Meningitis in HIV Diagnostic and Therapeutic Challenge Yunus






























- Slides: 33

Meningitis in HIV Diagnostic and Therapeutic Challenge Yunus Moosa AWACC- November 2015

Case: 59 yr. old female- 1 st Wk. Feb Known HIV positive since Oct 2014 on first line treatment Non specific symptoms- dizziness, malaise, lethargy, fatigue PMH: Cervical TB lymphadenitis – treated for 9 mths(2013) Chronic medication: – Tribuss – Ecotrin – Epilim CR 400 mg bid Clinically – shotty cervical L/N, otherwise NAD

Investigations FBC- 13. 3/255/4. 19 U&E- 136/4. 3/100/26/3. 2/60 (>89) LFT- 69/31/2 -1/107/19/15/12, CCa 2. 3, Mg 0. 83, PO 4 0. 88 HBV s. Ab positive HCV negative HAV negative RPR – negative, TSH normal, Total cholesterol 3. 6, LDL 2. 2, TGA 0. 80 CD 4 - 24 cell/u. L, VL 5420 (3. 734 Log 10) Chest x-ray: normal.

Management ATV/r (300/100)- 1 Daily AZT/3 TC (300/150) - 1 bid Cotrimoxazole- 960 daily Ecotrin 1 daily Epilim CR 400 mg bid

2 weeks later Brought in by family: two seizures at home Disoriented, responded appropriately to commands no meningism, no focal signs, no papilloedema. FBC- 14. 6/328/7. 25, U&E- 133/4. 7/97/20/4. 8/83 (>89) LFT- 84/38/17 -3/117/23/15/22, CCa 2. 28, Mg 0. 96, PO 4 1. 52 Contrast CTS- normal LP- pressure normal, CRAG > 1: 320, AFB negative. Date 22/02 Appearance Polys Xanthochromic 12 L/C 46 RBC Protein Glu Plasma Glu Ratio 0 11. 32 1. 1 7. 1 0. 15

What is the most likely diagnosis? 1. Cryptococcal meningitis 2. Tuberculosis 3. Histoplasmosis 4. CM IRIS 5. TB IRIS 6. Histoplasmosis IRIS 7. TB and CM 8. TB IRIS and CM IRIS

Repeat CSF 6 Days later Treatment was modified and LP repeated Date 22/02 28/02 Appearance Xanthochromic Blood stained Polys L/C 12 46 8 184 RBC Protein Glu Plasma Glu Ratio 0 11. 32 1. 1 7. 1 0. 15 +++ 4. 27 0. 2 7. 4 0. 03

What is the most likely diagnosis? 1. Cryptococcal meningitis 2. Tuberculosis 3. Histoplasmosis 4. CM IRIS 5. TB IRIS 6. Histoplasmosis IRIS 7. TB and CM 8. TB IRIS and CM IRIS

How would you manage this patient? 1. Continue ATV/r/AZT/3 TC and start AMB/FLZ 2. Continue ATV/r/AZT/3 TC and start AMB/FLZ and rifafour 3. Discontinue ART and start AMB/FLZ 4. Discontinue ART and start AMB/FLZ and rifafour 5. Change ART to LPV/r/AZT/3 TC and start AMB/FLZ 6. Change ART to LPV/r/AZT/3 TC and start AMB/FLZ & rifafour 7. Refer to someone who thinks they know more

Management ART stopped Started on AMB Started on rifafour Optimized dose of epilim Continued cotrimoxazole Continued ecotrin

What do you think is the most central diagnostic tool for TBM? 1. 2. 3. 4. 5. 6. 7. 8. Clinical presentation Blood investigations Immunologic tests – (IGRAS/PPD skin test) CSF-chemistry and cell counts CSF- microbiology CSF -molecular tests CSF – adenosine deaminase Imaging – (Cx. R/Brain CTS/MRI)

Presentation Time from symptom to presentation – Median 10 days – Range 1 day to 9 months Symptoms/Signs – low grade fever, malaise, headache, dizziness, vomiting – Personality changes, altered mental status – Stroke, hydrocephalus – Cranial neuropathies – Seizures uncommon - should prompt search for alternate diagnoses

Clinical Staging of TBM Stage I (early) Clinical signs and symptoms • Non specific symptoms • Few or no signs of meningism • Fully conscious and alert II (intermediate) • Signs of meningitis • Drowsiness and lethargy • Cranial nerve palsies III (late) Systemic toxicity Stupor or coma Severe neurologic deficit

CSF Cell count and Biochemistry Abnormalities -not pathognomonic L/C predominant pleocytosis Total WCC usually 100 - 500 cells/μL Earlier -lower counts, neutrophil predominance Elevated protein levels, typically between 1 g/L and 5 g/L Low glucose usually less than 2. 5 mmol/L CSF: plasma ratio <0. 5.

Microbiology of CSF Factors influence sensitivity of smear: – CSF volume – Timing delivery to the lab – Time to analysis – Technical expertise of lab- (30 min under 1000 x) AFB Smear – 1 sample sensitivity 20%– 40% – 4 samples sensitivity >85% (10– 15 m. L) Culture sensitivity 40– 80% Important to determine drug susceptibility.

What is the rate of CSF Production? 1. 5 mls/day 2. 10 mls/day 3. 50 mls/day 4. 100 mls/day 5. 500 mls/day 6. 1000 mls/day

What is the total volume of CSF in the CNS? 1. 50 -100 mls 2. 90 -150 mls 3. 200 -500 mls 4. 1000 -2000 mls

Adenosine Deaminase: ADA Meta-analysis: – Sensitivity 79% – Mean specificity 91% Specificity is low – levels seen in other CNS diseases like neurosarcoid, meningeal lymphoma, subarachnoid hemorrhage Not useful in HIV-positive patients. Journal of Clinical Medicine Research (2010), 2 (5), 220– 224, European Journal of Clinical Microbiology and Infectious Diseases (2004), 23 (6), 471– 476

CSF Molecular Tests Used as a rule in test – positive test confirms TBM Sensitivity of GXP is ~80% (50% in HIV neg) Negative test does not exclude TBM Health Technology Assessment (2007)11 (3), 1– 196

Imaging: CTS Widely used to aid diagnosis of TBM. Features suggestive of TBM – Basal meningeal enhancement (Sn 34%/Sp 75%) – Hydrocephalus (Sn 45%/Sp 75%) – Infarcts (Sn 44%/) – Tuberculoma(s) (Sn 31%) Radiologic interpretations are subjective- inter-radiologists reliability of findings suggestive of TBM is very poor. Basal meningeal enhancement was most unreliable feature PLo. S ONE 7(6): e 38982. doi: 10. 1371/journal. pone. 00389

Value of CSF as Monitoring Tool 1. Not worth the trouble 2. Somewhat valuable 3. Very valuable

The most useful/reliable objective measure of response to treatment 1. CSF Pressure 2. CSF Chloride 3. CSF glucose 4. CSF protein 5. CSF pleocytosis


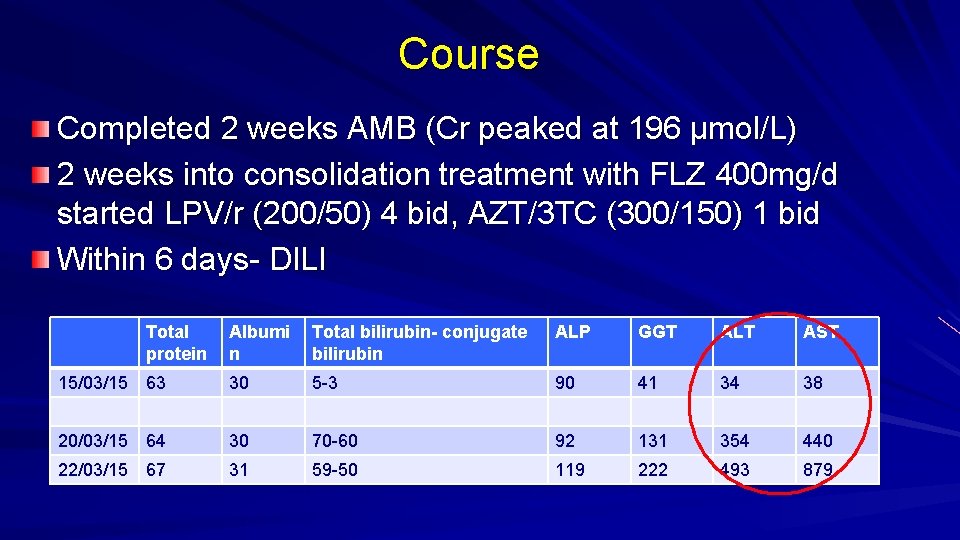
Course Completed 2 weeks AMB (Cr peaked at 196 µmol/L) 2 weeks into consolidation treatment with FLZ 400 mg/d started LPV/r (200/50) 4 bid, AZT/3 TC (300/150) 1 bid Within 6 days- DILI Total protein Albumi n Total bilirubin- conjugate bilirubin ALP GGT ALT AST 15/03/15 63 30 5 -3 90 41 34 38 20/03/15 64 30 70 -60 92 131 354 440 22/03/15 67 31 59 -50 119 222 493 879

Cause for DILI 1. 2. 3. 4. 5. 6. 7. Rifampicin Isoniazid PZA FLZ LPV/r AZT 3 TC

What ART do we use? 1. LPV/r, AZT, 3 TC 2. ATV/r, AZT, 3 TC 3. EFV, AZT, 3 TC 4. LPV/r, TDF, FTC 5. ATV/r, TDF, FTC 6. EFV, TDF, FTC

TB Treatment should we use? 1. INH, EMB, PZA, Rifampicin 2. INH, EMB, PZA, Rifabutin 3. INH, EMB, PZA, Moxifloxacin 4. INH, EMB, PZA, Streptomycin

Cytochrome P 450 enzymes essential for the metabolism of many drugs Induction increases synthesis of enzymes increases metabolism of target drug therapeutic failure – Effect is usually delayed Inhibition blocks activity of enzymes toxicity – Effect usually immediate – Often used to enhance levels of target drug

Rifampin and Cy. P 450 Not metabolized by the Cy. P 450 enzymes Potent inducer affects drugs metabolized by Cy. P 450 Do not modify dose when combined by Cy. P 450 modifiers Rifabutin and Cy. P 450 Metabolized by the Cy. P 450 enzymes Requires adjustment when combined with drugs that modify Cy. P 450 Poor inducer of Cy. P 450 minimal or no adjustment for drugs metabolized by Cy. P 450

How Dose of Rifabutin when using a PI 1. 450 mg daily 2. 300 mg daily 3. 150 mg daily 4. 150 mg 3 x / week

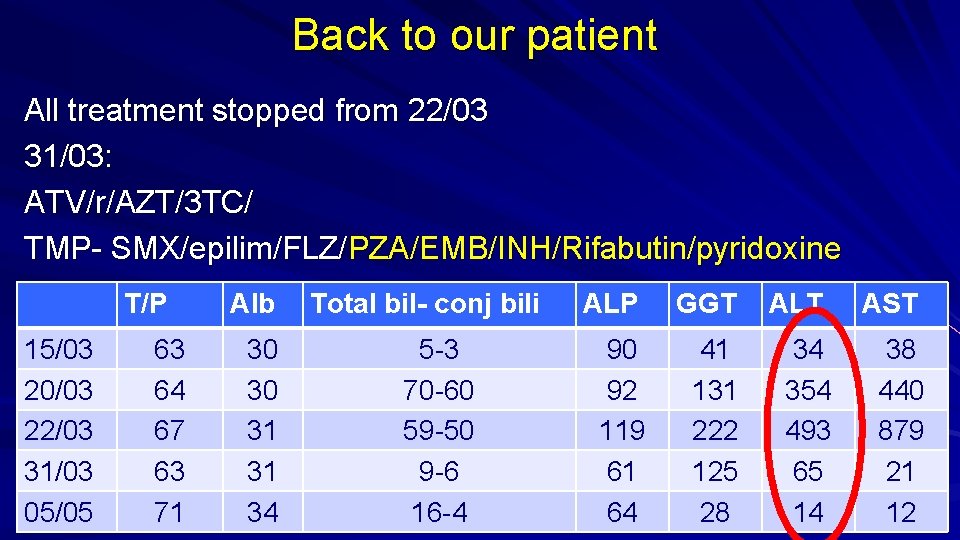
Back to our patient All treatment stopped from 22/03 31/03: ATV/r/AZT/3 TC/ TMP- SMX/epilim/FLZ/PZA/EMB/INH/Rifabutin/pyridoxine T/P 15/03 20/03 22/03 31/03 05/05 63 64 67 63 71 Alb 30 30 31 31 34 Total bil- conj bili 5 -3 70 -60 59 -50 9 -6 16 -4 ALP GGT ALT AST 90 92 119 61 64 41 131 222 125 28 34 354 493 65 14 38 440 879 21 12

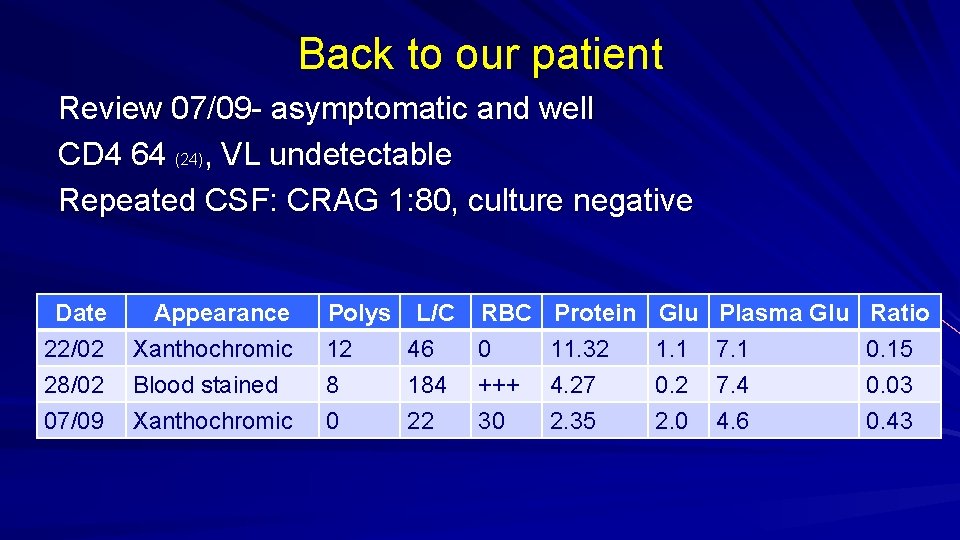
Back to our patient Review 07/09 - asymptomatic and well CD 4 64 (24), VL undetectable Repeated CSF: CRAG 1: 80, culture negative Date 22/02 28/02 07/09 Appearance Xanthochromic Blood stained Xanthochromic Polys L/C RBC 12 46 0 8 184 +++ 0 22 30 Protein 11. 32 4. 27 2. 35 Glu 1. 1 0. 2 2. 0 Plasma Glu 7. 1 7. 4 4. 6 Ratio 0. 15 0. 03 0. 43

Take home message The diagnosis of TBM is challenging Diagnosis is often based on clinical and CSF findings without definitive microbiologic confirmation CSF lacks sensitivity and specificity Send at least 6/8 mls CSF for proper microbiology evaluation Imaging is mainly of value in evaluating for complications and exclude alternate diagnosis Rifampicin can only be used with LVP/r and not any other PI. Drug of choice with any other PI is rifabutin