MENTAL HEALTH IS EVERYONES RESPONSIBILITY Delivered by Simone

MENTAL HEALTH IS EVERYONE'S RESPONSIBILITY. Delivered by Simone Taylor RMN

Aims of this session ■ To help you understand what is meant by “mental health”. ■ To give knowledge that instils confidence when assisting with the treatment of, or leading the treatment of someone with a mental illness. ■ To use what you know now, and the experiences you’ve had to inform the development of your knowledge and application of skills. ■ To improve the treatment of those with a mental illness while under the care of a physical health practitioner in acute and community settings.

You ■ What do you know about mental health ■ What do you worry about when treating someone with a mental health problem? ■ What do you want gain from today?

What experiences have you had?

What is Mental Health? ■ Mental health is defined as a state of well-being in which every individual realizes his or her own potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to her or his community (WHO, 2018) ■ Our mental health affects how we think, feel, act and interpret the world around us. We are all vulnerable to having our mental health becoming fragile at one point or another in life. The stress vulnerability model is one of the easiest ways to explain how we may become increasingly vulnerable to our mental health breaking down. ■ Mental health is something we all have. It is a continuum and can change depending on our individual vulnerabilities, life and social stressor. ■ Our mental health is considered to be poor when our ability to function in daily tasks is affected or altered. ■ 1 in 4 people will suffer poor mental health The World Health Organisation, 2018

Causes of Mental Health Illness ■ Trauma ■ Life event ■ Stress ■ Predisposed – genetic ■ Breakdown of marriage/loss of job ■ Bereavement ■ Substance abuse ■ Homelessness
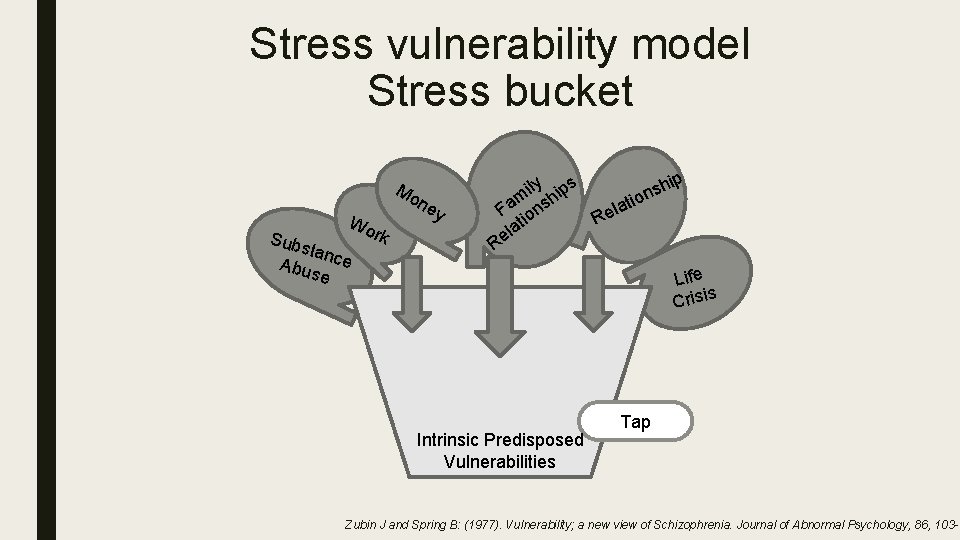
Stress vulnerability model Stress bucket Mo Wo rk Sub stan Abu ce se ne y ip h ily ips s m sh ion t a a l F ion e R t la e R Life s Crisi Intrinsic Predisposed Vulnerabilities Tap Zubin J and Spring B: (1977). Vulnerability; a new view of Schizophrenia. Journal of Abnormal Psychology, 86, 103 -1

What are the different types of mental health illness’s, how do they affect people and what are there symptoms

Schizophrenia ■ 1 in 100 people live with a diagnosis of schizophrenia, ■ Life long illness / SMI – Serious Mental Illness ■ Characterised by a cluster of negative and positive symptoms. ■ Positive symptoms: things that people without this illness do not experience; hallucinations – 5 types, delusions, thought disorder, poverty of speech ■ Negative symptoms: things that a person has ceased to do. self neglect, social withdrawal, poverty of speech, flattened affect. ■ Antipsychositc medications that may be used in treating the symptoms of schizophrenia – Clopixol , Paliperidone, Olanzapine, Aripiprazole, Clozapine, Haldol, Halperidol. ■ CBT is also part of the NICE pathway, along with family interventions and physical health monitoring and interventions.

Psychosis ■ ■ ■ 0. 07% or 4, 6000 of the UK population have psychosis. ■ ■ A recurrent psychotic disorder – more than one episode 70% of the British public have had a ‘hearing voices’ experience. Prodromal period – before a psychotic episode A blip – 1 -4 day episode A psychotic episode – a prolonged period of both negative and positive symptoms effecting the individuals daily function. Characterised by positive and negative symptoms May not be life long illness. Symptoms of psychosis may also be seen in Bipolar disorder, Borderline personality disorder and obsessive compulsive disorder. ■ Medications to treat are much the same as schizophrenia. A mood stabiliser or antidepressent may be added if there is a depressive presentation that would benefit from a mood stabiliser or SSRI. ■ CBT is also part of the NICE pathway, along with family interventions and physical health monitoring and interventions.

What’s it like to hear voices? ■ https: //www. youtube. com/watch? v=0 vv. U-Ajwbok

Bipolar disorder ■ 1 in 100 people live with this diagnosis ■ Once known as Manic Depression ■ Characterised by prolonged periods of extremely low mood and with comparably shorter periods of elation and mania. ■ Bipolar type 1 – severe mania ■ Bipolar type 2 – hypomania ■ Usually a pattern to manic episode – mixed cycle and rapid cycle. Some OTCs such as St Johns wart can have a negative effect on Bipolar, and may cause hypomania in untreated Bipolar. ■ Medications used to manage Bipolar – antipsychotics such as ; risperidone, quetiapine, olanzapine, aripiprazole. Mood stabilisers such as; lithium and valproate

Personality disorder ■ 1 in 10 people live with this diagnosis ■ The ICD 10 reports 10 types of personality disorder; ■ Suspicious – paranoid, schizotypal and antisocial. ■ Emotional and impulsive – borderline, histrionic and narcissistic. ■ Anxious – avoidant, dependent and obsessive compulsive. ■ No single medication is used to manage the disruptive symptoms of a personality disorder. ■ Borderline Personality Disorder is most common in women, around 70% of those with the diagnosis are female. ■ Diagnostic criteria for BPD has 9 characteristics, 5 must be present along with – a real or perceived fear of abandonment and marked impulsivity from early adulthood – risk.

Anxiety and Depression ■ 17. 8% of the population in the UK – live with these conditions ■ Some symptoms of anxiety often include; physiological symptoms, panic, avoidance, catastrophising, withdrawal, self neglect in severe cases. ■ 5 types of anxiety – GAD, Phobias social anxiety, panic disorder and PTSD ■ Some symptoms of depression may include; low mood persistent consistently for 2 weeks, self neglect, social withdrawal, hopeless and or helpless. ■ First line medical treatment may be in the form of an undepression or an antianxiety medication. ■ Antidepressants may take up to 6 weeks to reach therapeutic effect. ■ Once therapeutic effect has been reach, this is when a person needs extra monitoring. ■ Antidepressants – duloxetine, fluoxetine, venlafaxine, sertraline , citalopram. ■ Anti-anxiety medications – all the pams! Clonazepam, diazepam, lorazepam. ■ CBT, psychoeducation group therapy, and IAPT pathways are recommended therapies for depression and anxiety types.
![Obsessional Compulsive Disorder [OCD] ■ 12 in ever 1000 people live with this condition Obsessional Compulsive Disorder [OCD] ■ 12 in ever 1000 people live with this condition](http://slidetodoc.com/presentation_image/9591c40a2a3f8336f79007f31980ca71/image-15.jpg)
Obsessional Compulsive Disorder [OCD] ■ 12 in ever 1000 people live with this condition ■ A obsession ■ A compulsion ■ Medication/therpy to treat/manage; ■ Antidepressant, Anti-anxiety medication, , Antispychotics, Beta Blockers ■ CBT , Exposure and Response Prevention [ERP]

Eating disorders ■ Anorexia nervosa ■ Bulimia ■ Binge eating disorder ■ ‘Other specified feeding or eating disorder’ ■ Orthorexia – preoccupation with ‘clean/healthy’ foods ■ Avoidant/Restrictive Food Intake Disorder – foods limited due to appearance/taste/texture/brand etc ■ Diabulimia – restriction of insulin for the purpose of weightloss ■ In the UK we have 1. 6 million people with a diagnosed ED ■ No one medication or treatment is used to treat an eating disorder. ■ Supplements, strict eating regime (inpatient), weekly weigh ins, psychological interventions.

Child and Adolescence Mental Health Services ■ Suicide ■ Depression ■ Self harm ■ Anxiety ■ Eating disorder ■ OCD ■ Psychosis ■ ADHD & ADD. ■ 284, 599 young people are in contact with MH service under age of 19

Self harm and suicidal thoughts ■ Around 20% of adults experience suicidal thoughts ■ 6. 7 % of those attempt to take their life ■ 6133 suicides record in 2014 age 10 and above ■ 7. 3 % self harm – 1 in 15 people ■ 66. 9% do not seek help for self harm ■ Under 19 s – 12. 1% had self harmed at some point ■ Accurate figures? ■ Types of self harm : cutting , burning, ligitures, swallowing foreign objects , inserting foreign objects , punching , restricting food or food groups , alcohol and drug abuse , self exposed sexual vulnerability. Figures taken from the Fundamental facts about mental health (2016) from www. mentalhealth. org. uk

What is A&E like for a Mental Health service user? “You are told to sit on a chair or if your lucky a bed, then you are left there for ages, no one popping over every so often to check if your ok like they do those are in with a physical illness. Is it any wonder we either don’t want to attend A&E and have to be dragged there. I have run off at times and had to be brought back by the police or security” “A&E makes you very anxious and the staff don’t get that. A&E is not a nice place to go when your struggling with your mental health, everyone makes you feel like your just wasting their time “ Pseudonyms have been used to protect the identity and retain anonymity of the individuals throughout this presentation, in line with NMC confidentially requirements. (NMC, 2015)

Scenario A 14 year old comes into the A&E department with ongoing stomach pain. You are the nurse in charge of their care after triage. Parents are around but have stepped out to call family/work. The 14 year old then discloses to you that they have recurrent thoughts of harming themselves. So now think about how you would deal with this situation, what skills you may need to apply, and what you may need to consider in you care of this minor.

Points to consider: o Do you want to deal with this situation? o What is your gut telling you? o Admission to paediatric ward for psychiatric assessment? o Disclosing information to parents who are not present? o Safeguarding referral ? o Risk ? o How comfortable do you feel with dealing with this patient? – Very comfortable, unsure, uncomfortable, very uncomfortable.

Non-prescriptive answer to scenario 1 o o o o o Take a minute to digest the information , reflect and speak to colleagues Validate the disclosure facial expressions and body language. confidentiality Find out more about the girls current life Intent behind thoughts Explore current risk - have they already self harmed? Call CAMHs front line worker Encourage the young person to speak to their parents o Safeguarding ? o Admission to paediatric ward for psychiatric assessment? ? o Stomach pain?

How comfortable do you feel now approaching this scenario?
Scenario During a community visit to a 27 year old female and 6 month old baby, you notice a open bottle of vodka on the table and several packets of paracetamol. The mother tells you she has taken 32 paracetamol with a glass of vodka 1 hour ago. The baby is asleep in the cot upstairs. So now think about how you would deal with this situation, what skills you may need to apply and what you may need to consider in you care of this situation.

Points to consider: o Do you want to deal with the situation? o What is your gut telling you? o Risk o Safeguarding? o How comfortable would you feeling with dealing with this patient? - Very comfortable, unsure, uncomfortable, very uncomfortable

Non-prescriptive answer to Scenario 2 ■ Where is baby now ■ Call 999 and ask for ambulance ■ Find out exactly how many paracetamol and quantity of vodka taken ■ Give her reassurance ■ Call base and inform them of the situation ■ Call next of kin to take care of baby ■ Report to safeguard (babies DOB and full name)

How comfortable do you feel now approaching this scenario?

Scenario A 32 year old man presents at A&E, having been brought there by the police due to him stating that he has been followed by the government and fears he may have been abducted by aliens. This man has large cuts down his legs and the police commented that he was found in the woods. How do you respond? So now think about how you would deal with this situation, what skills you may need to apply and what you may need to consider in you care of this situation.

Points to consider: o Do you want to deal with the situation? o What is your gut telling you? o Risk o Safeguarding referral ? o How comfortable would you feeling with dealing with this patient? - Very comfortable, unsure, uncomfortable, very uncomfortable

Non-prescriptive answer to Scenario 3 o Visual assessment o Validate his experience o He’s a human in need of care o Communicate o Safety and trust o Explore his current life situation o Speak to liaison psychiatry for reassurance o Risk

How comfortable do you feel now approaching this scenario?
Scenario A 42 year old women has presented at A&E with fleeting suicidal thoughts and you can see she has already self harmed today. Your colleagues are telling you that they believe she has a personality disorder and is wasting time. So now think about how you would deal with this situation, what skills you may need to apply and what you may need to consider in you care of this situation.

Points to consider: o. Do you want to deal with the situation? o. What is your gut reaction when you hear a person is ‘PD’? o. What is your gut telling you? o. Risk o. Safeguarding referral ? o. Liaison psychiatry referral? o. How comfortable would you feeling with dealing with this patient? - Very comfortable, unsure, uncomfortable, very uncomfortable

Non-prescriptive answer to Scenario 4 o Do your research o Visual assessment o She a human being in need of compassionate care – validate her experience o Communicate o Trust o Explore her current life situation o Explore her suicidal intent o Speak to liaison psychiatry for reassurance o Risk o Safeguarding

How comfortable do you feel now approaching this scenario?

Final words from Mental Health Service user: “Don’t judge me for my scars, or my reason for seeking out help. Treat me like you would expect to be treated if you felt vulnerable and scared”. Pseudonyms have been used to protect the identity and retain anonymity of the individuals throughout this presentation, in line with NMC confidentially requirements. (NMC, 2015)

Remember. . Mental health is everywhere and not just on mental health wards, so we need to ensure that our friends and colleagues feel empowered in facing theses situations as they arise. o Remain calm and ask your colleagues for support o Its ok to be anxious when dealing with situations o Listen to your gut, its usually not wrong

Thank you

Reference’s • Biskin, R. S. , & Paris, J. (2012). Diagnosing borderline personality disorder. CMAJ : Canadian Medical Association journal = journal de l'Association medicale canadienne, 184(16), 1789 -94. • BEAT eating disorder. (2018). https: //www. beateatingdisorders. org. uk/types • British Medication Journal. (2018). Obsessive-compulsive disorder. https: //bestpractice. bmj. com/topics/en-gb/362 • Mental Health Foundation. (2017). Fundamental facts about mental health. www. mentalhealth. org. uk, • Frith, C. D. (1987). The positive and negative symptoms of schizophrenia reflect impairments in the perception and initiation of action. Psychology Medicine, 17, 631 -648 • Joint Commissioning Panel For Mental Health (2017) www. jcpmh. info/wpcontent/uploads/10 keymsgs-eatingdisorders. pdf • Joint Commissioning Panel For Mental Health Eating Disorders (2017) • Office For National Statistics (2018) https: //www. ons. gov. uk/peoplepopulationandcommunity/wellbeing/datasets/measuringnationalwellb eingdomainsandmeasures

Reference’s • Public Health England. (2016). Psychosis Data Report : Describing variation in numbers of people with psychosis and their access to care in England. https: //assets. publishing. service. gov. uk/government/uploads/system/uploads/attachment_ data/file/611422/Psychosis_data_report. pdf • National Collaborating Centre for Mental Health (UK). (2014). Psychosis an d Schizophrenia in Adults: Treatment and Management. https: //www. ncbi. nlm. nih. gov/books/NBK 333029/ • Mind. (2018). Personality Disorders. https: //www. mind. org. uk/information-support/types-of -mental-health-problems/personality-disorders/types-of-personality-disorder/#. XBK 4 t. Ccbs. E • The Royal College of Nursing. (2017). Child and Adolescent Mental Health Key facts. https: //www. rcn. org. uk/-/media/royal-college-of-nursing/. . . /may/pub-006021. pdf
- Slides: 40