Mental health and Aging Vineeth John MD MBA

Mental health and Aging Vineeth John MD MBA

Case of a new onset Bipolar Disorder • A 60 -year-old, right-handed, previously successful and psychiatrically healthy businessman was brought by his family to a university hospital neuropsychiatry service for consultation regarding behavioral and personality changes. • When he was age 55 years, his customarily excellent financial and social judgment began to decline. Over the next 4 years, his attention to personal hygiene deteriorated, his business decisions became financially and ethically unsound, his range of social interests narrowed dramatically, and he developed an insatiable "sweet tooth. "

Case of a new onset Bipolar Disorder In the year preceding the consultation, his ability to maintain sleep diminished, he began spending money recklessly and impulsively and became unable to appreciate the feelings and concerns of others, and his speech and behavior took on a perseverative quality. Concurrently, he developed unprovoked, brief, frequent, and excessively intense episodes of tearfulness and laughing. These episodes lasted minutes at most, after which he would return to his usual euthymic emotional state.

Case of a new onset Bipolar Disorder One month before the neuropsychiatric consultation, he had received a diagnosis of late-onset bipolar disorder and had begun treatment with lithium carbonate. When his serum lithium level reached therapeutic range, his cognitive, behavioral, and motor function declined precipitously, prompting the consultation for a second diagnostic opinion.
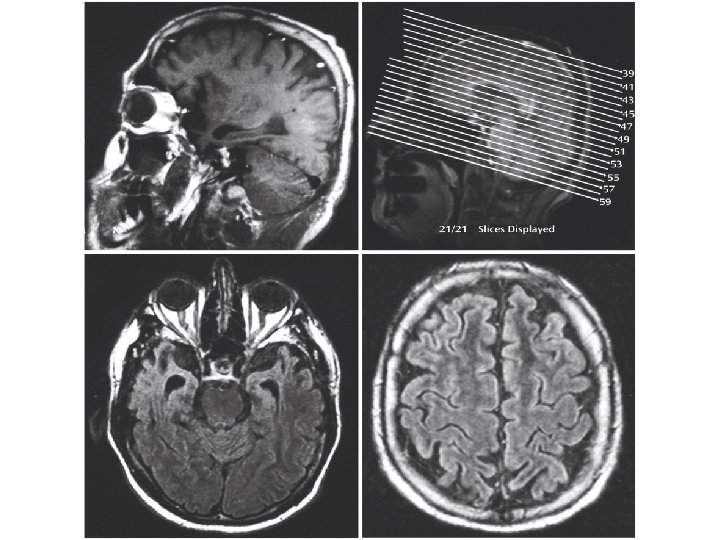

Late onset psychosis Psychosis of Alzheimer's disease Late onset Schizophrenia Late life delusional disorder Psychotic disorders secondary to General Medical Conditions

Psychosis in AD • • • Increased risk of agitation Increase in aggression Poor self care Disruptive behavior Wandering High rate of institutionalization

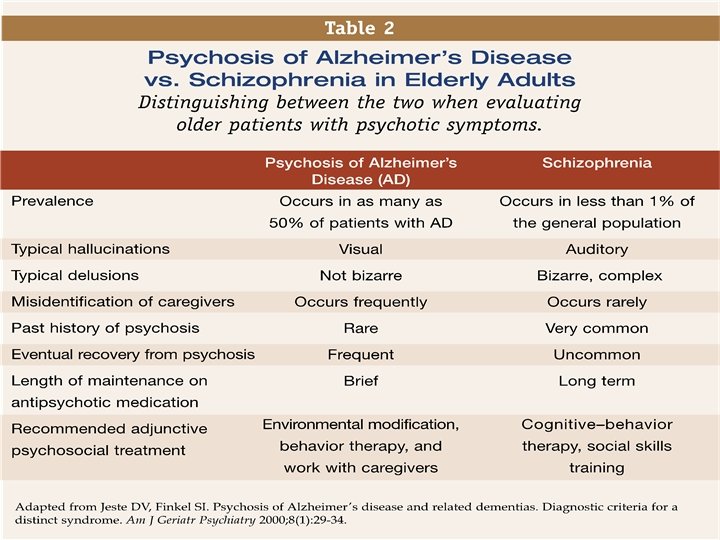
Psychosis in AD • Between 30 to 50 % of AD patients have psychotic symptoms • Psychotic symptoms are more prevalent as the disease progresses but are more common in the middle stages. • Visual hallucinations are more common than auditory hallucinations.

Common themes of delusions in AD • Stealing • Stranger in the house • Spying • Impersonating the spouse or loved one

Psychosis in other dementias • Dementia of Lewy bodies -VH and Delusions • Parkinson's Disease - Delusions and hallucinations • Vascular Dementia

Treatment of Psychotic Symptoms in Dementia • Low dose antipsychotics are the norm. • Careful balancing of the risks and benefits need to be performed.
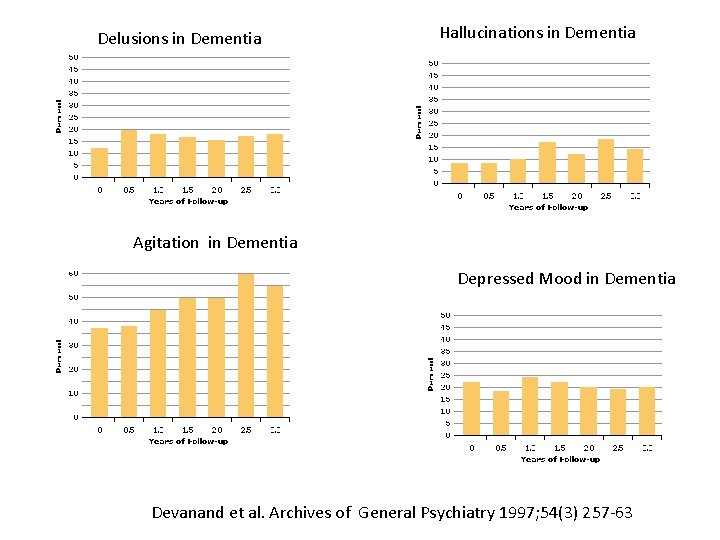
Delusions in Dementia Hallucinations in Dementia Agitation in Dementia Depressed Mood in Dementia Devanand et al. Archives of General Psychiatry 1997; 54(3) 257 -63

Agitation in Dementia • Treat reversible causes of agitation-UTI, medications, alterations in renal functions, pain and discomfort • Behavioral Interventions • Antipsychotic medications • Anticonvulsants • Acetyl Cholinesterase Inhibitors/Memantine • SSRIs and antidepressant therapy

Factors affecting Psychosocial interventions Individual biography Individual’s personality Coexisting physical and mental health problems Person’s social relationships Physical environment in which the person is living Community and cultural understandings of tolerance for confusion and frailty • Extent and location of the disease • • •

Psychotherapeutic Interventions • • Behavior management training Caregiver training Scheduled toileting Reminiscence therapy Validation therapy Supportive therapy Reality orientation Art therapy
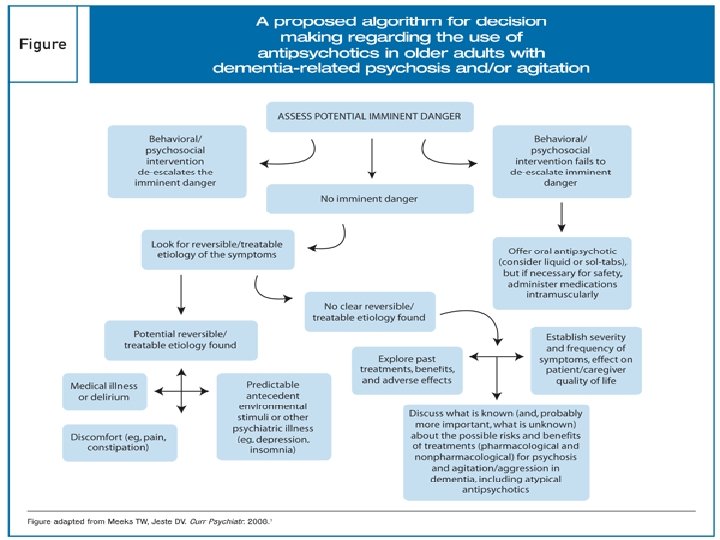
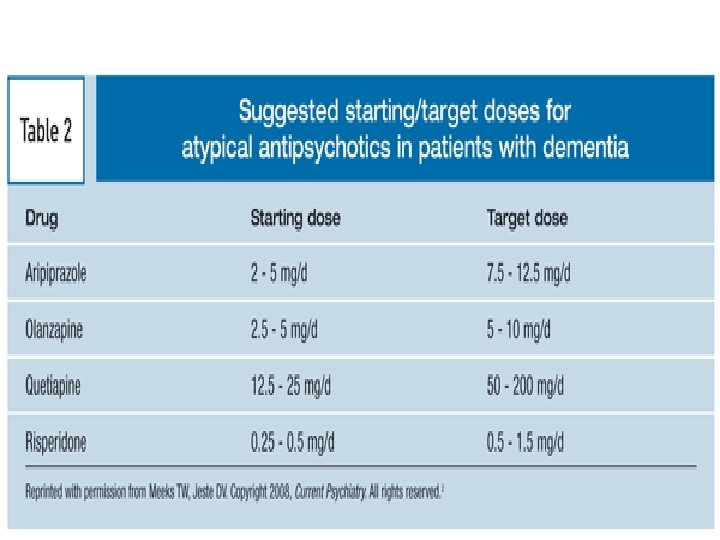

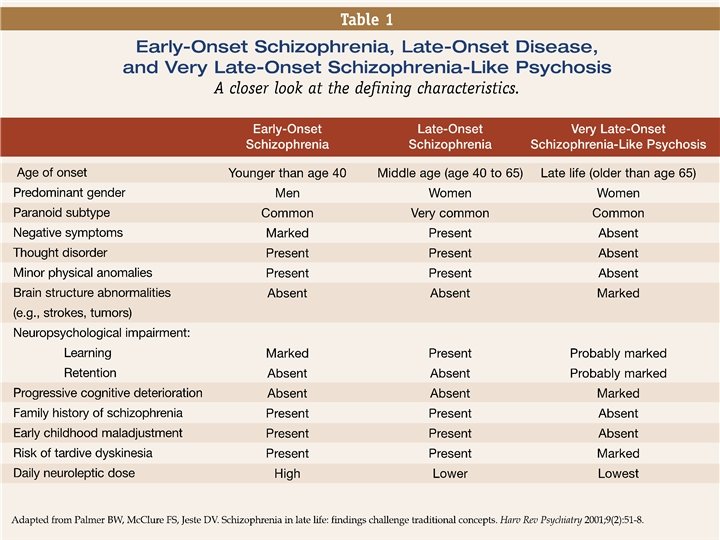
Late onset Schizophrenia • Schizophrenia is characterized by it's onset in youth and subsequent deterioration of functionality. • Schizophrenia after 45 years of age was considered late onset by APA DSM III R, 1987. International consensus panel chose 40 years as the cut off point. • No such distinction is elaborated in DSM IV TR version.

What are the distinct features of late onset schizophrenia? • Lack of negative symptoms • Lack of thought disorder • More paranoid schizophrenia subtype • Presence of the features of neurodegeneration –CVAs. • More in women than in men • Patients who develop late onset schizophrenia were also noted to have sensory deficits - visual and hearing

Differential diagnosis of late onset schizophrenia • Psychotic disorders secondary to general medical conditions • Psychotic symptoms which might be part of delirium • Early onset schizophrenia undetected • Mood disorders with psychotic features • Delusional disorders
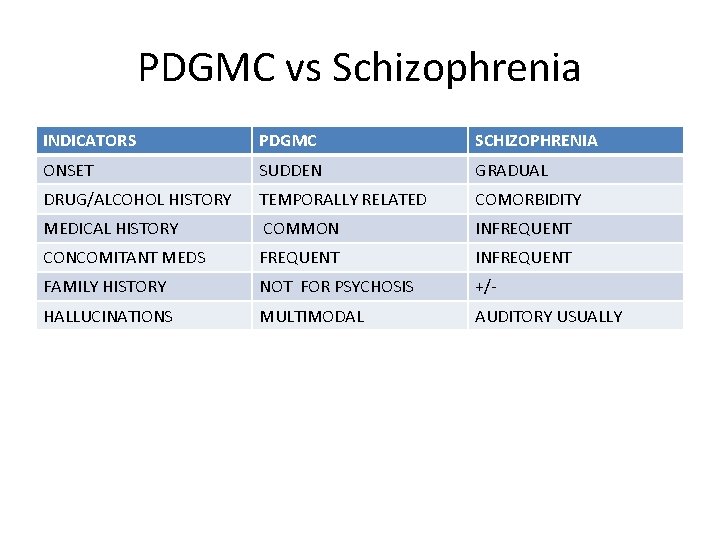
PDGMC vs Schizophrenia INDICATORS PDGMC SCHIZOPHRENIA ONSET SUDDEN GRADUAL DRUG/ALCOHOL HISTORY TEMPORALLY RELATED COMORBIDITY MEDICAL HISTORY COMMON INFREQUENT CONCOMITANT MEDS FREQUENT INFREQUENT FAMILY HISTORY NOT FOR PSYCHOSIS +/- HALLUCINATIONS MULTIMODAL AUDITORY USUALLY

Treatment of late onset schizophrenia • Atypical antipsychotics • Psychosocial treatments-social skills, CBT • Family interventions for relapse prevention

Aging and Early onset Schizophrenia • Around 30% could show evidence for improvement and remission. • Cognitive deterioration is reasonably steady and do deteriorate significantly

John Nash Jr- “ A beautiful mind”

John Nash, Jr- In his own words “But after my return to the dream-like delusional hypotheses in the later 60's I became a person of delusionally influenced thinking but of relatively moderate behavior and thus tended to avoid hospitalization and the direct attention of psychiatrists. Thus further time passed. Then gradually I began to intellectually reject some of the delusionally influenced lines of thinking which had been characteristic of my orientation. This began, most recognizably, with the rejection of politically-oriented thinking as essentially a hopeless waste of intellectual effort. ”

Psychotic disorders due to general medical conditions in the elderly • Stroke • Parkinson's disease • Epilepsy • Herpes Encephalitis • Thyroid and adrenal disorders • Folate, B 12 deficiencies • Systemic lupus erythematosus • Alcoholic hallucinosis

Medications causing psychotic symptoms • • • Levadopa Bromicriptine Amantadine Isoniazid Corticosteroids Amphetamines Methylphenidate Lidocaine Cimetidine

Mood disorders secondary to general medical conditions • Rate of depression in the medical population is 12 to 20%. • Many physical illnesses and medications can cause symptoms mimicking depression.

Common medical conditions causing depression • Strokes • Parkinson's Disease • Hypothyroidism • Addison's Disease • Occult carcinoma of the Pancreas • Collagen vascular disease • Multiple sclerosis

Most common medications causing depression • Antihypertensives - reserpine and methyl dopa • Steroids

Secondary Mania • Stroke • Right hemisphere cerebral neoplasms • Multiple sclerosis • Encephalitis • Syphilis • Head injury • Uremia

Secondary Mania • Corticosteroids • Thyroxin • Levodopa • Bromocriptine • Amphetamines • Cimetidine

Dimensions of Grief and Bereavement • Emotional and cognitive experiences • Coping strategies • Continuing relationship with the deceased • Health, occupational and social functioning • Relationships • Social identity and Self esteem

Complications of Grief and Bereavement • Morbidity • Increased somatic complaints • Worsening of pre existing illnesses • Increased use of medical services • Mortality • Widowers: highest risk in the first six months • Widows: period of risk delayed by 1 or 2 years.

Psychiatric complications of grief • Substance use • Anxiety symptoms • PTSD • Depression

Risk factors leading to Depression in the Grieving process • Unnatural sudden unexpected death • Preexisting mood disorder • Early, intense depressive reaction after the loss • Poor physical health • Increased alcohol consumption • Family history of major depression • Poor social support system

Geriatric depression • Prevalence of geriatric depression is much higher in medical settings than in the community -30%. • 50% of nursing home residents are at risk to develop depression. • Cognitive impairment is an expected complication in elderly patients who develop depression

Under diagnosis of depression in the elderly • • • Under reporting of symptoms More focus on physical symptoms More anhedonia than sadnesss Subsyndromal depression not meeting criteria Medical illness detection overshadow the diagnosis of depression

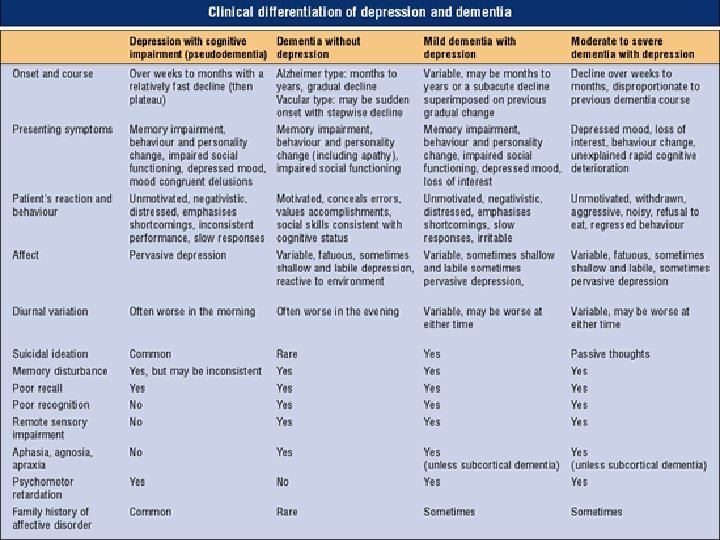

Co-morbidity and complications of late life depression • Depression worsens outcomes and prognosis of medical illnesses • Depression lengthens hospital stay • Depression increases perception of ill health • Depression increases economic burden on the health care system • Depression worsens disability • Depression also results in increased suicide risk -White men over the age of 65 has the highest suicide rate

Risk factors for suicide in the elderly • Loneliness and poor social support • Presence of psychiatric disorder • Presence of fire arm • Impaired ability with IADLs • Medical co-morbidity

Treatment options for Depression in the elderly • SSRIs • TCAs • MAOIs • Bupropion • Mirtazapine • Augmenting agents • ECT • Psychotherapy

Characteristics of Delirium • • • Disturbance of consciousness Abnormal cognition Acute onset and fluctuating in course Multifactorial etiology Hyperactive, hypoactive, and mixed forms

Characteristics of delirium • Misdiagnosis is frequent – confused with depression and mania • May develop over hours to days. – Abrupt onset more common. – The line between dementia and delirium is often unclear.

Etiology of delirium • • Etiology - Multifactorial Infections Toxins, including drugs Substance withdrawal Organ failure: heart, liver, kidney, etc Metabolic derangements Primary brain disorders

Pathogenesis of Delirium • Pathogenesis: – – – No specific structural brain lesion identified: EEG showing slow waves but nonspecific Depleted acetylcholine Dopamine, GABA, serotonin, acetylcholine imbalance Cytokine activation (sepsis)

Risk Factors • Dementia is the strongest risk factor – 25 to 75% of patients have dementia. • Other predisposing brain diseases: stroke, Parkinson’s • Advanced age • Severe medical illness • Hyponatremia, dehydration, other metabolic problems • Anticholinergic drugs, sedative hypnotics, narcotics

Clinical Presentation • Disorientation to place, time, situation • Impaired consciousness – Reduced awareness – Reduced or clouded consciousness with or without overt hallucinations

Clinical Presentation • Decreased ability to focus, sustain, or shift attention – Decreased selective attention – Distractibility • Cognition is made worse by inattention. • Speech: – – Tangential Poorly organized Slowed, slurred Word finding difficulties

Clinical Presentation • Impaired registration, recent/remote memory with associated confabulation • Perceptual abnormalities: – May be agitated in response to hallucinations

Diagnosis • • History from family and/or caregivers Bedside observations DSM-IV diagnostic criteria Reliable diagnostic instruments: – Confusion Assessment Method – The Delirium Rating Scale – Delirium Symptom Review • Diagnostic errors are common in: – Hypoactive form – The setting of rapid fluctuations of cognition.

Differential Diagnosis • Dementia – Alzheimer dementia – Lewy body dementia • Depressive states • Psychotic disorders
- Slides: 55