Mental Health Awareness 2 Classroom Strategies AWARENESS Possible

Mental Health Awareness 2 Classroom Strategies

AWARENESS Possible Signs/Symptoms of Mental Illness THOUGHTS/PERCEPTIONS • Confused thinking • Expression of strange or grandiose ideas • Delusions • Suicidal thoughts • Difficulty concentrating, making decisions, remembering things • Hallucinations

AWARENESS Possible Signs/Symptoms of Mental Illness FEELINGS • Prolonged depression (sadness or irritability) • Helpless; overwhelmed • Extreme highs and lows • Excessive fears, worries • Anger; blaming others • Suspiciousness

AWARENESS Possible Signs/Symptoms of Mental Illness BEHAVIOURS • Growing inability to cope with daily challenges and activities • Increased anxiety, agitation, frustration • Excessive fatigue, lack of energy • Rapid, pressured speech

AWARENESS Possible Signs/Symptoms of Mental Illness BEHAVIOURS • Dramatic changes in eating or sleeping habits • Easily distracted • Numerous unexplained physical ailments • Social withdrawal

AWARENESS Possible Signs/Symptoms of Mental Illness BEHAVIOURS • Self-harming behaviours • Excessive risk taking; impaired judgment • Substance use • Denial of obvious challenges

Create a Positive, Caring Learning Environment

UNDERSTANDING STIGMA • Main reason individuals do not seek help • Fuelled by myths and the media • Individuals internalize the stigma

PARTNER with STUDENTS to MINIMIZE STIGMA • Education – facts versus fiction • Talk about mental illness • Challenge biases • Do not label (schizophrenic, bipolar, anorexic, cutter etc. ) • Avoid using derogatory terms (lunatic, crazy, nuts, etc. )

PARTNER with STUDENTS to MINIMIZE STIGMA • Challenge family, friends, peers who perpetuate stigma • Challenge the media stereotypes • Be supportive • Share your story "Mental illness is nothing to be ashamed of, but stigma and bias shame us all. " Bill Clinton

FOSTERING RESILIENCE • Get to know students – spend one on one time • Observe for precipitating factors, triggers • Become aware of warning signs of relapse • See each student as unique – appreciate their strengths; abilities • Encourage students to get to know each other

FOSTERING RESILIENCE • Promote cooperation rather than competition • Set high expectations – convey belief in their ability to succeed • Encourage taking risks, trying something new • Celebrate effort, willingness to try

FOSTERING RESILIENCE • Honour mistakes as an important part of the learning process • Talk about the wisdom of failure • Working through adversity – develops coping mechanisms • Importance of believing in oneself

Role Model Effective Communication

ACTIVE LISTENING • Listen to the whole message (not just the words) • Pay attention to nonverbal – eye contact, body language • Demonstrate you’re listening (smiling, nodding, verbal comments) • Provide feedback (reflect, clarify, summarize) • Reserve judgment (allow person to “tell their story”)

ACTIVE LISTENING QUOTES Nature gave us 2 ears & only one tongue Listen twice as much as you talk The heart of a fool is in his mouth, but the mouth of a wise man is in his heart (Ben Franklin)

RESPONDING with EMPATHY Ability to “walk in someone else's shoes” ; imagine how they feel Respond to the feelings expressed (overtly; covertly) “Sounds like you are feeling……. . ” “It must be very frightening to believe that……” “I understand you are feeling very angry…. . ” “I can imagine this might feel like……. ”

CONNECTING with the PERSON • Remember mental illness is no different than a physical illness • Be honest, caring, professional in your approach • Make person feel as comfortable as possible • Emphasize safety for everyone • Privacy; confidentiality

CONNECTING with the PERSON • Be mindful of personal space; stay in person’s visual field • Minimize distractions • Share your concerns; observations • Encourage them to express their feelings with words

CONNECTING with the PERSON • Actively listen to what they have to say • Empathize with the feelings/emotions expressed • Don’t try to label/diagnose • Don’t ask to explain their behavior (may not know)

CONNECTING with the PERSON • Emphasize you want to help/support them • Ask what they think will help, what’s helped before • Ask them how you can help • Develop a sense of working together – “help me to understand…. ”

COMMUNICATION STRATEGIES • Assess any risk (hearing voices; suicidal behaviour) • Listen nonjudgmentally • Be aware of your nonverbal behaviour (smile) • Be calm, quiet; lower your voice • Speak slowly, keep it short, simple

COMMUNICATION STRATEGIES • Open-ended questions • Give person time to respond • Explain your actions; responsibilities (transparency) • Be honest; never lie • Listen more; talk less

COMMUNICATION STRATEGIES • Focus on person’s strengths/positives (not problems) • Ask about their goals • Convey sense of hope; you believe in the person’s abilities • Offer choices; empower the person

COMMUNICATION STRATEGIES • Delusions • Hallucinations

ADDITIONAL STRATEGIES • Mindfulness – 2 -3 minutes at the beginning of class • Mindfulness breaks • Avoid comparing students, academics, behaviours • Begin with easier concepts, tasks, and build on successes

ADDITIONAL STRATEGIES • Break tasks, assignments down into smaller sections, components • Provide lots of positive feedback • Positive journaling – diminishes worrying – write down the negative incident – 6 positive things that happened • Remind students mental health is a continuum • Decatastrophize – thoughts are mental events, not ‘reality’

Barriers to Communication • Talking too much • Interrupting person • Changing subject • Talking over a person (as if they are not there)

Barriers to Communication • Asking leading or biased questions • Asking “why” questions (can become defensive) • Using professional jargon

Barriers to Communication • Minimizing person’s feelings (everyone feels that way sometime) • False reassurance (everything will work out) • Trying to cheer the person up (things will get better)

Barriers to Communication • Giving advice (take away person’s decision making; lessens confidence) • Showing approval or disapproval • Threatening consequences • Becoming defensive in response to criticism

Self Harming Behaviour • Deliberate, repetitive, without suicidal intent • Early adolescence; peak 16 -26 years • Most common - cutting

Understanding Self Harm • Feel numb; want to feel more alive • Attempt to gain control • Attempt to reduce anxiety

Understanding Self Harm • Escape feelings of depression • Relieve emotional pain • Relieve anger, aggression

Self Harm as a Coping Strategy • Attempt to cope/problem-solve (ineffective) • Attempt to punish themselves • Desire to feel emotions more intensely • People who attempt suicide intend to end their life • People who self harm intend to cope with their life!

Understanding Self Harm • Can become addictive – Endorphins released (creates a high) – Gain some relief – sense of calm/soothing (temporary) – Self harm again • Do not feel same level of pain • Often embarrassed – hide the evidence

Recovery from Self Harming Behaviour • Often lessens/stops as person gets older • Active listening; non judgmental • Be empathic and acknowledge the distress • Lengthen time between urge to self harm • Assist to develop alternative coping strategies • Refer to counselling – talk about feelings • Medication has limited effect ****May accidently be seriously injured****

Prevalence of Suicide/Suicidal Behaviour • About 4000 suicides in Canada every year • 2 nd leading cause of death for ages 10 -24 • 24% of all deaths among Canadians 15 – 24 • 16% of all deaths for the age group 25 – 44 • More women attempt; more men succeed • Statistics are incomplete – many go unreported
Myths about Suicide • Young people don’t think about suicide • People who talk about it, don’t do it • Talking about it may give a depressed person the idea • Happens without warning

Myths about Suicide • People wish to die • Once suicidal, always so • Once no longer depressed, danger is over • Suicide is inherited, runs in families

Risk Factors for Suicide • Gender (male) • Age (elderly, youth) • Stressors (unemployed, divorced, single, abuse, loss) • Major health challenges

Risk Factors for Suicide • Depression (hopelessness) – going into and coming out • Schizophrenia (command hallucinations) • Substance abuse (impaired judgment) • Personality traits (angry, negative, low self-esteem) • Previous attempts

Warning Signs for Suicide • Sudden change in behaviour (for better or worse) • Sudden and unexpected change to a cheerful attitude • Mood swings, emotional outbursts • High level of irritability or aggression

Warning Signs for Suicide • Signs of depression - sleeplessness, social withdrawal, loss of appetite, loss of interest in usual activities • Cycle of hopelessness, helplessness, desperation • Withdrawal from friends and activities

Important Strategies • Ask directly • Assess lethality – Idea/intent – Plan – level of detail – Means – to carry out their plan

Important Strategies • Convey empathy (connect with feelings) • Never minimize previous attempts • Help identify reasons to continue living • Get person help – Form 1 assessment; JP; Police

Final Thoughts • Partnership – supporting the person on their journey to wellness • Not looking for us to “fix” their problems • Want to be heard; treated like a person, not an illness • Want to be accepted and not judged

FINAL THOUGHTS • Individuals get better in spite of the system • Recovery is different for every person • Recovery takes time Mental Illness Awareness is a Required Life Skill!

Provincial Resource – Connex. Ontario (24/7) Mental Health Helpline • 1 -866 -531 -2600 • http: //www. mentalhealthhelpline. ca/ Drug and Alcohol Helpline • 1 -800 -565 -8603 • http: //www. drugandalcoholhelpline. ca/ Problem Gambling Helpline • 1 -888 -230 -3505 • http: //www. problemgamblinghelpline. ca/

Mindsight – An Online Mental Illness Awareness Resource Website: http: //mindsight. uoit. ca
Stigma Section
Description of Illness
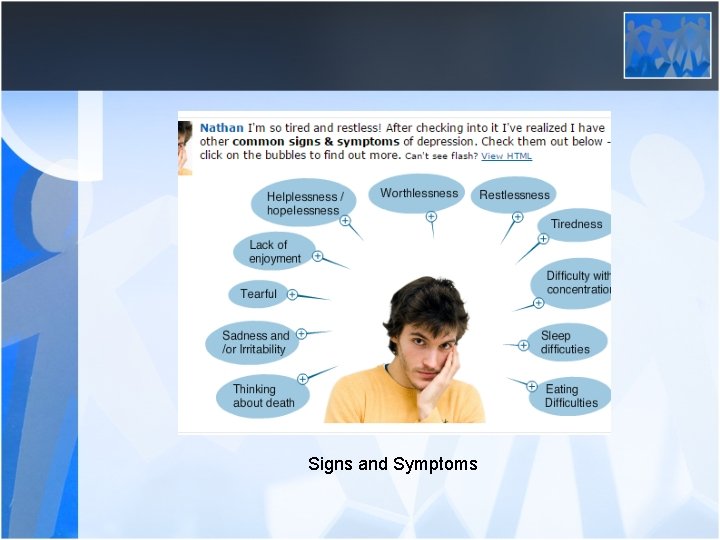
Signs and Symptoms
Video Clip
Strategies to Help a Friend, Colleague, Family Member
Strategies to Help Yourself

Possible Treatments
Example of Support Section

Example of Quiz Section
Certificate of Completion

Contact Information Wendy Stanyon Associate Professor Collaborative BSc. N Program Faculty of Health Sciences University of Ontario Institute of Technology Phone: 905 -721 -8668 ext. 2250 Email: wendy. stanyon@uoit. ca
- Slides: 61