Melbourne Medical School Thyroid disorders Hyper and hypothyroidism


Melbourne Medical School Thyroid disorders Hyper- and hypothyroidism Deepak Dutta Richard O’Brien

Learning objectives By the end of this session, students should be able to • Describe the common conditions that can lead to hyper and hypo functioning of the thyroid gland • List the clinical features of hyperthyroidism and hypothyroidism • Understand thyroid function tests and interpret abnormalities • List the appropriate radiological or nuclear medicine imaging tests to diagnose common thyroid disorders • Describe the different therapeutic agents used to treat thyroid disease • Explain how to monitor the thyroid status of a patient once treated NOTE: Thyroid nodules and thyroid cancer will be covered in a separate clinical colloquium

A quick epidemiology Thyroid problems are not uncommon Women are affected much more often than men Lifetime risk of thyroid disease in a woman is about 20% Can sometimes cause serious morbidity and even mortality • Often undiagnosed – important especially in pregnancy/peripartum and in cardiac disease • Inappropriate investigation can waste resources and lead to unnecessary anxiety • •

What can go wrong with the thyroid? • Decreased function - hypothyroidism • Increased function – hyperthyroidism • Enlargement – nodular disease – Obstructive symptoms – Cosmetic concerns • Inflammation • Cancer

Mrs Elena Varshavsky 62 y. o HTN on enalapril Type 2 diabetes (well-controlled) on gliclazide IHD with previous PTCA and stent, on a statin, aspirin, atenolol. Stable, asymptomatic, reasonable exercise tolerance • Complains of gradual increase in weight (79 to 86 kg in the last 2 years since diagnosis of DM and IHD) • “Always tired” • •

Mrs Elena Varshavsky • Could she be hypothyroid? • What other causes might there be for her symptoms? • What further questions should you ask? • What should you particularly look for in the examination?

Hypothyroidism - symptoms • Malaise, tiredness, myalgia, depression • Cold intolerance, constipation, weight gain • Delayed tendon reflexes, bradycardia, myxoedema, voice change, myopathy, hypothermia, effusions • These symptoms and signs are not very sensitive or specific

Causes of hypothyroidism Primary • Autoimmune hypothyroidism: Hashimoto's thyroiditis, atrophic thyroiditis • Iatrogenic: 131 I treatment, subtotal or total thyroidectomy, external irradiation of neck for lymphoma or cancer • Drugs: iodine excess (including iodine-containing contrast media and amiodarone), lithium, antithyroid drugs, p-aminosalicyclic acid, interferon- and other cytokines, aminoglutethimide • Congenital hypothyroidism: absent or ectopic thyroid gland, dyshormonogenesis, TSH-R mutation • Iodine deficiency • Infiltrative disorders: amyloidosis, sarcoidosis, hemochromatosis, scleroderma, cystinosis, Riedel's thyroiditis Transient • Silent thyroiditis, including postpartum thyroiditis • Subacute thyroiditis • Withdrawal of thyroxine treatment in individuals with an intact thyroid • After 131 I treatment or subtotal thyroidectomy for Graves' disease Secondary • Hypopituitarism: tumors, pituitary surgery or irradiation, infiltrative disorders, Sheehan's syndrome, trauma, genetic forms of combined pituitary hormone deficiencies • Isolated TSH deficiency or inactivity • Hypothalamic disease: tumors, trauma, infiltrative disorders, idiopathic

Mrs Elena Varshavsky What tests should be done?
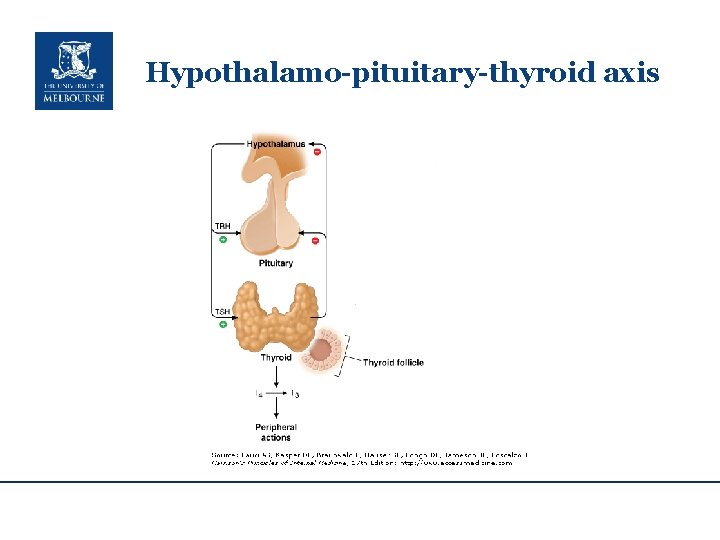
Hypothalamo-pituitary-thyroid axis
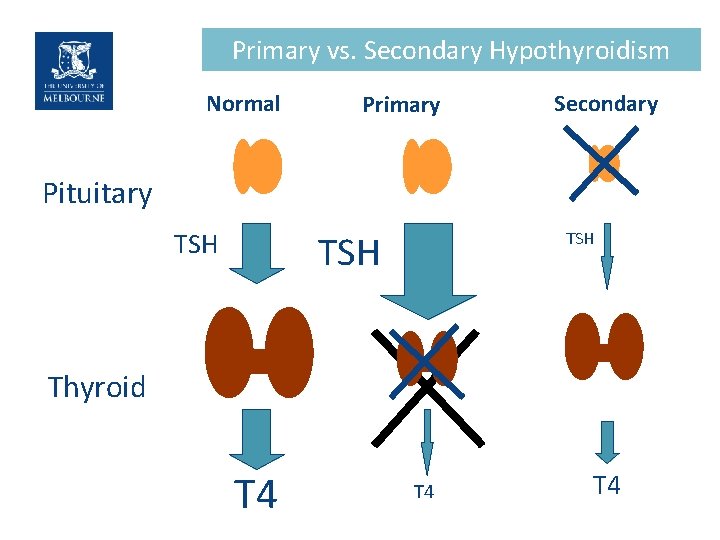
Primary vs. Secondary Hypothyroidism Normal Primary Secondary Pituitary TSH TSH Thyroid T 4 T 4

Hypothyroidism – diagnosis • Check TSH • Reconfirm elevated TSH, confirm FT 4 is low – (some weeks apart? ) • Correlate with symptoms and clinical examination • Consider a thyroid ultrasound only if there is a palpable goitre • No need for a nuclear scan • Anti-thyroid antibodies (anti-thyroid peroxidase TPO) can sometimes be helpful in this situation – especially if the TSH is borderline elevated

Hypothyroidism – treatment • Is the diagnosis confirmed? • Is treatment required? – Could the hypothyroidism be transient? • Is the patient post-partum? • Thyroiditis? • Are there any modifying factors? – Is the patient pregnant? – Ischaemic heart disease – Elderly, frail

Hypothyroidism – treatment • Usually 75 -150 mcg/day, single dose • Some patients – 50 or even 25 mcg/day as a starting dose • Aim for TSH in the low normal range

Hypothyroidism – treatment • Only adjust thyroxine dose after 6 -8 weeks • There is no hurry except in pregnancy • To be taken separately from medications that may decrease thyroxine absorption – Iron tablets – Calcium tablets – Antacids – Cholestyramine

Common mistakes • Rechecking TFTs earlier than 6 weeks (except in pregnancy) • Adjusting treatment earlier than 6 weeks • Requesting a nuclear scan in hypothyroidism

Mrs Jane Smith • Mrs Jane Smith – 33 y. o. – Secretarial work – 2 children aged 9 and 7, husband 2 month history of – Tiredness (“feel totally washed out”) – Palpitations (“rapid heart beat”), panic – Shortness of breath at times – Insomnia (difficulty sleeping, waking with palpitations)

• What are some possible diagnoses? • What further questions would you like to ask?

• What are some possible diagnoses? – Caffeine or cola drinks in excess – Thyrotoxicosis – Anxiety or panic disorder – A primary pulmonary or cardiac disorder • What further questions would you like to ask?

What are the symptoms of thyrotoxicosis?

• What further questions would you like to ask? – Intake of caffeine/cola/energy drinks – Any • • • Heat intolerance Loss of weight Increase in appetite Increase in sweating Tremulousness Anxiety, emotional lability Loss of hair Increased frequency of bowel movements Menstrual irregularity

Mrs Jane Smith • Family history of thyroid problems (mother, sister) • Weight loss (from 74 to 68 kg in 6 months) • Increased frequency of bowel movements (not diarrhoea) • Emotional lability

Hyperthyroidism - causes • Graves’ disease • Toxic nodular goitre – Multinodular – Solitary adenoma • Iodine-induced – Radiographic contrast – Naturopathic remedies – Amiodarone • Factitious (surreptitious thyroxine use) • Transient (with thyroiditis)

Mrs Jane Smith • What will you particularly look for in the examination?

Mrs Jane Smith • What will you particularly look for in the examination? – Heart rate and rhythm (any AF? ) – Tremor – Skin, nail and hair changes (often normal) – Thyroid size, consistency, bruit • May have a diffuse soft goitre • May have a bruit over the thyroid – Usually no cervical lymph nodes

Mrs Jane Smith • Eyes – (these changes may not be present in many patients) • Redness, irritation • Staring appearance • Mild double vision on right extreme gaze http: //www. endocrinesurgery. net. au/

Mrs Jane Smith • What is the diagnosis? • What investigations may help – Confirm hyperthyroidism – Confirm the cause

Hyperthyroidism - tests • • TSH is very low – less than 0. 1 FT 4 and/or FT 3 are elevated (why “free” T 4 and. T 3? ) Re-confirm the result Consider a nuclear scan – Not in pregnancy – Distinguishes between Graves’ disease, toxic nodular disease, iodine or thyroiditis-induced thyrotoxicosis and factitious • Antibodies against the TSH receptor are often present in high titres and may help confirm the cause of thyrotoxicosis and provide some prognostic information
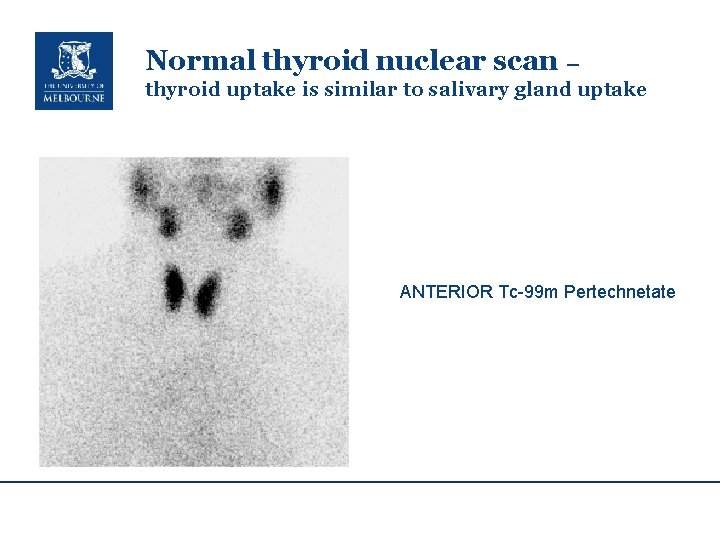
Normal thyroid nuclear scan – thyroid uptake is similar to salivary gland uptake ANTERIOR Tc-99 m Pertechnetate
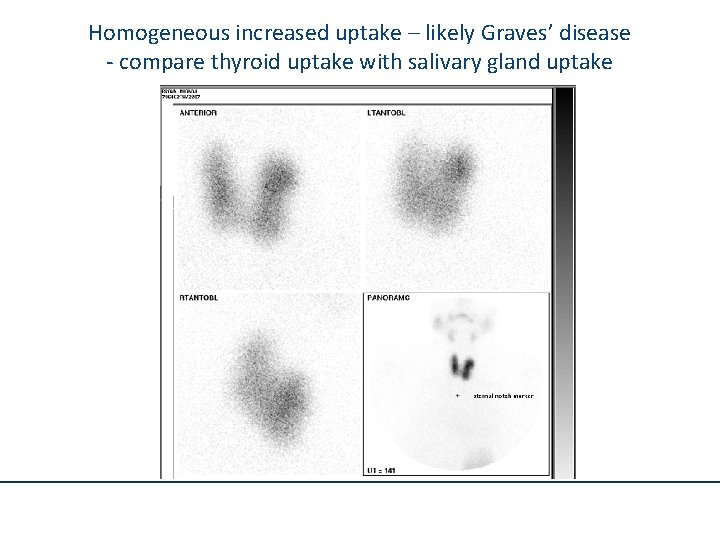
Homogeneous increased uptake – likely Graves’ disease - compare thyroid uptake with salivary gland uptake
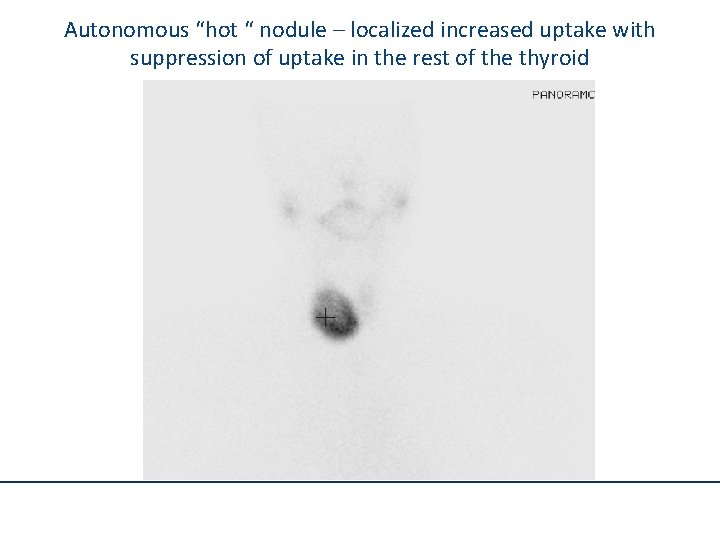
Autonomous “hot “ nodule – localized increased uptake with suppression of uptake in the rest of the thyroid
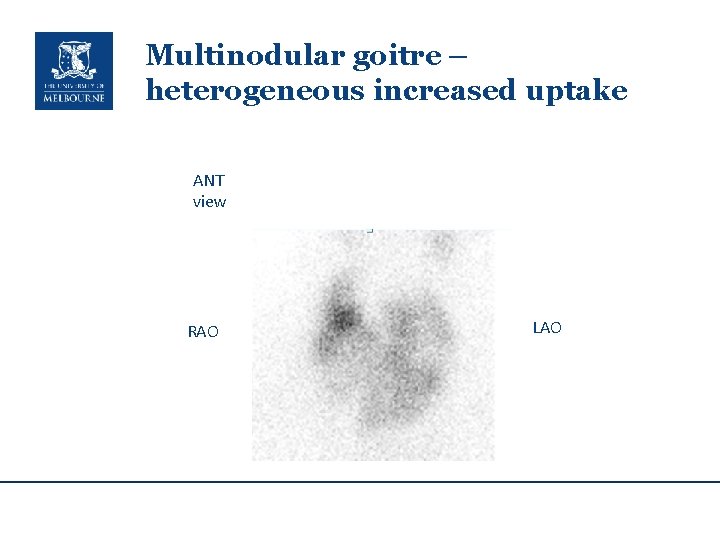
Multinodular goitre – heterogeneous increased uptake ANT view RAO LAO

Mrs Norma Bolton • • • 74 y. o. Widowed, active, independent, living alone Usually able to walk long distances HTN, ex-smoker On perindopril for HTN, no other medications • Now presents with dyspnoea – now SOB on walking 50 m or gardening – Aware of palpitations sometimes when SOB – Weight stable, no chest pain, ankle oedema

Mrs Norma Bolton • Specific questioning unrevealing • Examination – – – Af 96 JVP not elevated, no ankle oedema Minimal basal crepitations Cardiac examination normal Small multinodular goitre (longstanding), non-tender No abnormal cervical LN

Mrs Norma Bolton • What tests should be done? • In older patients especially, hyperthyroidism may have few symptoms or signs
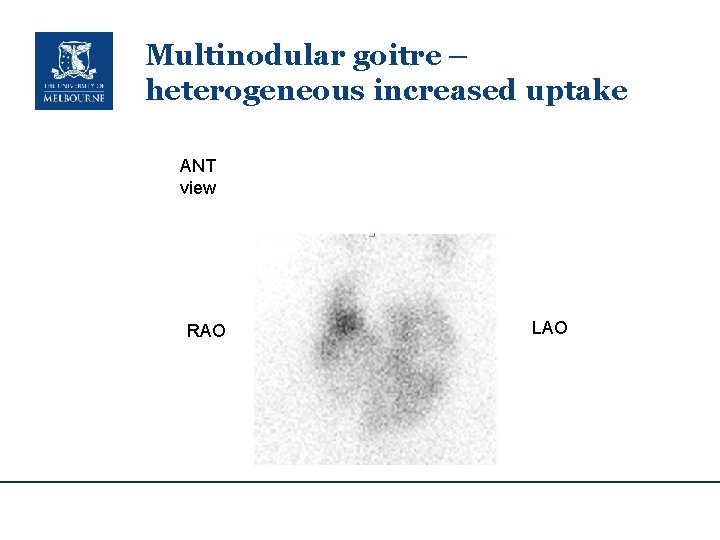
Multinodular goitre – heterogeneous increased uptake ANT view RAO LAO

Hyperthyroidism - treatment • Antithyroid drugs – Carbimazole – Propylthiouracil • Radioactive iodine • Surgery – Only if there are other reasons • Adverse reactions to drugs • Cosmetic/patient preference • Risk of malignancy

Antithyroid drugs • May be “curative” in Graves’ disease • Not curative but useful in toxic nodular disease • Can be used in pregnancy and lactation • Small risk of allergy • Very small risk of agranulocytosis

Antithyroid drugs • In Graves’ disease – Need to treat for 12 -18 months – Usually 10 to 40 mg carbimazole a day in divided doses) – Adjust dose ever 6 weeks or so (gradual reduction in doses depending on clinical state and TFTs) – Initially b-blockers may help alleviate symptoms • In toxic nodular disease – Likely to need long term treatment – Low doses are usually effective (5 -10 mg CBZ a day)

Radioactive iodine • Very effective, permanent • Permanent hypothyroidism frequent outcome • Small risk of thyroid eye disease • Patient must not be pregnant • Must not have had ordinary iodine for months (radiographic contrast, kelp etc)

Surgery for thyrotoxicosis • Usually only considered if – Large goitre with obstructive or cosmetic concerns – Significant possibility of incidental thyroid malignancy – Intolerant of antithyroid drugs and radioactive iodine therapy refused or contraindicated

Some mistakes • Requesting an ultrasound in hyperthyroidism • Even worse is performing a contrast CT scan • Asking for antithyroid antibodies (anti-TSH receptor antibodies can be helpful) • Checking TFTs and adjusting treatment outside the 4 to 12 week interval

Angela Thurston • 26 y. o • No past medical history, not on any medications • 2 week history of ear and jaw pain • Malaise • Sweats, weight loss, occasional palpitations especially at the gym

Angela Thurston • • • HR 90, regular Hint of a tremor Lid lag but no eye signs Mouth, jaw and ear examinations normal Tenderness over the thyroid Palpable firm thyroid, not perceptibly enlarged

Angela Thurston • What is the likely diagnosis? • What tests may be helpful?

Angela Thurston • What would you expect the results of the following tests to be – TFTs – Thyroid nuclear scan – ESR • What is the natural history of this condition?

Emma Watson 23 y. o. nurse New to your practice History of anxiety/depression – on an SSRI Smoker, irregular periods Concerned about her weight despite diet supplements and naturopathic treatments • Requests OCP • • • Overweight (BMI 29) HR 90 regular (repeated testing) Hint of a tremor, brisk normal reflexes No goitre

Emma Watson • Routine blood tests show a suppressed (undetectable TSH) • Repeat TFTs confirm the suppressed TSH and show significantly elevated FT 4 and FT 3 levels • Possible diagnoses? • What tests may be helpful?

Subclinical hypothyroidism • TSH elevated but FT 4 and FT 3 normal • Increased (but still small) risk of overt hypothyroidism • Possible increased cardiovascular risk in long-term (evidence is not conclusive) • Observe or treat according to clinical circumstances • Anti-TPO antibodies may be helpful as high titres increase the risk of progression to overt hypothyroidism

Thank you
- Slides: 51