Mental Health Workshop Carly Harries LLB Law degree

Mental Health Workshop

Carly Harries LLB Law degree Appropriate Adult Kingston Police Station CARAT worker at Wandsworth Prison Youth Worker School Governor – Child Protection, LAC and SEND Presenter Home School Link Worker Family Links Practitioner Solution Focused Family Support Facilitator Young Carers Operational Lead Play and Creative Arts Therapist Mental Health Specialist Leader of Education for Mental Health

The current picture of mental health for children and young people SEMH services in Surrey – Commissioning input and the Thrive Model at macro and micro level Mentally Healthy Schools Mental health spectrum of needs and SEMH provision in school – a practical working model SEMH measurement and impact Attachment and Domestic Abuse training tasters Today’s workshop

Health Care Warning Be kind to yourself

The Current Picture • 12. 6% of children have a mental health condition/disorder • 1 in 10 children in your classroom • 1 in 5 of those children access Camhs • 1 in 2 speak to a teacher • Health and Education working together • Context of limited resources • ‘Good enough’ school provision • Anna Freud December 2018

• increase in mental health problems can’t be reduced to a single cause. What we do know is that overwhelmingly and consistently poor mental health has been linked to social pressure and deprivation. It shows that children living in households with the lowest income are about twice as likely as those living in the highest to have a disorder. Current picture continued… • young people who identify as lesbian, gay, bisexual or with another sexual identity are roughly two-and-a-half times as likely to have a mental disorder • increase in emotional disorders in girls as they grow older is deeply worrying and anxiety and low mood in girls is rising and the figures today on body dysmorphia may reflect some of the pressures that contribute to this. • need for early intervention in pre-school children given that one in eighteen had a mental health disorder - early recognition of emotional problems and the impact of trauma, stress and deprivation on pre-school children also draws attention to the need to intervene before school starts. • 90% GPs surveyed said health and social care services for young people who have anxiety, depression, eating disorders and other conditions are inadequate and 99% fear patients will come tio harm through lack of access to treatment. Source: Survey of 1000 GPs by Mede. Connect Healthcare Insight, 14 -28 Nov 2018

‘Transforming children and young people’s mental health provision: a green paper’ December 2017 A mental health lead in every school – SLT Lead and Operational Lead Mental health support teams – trained staff linked to groups of schools offering 121 and group help with mild to moderate mental health difficulties – will be the link between school and NHS – focus on anxiety, behaviour, low mood. Shorter waiting times to mental health services. Improve understanding of mental health – social media impact, how to support families and research how to prevent mental health problems. All Therapy in schools should be delivered by a professional counsellor or therapist who is a member of a professional body, on a professional register overseen by the Professional Standards Authority and should be inspected by Ofsted. Education and Health working together

• Designing the right Emotional Wellbeing and Mental Health service for Children and Young People across Surrey • Thrive model • On Monday 14 th January 2019, the government announced their Long Term Plan for the NHS. This included the prioritisation of mental health and the committed funding with a vision of support that extends beyond traditional NHS boundaries. The THRIVE Framework is mentioned in the plan and represents a way to ensure the necessary paradigm shift takes place. Surrey • The THRIVE Framework was developed at the Anna Freud Centre and the Tavistock and Portman NHS Trust as a way to provide major whole-system change for children’s mental health support. • Since its creation, the Framework has been widely implemented across England. This means that currently almost half of all children and young people in England already live within a locality that is a member of the i. THRIVE (Implementing THRIVE) Community of Practice. • Surrey have now adopted the Thrive Approach for Children and Young people’s Mental Health and Wellbeing -Emotional Wellbeing Mental Health Strategy for Children and Young People in Surrey May 2019 http: //www. guildfordandwaverleyccg. nhs. uk/website/X 09413/files/190507 Surrey_CYP_EWMH_Strategy_CYP_version_v 6_0_GWCCG. pdf
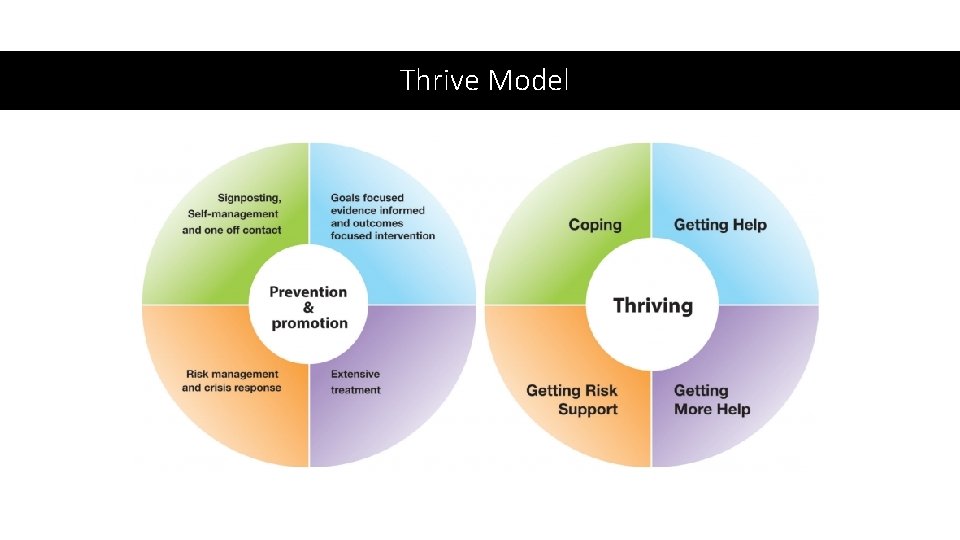
Thrive Model
Thrive • • • Thriving Getting Advice Children Getting Help Children Getting More Help Children Getting Risk Support Children

Mental Health and Wellbeing • ‘Emotional wellbeing Emotional health is an important part of overall health. People who are emotionally healthy are in control of their thoughts, feelings, and behaviours. They can cope with life's challenges’. • ‘Mental Health A state of wellbeing in which the individual realises his or her own abilities, can cope with the normal stresses of life, can work productively and fruitfully, and is able to contribute to his or her community. ’ Emotional Wellbeing Mental Health Strategy for Children and Young People in Surrey May 2019

Mental health classification – an ongoing difficulty to define and diagnose A Spectrum of Needs Mental Health/ Wellbeing– a state of wellbeing in which individuals can realise their potential Mental Distress –symptoms/experiences that are troubling and confusing Mental Health problem – Interfere with the ability to learn and enjoy life and deal with challenge Mental Health Disorder – similar to problems, but more severe, persistent or complex Mental Illness – psychosis, clinical depression – bipolar (manic depression) Mental Health Problems / Disorders Emotional – anxiety and fear, elective mutism, OCD (repetition) Hyperactivity - ADHD Conduct – aggressive, antisocial behaviours (boys in middle childhood), ODD Developmental – Autistic Spectrum Can have a mental health problem and good mental health if effectively managed www. mind. org. uk/information-support/a-z-mental-health/ 12
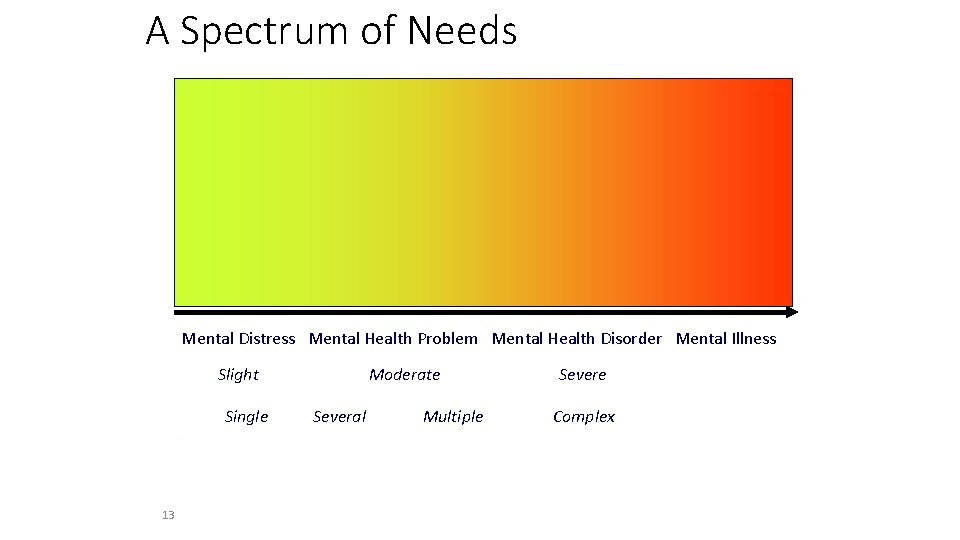
A Spectrum of Needs Mental Distress Mental Health Problem Mental Health Disorder Mental Illness Slight Single 13 Moderate Several Multiple Severe Complex
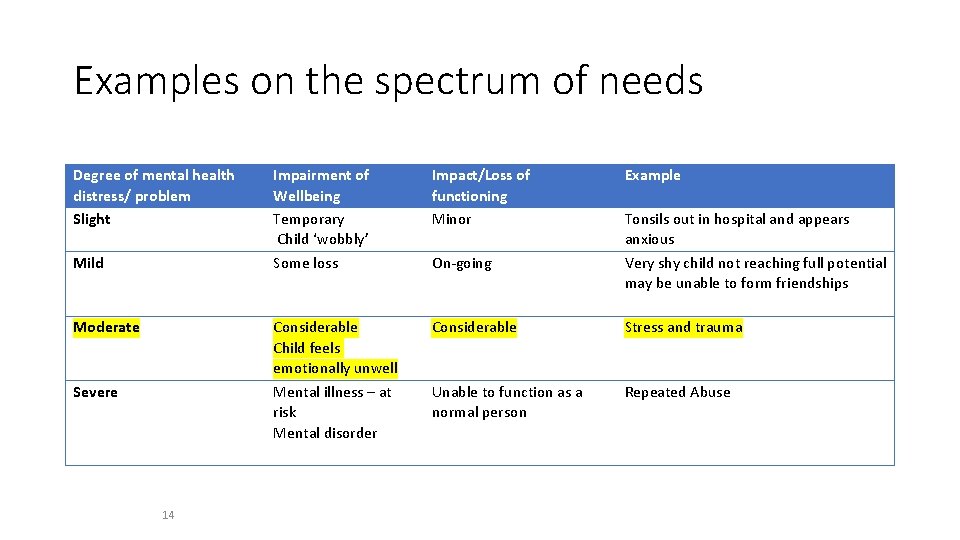
Examples on the spectrum of needs Degree of mental health distress/ problem Slight Mild Moderate Severe 14 Impairment of Wellbeing Temporary Child ‘wobbly’ Some loss Impact/Loss of functioning Minor Considerable Child feels emotionally unwell Mental illness – at risk Mental disorder Considerable Stress and trauma Unable to function as a normal person Repeated Abuse On-going Example Tonsils out in hospital and appears anxious Very shy child not reaching full potential may be unable to form friendships


• SDQs • Boxall Profile • ELSA scoring sheet • The Leuven scale for well-being and involvement SEMH Impact • Warwick Edinburgh Mental Wellbeing Scale (WEMWBS) • Spence Anxiety Scale • Case studies • Questionnaires • www. annafreud. org/media/4612/mwb-toolki-final-draft 4. pdf • A new way to measure impact across SEMH provision/interventions to meet organisation’s needs
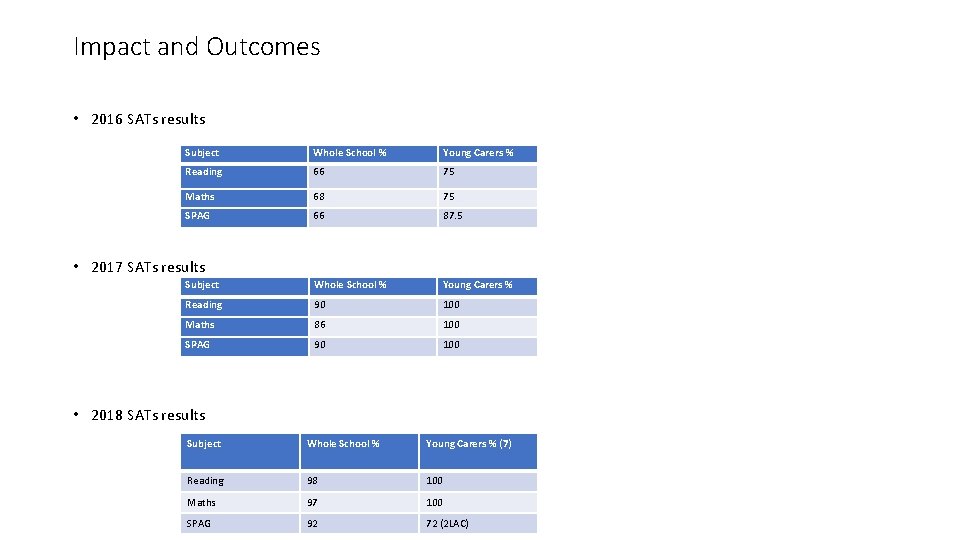
Impact and Outcomes • 2016 SATs results Subject Whole School % Young Carers % Reading 66 75 Maths 68 75 SPAG 66 87. 5 Subject Whole School % Young Carers % Reading 90 100 Maths 86 100 SPAG 90 100 • 2017 SATs results • 2018 SATs results Subject Whole School % Young Carers % (7) Reading 98 100 Maths 97 100 SPAG 92 72 (2 LAC)
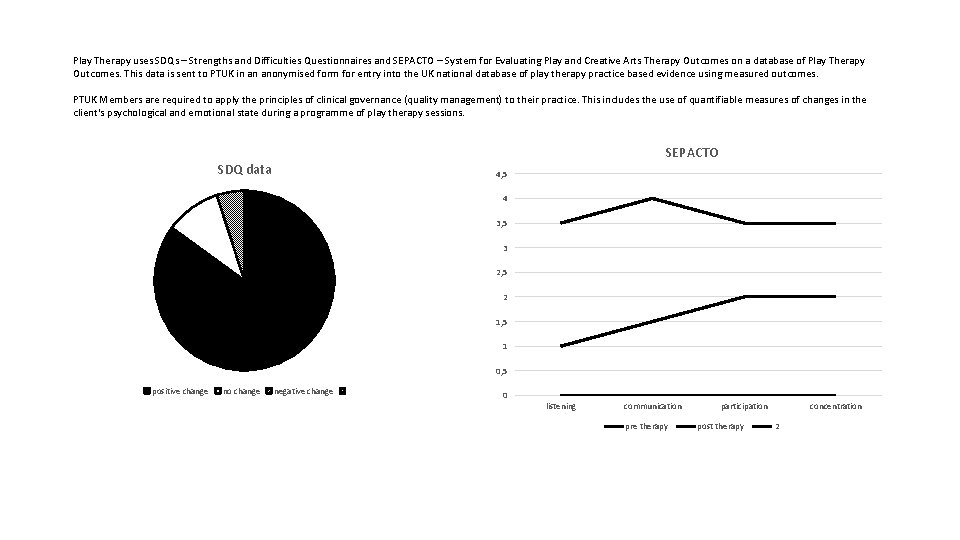
Play Therapy uses SDQs – Strengths and Difficulties Questionnaires and SEPACTO – System for Evaluating Play and Creative Arts Therapy Outcomes on a database of Play Therapy Outcomes. This data is sent to PTUK in an anonymised form for entry into the UK national database of play therapy practice based evidence using measured outcomes. PTUK Members are required to apply the principles of clinical governance (quality management) to their practice. This includes the use of quantifiable measures of changes in the client's psychological and emotional state during a programme of play therapy sessions. SEPACTO SDQ data 4, 5 4 3, 5 3 2, 5 2 1, 5 1 0, 5 positive change no change negative change 0 listening communication pre therapy participation post therapy concentration 2

SEMH provision in pictures…


Moving forward with the Thrive Model New language Moving away from diagnosis Based on need Shared decision making School’s signposting and referring, wellbeing and resilience provision for all, commissioning services, working together • A case study using thrive at a micro level • • •




Mentally Healthy Schools

What is a Mentally Healthy School?

Key Elements Opportunities for staff and children and young people to develop their strengths. Opportunities for staff and children and young people to develop their coping skills and resilience. Mental Health and Wellbeing is fundamental part of school’s values. Mental Health and Wellbeing is embedded into school culture. Mental Health and Wellbeing is everyone’s business.

Staff training Staff development Developing strengths Extra curricular activities Inclusive celebration Clubs Signposting and referral Parent and Carer engagement

Resilience Framework Resilience Audit – staff and SLT Developing coping skills and resilience Extra curricular activities Clubs – sense of belonging Lunch time clubs Nurture Groups Parenting Courses

Positive mental health and wellbeing as fundamental to its values, mission and culture Fundamental part of Values Inclusive Christian Values Resilience as a Value Part of School Vision and Aims – ‘A school where everyone recognises that they are valued and respected and in return value and respect one another, prioritising the well-being and mental health of all, children, staff and families, incorporating this into every aspect of provision. ’ The Ridgeway 2019

SLT Lead (role modelling, open-door policy, consultation) Mental Health and Wellbeing School Council (like Eco Council, Faith Team) – involving children as decision makers Policies – Young Carers, SEND, PSHE Embedded culture Assemblies PSHE Class circle times Review regularly Training Schedule – hot topics (for example attachment, trauma, young carers, ASD) Staff Wellbeing Strategy

Governors – Link Governor, agenda item on FGB SLT Lead Operational Lead Everyone’s Business Mental Health and Wellbeing School Council Children’s Voice – ‘Children can offer unique perspectives on what it is like to be a pupil at their school; involving them in decision-making can create meaningful change and better academic outcomes, as well as facilitating a sense of empowerment and inclusion’. www. mentallyhealthyschools. org. uk/whole-schoolapproach/childrens-voice/ Parent’s Voice and Parent/Carer Engagement – Parent Forum Staff Voice – Staff Wellbeing Forum

Next steps and Questions… • Decide who is going to be the lead for Mental Health in your school. Do you need an SLT Lead an Operational Lead? How will this team work? • Reflect on your SEMH provision – put it into a working model of interventions and presenting conditions. Where are the gaps? How can these be filled? • Training needs of your staff. From your SEMH provision model, reflect on the training needs of your staff. Do you have a rolling programme of hot topics in your staff meetings for mental health, do you have training on young carers, trauma, attachment? How can these needs be met? • How are your organisation’s needs going to be integrated into your SEMH provision – how can this be measured to show impact? • Utilise all the free resources you can to build your own working knowledge of mental health, know where to go for information and share your learning and experiences with colleagues. You do not need to be a specialist or diagnose – understand the basics and be open to learning more. • Think about your whole school approach to mental health and build up from there. • Underpin your work with the resilience framework and think about a risk and resilience approach to mental health planning. Audit with staff and as SLT. • Build in peer support for teachers and those working with vulnerable children. • How can we share good practice and resources?

Attachment and Domestic Abuse Workshop Taster • Attachment Training overview and learning outcomes • Domestic Abuse as a hot topic and example of how it may look in therapy • Putting the puzzle together

• Develop understanding and insight of Attachment as a theory and what attachment behaviours look like in practice. Attachment Workshop Outcomes… • Understand the different types of attachment styles and how they may present in our school environments. • Reflect and wonder how our schools can support children and young people with attachment behaviours. • Consider how attachment fits in Mental Health and Wellbeing provision in our schools and any training needs for our staff. • Look at Domestic Abuse as a hot topic. • Any other expectations?

How can Attachment Awareness and Training help us in Education? • Identifying those who are at risk within education • Understanding the need for translation due to insecure attachment • Understanding why investing into relationships is vital for adaption and recovery • Differentiating emotional and social tasks and expectations. Neuroscience and the nervous system - the optimum state for learning • Stress regulators vs behaviour managers • Behaviour as communication • Connection first - building relationships • The reality of secondary stress • Staff care • The Attachment framework • The impact of developmental trauma • The Attachment Aware School • Co- regulation and windows of tolerence • Being kept in mind and support to develop a robust sense of self

Think of a person, child or young person. It could be a member of staff, a child or young person in your school. This is confidential, you will not be sharing who this is. Pick a pair of shoes to represent your person. Pair of shoes exercise We are going to try and understand why they might behave/present how they do and what this may bring up for us and our responses through attachment theory. Empathy – what it might be like for them, to walk in their shoes. Keep reflecting about your person and holding them in your mind as we go through the slides. This may be challenging and bring up big feelings. Be kind to yourself.

Attachment is a close emotional bond between two people (Sandrock) The importance of attachment and responsiveness of primary caregiver. The attachment experience that shapes us. Each individual’s experiences shape their brain – wiring together (neuroscience) Internal working model and Window of Tolerence Attachment as a Child Development Theory

Attachment Theory - John Bowlby, Mary Ainsworth and the Stranger Situation, Pat Crittenden Dynamic. Maturational Model of Attachment and Adaptation (DMM) • Bowlby believed that infants and their primary caregivers are predisposed to form attachments. He argues that the newborn baby is biologically equipped to illicit attachment behavior – baby cries, clings, coos, smiles to keep primary caregiver nearby and long term effect is to increase infants’s chance of survival. • Consequences throughout the lifespan – if attachment is positive and secure, the individual has a foundation for developing into a competent individual who has positive social relationships and is emotionally mature. If this relationship is negative and insecure, according to Bowlby, as the child grows, he or she is likely to encounter difficulties in social relationships and dealing with emotions.
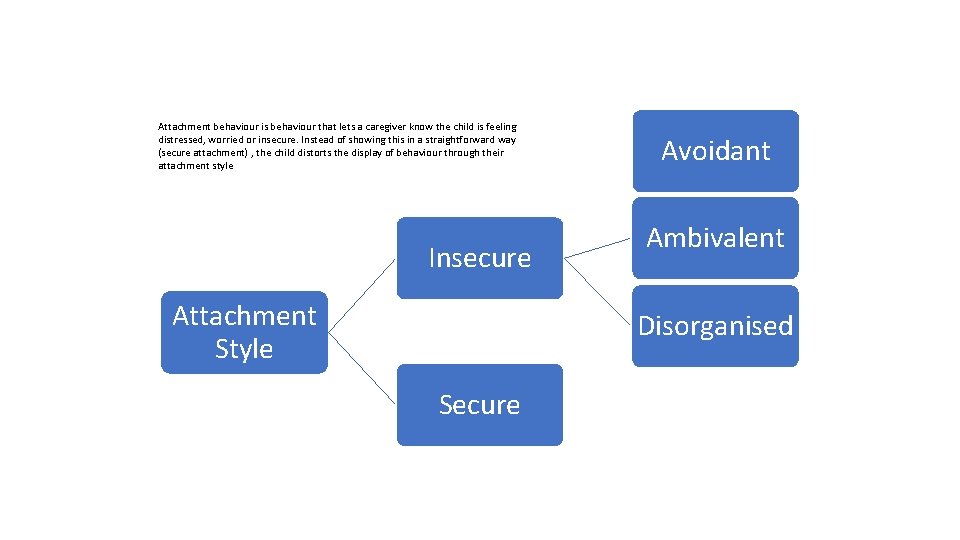
Attachment behaviour is behaviour that lets a caregiver know the child is feeling distressed, worried or insecure. Instead of showing this in a straightforward way (secure attachment) , the child distorts the display of behaviour through their attachment style Insecure Attachment Style Avoidant Ambivalent Disorganised Secure

• Secure attachment • Avoidant attachment – 20%population, needs not met by caregiver, I’m not going to need anything from anybody, do not seek comfort or form friendships naturally, feel safe when in control and are self-reliant. Often have low self-esteem. Children minimize attachment behaviour to maintain closeness to caregiver who is already rejecting. Appear less emotionally distressed or worried than they feel, expressed through passive and withdrawn behavior displaying little emotional distress. Children act as if they don’t need the parent. • Ambivilant attachment – inconsistent care from caregiver, I don’t know if I’m your friend, can be clingy and then aggressive. Child may maximise behaviour to elicit care from inconsistent parents. They may appear more emotionally distressed or worried than they feel and show this through clingy behaviour and resisting being soothed. Trauma and Attachment • Disorganised attachment – Caregiver inconsistent and unpredictable – one minute loving, the next abusive. Child does not know how to predict behaviour of caregiver so remains in defensive, threat response. I can’t regulate my emotions, under stress I can’t think, don’t get much from relationships – I’m going to take from you (abuse or neglect). Leads to most complex trauma. Develops when parents are frightened (domestic abuse) or frightening to the child (abuse). Child will be frightened if parent is frightened. They may increase feelings of safety by increasing degree to which they feel in control. Cannot trust parent to keep them safe so become controlling in their behaviour and take control of the relationship. • Each child or adult experiences trauma and attachment differently. Our experiences sculpt our brain. • Trauma and attachment styles sit in the limbic system – our automatic reactions, our temperament, how we experience the world. Dysregulation of fight, flight, freeze happens in the limbic system. Leads to: Hypoarousal –dissociative, numbing of emotions, withdrawn or hyperarousal – hypervigilant, agitated, anxious. Window of tolerance inbetween is often small.

Case studies for understanding attachment style Tommy’s mother has learning difficulties and struggles to meet the needs of her children. Following his birth, Tommy’s mother suffered post-natal depression and Tommy was severely neglected as a small child left for long periods of time in his cot or strapped in his buggy. Jane’s mother had a very difficult childhood and spent long periods in care. Her mother’s partner is aggressive and violent in the home and would often resort to hitting Jane if she misbehaves. She was removed from the family home due to serious child protection concerns and her behavior has become increasingly challenging and unpredictable. Sammy’s mum was 16 when she had him and she does not know who the father is. Sammy cries out in the night because this might bring him some comfort, sometimes someone might put a bottle in his mouth or occasionally give him a cuddle but he doesn’t know if they’ll come or not. He has learnt to cry loudly in the hope that someone will come.
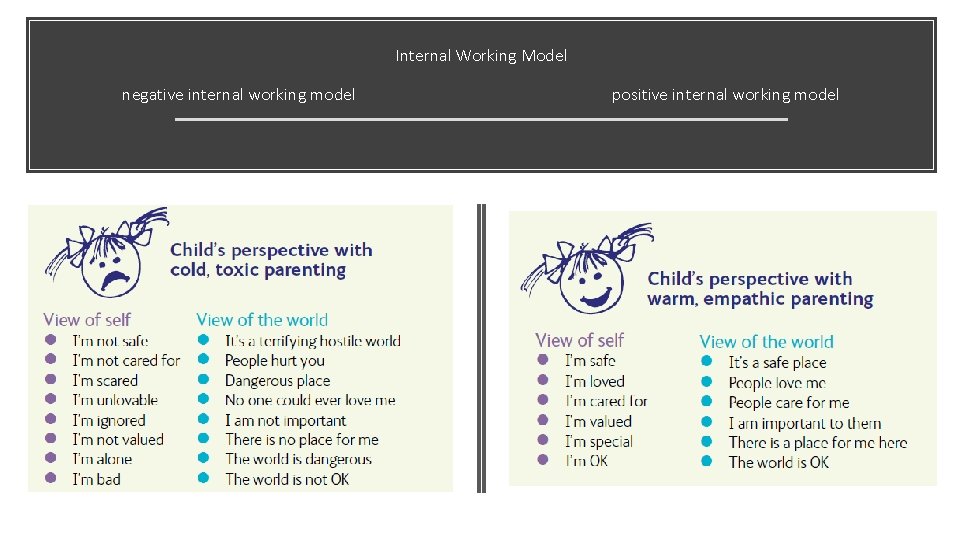
Internal Working Model negative internal working model positive internal working model

Developmental Trauma When children experience early loss, separation, abuse or neglect their brain development is affected in significant ways. They often experience what is known as Developmental Trauma, which means their development has gone off track and they cannot behave, feel, relate and learn like other children their age. • Signs of sensory problems at school - difficulty with concentration & attention, overwhelmed by noisy busy classrooms, difficulty throwing and catching a ball, difficulty with co-ordination and balance, poor handwriting and pencil grip, shutting down/zoning out frequently throughout the day • Signs of attachment insecurity at school - difficulties processing new information, under performance or over-dependence on academic perfection, difficulties planning, organising and completing tasks , struggles with transitions, loss and change, big reactions or zoning out for reasons not obvious to others, difficulties in friendships, find it hard to ask for help or the child is always needing help, over compliance or disruptive behaviour in class • Signs of emotional dysregulation at school - outbursts of anger or distress at small events such as a change in activity, immaturity in friendships – jealousy, possessiveness, struggles to share, too emotional to take on board new learning, tearfulness and anxiety at drop off , overdependence on adults, rule breaking, aggression, running off and hiding • Signs of behaviour dysregulation at school - lying, stealing, hoarding, disruptive in class, restless, fidgety, moves about the classroom lots slowed down, unresponsive • Signs of disassociation at school – frequent day dreaming and lack of focus leading to under achievement, abilities to read, write, learn change drastically from one task to the next, the child is forgetful or confused about things s/he should know, such as friends’ names, confusion about day and time, they get back homework that they have no memory of doing, voice hearing. • Poor cognitive skills at school - difficulties problem-solving , struggles to complete a task, unable to process information quickly, cannot remember new information , cannot put into words what they are thinking, poor ability to read social cues, cannot organise their belongings • Poor self concept/ identity at school - being knocked back easily, becoming upset at failure, self doubt and self criticism, not trying for fear of failure

Transference • Why are these children’s behaviour so difficult for us to manage and bring a big emotional response in ourselves? • The answer is in part due to transference. Transference is the unconscious redirection of feelings a person has especially those retained from childhood experiences. Counter transference then takes these feelings, mixes them with our own childhood experiences and feelings and throws them back out. • My brain cannot cope with these feelings, I am overwhelmed and feel safe to show you how I am feeling, I am throwing my feelings at you to hold. • I cannot hold your stuff and your feelings, it is too much and triggers my own feelings of fear, failure, overwhelm…… therefore I am finding it more difficult to manage your behaviour as my emotions have been activated. • Co-regulating and holding children in our window of tolerence

What can we do…. . Trauma Informed School, Trauma Sensitive School, Attachment Aware School – Beacon House resources, Whole School Trauma and Attachment training Teach with an awareness that provides support and understanding for all children (Sitler, 2008). Evidence suggests that having a teacher who understands the impact trauma has on a child is already a positive strategy to facilitate a healthier, calmer, happier learning environment. Shield, look after ourselves and know our triggers. Self care and self awareness are the most important part of what we do. Links to development of our emotional intelligence. Build relationships – everything you are already doing. Keep going and know it’s working. Traumatised children need relationships to heal. But remember we cannot replace a primary caregiver and make things all better. Model self regulation and repair (attachment needs rupture and repair) Boundaries – strong, consistent, nurturing boundaries. Disorganised attachment often needs drawstring boundaries. Keep understanding what might be happening in their brain, keep wondering what might be happening for them. This allows us to think outside the box and an insight into their inner world that drives their behaviour. Shame is toxic – it increases negative behaviour – avoid at all costs PACE – Playful, Accepting, Curious and Empathic (Dan Hughes 2009) – four essential attitudes to hold when relating to children Refer to therapy – play therapy- it calms the amydga! Family therapy, Counselling, Camhs. Access support and supervision including peer supervision. Slow down – have a mental health plan, get background information, parental consent, review, refer on. Mindfulness Keep filling in Child Protection concern forms – referrals to Childrens Services and Early Help Provide vulnerable children with daily access to at least one named, emotionally-available adult, who believes in them, relates to them with compassion, empathy and positive regard, provides appropriate limit setting, understands their attachment and mental health needs, knows their life story, and offers repeated enriched relational, regulatory and reflective opportunities. For example Potters Gate Champions Catch children as they are ‘falling’ not after they have fallen. When the child is experiencing a painful life event, the emotionally-available adult/s will help them process, work through and make sense of what has happened, rather than waiting until the pain of the trauma has transformed into challenging behaviour and/or physical and mental health problems. ELSA, HSLW, Therapist, Champion, Early Help Staff training that includes trauma awareness, good listening, understanding and finding the words to convey accurate empathy. Whole school inset training including trauma awareness, attachment, a script to support? Hot topics and CP A commitment to relating to children in a school in ways that help them feel calm, soothed and safe, instead of over- stimulated, bombarded anxious. Includes environment for example nurture group. Staff/adults interacting with all children in such a way that they feel valued as individuals throughout their day Staff/adults adjusting their expectations of vulnerable children to correspond with their developmental capabilities and experience of traumatic stress. The emotional well-being and stress regulating of staff is treated as a priority. This is to prevent burnout, stress-related absence, and staff leaving the profession through stress-related illness or secondary trauma. PSHE lessons

• Safeguarding Hot Topic – Health Warning • This can be a difficult topic and there may be some of us in the room who have witnessed domestic violence or been a victim of domestic violence. Look after yourselves and seek support or time out if required • The terms domestic violence and domestic abuse have the same meaning and are interchanged in this presentation. Domestic Abuse Impact on children

Any incident or pattern of incidents of controlling, coercive or threatening behaviour, violence or abuse between those aged 16 or over who are or have been intimate partners or family members regardless of gender or sexuality. This can encompass but is not limited to the following types of abuse: • psychological • physical • sexual • financial Domestic Violence Definition • emotional Controlling behaviour is: a range of acts designed to make a person subordinate and/or dependent by isolating them from sources of support, exploiting their resources and capacities for personal gain, depriving them of the means needed for independence, resistance and escape and regulating their everyday behaviour. Coercive behaviour is: an act or a pattern of acts of assault, threats, humiliation and intimidation or other abuse that is used to harm, punish, or frighten their victim. ” * This definition, which is not a legal definition, includes so called ‘honour’ based violence, female genital mutilation (FGM) and forced marriage, and is clear that victims are not confined to one gender or ethnic group. (Home Office 2013) Strangulation and rape are high risk factors for homicide.

Statistics • Will affect 1 in 4 women and 1 in 6 men in their lifetime • Leads to, on average, two women being murdered each week and 30 men per year • Accounts for 16% of all violent crime (Source: Crime in England Wales 04/05 report), however it is still the violent crime least likely to be reported to the police • Has more repeat victims than any other crime (on average there will have been 35 assaults before a victim calls the police) • Is the single most quoted reason for becoming homeless (Shelter, 2002) • In 2010 the Forced Marriage Unit responded to 1735 reports of possible Forced Marriages. • In addition, approximately 400 people commit suicide each year who have attended hospital for domestic abuse injuries in the previous six months, 200 of these attend hospital on the day they go on to commit suicide

Statistics for our children and young people • Around 1 in 5 children have been exposed to domestic abuse. • Domestic abuse is a factor in over half of serious case reviews • The definition of domestic violence in England Wales was expanded in March 2013 to include victims aged 16 and 17 years old. It also now includes controlling behaviour and coercive behaviour. • A third of children witnessing domestic violence also experienced another form of abuse. • 1 in 5 teenagers have been physically abused by their boyfriends or girlfriends. • 130, 000 children live in households with high-risk domestic abuse. • Children exposed to domestic violence are more likely to have behavioural and emotional problems.
Impact of domestic abuse on children and young people Womb – 1 year 2 -5 years old 5 -9 years old 9 -13 years old Teenagers Link to Trauma, Attachment and Neuroscience

What can we do? • The longer children remain within unsafe and abusive situations, the more complex their needs can be. Early intervention and support can minimise risks of domestic abuse to children and young people. • Always report any disclosures of domestic abuse to your DSL. A referral to the MASH should be made. • The emotional abuse caused by witnessing domestic violence can be serious enough to meet thresholds and a child be placed on a child protection plan or protected legally. • Signpost victims and survivors to outreach services. Refer children to therapeutic support. • Do not work with perpetrators of domestic abuse – this must be done by trained services like probation.
- Slides: 52