Microbial Toxins BIOC 422 Bacterial Toxins Endotoxins Dr

Microbial Toxins (BIOC 422) Bacterial Toxins (Endotoxins) Dr. Ayat B. Al-Ghafari Associate Professor of Biomedical Sciences e. mail: abalghafari@kau. edu. sa
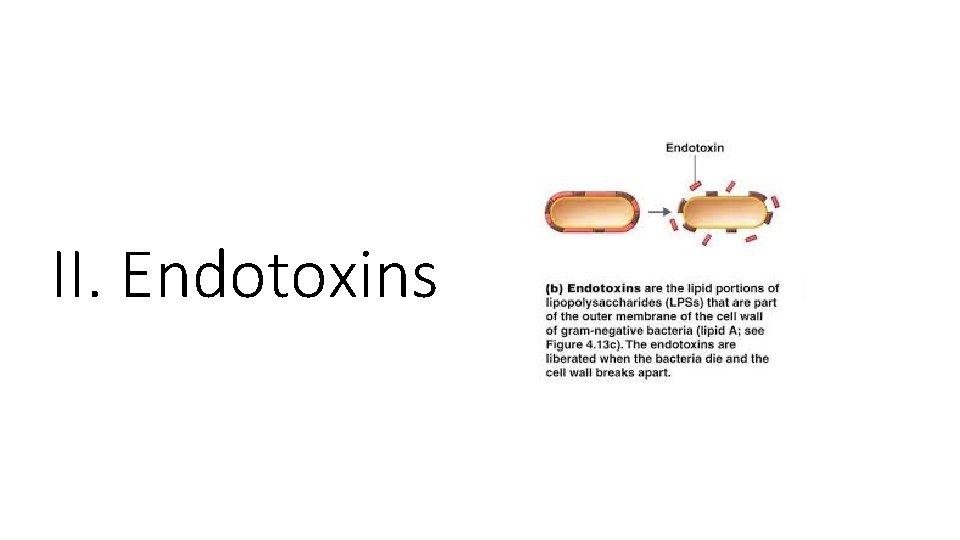
II. Endotoxins

4 - Production of toxins : II. Endotoxins • Endotoxin is a complex lipopolysaccharide (LPS) found in the outer cell membrane of gram-negative bacteria. • The toxic activity of lipopolysaccharides “LPS” was first discovered and termed “Endotoxin" by: “ Richard Friedrich Johannes Pfeiffer”. • He distinguished between exotoxins, which he classified as a toxin that is released by bacteria into the surrounding environment, and endotoxins, which he considered to be a toxin kept "within" the bacterial cell and released only after destruction of the bacterial cell wall. • The term endotoxin is used synonymously with the term lipopolysaccharides (LPS)

4 - Production of toxins : II. Endotoxins Main Characteristics: • Endotoxins are less potent than exotoxins. • They are less specific in their action, since they do not act enzymatically. • Endotoxins are heat stable (boiling for 30 minutes does not destabilize endotoxin), but certain powerful oxidizing agents such as superoxide, peroxide and hypochlorite, have been reported to neutralize them. • They are amphipathic molecules (having both polar and non-polar portions) that carry a net negative charge in solution. Because of their hydrophobicity, they are likely to have strong affinities for other hydrophobic materials like plastic products used in the laboratory. For this reason, carryover contamination from laboratory beakers, stir bars, and other lab ware is common. • Endotoxins, although antigenic (produces an antibody when introduced into the body), cannot be converted to toxoids (a chemically modified toxin, which is no longer toxic but is still antigenic and can be used as a vaccine).

4 - Production of toxins : II. Endotoxins Biological activity: Ø The biological activity of endotoxin is associated with the lipopolysaccharide (LPS). • Toxicity is associated with the lipid component (Lipid A) • Immunogenicity (is the ability to provoke an immune response in the body) associated with the polysaccharide components. Ø Bacteria shed endotoxin in large amounts upon cell death and when they are actively growing and dividing. A single Escherichia coli contains about 2 million LPS molecules per cell.
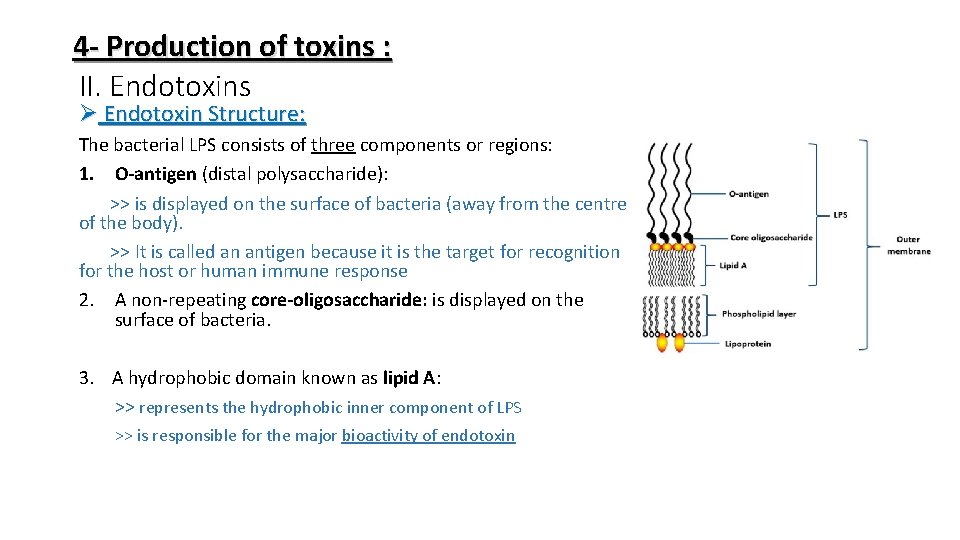
4 - Production of toxins : II. Endotoxins Ø Endotoxin Structure: The bacterial LPS consists of three components or regions: 1. O-antigen (distal polysaccharide): >> is displayed on the surface of bacteria (away from the centre of the body). >> It is called an antigen because it is the target for recognition for the host or human immune response 2. A non-repeating core-oligosaccharide: is displayed on the surface of bacteria. 3. A hydrophobic domain known as lipid A: >> represents the hydrophobic inner component of LPS >> is responsible for the major bioactivity of endotoxin
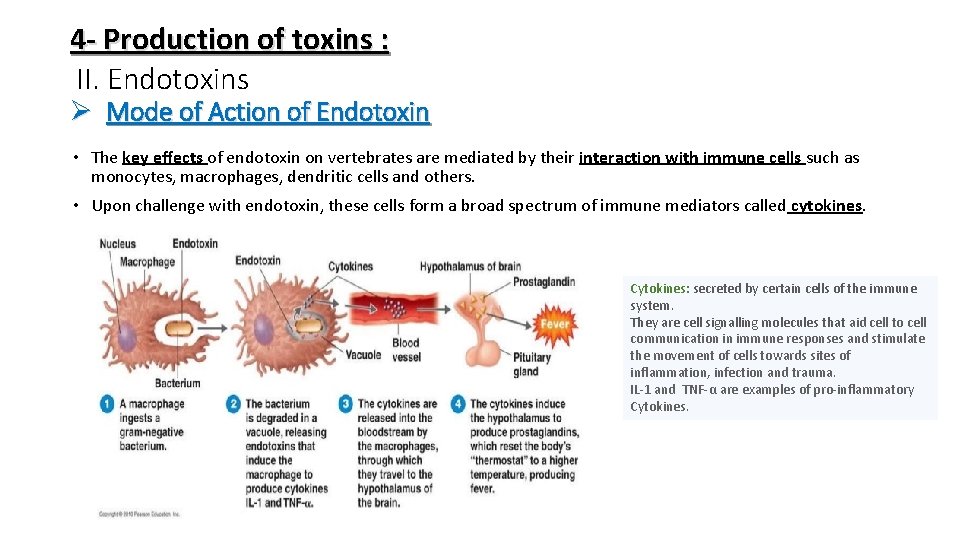
4 - Production of toxins : II. Endotoxins Ø Mode of Action of Endotoxin • The key effects of endotoxin on vertebrates are mediated by their interaction with immune cells such as monocytes, macrophages, dendritic cells and others. • Upon challenge with endotoxin, these cells form a broad spectrum of immune mediators called cytokines. Cytokines: secreted by certain cells of the immune system. They are cell signalling molecules that aid cell to cell communication in immune responses and stimulate the movement of cells towards sites of inflammation, infection and trauma. IL-1 and TNF-α are examples of pro-inflammatory Cytokines.

II. Endotoxins Salmonella • Salmonellosis is an infection caused by Salmonella bacteria. • There are over 2, 500 different types of Salmonella subspecies (spp) >> but most produce a similar clinical picture to other forms of infective gastroenteritis. • Salmonellosis ranges clinically from the common Salmonella gastroenteritis (diarrhoea, abdominal cramps, and fever) to enteric fevers (serious infection marked by intestinal inflammation and ulceration; including typhoid fever) which are life-threatening febrile systemic illness requiring prompt antibiotic therapy. • Salmonella gastroenteritis (Non-typhoidal salmonellosis): is a worldwide disease of humans and animals where animals are the main reservoir >> the disease is usually food borne, although it can be spread from person to person. • Typhoidal salmonellosis: The salmonella that cause Typhoid fever and other enteric fevers. >> Salmonella typhi and Salmonella paratyphi can cause systemic infection (Typhoid fever) >> spread mainly from person-to-person via the faecal-oral route and have no significant animal reservoirs. >> Asymptomatic human carriers (“typhoid Marys”) may spread the disease.

II. Endotoxins 1. Salmonella Gastroenteritis Epidemiology • CDC estimates that approximately 1. 2 million illnesses and approximately 450 deaths occur due to non-typhoidal Salmonella annually in the United State. • The Health Protection Agency (HPA) - part of Public Health England - reported 14, 465 cases of all salmonella in the year 2000, which had dropped by 2015 to 8451. • Worldwide, the World Health Organization (WHO) estimate that tens of millions of human cases occur every year and the disease results in more than hundred thousand deaths

II. Endotoxins 1. Salmonella Gastroenteritis Transmission: • Salmonella live in the intestinal tracts of humans and animals. • You can get Salmonella infection from a variety of sources, including: Ø Eating contaminated food or drinking contaminated water. Ø Touching infected animals and not washing your hands afterwards. • The bacteria can survive for several weeks in water and several years in soil if conditions of temperature, humidity, and p. H are favourable. Infected humans can also serve as reservoirs transmitting salmonellosis from human to human.

II. Endotoxins 1. Salmonella Gastroenteritis Mode of Action: • Pathogenic salmonella ingested in food survive passage through the gastric acid barrier and invade the mucosa of the small and large intestine and produce toxins. • Once they reach the small and large intestines, the ability of Salmonella organisms to multiply and cause infection depends on the infecting dose as well as competition with normal flora. • Invasion of epithelial cells stimulates the release of proinflammatory cytokines; including: IL-1, IL-6, IL-8, TNF-α, which induce an inflammatory reaction. • These evoke an acute inflammatory response and may also be responsible for damage to the intestine. The acute inflammatory response causes fever, chills, abdominal pain and diarrhoea are common. • The bacteria can spread from the intestines to cause systemic disease.

II. Endotoxins 1. Salmonella Gastroenteritis Symptoms of acute gastroenteritis: q Gastroenteritis: inflammation of the stomach and large and small intestines that may result in vomiting or diarrhoea. Symptoms include: • Sudden onset of diarrhoea (which may be bloody) • Abdominal cramps • Fever (almost always present) • Nausea, vomiting, and headache may occur, though less frequent ü Diarrhoea may last for several days and lead to potentially severe dehydration, especially in infants and children under 2 years old and in adults over 65 years old. ü Even after clinical symptoms are no longer obvious, Salmonella bacteria may be found in the stool for several weeks. ü Most people with diarrhoea due to a Salmonella infection recover completely, although it may be several months before their bowel habits are entirely normal.

II. Endotoxins 1. Salmonella Gastroenteritis Symptoms of acute gastroenteritis: q Invasive Salmonella Infections When Salmonella infections become invasive, they can spread to urine, blood, bones, joints, the brain, or the nervous system, causing symptoms related to that body part or system. Some of these extra-intestinal infections can have long-term effects, depending on which part of the body is infected. Ø Invasive Salmonella infections can be severe and potentially life-threatening. Ø Occur in about 8 percent of persons with laboratory-confirmed Salmonella infection. May occur as: Bacteremia (infection of the blood) Meningitis (infection of the membranes lining the brain and spinal cord) Osteomyelitis (infection of the bone) Septic arthritis (infection of a joint). Are rarely fatal, but most commonly occur in people who are very young or old or have a weakened immune system.

II. Endotoxins 1. Salmonella Gastroenteritis q Complications of salmonella: salmonella • Complications of Salmonella poisoning are more likely to occur among young children and people age 65 or older. • Possible complications include: Reactive Arthritis: Reactive arthritis is thought to occur in 2 to 15 percent of Salmonella patients. Symptoms include inflammation of the joints, eyes, or reproductive or urinary organs. On average, symptoms appear 18 days after infection.

II. Endotoxins 1. Salmonella Gastroenteritis Outbreak: • Salmonella outbreaks are commonly associated with eggs, meat and poultry, but these bacteria can also contaminate other foods such as fruits and vegetables. • Foods that are most likely to contain Salmonella include raw or undercooked eggs, raw milk, contaminated water, and raw or undercooked meats.

II. Endotoxins 1. Salmonella Gastroenteritis Diagnosis: • Diagnosing salmonellosis requires testing a clinical specimen (such as stool or blood) from an infected person to distinguish it from other illnesses that can cause diarrhoea, fever, and abdominal cramps.

II. Endotoxins 1. Salmonella Gastroenteritis Treatment: • Salmonella infections often do not require treatment. People with severe dehydration may need rehydration through an IV. • Antibiotics are not routinely recommended since they tend to increase adverse effects as well as prolong Salmonella strains detected in stools. • However, antibiotics are recommended for those at risk of invasive disease, including infants under three months old. • Treatment of Salmonella has become more difficult as it has become more resistant to antibiotics.

II. Endotoxins 1. Salmonella Gastroenteritis Risk Factors • Salmonella infection is more common in the summer months (June, July, and August) than winter. • Children under 5 years old are the most likely to get a Salmonella infection. • Infants who are not breast fed are more likely to get a Salmonella infection. • Adults over 65 years old, and people with weakened immune systems are the most likely to have severe infections. • Certain medications (for example, medications to reduce stomach acid) can increase the risk of Salmonella infection.

II. Endotoxins 1. Salmonella Gastroenteritis Prevention: Quick Tips for Preventing Salmonella • Cook poultry, ground beef, and eggs thoroughly. Do not eat or drink foods containing raw eggs, or raw (unpasteurized) milk. • If you are served undercooked meat, poultry or eggs in a restaurant, don't hesitate to send it back to the kitchen for further cooking. • Wash hands, kitchen work surfaces, and utensils with soap and water immediately after they have been in contact with raw meat or poultry. • Wash hands with soap after handling reptiles, birds, or baby chicks, and after contact with pet faeces. • Be particularly careful with foods prepared for infants, the elderly, and the immunocompromised. • Avoid direct or even indirect contact between reptiles (turtles, iguanas, other lizards, snakes) and infants or immunocompromised persons. • Don't work with raw poultry or meat, and an infant (e. g. , feed, change diaper) at the same time. • Mother's milk is the safest food for young infants. Breast feeding prevents salmonellosis and many other health problems.

II. Endotoxins 2. Salmonella Typhoid Fever • Salmonella infection is usually caused by eating raw or undercooked meat, poultry, eggs or egg products. • Most salmonella infections can be classified as gastroenteritis. • A few varieties of salmonella bacteria result in typhoid fever, a sometimes deadly disease that is more common in developing countries. • The salmonella that cause Typhoid fever and other enteric fevers: >> Salmonella typhi and Salmonella paratyphi can cause systemic infection (Typhoid fever) >> spread mainly from person-to-person via the faecal-oral route and have no significant animal reservoirs. >> Asymptomatic human carriers (“typhoid Marys”) may spread the disease.

II. Endotoxins 2. Salmonella Typhoid Fever Epidemiology: According to WHO (published in 2014), approximately 21 million cases and 222, 000 typhoid-related deaths occur annually worldwide

II. Endotoxins 2. Salmonella Typhoid Fever q. Transmission: Typhoid fever is caused by virulent bacteria called Salmonella typhi (S. typhi) and Salmonella paratyphi (S. paratyphi). >> Although they're related, S. typhi and the bacteria responsible for salmonella gastroentritis, aren't the same. I. Fecal-oral transmission route The bacteria spread through contaminated food or water and occasionally through direct contact with someone who is infected. II. Typhoid carriers Ø Even after treatment with antibiotics, a small number of people who recover from typhoid fever continue to carry the bacteria in their intestinal tracts or gallbladders, often for years. These people, called chronic carriers, shed the bacteria in their faeces and are capable of infecting others, although they no longer have signs or symptoms of the disease themselves. Ø Asymptomatic human carriers (“typhoid Marys”) may also spread the disease.
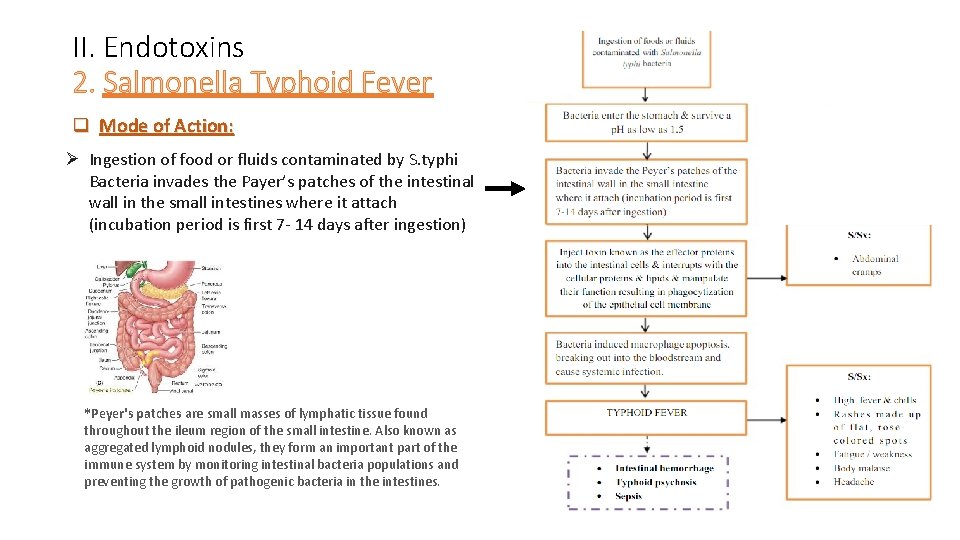
II. Endotoxins 2. Salmonella Typhoid Fever q Mode of Action: Ø Ingestion of food or fluids contaminated by S. typhi Bacteria invades the Payer’s patches of the intestinal wall in the small intestines where it attach (incubation period is first 7 - 14 days after ingestion) *Peyer's patches are small masses of lymphatic tissue found throughout the ileum region of the small intestine. Also known as aggregated lymphoid nodules, they form an important part of the immune system by monitoring intestinal bacteria populations and preventing the growth of pathogenic bacteria in the intestines.
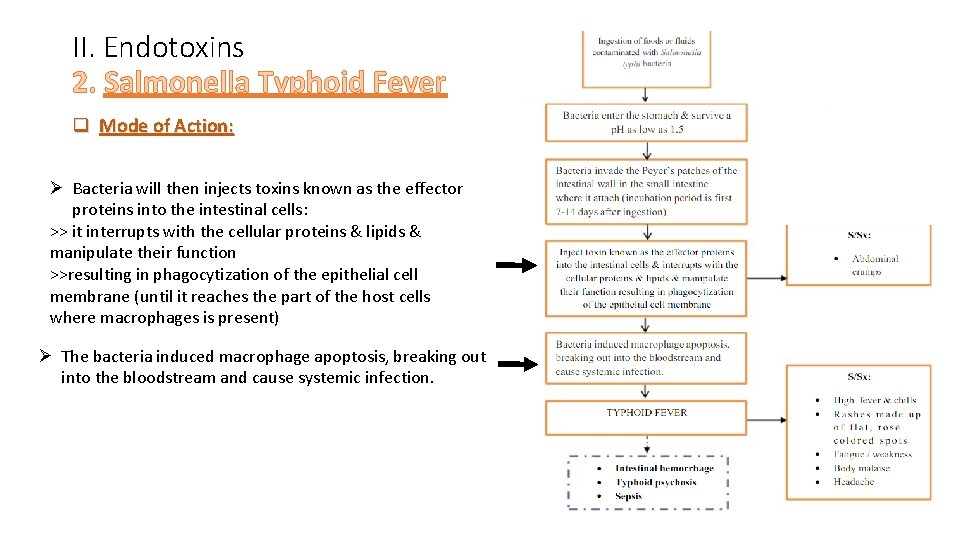
II. Endotoxins 2. Salmonella Typhoid Fever q Mode of Action: Ø Bacteria will then injects toxins known as the effector proteins into the intestinal cells: >> it interrupts with the cellular proteins & lipids & manipulate their function >>resulting in phagocytization of the epithelial cell membrane (until it reaches the part of the host cells where macrophages is present) Ø The bacteria induced macrophage apoptosis, breaking out into the bloodstream and cause systemic infection.

II. Endotoxins 2. Salmonella Typhoid Fever q Symptoms: § It's hard to tell when typhoid got started, because the symptoms are pretty similar to other gastroenteritis someone can get from drinking dirty water. § Signs and symptoms are likely to develop gradually — often appearing one to three weeks after exposure to the disease: Week 1: Fever, headache, cough and sometimes a bloody nose -symptom appeared. Week 2: A very high fever(40. 5 C), diarrhoea, rash (small flat pink spots on the trunk of the body) and confusional state (which gave typhoid the name of 'nervous fever: Many people are delirious).

II. Endotoxins 2. Salmonella Typhoid Fever q Symptoms: Third week: while most people start to get better, some people get internal bleeding or brain swelling or other problems. § The patient becomes weak with a weak pulse and raised respiratory rate. § Complications which are most likely to develop at this stage include: Intestinal haemorrhage due to bleeding from congested Peyer's patches. weak with a weak pulse and raised respiratory rate Week four: In the untreated patient the fourth week sees the fever, mental state and abdominal distension slowly improve over a few days, BUT intestinal complications (due to intestinal haemorrhage) may still occur, and most relapses occur at this stage.

II. Endotoxins 2. Salmonella Typhoid Fever q Diagnosis: Ø is by either culturing the bacteria or detecting the bacterium's DNA in the blood, stool, or bone marrow. q Treatment: Ø It is treated with antibiotics. One week after being treated, it is important to do the following: Keep taking the prescribed antibiotics for as long as the doctor has asked you to take them. Wash your hands carefully with soap and water after using the bathroom, and do not prepare or serve food for other people. This will lower the chance that you will pass the infection on to someone else. Have your doctor perform a series of stool cultures to ensure that no Salmonella Typhi bacteria remain in your body. Carrier status (Mary Typhoid) 2 -3% of patients infected with typhoid fever may have a low-grade infection. They may not develop any significant symptoms, and then become carriers of the disease.

II. Endotoxins 2. Salmonella Typhoid Fever q Vaccine: There are two vaccines to prevent typhoid: 1. An inactivated (killed) vaccine gotten as a shot. 2. A live, attenuated (weakened) vaccine which is taken orally (by mouth). Who should get typhoid vaccine and when? Typhoid vaccine is recommended for: § Travelers to parts of the world where typhoid is common. (NOTE: typhoid vaccine is not 100% effective and is not a substitute for being careful about what you eat or drink). § People in close contact with a typhoid carrier. § Laboratory workers who work with Salmonella Typhi bacteria.

II. Endotoxins 2. Salmonella Typhoid Fever q Vaccine: Who should get typhoid vaccine and when? v ü ü ü Inactivated typhoid vaccine (shot): One dose provides protection. It should be given at least 2 weeks before travel to allow the vaccine time to work. A booster dose is needed every 2 years for people who remain at risk. v Live typhoid vaccine (oral) ü Four doses: one capsule every other day for a week. The last dose should be given at least 1 week before travel to allow the vaccine time to work. ü A booster dose is needed every 5 years for people who remain at risk.

II. Endotoxins 2. Salmonella Typhoid Fever q Risk Factors Ø Typhoid fever remains a serious worldwide threat — especially in the developing world. Ø The disease is endemic in India, Southeast Asia, Africa, South America and many other areas. Ø Worldwide, children are at greatest risk of getting the disease, although they generally have milder symptoms than adults do. Ø If you live in a country where typhoid fever is RARE, you're at increased risk IF you: • Work in or travel to areas where typhoid fever is endemic • Work as a clinical microbiologist handling Salmonella typhi bacteria • Have close contact with someone who is infected or has recently been infected with typhoid fever • Drink water contaminated by sewage that contains S. typhi

II. Endotoxins 2. Salmonella Typhoid Fever q Prevention: ü Get vaccinated for typhoid: Typhoid vaccine is only 50%-80% effective, so you should still be careful about what you eat and drink. ü Eat safe foods: Eat: Food that is cooked and served hot, Hard-cooked eggs, Fruits and vegetables you have washed in clean water or peeled yourself, Pasteurized dairy products Don't Eat: Food from street vendors, Raw or soft-cooked (runny) eggs, Raw or undercooked (rare) meat or fish, Unwashed or unpeeled raw fruits and vegetables ü Drink safe beverages: Drink: Bottled water, Ice made with bottled or disinfected water, Bottled and sealed carbonated and sports drinks Don't Drink: Tap or well water, Ice made with tap or well water, Drinks made with tap or well water (such as reconstituted juice), Unpasteurized milk ü Practice hygiene and cleanliness: • • Wash your hands often. If soap and water aren’t available, clean your hands with hand sanitizer (containing at least 60% alcohol). Don’t touch your eyes, nose, or mouth. Try to avoid close contact, such as kissing, hugging, or sharing eating utensils or cups with people who are sick.
- Slides: 31