METABOLISM OF PURINE NUCLEOTIDES PURINE DISORDERS ROLES OF

METABOLISM OF PURINE NUCLEOTIDES & PURINE DISORDERS
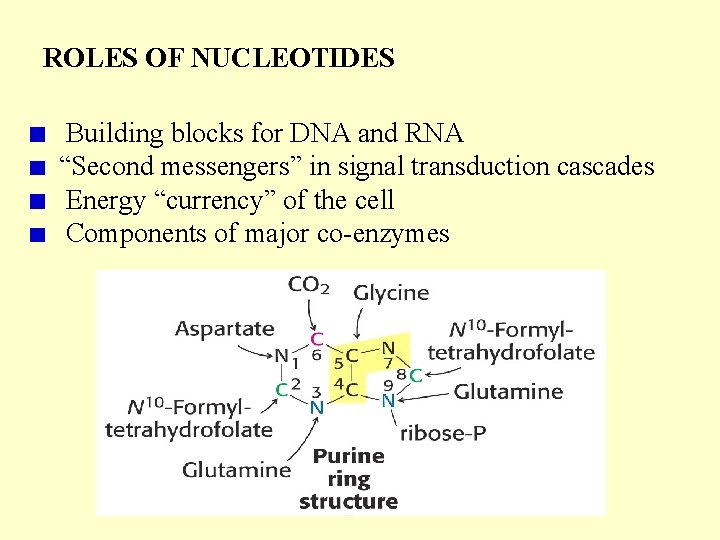
ROLES OF NUCLEOTIDES Building blocks for DNA and RNA “Second messengers” in signal transduction cascades Energy “currency” of the cell Components of major co-enzymes

Purine Biosynthesis • Major site – (Adenine & Guanine) in the Liver. • Synthesis starting from Ribose-5 -phosphate Denova pathway: Precursors contribute to form the Purine ring: Glycine (C 4, C 5, N 7), Glutamine ( N 3, N 9), THF (C 2, C 8 atoms) Aspartate (N 1 atom), & CO 2 (C 6 atom). • The construction of 6 -membered ring forms Inosine- 5 monophosphate (IMP) – 1 st Purine. • Energetics – expenditure of 6 high energy bonds. Salvage pathway - Free & dietary purine can be converted into corresponding nucleotides (no need ATP). • RBC, Neutrophils & Brain cannot produce Purines by de novo synthesis. But by only salvage pathway (HGPRTase).
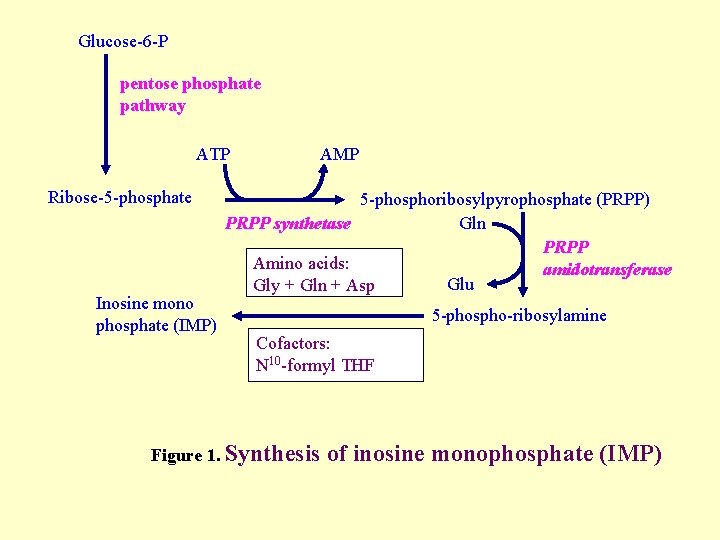
Glucose-6 -P pentose phosphate pathway ATP Ribose-5 -phosphate Inosine mono phosphate (IMP) AMP 5 -phosphoribosylpyrophosphate (PRPP) PRPP synthetase Gln PRPP Amino acids: amidotransferase Glu Gly + Gln + Asp 5 -phospho-ribosylamine Cofactors: N 10 -formyl THF Figure 1. Synthesis of inosine monophosphate (IMP)
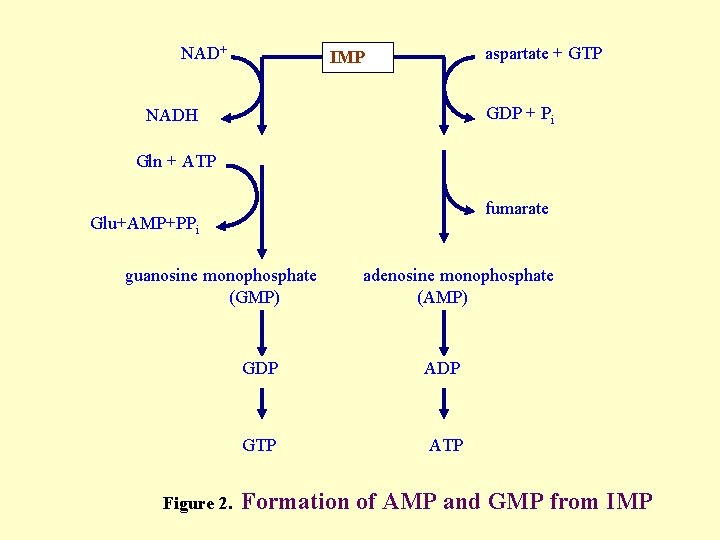
NAD+ aspartate + GTP IMP GDP + Pi NADH Gln + ATP fumarate Glu+AMP+PPi guanosine monophosphate (GMP) Figure 2. adenosine monophosphate (AMP) GDP ADP GTP ATP Formation of AMP and GMP from IMP
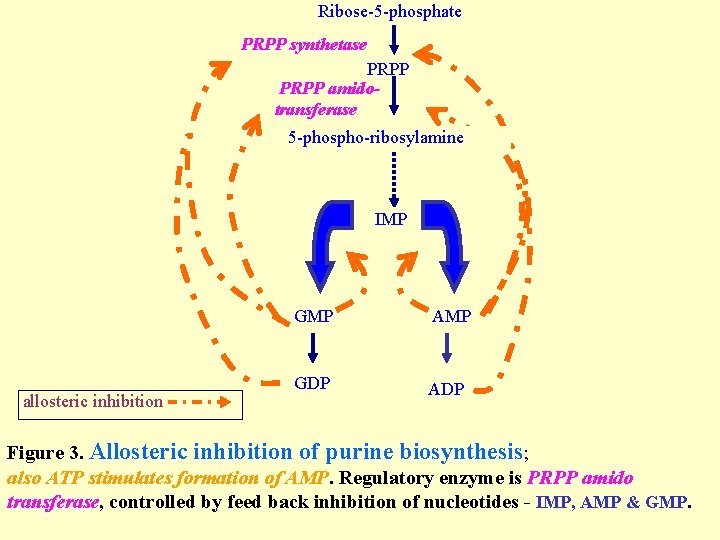
Ribose-5 -phosphate PRPP synthetase PRPP amidotransferase 5 -phospho-ribosylamine IMP allosteric inhibition GMP AMP GDP ADP Figure 3. Allosteric inhibition of purine biosynthesis; also ATP stimulates formation of AMP. Regulatory enzyme is PRPP amido transferase, controlled by feed back inhibition of nucleotides - IMP, AMP & GMP.
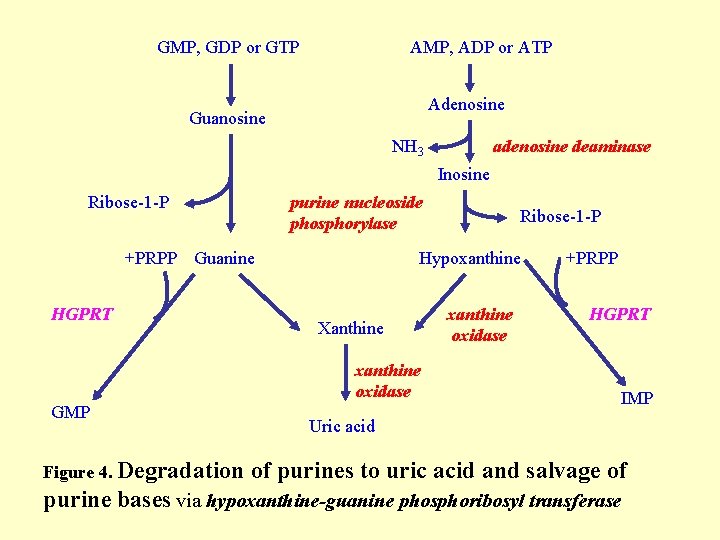
GMP, GDP or GTP AMP, ADP or ATP Adenosine Guanosine NH 3 adenosine deaminase Inosine Ribose-1 -P purine nucleoside phosphorylase +PRPP Guanine HGPRT Ribose-1 -P Hypoxanthine Xanthine xanthine oxidase +PRPP HGPRT xanthine oxidase GMP Figure 4. Degradation IMP Uric acid of purines to uric acid and salvage of purine bases via hypoxanthine-guanine phosphoribosyl transferase
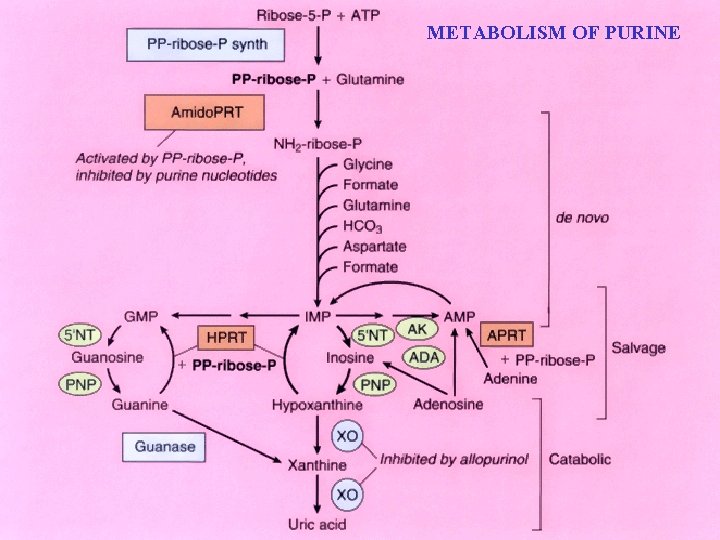
METABOLISM OF PURINE
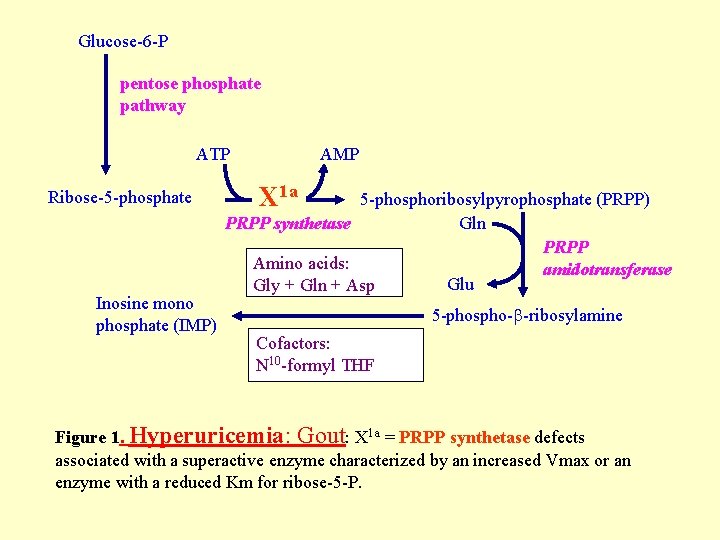
Glucose-6 -P pentose phosphate pathway ATP Ribose-5 -phosphate Inosine mono phosphate (IMP) AMP X 1 a 5 -phosphoribosylpyrophosphate (PRPP) PRPP synthetase Gln PRPP Amino acids: amidotransferase Glu Gly + Gln + Asp 5 -phospho- -ribosylamine Cofactors: N 10 -formyl THF Figure 1. Hyperuricemia: Gout: X 1 a = PRPP synthetase defects associated with a superactive enzyme characterized by an increased Vmax or an enzyme with a reduced Km for ribose-5 -P.

Disorder of Purine catabolism • In humans, Purine rings are degraded to the metabolically inert uric acid. • Normal level of uric acid in blood is 2 -7 mg/dl (Female) & 3 -8 mg/dl (Male). • Uric acid excretion in urine is about 500 – 700 mg/day. 1. GOUT (Hyper uricemia) • An inherited metabolic disease • Incidence - 3 /1000 person • Defect - partial deficiency of HGPRTase or increased levels of PRPP caused by a hyperactive synthetase. • Causes - ↓ Synthesis of GMP and IMP & ↑ in PRPP levels --> ↑d Purine biosynthesis by de novo pathway.

Gout 1. Primary gout: • Inborn error of metabolism due to over production of uric acid • Causes: Varient PRPP synthetase, PRPP gltamyl amido transferase, HGPRT deficiency, Glu-6 -Pase defiecincy. 2. Secondary gout: • Various disease causing ↑or ↓uric acid excretion. • E. g. : Cancer, Psoriasis, Trauma, Starvation, Impairment in renal function leads to gout.

GOUT Causes • Uricosuria • Accumulation of sodium urate crystals in the soft tissues called Tophi -causes painful Gouty - Arthritis. • Deposition of Na-urate crystals -Renal calculi • Clinical finding- Red faced, Acidosis & Renal damage. Treatment • Reduced dietary Purine intake & restrict alcohol is advised. • Uricosuric drugs. For example – Probenecid (Benemide), Salicylates and Halofenate. • Allopurinol (analog of hypoxanthine) competitively inhibits Xanthine oxidase & thus uric acid synthesis (Suicide inhibition) • Coichicine is an anti-inflammatory drug to relieve pain. Other useful drugs include Indomethacin, Naproxen, Brufen, Corticosteroids etc.

2. LESCH-NYHAN SYNDROME • • • X-linked recessive disorder of Purine metabolism. Incidence is 1 in 10, 000 males Defect - Total lack of HGPRTase, salvage pathway Thus ↑ PRPP (de novo pathway), ↑ production of uric acid. Diagnosis - Murexide test (reddish deposit) to detect urine uric acid Clinical manifestations • ↑ Production of uric acid causes severe gout, poor growth, and renal failure due to Nephrolithiasis. • Neurological abnormalities such as Mental retardation, Aggressive behavior, learning disability & compulsive selfdestructive behavior. • Irresistible urge to bite their finger & lips (Self mutilation) • It shows that abnormal behavior can be caused by absence of a single enzyme.
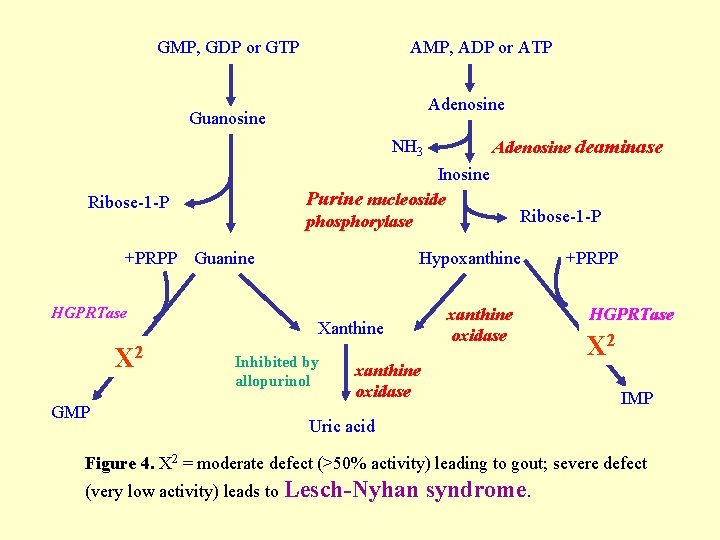
GMP, GDP or GTP AMP, ADP or ATP Adenosine Guanosine NH 3 Inosine Purine nucleoside phosphorylase Ribose-1 -P +PRPP Guanine HGPRTase X 2 GMP Adenosine deaminase Ribose-1 -P Hypoxanthine Xanthine Inhibited by allopurinol xanthine oxidase +PRPP HGPRTase X 2 IMP Uric acid Figure 4. X 2 = moderate defect (>50% activity) leading to gout; severe defect (very low activity) leads to Lesch-Nyhan syndrome.

3. Immunodeficiency diseases • Immunodeficiency diseases are associated with Purine degradation disorders. • Defect: Adenosine deaminase & Purine nucleoside phosphorylase involved in uric acid synthesis. • Causes: Severe combined immunodeficiency (SCID) involving T-cell & usually B-cell dysfunctions and thus impaired the immunity. • Uric acid synthesis ↓& tissue level of N. S & N. T↑ • Treatment: Transferring ADA gene by Gene therapy.

4. Hypo uricemia Hypoxanthine • When serum uric acid level is less than 2 mg/dl represents hypouricemia. • A rare congenital Xanthine oxidase deficiency • Incidence is 1 in 45, 000. xanthin e Xanthine oxidase xanthin e oxidase Uric acid • It leads to the increased excretion of Xanthine & Hypoxanthine. • Causes: Excretion of xanthine in urine - Xanthinuria. Frequently causes the formation of Xanthine stones in the urinary tract.

SYNTHESIS OF PYRIMIDINE NUCLEOTIDES & PYRIMIDINE DISORDERS

SYNTHESIS OF PYRIMIDINE NUCLEOTIDES • Synthesis of the Pyrimidine is less complex than that of the purines, since the base is much simpler (6 member ring). • Precursors – Carbomyl phosphate & Aspartate • De novo synthesis - in the Liver cytosol • Energetic: Requires 2 ATP
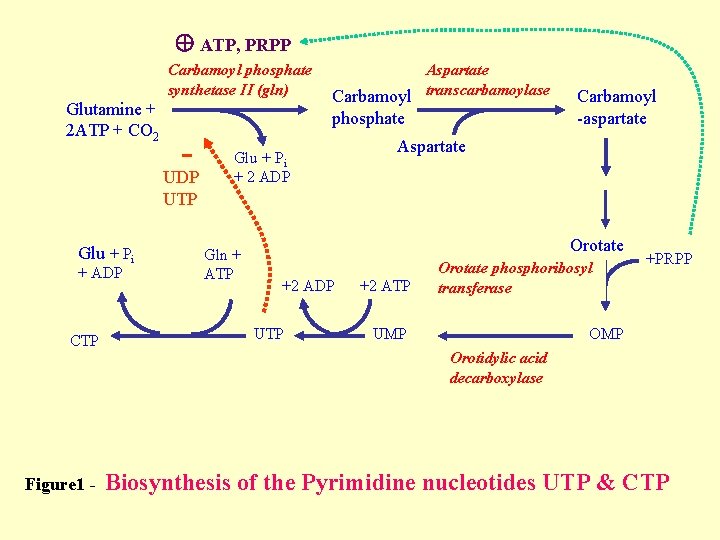
ATP, PRPP Carbamoyl phosphate synthetase II (gln) Glutamine + 2 ATP + CO 2 phosphate - UDP UTP Glu + Pi + ADP CTP Figure 1 - Aspartate Carbamoyl transcarbamoylase Glu + Pi + 2 ADP Gln + ATP Carbamoyl -aspartate Aspartate Orotate +2 ADP UTP +2 ATP Orotate phosphoribosyl transferase UMP +PRPP OMP Orotidylic acid decarboxylase Biosynthesis of the Pyrimidine nucleotides UTP & CTP
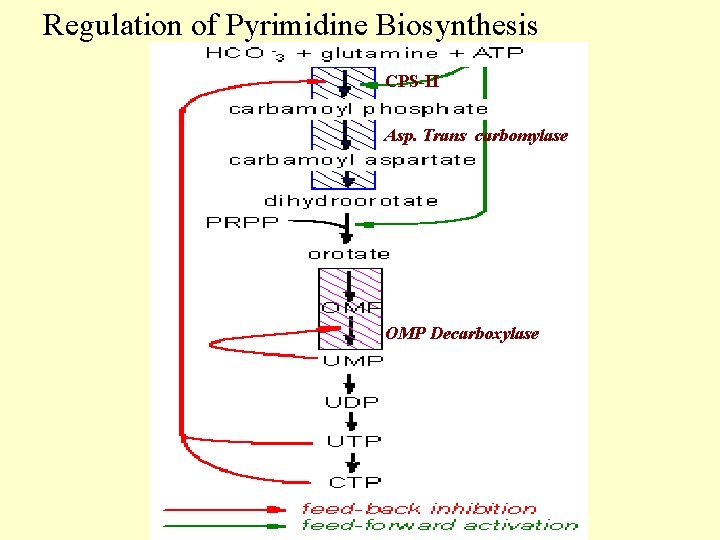
Regulation of Pyrimidine Biosynthesis CPS-II Asp. Trans carbomylase OMP Decarboxylase

CATABOLISM OF PYRIMIDINE NUCLEOTIDES • Pyrimidine degraded in the liver. • The end products - are nitrogenous bases Cytosine, Uracil and Thymine. • The bases are then degraded to amino acids, namely β -Alanine (from Cytosine & Uracil) & β-Amino isobutyrate (from Thymine). • These amino acids undergo transamination & other reactions to finally produce Acetyl co. A, Succinate & CO 2. • Clinical significance: β-Aminoisobutyrate is excreted in large quantity in Leukemia & when body subjected to X-ray irradiation.
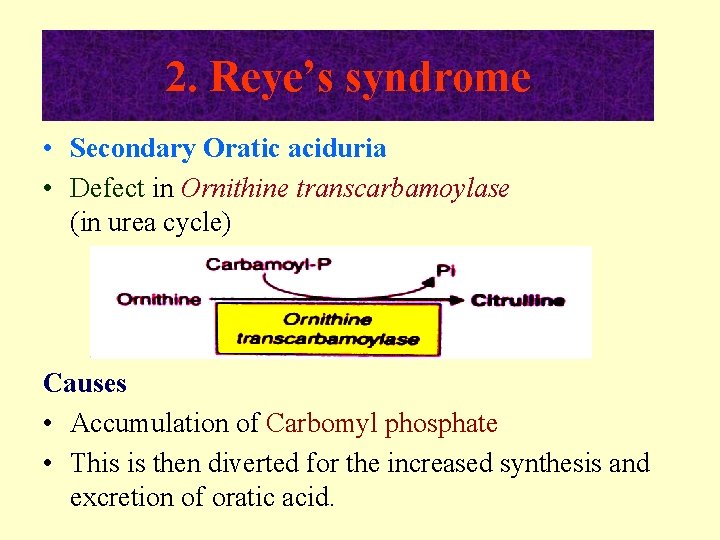
2. Reye’s syndrome • Secondary Oratic aciduria • Defect in Ornithine transcarbamoylase (in urea cycle) Causes • Accumulation of Carbomyl phosphate • This is then diverted for the increased synthesis and excretion of oratic acid.
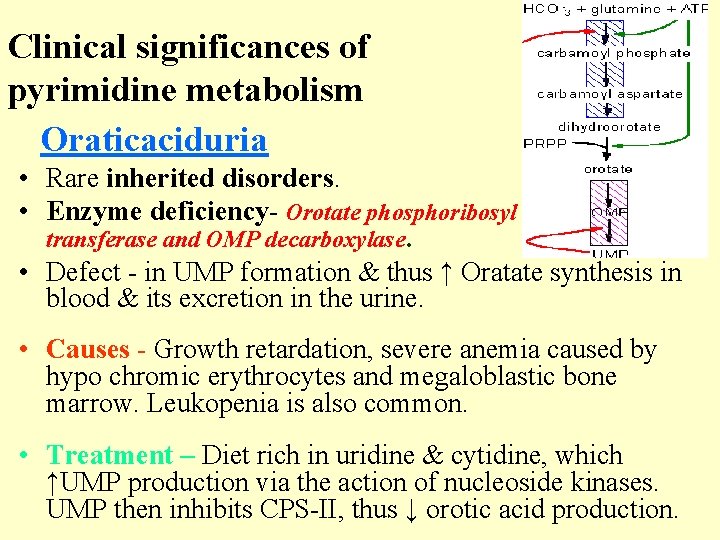
Clinical significances of pyrimidine metabolism Oraticaciduria • Rare inherited disorders. • Enzyme deficiency- Orotate phosphoribosyl transferase and OMP decarboxylase. • Defect - in UMP formation & thus ↑ Oratate synthesis in blood & its excretion in the urine. • Causes - Growth retardation, severe anemia caused by hypo chromic erythrocytes and megaloblastic bone marrow. Leukopenia is also common. • Treatment – Diet rich in uridine & cytidine, which ↑UMP production via the action of nucleoside kinases. UMP then inhibits CPS-II, thus ↓ orotic acid production.
- Slides: 23