Microbial Mechanisms of Pathogenicity Basic Medical Microbiology 2016

Microbial Mechanisms of Pathogenicity Basic Medical Microbiology, 2016

Pathogenic mechanisms of microorganisms Øpathogenicity Øvirulence factors Øtoxigenesis Ønormal micro biota

Resident flora The resident flora are a huge and rich mixed population of microorganisms residing on body surfaces exposed to the environment including the skin, mucous membranes, parts of the gastrointestinal tract, urinary tract, reproductive tract, and upper respiratory tract, and are important to the host. Respiratory System w Staphylococcus, Corynebacterium, Haemophilus influenzae, Strep. Pneumoniae, Step. Viridans Skin w Staphylococcus, Corynebacterium, Propionibacterium genera, fungi (genus

Factors affecting the Course of Infection and Disease Pathogenicity and Virulence 2. Mechanism of Infection and Disease 3. Virulence factors 1.

Pathogenicity and Virulence • Pathogenicity is a property/ability of microorganisms to cause infection and disease • Virulence is the precise factors used by the microbe to invade, and damage host tissues (helps define the degree of pathogenicity) • Pathogenicity varies with a microbe’s ability to invade or harm host tissues, and with the condition of host defenses • A true /primary pathogen produces virulence factors that allow it to readily evade host defenses and to harm host tissues. True pathogens can infect normal, healthy hosts with intact defenses • An opportunistic pathogen is not highly virulent but can cause disease in persons whose defenses are compromised by predisposing conditions such as age, genetic defects, medical procedures, and underlying organic disease.

Mechanism of Infection and Disease • The portal of entry is the route by which microbes enter the tissues; primarily via skin, alimentary tract, respiratory tract (pneumonia, tuberculosis), urinogenital tract (sexually transmitted diseases), or placenta. • Pathogens that come from outside the body are exogenous; those that originate from normal flora are endogenous • The size of the infectious dose is of great importance in pathogenesis • In the process of adhesion, a microbe attaches to the host cell by means of fimbriae, flagella, capsules or receptors that position it for invasion

Virulence Factors • Exoenzymes digest epithelial tissues, disrupt tissues, and permit invasion of pathogens • Toxigenicity is a microbe’s capacity to produce toxins at site of multiplication which affect cellular targets. • Antiphagocytic factors include Leukocidins (white blood cell poisons) and capsules

Steps for infections by pathogenic bacteria include; Maintain a reservoir Initially be transported to the host. Adhere to, and/ or colonize the host Multiply (grow) or complete its life cycle on or in the host or the host’s cells. 5. Initially evade the host defense mechanisms 6. Possess the ability to damage the host. 7. Leave the host and return to the reservoir or enter a new host (portal of exit). 1. 2. 3. 4.

Pathogenicity - ability to cause disease Virulence - degree of pathogenicity w Many properties that determine a microbe’s pathogenicity or virulence are unclear or unknown w But, when a microbe overpowers the hosts defenses, disease results!
10

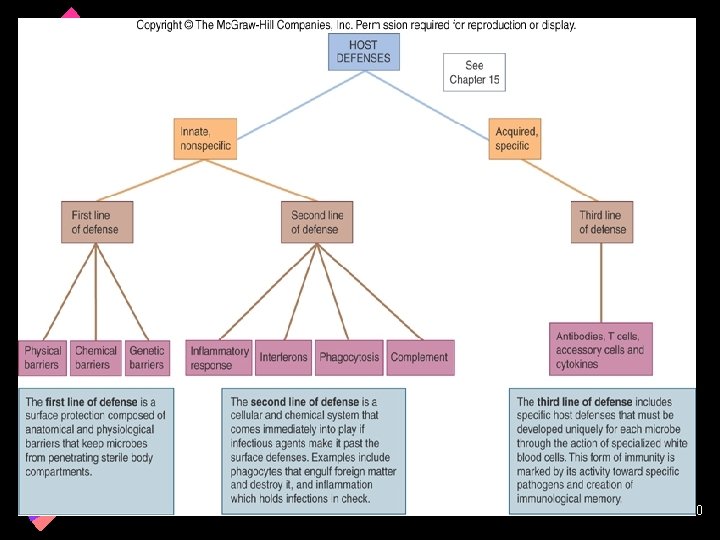
Defense Mechanisms of the Host w To protect the body against pathogens, the immune system relies on a multilevel network of physical barriers, immunologically active cells, and a variety of chemicals. • first line of defense – any barrier that blocks invasion at the portal of entry – nonspecific • second line of defense – protective cells and fluids; inflammation and phagocytosis – nonspecific • third line of defense – acquired with exposure to foreign substance; produces protective antibodies and creates memory cells – specific 11

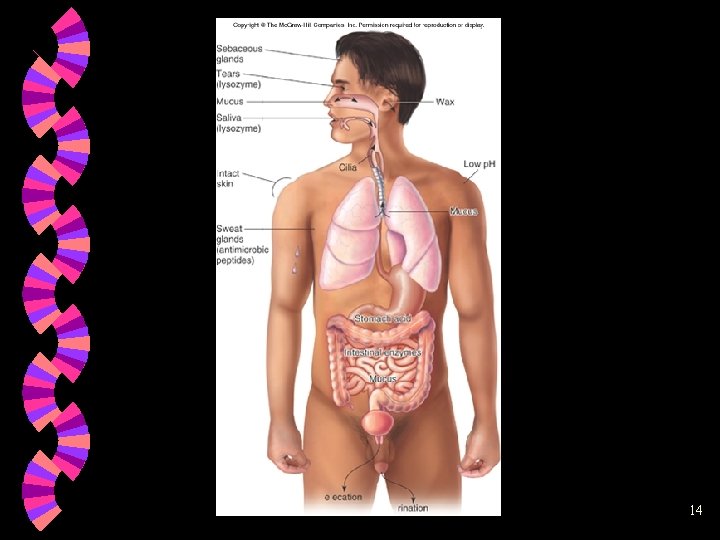
Physical or Anatomical Barriers: First Line of Defense Skin and mucous membranes of respiratory, urogenital, eyes and digestive tracts • outermost layer of skin is composed of epithelial cells compacted, cemented together and impregnated with keratin; few pathogens can penetrate if intact • flushing effect of sweat glands • damaged cells are rapidly replaced • mucous coat impedes attachment and entry of bacteria • blinking and tear production • stomach acid • nasal hair traps larger particles 12

Nonspecific Chemical Defenses w w w w Sebaceous secretions Lysozyme, an enzyme that hydrolyzes the cell wall of bacteria, in tears High lactic acid and electrolyte concentration in sweat Skin’s acidic p. H Hydrochloric acid in stomach Digestive juices and bile of intestines Semen contains antimicrobial chemical. Vagina has acidic p. H. 13
14

Genetic Defenses Some hosts are genetically immune to the diseases of other hosts. w Some pathogens have great specificity. w Some genetic differences exist in susceptibility. w 15

Portals of Entry w 1. Mucus Membranes w 2. Skin w 3. Parentarel
1. Mucus Membranes w A. Respiratory Tract • microbes inhaled into mouth or nose in droplets of moisture or dust particles • Easiest and most frequently traveled portal of entry

Common Diseases contracted via the Respiratory Tract w w w w Common cold Flu Tuberculosis Whooping cough Pneumonia Measles Strep Throat Diphtheria
Mucus Membranes w B. Gastrointestinal Tract • microbes gain entrance thru contaminated food & water or fingers & hands • most microbes that enter the G. I. Tract are destroyed by HCL & enzymes of stomach or bile & enzymes of small intestine

Common diseases contracted via the G. I. Tract w Salmonellosis • Salmonella sp. w Shigellosis • Shigella sp. w Cholera • Vibrio cholorea w Ulcers • Helicobacter pylori w Botulism • Clostridium botulinum

Fecal - Oral Diseases w These pathogens enter the G. I. Tract at one end and exit at the other end. w Spread by contaminated hands & fingers or contaminated food & water w Poor personal hygiene.
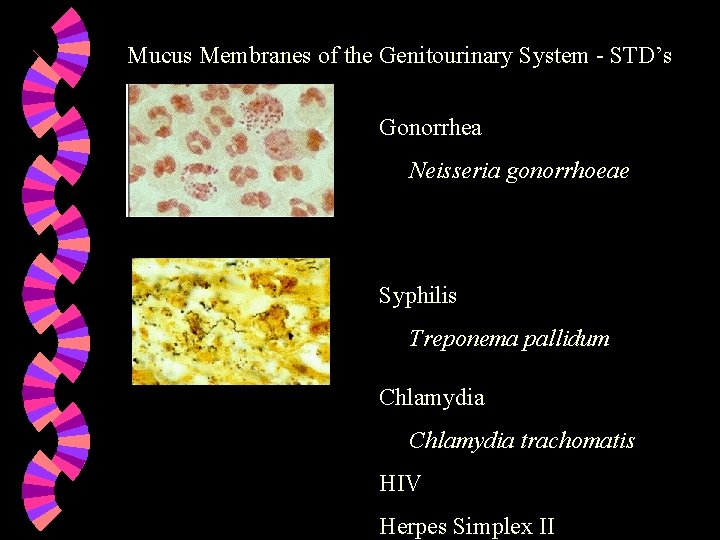
Mucus Membranes of the Genitourinary System - STD’s Gonorrhea Neisseria gonorrhoeae Syphilis Treponema pallidum Chlamydia trachomatis HIV Herpes Simplex II
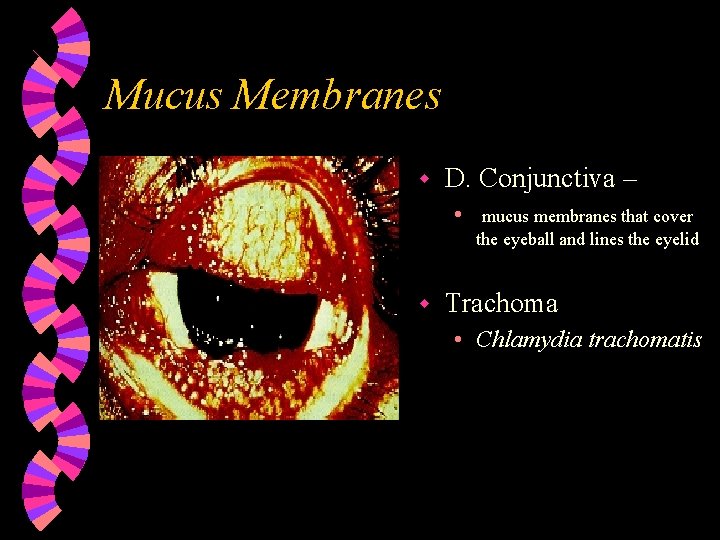
Mucus Membranes w D. Conjunctiva – • w mucus membranes that cover the eyeball and lines the eyelid Trachoma • Chlamydia trachomatis

2 nd Portal of Entry: Skin w Skin - the largest organ of the body. When unbroken is an effective barrier for most microorganisms. w Some microbes can gain entrance thru openings in the skin: hair follicles and sweat glands

3 rd Portal of Entry: Parentarel w w w w Microorganisms are deposited into the tissues below the skin or mucus membranes Punctures injections bites scratches surgery splitting of skin due to swelling or dryness

Preferred Portal of Entry w w Just because a pathogen enters your body it does not mean it’s going to cause disease. pathogens - preferred portal of entry

Preferred Portal of Entry w Streptococcus pneumoniae • if inhaled can cause pneumonia • if enters the G. I. Tract, no disease w Salmonella typhi • if enters the G. I. Tract can cause Typhoid Fever • if on skin, no disease

Number of Invading Microbes LD 50 - Lethal Dose of a microbes toxin that will kill 50% of experimentally inoculated test animal w ID 50 - infectious dose required to cause disease in 50% of inoculated test animals w • Example: ID 50 for Vibrio cholerea 108 cells (100, 000 cells) • ID 50 for Inhalation Anthrax - 5, 000 to 10, 000 spores ? ?
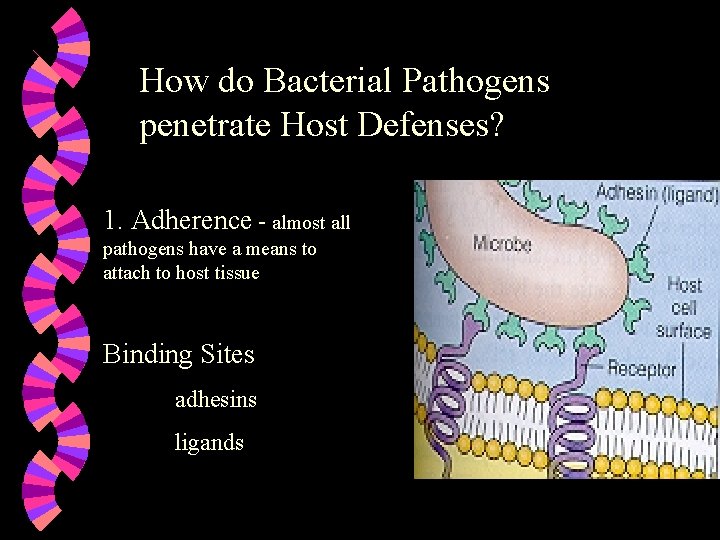
How do Bacterial Pathogens penetrate Host Defenses? 1. Adherence - almost all pathogens have a means to attach to host tissue Binding Sites adhesins ligands
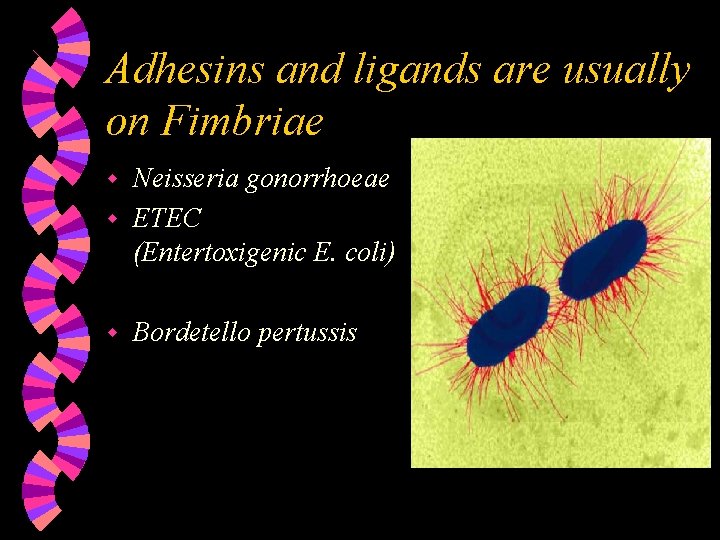
Adhesins and ligands are usually on Fimbriae Neisseria gonorrhoeae w ETEC (Entertoxigenic E. coli) w w Bordetello pertussis
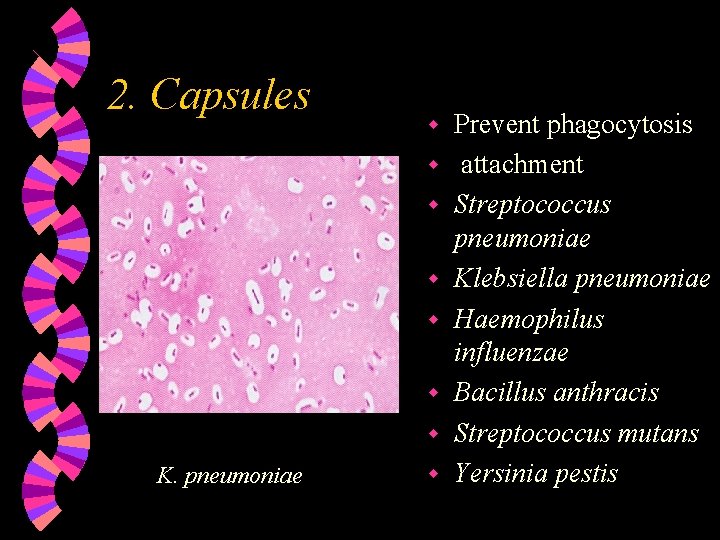
2. Capsules w w w w K. pneumoniae w Prevent phagocytosis attachment Streptococcus pneumoniae Klebsiella pneumoniae Haemophilus influenzae Bacillus anthracis Streptococcus mutans Yersinia pestis

3. Enzymes w Many pathogens secrete enzymes that contribute to their pathogenicity

A. Leukocidins w Attack certain types of WBC’s 1. Kills WBC’s which prevents phagocytosis w 2. Releases & ruptures lysosomes w • lysosomes - contain powerful hydrolytic enzymes which then cause more tissue damage
B. Hemolysins - cause the lysis of RBC’s Streptococci

1. Alpha Hemolytic Streptococci - secrete hemolysins that cause the incomplete lysis or RBC’s
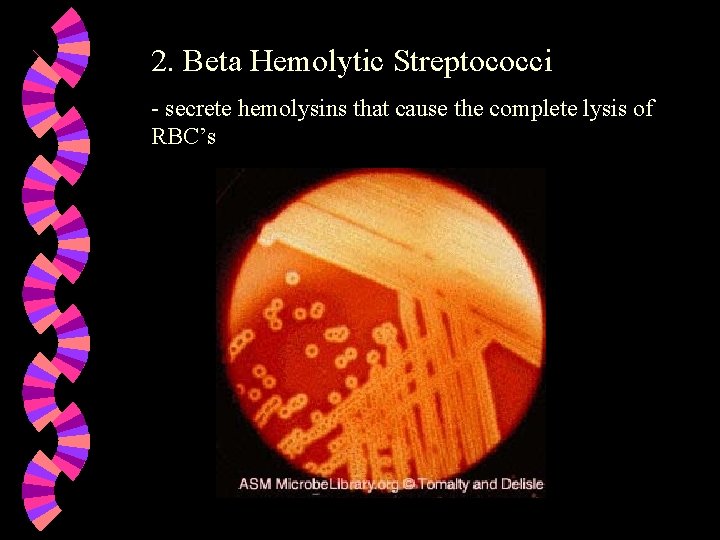
2. Beta Hemolytic Streptococci - secrete hemolysins that cause the complete lysis of RBC’s

3. Gamma Hemolytic Streptococci - do not secrete any hemolysins

C. Coagulase - cause blood to coagulate w Blood clots protect bacteria from phagocytosis from WBC’s and other host defenses w Staphylococci - are often coagulase positive • boils • abscesses

D. Kinases - enzymes that dissolve blood clots 1. Streptokinase - Streptococci w 2. Staphylokinase - Staphylococci w w Helps to spread bacteria - Bacteremia w Streptokinase - used to dissolve blood clots in the Heart (Heart Attacks due to obstructed coronary blood vessels)

E. Hyaluronidase w Breaks down Hyaluronic acid (found in connective tissues) w “Spreading Factor” w mixed with a drug to help spread the drug thru a body tissue

F. Collagenase w Breaks down collagen (found in many connective tissues) w Clostridium perfringens - Gas Gangrene • uses this to spread thru muscle tissue
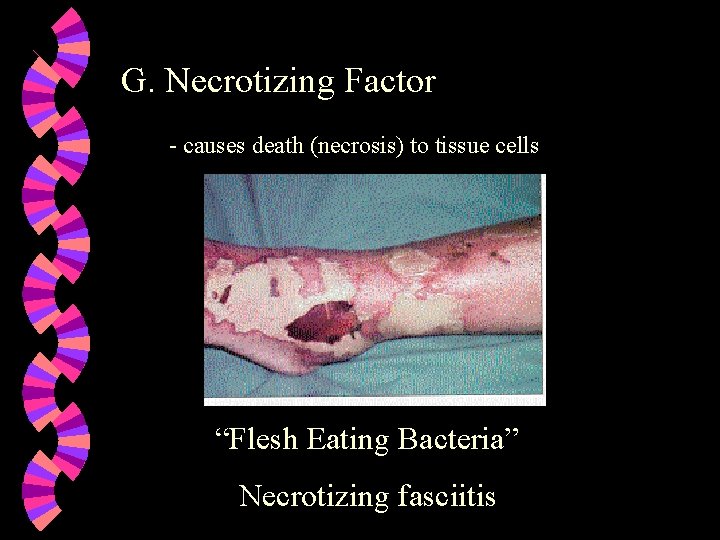
G. Necrotizing Factor - causes death (necrosis) to tissue cells “Flesh Eating Bacteria” Necrotizing fasciitis

Summary of How Bacterial Pathogens Penetrate Host Defenses 1. Adherence w 2. Capsule w 3. Enzymes w • • A. leukocidins B. Hemolysins C. Coagulase D. Kinases E. Hyaluronidase F. Collagenase G. Necrotizing Factor

4. Toxins Poisonous substances produced by microorganisms w toxins - primary factor - pathogenicity w 220 known bacterial toxins w • 40% cause disease by damaging the Eukaryotic cell membrane w Toxemia • Toxins in the bloodstream

Diseases caused by exotoxins Disease Bacterium Botulinism Clostridium botulinum Tetanus Clostridium tetani Gas gangrene & food poisoning Clostridium perfringens & other species of clostridium Diphtheria Corynebacterium diphtheriae Scalded skin syndrome, food poisoning, and toxic shock syndrome Staphylococcus aureus Cholera Vibrio cholera Scarlet fever Streptococcus pyogenes Traveler’s diarrhea Enterotoxigenic E. coli & Shigella spp

2 Types of Toxins w 1. Exotoxins • secreted outside the bacterial cell w 2. Endotoxins • part of the outer cell wall of Gram (-) bacteria

Exotoxins w Mostly seen in Gram (+) Bacteria w Most gene that code for exotoxins are located on plasmids or phages

3 Types of Exotoxins w 1. Cytotoxins • kill cells w 2. Neurotoxins • interfere with normal nerve impulses w 3. Enterotoxins • effect cells lining the G. I. Tract

Response to Toxins If exposed to exotoxins: antibodies against the toxin (antitoxins) w Exotoxins inactivated ( heat, formalin or phenol) no longer cause disease, but stimulate the production of antitoxin w • altered exotoxins - Toxoids w Toxoids - injected to stimulate the production of antitoxins and provide immunity

Example: DPT Vaccine w D - Diphtheria • Corynebacterium diphtheriae w P - Pertussis • Bordetello pertussis w T - Tetanus • Clostridium tetani DPT - Diphtheria Toxoid Pertussis Antigen Tetanus Toxoid

Required Immunizations w w w 1. Diphtheria 2. Pertussis 3. Tetanus 4. Measles 5. Mumps 6. Rubella w w w Corynebacterium diphtheriae Bordetello pertussis Clostridium tetani Measles virus Mumps virus Rubella virus • German Measles 7. Polio w 8. Hib w 9. Hepatitis B w 10. Chicken Pox w Polio virus w Haemophilus influenzae w Hepatitis B Virus w Varicella-zoster virus w

Type of Vaccines w w w w D P T M M R Polio • Salk • Sabin Hib w HBV w w w Toxoid Antigen Toxoid Attenuated IPV – Inactivated Polio virus (Killed) 1953 OPV – Oral Polio vaccine (attenuated) 1964 Conjugated vaccine Recombinant vaccine (antigen) yeast • Capsid produced by genetically engineered yeast w Chicken Pox w Attenuated
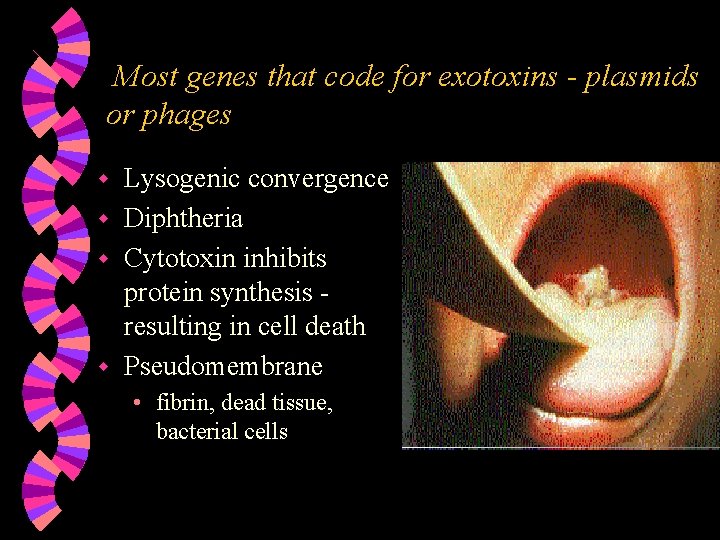
Most genes that code for exotoxins - plasmids or phages Lysogenic convergence w Diphtheria w Cytotoxin inhibits protein synthesis resulting in cell death w Pseudomembrane w • fibrin, dead tissue, bacterial cells

Lysogenic Convergence Scarlet Fever w Streptococcus pyogenes w • lysogenic convergence w prophage • cytotoxin - damages blood capillaries and results in a skin rash • Strep Thoat with a rash

Diseases caused by Neurotoxins w Botulism • Clostridium botulinum • Gram (+), anaerobic, spore-forming rod, found in soil • works at the neuromuscular junction • prevents impulse from nerve cell to muscle cell • results in muscle paralysis

Tetanus (Lock Jaw) w Clostridium tetani Gram (+), spore-forming, anaerobic rod w neurotoxin acts on nerves, resulting in the inhibition of muscle relaxation w tetanospasmin - “spasms” or “Lock Jaw” w
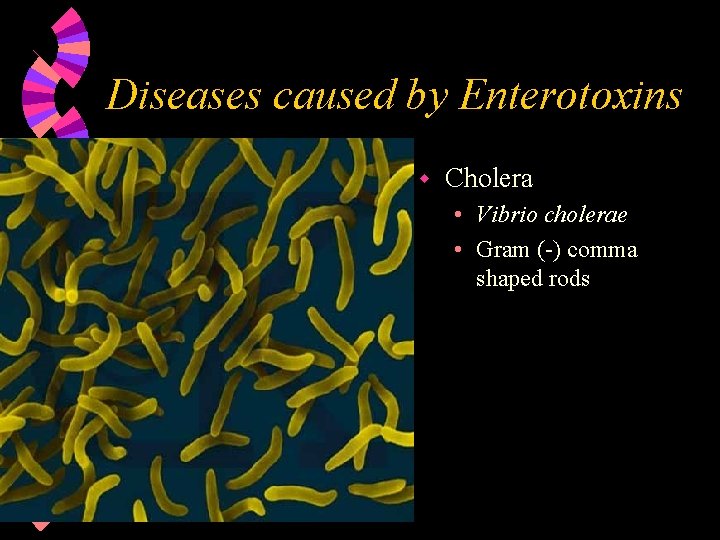
Diseases caused by Enterotoxins w Cholera • Vibrio cholerae • Gram (-) comma shaped rods

Cholera toxin Converts ATP into c. AMP w causes cells to excrete Cl- ions and inhibits absorption of Na+ ions w Electrolyte imbalance w H 2 O leaves by osmosis w H 2 O Loss (Diarrhea) w

Severe cases, 12 - 20 liters of liquid lost in a day w Untreated cases - Mortality Rate about 50% w Mortality may be reduced to about 1% • administering fluids and electrolytes

EHEC (Enterohemorrhagic E. coli) E. coli (0157: H 7) w enterotoxin causes a hemolytic inflammation of the intestines w results in bloody diarrhea w • Toxin • • • alters the 60 S ribosomal subunit inhibits Protein Synthesis Results in cell death lining of intestine is “shed” Bloody Diarrhea (Dysentary)

Endotoxins - part of the Gram (-) Bacterial cell wall w LPS (Lipopolysaccharides) • O Antigen • Lipid A w Lipid A - Toxin portion of the LPS • responsible for Fever that is associated with many Gram (-) Bacterial infections • Gram (-) cells are “digested” endotoxins are released - fever • Antibiotics

Differences between exotoxins and endotoxins Property Exotoxins Endotoxins Bacterial source Mostly from gram-positive bacteria Almost exclusively from gram-negative bacteria plus a few gram-positive bacteria Metabolic product of growing cell Presence from LPS of outer membrane of cell wall & released only with lysis of cell Chemistry Protein or short peptide Lipid portion (lipid A) of LPS of outer membrane Heat stability Unstable; can easily be destroyed at 60 - 80 o. C (except staphylococcal enterotoxins) Stable, can withstand autoclaving (121 o. C for one hour. Toxicity High Low Immunology Can be converted to toxoids, neutralized by antitoxins Not easily neutralized by antitoxin, therefore effective toxoids cant be made Pharmacology Specific for a particular cell structure or function in the host (mainly cytotoxins, neurotoxins & enterotoxins) General such as fever, weakness, aches, and shock; all produce the same effects Lethal dose Small Considerably large Representative disease Gas gangrene, tetanus, botulinism, diphtheria, scarlet fever, cholera, traveler’s diarrhea Typhoid fever, urinary tract infections, and meningococcal meningitis Relation microbe to

Thx for listening attentively, Any questions?
- Slides: 64