Microbiology of Bone Joint Infections Myositis Myositis refers

Microbiology of Bone & Joint Infections

Myositis �Myositis refers to any condition causing inflammation in one or more muscles �Weakness, swelling, and pain are the most common myositis symptoms �Myositis causes include infection, injury, autoimmune conditions, and drug side effects �Treatment of myositis varies according to the cause

Causes of Myositis �Myositis is caused by any condition that leads to inflammation in the muscles �Myositis causes can be divided into several major categories: �Inflammatory conditions causing myositis �Myositis caused by microbial infection �Myositis caused by drugs �Myositis due to injury

Myositis caused by microbial infection �Known pathogens include the following: �Viral �HIV (one of the most common causes of myositis), HTLV-1, Cytomegalovirus, Coxsackie B virus (epidemic myalgia), Influenza �Bacterial �S. aureus (most common, 70%); Streptococcus viridans; Salmonella enteritidis; Neisseria species , Yersinia species

�Spirochetal �Borrelia burgdorferi �Mycobacterial �Mycobacterium avium �Parasitic �Echinococcus granulosus, Taenia solium, T. cruzi �Fungal �Cryptococcus neoformans, Candida species, Histoplasma capsulatum, Aspergillus species

Symptoms of Myositis �Muscle pain (myalgias) �Dermatomyositis, polymyositis �The weakness affects large muscle groups � including the neck, shoulders, hips, and back Dermatomyositis �The main symptom of myositis is muscle weakness that may be detectable with testing
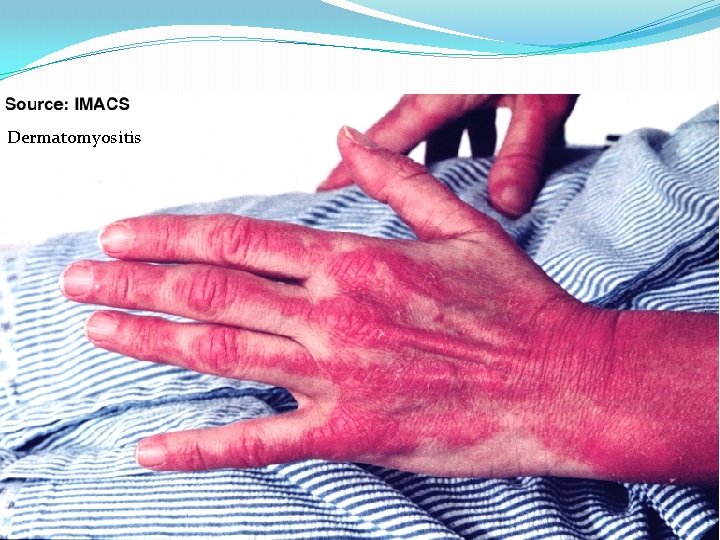
Dermatomyositis

�The weakness from myositis can lead to falls �make it difficult to get up from a chair or after a fall �Other myositis symptoms that may be present with inflammatory conditions include: �Rash �Fatigue �Thickening of the skin on the hands �Difficulty swallowing �Difficulty breathing

Diagnosis of Myositis �Blood tests �Magnetic resonance imaging (MRI scan) �Electromyography (EMG) �Muscle biopsy
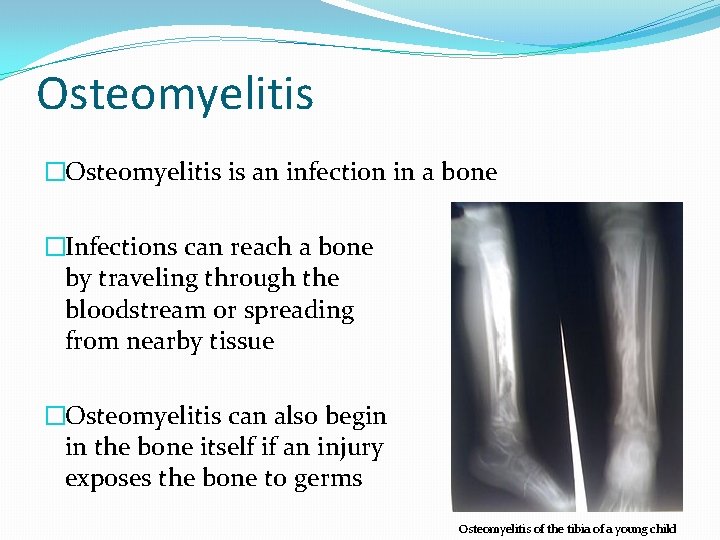
Osteomyelitis �Osteomyelitis is an infection in a bone �Infections can reach a bone by traveling through the bloodstream or spreading from nearby tissue �Osteomyelitis can also begin in the bone itself if an injury exposes the bone to germs Osteomyelitis of the tibia of a young child
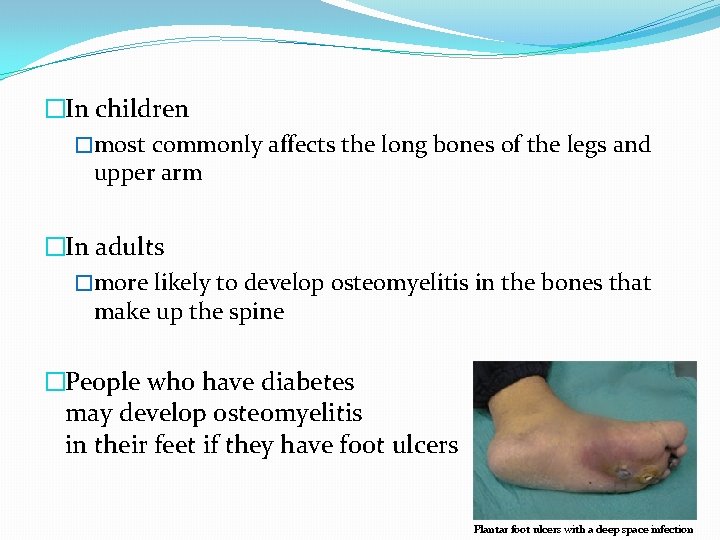
�In children �most commonly affects the long bones of the legs and upper arm �In adults �more likely to develop osteomyelitis in the bones that make up the spine �People who have diabetes may develop osteomyelitis in their feet if they have foot ulcers Plantar foot ulcers with a deep space infection

�Once considered an incurable condition, osteomyelitis can be successfully treated today �Most people require surgery to remove parts of the bone that have died �followed by strong antibiotics �often delivered intravenously �typically for at least six weeks

Symptoms �Signs and symptoms of osteomyelitis include: �Fever or chills �Irritability or lethargy in young children �Pain in the area of the infection �Swelling, warmth and redness over the area of the infection

Causes �Most cases of osteomyelitis are caused by staphylococcus bacteria �Germs can enter a bone in a variety of ways, including: �Via the bloodstream �From a nearby infection �Direct contamination

�Via the bloodstream �Germs in other parts of the body can travel through bloodstream to a weakened spot in a bone �From a nearby infection �Severe puncture wounds can carry germs deep inside the body �If such an injury becomes infected, the germs can spread into a nearby bone

�Direct contamination �This may occur if a bone have broken so severely that part of it is sticking out through skin �Direct contamination can also occur during surgeries to replace joints or repair fractures

Disease causative agent Age group Most common organisms Newborns (younger than 4 mo) S. aureus, Enterobacter species, and group A and B Streptococcus species Children (aged 4 mo to 4 y) S. aureus, group A Streptococcus species, Haemophilus influenzae, and Enterobacter species Children, adolescents (aged 4 y to adult) S. aureus (80%), group A Streptococcus species, H. influenzae, and Enterobacter species Adult S. aureus and occasionally Enterobacter or Streptococcus species Sickle cell anemia patients Salmonella species are more common in patients with sickle cell disease than in normal patients. However, S. aureus is still most likely to occur.

Acute Osteomyelitis �Vertebral osteomyelitis can occur in adults secondary to a UTI or prostatitis �Candidemia from infected central venous catheters can lead to fungal osteomyelitis �Contiguous infection �Bacteria related to primary focus, it includes � Gram positive cocci, Gram negative bacilli, Anaerobes, and Poly-microbial infection
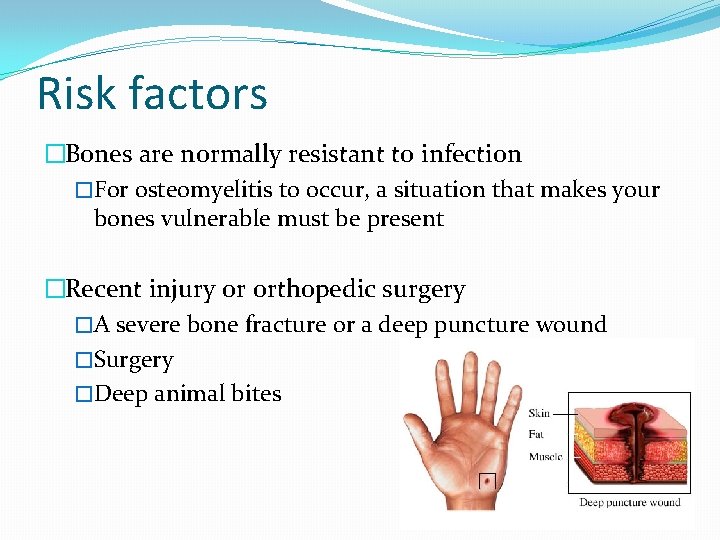
Risk factors �Bones are normally resistant to infection �For osteomyelitis to occur, a situation that makes your bones vulnerable must be present �Recent injury or orthopedic surgery �A severe bone fracture or a deep puncture wound �Surgery �Deep animal bites
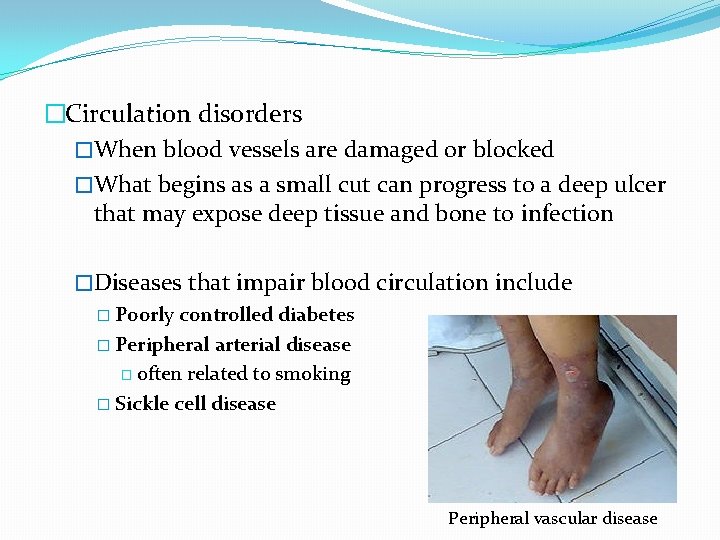
�Circulation disorders �When blood vessels are damaged or blocked �What begins as a small cut can progress to a deep ulcer that may expose deep tissue and bone to infection �Diseases that impair blood circulation include � Poorly controlled diabetes � Peripheral arterial disease � often related to smoking � Sickle cell disease Peripheral vascular disease

�Problems requiring intravenous lines or catheters �Examples of when this type of tubing might be used include � Dialysis machines � Urinary catheters � Long-term intravenous tubing

�Conditions that impair the immune system �Factors that may suppress your immune system include � Chemotherapy � Poorly controlled diabetes � Having had an organ transplant � Needing to take corticosteroids � For unclear reasons � people with HIV/AIDS don't seem to have an increased risk of osteomyelitis �Illicit drugs �nonsterile needles �unsterilized skin before injections
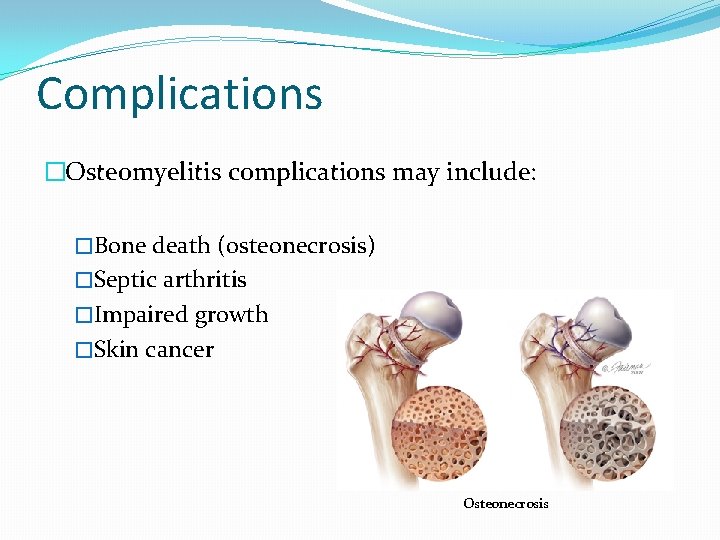
Complications �Osteomyelitis complications may include: �Bone death (osteonecrosis) �Septic arthritis �Impaired growth �Skin cancer Osteonecrosis

Tests and diagnosis �Blood tests �Imaging tests �X-rays �Computerized tomography (CT) scan �Magnetic resonance imaging (MRI) �Bone biopsy

Treatments and drugs �The most common treatments for osteomyelitis are antibiotics and surgery to remove portions of bone that are infected or dead �Hospitalization is usually necessary
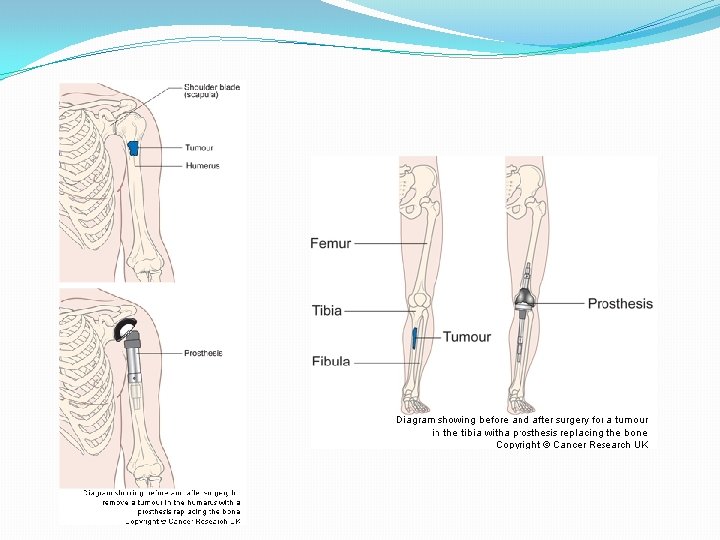

�Medications �A bone biopsy will reveal what type of germ is causing the infection �The antibiotics are usually administered through a vein for at least four to six weeks �Side effects may include nausea, vomiting and diarrhea �An additional course of oral antibiotics may also be needed for more-serious infections

�Surgery �Depending on the severity of the infection, osteomyelitis surgery may include one or more of the following procedures � Drain the infected area � Remove diseased bone and tissue � Remove any foreign objects � Amputate the limb

Arthritis �Infectious Arthritis is inflammation of the joint space �Generally affects a single joint and result in suppurative inflammation �Hematogenous seeding of joint is most common �Pain, swelling, limitation of movement common symptoms

Etiology, Epidemiology & Risk factors �Gonococcal infection most common cause in young adults caused by Neisseria gonorrheae �Nongonococcal arthritis occurs in older adults

�Occasionally results from direct trauma, procedures (arthroscopy) or from contiguous soft tissue infection �S. aureus is most common cause �Other organisms : streptococci and aerobic Gram negative bacilli �Lyme disease in endemic areas �Risk factors: age, diabetes, immunosuppression, IV drug use, catheters, prior joint damage, sexually transmitted diseases

Diagnosis of Infectious Arthritis �History/examination to exclude systemic illness �Blood cultures �culture or DNA testing for N. gonorrheae �Urine may be used for DNA testing also �Culture of joint fluid, and skin lesions also indicated

Treatment & Management �Arthrocentesis with drainage of infected synovial fluid �Repeated therapeutic arthrocentesis often needed �Occassionally, arthroscopic or surgical drainage/debridement �Antimicrobial therapy should be directed at suspected and susceptibility results �Gonococcal arthritis: IV Ceftriaxone ( or Ciprofloxacin or Ofloxacin) then switch to oral Quinolone or Cefixime for 7 -10 days

�Nongonococcal infectiuos arthritis �MSSA: Nafcillin or Cefazolin. �MRSA: Vancomycin �Streptococci: Penicillin or Ceftriaxone or Cefazolin �Enterobacetriacae: Ceftriaxone or Fluroquinolone �Pesudomonas: Piperacillin and Aminoglycoside �Animal bite : Ampicillin-Sulbactam �Lyme disease arthritis: Doxycycline for 1 month

Prognosis & Complications �Gonococcal arthritis has an excellent outcome �Nongonococcal arthritis �can result in scarring with limitation of movement, ambulation is affected in 50% of cases �Risk factors for long–term adverse sequellae include �Age, prior rheumatoid arthritis, poly-articular joint involvement, hip or shoulder involvement, virulent pathogens and delayed initiation or response to therapy
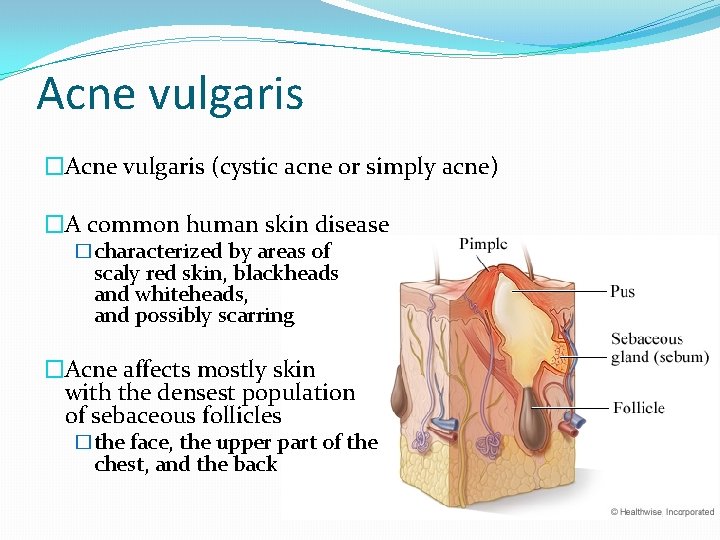
Acne vulgaris �Acne vulgaris (cystic acne or simply acne) �A common human skin disease �characterized by areas of scaly red skin, blackheads and whiteheads, and possibly scarring �Acne affects mostly skin with the densest population of sebaceous follicles �the face, the upper part of the chest, and the back
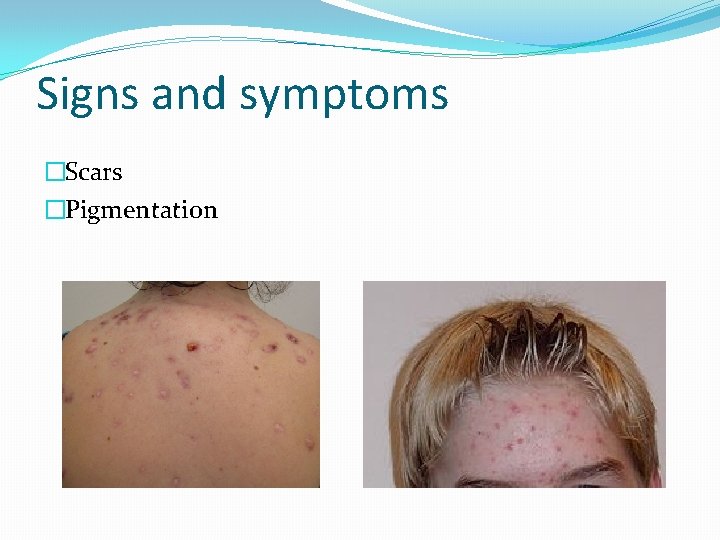
Signs and symptoms �Scars �Pigmentation
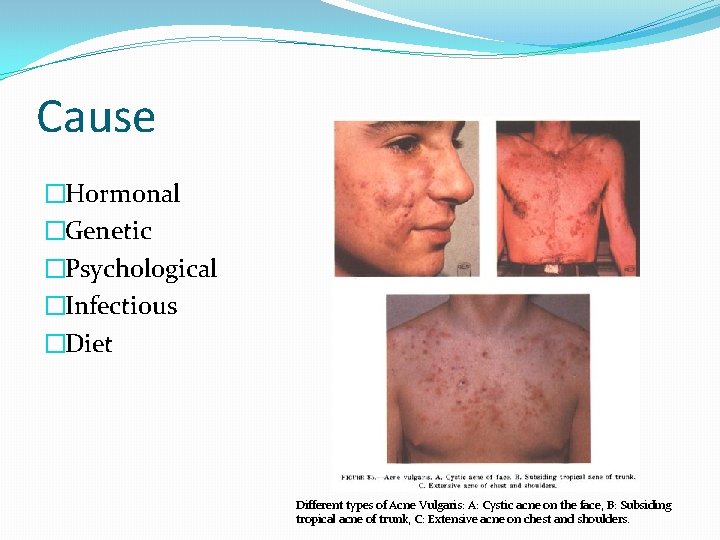
Cause �Hormonal �Genetic �Psychological �Infectious �Diet Different types of Acne Vulgaris: A: Cystic acne on the face, B: Subsiding tropical acne of trunk, C: Extensive acne on chest and shoulders.

Infectious Agent �Propionibacterium acnes (P. acnes) is the anaerobic bacterium species that is widely concluded to cause acne �Staphylococcus epidermidis has been universally discovered to play some role in acne formation

Medications �Benzoyl peroxide �Antiseptics �Antibiotics �Hormones �Topical retinoids �Oral retinoids �Anti-inflammatories Benzoyl peroxide cream
- Slides: 40