Metabolism of heme Alice Skoumalov Heme structure a

Metabolism of heme Alice Skoumalová
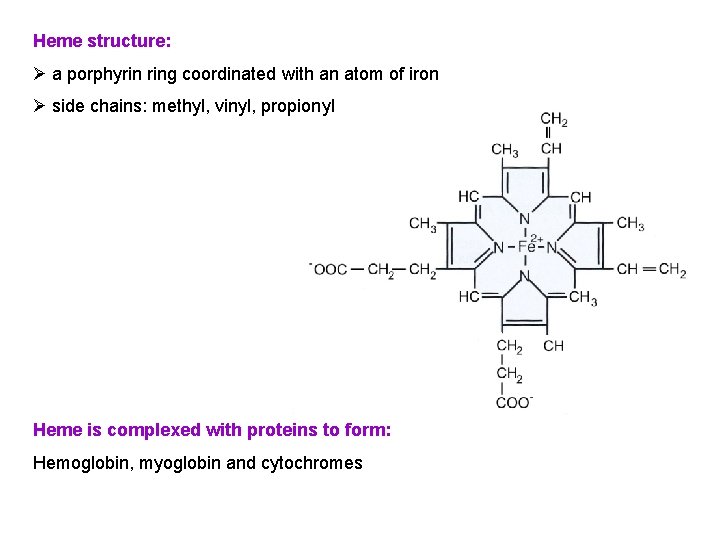
Heme structure: Ø a porphyrin ring coordinated with an atom of iron Ø side chains: methyl, vinyl, propionyl Heme is complexed with proteins to form: Hemoglobin, myoglobin and cytochromes
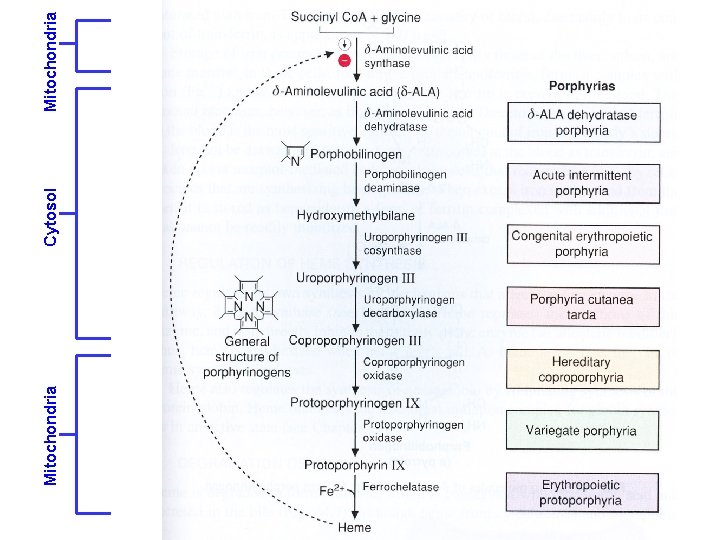
Mitochondria Cytosol Mitochondria
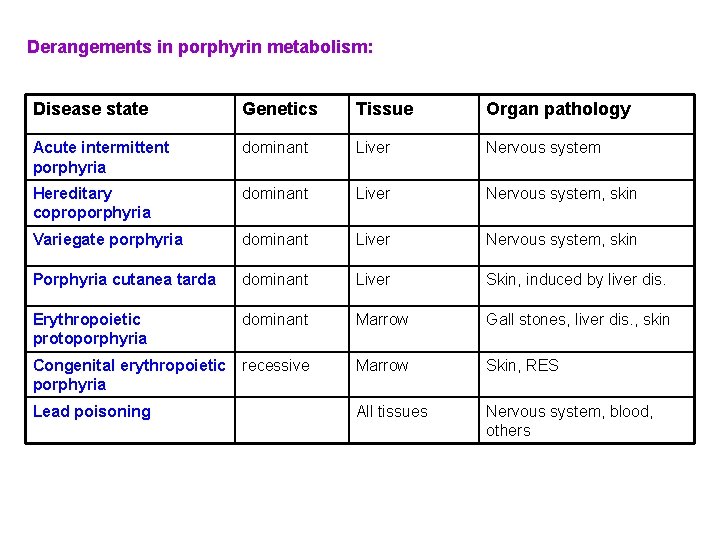
Derangements in porphyrin metabolism: Disease state Genetics Tissue Organ pathology Acute intermittent porphyria dominant Liver Nervous system Hereditary coproporphyria dominant Liver Nervous system, skin Variegate porphyria dominant Liver Nervous system, skin Porphyria cutanea tarda dominant Liver Skin, induced by liver dis. Erythropoietic protoporphyria dominant Marrow Gall stones, liver dis. , skin Congenital erythropoietic porphyria recessive Marrow Skin, RES All tissues Nervous system, blood, others Lead poisoning
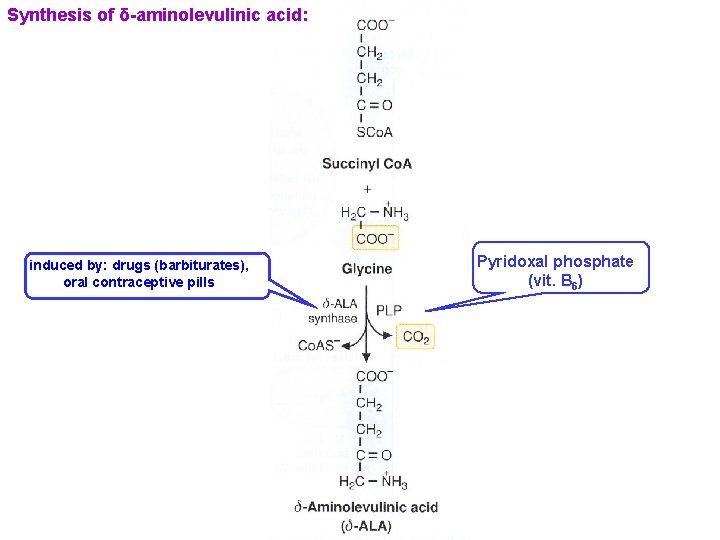
Synthesis of δ-aminolevulinic acid: induced by: drugs (barbiturates), oral contraceptive pills Pyridoxal phosphate (vit. B 6)
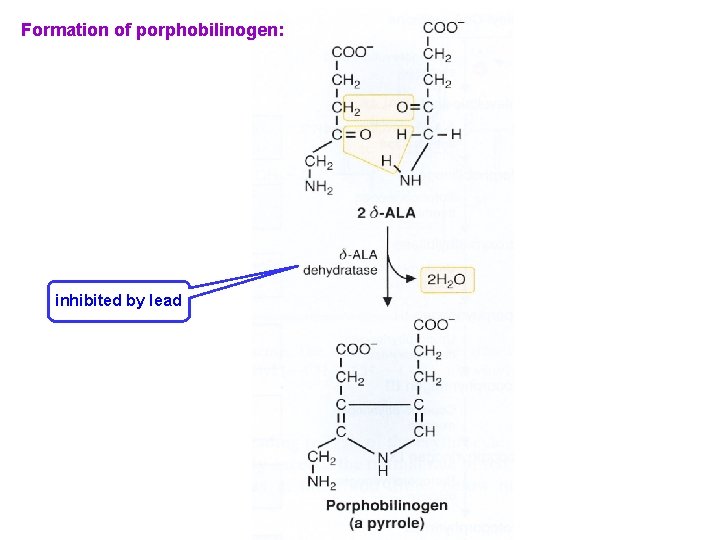
Formation of porphobilinogen: inhibited by lead
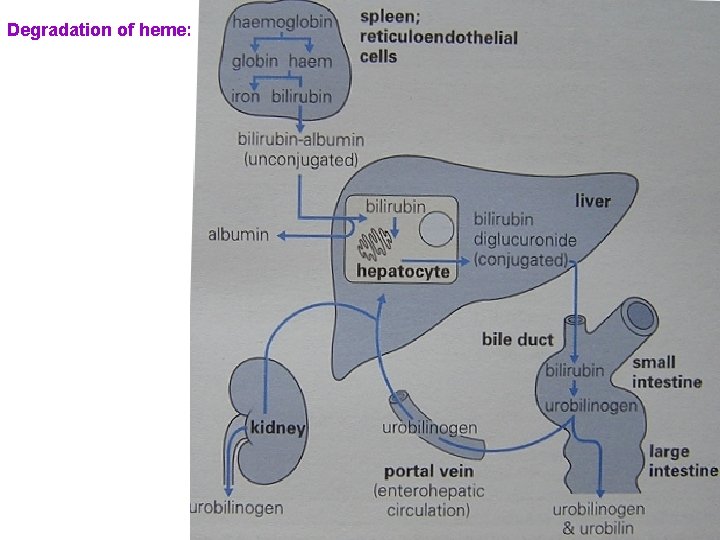
Degradation of heme:
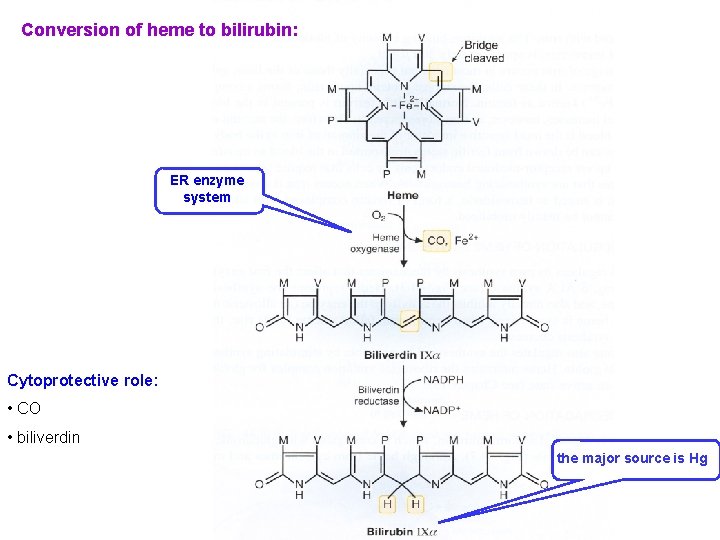
Conversion of heme to bilirubin: ER enzyme system Cytoprotective role: • CO • biliverdin the major source is Hg
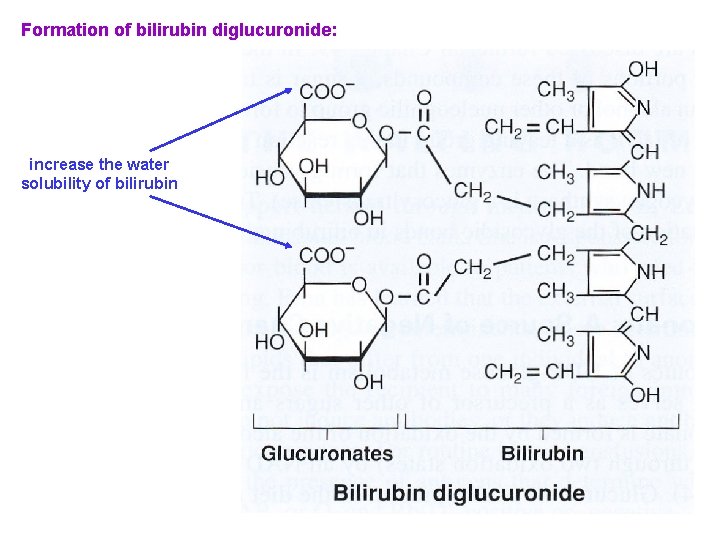
Formation of bilirubin diglucuronide: increase the water solubility of bilirubin

Hyperbilirubinemia Ø Elevated bilirubin levels in the blood (>10 mg/l); bilirubin may diffuse into peripheral tissues, giving them a yellow color (jaundice) Ø Cause: 1. Pre-hepatic: excessive formation of bilirubin by increased degradation of erythrocytes (icterus neonatus, hemolytic anemia) 2. Hepatic: insufficient processing of bilirubin as a result of liver defects (hepatitis, liver toxic damage, cirrhosis, hepatic failure) 3. Post-hepatic: by impaired excretion of gall (obstructive jaundice due to gallstones, inflammation of biliary tract) Ø Unconjugated bilirubin can cross the blood-brain barrier, leading to brain damage Ø Jaundice in neonates (increased bilirubin degradation+immaturity of the conjugation enzymes): phototerapy – isomerization of bilirubin to more soluble pigments
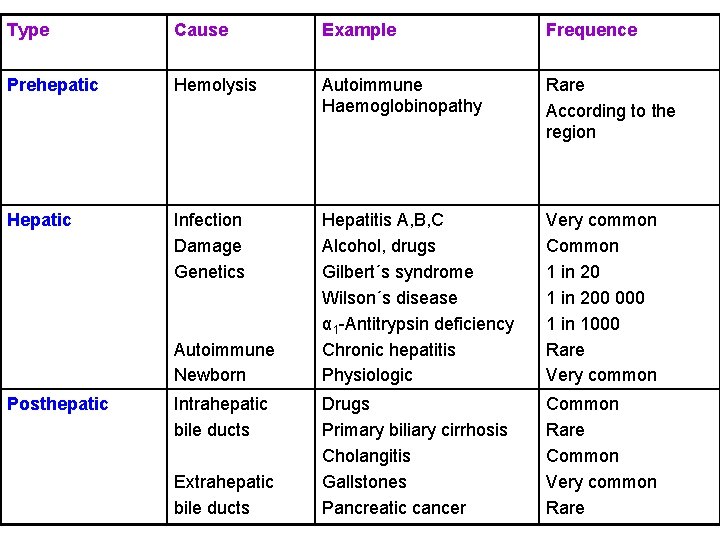
Type Cause Example Frequence Prehepatic Hemolysis Autoimmune Haemoglobinopathy Rare According to the region Hepatic Infection Damage Genetics Hepatitis A, B, C Alcohol, drugs Gilbert´s syndrome Wilson´s disease α 1 -Antitrypsin deficiency Chronic hepatitis Physiologic Very common Common 1 in 200 000 1 in 1000 Rare Very common Drugs Primary biliary cirrhosis Cholangitis Gallstones Pancreatic cancer Common Rare Common Very common Rare Autoimmune Newborn Posthepatic Intrahepatic bile ducts Extrahepatic bile ducts
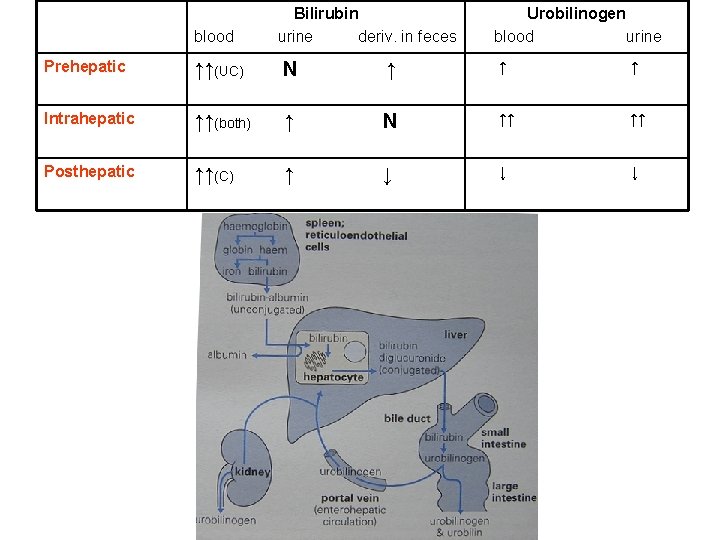
blood Bilirubin urine deriv. in feces Urobilinogen blood urine Prehepatic ↑↑(UC) N ↑ ↑ ↑ Intrahepatic ↑↑(both) ↑ N ↑↑ ↑↑ Posthepatic ↑↑(C) ↑ ↓ ↓ ↓

Summary: Synthesis of heme: Ø from glycine and succinate Ø induction by drugs and ↓ glucose; inhibition by lead Ø intermediates → porphyrinogens (porphyrins) Ø porphyrias Degradation of heme Ø to bilirubin (hydrophobic) Ø conjugation in liver Ø conversion to urobilinogen in intestine Ø hyperbilirubinemia (differential diagnosis)

Pictures used in the presentation: Marks´ Basic Medical Biochemistry, A Clinical Approach, third edition, 2009 (M. Lieberman, A. D. Marks) Principles of Biochemistry, 2008, (Voet D, Voet J. G. , and Pratt C. W)
- Slides: 14