META PHI in Primary Care Implementing Best Practices

META: PHI in Primary Care: Implementing Best Practices for Addictions Managing Problematic Alcohol Use

What is META: PHI? • Mentoring, Education, and Clinical Tools for Addiction: Primary Care–Hospital Integration • Collaborative project to implement integrated care pathways for addiction throughout Ontario • Partnership between hospitals, withdrawal management services, FHTs, CHCs, and community agencies • Goals: 1. Improve care for patients with addictions 2. Improve care provider experience 3. Improve population health 4. Reduce service use 5. Provide sustainable care 2

How it works • Patients presenting with addiction-related concerns receive evidence-based interventions and are referred to rapid access addiction medicine (RAAM) clinics for treatment • RAAM clinics offer substance use disorder treatment on walk -in basis; no formal referral/appointment needed • Patients stabilized at RAAM clinic referred back to primary care for long-term addiction treatment (with ongoing support from RAAM clinic as required) • Key components: • Integration of care at hospital, RAAM clinic, primary care • Training, support, and mentorship from addictions specialists • Capacity-building 3

Role of PCP With support from META: PHI team: • Follow best practices for prescribing opioids • Screen and diagnose patients for substance use disorders • Refer patients to treatment at RAAM clinic when necessary • Take over long-term addiction care for patients (with ongoing support from RAAM clinic doctor) 4

PRACTICE GOALS FOR MANAGING PATIENTS’ ALCOHOL USE 5

Practice goals 1. Screen all patients for problematic alcohol use at least once per year 2. Screen patients who present with medical or psychosocial problems that could be connected to problematic alcohol use 3. Diagnose patients with at-risk drinking or alcohol use disorder (AUD) 4. Offer brief advice for patients with at-risk drinking 5. Offer patients with AUD appropriate counselling, pharmacotherapy, and referral 6

CATEGORIES OF ALCOHOL USE 7

Alcohol use categories • Abstinence: Patient does not drink alcohol • Low-risk drinking: Patient drinks within low-risk guidelines • At-risk drinking: Patient drinks in excess of the low-risk guidelines but experiences minimal adverse effects • Alcohol use disorder (AUD): Patient meets DSM-V criteria • 2– 3 = mild AUD • 4– 5 = moderate AUD • 6+ = severe AUD 8

Canadian low-risk drinking guidelines Canadian Centre on Substance Use and Addiction, 2013 9
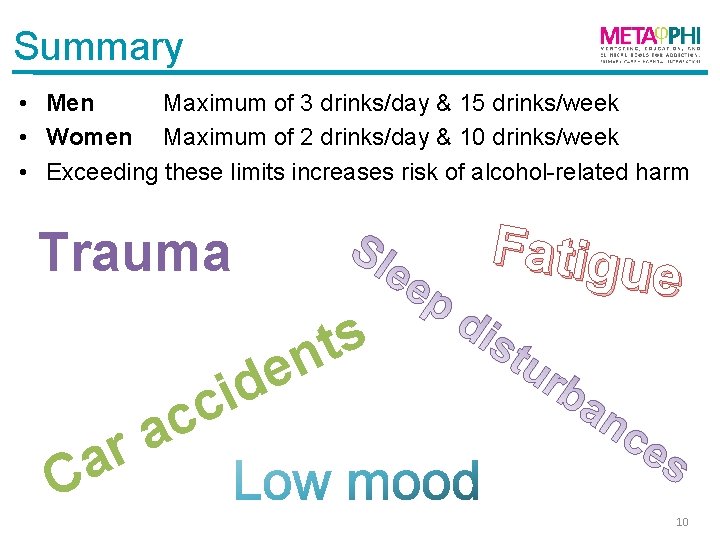
Summary • Men Maximum of 3 drinks/day & 15 drinks/week • Women Maximum of 2 drinks/day & 10 drinks/week • Exceeding these limits increases risk of alcohol-related harm Fatigu e Trauma s t n e id c c ra a C 10

AUD DSM-V criteria (1) Impaired control: • Alcohol is taken in larger amounts or for a longer period than intended • There is a persistent desire or unsuccessful efforts to cut down or control alcohol use • A great deal of time is spent in activities necessary to obtain alcohol, use alcohol, or control alcohol use • There are cravings or a strong desire to use alcohol 11

AUD DSM-V criteria (2) Social impairment: • There is recurrent alcohol use resulting in a failure to fulfill important role obligations at work, school, or home • There is continued use despite persistent or recurrent social or interpersonal problems caused or exacerbated by the effects of alcohol • Important social, occupational, or recreational activities are given up or reduced because of alcohol use 12

AUD DSM-V criteria (3) Risky use: • There is recurrent alcohol use in situations where it is physically hazardous • Alcohol use is continued despite knowledge of having a persistent or recurrent physical or psychological problem that is caused or exacerbated by alcohol 13

AUD DSM-V criteria (4) Physiological dependence: • Tolerance: There is either a need for markedly increased amounts of alcohol to achieve intoxication or desired effect or there is a markedly diminished effect with continued use of the same amount of alcohol • Withdrawal: There is either characteristic withdrawal syndrome for alcohol is taken to relieve or avoid withdrawal symptoms 14

SCREENING FOR PROBLEMATIC ALCOHOL USE 15

Single-item screening test “How many times in the past year have you had 5 (men)/4 (women) drinks in one day? ” • Positive screen is once or more 16

Alcohol history • Take an alcohol history for patients with a positive screen • Helps determine between at-risk drinking and AUD • Can track changes in patients’ consumption patterns • Ask patients for daily or weekly amount • “Would you say your drinking is closer to 14 drinks a week or 30 drinks a week? ” • “What is the most you would have in one day? ” • “How many bottles of wine/liquor do you consume in a week? What size bottles do you most often buy? ” • Convert responses to standard drinks: 12 oz. beer bottle, 5 oz. glass of wine, 1½ oz. liquor 17
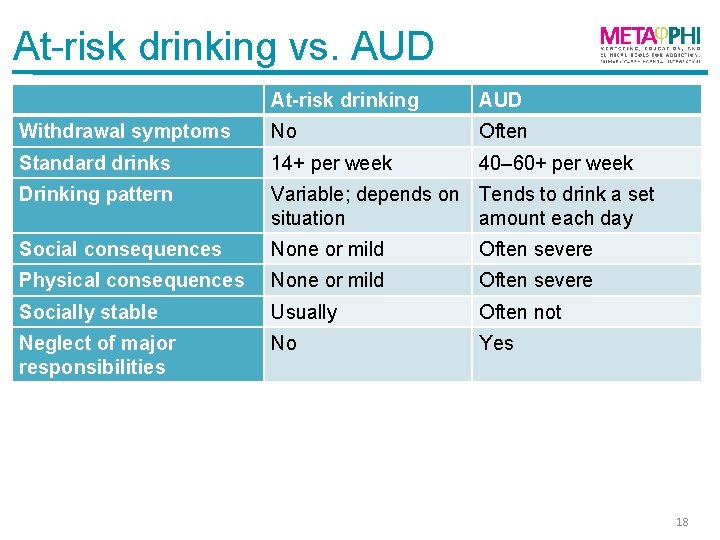
At-risk drinking vs. AUD At-risk drinking AUD Withdrawal symptoms No Often Standard drinks 14+ per week 40– 60+ per week Drinking pattern Variable; depends on Tends to drink a set situation amount each day Social consequences None or mild Often severe Physical consequences None or mild Often severe Socially stable Usually Often not Neglect of major responsibilities No Yes 18

MANAGING AT-RISK DRINKING 19

Inform • Review low-risk drinking guidelines • Link drinking with health status, mood, sleep, and energy • Review precautions and contraindications to alcohol consumption • Pregnancy, active peptic ulcer disease or gastritis, cirrhosis, alcohol or viral hepatitis, pancreatitis • Potential adverse effects of alcohol use if patient has diabetes, bleeding disorders, or seizure disorders • Potential adverse effects of alcohol use if patient is taking antidepressants, ASA, NSAIDs, opioids, benzodiazepines and other sedating drugs 20

Assess • Assess patient’s state of change: • “Are you willing to commit to cutting down on your drinking in the next month? ” • Not ready to change: Restate concern, encourage reflection, motivation, address barriers, reaffirm willingness to help • Ready to change: Help set goals, agree to plan, educational materials, community resources, medications, follow-up 21

Create plan (1) • Help patient set drinking goal: amount per occasion, frequency, and circumstances • Strategies to reduce consumption: • Drink no more than one standard drink per hour • Start drinking later in the evening • Sip drinks, don't gulp • Avoid drinking on an empty stomach • Dilute drinks with mixer • Alternate alcoholic with non-alcoholic drinks • 20 -minute pause between the decision to drink and drinking 22

Create plan (2) • Ask patient to keep a daily drinking diary • Order GGT and MCV • Elevated test results can motivate patient to change • Changes can be tracked over time • Arrange regular follow-up • Ask about changes in consumption • Ask about changes in health status, mood, energy, etc. • Note successes • Address challenges • Keep patient engaged • If problem persists or worsens, consider more intensive treatment 23

MANAGING ALCOHOL USE DISORDERS 24

Present diagnosis (1) • Be clear but sensitive: • “I’m concerned about your use of alcohol. It is above the levels recommended by the low-risk drinking guidelines and appears to be causing you harm. ” • “Based on my assessment, you have an alcohol use disorder. ” • “Alcohol use disorders can be caused by many things, such as trauma (both in childhood and as an adult), genetics, mental health problems, and life stressors such as the end of a relationship or loss of a job. ” • “An alcohol use disorder is a chronic illness; it doesn’t mean that you’re weak, or that you’re not a good person. ” 25

Present diagnosis (2) • Offer help: • “I know it can be very difficult to change your drinking patterns, but I can offer you some treatments that can help you (medications, counselling), and I can help connect you to treatment programs, counseling, or support groups. ” • “Within days or weeks of abstinence, most people have improved sleep, mood, and energy levels. ” • “This is a treatable condition. If you’re not ready to change right now, we can discuss it again at your next visit. ” 26

Assess • Assess patient’s state of change: • “Are you willing to commit to cutting down on or stopping your drinking in the next month? ” • Not ready to change: Restate concern, encourage reflection, motivation, address barriers, reaffirm willingness to help • Ready to change: Negotiate written goal Treatment Agreement • Abstinence is more likely to be Goal: Abstinence Date: April 15 successful Plan: • If reduced drinking goal is chosen, encourage a time-limited trial 27

Treatment protocol (1) • Treat withdrawal if necessary • Treat concurrent conditions (anxiety, depression, hypertension, liver disease) • Prescribe anti-craving medication • Encourage patient to make healthy lifestyle choices: • Stay away from people/places associated with drinking • Spend time with supportive family and friends • Take daily walks • Maintain regular sleeping/waking schedule • Plan regular activities outside the house as feasible 28

Treatment protocol (2) • Review options formal treatment (residential, day, outpatient) • Recommend AA or other community groups for support, practical advice, and a way to overcome loneliness and boredom • Arrange follow-up; monitor drinking through self-report, GGT, MCV • Acknowledge successes, even if partial or temporary • If patient relapses, encourage contact and reconnection with treatment 29

MANAGING ALCOHOL WITHDRAWAL 30

Indications for office withdrawal • Patient reports frequent withdrawal symptoms (tremor, sweating, vomiting, anxiety, tachycardia, hypertension) • Patient is committed to abstinence and willing to start psychosocial treatment and/or pharmacotherapy • Patient has no history of seizures, DTs, or ED visits/ hospitalizations due to withdrawal • Patient is not on high doses of opioids or sedating medications • Patient does not have cirrhosis with liver dysfunction • Patient has supports at home 31

Protocol (1) • Advise patient to have their last drink the night before the morning appointment • If patient shows up intoxicated, reschedule and/or refer to a withdrawal management centre (if available) • Administer Clinical Institute Withdrawal Assessment for Alcohol, revised (CIWA-Ar) scale q 1– 2 H • Dispense diazepam 10– 20 mg (or lorazepam 2– 4 mg) for CIWA-Ar ≥ 10 • Treatment is complete when CIWA-Ar < 8 on two consecutive occasions • Ensure patient has minimal or no tremor 32

Protocol (2) • Send patient to emergency department if: • Worsening/no improvement despite 3– 4 doses • Patient displays marked tremor/vomiting/sweating or agitation/confusion • Risk factors for electrolyte imbalance or arrhythmias (e. g. , diuretics, heart disease, diabetes) • Prior to discharge: • Initiate anti-alcohol medication • Advise patient to attend AA or another community service • Schedule follow-up (within 1– 2 days if lorazepam used) • Ensure patient leaves accompanied by friend or relative 33

Indications for home withdrawal • Office management not feasible • A partner, relative, or friend agrees to dispense medication • Patient has no history of seizures, DTs, or ED visits/ hospitalizations due to withdrawal • Patient has treatment plan in place (anti-alcohol medication, ongoing counselling, psychosocial program, etc. ) • Age < 65 • No hepatic decompensation (ascites, encephalopathy) • Patient agrees not to drink while taking medication 34

Protocol • Instruct patient to have last drink the night before • Instruct patient to take diazepam 10 mg every 4 hours as needed for tremor (dispensed by partner, relative, or friend) • Prescribe no more than 60 mg diazepam • Reassess the next day (by phone or in person) • Clinic visit within 2– 3 days 35
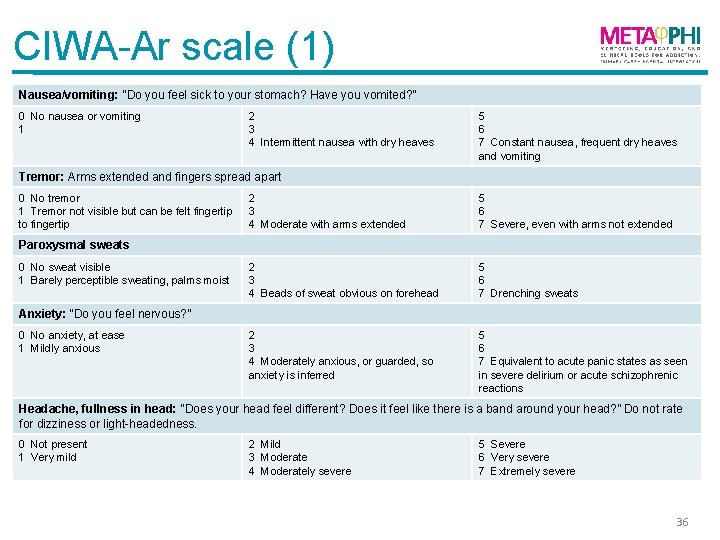
CIWA-Ar scale (1) Nausea/vomiting: “Do you feel sick to your stomach? Have you vomited? ” 0 No nausea or vomiting 1 2 3 4 Intermittent nausea with dry heaves 5 6 7 Constant nausea, frequent dry heaves and vomiting Tremor: Arms extended and fingers spread apart 0 No tremor 1 Tremor not visible but can be felt fingertip to fingertip 2 3 4 Moderate with arms extended 5 6 7 Severe, even with arms not extended 2 3 4 Beads of sweat obvious on forehead 5 6 7 Drenching sweats 2 3 4 Moderately anxious, or guarded, so anxiety is inferred 5 6 7 Equivalent to acute panic states as seen in severe delirium or acute schizophrenic reactions Paroxysmal sweats 0 No sweat visible 1 Barely perceptible sweating, palms moist Anxiety: “Do you feel nervous? ” 0 No anxiety, at ease 1 Mildly anxious Headache, fullness in head: “Does your head feel different? Does it feel like there is a band around your head? ” Do not rate for dizziness or light-headedness. 0 Not present 1 Very mild 2 Mild 3 Moderate 4 Moderately severe 5 Severe 6 Very severe 7 Extremely severe 36
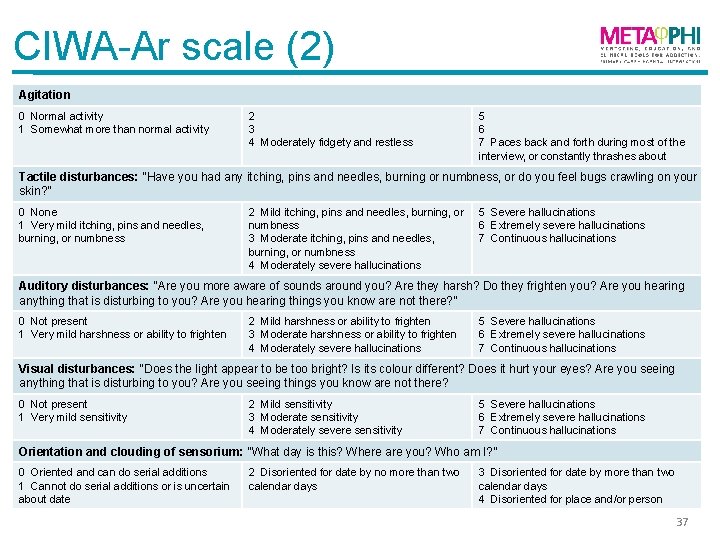
CIWA-Ar scale (2) Agitation 0 Normal activity 1 Somewhat more than normal activity 2 3 4 Moderately fidgety and restless 5 6 7 Paces back and forth during most of the interview, or constantly thrashes about Tactile disturbances: “Have you had any itching, pins and needles, burning or numbness, or do you feel bugs crawling on your skin? ” 0 None 1 Very mild itching, pins and needles, burning, or numbness 2 Mild itching, pins and needles, burning, or numbness 3 Moderate itching, pins and needles, burning, or numbness 4 Moderately severe hallucinations 5 Severe hallucinations 6 Extremely severe hallucinations 7 Continuous hallucinations Auditory disturbances: “Are you more aware of sounds around you? Are they harsh? Do they frighten you? Are you hearing anything that is disturbing to you? Are you hearing things you know are not there? ” 0 Not present 1 Very mild harshness or ability to frighten 2 Mild harshness or ability to frighten 3 Moderate harshness or ability to frighten 4 Moderately severe hallucinations 5 Severe hallucinations 6 Extremely severe hallucinations 7 Continuous hallucinations Visual disturbances: “Does the light appear to be too bright? Is its colour different? Does it hurt your eyes? Are you seeing anything that is disturbing to you? Are you seeing things you know are not there? 0 Not present 1 Very mild sensitivity 2 Mild sensitivity 3 Moderate sensitivity 4 Moderately severe sensitivity 5 Severe hallucinations 6 Extremely severe hallucinations 7 Continuous hallucinations Orientation and clouding of sensorium: “What day is this? Where are you? Who am I? ” 0 Oriented and can do serial additions 1 Cannot do serial additions or is uncertain about date 2 Disoriented for date by no more than two calendar days 3 Disoriented for date by more than two calendar days 4 Disoriented for place and/or person 37

PRESCRIBING ANTI-CRAVING MEDICATIONS 38

Role of anti-craving medications • Should be routinely offered to patients with AUD • Shown to reduce alcohol use • Good safety profiles • Help retain patients in treatment • Choice of medication depends on individual considerations (e. g. , cost, side effects) • Titrate dose until cravings are mild and patient is abstinent, or until troublesome side effects emerge • Maintain until patient has been abstinent for at least several months, has minimal cravings, has social supports and new ways of coping with stress, and is confident that medication is no longer needed to prevent relapse • Usually at least 6 months 39

Medication availability • Front-line medications naltrexone and acamprosate covered under ODB formulary with LU codes: • Naltrexone: LU 532 “For the treatment of AUD in patients who meet clinical criteria for AUD; express a commitment to reduce or abstain from alcohol; and have confirmed participation in counselling and treatment for AUD” • Acamprosate: LU 531 “For the treatment of AUD in patients who meet clinical criteria for AUD; express a commitment to abstain from alcohol; have been abstinent from alcohol for at least 3 days prior to starting acamprosate; and have confirmed participation in counselling and treatment for AUD” • Disulfiram only available in Canada as compounded medication 40
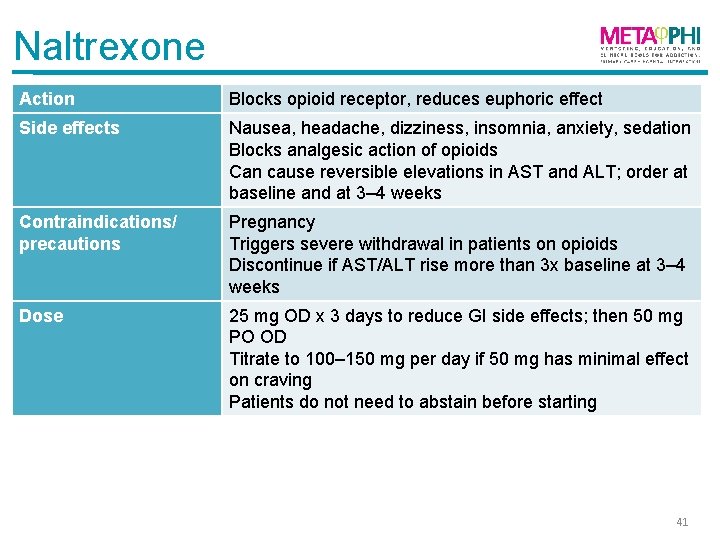
Naltrexone Action Blocks opioid receptor, reduces euphoric effect Side effects Nausea, headache, dizziness, insomnia, anxiety, sedation Blocks analgesic action of opioids Can cause reversible elevations in AST and ALT; order at baseline and at 3– 4 weeks Contraindications/ precautions Pregnancy Triggers severe withdrawal in patients on opioids Discontinue if AST/ALT rise more than 3 x baseline at 3– 4 weeks Dose 25 mg OD x 3 days to reduce GI side effects; then 50 mg PO OD Titrate to 100– 150 mg per day if 50 mg has minimal effect on craving Patients do not need to abstain before starting 41

Acamprosate Action Glutamate antagonist Relieves subacute withdrawal symptoms (insomnia, dysphoria, craving) Side effects Diarrhea Contraindications/ precautions Pregnancy Renal insufficiency Dose 666 mg tid; 333 mg tid if renal impairment or BW < 60 kg Works best if patient is abstinent several days prior to initiation 42

Disulfiram Action Acetaldehyde accumulates when alcohol consumed Most effective when dispensed by family member Side effects With alcohol: Vomiting, flushed face, headache Without alcohol: Headache, anxiety, fatigue, garlic-like taste, acne, peripheral neuropathy (with prolonged use) Contraindications/ precautions Cirrhosis Pregnancy Unstable cardiovascular disease Alcohol reaction cause severe hypotension and arrhythmias, especially in patients with heart disease or on antihypertensives May trigger psychosis at higher doses (500 mg) Can cause toxic hepatitis Dose 125 mg PO OD; increase to 250 mg if patient reports no reaction to alcohol Wait at least 24– 48 hours between last drink and first pill Wait at least 7– 10 days between last pill and first drink 43
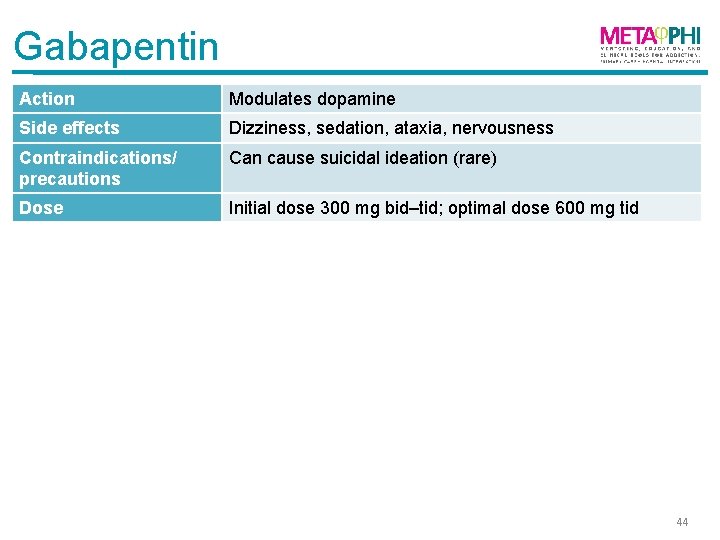
Gabapentin Action Modulates dopamine Side effects Dizziness, sedation, ataxia, nervousness Contraindications/ precautions Can cause suicidal ideation (rare) Dose Initial dose 300 mg bid–tid; optimal dose 600 mg tid 44

Topiramate Action Modulates GABA system May improve sleep/mood disturbance in early abstinence Side effects Sedation, dose-related neurological effects (dizziness, ataxia, speech disorder, etc. ) resolve over time Contraindications/ precautions Can cause weigh loss (risk for underweight patients) Can clause glaucoma or renal stones Dose Initial dose 50 mg OD; titrate by 50 mg to a maximum dose of 200– 300 mg daily Lower dose needed in renal insufficiency 45

Baclofen Action GABA agonist Side effects Drowsiness, weakness, can cause or worsen depression Contraindications/ precautions Use with caution in patients on tricyclic anti-depressants or MAO inhibitors Dose Initial dose 5 mg tid, increase to 10 mg tid; maximum daily dose 80 mg Lower dose needed with renal insufficiency 46

WRAP-UP: KEY MESSAGES 47

Our responsibility • Treating addicted patients is our responsibility as health care providers • Addiction is the same as any other chronic illness: patients need specialist referrals, medication, treatment of co-occurring conditions, and regular follow-up • Effective addiction treatments are available • Purpose of META: PHI project is to facilitate adoption of best practices and support clinicians 48

Resources • META: PHI website: www. metaphi. ca • META: PHI mailing list for clinical questions and discussion (e -mail sarah. clarke@wchospital. ca to join) • META: PHI contacts: Medical lead: Dr. Meldon Kahan Manager: Kate Hardy Knowledge broker: Sarah Clarke meldon. kahan@wchospital. ca kate. hardy@wchospital. ca sarah. clarke@wchospital. ca 49
- Slides: 49