Mental Health System CNA 2 OSBN Curriculum Mental

Mental Health System CNA 2 OSBN Curriculum


Mental Health �Level �WHO of Psychological Well-being ◦ State of Well-Being ◦ Individual realizes own abilities ◦ Cope W/stresses ◦ Work Productively ◦ Contribute to their Community

Mental Illness �Significant ◦ Thinking ◦ Feeling ◦ Behavior �Bad Enough Changes in ◦ Affecting Functioning ◦ Cause Distress to self/others

Anxiety �Uneasy Feeling ◦ Discomfort ◦ Dread �Source Unknown �Feeling Apprehensive �Anticipation of Danger
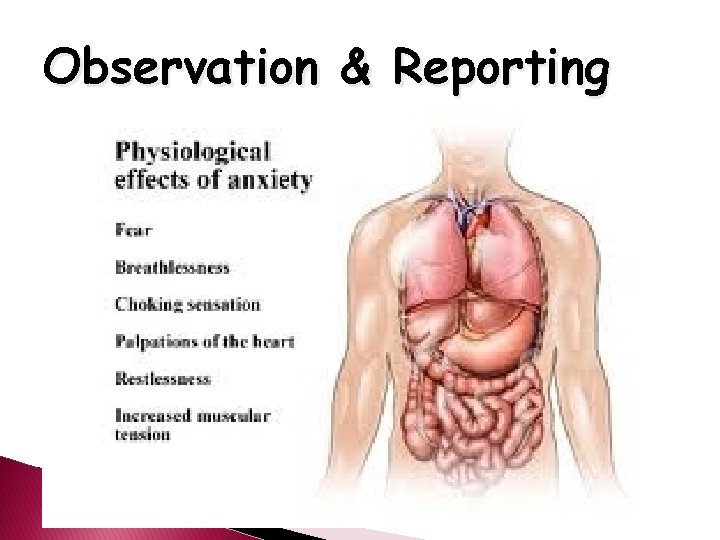
Observation & Reporting

Depression �Related to Life Events ◦ Excessive Sadness ◦ Hopelessness �Meds in a Crisis �Counseling in a Crisis �May not be r/t Life Events �Can be Severe and Persistent

Clinical Depression �Very Common Mental Illness �Familial �Women > Men �Most Frequent among Elderly �Contributing Factors ◦ Chemical Imbalance in Brain ◦ Low Self-Esteem ◦ Poor Coping Skills ◦ Hormonal Changes

Observation & Reporting �Loss of Interest �Feelings of ◦ Sadness ◦ Anxiousness �Sleep Issues �Restlessness/Irritability �Guilt/Worthlessness �Thoughts of Death/Suicide

Post Traumatic Stress Disorder PTSD � Intense Distress �Psychologically Traumatic Event

Observation & Reporting �Horrifying Memories �Recurring Fears �Flashbacks

CNA 2 Actions �Report Abnormal S&S to Nurse �Emotional Support �Calm Environment �Spend Extra Time

Suicide �Taking One’s Life ◦ Intentionally ◦ Voluntarily Observations & Reporting � Changes in Behavior or Mood

CNA 2 Actions �Report Abnormal S&S to Nurse �Close, Continual, Visual Observations

Addiction �Compulsive �Substance ◦ Alcohol ◦ Drugs ◦ Tobacco �Behavior ◦ Gambling ◦ Video Game & Maladaptive Dependence

Alcoholism �Chronic Disease (Progressive) �Can be Fatal �Impaired Control over Alcohol �Dependence & Tolerance �Remissions and Relapses �Psychological Features ◦ Preoccupation ◦ Denial of Addiction �Major Threat to Health in U. S.

Alcohol Withdrawal � Neurological, Psychiatric & Cardiovascular S&S in a person accustomed to consuming lg quantities of ETOH suddenly abstains � A Predictable Pattern � 12 -48 hrs Post Consumption Begins ◦ May have a seizure � May last up to 96 hours

Observation & Reporting �Tremor �Weakness �Sweating �Hyper-Reflexia �GI Symptoms ◦ N/V �Hallucinations

Delirium Tremens: DTs �Severe Withdrawal Syndrome �Hallucinations ◦ Visual ◦ Auditory ◦ Tactile �May be Threatening � 15% may Die �Recovery: 3 -5 days

Observation & Reporting �Anxiety Attack �Restlessness �Increasing Confusion �Disorientation �Profound Depression �Hyperactivity ANS ◦ Tachycardia ◦ HTN ◦ Profuse Sweating

Delirium �Temporary State of Confusion �Acute Onset �Sx of Underlying Disorder ◦ Infection ◦ Dehydration ◦ Fever ◦ Low Sodium (Electrolyte) Level �Side Effect of Meds �Remove Cause/Delirium Resolved

Observation & Reporting �Loss or Decreased Orientation �Lack Attention �Memory Issues �Sometimes: Tremors

Dementia �Memory Impairment �Attention Problems �Inability to ◦ Learn New Info ◦ Recall Old Info

CNA 2 Actions �Report Abnormal S&S to Nurse �Follow Pt. ’s Care Plan �Safety �Normal Routine �Stimulation �Don’t Argue �Clear, Simple, Directions �Emotional Support �Encourage PO Fluids

Eating Disorders Bulimia Nervosa Anorexia Nervosa

Anorexia Nervosa �Excessively Thin �See Themselves as Overweight �Exercise Excessively

Observation & Reporting �Loss of Appetite �Skips Meals �Takes Tiny Portions �Excuses for not Eating �Low-Calorie Foods

Bulimia Nervosa Binging �Eat Huge Amount of Food Purging � Induce Vomiting/Laxatives �Focused on ◦ Body Wt. ◦ Shape ◦ Feels Excessively Overwt.

Observation & Reporting �Abnormal Eating Patterns �BR Immediately after Meal

CNA 2 Actions �Report Abnormal S&S to Nurse �Encourage Frequent, Small Meals �Emotional Support �Monitor Food Intake

Personality Disorders �Pathological ◦ Perception ◦ Communication ◦ Thinking Disturbance of Patterns of �Impairing Ability to Function Effectively �At Least 2 of: ◦ ◦ Cognition Affect Interpersonal Functions Impulse Control �Onset Can be Traced to Adolescence

Observation & Reporting � 10 Different Categories �Odd/Eccentric Behavior �Overly Emotional �Dramatic �Tense �Anxiety-Ridden

Psychosis �Loss of Contact w/Reality ◦ Delusions ◦ Hallucinations �Causes: ◦ ◦ ◦ ETOH/Drugs Brain Tumors Dementia Epilepsy Psychotic Depression �Examples: Schizophrenia & Bi-Polar

Schizophrenia �Thought Disorder � 1% of Population �Marked by ◦ Delusions ◦ Hallucinations ◦ Disorganized Speech/Behavior �Flat Affect �Social Withdrawal

Bi-Polar: Manic Depression �Causes Mood Swings ◦ Excessive Happiness ◦ Excessive Sadness

Observation & Reporting �Confusion �Depression �Disorganized ◦ Thought ◦ Speech �Delusions �Loss Touch w/Reality �Illusions �Unfound Fear/suspicion

CNA 2 Actions �Report Abnormal S&S to Nurse �Consistent Approach

Mental Health Scenarios

Just as CPR helps you assist an individual having a heart attack — even if you have no clinical training — Mental Health First Aid helps you assist someone experiencing a mental health related crisis.

Mental Health First Aid � � � http: //www. youtube. com/watch? v=ffl. Qf-T 155 o http: //www. youtube. com/watch? v=RVk 5 QM 6 Qwt. Q&list=PLHt 1 em. At. Prf. Iw. Hmg. Wj 2 Ber. CWRc FH 72 Zy. C http: //www. youtube. com/watch? v=w. SAq 7 Rwuh. Gs


Assess for risk of suicide or harm When helping a person going through a mental health crisis, it is important to look for signs of suicidal thoughts and behaviors, non-suicidal self-injury, or other harm. Some warning signs of suicide include: � Threatening to hurt or kill oneself � Seeking access to means to hurt or kill oneself � Talking or writing about death, dying, or suicide � Feeling hopeless � Acting recklessly or engaging in risky activities � Increased use of alcohol or drugs � Withdrawing from family, friends, or society � Appearing agitated or angry � Having a dramatic change in mood � Always seek emergency medical help if the person’s life is in immediate danger.

Listen nonjudgmentally It may seem simple, but the ability to listen and have a meaningful conversation requires skill and patience. Listening is critical in helping an individual feel respected, accepted, and understood. Use verbal and nonverbal skills such as open body posture, comfortable eye contact, and other strategies to engage in appropriate conversation.

Give reassurance and Information It is important to recognize that mental illnesses and addictions are real, treatable illnesses from which people can and do recover. When talking to someone you believe may be experiencing symptoms of a mental illness, approach the conversation with respect and dignity and don’t blame the individual for his or her symptoms.

Encourage appropriate professional help There are many professionals who can offer help when someone is in crisis or may be experiencing the signs and symptoms of a mental illness or addiction. Types of Professionals Doctors (primary care physicians or psychiatrists) Social workers, counselors, and other mental health professionals Certified peer specialists Types of Professional Help “Talk” therapies Medication Other professional supports

Encourage self-help and other support strategies Individuals with mental illness can contribute to their own recovery and wellness through: �Exercise �Relaxation and meditation �Participating in peer support groups �Self-help books based on cognitive behavioral therapy �Engaging with family, friends, faith, and other social networks

Suicidal Intervenions �http: //www. youtube. com/watch? v= Bqhl. GZp. EYf. Y&list=PLHt 1 em. At. Prf. I w. Hmg. Wj 2 Ber. CWRc. FH 72 Zy. C �http: //www. youtube. com/watch? v=a RV 7 d. YZNBw&list=PLHt 1 em. At. Prf. Iw. Hmg Wj 2 Ber. CWRc. FH 72 Zy. C

- Slides: 48