MENINGITIS Prof Mohammad Abduljabbar Definition Meningitis is defined

MENINGITIS Prof. Mohammad Abduljabbar

Definition Meningitis is defined as an infection of the tow layers of meninges ( Pia And Arachnoid ) including the fluid in between namely cerebrospinal fluid (CSF)

CAUSES 1 -Bacterial 2 -Viral 3 -Fungal
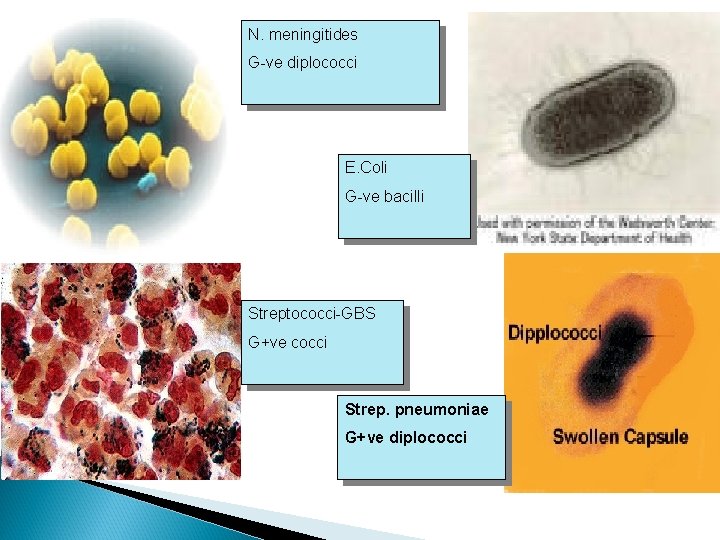
N. meningitides G-ve diplococci E. Coli G-ve bacilli Streptococci-GBS G+ve cocci Strep. pneumoniae G+ve diplococci

Bacterial Meningitis Organisms - Birth - 4 weeks: GBS, E. coli - 4 - 12 weeks : GBS, E. coli, Pneumococcus, Salmonella, Listeria and H. Influenza - 36 months: Pneumococcus, Meningococcus and H. Influenza - 3 years - adult: Pneumococcus, Meningococcus

Pathogenesis Infection of upper respiratory tract Invasion of blood stream (bacteraemia) Seeding & inflammation of meninges

Clinical Presentation Triad of Meningitis Headache Fever Neck pain

Clinical features New born & Infants: Non-specific symptoms including: - Fever - Irritability - Lethargy - Poor feeding - High pitched cry and bulging AF - Convulsions and opisthotonus
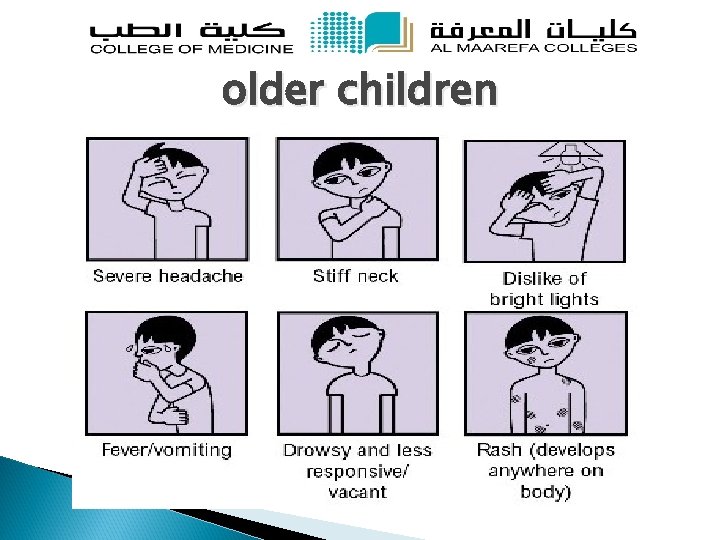
older children
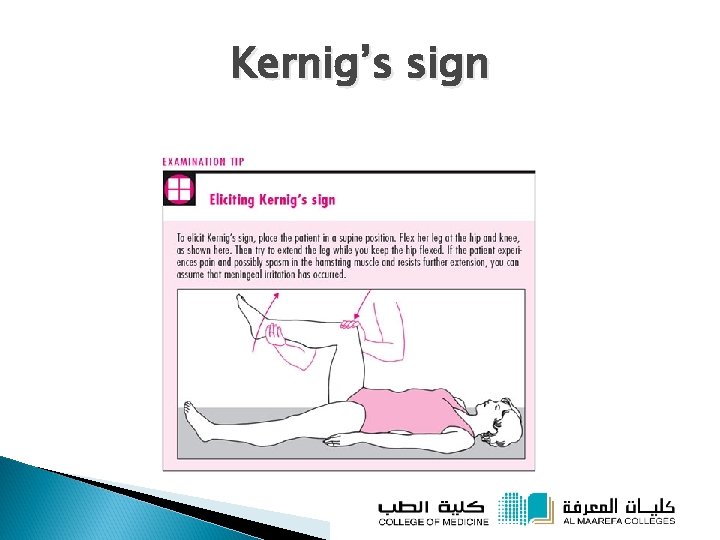
Kernig’s sign
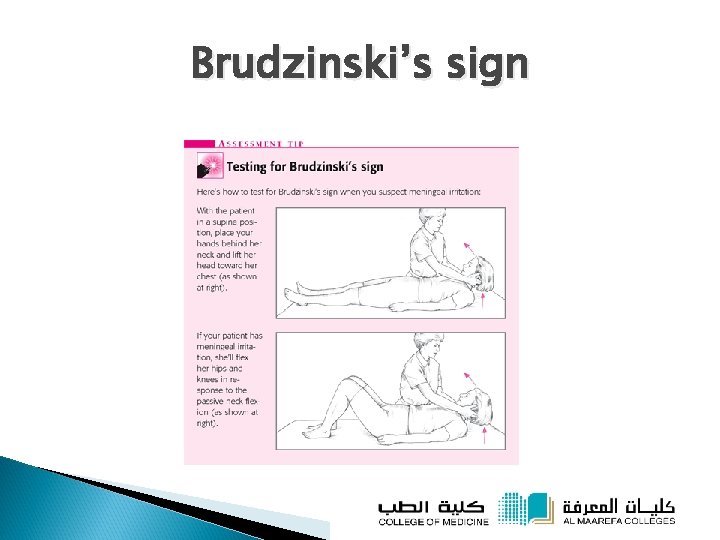
Brudzinski’s sign

Acute Meningococcaemia Neisseria meningitidis: serotype Group B Endotoxin causes vascular damage vasodilatation, third spacing, severe shock Severe complication: Waterhouse-Friderichsen syndrome: massive haemorrhage of adrenal glands secondary to sepsis: adrenal crisis-low B. P, shock, DIC, purpura, adreno-cortical insufficiency
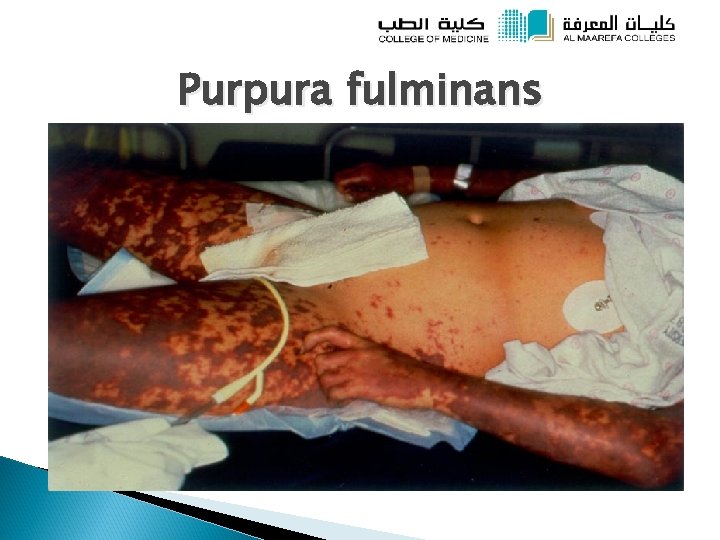
Purpura fulminans
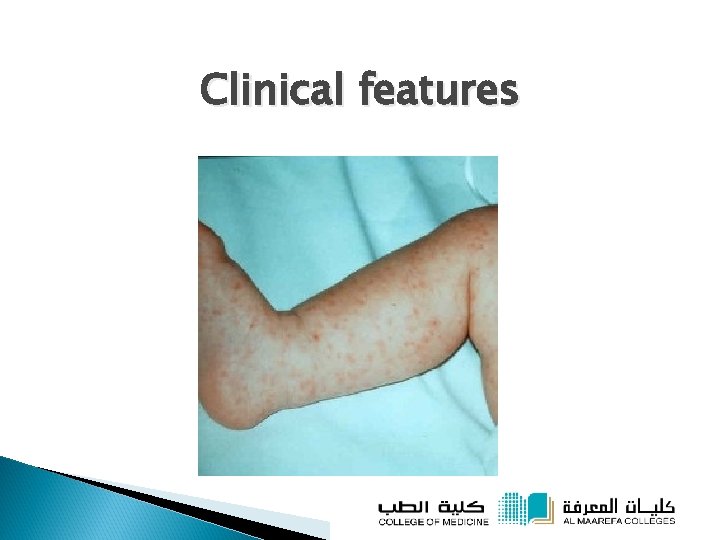
Clinical features
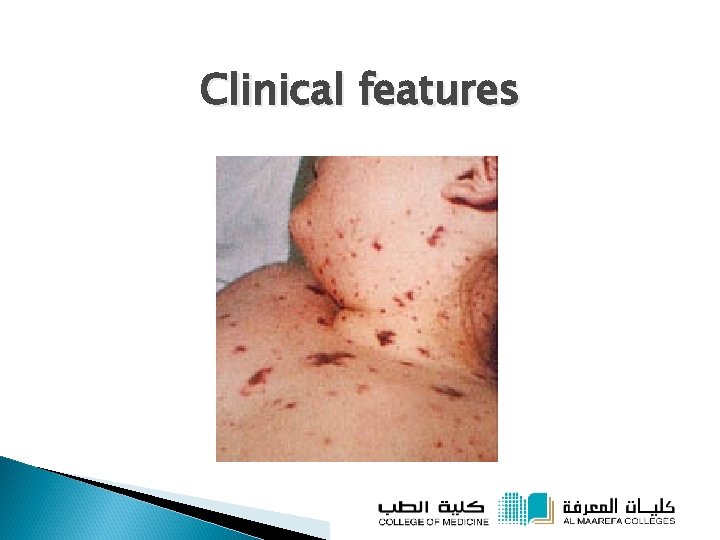
Clinical features
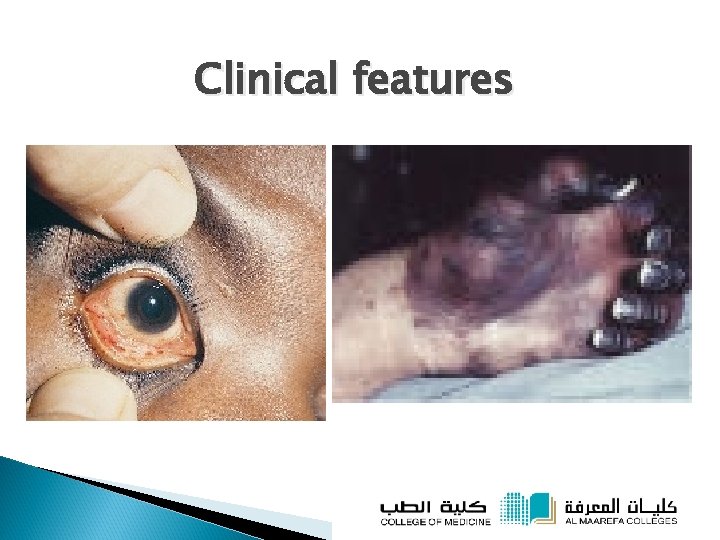
Clinical features

DIAGNOSIS 1 - History 2 - physical examination 3 - Investigations: including CBC Renal profile CRP Coagulation Blood gas Glucose Blood C/S Skin scrapings PCR CXR Skin test
Diagnosis
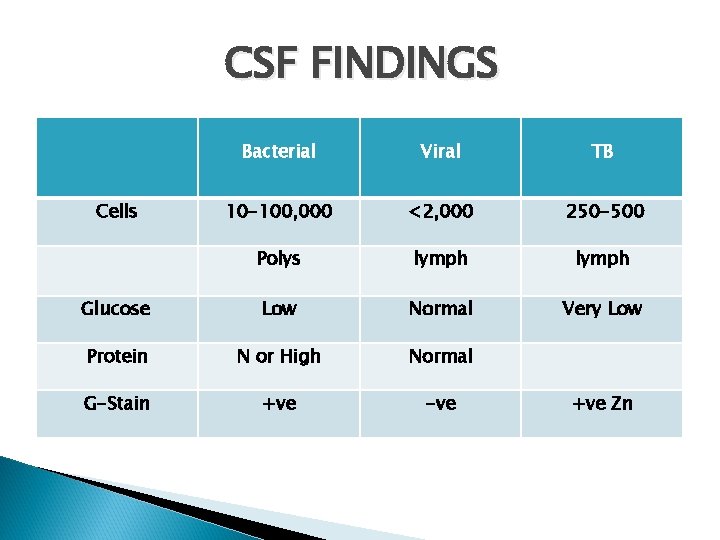
CSF FINDINGS Bacterial Viral TB 10 -100, 000 <2, 000 250 -500 Polys lymph Glucose Low Normal Very Low Protein N or High Normal G-Stain +ve -ve Cells +ve Zn

Management v v v Medical emergency Early diagnosis essential - Immediate optimum treatment - Intensive supportive therapy Rehabilitation Prophylaxis to family Notification to GP & Public Health

Bacterial Meningitis ABC ICU admission Fluid management: Aggressive resuscitation Dexamethasone: Only in Pneumococcal and H I bacteria, given in children Inotropes: Increasing aortic diastolic pressure to improve myocardial contractility

Antibiotics q Less than 2 months of age: • Ampicillin + Cefotaxime+/- Gentamicin • Treat for 3 weeks (neonate) q Over 2 months: • Cefotaxime • Treat for 7 -10 days

Prophylaxis v v Rifampicin: • Children: 5 mg/kg bid x 2/7 • Adults: 600 mg bid x 2/7 Cefuroxime: • IM x 1 dose in • Pregnant contact

Complications Septic shock - DIC Cerebral oedema Seizures Arteritis/venous thrombosis Subdural effusions Hydrocephalus. Abscess. Brain damage Deafness

Meningococcemia poor prognosis Index • • • Onset of Petechial within 12 hrs Absence of meningitis signs Shock (BP 70 or less) Normal or low WBC Normal or low ESR

Subdural Effusion Failure of temperature to show progressive reduction after 72 hours Persistent positive spinal cultures after 72 hours Occurrence of focal/ persistent convulsions Persistence/recurrence of vomiting Development of focal neurological signs Clinical deterioration after 72 hours especially ICP

Partially treated meningitis 50% cases prior antibiotic ( alters the findings in bacterial meningitis ) Accurate history is vital CSF mainly lymphocytic (usual polys) Can have normal glucose Positive cultures reduced by 30% Gram stain reduced by 20%

Viral meningitis Most common CNS infection in <1 yr old Causes: enterovirus (commonest, meningitis occurring in 50% of children <3 mth ) herpes, influenza, rubella, echo, coxsackie, EBV, adenovirus Mononuclear lymphocytes in CSF Symptomatic treatment. Complications associated with encephalitis and ICP

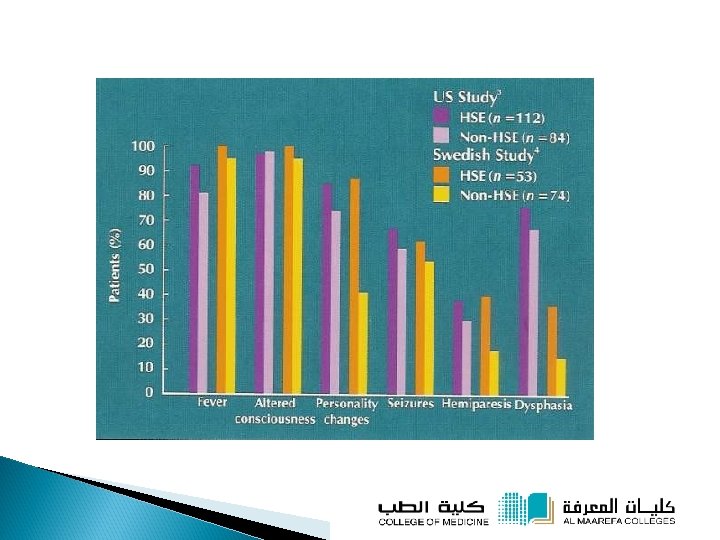
Herpes Simplex Encephalitis • The most commonly identified cause of acute, sporadic viral encephalitis: 10 to 20% of all cases • Subtype 1 virus causes more than 95% of cases of HSV encephalitis • In children and young adults, primary HSV infection may result in encephalitis (virus enters the central nervous system (CNS) by neurotropic spread from the periphery via the olfactory bulb)

Herpes Simplex Encephalitis q Most adults with HSV encephalitis have clinical or serologic evidence of mucu-cutaneous HSV-1 infection before the onset of the CNS symptoms. HSV DNA has been demonstrated in brain tissue from healthy adults. ( = reactivation) q In about 25% of the patients, the HSV-1 strains from the oropharynx and brain tissue of the same patient differ (some cases may result from reinfection with another strain of HSV-1 that reaches the CNS)

Herpes Simplex Encephalitis Diagnosis q CSF WBC: 20 -300 cells/mm 3 (rarely < 5) Protein: mildly elevated, median 80 (normal<60) Glucose usually normal q EEG: spike and slow wave activity from the temporal lobe. Sensitivity 85%. Specificity 33%.

Herpes Simplex Encephalitis Diagnosis q CT: Edema in the temporal lobe hemorrhagic necrosis midline shift First 5 days: CT sensitivity 73%, specificity 89% >5 days: CT sensitivity 90%, specificity 92%
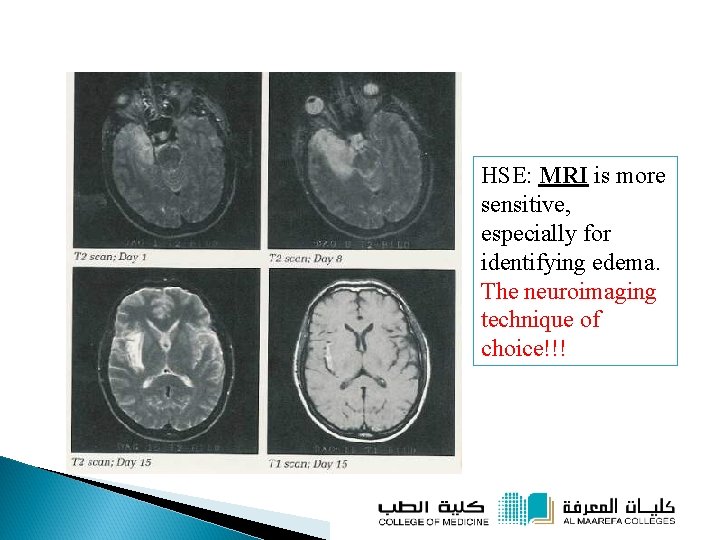
HSE: MRI is more sensitive, especially for identifying edema. The neuroimaging technique of choice!!!

Herpes Simplex Encephalitis confirmation of etiology q Brain biopsy (complications 3%) q Serologic analysis in serum and CSF: low sensitivity in the first 10 days. q CSF Cultures: negative q PCR in CSF: highly sensitive and specific. The diagnostic procedure of choice.
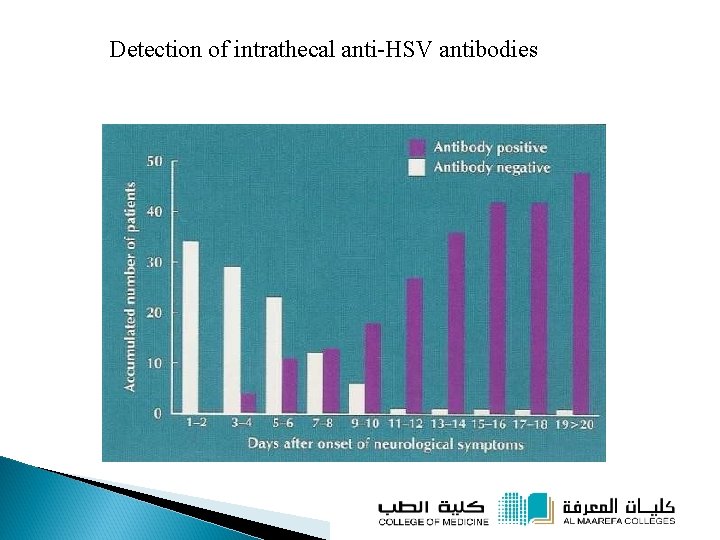
Detection of intrathecal anti-HSV antibodies
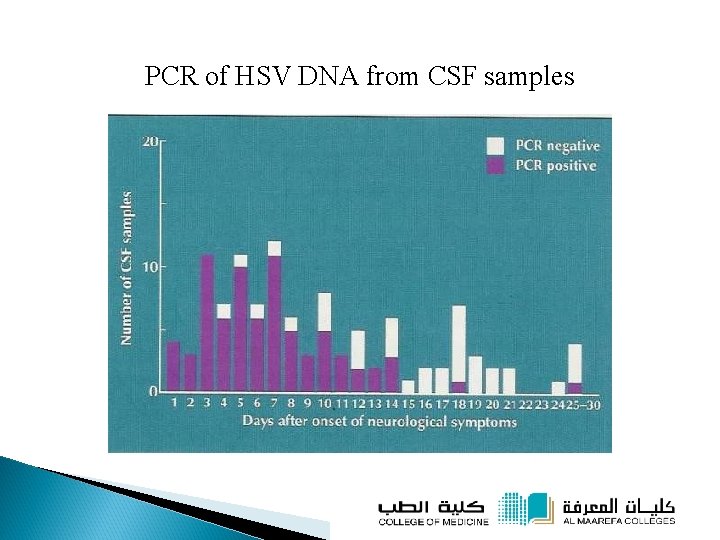
PCR of HSV DNA from CSF samples
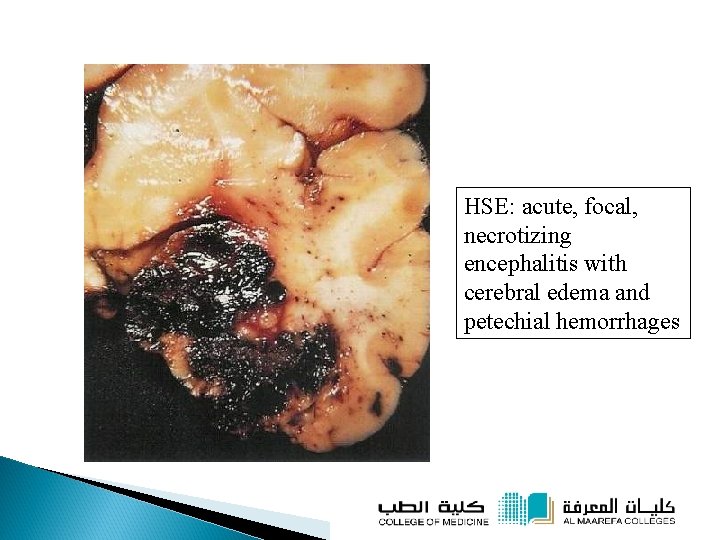
HSE: acute, focal, necrotizing encephalitis with cerebral edema and petechial hemorrhages

Herpes Simplex Encephalitis Treatment q Early therapy is a critical factor in outcome!!! q In suspected cases: start Acyclovir empirically q IV Acyclovir (10 mg/kg x 3/day over 1 hour) is effective in reducing the rates of death (70% 24%) and morbidity q If PCR negative and no other support for HSE, stop acyclovir

TB Meningitis Usually insidious: difficult to diagnose in early stages (fever 30%, URTI 20%) Rare in children in developed countries If untreated is usually fatal Meningitis usually occurs 3 -6 mths after primary infection 1 stage ( lasts 1 -2 wk, fever malaise, headache ) 2 stage (+/- suddenly, meningeal signs ) 3 stage (worsening neurological condition, death )

Mortality/Morbidity Bacterial meningitis: Overall mortality 510% Neonatal meningitis: 15 -20% Older children: 3 -10% Strep. pneumonia: 26 -30% H. influenza type B: 7 -10% N. meningitidis: 3. 5 -10% 30% neurological complications 4% Profound bilateral hearing loss (sensory neural) in all bacterial meningitis

Mortality/Morbidity Viral meningio-encephalitis: Enteroviral fewer complications Tuberculous meningitis: related to stage of disease Stage I (30%) morbidity. Stage II (56%) Stage III (94%)

- Slides: 43