Meningitis brain abscess Encephalitis etc 1 2 Meningitis

Meningitis, brain abscess. Encephalitis etc 1
2

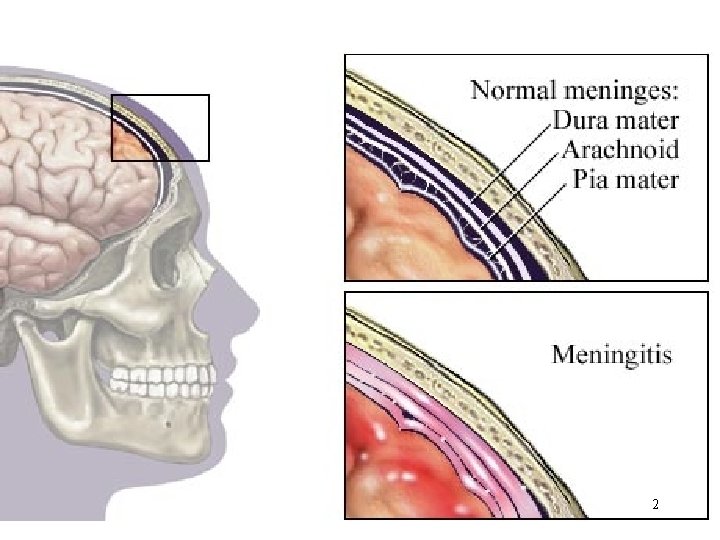
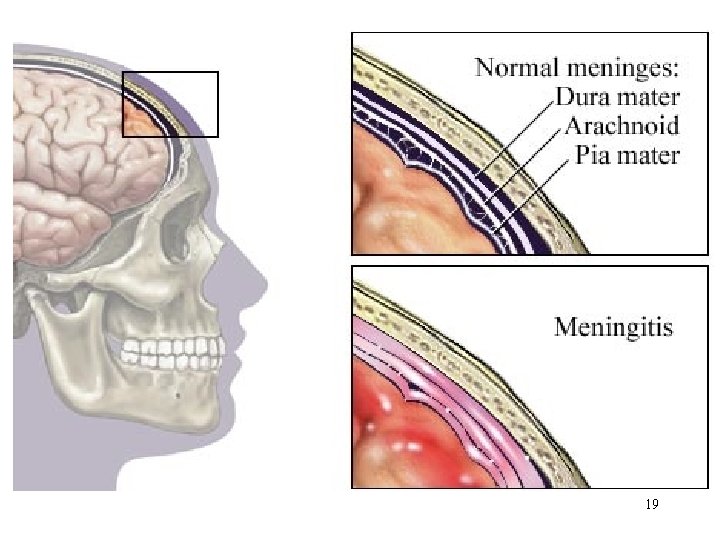
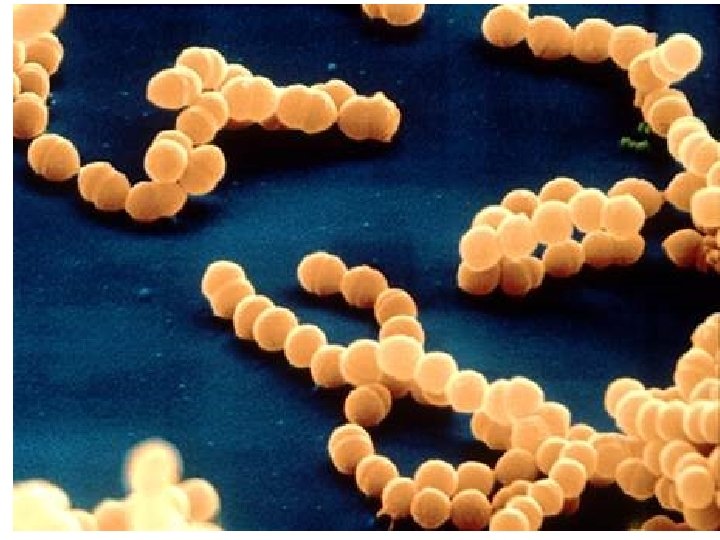
Meningitis • Inflammation of the meninges • Classified into aseptic and septic Aseptic : not bacteria. Virus or secondary to lymphoma, leukemia or brain abscess Septic : bacteria • Most common : Neisseria meningitidis, Haemophilus influenzae, Streptococcus pneumoniae • Factors that increase the risk of meningitis : viral URI, otitis media, mastoiditis 3
Pathophysiology • Infection through the blood stream as a consequence of other infections • Or by direct extension – traumatic injury to the facial bones or secondary to invasive procedures • Aids may predispose to meninges – mostly S. pneumoniae • The bacteria in the blood stream cross the bloodbrain barrier and cause inflammation of the meninges • Inflammatory cells from the meninges spill into the csf and the cell count in the csf increases 4

Complications of meningitis • • • Visual impairment Deafness Seizures Paralysis Hydrocephalus septic shock 5

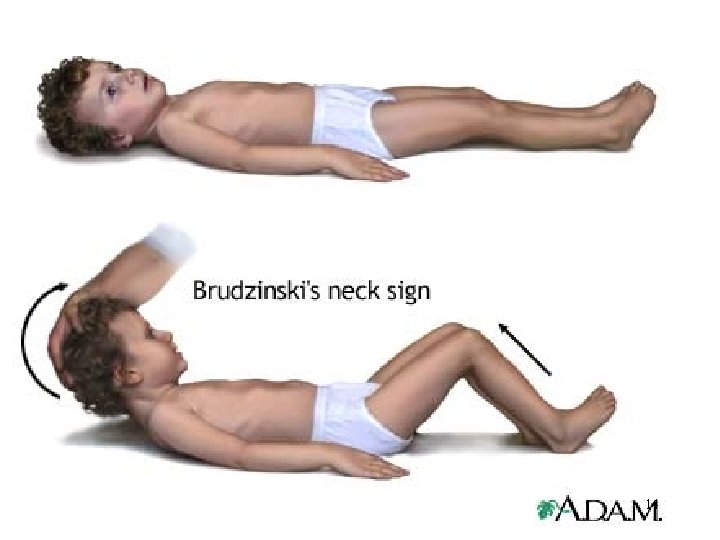
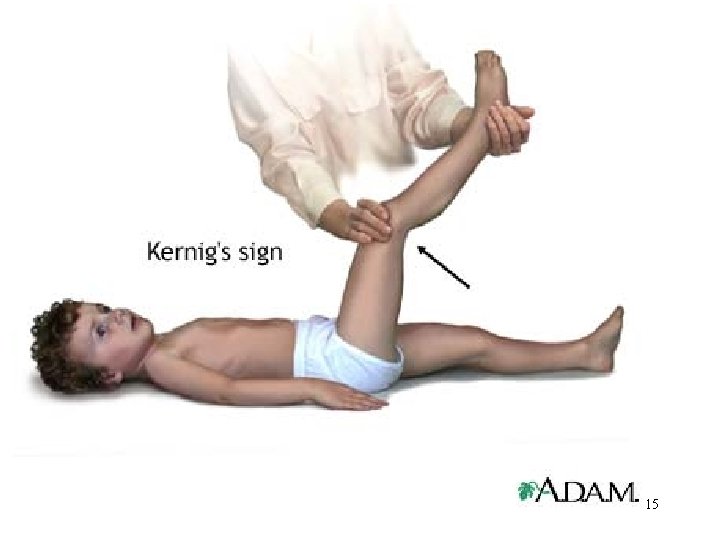
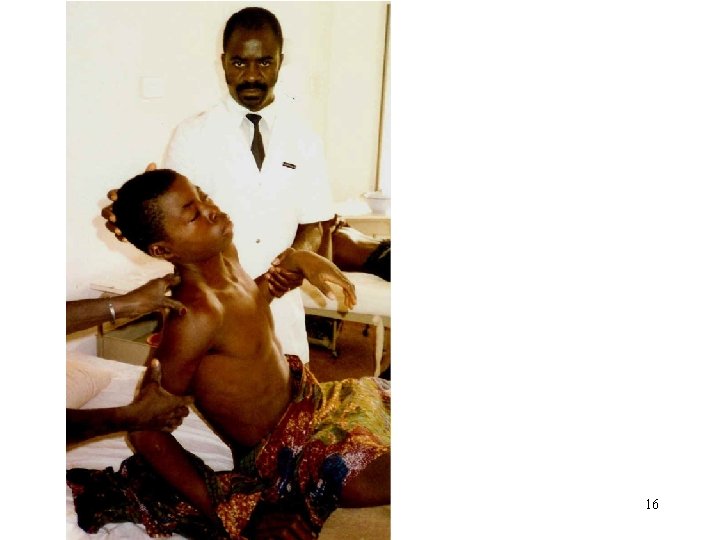
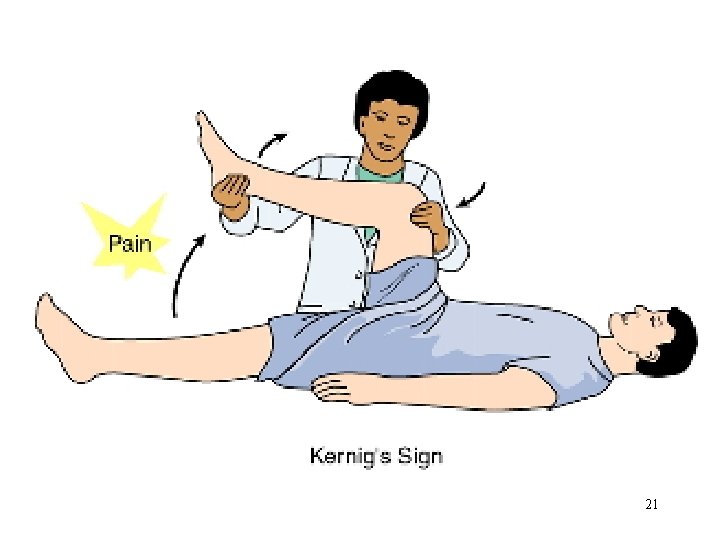
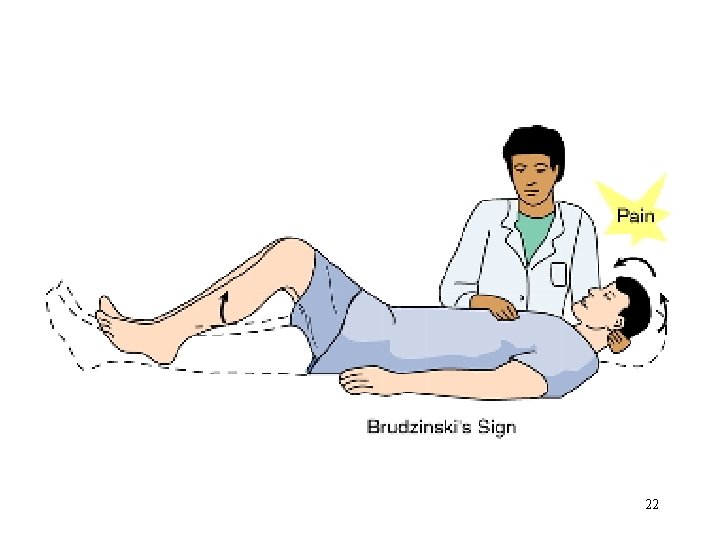
Clinical Manifestations • Headache (severe) • Fever (these two are initial symptoms)(high throughout the illness. ) • Signs of meningeal irritation : neck rigidity positive Kernig’s sign positive Brudzinski’s sign photophobia • A rash – N. meningitidis infection. Skin lesions develop, ranging from a petechial rash with purpuric lesions to large areas of ecchymosis. • Disorientation • Memory impairment 6

• • • Behavioural changes As the disease advances – lethargy Unresponsiveness Coma Seizures ↑ ICP – decreased level of consciousness and focal motor deficits – later herniation and cranial nerve dysfunction and depression of centres of vital function • Septicemia – high fever, extensive purpuric lesions intravascular coagulopathy (DIC). • Death 7

Assessment and diagnostic findings • Lumbar puncture – CSF culture and sensitivity, Gram’s staining, CSF analysis : the presence of polysaccharide antigen supports the diagnosis of bacterial meningitis. 8

Prevention • Vaccinating against meningococcal meningitis – college freshmen, people living in dormataries • Prophylactic treatment of people in contact with meningitis cases – rifampin, ciprofloxacin, ceftrioxone Na. 9

Medical Management • Penicillin antibiotics • Cephalosporins (eg ceftrioxone Na. , cefotaxime Na) • Vancomycin, in combination with rifampicin for resistant strains • Steroids 15 minutes befor the antibiotics • Dehydration and shock treated • Phenytoin for seizures • Increased ICP is treated as necessary 10

Nursing Management • Patient is usually critically ill • Neurologic status and vital signs are continually assessed. • Pulse oximetry and arterial blood gas values monitored • Respiratory support if needed • Increasing ICP compromises the brain stem. • Arterial blood pressures monitored – to predict shock and prevent cardiac or respiratory failure 11

Nursing Management • Rapid IV fluids may be needed • If fever + reduce temperature – (fever increased metabolic demand) • Monitor body weight, serum electrolytes and urine volume, specific gravity and osmolarity, esp. if the syndrome of inappropriate antidiuretic hormone secretion is suspected. 12

Nursing Management • Protect from injury secondary to seizure activity or altered level of consciousness • Prevent complications associated with immobility, such as pressure ulcers and pneumonia • Institute droplet precautions until 24 hours after the initiation of antibiotic therapy (oral and nasal discharge is considered infectious) • Communicate with the patient’s family and allow them to see the patient. Give them moral support 13
14
15
16
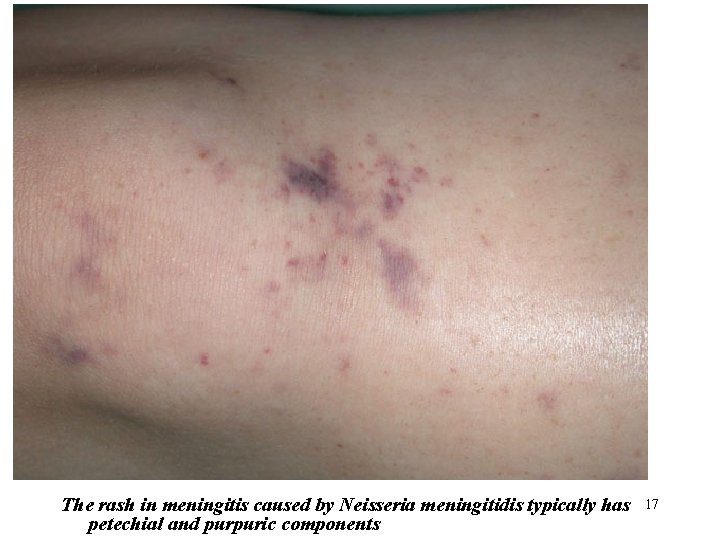
The rash in meningitis caused by Neisseria meningitidis typically has petechial and purpuric components 17
18
19
20
21
22
23
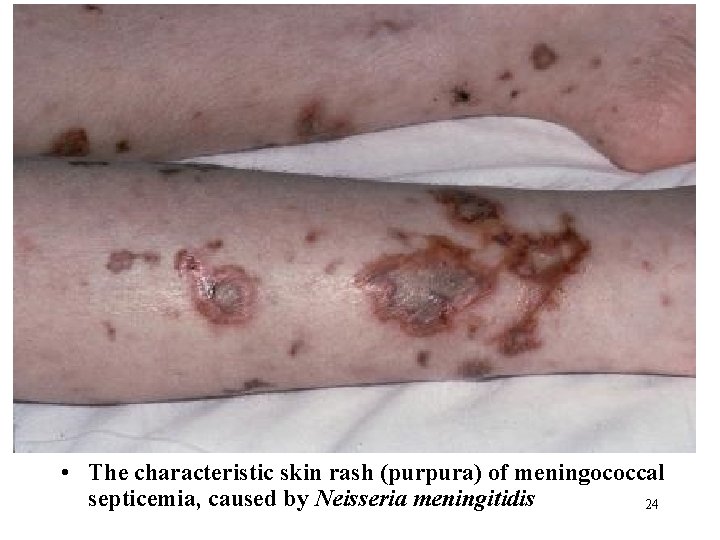
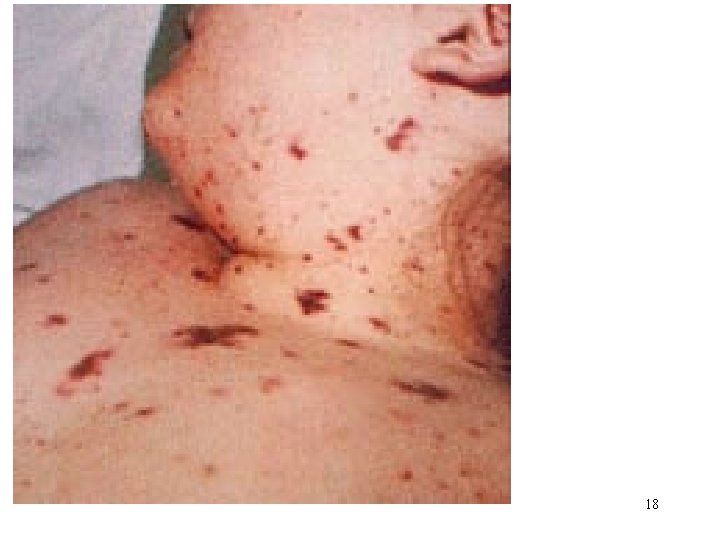
• The characteristic skin rash (purpura) of meningococcal septicemia, caused by Neisseria meningitidis 24

25

26

27
- Slides: 27