Mental Health Screening in Primary Care Valerie Dzubur

Mental Health Screening in Primary Care Valerie Dzubur Ed. D APRN FNP-BC

Mental Health All medical care flows through the relationship between physician (provider) and patient, and the spoken word is the most important tool Eric Cassell

Psychiatric Disorders Objectives: Identify & Rx Psychiatric disorders in Primary Care Discuss Co-morbidities

Psychiatric Disorders Depressive Disorders Anxiety Disorders Suicidal Ideation Personality Disorders The difficult patient Somatoform Disorder

Why Concerned? Prevalence of mental illness (NIMH) 22% of U. S. adults (~44 million persons) have a diagnosable mental disorder The most common problem in primary care 4 of 10 disability are mental disorder 50 % of the time depressed persons will be treated by primary care provider 80 % of Rx written by non-psychiatrist Depressed persons use 50 – 75 % more health care services than other chronic illnesses
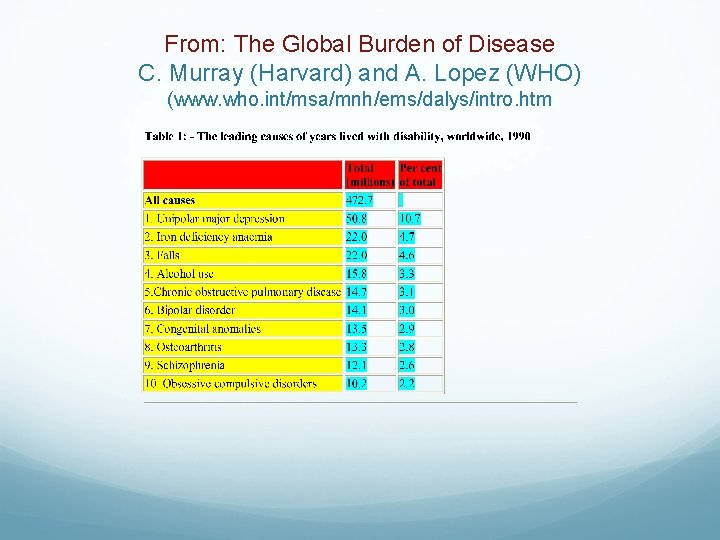
From: The Global Burden of Disease C. Murray (Harvard) and A. Lopez (WHO) (www. who. int/msa/mnh/ems/dalys/intro. htm

Psychiatric Disorders Axis I Neurosis & Psychosis A clinical disorder that can be effectively relieved with interventions Mood disorders Thought disorders Anxiety disorders

Psychiatric Disorders Axis II Personality & Developmental Disorder Long standing Ingrained in the developmental process of childhood May causes major life-long dysfunction in many spheres of life Can be difficult to treat

Primary Care Setting 74% of Americans seeking help for depression Will go to a PC provider Not a mental health professional [Montano B: Journal of Clinical Psychiatry 1994]

Primary Care Clinical Tips Anxiety and Depression hold hands Future Focused Symptoms Consider Anxiety Past Focused Symptoms Consider Depression

Primary Care Clinical Tips Anxiety and Depression hold hands Future Focused Symptoms Consider Anxiety Past Focused Symptoms Consider Depression

Primary Care Treatments Have referral information in hand Use Medications early for Symptom and Mood Management Counseling helps people Understanding the cause & meaning

Counseling Meaning is not something you stumble across, like the answer to a riddle or the prize in a treasure hunt. Meaning is something you build into your life. You build it out of your own past, out of your affections and loyalties…out of the things you believe in, out of the things and people you love, out of the values for which you are willing to sacrifice something” John Gardner

Mental Health Clinical Wisdom Medications Management A witches brew Each persons treatment is individualized Consider side effect profile Personal Goals Use different combinations of medications Creating the recipe Making a stew

Co-morbidity People seen in a PC Setting 5 - 10 % will have depression People in the hospital 10 to 14% [National Institute of Mental Health, “Co-occurrence of Depression with Medical, Psychiatric and Substance Abuse Disorders, ” http: //www. nimh. nih. gov/depression/co_occur/abuse. htm. ]

Co-morbidity There is a reciprocal relationship Between people who are depressed And the occurrence of major CV events People who are depressed are at risk for a cardiovascular event People who have a cardiovascular event are at risk for depression

Co-morbidity Heart Disease and Depression occurs in 40 to 65 % who have had an MI 18 to 20 % who have CAD W/O MI

CAD & Depression After an MI A person with clinical depression Has a 3 - 4 X > chance of death Within the next six months. [http: //www. nimh. nih. gov/depression/co_occur/heart. htm. ]

CVA & Depression occurs in 10 - 27 % of CVA survivor can last one year 15 - 40% of CVA survivors experience some symptoms of depression within two months after the stroke. [http: //www. nimh. nih. gov/depression/co_occur/stroke. htm]

CVD & Depression Reciprocal relationship Psychosocial risk factors Loss of social roles/independence after MI or CVA contributes to depression. Depression may result in impaired adherence to treatment and interfere with physical rehabilitation.

Physiology of Depression Hypercortisolemia increases the risk of arteriosclerosis. Depression is associated with increased heart rate variability (interferes with parasympathetic function) and increases the risk of arrhythmia. Depressed people have been shown to have increased platelet activation (serotonergic mechanism).

Depression & CV Disease

Depression and Diabetes People with adult onset diabetes 25% have depression. People with diabetic complication 70% have depression [Lamberg L: JAMA 1996]

Importance of Treatment People who tx for co-occurring depression An improvement in overall health Better compliance with medical care Better quality of life

Importance of Treatment 80% of people with depression can be treated Medication psychotherapy Combination of both

Importance of Treatment Early diagnosis and tx reduces Patient discomfort Morbidity Cost Suicide

ANXIETY DISORDERS

Anxiety Prevalence 2. 5 – 8% of the population Women affected twice as often as men 20 % will have co-morbid substance abuse problems A symptom A Syndrome A Disorder

Prevalence of Anxiety Common Medical Complaints Symptom Chest pain Fatigue % with Anxiety 33% 26% 28% Headache 35% Insomnia 31%

Anxiety Disorders Panic Disorder (+/- Post-traumatic Stress Generalized Anxiety Disorder Social Phobia Obsessive-Compulsive Specific Phobia agoraphobia) Disorder Secondary to a Generalized Medical Condition Substance-Induced

Medical Causes of Anxiety Endocrine: Hyper/Hypo Thyroid Pheochromocytoma Hypoglycemia Carcinoid syndrome Hypo-parathyroidism Insulinoma Cushing’s syndrome Acute intermittent porphyria

Medical Causes of Anxiety Respiratory COPD Hypoxia from any cause PE Asthma

Medical causes of Anxiety Neurological Disorders Aura of migraine Early dementia Cerebral neoplasia Delirium Partial complex seizures Demyelinating disease Post concussive disorder Withdrawal from sedativehypnotics, caffeine, or nicotine

General Anxiety Disorder Manifested by unrealistic or excessive anxiety or worry about two or more life circumstances that persists for 6 months or longer

GAD Symptoms Restlessness/nervousness Fatigue Concentration difficulties Irritability Tension Sleep disturbances

GAD Treatment Patient Education – Life style modification Avoid caffeine, nicotine, alcohol, & other stimulants Increase exercise Sleep hygiene Stress management acupressure/acupuncture, reflexology Psycho Therapy – client centered Behavior cognitive therapy Support groups Complimentary medicine, meditation, massage

Social Phobias Occurs > in women than men Crosses all social Cultural & class lines The fears are life changing

Social Phobia Symptoms include Palpitations Pounding heart Increase HR sweating trembling Chest pain Dizziness SOB Fear of dying Numbness Tingling Chills Hot flashes Nausea Vomiting Abdominal pain

Social Phobias The key behavior changes… Avoid dating Fear they will never marry Avoid classes or jobs that require working in groups

Social Phobias Decide not to go to college Avoid employment opportunities Work at a lower level than ability Avoid public places Stay at home more and more Avoid anxiety producing events

Social Phobias As social phobia worsens if begins to effect every aspect of life and leads to Depression Substance Abuse Isolation Family disruption

Social Phobias The patient’s fears direct the patients choices Limit their opportunities Spoiling their life As they adapt to accommodate the social phobia

Social Phobias Treatment Medications SSRI Name the disorder people get relief by knowing they have a recognized & treatable condition Patient education Act to rebuild self esteem Cognitive Behavior & Support Groups learn new coping skills

Social Phobias Goal of treatment Focus on small gains over time Focus to improve or minimize symptoms Avoidance behaviors
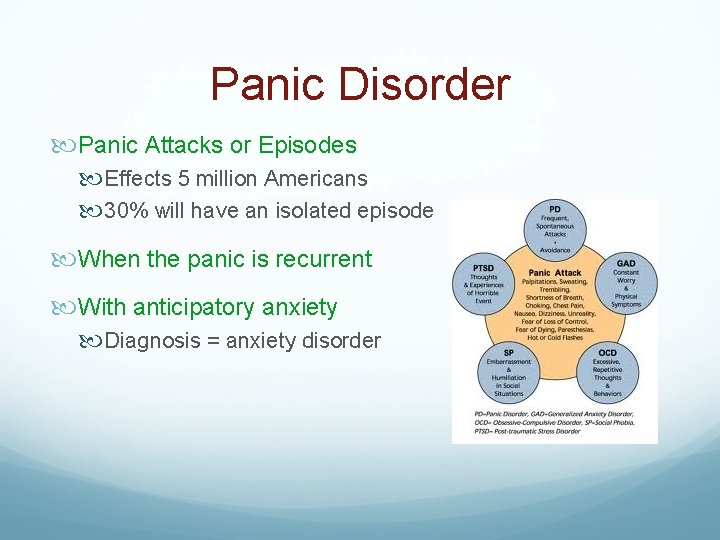
Panic Disorder Panic Attacks or Episodes Effects 5 million Americans 30% will have an isolated episode When the panic is recurrent With anticipatory anxiety Diagnosis = anxiety disorder

Panic Disorder Patients with panic disorder Discrete episodes of intense fear A sense of physical discomfort Episodes vary in frequency & severity

Panic Disorder Panic Episodes Sometimes described as a wave Happen for no apparent reason Last from 10– 30 minutes

Panic Disorder Over time the anxiety becomes pathological…

Panic Disorder The person begins avoiding the situation where the attacks first occur As more and more attacks occur There are more and more situations to avoid

Abrupt Onset 4 or > Chest Pain Sweating Nausea Trembling GI Distress Shaking Shortness of breath Palpations Increased heart rate Feels like choking Diff. breathing

Abrupt Onset 4 or > Dizzy Fear of dying Light-headed Paresthesias De-realization Chills or Depersonalization Hot flashes Fear of losing Going crazy

Panic Disorder In the Worst Case The person becomes housebound Avoiding all possible situations That might bring on an attack

Panic Disorder 50 % of the time People also suffer from depression

Treatment SSRI & SSSRNIs Benzos (? ) Client Centered counseling Cognitive Behavior Therapy Support Groups Patients Education
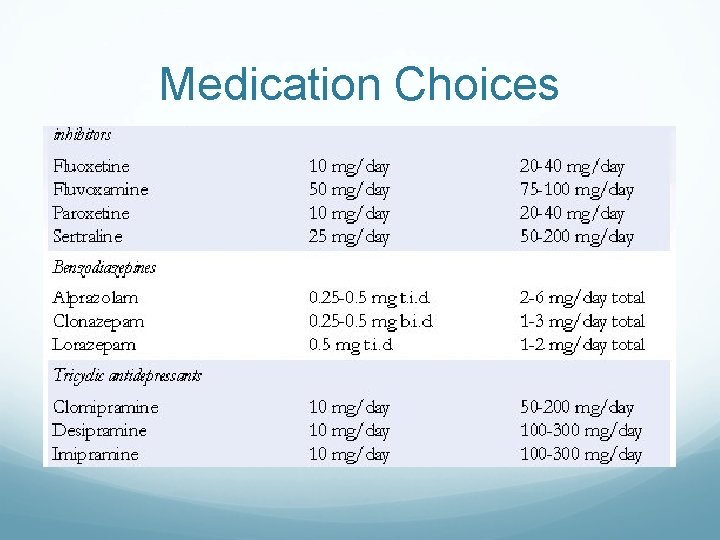
Medication Choices

OCD Reoccurring obsessions and or compulsions that are severe enough to be time consuming ( > 1 hours per day) These behaviors cause significant distress or impairment The person may recognize that the obsession or compulsion is excessive or unreasonable but they can not resist 4 th most common anxiety disorder, can begin at any age, 50 % of the time begins in childhoods

OCD At first the person can not finish anything than as things get worse the person can not start anything

OCD Obsessions Compulsions Recurrent, persistent Repetitive behaviors with thoughts, images, impulses, etc. Intrusive, inappropriate Marked anxiety/distress Not excessive real-life worries Attempts to ignore/suppress driven quality Rigidly applied rules Aimed at reducing distress or preventing a dreaded event or outcome but are unrealistic or excessive

OCD Left untreated symptoms will worsen leading to Loss of employment Isolation Depression Divorce or other family disruption

OCD - Treatment Medications are the mainstay Name the disorder SSRI - high doses Behavior focused therapy Patient Education Not a moral/character failing Relief from a sense of shame

OCD Goal gradual improvement over time as the person begins to be able to let go of unwanted thoughts You may not see any improvement from medication for 4 6 months

Traumatic Stress Disorder ATSD & PTSD Acute Traumatic Stress Symptoms < 3 months Post Traumatic Stress Symptoms > 3 months Delayed Onset Symptoms can occur 6 mos - 30 yrs

PTSD Delayed Onset The Kindling Effect The process in which repeated sub-threshold stimulation of a neuron eventually generates an action potential

PTSD The Origin is Trauma Child Abuse Beatings Sexual assault Serious accident Incurring a significant injury Sudden unexpected death Captivity War

ATSD/PTSD Exposure to a traumatic event in which both of the following were present: Events involved threat of actual death of self or other serious injury of self or other Disintegration of the integrity of self/others Response involves intense fear helplessness horror

PTSD Persistent re-experiencing of trauma (1 or more) Recurrent, intrusive images, thoughts, perception Distressing dreams, flashbacks, illusions, hallucinations Intense psychological & physical distress in response to symbolic internal or external cues

PTSD Persistent avoidance & numbing 3 or more Avoidance of thoughts & feelings Avoidance of activities, places or persons associated with or triggering recall of trauma Inability to recall important aspects of trauma Disassociation from time or place

PTSD Persistent avoidance & numbing 3 or more Diminished interest or participation Feeling detached or estranged from others Restricted affect Sense of a foreshortened future

PTSD Persistent arousal 2 or > Sleep disturbance Irritability or outbursts of anger Unstable mood Difficulty concentrating Hyper-vigilance Exaggerated startle response

PTSD Treatment The first principle of recovery is empowerment of the survivor A person must be the author and arbiter of recovery. Restoration of control

PTSD Treatment Client Center Counseling Cognitive Behavior Therapy Disclosure therapy Support Groups Complimentary Medicine < stress Patient Education

PTSD Recovery unfolds in a spiral First central task of therapy Safety Second task of therapy Remembrance and mourning Third task of therapy Reconnection with ordinary life

PTSD Pharmacotherapy Mood Stabilizer Anti-anxiety Rx with caution Sedative hypnotics Rx with caution Buspirone (Bu. Spar) Antidepressants

DEPRESSION

Major Depression At least 4 of the following present for at least 2 weeks Low mood Anhedonia Poor concentration Low energy Guilt or worthlessness Pessimism or hopelessness Sleep disturbance Agitation or retardation Appetite disturbance Loss of libido Suicidal ideation

Depression Screening SALSA Sleep disturbance Anhedonia Low Self esteem Appetite decreased 97% sensitivity 94% selectivity (Brody, Arch Int Med, 1998)

Depression Screening SIG-E-CAPS Energy decreased Depressed Mood Plus: Concentration difficulties Sleep decreased Appetite disturbance or Interest decreased in Psychomotor activities (Anhedonia) Guilt or worthlessness (Not a major criteria) weight loss retardation/agitation

Pharmacology SSRI SSRNI TCA Mood Stabilizer Sleeping Meds Anti-psychotics Atypical More than One Rx

TCAs Avoid the use of TCAs with co-morbid CV “Dirty”- non-selective with many side effects Altered cardiac conduction increases risk of arrhythmia. (Class I anti-arrhythmic effect) Orthostatic hypotension (alpha-adrenergic) Exacerbation of hypertension (noradrenergic)

TCAs Clomipramine (Anafranil) Class TCA Starting does 25 – 50 mgs Dosage Range 100 – 250 mgs Approved of OCD

SSRI Selective Serotonin Reuptake Inhibitors 2 D 6 inhibitors Citalopram, Sertraline, Fluoxetine, Paroxetine, Escitalopram Weight gain, sleep disturbance, sexual dysfunction, may reduce platelet aggregation.

SSRI Clinical Tip: They will all work Think about the side effects Consider Escitalopram for crying They all cause sexual dysfunction Consider a lower dose Drug Holidays Check Akathisia Avoid in bi-polar can cause mania

SSRI Fluvoxamine (Luvox) Class SSRI Starting dose 25 – 50 mgs Dosage Range 100 – 300 mgs Approved for OCD SAD depression Careful management of interactions

SSRI Paroxetine (Paxil) Starting dose 10 – 20 mgs Dosage Range 40 – 60 mgs Approved for PD OCD SAD depression

SSRI Sertraline (Zoloft) Starting dose 25 mgs Dosage Range 50 – 200 mgs Approved for PD OCD (adults children) PTSD depression

SSRI Fluozetine (Prozac) Starting Dose 10 – 20 mgs Dosage Range 20 – 80 mgs Approved for OCD anxiety depression

SSRNI Venlafaxine - Effexor 37. 5 - 150 mgs May exacerbate HNT Take at the same time each day, don’t miss a dose Taper to discontinue or use prozac Cymbalta - Duloxetine HCL 20 - 60 mgs May exacerbate HNT If diabetic monitor glucose

Other Buspar Class azapirones Starting dose 15 mgs Dose Range 15 – 60 mgs Therapeutic Response 3 – 6 weeks

Other Beta Blockers Inderal 10 – 20 mgs TID or QID Metoprolol 25 – 50 mgs BID Atenolol 50 – 100 mgs QD Careful history and assessment of B/P, HR, Lungs, History of CHF, arrhythmia, COPD, Asthma

SDRI Bupropion (Wellbutrin) 150 - 300 mgs Reduce seizure threshold dose related Activating, smoking cessation Use for couch potatoes and grazers

Serotonin Syndrome A potentially fatal toxic encephalitis Confusion Agitation Rigidity Hyper-reflexia Fever Hyperthermia

Serotonin Syndrome Usually a drug interaction that raises the blood level of serotonin Needs hospitalization for support Check medication profile for drug interactions Any selective 5 HT receptor antagonist for example Zofran

Tetracyclic Mirtazipine (Remeron) 15, 30, 40 mgs Causes weight gain Good for sleep Good for nausea

Triazolopyridine Trazadone 50 -300 mgs Good for sleep Good for alcoholics - not addictive Priapism Avoid with an acute MI Urinary Retention

Suicide Annual suicide rate (U. S. ) = 11. 2/100, 000 9 th leading cause of death

Suicide Risk Factors Socio-demographics Elderly (men>70 years) Unmarried Native American or Caucasian Male (white men = 70% of U. S. suicides) Living alone Increasing rates among adolescents

Suicide Risk Factors Recent stressors Health, Financial Marital, Family Legal, Occupational Psychiatric disorder Depression Anxiety (panic) Schizophrenia Bipolar Disorder Personality disorder Alcohol/drug use Command Hallucinations Previous attempts Family history

Suicide Risk Assessment Ask about suicidal ideation Check for risk factors Listen to comments about suicide If the patient discusses Putting affairs in order Care of pets Other cues and clues

Suicide Risk Assessment If patient responds positively Do you have a plan How would do this Are there means available Have you rehearsed or practiced How strong is your intent Do you tend to be impulsive Can you resist the impulse

Suicide Risk Assessment Suicide Contract Dependent on the strength of relationship Agreement to call provider Use support system, resources, suicide prevention Inform family, significant other, close friend Close follow-up Referral to mental health provider If unable to contract or at imminent risk refer for emergency psychiatric assessment.

Suicide Risk Assessment When treating a patient for depression The risk for suicide may increase In the early phase of treatment As the patient’s energy levels lifts. The patient simply develops enough New energy to carry out a plan

BIPOLAR DISORDER

Bipolar Disorder Manic Episode: A. elevated, expansive, or irritable mood, lasting at least 1 week B. three (or more) of the following symptoms C. inflated self-esteem or grandiosity D. decreased need for sleep E. Hyper-verbal or pressured speech

Bi-Polar A. insomnia or hypersomnia B. psychomotor agitation or retardation C. flight of ideas or racing thoughts D. distractibility E. increase in goal-directed activity at work or psychomotor agitation F. excessive involvement in pleasurable activities that have a high potential for painful consequences

Bipolar Disorder 25% suicide attempt w/o treatment 15% successful attempt Recurrent illness 80 -90% Repeat events-progressive deterioration Untreated 9 year < in life expectancy 14 year < in productivity Treatment > 6. 5 - 10 yrs

Variations of Bipolar Disorder Bipolar I=periods of mania +/- depression Bipolar II=periods of depression/hypomania Mixed states=periods of mania & depression Rapid Cycling = 4 episodes in 12 mos More common in bipolar II

Pharmacotherapy Lithium Anticonvulsants Atypical antipsychotics Traditional antipsychotics Antidepressants

Mood Stabilizers Lamictal 12. 5 - 200 mgs bid Stop for any rash (life threatening) Raise dose q 2 weeks 25 mgs Trileptal 150 - 600 mgs bid Small dose in am Larger dose in pm

Single Agent Therapy Mood Stabilizer May use a higher dose

Adjunctive Therapy When one medication is not enough Mood instability at the end of the day Break through symptoms Nothing works Stopped working Medication failure New symptoms

Adjunctive Therapy Add a mood stabilizer Depakote 125 - 1500 mgs bid blood level, Liver Function Lithium 300 - 600 bid blood levels, narrow therapeutic range Lamictal 12. 5 - 200 mgs bid

Adjunctive Therapy Add a mood stabilizer Topomax 25 - 100 mgs bid may cause glaucoma, expensive Trileptal 1200 - 1500 mgs bid Tegretol 100 - 1200 mgs bid blood levels, interactions Zyprexa 2. 5 - 5 mgs bid Weight gain diabetes

Adjunctive Therapy Add an antipsychotic Navane 5 mgs bid Trilafon 2 - 8 mgs bid Abilify 5 - 20 mgs qd

Adjunctive Therapy Add an antipsychotic Seroquel 25 mgs bid Risperdal. 25 -. 5 mgs bid Geodon 40 mg - 60 mgs bid

Adjunctive Therapy Titrate the dose up according to the patient’s mood q 1 - 2 weeks Need a lower dose as adjunctive When stable consider QD dosing Change to HS is sleepy Change to am if activated If suddenly can’t sleep change dose earlier in the evening

Changing medications Taper one medication Start new medication low & slow Increase dose every 3 - 4 days Use Prozac 20 mgs for self taper off of SSRI Listen to your patient

The Frustrating Patient

The Frustrating Patient As the Provider you may experience: You’re working hard but getting no where 4 or more problems vaguely or unrelated Everything has been tried – nothing worked Consider the diagnosis of Personality Disorder

The Frustrating Patient 15% or more of patients (Hahn et al J Gen Intern Med, 1996) Overly dependent, “clinging” Demanding “entitled” “manipulative, unwilling to accept recommendations “self destructive” (Groves, NEJM, 1976) Consider personality disorder

Personality Disorders Characterized by chronic Rigid maladaptive behaviors Persons with personality disorders may appear odd or eccentric cluster A dramatic, emotional, or erratic cluster B anxious and fearful cluster C

Personality Disorders Personality disorders frequently co-occur with other psychiatric & substance use disorders depressed, emotionally labile, & prone to suicidal ideation High users of medical and psychiatric services

Treatment Severe disorders require referral to mental health services. Treatment includes psychotherapy medication for depression

The Frustrating Patient Self-awareness: acknowledge frustration Verbalize concerns Allow more time Schedule regular f/u visits Set limits Cultivate participation & Monitor for “burn-out” Seek consultation partnership

Dialectical Behavior Therapy Developed in the 1980’s by Dr. Linehan Emphasis Acceptance that encourages change Firmness with flexibility Nurturance with benevolent demands Non-re-enforcement of self destructive behaviors Patient completes behavior change analysis

DBT Developed out of research on suicidal behavior Combines Western and Eastern points of view Radical acceptance Self Responsibility for change

Somatoform Disorder Physical complaints can not be completely or adequately explained by a general medical condition substance abuse mental disorder

Somatoform Disorder Symptoms must be Clinically significant Cause distress Functional impairment Symptoms are not intentional

Unexplained Symptoms Disorders Include Somatization Disorder Undifferentiated somatoform disorder Conversion disorder Pain disorder Hypochondriasis Body Dysmorphic Disorder Somatoform disorder See hand out

Unexplained Symptoms There are no specific Dx or Rx Standard medical evaluation assess for treatable cause

Unexplained Symptoms Considerations History of sexual/physical abuse Consider Hypochondriasis

Unexplained Symptoms Use primary care management principles Scheduling regular brief visits Avoid many tests and subspecialty referrals Avoid disputing the realty of the complaint Use symptom management Give reassurance Listen Be flexible

Unexplained Symptoms Consider Cognitive Behavior Therapy Utilize complementary and alternative medicine intervention Aim for function not disability Time management Reassurance Avoid saying nothing is wrong

Unexplained Symptoms Reassurance can include Legitimize the suffering Explain symptoms without tests Symptoms are non-progressive Expect gradual improvement

Unexplained Symptoms Consider neurological symptom consider conversion disorder Unexplained pain Consider pain disorder Multiple Unexplained symptoms undifferentiated somatoform disorder somatization disorder

Unexplained Symptoms If suspect symptoms are intentionally feigned Malingering or Factitious Disorder To note in the record unexplained medical complaint

Motivational Interviewing Why Respectful Accepts The Client Encourages Self Responsibility Mobilizes Inner Resources

Motivational Interviewing Motivation is a key to change Motivation is multidimensional Motivation is a dynamic and fluctuating state Motivation is interactive The clinician’s style influences the client’s motivation

Motivational Interviewing In contrast with confrontational/denial A label is not necessary Focus on personal choice (does not force disease model Elicits client’s concerns instead of telling the client what to be concerned about Resistance is seen as interpersonal, influenced by therapist/NP Resistance is met with reflection, not argument

Motivational Interviewing As the interviewer you want to Develop Discrepancy Avoid Argument Roll with Resistance Express Empathy Support Self Efficacy Used along with the stages of change model can be a very effective method to support people with making changes in their lives

Motivational Interviewing Strategies of motivational interviewing might include Focus on the person’s strengths Respect their autonomy and decisions Individualize/patient centered treatment Avoid labels - they are dehumanizing Develop a therapeutic relationship Focus on early interventions or less intensive treatments

Motivational Interviewing Is a therapeutic style or way of interacting with people that facilitates an exploration of stage-specific motivational conflicts that can that hinder future progress

Motivational Interviewing Successful motivational interviewing includes being able to Express empathy through reflective listening Communicate respect and acceptance of the person and their feelings Establish a nonjudgmental, collaborative relationship Be supportive a knowledgeable consultant Compliment rather than denigrate

Motivational Interviewing Listen rather than tell Gently persuade with understanding Develop discrepancy Between the person’s goals/values & behavior Support people to recognize the discrepancies Between where they are and where they hope to be.

Motivational Interviewing Tip Treatment Improvement Protocol U. S Department of Health and Human Services National Clearinghouse for Alcohol and Drug Information DHHS Publication No. (SMA ) 02 -3629 1 -800 -729 -6686 1 -301 -468 -2600
- Slides: 144