Meningitis and Encephalitis Diagnosis and Treatment Update Definitions









































- Slides: 54

Meningitis and Encephalitis: Diagnosis and Treatment Update

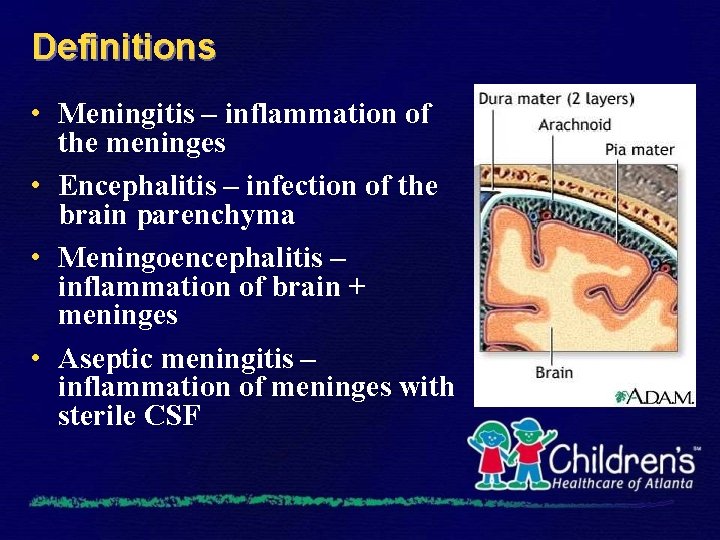
Definitions • Meningitis – inflammation of the meninges • Encephalitis – infection of the brain parenchyma • Meningoencephalitis – inflammation of brain + meninges • Aseptic meningitis – inflammation of meninges with sterile CSF

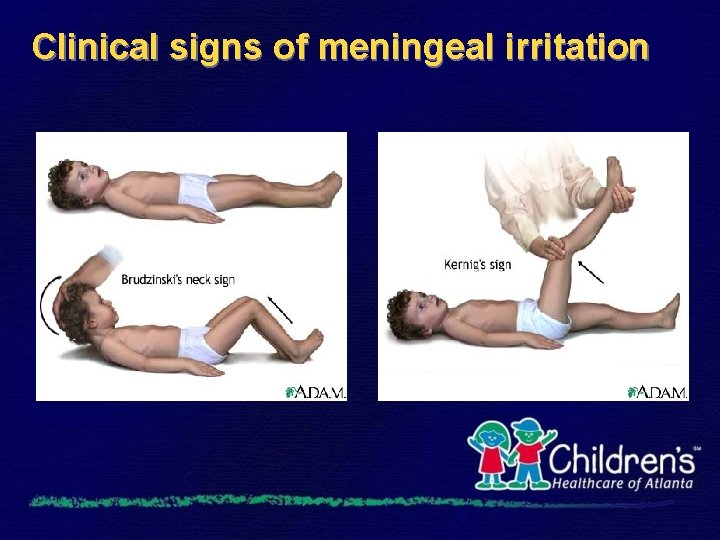
Symptoms of meningitis • Fever • Altered consciousness, irritability, photophobia • Vomiting, poor appetite • Seizures 20 - 30% • Bulging fontanel 30% • Stiff neck or nuchal rigidity • Meningismus (stiff neck + Brudzinski + Kernig signs)

Clinical signs of meningeal irritation

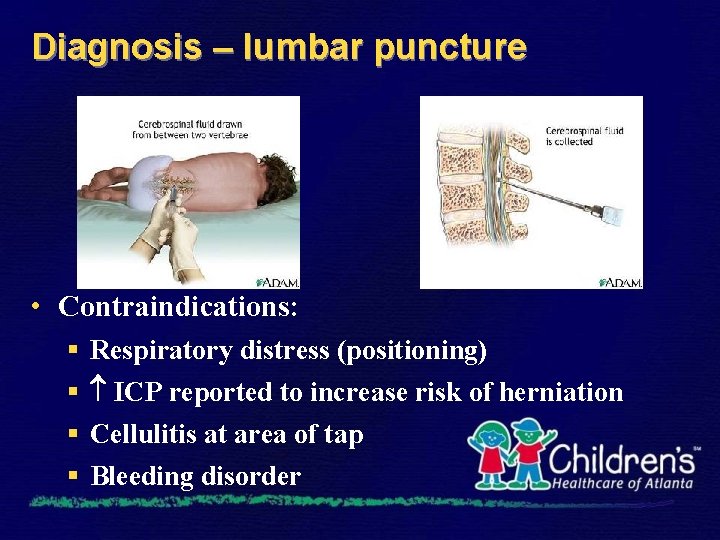
Diagnosis – lumbar puncture • Contraindications: § § Respiratory distress (positioning) ICP reported to increase risk of herniation Cellulitis at area of tap Bleeding disorder

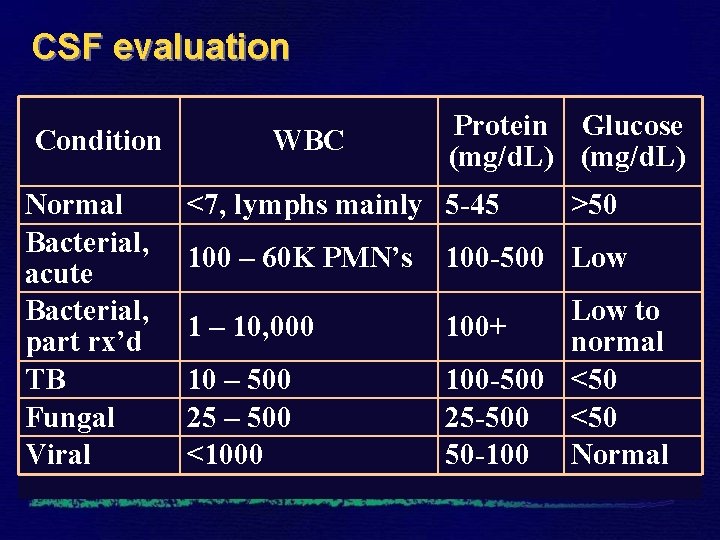
CSF evaluation Condition Normal Bacterial, acute Bacterial, part rx’d TB Fungal Viral WBC Protein Glucose (mg/d. L) <7, lymphs mainly 5 -45 >50 100 – 60 K PMN’s 100 -500 Low 1 – 10, 000 100+ 10 – 500 25 – 500 <1000 Low to normal 100 -500 <50 25 -500 <50 50 -100 Normal

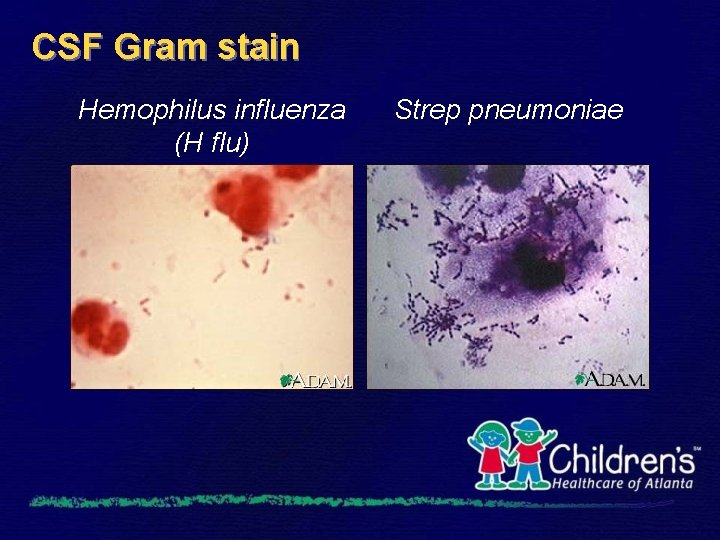
CSF Gram stain Hemophilus influenza (H flu) Strep pneumoniae

Not addressed • • • Indwelling CNS catheters S/P cranial surgery Anatomic defects predisposing to meningitis Immunocompromised patients Abscesses

Bacterial meningitis • 3 - 8 month olds at highest risk • 66% of cases occur in children <5 years old

Bacterial meningitis - Organisms • Neonates § Most caused by Group B Streptococci § E coli, enterococci, Klebsiella, Enterobacter, Samonella, Serratia, Listeria • Older infants and children § Neisseria meningitidis, S. pneumoniae, tuberculosis, H. influenzae

Bacterial meningitis – Clinical course • • Fever Malaise Vomiting Alteration in mental status Shock Disseminated intravascular coagulation (DIC) Cerebral edema § Vital signs § Level of mentation

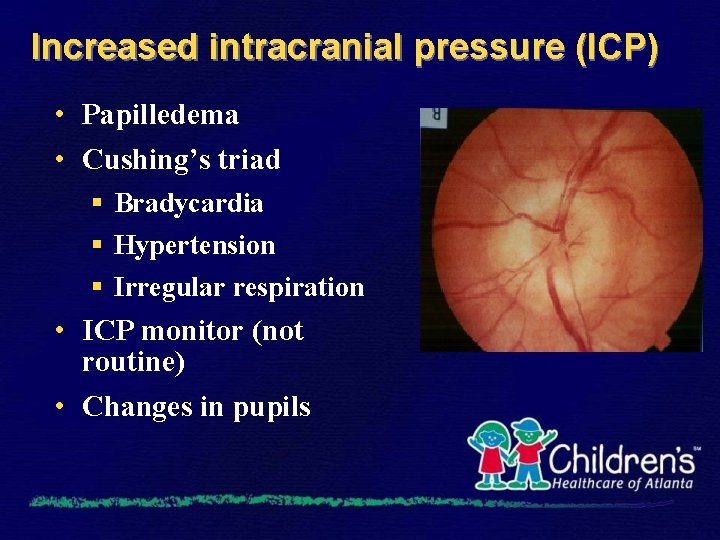
Increased intracranial pressure (ICP) • Papilledema • Cushing’s triad § Bradycardia § Hypertension § Irregular respiration • ICP monitor (not routine) • Changes in pupils

ICP treatment • 3% Na. Cl, 5 cc/kg over ~20 minutes • May utilize osmotherapy - if serum osms <320 • Mild hyperventilation § Pa. CO 2 <28 may cause regional ischemia § Typically keep Pa. CO 2 32 -38 torr • Elevate HOB 30 o

Meningitis - Fluid management • Restore intravascular volume & perfusion • Monitor serum Na+ (osmolality, urine Na+): § If serum Na+ <135 m. Eq/L then fluid restrict (~2/3 x), liberalize as Na+ improves § If severely hyponatremic, give 3% Na. Cl • SIADH § 4 - 88% in bacterial meningitis § 9 - 64% in viral meningitis • Diabetes insipidus • Cerebral salt wasting

Meningitis - Treatment duration • • Neonates: 14 – 21 days Gram negative meningitis: 21 days Pneumococcal, H flu: 10 days Meningococcal: 7 days

Bacterial Meningitis - Treatment Neonatal (<3 mo) • Ampicillin (covers Listeria) + • Cefotaxime § High CSF levels § Less toxicity than aminoglycosides § No drug levels to follow § Not excreted in bile not inhibit bowel flora

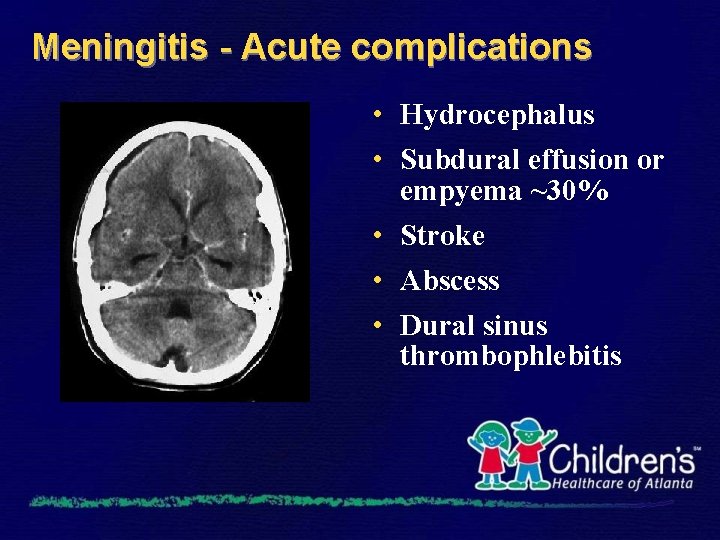
Meningitis - Acute complications • Hydrocephalus • Subdural effusion or empyema ~30% • Stroke • Abscess • Dural sinus thrombophlebitis

Bacterial meningitis - Outcomes • Neonates: ~20% mortality • Older infants and children: § <10% mortality § 33% neurologic abnormalities at discharge § 11% abnormalities 5 years later • Sensorineural hearing loss 2 - 29%

Bacterial meningitis - children • • Strep pneumoniae Neisseria meningitidis TB Hemophilus influenza

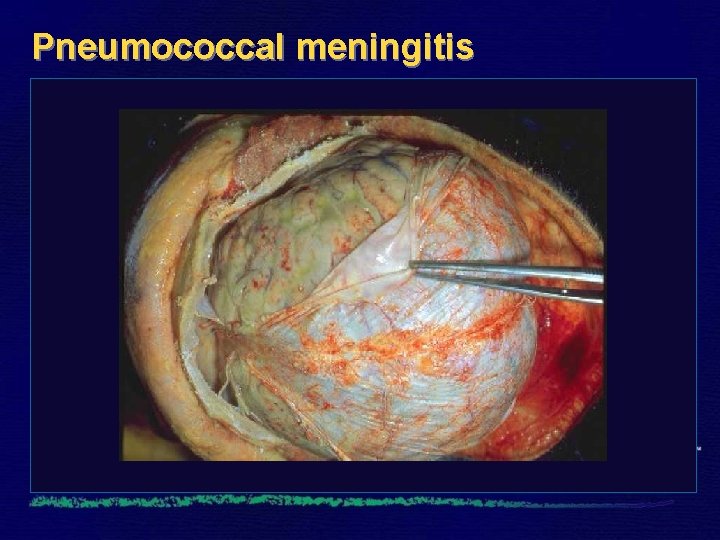
Pneumococcal meningitis

Antibiotic susceptibility • Susceptible • Non-susceptible • Resistant

Pneumococcal resistance • Strep pneumococcus - most common cause of invasive bacterial infections in children >2 months old • Incidence of PCN-, cefotaxime- & ceftriaxonenonsusceptible isolates has ’d to ~40% • Strains resistant to PCN, cephalosporins, and other -lactam antibiotics often resistant to trimethoprim-sulfamethoxazole (Bactrim™, Septra™), erythromycin, chloramphenicol, tetracycline

Mechanism of resistance • PCN-binding proteins synthesize peptidoglycan for new cell wall formation • PCN, cephalosporins, and other -lactam antibiotics kill S pneumoniae by binding irreversibly to PCN-binding proteins located in the bacterial cell wall • Chromosomal changes can cause the binding affinity for the -lactam antibiotics to decrease

Pneumococcal meningitis – Mgmt • Vancomycin + cefotaxime or ceftriaxone, if > 1 month old • If hypersensitive (allergic) to -lactam antibiotics, use vancomycin + rifampin • D/C vancomycin once testing shows PCNsusceptibility • Consider adding rifampin if susceptible & condition not improving, or cefotaxime or ceftriaxone MIC high • Not vancomycin alone

Antibiotic use in Pneumococcal meningitis • PCN-susceptible organism: § § Pen. G 250, 000 - 400, 000 U/kg/day Q 4 - 6 h Ceftriaxone 100 mg/kg/day Q 12 - 24 h Cefotaxime 225 - 300 mg/kg/day Q 8 h Chloramphenicol 50 - 100 mg/kg/day Q 6 h • Adequate cephalosporin levels in CSF ~2. 8 hours after dose administration

Vancomycin use in pneumococcal meningitis • Combination therapy since late 90’s • At initiation§ Baseline urinalysis § BUN and creatinine • Enters the CSF in the presence of inflamed meninges within 3 hours • Should not be used as solo agent, but with cephalosporin for synergy

Vancomycin use in pneumococcal meningitis • Vancomycin 60 mg/kg/day Q 6 h • Trough levels immediately before 3 rd dose • (10 -15 mcg/m. L or less) • Peak serum level 30 -60 minutes after completion of a 30 -minute infusion (35 -40 mcg/m. L)

Other antibiotics in pneumococcal meningitis (resistant) • Meropenem • Rifampin § Carbapenem § 20 mg/kg/day Q 12 § 120 mg/kg/day Q 8 h § Not a solo agent § seizure incidence, not generally used in meningitis § Slowly bactericidal § Resistance reported

Dexamethasone use in meningitis • Consider if H flu & S pneumo meningitis & > 6 wks old 0. 6 mg/kg/day Q 6 h x 2 d • local synthesis of TNF- , IL-1, PAF & prostaglandins resulting in BBB permeability, meningeal irritation • Debate if it incidence of hearing loss • If used, needs to be given shortly before or at the time of antibiotic administration • May adversely affect the penetration of antibiotics into CSF

Pneumococcal meningitis - Treatment • LP after 24 -48 hours to evaluate therapy if: § § Received dexamethasone PCN-non-susceptible MIC’s not available Child’s condition not improving

Infection control precautions (invasive pneumococcus) • CDC recommends Standard Precautions • Airborne, Droplet, Contact are NOT recommended • Nasopharyngeal cultures of family members and contacts is NOT recommended • No isolation of contacts • No chemoprophylaxis for contacts

Meningococcal meningitis • Neisseria meningitidis • ~10 - 15% with chronic throat carriage • Outbreaks in households, high schools, dorms § Accounts for <5% of cases • 2, 400 - 3, 000 cases occur in the USA each year • Peaks <2 years of age & 15 -24 years

Meningococcal disease • Can cause purulent conjunctivitis, septic arthritis, sepsis +/- meningitis • Diagnose presence of organism (Gram negative diplococci) via: § § § CSF Gram stain, culture Sputum culture CSF (not urine) Latex agglutination Petechial scrapings Buffy coat Gram stain

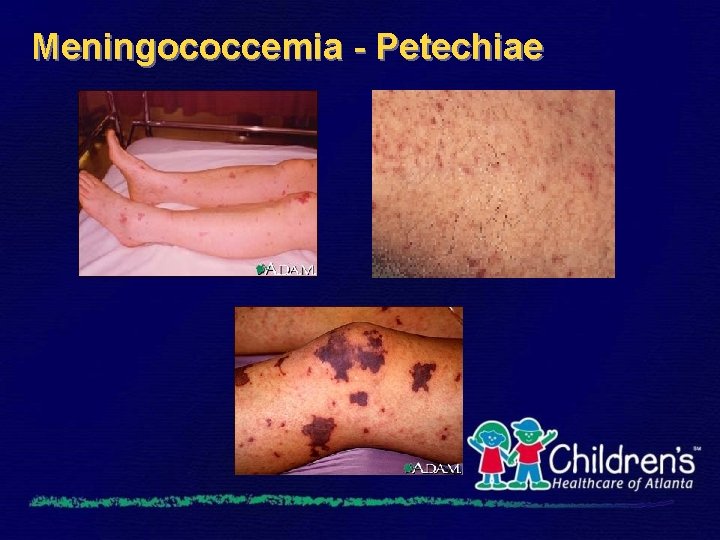
Meningococcemia - Petechiae

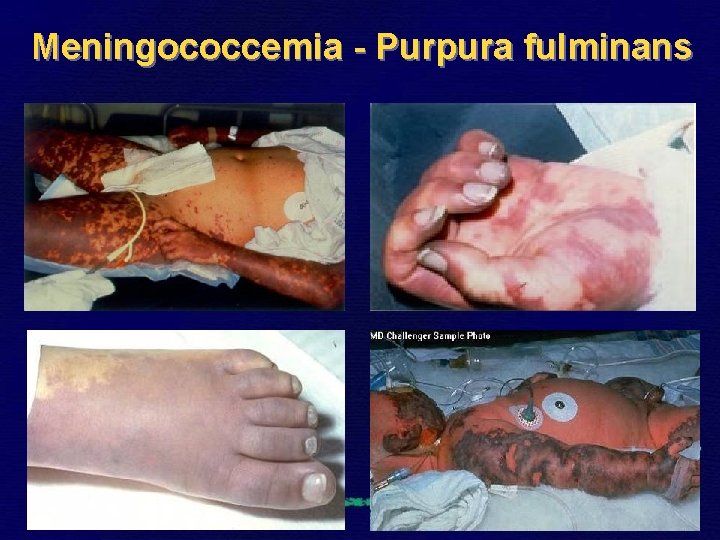
Meningococcemia - Purpura fulminans

Meningococcemia - Isolation • Capable of transmitting organism up to 24 hours after initiation of appropriate therapy • Droplet precautions x 24 hours, then no isolation • Incubation period 1 - 10 days, usually <4 days

Meningococcemia - Treatment • Antibitotic resistance rare • Antibitotics: § PCN § Cefotaxime or Ceftriaxone • Patient should get rifampin prior to discharge

Meningococcal disease - Care takers • Day care where child attends >25 h/wk, kids are >2 years old, & 2 cases have occurred • Day care where kids not all vaccinated • Persons who have had “intimate contact” w/ oral secretions prior & during 1 st 24 h of antibiotics • “Intimate contact” – 300 -800 x risk (kissing, eating/ drinking utensils, mouth-to-mouth, suctioning, intubating)

Meningococcemia - Prophylaxis • No randomized controlled trials of effectiveness • Treat within 24 hours of exposure • Vaccinate affected population, if outbreak

Meningococcemia - Prophylaxis • Rifampin § Urine, tears, soft contact lenses orange; OCP’s ineffective § <1 mo 5 mg/kg PO Q 12 x 2 days § >1 mo 10 mg/kg (max 600 mg) PO Q 12 x 2 days • Ceftriaxone § 12 y 125 mg IM x 1 dose § >12 y 250 mg IM x 1 dose • Ciprofloxacin § 18 y 500 mg PO x 1 dose

Meningococcal meningitis - Outcomes • Substantial morbidity: 11% - 9% of survivors have sequelae § Neurologic disability § Limb loss § Hearing loss • 10% case-fatality ratio for meningococcal sepsis • 1% mortality if meningitis alone

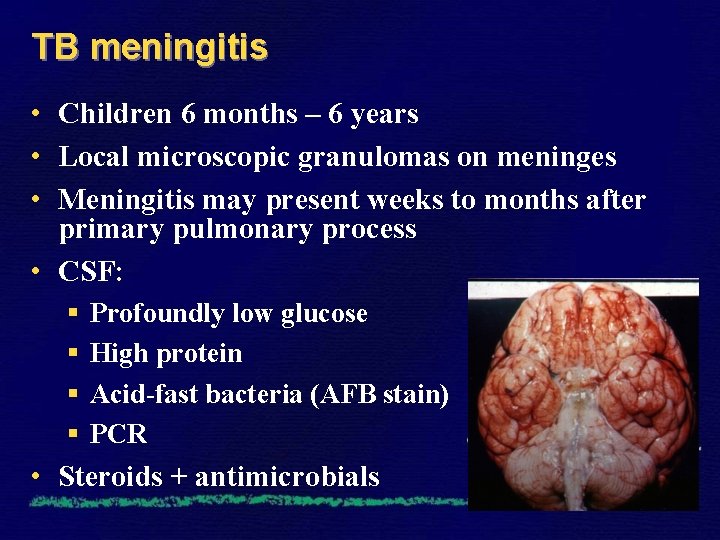
TB meningitis • Children 6 months – 6 years • Local microscopic granulomas on meninges • Meningitis may present weeks to months after primary pulmonary process • CSF: § § Profoundly low glucose High protein Acid-fast bacteria (AFB stain) PCR • Steroids + antimicrobials

Aseptic vs. partially treated bacterial meningitis • Aseptic much more common • Gram stain positive CSF: § 90 - 100% in young patients § 50 - 68% positive in older children • If CSF fails to show organisms in a pretreated patient, then very unlikely that organism is resistant

Viral meningitis • Summer, fall • Severe headache • Vomiting • Fever • Stiff neck • CSF - pleocytosis (monos), NL protein, NL glucose

Etiology viral meningitis • Enteroviruses predominate • Less common: § Mumps § Spring, summer § HIV § Oral-fecal route § Lymphocytic choriomeningitis § ± initial GI symptoms § Meningitic symptoms appear 7 -10 days after exposure § HSV-2

Other causes of aseptic meningitis • Leptospira § § Young adults Late summer, fall Conjunctivitis, splenomegaly, jaundice, rash Exposure to animal urine • Lyme Disease (Borrelia burgdorferi) § Spring-late fall § Rash, cranial nerve involvement

Viral meningitis - Treatment • • • Supportive No antibiotics Analgesia Fever control Often feel better after LP No isolation - Standard precautions

Viral meningitis - Outcomes • Adverse outcomes rare • Infants <1 year have higher incidence of speech & language delay

Meningoencephalitis - etiology • Herpes simplex type 1 • Rabies • Arthropod-borne § § § St. Louis encephalitis La Crosse encephalitis Eastern equine encephalitis West Nile

Herpes simplex 1 encephalitis • Symptoms § § § Depressed level of consciousness Blood tinged CSF Temporal lobe focus on CT scan or EEG + PCR Neonates typically will have cutaneous vessicles • Treatment - IV acyclovir

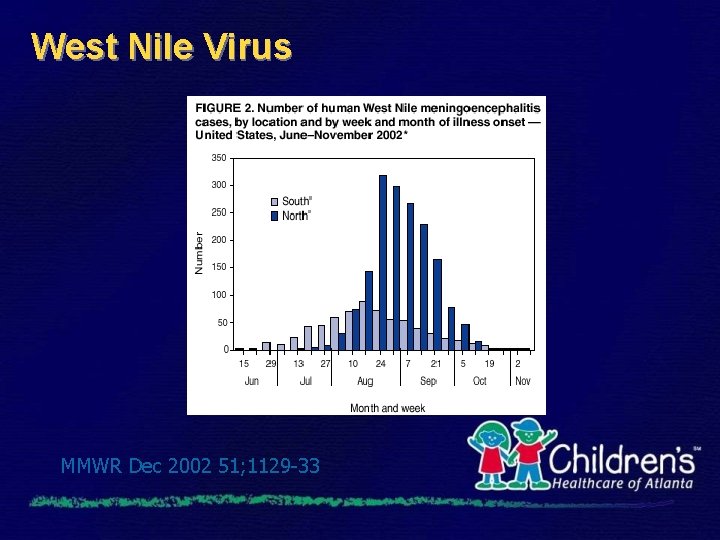
West Nile Virus • Via bite of infected mosquito • Incubation period 3 - 14 days • 1 in 150 infected persons get encephalitis § 4% of those are <20 years of age • H/A, fever, neck stiffness, stupor, coma, convulsions, weakness, & paralysis • Supportive therapy • Mortality 9%

West Nile Virus MMWR Dec 2002 51; 1129 -33

Summary • Antibiotics ASAP, even if LP not yet done • Vanco + cephalosporin until some identification known § CSF, Latex, exam • Isolate if bacterial x 24 hours, Universal Precautions • Monitor for status changes § § § Pupils, LOC, HR, BP, resp Seizures Hemodynamics DIC, coagulopathy Fluid, electrolyte issues
