META PHI in Primary Care Implementing Best Practices

META: PHI in Primary Care: Implementing Best Practices for Addictions Managing Opioid Use Disorders in Chronic Pain Patients

What is META: PHI? • Mentoring, Education, and Clinical Tools for Addiction: Primary Care–Hospital Integration • Collaborative project to implement integrated care pathways for addiction throughout Ontario • Partnership between hospitals, withdrawal management services, FHTs, CHCs, and community agencies • Goals: 1. Improve care for patients with addictions 2. Improve care provider experience 3. Improve population health 4. Reduce service use 5. Provide sustainable care 2

How it works • Patients presenting with addiction-related concerns receive evidence-based interventions and are referred to rapid access addiction medicine (RAAM) clinics for treatment • RAAM clinics offer substance use disorder treatment on walk -in basis; no formal referral/appointment needed • Patients stabilized at RAAM clinic referred back to primary care for long-term addiction treatment (with ongoing support from RAAM clinic as required) • Key components: • Integration of care at hospital, RAAM clinic, primary care • Training, support, and mentorship from addictions specialists • Capacity-building 3

Role of PCPs With support from META: PHI team: • Follow best practices for prescribing opioids • Screen and diagnose patients for substance use disorders • Refer patients to treatment at RAAM clinic when necessary • Take over long-term addiction care for patients (with ongoing support from RAAM clinic doctor) 4

IDENTIFYING AND DIAGNOSING OPIOID USE DISORDER (OUD) 5

OUD in patients • OUD can occur as a complication of opioid therapy • All patients on opioid therapy for chronic pain should be regularly monitored for signs of OUD • Risk factors • < 40 years old • Male • Concurrent substance use disorder (alcohol, benzodiazepines, etc. ) • Active mental illness (depression, anxiety, PTSD, etc. ) 6

OUD DSM-V criteria (1) Impaired control: • Opioids taken in larger amounts or for a longer period than intended • There is a persistent desire or unsuccessful efforts to cut down or control opioid use • A great deal of time is spent obtaining or using opioids, or recovering from their effects • There are cravings or a strong desire to use opioids 7

OUD DSM-V criteria (2) Social impairment: • There is recurrent opioid use resulting in a failure to fulfill important role obligations at work, school, or home • There is continued use despite persistent or recurrent social or interpersonal problems caused or exacerbated by the effects of opioids • Important social, occupational, or recreational activities are given up or reduced because of opioid use 8

OUD DSM-V criteria (3) Risky use: • There is recurrent opioid use in situations where it is physically hazardous • Continued use despite knowledge of having a persistent or recurrent physical or psychological problem that is caused or exacerbated by opioids 9

OUD DSM-V criteria (4) Physiological dependence: • Tolerance: There is either a need for markedly increased amounts of opioids to achieve intoxication or desired effect or there is a markedly diminished effect with continued use of the same amount of opioids • Withdrawal: There is either characteristic withdrawal syndrome for opioids are taken to relieve or avoid withdrawal symptoms 10

Clinical features of OUD in patients • High opioid dose for underlying condition • Aberrant behaviours: Running out early, crushing/biting oral tabs, accessing opioids from other sources • Strong resistance to switching or tapering • Importance attached to drug outweighs analgesic benefit (e. g. , “Pain is 10/10, medication only takes edge off, but I would die if you stopped it”) • Binge rather than scheduled use • Deteriorating mood and functioning • Concerns expressed by friends/family • Reports recurrent, frightening withdrawal symptoms • May acknowledge immediate mood improvement after dose 11

Presenting a diagnosis • Be clear and non-judgmental • Inform patient that their opioid use is harming them and that treatment will improve their pain, mood, and functioning • Do not abruptly stop opioid prescribing • This puts patient at increased risk of overdose death • Give patient harm reduction advice • Offer treatment 12

OUD TREATMENT OPTIONS 13

Treatment options 1. Abstinence-based treatment 2. Structured opioid therapy 3. Opioid maintenance therapy 14

Abstinence-based psychosocial treatment • Treatment goal: Cessation of all opioids (sometimes including opioid agonist treatment) • Advantages • Often preferred by patients to long-term opioid agonist treatment • Often provides participants with a sense of community • Gives structure to participants’ lives • Disadvantages • Does not provide physical relief from withdrawal symptoms/cravings, which can last for weeks or months • Increased risk of relapse and opioid overdose; patients should be given harm reduction advice 15

Harm reduction advice (1) • Never use opioids alone • Make sure you and your friends know the signs of overdose (pinpoint pupils, falling asleep, slowed/stopped breathing, bluish skin around lips or under nails) • Always carry naloxone • If a friend has overdosed: • Shake them and call their name • Call 911 • Administer naloxone and start chest compressions • If you are taking opioids after a period of abstinence (even a few days), take a much smaller dose than you used to 16

Harm reduction advice (2) • Only medications obtained from a prescription and purchased at a pharmacy are guaranteed to be what they are supposed to be • Many opioids (and other drugs, such as cocaine) are laced with fentanyl • Fentanyl is very potent and can be lethal even in tiny amounts • Do not inject opioids • Do not mix opioids with other substances, especially alcohol or benzodiazepines 17

Structured opioid therapy (1) • Opioid prescribing under conditions that limit misuse • Indications • Has or is at high risk for OUD • Has pain condition requiring opioid therapy • Only uses opioids supplied by one prescriber • Does not alter route of delivery (inject/crush oral tabs) • Is not currently addicted to alcohol or other drugs 18

Structured opioid therapy (2) • Protocol • Taper dose: • Typically 10% of total daily dose at each visit, no more than 10% of total daily dose every 1– 2 weeks • Taper more slowly when 1/3 of total dose is reached • Dispense small amounts frequently • Do not refill if patient runs out early • Monitor with office visits, pill counts, urine drug screens • Switch to opioid maintenance therapy if structured opioid therapy fails (i. e. , patient continues to use more than prescribed) 19

Opioid agonist therapy (1) • Substitution of illegal and/or euphoria-inducing opioid with longer-acting, less euphoric opioid • Relieves withdrawal symptoms/cravings for 24 hours • Indications • Has OUD • Failed at/not a candidate for opioid tapering • Acquires opioids from multiple sources (e. g. , other doctors, friends/relatives, the street) • Alters route of delivery (inject/crush oral tabs) • Current risky use of alcohol or other drugs 20

Opioid maintenance therapy (2) • Maintenance therapy has historically used methadone • Full, potent opioid agonist • Risk of sedation/overdose • Requires a federal exemption to prescribe • Another option is buprenorphine • Partial opioid agonist with a ceiling effect • Even very high doses rarely cause respiratory depression (unless combined with alcohol/sedatives) • Binds tightly to receptors, displacing other opioids • Usually combined 4: 1 with naloxone as abuse deterrent • Can be prescribed by any doctor in Ontario 21

PRESCRIBING BUPRENORPHINE 22

Why prescribe buprenorphine? (1) • Attending a methadone clinic is not always possible: • Patient reluctance • No local clinic • Long waiting list • Larger methadone clinics sometimes have rigid rules (e. g. , frequent urine drug screens) and often do not provide counselling or primary care • Evidence has demonstrated that buprenorphine in primary care settings is as effective as in specialized settings • Patients often prefer receiving buprenorphine from their PCP: • Less stigmatizing • Patient has close relationship with PCP 23

Why prescribe buprenorphine? (2) • Prescribing buprenorphine to a patient with OUD is much more satisfying than prescribing opioids: • Patients usually feel and function better • Behaviours associated with OUD (running out early, missed appointments, drug seeking, etc. ) usually resolve • Patients usually very grateful for PCP’s role in their recovery 24

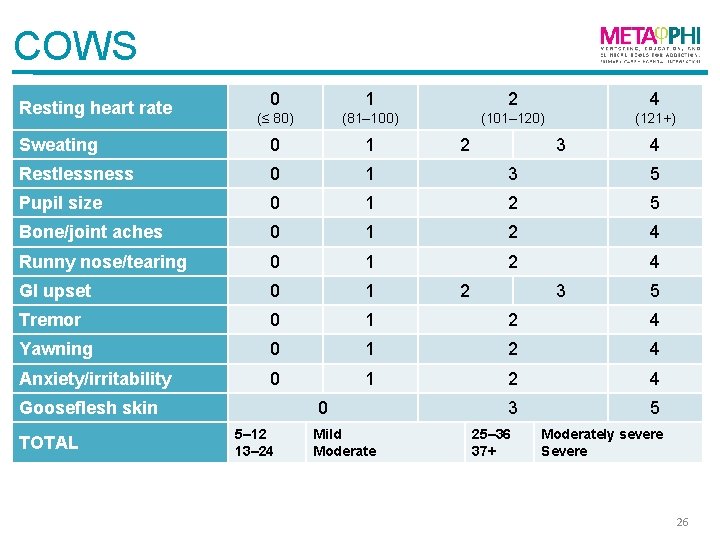
Initiation • Biggest risk of initiation is precipitated withdrawal • Buprenorphine displaces currently attached opioids • Causes rapid onset of intense withdrawal • Not medically dangerous but can deter patients from treatment • Before first dose, patient should have no opioid in serum and be in moderate withdrawal • Measure withdrawal using Clinical Opioid Withdrawal Scale (COWS) 25
COWS 0 1 2 4 (≤ 80) (81– 100) (101– 120) (121+) Sweating 0 1 Restlessness 0 1 3 5 Pupil size 0 1 2 5 Bone/joint aches 0 1 2 4 Runny nose/tearing 0 1 2 4 GI upset 0 1 Tremor 0 1 2 4 Yawning 0 1 2 4 Anxiety/irritability 0 1 2 4 3 5 Resting heart rate Gooseflesh skin TOTAL 0 5– 12 13– 24 Mild Moderate 2 3 25– 36 37+ 4 5 Moderately severe Severe 26

Initiation protocol (1) • • • At least 12 hours since last oral dose Patient reports typical withdrawal symptoms COWS score 12+ First dose: 4 mg SL (takes several minutes to dissolve) Reassess in 2 hours • If patient improved but still in withdrawal, give another 4 mg to take in office or at home • Maximum dose first day: 12 mg 27

Initiation protocol (2) • Office induction is preferred to ensure patient does not go into precipitated withdrawal • If patient cannot attend for office induction, write prescription (2 mg SL q 4 H PRN, up to 6 tabs over 24 hours, x 1– 3 days) and give patient clear instructions: • Wait at least 12– 16 hours since your last opioid use • Make sure your COWS score is at least 12 (give scale) • Put 2 tablets under your tongue and let them dissolve • Wait 2 hours and measure your COWS score again • If still in withdrawal, take another 2 tablets • Do not take more than 6 tablets (12 mg) in first 24 hours • Next day: Take total first-day amount as single dose 28

Titration • Reassess in 1– 3 days • Increase dose by 2– 4 mg at each visit if patients reports withdrawal symptoms/cravings near end of dosing interval • Optimal dose should relieve withdrawal symptoms/cravings for 24 hours without significant sedation or other side effects • Optimal maintenance dose: 8– 16 mg SL OD • Maximum maintenance dose: 24 mg SL OD • Arrange frequent office visits for counselling and urine drug screen monitoring • Screen for presence of norbuprenorphine/absence of other opioid metabolites 24 h 29

Dispensing • If possible, buprenorphine should initially be dispensed daily and taken under pharmacist’s observation • Especially important if patient has been accessing opioids from other sources • Take-doses should be prescribed when patient is at optimal dose and has stopped unauthorized use • Consider early take-home doses if patient… • Acquires opioids only from physician • Does not inject or crush oral opioid tablets • Does not buy, sell, or use illicit drugs 30

Prescriptions Specify pharmacy and send by fax Specify observed and take-home doses 31

At each office visit • Ask about withdrawal symptoms or cravings • Sometimes minor dose adjustments required (2– 4 mg) • Perform urine drug screens • Ask about alcohol and cannabis use (usually not tested on urine drug screen) • Ask about overall mood and functioning • Manage chronic medical conditions (e. g. , hepatitis C) or psychiatric conditions (e. g. , anxiety, depression) • Perform regular screening and health maintenance (e. g. , pap tests, mammograms, immunizations, etc. ) 32

Buprenorphine failures • Buprenorphine is effective for many patients • However, in some cases, it does not fully relieve withdrawal symptoms or suppress opioid use • If patient continues to experience withdrawal symptoms/ cravings or use illicit opioids despite an adequate dose of buprenorphine, refer to a methadone clinic that provides high -quality care 33

Tapering buprenorphine • Indications • Wants to taper • At least six months without any substance use • Socially stable, supportive family or social network • Stable mood, good coping strategies • Protocol • Decrease by small amounts (1– 2 mg) • Leave at least two weeks between dose decreases • Hold taper at patient’s request • Return to original dose if opioid use restarts • Provide regular support and encouragement: it is not a “failure” if taper has to be held/reversed 34

WRAP-UP: KEY MESSAGES 35

Our responsibility • Treating addicted patients is our responsibility as health care providers • Addiction can occur as a complication of opioid therapy • Addiction is the same as any other chronic illness: patients need specialist referrals, medication, treatment of co-occurring conditions, and regular follow-up • Effective addiction treatments are available • Purpose of META: PHI project is to facilitate adoption of best practices and support clinicians 36

Resources • META: PHI website: www. metaphi. ca • META: PHI mailing list for clinical questions and discussion (e -mail sarah. clarke@wchospital. ca to join) • META: PHI contacts: Medical lead: Dr. Meldon Kahan Manager: Kate Hardy Knowledge broker: Sarah Clarke meldon. kahan@wchospital. ca kate. hardy@wchospital. ca sarah. clarke@wchospital. ca 37
- Slides: 37