Mental state assessment Dr hab med Wiktor Drzdz

Mental state assessment Dr hab. med. Wiktor Drózdz

Basic contradiction during psychiatric examination need to establish interpersonal relationship with a patient OR need to obtain data necessary for diagnosis and intervention Patients do not always cooperate • Open refusal to comply during examination of mental state • Problem of „shame cooperation”

Mental state examination • Crucial circumstances: – conversation in a quiet room with no other persons – TIME • Format: interview + observation of behavior • Additional information: – Medical documents – General medical examination – Lab tests – Inteview with near relative, friend or somebody who has observed patient (hospital staff)

Five Phases of the Psychiatric Interview • • • Phase 1: Warm-up and Chief Complaint Phase 2: The Diagnostic Decision Loop Phase 3: History and Database Phase 4: Diagnosing and Feedback Phase 5: Treatment Plan and Prognosis

Mental state examination aspects that must be considered 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 13. 14. Reason for examination Current mental health problem and course of the problem Somatic interview Interview toward substance abuse/other forms of addiction Interview concerning past psychosocial development Interview concerning past social functiong Interview concerning past school/occupational functiong Family interview Current general medical sufferings General medical examination Examination of current mental state Current level of functiong in social roles Lab tests performed lately Impressions from the examination

Openers • Opening questions or statements target a problem of varying scope. • Narrow scope: “What troubles bring you here to see me? ” – The interviewer expects a prioritized brief list of difficulties. – Problem: The patient rambles. – Solution: The interviewer narrows the scope of the question or curbs the response. For instance (if patient cooperates): — P: (Responds with a long list of events that went wrong in his or her life). — I: Just tell me what problem has troubled you most during the last 3 days. — P: That I can't sleep. • Broad scope: “Give me a sense of how your life is going. ”

Continuation • The interviewer tends to the patient's talk by raising eyebrows or uttering hmmms to signal to the patient nonverbally to continue. If his or her nonverbal signals get ignored the interviewer may use short tracking phrases, such as • • • “And? ” “Then what? ” “How is that? ” “That's interesting, ” “ “Really? ” “Oh, no!” to reward the patient with his or her attention and to encourage the patient to continue.

Five Ws of interviewing • What? • When? • Where? • Who? • Why?

Cues in psychiatric examination • Verbal – Vocabulary – Fluency? – Narration: structuralised? informative? • Non-verbal – eye contact – facial expression – gesticulation, body language – cadence, intonation – dress code

Methods to gain information 1. 2. 3. 4. Conversation Additional sources of information Application of structuralised tools Application of medical tests: EEG, MRI, urine test for psychoactive compounds, MDD Score(? ) 5. Cooperation with other physicians/health care workers 6. Examination of medicated/intoxicated patient and/or under constraint (i. e. in emergency) 7. General medical examination

Some suggestions concerning interview • Decrease patient’s anxiety, create feeling of comfort • Decrease your own anxiety • Be patient, be commiserate and consolate • Things to be avoided: – Confrontation/argument – Medical jargon, scientific jargon, sophisticated terminology, weird sentences – Jokes (but sense of humour is OK) • Extract the time as much as possible • Learn from patients • Create adequate type of conversation

OCET • • Observation Exploration Conversation Testing

Mental state assessment 1. Appearance, attitude & behavior 2. Cognitive status: awareness, memory, attention, IQ 3. Disorders of perception 4. Thought disorders 5. Obsessions and compulsions 6. Speech disorders 7. Mood, affect and emotions 8. Psychophysiological (vegetative) symptoms 9. Stressful life situations 10. Suicide risk assessment

1. Appearance (O) • • • Well-groomed? dowdy? Reek of sweat? of alcohol? Needle marks? Scars (on forearm, wrist)? Inappropriate attire? Missing eyelashes, eyebrows, hair? Bitten-off nails? Reddened, chapped hands? Excessive piercing or tattoos?

1. Patient attitude • • • Cooperative? Frank? Eye contact: appropriate? Withdrawn? Defensive? Anxious? Hostile? Angry? Too friendly? Evasive? Suspicious? Distrustful? Seductive? Claim? Apathetic?

1. Insight & criticism • Slight awareness? • Blames others? • Complete denial? Level of cooperation: » Withdrawn? » Guarded? » Passive? » Acting Out? » Oppositional? » Hostile?

1. Insight & criticism • awareness of morbid change in oneself and a correct attitude to this change including a realization that it indicates for a mental disorder – Is the patient aware of phenomena that others have observed? – If so, does he recognize the phenomena as abnormal? – If so, does he/she consider that they are caused by mental illness? – If so, does he/she think that treatment is needed? • degree of insight indicates whether a patient is likely to comply with treatment.

1. Insight & criticism • ANOSOGNOSIA present in: – Psychosis – Dementia – Mania – Dependence – Anorexia

1. Motor activity • Slowed • Restless • Agitated

1. Psychomotor disturbances (O, C, T) • • • Rigidity Tremor Tics (motor, vocal) Restless fidgeting, mannerisms Choreatic, athetotic movements Buccolingual movements Catalepsy Opposing movements Echopraxia • Pseudoaphonia, pseudoparalysis, pseudoseizures • Avoidance of touching • Apraxia • Seizures • Cataplexy • Micrographia • Stereotypical movements • Picking

1. Dangerous? • DANGER TO OTHERS: – – – Violent temper Threatens others Physical abuser Hostile Assaultive Homicidal ideation, homicidal threats, homicide attempt • DANGER TO SELF: – Self-injury – Self-mutilation

2. Consciousness (O, T) • Consciousness - awareness of the self and the environment. Orientation: – personal – external (time, place, situation) • Hyperalertness? • Lethargy? Stupor? Coma?

2. Confusion & delirium • Confusion- an inability to think clearly. It occurs in states of impaired consciousness but may occur when consciousness is normal. • Clouding of conciousness? • Delirium? • Confused: periodically? permanently?

2. Stupor • the patient is immobile, mute, and unresponsive but appears to be fully conscious (eyes are usually open and follow external objects), reflexes are also normal and resting posture is maintained

2. Memory • Immediate memory - the retention of information over a short period measured in minutes. • Recent memory - events that took place in last few days. • Long term memory - events over longer periods of time. • Ecmnesia? • Hypermnesia? • Confabulation- reporting memories as current events, or fulfilling memory gaps with description of events that never took place. It is characteristic for amnestic syndrome. • Criticism toward memory dysfunctions preserved?

2. Attention Concentration: ability to focus the attention • Impaired concentration may be present in a wide variety of psychiatric disorders i. e. depression, mania, anxiety, schizophrenia and delirium • It is crucial symptom of ADHD

2. Cognitive functions assessment • Digit Span (forward and reverse): – “I will recite a series of numbers to you, and then I will ask you to repeat them to me, first forward and then backwards. ” [Begin with 3 numbers – not consecutive numbers, and advance to 7 -8 numbered sequence. ] • Spelling Backwards: – “Spell the word ‘world. ’ Now spell the word ‘world’ backwards. ” • Calculations: – (Serial 7’s) “Starting with 100, subtract 7 from 100, and then keep subtracting 7 from that number as far as you can go. ” – (Serial 3’s) “Starting with 20, subtract 3 from 20, and then keep subtracting 3 from that number as far as you can go. ” [Monitor for speed, accuracy, effort required, and monitor patient reactions to the request] – “Add these numbers: (15 + 12 + 7)” – “Multiply these numbers: (25 x 6)”

2. IQ • Approximate assessment of intellect important in patients with intellectual disability – Mild – Moderate – Severe

3. Disorders of perception • Illusions: perception of a real object or event, which is misinterpreted. May be present in delirium • Hallucinations: sensory perceptions occuring without external stimuli – Auditory, visual, tactile, olfactory, gustatory – Complexity: elementary or complex – Pseudohallucitations: identified in patient’s psychic space. Real hallucinations: identified in external space

3. Disorders of perception • The most common hallucination are auditory hallucinations, usually in the form of voices. • Voices talking to each other about the patient, and voices commenting about the patient‘s ongoing acting or thinking, are considered to be typical to schizophrenia (third-person hallucination). • Voices which anticipate, speak or repeat (echo of thoughts) the patient’s thoughts also suggest schizophrenia.

3. Disorders of perception- examples • „I can see a snake in the corner”- in fact it is a length of rope. Illusion • „I can hear some people talking with each other about my very private affairs just outside of the room” – other people in the same room hear nothing. Auditory hallucination (third-person)

4. Thinking (C, E, T) • Linear, logical? • Goal-directed?

4. Thought disorders • PACING: – increased? decreased? • CONTENT: • FORM: – Coherent thinking? – Incoherent? loosening of associations, lack of consistency, chaotic

4. Thought disorders • Disorders of content of thinking (adequacy): delusion- a belief that is firmly held on inadequate grounds, it could not be affected by rational argument or evidence to the contrary, and is not a conventional belief that the person might be expected to hold given his/her educational, cultural and religious background. Briefly- a false unshakable belief hold against the evidence

4. Thought disorders • Delusional mood is preceding unclear conviction that some as yet unidentified change or event is about to take place, then the delusion follows, and the delusion is perceived like explaining of this mood. • Delusional perception is the attaching the new significance to a familiar percept without any rational reason. • Delusional memory is a delusional interpretation attached to past event.

4. Thought disorders: types of delusions • • Paranoid (bizarre) Affective (mood congruent & coherent) persecutory delusion of reference delusion of control thoughts insertion thoughts withdrawal thoughts broadcasting delusions of marital infidelity • Depressive: guilt, punishment, catastrophic, hypochondric, • Maniacal: grandiosity, charismatic, exceptional abilities/features

4. Thought disorders: paranoid • The most common theme of delusion is persecution – The patient believes/is sure that some persons or organizations are trying to inflict harm on the patient, damage his/her reputation, or make him/her insane.

4. Thought disorders: paranoid • Delusion of reference – the unwarranted idea based upon a trivial occurrence (e. g. the person at the next table looked at the patient) that a person is talking about you, watching you, or noticing you (the belief continues in spite of no evidence supporting the belief) – the idea that objects, events or people have a personal significance for and association with the patient (usually of very strong intensity) but in fact these events, objects or people (also: messages in TV, internet, news) have in common with the patient

4. Thought disorders: paranoid • Delusion of control: beliefs that patient’s actions, movements or thoughts are controlled by an external agency, people or power and not driven by himself/herself • Delusion of possession of thoughts: i. e. thoughts insertion (thoughts are not the patient’s own but implanted from outside), thoughts withdrawal and thoughts broadcasting (due to lack of normal convictions that thoughts are private and cannot be shared unwillingly)

4. Thought disorders: paranoid • Thought insertion – insertion of a thought into one’s mind by an outside agent • Thought withdrawal – having one’s thought withdrawn from one’s mind • Thought broadcasting – being able to broadcast one’s thoughts

4. Thought disorders: maniacal delusions • Grandiose delusions: beliefs of exaggerated self-importance • Charismatic delusions: beliefs of kind of mission, special task and exceptional abilities to do this • Delusion of power: the patient is sure to have extraordinary strengths and capacities and therefore does not need to care for money, rules, other people etc.

4. Thought disorders: depressive delusions • Guilty delusions: beliefs of deep, unbearable sinfulness • Punishment delusions: beliefs of penalty which is impossible to avoid because of great fault (without real reason) • Catastrophic delusions: beliefs that everything has gone wrong and there is no future due to lack of money, house, family etc. • Hypochondric delusions: beliefs of serious (even fatal) illness without evidence of disease

4. Thought disorders • Overvalued idea: an acceptable comprehensible idea pursued by the patient beyond the bounds of reason. – The content of the overvalued idea is usually understandable and acceptable considering the person’s background • Hypochondria: preoccupation with (usually exagerrated or unreal) problems associated with organism and health

4. Thought disorders • In pressure of thought: occurs in mania, ideas arise in unusual variety and abundance , thought pass through the mind rapidly. • In poverty of thought which occurs in depression, the patient has few thoughts and these lack variety and richness , thoughts seem to move slowly through the mind. • In thought block the stream of thoughts is interrupted suddenly, and the patient feels that his mind has gone blank. It suggests schizophrenia

4. Formal thought abnormalities • Paralogy: ignoring rules of logic and common sense • Metonyms (paraphasia): words used in a new, private and unconventional way • Ambivalency • Catathymia • Evasive, racing thinking, flight of ideas • Blocking • Perseveration: persistent and inappropriate repetition of the same thought content

4. Formal thought disorders • Loose associations, incoherent thinking, derailment (ideas slip off the track and onto another one that is obliquely related): a loss of the normal structure of thinking; thinking (constantly) missing the point and senseless; rules of syntax and grammar are ignored – Example: „My friend has an electric-radio receiver, but he never told me where it is. In fact, I have been to nuclear power plant, and there is nothing dangerous” • Circumstantiality (inclusion of too many trivial details, seriously indirect) • Tangentiality (oblique or irrelevant answers)

4. Thought disorders • Derealization: feeling that the world surrounding is unreal/substantially changed in some alien way • Depersonalization: feeling that the body and/or personal identity is unreal/substantially changed/lost both may be associated with anxiety or psychosis

Examples of questions about thought disorders • “What’s been on your mind lately? ” • “Do you find yourself ruminating about things? ” • “Are there thoughts or images that appear really difficult if getting out of your head? ” • “Are you worried/scared/frightened about something or sb? ” • “Do you have beliefs that are not shared by others? ” • “Do you ever feel detached/removed/changed/different from others around you? ” • “Do things seem unnatural/unreal to you? ”

Examples of questions about thought disorders & hallucinations • “Do you think someone or some group intend to harm you in some way? ” • [In response to something the patient says] “What do you think they meant by that? ” • “Does it ever seem like people are stealing your thoughts, or perhaps inserting thoughts into your head? Does it ever seem like your own thoughts are broadcast out loud? ” • “Do you ever see (visual), hear (auditory), smell (olfactory), taste (gustatory), and feel (tactile) things that are not really there, such as voices or visions? ” (Hallucinations are false perceptions) • “Do you sometimes think that real things around you, such as muffled noises or shadows may denote something special? ” (Illusions are misinterpreted perceptions)

5. Obsessions & compulsions • Obsessions: recurrent persistent thoughts, impulses, or images that enter the mind despite efforts to exclude them. Obsessions are regarded as untrue, useless, or senseless. • The characteristic feature of obsessions is the subjective sense of a struggle, the patient resists the obsession, which nevertheless intrudes into awareness. • There may be obsessional thoughts, ruminations, impulses or doubts

5. Obsessions & compulsions • Compulsions: repetitive purposeful behaviors, performed in a stereotyped way (which is also called compulsive ritual), in response to an obsession. • Recognized as absurd and senseless but the compulsive behavior must be carried out: checking, cleaning, counting, dressing • Compulsive behavior transiently reduces the anxiety associated with the obsession

5. Questions about obsessions & compulsions • Have you ever been bothered by certain embarrassing, scary, or ridiculous thoughts that came into your mind over and over even though you tried to ignore or stop them? • If yes: Please describe them. • Have you ever felt you had to repeat a certain act over and over even though it did not make much sense? Like checking or counting something over and over or washing your hands over and over again, although you knew they were clean?

6. Disorders of speech • Quantity: – talkative, spontaneous, expansive, rapid – paucity, poverty of speech – restriction in the amount of spontaneous speech – (poverty of content of speech – speech that conveys little information even though amount is adequate) • Rate: – Fast, slow, hesitant, pressured? • Volume (tone): – Loud, strong, soft, monotonous, mumbled, weak? • Fluency and rhythm: – slurred, clear, with appropriately placed inflections, hesitant, with good articulation, aphasic?

6. Disorders of speech (C, E, T) • • Dysarthria Stuttering, stammering Vocal tics Aphasias • • Lack of coherence Neologisms Ambisentences Poverty of speech • Clang association (choice of words based on their sounds) • Verbigeration • Echolalia • Word salad

7. Affect & mood disorders (O, C, E, T) • Mood - prevailing and prolonged emotional state that determines a person’s overall perception, feeling, thinking and behaviour for a considerable period of time: – Elevated – Decreased – Dysphoric

7. Affect & mood disorders • Affect - short-lived and changeable emotions that emerge in immediate reaction to a particular aspect or object & expression of a subjectively experienced feeling state (emotion) – Appropriateness to situation? consistency with mood? congruency with thought content? – Fluctuations: labile? even? – Range: broad? restricted (flat, blunted)?

7. Mood disorders • Depressive mood is abnormal when it is out of proportion to the misfortune, or is unduly prolonged. Usually associated with: – Lowering self-esteem – Pessimistic or negative thinking • Anhedonia: marked reduction or loss of the experience of pleasure.

7. Mood disorders: questions about depression • Have there ever been times when you felt unusually depressed, empty, sad, or hopeless for several days or weeks at a time? • Have there ever been times when you felt very irritable or tired most of the time for hardly any reason at all? • Have there ever been times when you felt no or markedly decreased satisfaction and pleasure doing things which usually were pleasant for you? • Have these feelings ever stayed with you most of the time for as long as 2 weeks?

7. Mood disorders • Elation - an extreme degree of happy mood often coupled with other changes, including increased feeling of – self-confidence – well-being – increased activities • Dysphoria: angriness as a dominant emotion and type of reaction; usually associated with tendency for agression

7. Mood disorders- mania • • D I G F A S T Distractible Irritability Grandiosity Flight of ideas Activity (increase) Sleep (decrease) Talkative

7. Mood disorders: questions about mania • Have there ever been times when you felt unusually high, charged up, excited, or restless for 1 week at a time? • Have there ever been times when other people said that you were too high, too charged up, too excited, or too talkative? • Have these high, excitable moods ever stayed with you most of the time for at least 1 week?

7. Mood & emotions disorders • Anxiety is abnormal when its severity is out of proportion to the threat of danger or when it outlasts the threat. – Mental symptoms of anxiety: restlessness, narrowing attention, worrying thoughts, increased alertness and irritability – Somatic (vegetative) symptoms of anxiety: tachycardia, sweating, dread, tachypnoe (hyperventilation) and/or feeling of suffocation, muscle tension, urge to urinate or defecate

7. Mood & emotions disorders • Types of anxiety disorders: – Panic attacks – General anxiety (long-lasting worrying) – Phobias: • intense, unreasonable fear associated with some situation or object • simple or complex

7. Questions about panic attacks • Have you ever had sudden spells or attacks of nervousness, panic, or a strong fear that just seems to come over you all of a sudden, out of the blue, for no particular reason? • If yes: Did you have these attacks even though a doctor said that there was nothing seriously wrong with your heart?

7. Questions about generalized anxiety • Have there ever been days at a time when you felt extremely nervous, anxious, or tense for no special reason? • If yes: Have you sometimes felt this way even when you were at home with nothing special to do? • If yes: Have these nervous or anxious feelings ever bothered you off and on for as long as 6 months or more at a time?

7. Questions about phobias • Have you ever been much more afraid of things the average person is not afraid of? Like flying, heights, animals, needles, thunder, lightning, the sight of blood, or things like that? • Have you ever been so afraid to leave home by yourself that you would not go out, even though you knew it was really safe? • Have you ever been afraid to go into places like supermarkets, tunnels, or elevators because you were afraid of not getting out? • Have you ever been so afraid of embarrassing yourself in public that you would not do certain things most people do? Like eating in a restaurant, using a public restroom, or speaking out in a room full of people? • If yes to any of the above: When your fears were the strongest, did you try to avoid or stay away from (name feared stimulus) whenever you could?

8. Vegetative (psychophysiological) disturbances aka medically unexplained symptoms Abnormalities of: – Sleep – Appetite – Sex – Pain Questions about MUS: • Have you had a lot of physical problems in your life that forced you to see different doctors? • If yes: Have doctors had trouble finding what caused these physical problems?

8. Questions about anorexia & bulimia • Have you ever deliberately lost so much weight on a diet that people started to seriously worry about your health? • If yes: Were you afraid of getting fat even when other people said you were thin enough? • Did you ever have a problem with binge eating, when you would eat so much food so fast that it made you feel sick? • If yes: When you were doing this, did you feel your eating binges were not really normal? • If yes: Was the urge to binge sometimes so strong that you could not stop, even though you wanted to? • If yes: Did you ever vomit after eating, use laxatives, or excessively exercise?

9. Stressful events: current and past • • Unemployment Bad financial situation Legal problems Loss of close relative, health, reputation, social position • Substantial change of life situation, i. e. marriage/relationship breakdown • Rape, sexual harrasment

10. Suicide risk assessment: levels 1. Suicidal thoughts (passing through) 2. Suicidal ideations: a. Unspecific (exploring possibility) b. Precise 3. Suicidal preparations: collecting drugs, choosing place for fall, etc. 4. Farewell: testimony, dispensing things, good-bye letters (tweets, sms), unexpected reconcile with enemies etc.

10. Suicide risk assessment • It is NOT true that: – Patient considering suicide does not want to talk about it – Open talking about suicide increases risk of sucide attempt • It is true that c. a. 70% suicide victims visited a doctor in a month before an attempt

10. Suicide risk assessment • Risk factors for sucide – Male gender – Psychosis and/or depression – Substance dependence – Loneliness (lack of a social support ) – Insomnia – Chronic intractable pain – Serious stressful situation, loss of sb or sth very important for patient – Age: teen or elderly – History of sucicide attempts and or familial history of suicide

The ICD-10 definition of mental disorder • Clinically recognizable set of symptoms and/or behaviors associated in most cases with distress and worsening personal functions. • Important: social deviance or conflict alone, without personal dysfunction, should not be included in mental disorder

DSM-IV – Axis I- clinical syndromes – Axis II- developmental/personality problems – Axis III- general medical problems – Axis IV- social and environmental problems – Axis V- level of social adjustment (GAFGlobal Assessment of Functioning: 0 - 100)

Family History • Psychiatric Axis I and II disorders are familial. Monozygotic twin and adoption studies suggest that the familial occurrence is not merely learned but follows a genetic disposition. – having a parent with bipolar disorder, for example, raises the patient’s risk of developing the same disorder by at least 7 -fold • The familial occurrence in first-degree relatives and their treatment response can therefore confirm the patient's diagnosis and predict the treatment response. • Therefore, family history is the most important predisposing factor of the biological part of the patient's biopsychosocial condition.

Developmental History Even if a psychiatric diagnosis during childhood or adolescence is not made, the interviewer should consider five important areas: • Developmental milestones: delayed psychomotor and speech development and toilet training may point to early developmental problems. • Ability to learn in school: slow learning or repetition of the first grade may point to mental retardation; circumscribed deficits, such as dyslexia or acalculia, may indicate a learning disorder. • Attention problems with hyperactivity and poor impulse control may contribute to substance abuse and to the development of a personality disorder, such as antisocial personality disorder.

Developmental History • Disciplinary problems may cover a broad range. Arguments with teachers, objections to rules, temper tantrums, resentfulness, and vindictiveness point to oppositional defiant disorder. Fighting, stealing, vandalism, and school discipline problems characterize males; lying, truancy, running away from home, substance use, and prostitution characterize females with conduct disorder. Furthermore, symptoms such as violent behavior toward superiors, peers, or animals and fire setting also suggest conduct disorder, which, in later adolescence, may progress to antisocial personality disorder. The earlier the onset of conduct disorder, the worse the prognosis and the greater the risk for later mood, anxiety, somatoform, and substance-related disorders. • During childhood and adolescence, social withdrawal with decline in hygiene, truancy, and anger outbursts may herald schizophrenia; phobias, obsessions, compulsions, and depressive symptoms may precede adulthood psychiatric disorders.

Medical History (Axis III) • The medical history is of importance to the psychiatric interviewer for three reasons: (1) medical disorders can cause symptoms of panic, anxiety, depression, and delusional thinking diagnosed as “psychiatric disorder due to a medical condition; ” (2) side effects of medications prescribed for medical disorders may mimic psychiatric symptoms and disorders; (3) any medical disorder and its treatment can complicate course and treatment of psychiatric disorders and vice versa. Drug–drug interactions can range from mild to severe.

Burden of somatic illness • Somatic illness may be reason of delirium or psychosis: tumors, infections, metabolic diseases, cardiac arrythmias • Pharmacologic treatment may be reason of – delirium (hypoglicaemia, dehydratation) – psychosis (steroid therapy) – mania (steroid therapy) – depression (steroid therapy, interferon)

Social history • Premorbid versus postmorbid psychosocial functioning: family life and work, including school and military, friends, and community functions such as church and social organizations • Social factors as risks for psychiatric disorders: physical, sexual, and emotional abuse, rejection and neglect during upbringing, and provision of poor role models (be careful! patients with dissociative disorders, often report a history of physical and sexual abuse, especially during childhood barring memory distortions, the presence of abuse can often be confirmed by outside evidence). • Negative impact of psychiatric disorders on social advancement: psychiatric disorders can impede the patient's social development and can lead to demotion, job loss, and divorce

GAF • Global Assessment of Functioning
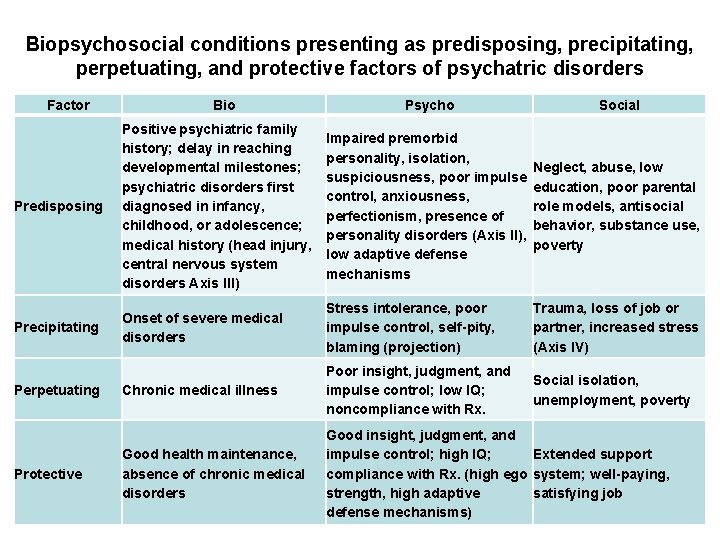
Biopsychosocial conditions presenting as predisposing, precipitating, perpetuating, and protective factors of psychatric disorders Factor Psycho Social Predisposing Positive psychiatric family history; delay in reaching developmental milestones; psychiatric disorders first diagnosed in infancy, childhood, or adolescence; medical history (head injury, central nervous system disorders Axis III) Impaired premorbid personality, isolation, suspiciousness, poor impulse control, anxiousness, perfectionism, presence of personality disorders (Axis II), low adaptive defense mechanisms Neglect, abuse, low education, poor parental role models, antisocial behavior, substance use, poverty Precipitating Onset of severe medical disorders Stress intolerance, poor impulse control, self-pity, blaming (projection) Trauma, loss of job or partner, increased stress (Axis IV) Chronic medical illness Poor insight, judgment, and impulse control; low IQ; noncompliance with Rx. Social isolation, unemployment, poverty Good health maintenance, absence of chronic medical disorders Good insight, judgment, and impulse control; high IQ; Extended support compliance with Rx. (high ego system; well-paying, strength, high adaptive satisfying job defense mechanisms) Perpetuating Protective Bio

Structuralised methods of psychiatric examination • SCID-I • SCAN (self-reported screening tool) • M. I. Neuropsychiatric Interview v. 6. 0 • PRIME-MD

SAD PERSONS • The comorbidity of major depression and substance use disorder leads to the highest risk of suicide. A mnemonic for risk factors of suicide is helpful: – Sex: Women are more likely to be attempters, men more likely to be committers. – Age: Highest rate of suicide is in teenagers and the elderly. – Depression: 15 percent commit suicide. – Previous attempts: 10 percent of previous attempters finally succeed. – Ethanol abuse: 15 percent of alcoholics commit suicide. – Rational thinking loss, psychosis. 10 percent of chronic schizophrenics commit suicide. – Social support is lacking. – Organized plan increases the suicide risk. – No spouse increases the suicide risk. – Sickness. Chronic illness increases the risk.

Questions for alcohol problems n wrong n right Does your wife And what about alcohol? say sometimes that you drink too much?
Questions for alcohol problems wrong How often do you drink alcohol? right How long did you not drink at all during last year?

CAGE • C Have you ever felt you needed to Cut down on your drinking? • A Have people Annoyed you by criticizing your drinking? • G Have you ever felt Guilty about drinking? • E Have you ever felt you needed a drink first thing in the morning ( Eye-opener) to steady your nerves or to get rid of a hangover? Tolerance, withdrawal, and loss of control in the amount or time of use can all be signs of dependence.

SOAP Four risk factors for the patient's and others' safety: • Suicidality, homicidality, physically assaultive, unpredictable, explosive, and self-injurious behaviors and implied or overt threats. • Organic disturbances of cognitive functions: disorientation, memory disturbances, decline of executive functions, aphasias and apraxias that prevent the patient from exercising the activities of daily living (ADL). • Alcohol and other substance abuse, ranging from occasional social use to uncontrollable addictive behavior and dependency that may endanger the patient's and others' safety on the road and in legal, marital, occupational, and financial status. • Psychotic features, such as delusions, especially delusions of control, and hallucinations, especially command hallucinations, and their dangerousness and the patient's obedience to these experiences. Included here are illogical thinking and speech and catatonic behavior.

How to deal with difficult patients type: dependent • Seem to need an inordinate amount of attention and yet never seem reassured. • Likely to make repeated urgent calls between scheduled appointments and to demand special consideration. • The doctor needs to be firm in establishing limits while reassuring the patient that his or her needs are taken seriously and are treated professionally.

How to deal with difficult patients type: demanding • Some patients have a difficult time delaying gratification and demand that their discomfort be eliminated immediately. They are easily frustrated and can become petulant or even angry and hostile if they do not get what they want when they want it. They may impulsively do something self-destructive if they feel thwarted, and they appear manipulative and attention seeking. Beneath their surface behavior, they may fear that they will never get what they need from others and thus must act in that inappropriately aggressive way. • The doctor must be firm with these patients from the outset and must clearly define acceptable and unacceptable behavior. These patients must be treated with respect and care, but they must also be confronted with their behavior.

How to deal with difficult patients type: isolated • Isolated and solitary patients do not appear to need or to want much contact with other people. Intimate contact with the doctor is viewed with distaste, and such patients would prefer to take care of themselves entirely without the doctor's help if it were possible. Some isolated patients would receive a diagnosis of schizoid personality disorder. They are withdrawn, absorbed in a world of fantasy, and are unable to talk about their feelings. • The doctor should treat these patients with as much respect for their privacy as possible and should not expect them to respond to the doctor's concern in kind.

How to deal with difficult patients type: psychotic • Patients with psychotic symptoms have difficulty thinking clearly and reasoning logically. Their ability to concentrate may be impaired, and they may be distracted by hallucinations and delusional beliefs. Psychotic patients are often frightened and may be quite guarded. • Quite often, the evaluation of a patient with psychotic symptoms needs to be more focused and structured than that of other patients. Open-ended questions and long periods of silence are apt to be disorganizing. Short questions are easier to follow than long ones. Questions calling for abstract responses or hypothetical conjectures may be unanswerable.

How to deal with difficult patients type: psychotic • For patients with hallucinations, the full phenomenology of the hallucination should be explored. The patient is asked to describe the sensory misperception as fully as possible. For auditory hallucinations, this includes content, volume, clarity, and circumstances; for visual hallucinations, this includes content, intensity, the situations in which they occur, and the patient's response. • The evaluator should distinguish between true hallucinations, on the one hand, and illusions, hypnagogic and hypnopompic hallucinations, and vivid imaginings, on the other. • Hallucinations are perceived as real sensory stimuli and should not be dismissed as fanciful; however, the psychiatrist should ask questions about their fixity and the patient's level of insight: “Does it ever seem that the voices are coming from your own thoughts? ” or “What do you think is causing the voices? ”

How to deal with difficult patients type: psychotic • Delusions, by definition, are fixed, false beliefs. Delusional patients often come to psychiatric evaluation having had their beliefs dismissed or belittled by friends and family. They are on guard for similar reactions from the examiner. It is possible to ask questions about delusions without revealing belief or disbelief (e. g. , “Does it seem that people are intent on hurting you? ” rather than “Is there a plot to hurt you? ”). • Careless use of psychiatric jargon should be avoided, particularly in evaluating delusions. Words such as grandiose and paranoid and, indeed, the word delusion itself seem harsh and judgmental and are unlikely to be helpful in eliciting information.

How to deal with difficult patients type: psychotic • Many psychiatrists have found that patients can speak more freely when asked to talk about the accompanying emotions rather than the belief itself (“It must be frightening to think there are people you don't know who are plotting against you”). • Although the psychiatrist does not attempt to reason them away, a gentle probe may determine how tenaciously the beliefs are held (“Do you ever wonder whether those things might not be true? ”).

How to deal with difficult patients type: psychotic • Patients with paranoid delusions (and patients with high levels of nondelusional suspiciousness) are best evaluated with a respectful, but somewhat distant, formality and with scrupulous honesty. Efforts to reassure or to ingratiate often increase suspicion. The psychiatrist must keep in mind the possibility of being incorporated into a delusional belief and should ask about it directly (“Are you concerned that I might try to hurt you? ”).

How to deal with difficult patients type: thought disorder • Disorders of thought form can seriously impair effective communications. The evaluating psychiatrist should note formal thought disorders while minimizing their adverse impact on the interview. When derailment is evident, the psychiatrist typically proceeds with questions calling for short responses. For a patient experiencing thought blocking, the psychiatrist needs to repeat questions, to remind the patient of what was already said, and, in general, to provide an organization for thinking that the patient is unable to provide.

How to deal with difficult patients type: depressed and potentially suicidal • Severely depressed patients may also have difficulty concentrating, thinking clearly, and speaking spontaneously. • The intensity of mood disturbance may well lead to distortions in thinking and perception. Some depressed patients have psychotic symptoms in addition to cognitive difficulties. • The psychiatrist evaluating a depressed patient may need to be more forceful and directive than usual.

How to deal with difficult patients type: depressed and potentially suicidal • A thorough assessment of suicide potential addresses intent, plans, means, and perceived consequences, as well as history of attempts and family history of suicide. Many patients mention their thoughts of suicide spontaneously. If not, the examiner can begin with a somewhat general question, such as – “Do you ever have thoughts of hurting yourself? ” or – “Does it ever seem that life isn't worth living? ” These questions can then be followed up with more specific questions.

How to deal with difficult patients type: depressed and potentially suicidal • The examiner must naturally ask simple, straightforward, noneuphemistic questions. • Asking about suicide does not increase the risk. The psychiatrist is not raising a topic that the patient has not already contemplated. • Specific, detailed questions are essential for prevention.

How to deal with difficult patients type: depressed and potentially suicidal • Intent: The examiner must determine the seriousness of the wish to die. Some patients report that they wish that they were dead but would never intentionally do anything to take their own lives. This level of intent is sometimes referred to as passive suicidal ideation. Other patients express greater degrees of determination. Near the other end of the spectrum of intent is the patient who says, “I've decided that I have to kill myself and nothing you can say or do will change that. ” • Patients who are the most difficult to help: those who tell no one about their suicidal plans and proceed in a deliberate, systematic manner

How to deal with difficult patients type: depressed and potentially suicidal • Plans Patients with well-formulated plans are generally at greater risk than patients who do not know what they would do, but the method of suicide is not always a reliable indication of the risk. Even though some actions, such as jumping or shooting, are much more likely to be fatal than others, patients make mistakes. A pill overdose taken at the time at which a spouse is expected to arrive home may become deadly if the spouse is delayed in traffic. The psychiatrist should also ask about preparatory actions, such as giving away goods and putting one's estate in order.

How to deal with difficult patients type: depressed and potentially suicidal • Means Asking patients about the intended means of suicide is helpful in two ways. First, it clarifies the urgency of the situation; persons wanting to shoot themselves who own a loaded gun are more dangerous than those who have no idea where to find a gun. Second, the understanding of intent is sharpened by knowing whether a patient has thought through the steps necessary to carry out the action.

How to deal with difficult patients type: depressed and potentially suicidal • Perceived Consequences – Patients who see something desirable resulting from their deaths are at increased risk for suicide. – A reunion fantasy, the belief that a person will be reunited with a deceased loved one, may be a powerful motivating force toward suicide. – On the other hand, some potentially suicidal patients are restrained by what they see as negative consequences (e. g. , “My children need me too much; they'd never be able to get along without me”)

How to deal with difficult patients type: agitated and potentially violent • Most unpremeditated violence is preceded by a prodrome of accelerating psychomotor agitation: i. e. pacing and pounding the fist in a hand, loud, abusive, obscene, and threatening speech • Prodrome usually lasts from 30 to 60 minutes before erupting into physical violence

How to deal with difficult patients type: agitated and potentially violent • How to minimize the agitation and potential risk: – The interview should be conducted in a quiet, nonstimulating environment. – There should be enough space for the comfort of the patient and the psychiatrist, with no physical barrier to leaving the examination room for either of them. – Be non-provocative. – During the interview, the examiner should avoid any behavior that could be misconstrued as menacing: standing over the patient, staring, speaking loud or touching. Constant control should be kept on non-verbal communication cues. – Only necessary questions to complete an adequate evaluation

How to deal with difficult patients type: agitated and potentially violent • The examiner should ask whether the patient is carrying weapons and may ask the patient to leave the weapon. • If the patient's agitation continues to increase, the examiner may need to terminate the interview. • Depending on the setting, assistance from security personnel or physical or chemical restraints may be appropriate. • The physician's own subjective sense of comfort or fear should be rational hint.
- Slides: 107