Menopause Sal Roberts RN RM MSc DFSRH PGA

Menopause Sal Roberts RN RM MSc DFSRH PGA Med Ed (SRH) FRT

What is Menopause ? Menopause • after a year of no periods (amenorrhoea) • usually diagnosed on symptoms, not blood tests unless <45 (NICE 2015) • doesn’t apply �after hysterectomy (unless ovaries removed) �endometrial ablation �Mirena �continuous hormones Perimenopause (Climacteric) • from the beginning of menopausal symptoms to the postmenopause

Types of Menopause • Premature Ovarian Insufficiency (before age 40) • Early menopause (before 45) • Surgical menopause • Medical menopause �chemotherapy �radiotherapy • Average at natural menopause 51 -52

Why is Menopause so important? • 18% rise in people >65 yr in last decade • 31% rise in people >85 yr • State Pension age rising 66/67 2019 • ONSS 47% of the current workforce is female • 1. 7 million (5%) working women affected by menopause and increasing!!
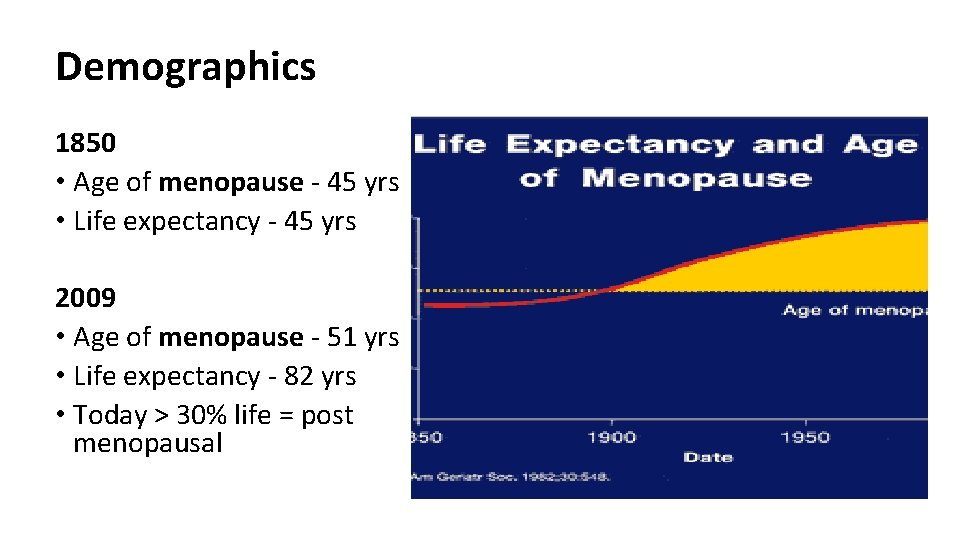
Demographics 1850 • Age of menopause - 45 yrs • Life expectancy - 45 yrs 2009 • Age of menopause - 51 yrs • Life expectancy - 82 yrs • Today > 30% life = post menopausal

Why is Menopause so important? • 45% menopausal women felt menopause had impact on work • 47% who had taken a day off work couldn't say why • 51% menopause affected sex life • 42% don’t feel as sexy • 36% impacted social lives • 23% more isolated • 50% impacted home life • 38% partners felt helpless to support menopausal woman • 28% partners said menopause caused conflict in relationship • 50% women aged 45 -65 with menopausal symptoms have not consulted a Health Professional for help!

Menopause Symptoms Vasomotor (Average 2 to 5 years. . . ) �Hot flushes 79% �Night sweats 70% �Anxiety �Palpitations Psychological symptoms �Poor memory and concentration 20% �Lack of confidence �Low mood/mood swings/Irritability �Panic attacks Sexual, vaginal and urinary symptoms �Reduced sex drive �Painful sex �Vaginal dryness/irritation �Pelvic floor problems 10 -40% �UTIs and stress incontinence �Dysuria, frequency, urge incontinence, nocturia �Prolapse of vaginal wall �? Body image change
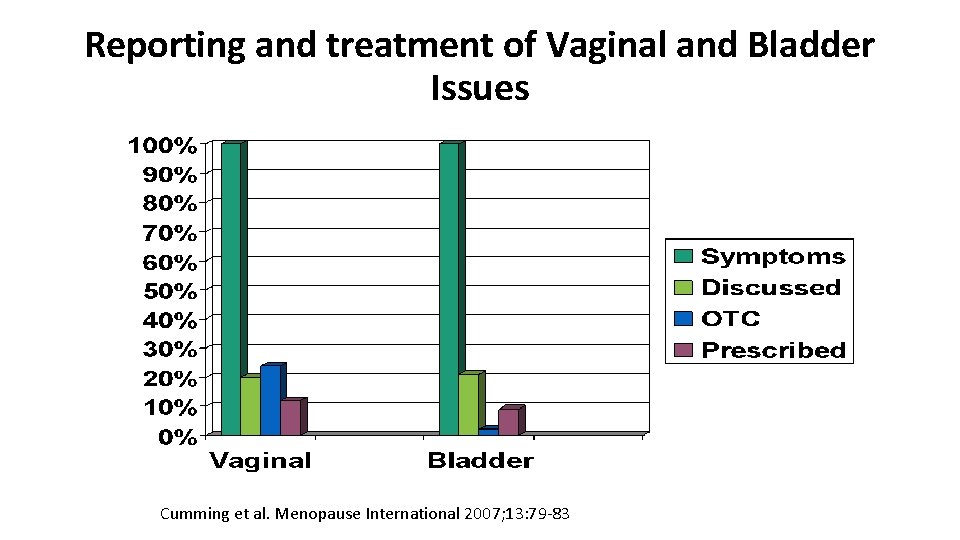
Reporting and treatment of Vaginal and Bladder Issues Cumming et al. Menopause International 2007; 13: 79 -83

Menopause Symptoms • • • Periods changing Insomnia 22% Weight gain Headaches Joint pain and stiffness 18% Hair loss Dry, thin, itchy skin Formication Osteoporosis 2016 Survey conducted by Ipsos MORI on behalf of the British Menopause Society (BMS)


Management of symptoms Discussion / counselling: �Diet and lifestyle �Over the counter options �Hormone replacement therapy �Cognitive Behavioural Therapy (CBT) �Non-hormonal medicines (SSRIs /Venlafaxine/Clonidine/Gabapentin)

Lifestyle advice - symptom control and prevention Loose cotton layers Fans Stop smoking Avoid spicy foods Avoid hot drinks � Especially caffeine • Exercise � Weight loss and improving bone health • • • Diet � Weight loss � Phytoestrogens � Improve sugars/carbs � Calcium/vitamin D � ? ? Herbal treatments � Reduce alcohol

Phytoestrogens Japanese women �Fewer hot flushes �High soya diet containing phytoestrogens �Lower risks of heart disease and hormonal cancers What are phytoestrogens? �Naturally occurring in plant sources �Structurally related to estradiol �Concentrated iso-flavones (phytoestrogens) are found in red clover �Can be taken in tablet form �CEREALS: oats, barley rye, brown rice, cous and bulgar wheat �SEEDS: sunflower, sesame, pumpkin, poppy, linseeds �PULSES: soya beans and all soya based products (except soya sauce which does not contain any!) �BEANS: chickpeas, kidney beans, haricot beans, broad beans, green split peas �VEGETABLES: red onions, green beans, celery, sweet peppers, sage, garlic, broccoli, tomatoes and bean sprouts �SOYA, LINSEEDS and RED CLOVER are the richest sources �COMMERCIAL PRODUCTS are also available such as Bergen bread, Provamel yoghurts and "So Good" milk

Herbal and OTC remedies • • Ginseng (mood) Cochrane 2014 Dong quai (-) Hirata 1997 Oil of evening primrose (-) Chenoy 1994 Vitamin E (marginal benefit) (+) Barton 1998 Multivitamin and minerals no studies Sage (-/+) Bommer 2011 Natural progesterone gel (-) Benster 2009 Magnets nil • Black Cohosh (-) Cochrane 2012

HRT WHY? • Control of menopause symptoms in peri or post menopausal women • Treatment of Premature Ovarian Insufficiency (POI) • Osteoporosis prevention

HRT Safety • The safety of HRT largely depends on age • Healthy women younger than 60 years should not be concerned about the safety profile of HRT • For most women, the potential benefits of HRT given for a clear indication are many and the risks are few when initiated within a few years of menopause • There actually very few women who should be advised that they should NEVER use HRT

HRT Benefits • Control of menopausal symptoms • Maintenance of BMD (bone mineral density) and reduced risk osteoporotic fractures • Reduced risk coronary heart disease and reduced risk of Alzheimers disease when estrogen started early • Reduced risk colorectal cancer • Reduced risk Type 2 diabetes • Improves muscle mass and strength

HRT Benefits For women with Premature Ovarian Insufficiency (Aged under 40): • the risks associated with not using HRT are �low bone density, earlier onset osteoporosis and fractures, �earlier onset of coronary heart disease and increased cardiovascular mortality and total mortality �diminished sexual well-being

HRT Risks • Endometrial cancer (if oestrogen only given when uterus present) reduced by addition of progestogen • DVT/PE risk with Oral HRT but not transdermal (patch or gel) • CHD increased when combined HRT started in older women(>60), or with pre-existing CHD – ideal is within 10 years of menopause • Stroke increased when HRT started in older women (> 60 years) • Breast cancer � Increased slightly after a minimum of 5 years’ use of combined HRT �Over the age of 50— additional 3 -4 cases per 1, 000 women �Risk associated with estrogen alone is very much less �Mortality is not increased.
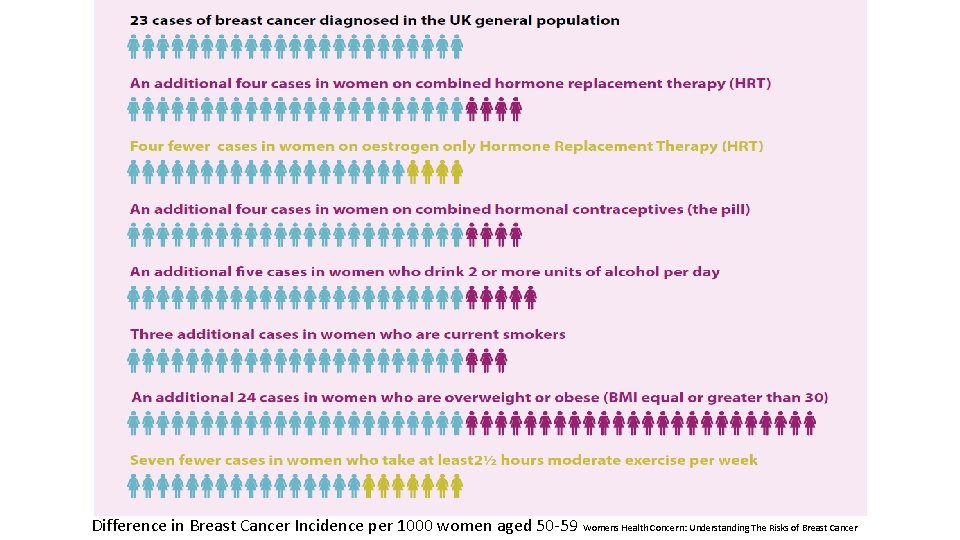
Difference in Breast Cancer Incidence per 1000 women aged 50 -59 Womens Health Concern: Understanding The Risks of Breast Cancer
Which HRT? Which regimen? Which route? Lots of options: • Systemic or local therapy • Estrogen only or combined therapy • Cyclical or continuous combined therapy • Oral, transdermal, subcutaneous or intrauterine • Tablets, patches, gels, implants, vaginal preparations

Cognitive Behavioural Therapy “CBT is a short-term, skills focused form of psychotherapy” • Helps to develop practical ways of managing problems and provides new coping skills and useful strategies • NICE 2015: should be considered for low mood/anxiety as a result of menopause

Non-hormonal vaginal options Moisturisers Lubricants • hold moisture on the vaginal walls and only needs to be used 2 or 3 times per week • Sylk • Yes • Durex Play • • Yes Replens Regelle Hyalofemme Petroleum-based lubricants can increase the likelihood of infection and damage latex condoms Check the label!
Non-medical options • • • Homeopathy Acupuncture Aromatherapy Reflexology Relaxation therapy � it’s all about getting through the menopause as comfortably as we can � for some it may involve hormones, for many it won’t

More Help Women's Health Concern - www. womens-health-concern. org Menopause Matters - www. menopausematters. co. uk Manage my menopause - www. managemymenopause. co. uk British Menopause Society - www. thebms. org. uk NICE - https: //www. nice. org. uk/Guidance/NG 23 Thank you!
- Slides: 25