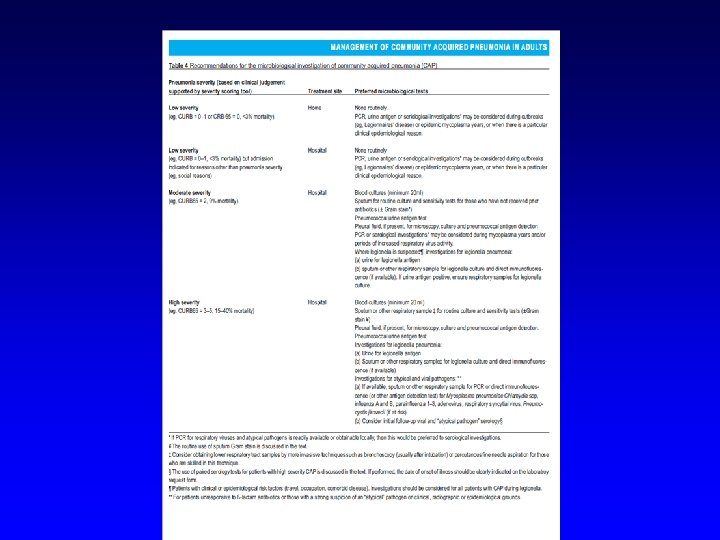

Infections of the lungs Diagnosis n Isolation of causal pathogen – – Sputum NB Quality of sputum sample important Blood culture (organism in blood of one third of patients with pneumonia)

Infections of the lungs Diagnosis n Detection of bacterial antigen – – n eg Legionella urinary antigen Direct immunofluorescence for PCP Serology – eg Legionella serology

Immunisation n UK guidance is summarised in a document called “The Green Book” available online at: – http: //www. dh. gov. uk/Policy. And. Guidance/Hea lth. And. Social. Care. Topics/Green. Book/fs/en

Pneumococcal immunisation n Pneumococcal polysaccharide vaccine covers 23 different capsule types – n Efficacy – 50 -70% reduction of bacteremia risk Pneumococcal conjugate vaccine covers 7 different capsular types – common childhood strains – Efficacy – 97% protection

Pneumococcal immunisation n Indications – – – All those aged 65 years and over Childhood immunisation schedule Risk groups n No spleen n Various chronic diseases including COPD n Immunosuppressed n Patients with CSF shunts
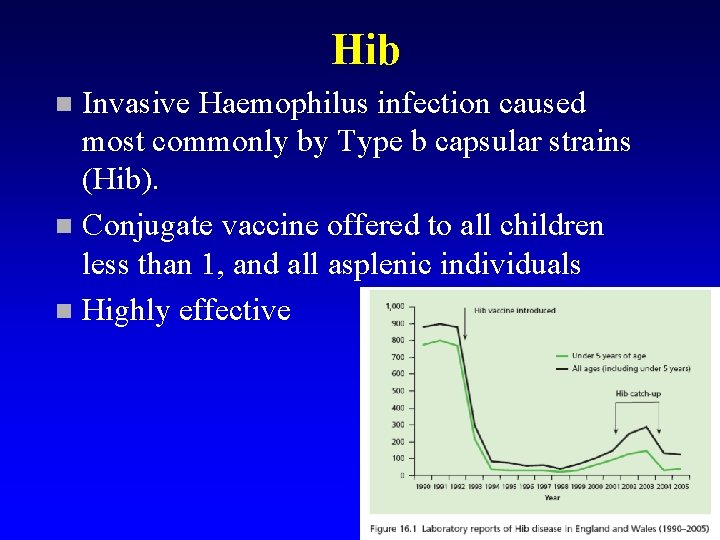
Hib Invasive Haemophilus infection caused most commonly by Type b capsular strains (Hib). n Conjugate vaccine offered to all children less than 1, and all asplenic individuals n Highly effective n

Pertussis immunisation Acellular vaccine – 5 purified pertussis components n Given as part of the childhood immunisation schedule n

Immunisation for Tuberculosis Live attenuated strain of Mycobacterium bovis n UK efficacy of 70% in protecting against TB n Risk based approach to identify those who receive the vaccine n

Community acquired pneumonia n Causative organisms: – – – Streptococcus pneumoniae Atypicals/viruses Staphylococcus aureus Other bacteria Haemophilus influenzae 70% 20% 4% 1% 5%
- Slides: 74