Microbiology Chapter 16 Adaptive Immunity 2018 Pearson Education

Microbiology Chapter 16 Adaptive Immunity © 2018 Pearson Education, Inc.
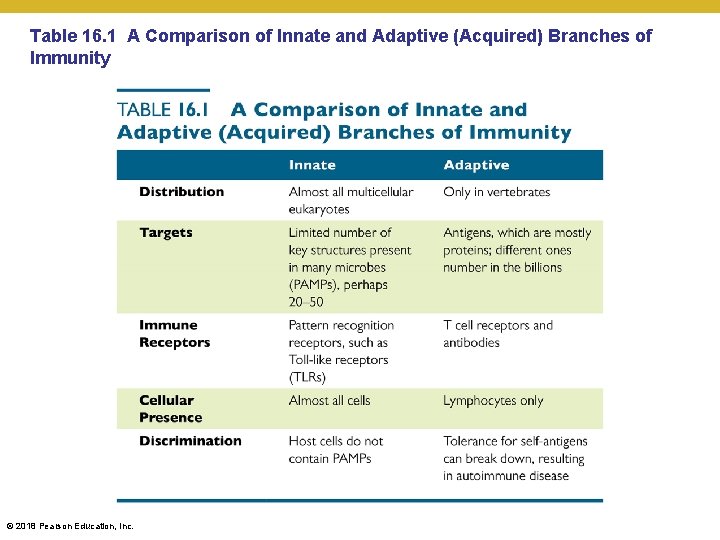
Table 16. 1 A Comparison of Innate and Adaptive (Acquired) Branches of Immunity © 2018 Pearson Education, Inc.

Overview of Adaptive Immunity • Adaptive immunity is the body’s ability to recognize and defend itself against distinct invaders and their products • Recognize specific sequences, not chemical patterns • Only found in vertebrates • Five attributes of adaptive immunity • Specificity – each cell recognizes only a unique biochemical structure • Inducibility – needs some time to get fully activated • Clonality – cells that recognize non-self are amplified • Unresponsiveness to self (or dampened response) • Memory – cells that recognize non-self are stored, and back-up’s made © 2018 Pearson Education, Inc.

Overview of Adaptive Immunity • Involves activity of lymphocytes • Two main types of lymphocytes • B lymphocytes (B cells) • Mature in the bone marrow • antigen-specific phagocytes • T lymphocytes (T cells) • Mature in the thymus • Control pathogen clearance (manage or directly kill cells) • Two types of adaptive immune responses • Cell-mediated immune responses • Targets localized and exactly defined; “surgical” cleansing • humoral immune responses • Targets diffuse or moving; “roaming” cleaning © 2018 Pearson Education, Inc.
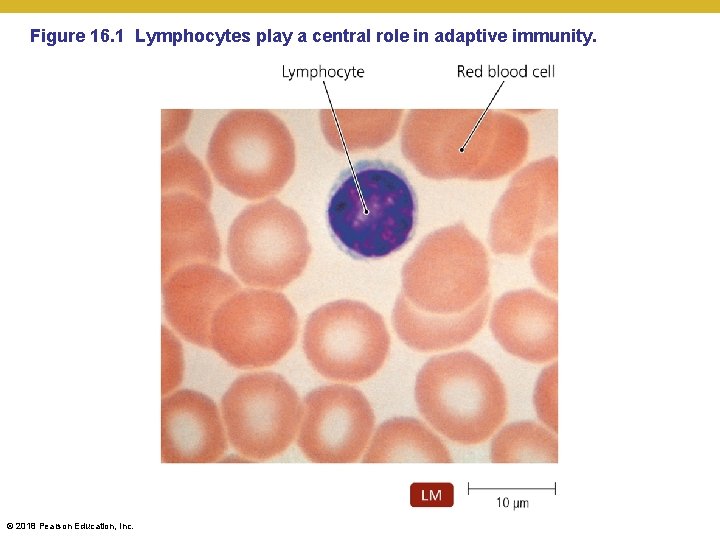
Figure 16. 1 Lymphocytes play a central role in adaptive immunity. © 2018 Pearson Education, Inc.

Figure 16. 1 T Cells in motion https: //www. youtube. com/watch? v=ntk 8 Xsx. VDi 0 https: //www. youtube. com/watch? v=Ue. W-l. Dmnl 9 M Note the amoeboid motion of the T cells Note how the T cells “suction” onto a target cells Note how “excited” they get when they attach © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • The Tissues and Organs of the Lymphatic System • Composed of lymphatic vessels and lymphatic cells, tissues, and organs (lymph nodes) • Screen the tissues of the body foreign antigens • First find antigens in fluid drained from tissues • Then find pathogens responsible for generating antigens © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • The Tissues and Organs of the Lymphatic System • The lymphatic vessels and the flow of lymph • Lymphatic vessels • One-way system that conducts lymph from tissues and returns it to the circulatory system • Runs somewhat parallel to veins • Returns interstitial fluid (vs. blood) to the heart • Lymph • Liquid with similar composition to blood plasma • Arises from fluid leaked from blood vessels into surrounding tissues • Contains salts and lipoproteins, as well as waste, debris, and any pathogens and their debris from infections © 2018 Pearson Education, Inc.
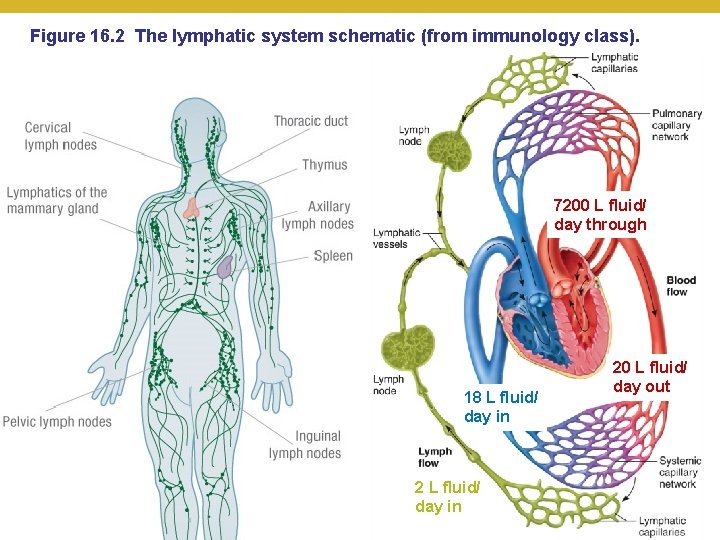
Figure 16. 2 The lymphatic system schematic (from immunology class). 7200 L fluid/ day through 18 L fluid/ day in 2 L fluid/ day in © 2018 Pearson Education, Inc. 20 L fluid/ day out
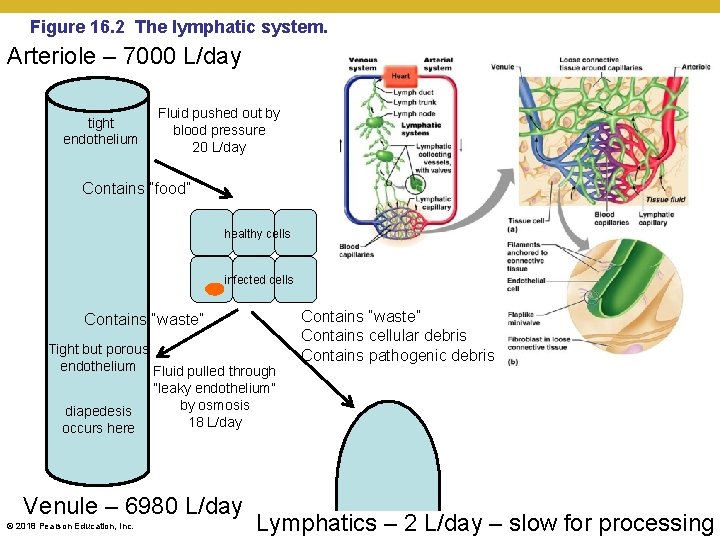
Figure 16. 2 The lymphatic system. Arteriole – 7000 L/day tight endothelium Fluid pushed out by blood pressure 20 L/day Contains “food” healthy cells infected cells Contains “waste” Tight but porous endothelium Fluid pulled through “leaky endothelium” by osmosis diapedesis 18 L/day occurs here Venule – 6980 L/day © 2018 Pearson Education, Inc. Contains “waste” Contains cellular debris Contains pathogenic debris Lymphatics – 2 L/day – slow for processing

Elements of Adaptive Immunity • The Tissues and Organs of the Lymphatic System • Lymphoid organs • Primary lymphoid organs – generate leukocytes • Red bone marrow – ALL cells, including early T cells • Thymus – T cell maturation and education • Secondary lymphoid organs • Initiating filters • Spleen – filters blood for pathogens • Tonsils – sense mouth, ear, eyes, nose fluid • Mucosa-associated lymphoid tissue (MALT) – sense gut, bronchioles, • Downstream filters • Lymph nodes – filter fluid from tissues and upstream lymphoid organs © 2018 Pearson Education, Inc.
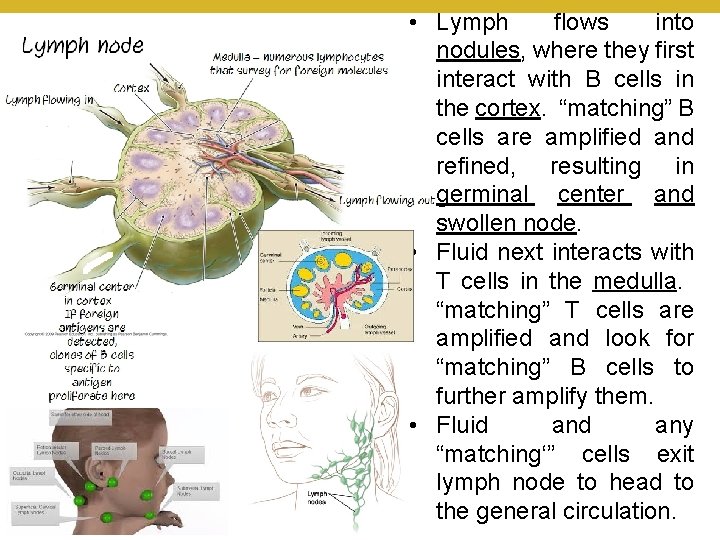
© 2018 Pearson Education, Inc. • Lymph flows into nodules, where they first interact with B cells in the cortex. “matching” B cells are amplified and refined, resulting in germinal center and swollen node. • Fluid next interacts with T cells in the medulla. “matching” T cells are amplified and look for “matching” B cells to further amplify them. • Fluid any “matching‘” cells exit lymph node to head to the general circulation.

Elements of Adaptive Immunity • Antigens • Properties of antigens • Molecules that antibodies can bind • Most are foreign and worthy of attack • Antibodies directly recognize threedimensional subsections of antigens called epitopes • Large foreign macromolecules make the best antigens, especially if they have repeating units of epitopes • Include various bacterial components (LPS) as well as proteins of viruses (capsomeres), fungi, and protozoa • Food and dust can also contain antigenic particles • Can be cell-associated or loose (toxins) • Can initiate allergic reactions (allergens) © 2018 Pearson Education, Inc.
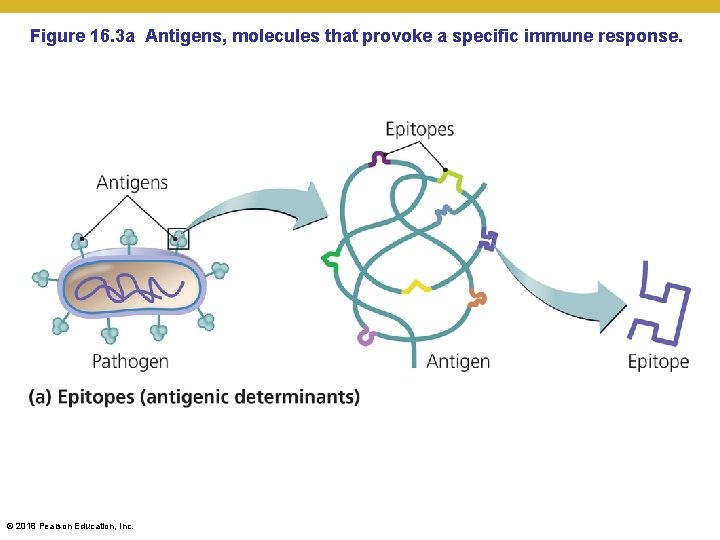
Figure 16. 3 a Antigens, molecules that provoke a specific immune response. © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • Antigens • Types of antigens • Exogenous antigens—include toxins and other components of microbial cell walls, membranes, flagella, and pili (cells have to ingest them to detect them) • Endogenous antigens—produced by microbes that reproduce inside a body's cells (viral proteins) • Autoantigens—derived from normal cellular processes • Autoreactive T cells not eliminated in thymus • Antigen could not be expressed during T cell education © 2018 Pearson Education, Inc.
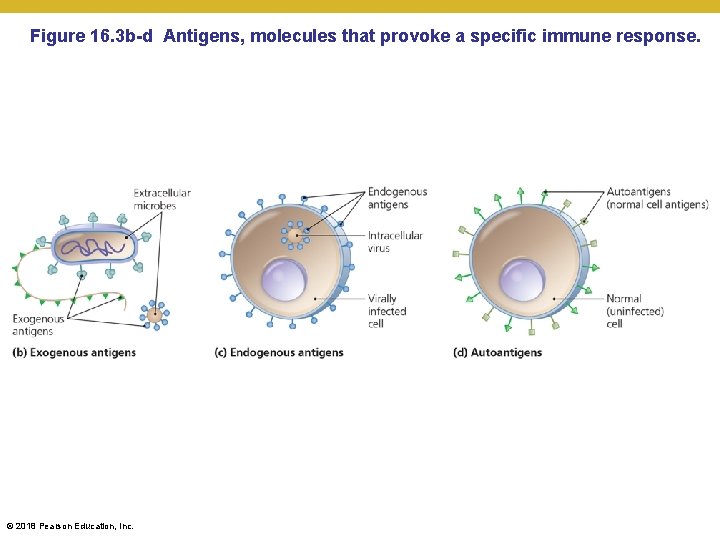
Figure 16. 3 b-d Antigens, molecules that provoke a specific immune response. © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • Preparation for an Adaptive Immune Response • Roles of the major histocompatibility complex (MHC) and antigen-presenting cells • Group of antigens first identified in graft patients • Important in determining compatibility of tissues for tissue grafting because • They are found on nearly all cells in the body • Their composition varies considerably from person to person in the population • Major histocompatibility antigens are glycoproteins found in the membranes of most cells of all vertebrate animals • Hold and position antigenic epitopes for presentation to various types of T cells © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • Preparation for an Adaptive Immune Response • Roles of the major histocompatibility complex (MHC) and antigen-presenting cells • Antigens bind in the groove of MHC molecules • Used to advertise epitopes to T cells • Two classes of MHC proteins • MHC class I • Found on all cells except red blood cells • Generally advertise endogenous antigens • Used to mediate effector-based immunity • MHC class II • found on antigen-presenting cells (APCs) macrophages, dendritic cells, and B cells • Generally advertise exogenous antigens • Used to initiate or boost immune responses © 2018 Pearson Education, Inc.
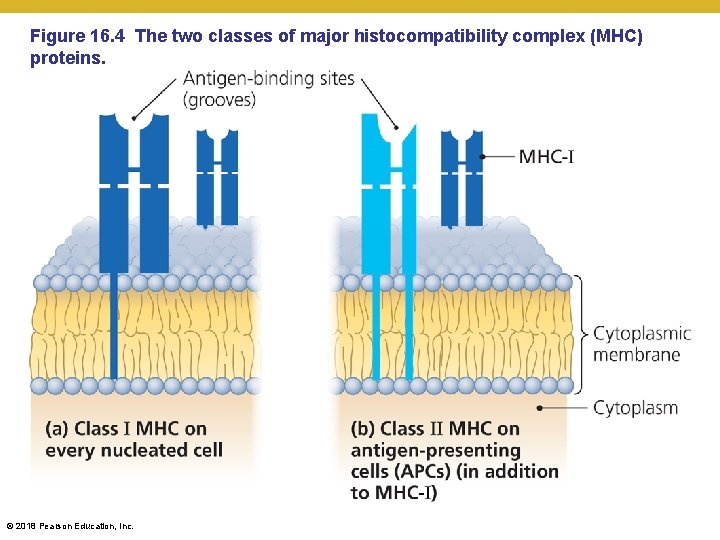
Figure 16. 4 The two classes of major histocompatibility complex (MHC) proteins. © 2018 Pearson Education, Inc.
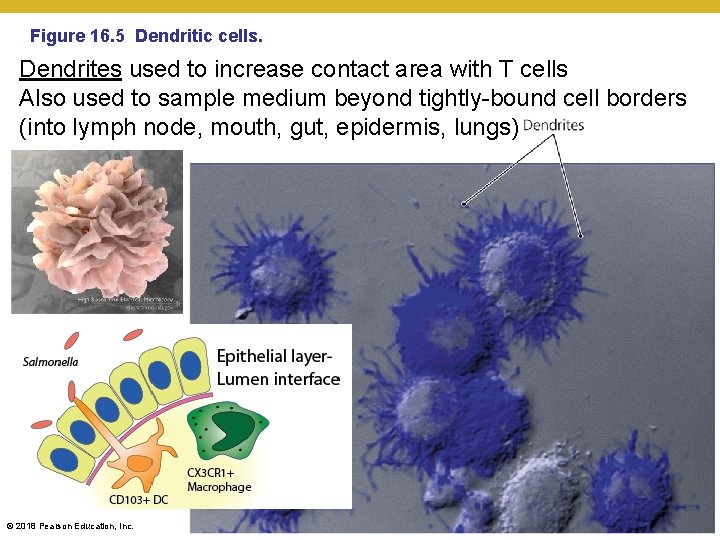
Figure 16. 5 Dendritic cells. Dendrites used to increase contact area with T cells Also used to sample medium beyond tightly-bound cell borders (into lymph node, mouth, gut, epidermis, lungs) © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • Preparation for an Adaptive Immune Response • Antigen processing • Antigens must be processed for MHC proteins to display epitopes – they can only hold sequences of 8 -20 amino acids • Different processes for endogenous and exogenous antigens • Exogenous antigens- obtained through phagocytosis; broken down in phagolysosomes • Endogenous antigens – obtained through proteasomes (general protein turnover); obtained by proteolysis and sent into lumen for loading © 2018 Pearson Education, Inc.
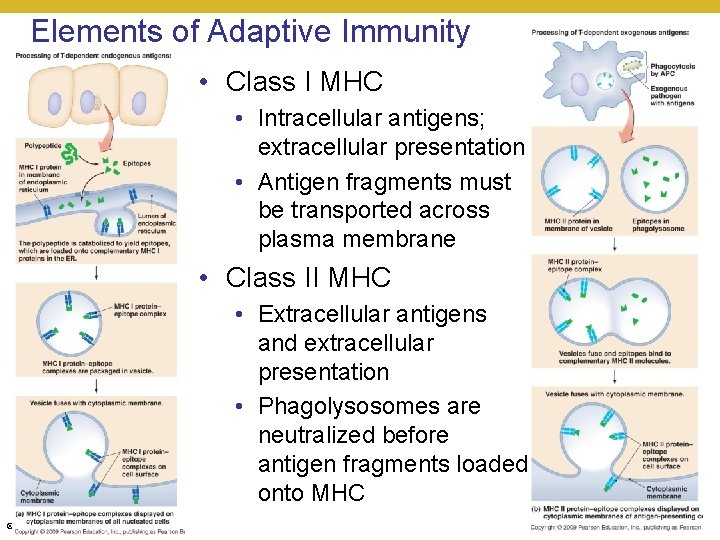
Elements of Adaptive Immunity • Class I MHC • Intracellular antigens; extracellular presentation • Antigen fragments must be transported across plasma membrane • Class II MHC • Extracellular antigens and extracellular presentation • Phagolysosomes are neutralized before antigen fragments loaded onto MHC © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • T Lymphocytes (T Cells) • Produced in the red bone marrow and mature in the thymus • Circulate in the lymph and blood • Migrate to the lymph nodes, spleen, tonsils, MALT, and Peyer’s patches • Have T cell receptors (TCRs) on their cytoplasmic membrane • T cells outside of thymus are specific to specific biochemical signatures © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • T Lymphocytes (T Cells) • Antigen specificity through its T cell receptor (TCR) • TCRs do not recognize epitopes directly (in isolation) • cf. BCR’s recognize antigens directly through their epitopes • TCRs only bind epitopes displayed with an MHC protein, both residing on an antigen-presenting cell • MHC Class I – found on all of our nucleated cells, will present endogenous antigens • MHC Class II – found on antigen presenting cells (B cells, macrophages, dendritic cells), will present exogenous antigens • CD 1 – advertises lipid-based endogenous antigens • Some T cells act against body cells that produce abnormal cell-surface proteins – this is how our body uses T cells to fight cancer © 2018 Pearson Education, Inc.
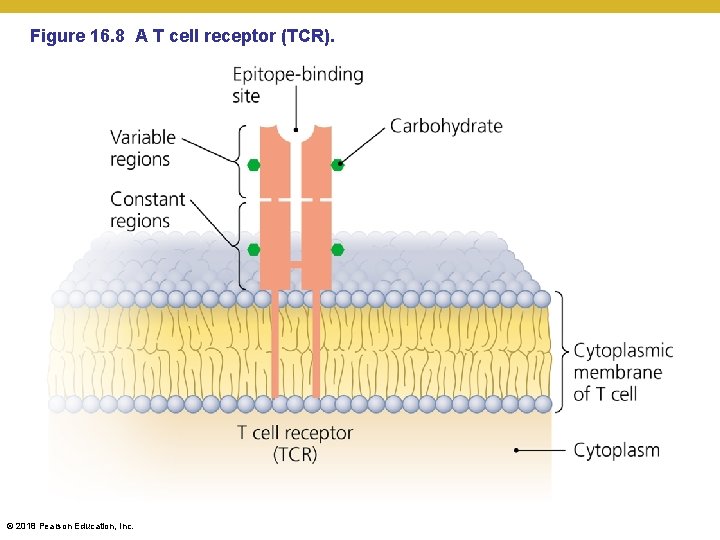
Figure 16. 8 A T cell receptor (TCR). © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • T Lymphocytes (T Cells) • Types of T lymphocytes • Four types based on surface glycoproteins and characteristic functions • Cytotoxic T lymphocyte • Directly kills other cells • Helper T lymphocyte • Helps direct effector immune response • Regulatory T lymphocyte • Represses adaptive immune responses • Follicular T lymphocyte • Activates B cells at germinal centers © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • T Lymphocytes (T Cells) • Clonal deletion of T cells • Vital that immune responses not be directed against autoantigens • Body eliminates self-reactive lymphocytes • Thymus – deletion during education prior to first contact • Tissues – deletion through excessive antigen contact in absence of infection signals • Tissue-specific antigen, neoantigen, chronic viral infection • Lymphocytes that react to autoantigens are silenced • Either become regulators (shut down others), undergo anergy (put on ice), undergo apoptosis (put to death) © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • T Lymphocytes (T Cells) • Clonal deletion of T cells • TCRs are generated semi-randomly to make sure an “infinite” combination of antigens are predicted • TCR’s are tested for activity by a library of MHC +self epitopes (the body does not store pathogens simply to train T cells) • Immature T cells undergo one of four reactions during their education: • They never recognize any MHC + antigen combinations, at all • They strongly recognize several MHC + antigen combination too frequently • They recognize only one or a few antigen combinations • They only weakly recognize MHC + antigen combinations © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • • • T cells that do not recognize body’s MHC protein undergo apoptosis (cell suicide) – they’ll never work reliably in the field T cells that recognize autoantigen +MHC too strongly die by apoptosis – far too frequently activated to be left alive Some “self-recognizing” T cells become regulatory T cells – they can shut down improperly activated T cells in tissues later (differentiated tissues, transient protein expression, pregnancy, resident microbes) Those weakly recognizing MHC and some sort of epitope are set loose to find foreign epotope+MHC T cells that recognize MHC protein and foreign epitopes (and fir the first time react strongly, especially when danger signal are also present) become repertoire of protective T cells © 2018 Pearson Education, Inc.
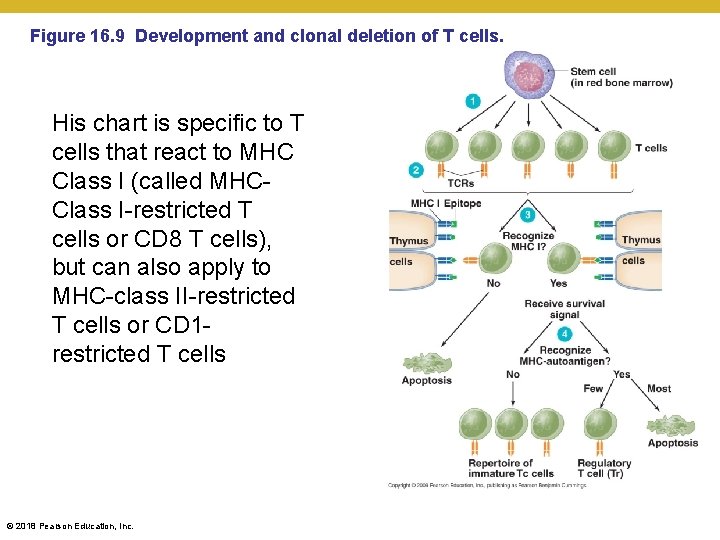
Figure 16. 9 Development and clonal deletion of T cells. His chart is specific to T cells that react to MHC Class I (called MHCClass I-restricted T cells or CD 8 T cells), but can also apply to MHC-class II-restricted T cells or CD 1 restricted T cells © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • B Lymphocytes (B Cells) and Antibodies • Found primarily in the spleen, lymph nodes, tonsils, and MALT • Small percentage of B cells circulate in the blood • Major functions are • Antigen-specific detection and presentation to T cells • Secretion of antibodies matching their antigen receptors © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • B Lymphocytes (B Cells) and Antibodies • Specificity of the B cell receptor (BCR) • Each B lymphocyte has multiple versions of each variable part of the BCR • Each mature B cell generates only a single BCR, formed by a single version of each of the above pieces • Each BCR recognizes only one epitope • Two variable regions of the BCR form the antigen-binding sites • The entire repertoire of an individual's BCRs is capable of recognizing millions to billions of different epitopes © 2018 Pearson Education, Inc.
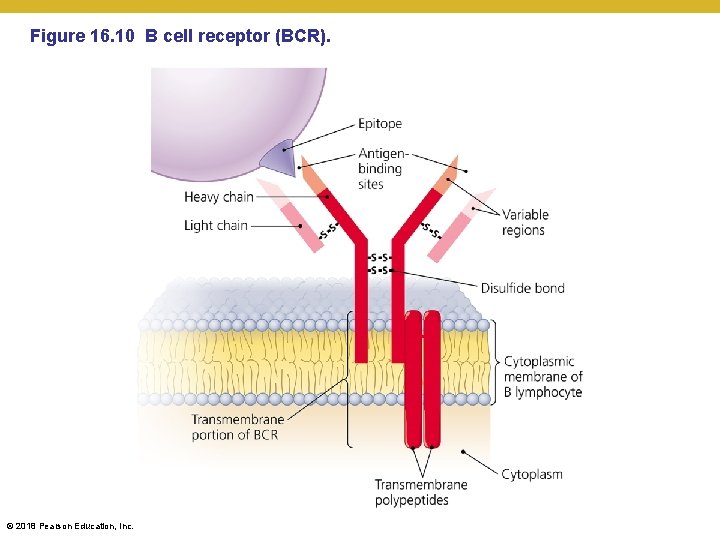
Figure 16. 10 B cell receptor (BCR). © 2018 Pearson Education, Inc.
Figure 16. 11 A plasma cell. © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • B Lymphocytes (B Cells) and Antibodies • Specificity and antibody structure • Specificity mediated through a proteins called immunoglobulin • Have antigen-binding sites (determined antibody specificity) and immune-system-interacting site (determines antibody function) • B cells express a cell surface-bound form and a secretable form • Membrane-bound form comprises the B cell receptor (BCR) and allows cell to be activated by and process only specific antigens • Antibodies recognize the same antigens, and are released by the cells whose BCR was activated by the same antigen • B cells that produce large amounts of antibodies are called plasma cells © 2018 Pearson Education, Inc.
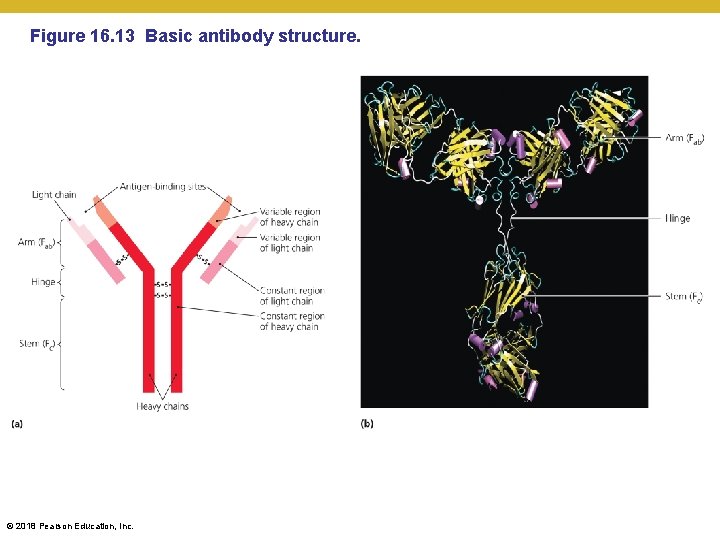
Figure 16. 13 Basic antibody structure. © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • B Lymphocytes (B Cells) and Antibodies • Antibody function • Antigen-binding sites are complementary to epitopes • Antibodies function in several ways – “kisses of death” • Activation of complement and inflammation – through classical complement pathway • Neutralization – block up active sites of pathogenic enzymes or prevent critical contacts from happening • Opsonization – antibody-coated pathogens are “very tasty” to the immune system • Agglutination – form a massive protein web that precipitates and stops moving • Antibody-dependent cellular cytotoxicity (ADCC) – antibodies bound to compromised cell are a call for “assisted suicide” by cytotoxic immune cells © 2018 Pearson Education, Inc.
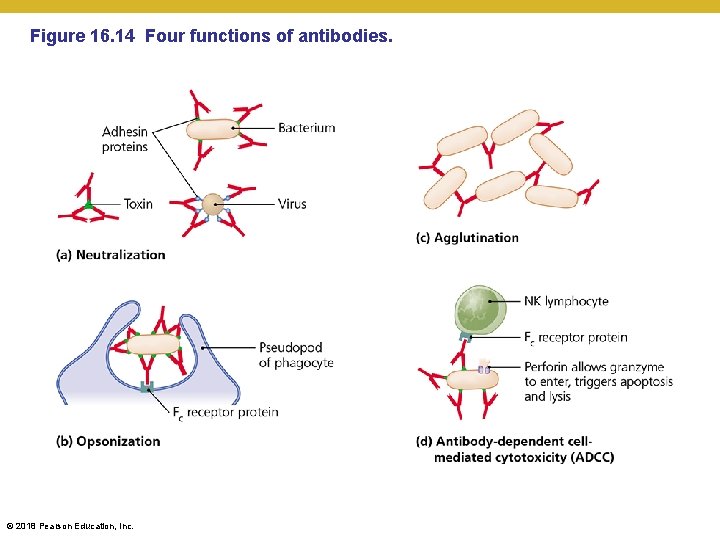
Figure 16. 14 Four functions of antibodies. © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • B Lymphocytes (B Cells) and Antibodies • Classes of antibodies • Threats confronting the immune system are variable • Antibody class involved in the immune response varies • Type of antigen (allergan vs. antigen) • Portal of entry (mucosal vs. parenteral) • Antibody function needed (complement vs. no complement) • Five different classes of antibodies – Ig. M, Ig. A, Ig. D, Ig. E, Ig. G © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • B Lymphocytes and Antibody Classes • “first guess” • All naïve and invariant B cells produce this antibody • Ig. M—first antibody produced; includes natural antibodies; strongly activate complement; allow even weak pathogen contacts to trigger strong response • Ig. D—exact function is not known (membrane-bound form) • “better guess” • Pathogen-experienced B cells produce these antibodies • Ig. A—associated with ALL body secretions • Ig. G—most common and longest-lasting antibody; transmits through mother’s milk • Ig. E—involved in response to parasitic infections and allergies; granulocyte activators © 2018 Pearson Education, Inc.
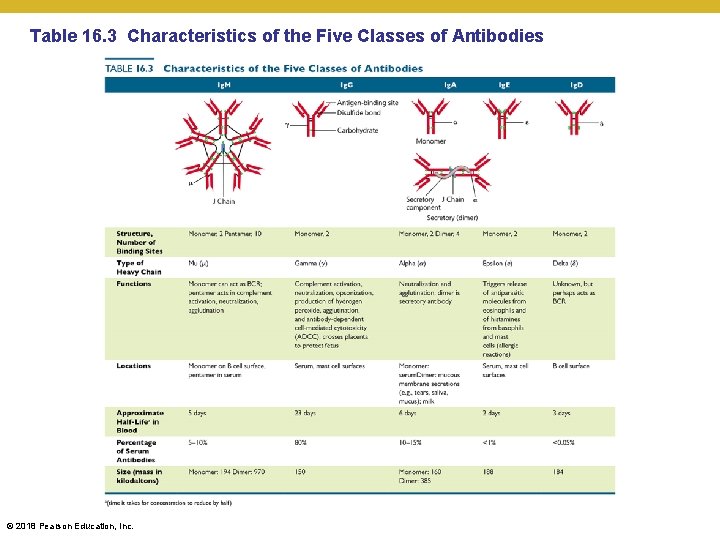
Table 16. 3 Characteristics of the Five Classes of Antibodies © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • B Lymphocytes (B Cells) and Antibodies • Clonal deletion of B cells • Occurs in the bone marrow in a manner similar to deletion of T cells • Self-reactive B cells may become inactive or change their BCR rather than undergo apoptosis • Regulatory B cells can emerge from this process and help stop immune responses in tissues © 2018 Pearson Education, Inc.
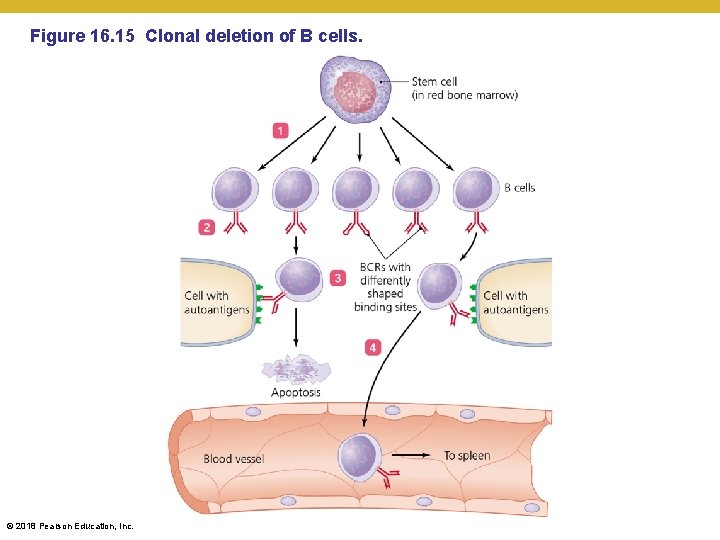
Figure 16. 15 Clonal deletion of B cells. © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • How we fight infections with adaptive immunity • Cytokines – communication network • Cells, pathogen detection, and tools are only part of the solution • Clearing the infection – which tools to do the job right! • Cell-mediated response • Antigens are found only associated with cells • Easily removed without damaging unaffected tissues • Humoral response • Antigens are found outside of cells and potentially all over the place • “carpet combing” type of response • Clearance will likely destroy innocent bystander tissues © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • Immune Response Cytokines • Soluble regulatory proteins that act as intercellular signals – coordinate immune system function during an infection and clearing of the infection and tissue repair afterward • Cytokines secreted by various leukocytes • Cytokine network • Complex web of signals among cells of the immune system © 2018 Pearson Education, Inc.

Elements of Adaptive Immunity • Immune Response Cytokines • Interleukins (ILs) • (classically) Signal (usually) among leukocytes • Interferons (IFNs) • Antiviral proteins that act as cytokines • Growth factors • Proteins that stimulate stem cells to divide • Involved in immune cell clonal expansion • Invovled in tissue repair after an infection is cleared • Tumor necrosis factor (TNF) • Secreted by macrophages and T cells to kill tumor cells and regulate immune responses and inflammation • Chemokines • Chemotactic cytokines that signal leukocytes to move © 2018 Pearson Education, Inc.
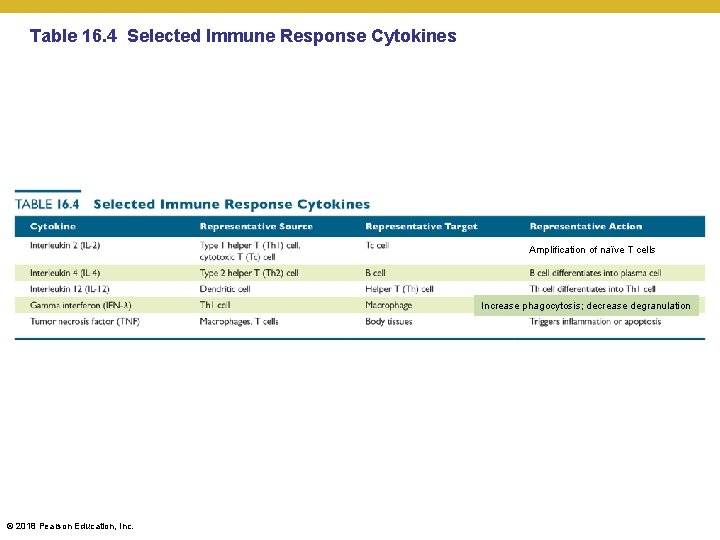
Table 16. 4 Selected Immune Response Cytokines Amplification of naïve T cells Increase phagocytosis; decrease degranulation © 2018 Pearson Education, Inc.

Cell-Mediated Immune Responses • Respond to intracellular pathogens and abnormal body cells • Common intracellular pathogens are viruses • The response is also effective against cancer cells, intracellular protozoa, and intracellular bacteria • All could be characterized as “cells gone bad” and cells expressing strange antigens the T cells did not know about as they were getting educated in the thymus in a young child (2 -10 years old) © 2018 Pearson Education, Inc.
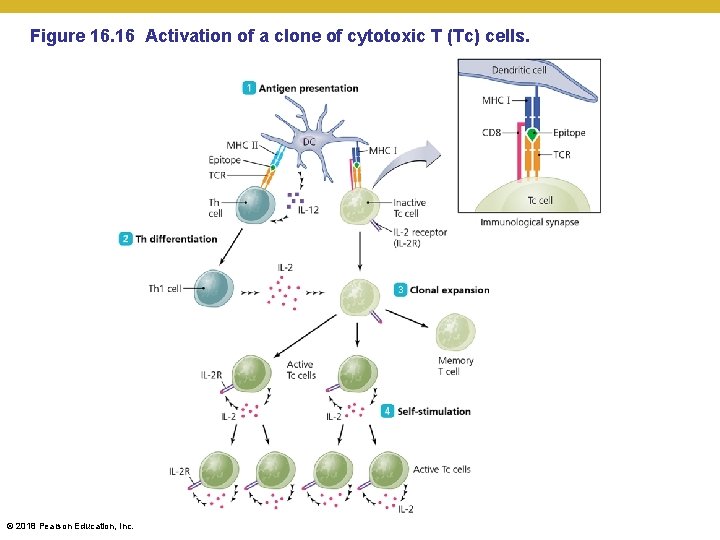
Figure 16. 16 Activation of a clone of cytotoxic T (Tc) cells. © 2018 Pearson Education, Inc.

Let’s go over a couple of scenarios • A B cell is going along and encounters an epitope on a bacterium that its membrane-bound Ig. M antibody is specific for • It phagocytizes the bacteria and processes the antigen • It presents ALL the epitopes (even those it did not initially recognize) from that antigen • A T helper (TH) cell with a TCR that recognizes one of the epitopes of that antigen in the MHC comes by • Interaction of the TCR and MHC causes a release of cytokines by the TH cell • Those cytokines induce a signal transduction pathway in both the T and B cell specific for this bacteria • Results in mitosis of these specific B and T cells • Results in the B cell secreting more of this specific antibody (will put the variable region on an Ig. D, Ig. G, Ig. E, and Ig. A antibody) • Results in the B and T cells with specificity for this bacteria to make memory cells of themselves (will last for decades) • Effector cells in the area (macrophages, granulocytes) are influenced by the cytokine milieu and act appropriately © 2018 Pearson Education, Inc. •

• A cell (non-APC) is infected by a virus • • • The cell is able to take some of the viral particles and put them on the MHC Class I molecules it has on its surface An MHC Class I-restricted (CD 8+) T cell (usually cytotoxic T (Tc) cell) with specificity for that virus comes by and recognizes the antigen and MHC It spreads itself over a large portion of the infected cell’s surface Interaction of the TCR on the Tc cell and MHC molecule results in release of perforin by the T cell Perforin causes holes in the surface of the infected cell, cell is forced to go through apoptosis, especially after granzyme B enters through the pores and starts eating proteins in the infected cell Goal is to kill the self cell before the virus is able to replicate, form new particles, and kill more cells © 2018 Pearson Education, Inc.
![Cell-Mediated Immune Responses [INSERT FIGURE 16. 14] © 2018 Pearson Education, Inc. Cell-Mediated Immune Responses [INSERT FIGURE 16. 14] © 2018 Pearson Education, Inc.](http://slidetodoc.com/presentation_image/ce9def58920f517fa6e70bfa6ca359e6/image-52.jpg)
Cell-Mediated Immune Responses [INSERT FIGURE 16. 14] © 2018 Pearson Education, Inc.
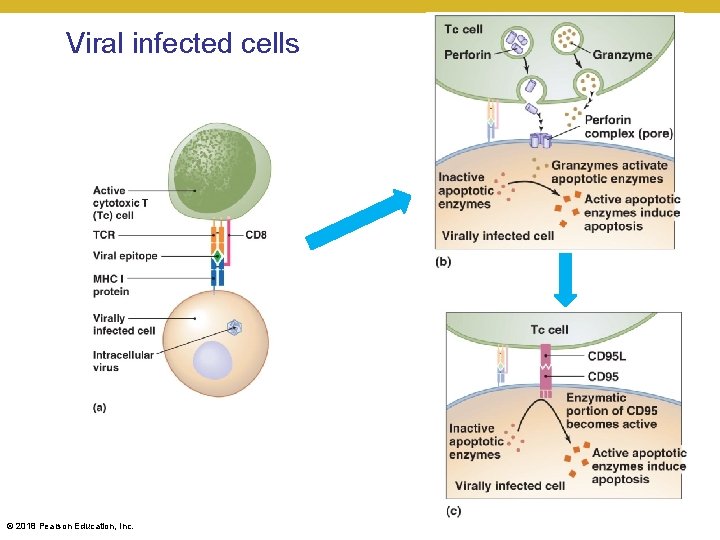
Viral infected cells © 2018 Pearson Education, Inc.

Cell-Mediated Immune Responses • Memory T Cells • Some activated T cells become memory T cells • They are “back-ups” saved among several stages of the T cells expansion, as T cells are being programmed and indoctrinated for specific cytokine environments • Persist for months or years in lymphoid tissues • Immediately functional upon subsequent contacts with epitope-MHC complex specific to its TCR • Memory response is more effective than the primary response (the two-day long stages of Naïve T cell initial activation have already occurred) © 2018 Pearson Education, Inc.

Cell-Mediated Immune Responses • T Cell Regulation • Regulation needed to prevent T cell response to autoantigens • T cells require additional signals from an antigenpresenting cell • Interaction of the T cell and antigen-presenting cell stimulates the T cell to respond to the antigen • Co-stimulatory signals from APC are quality-control • Danger signals indicated that the antigen detection is occurring with an infection; helps reduce misfiring from near-autoantigens presented by some pathogens. • Regulatory T cells also moderate cytotoxic T cell activity © 2018 Pearson Education, Inc.

Antibody Immune Responses • Induction of T-Dependent Antibody Immunity with Clonal Selection • Plasma cells • Majority of cells produced during B cell proliferation • Only secrete antibody molecules complementary to the specific antigen • Short-lived cells that die within a few days of activation • Their antibodies and progeny can persist © 2018 Pearson Education, Inc.
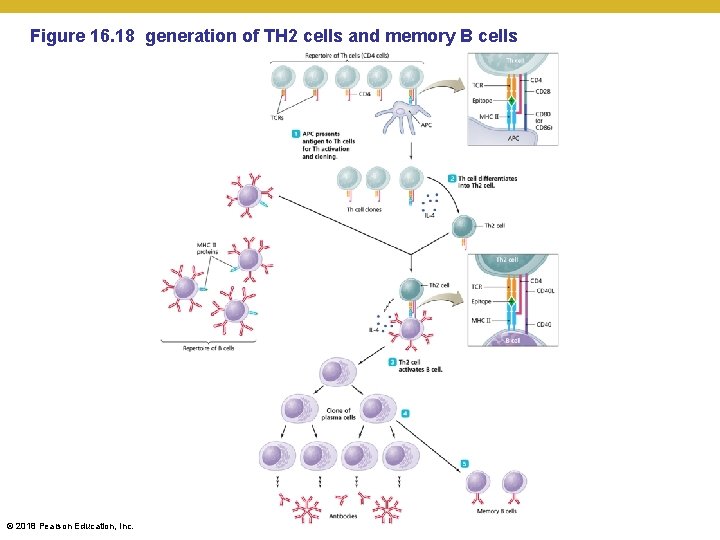
Figure 16. 18 generation of TH 2 cells and memory B cells © 2018 Pearson Education, Inc.

Antibody Immune Responses • Memory Cells and the Establishment of Immunological Memory • • Produced by B cell proliferation These cells do not secrete antibodies They are “backups” Have refined BCRs complementary but stronger-binding to the epitope that triggered their production • Give a stronger response to the antigen or respond to low levels of the antigen • Long-lived cells that persist in the lymphoid tissue • Initiate antibody production if antigen is encountered again – response is grater and faster © 2018 Pearson Education, Inc.

Antibody Immune Responses • Memory Cells and the Establishment of Immunological Memory • Primary immune response • Small amounts of antibodies produced • Tends to be of low affinity, primarily Ig. M • May take days to produce enough antibodies to eliminate the antigen from the body • Secondary immune response • • Memory cells respond to another exposure to the antigen Much faster than the primary response Tends to be high affinity response Tends to be mostly Ig. G © 2018 Pearson Education, Inc.
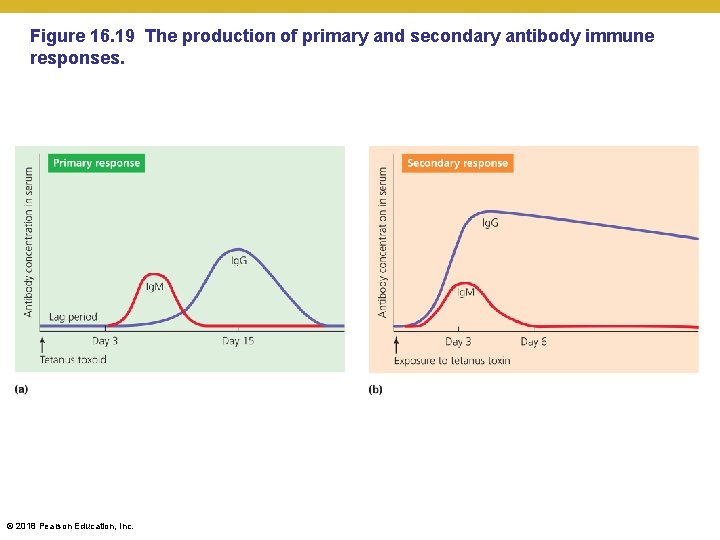
Figure 16. 19 The production of primary and secondary antibody immune responses. © 2018 Pearson Education, Inc.

Types of Acquired Immunity • Specific immunity acquired during an individual’s life • Two types • Naturally acquired • Response against antigens encountered in daily life • Obtained through NATURAL sources, i. e. , natural exposure or from mother’s milk • Artificially acquired • Response to antigens introduced via a vaccine • Distinguished as either active or passive • Active – the body generates its own response • Poassive – the protection comes from the outside © 2018 Pearson Education, Inc.

Table 16. 5 A Comparison of the Types of Acquired Immunity © 2018 Pearson Education, Inc.
- Slides: 62