Megaloblastic Anemia BY DR Hayam Hebah Associate Professor

Megaloblastic Anemia BY DR. Hayam Hebah Associate Professor of Internal Medicine AL Maarefa College

Objectives: �Background �Causes �B 12 �Folic acid �How to reach diagnosis �Management.

BACKGROUND: �Megaloblastosis describes a heterogeneous group of disorders characterized morphologically by large cells with an arrest in nuclear maturation. relative to cytoplasmic maturity. Cells seen in bone marrow aspirates and in peripheral smears have been called megaloblasts. �Megaloblastic changes are most apparent in rapidly dividing cells such as blood cells and gastrointestinal cells.

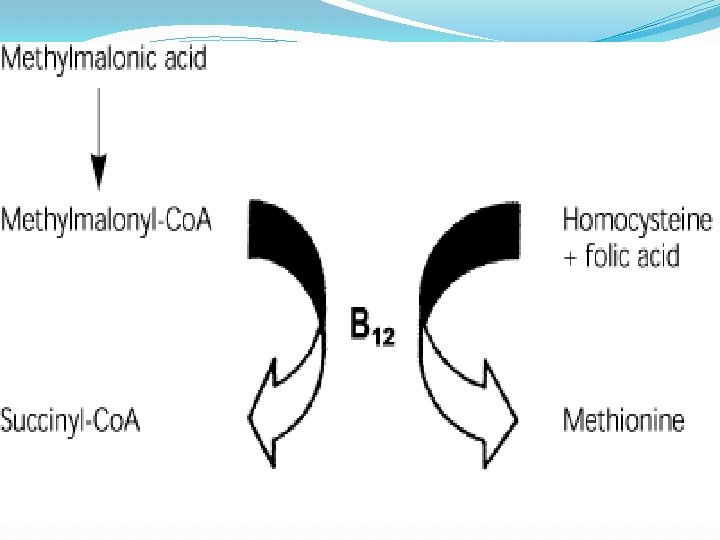
PATHOPHYSIOLOGY: � Defect : is in DNA synthesis in rapidly dividing cells. To a lesser extent, RNA and protein synthesis are impaired. � B 12 helps to synthesize thiamine, thus deficiency leads to problems with DNA replication

Causes of Megaloblastic Anemia � B 12 deficiency � Folate deficiency � Pernicious anemia � others

OTHER CAUSES OF MEGALOBLASTOSIS: *Medications (antimetabolite drugs as azathioprine) *Direct interference of DNA synthesis by: -- HIV infections -- myelodysplastic disorders. *Liver disease with inadequate cholesterol esterification *Alcohol abuse independent of folate (MCV 100 -105) *Post-splenectomy
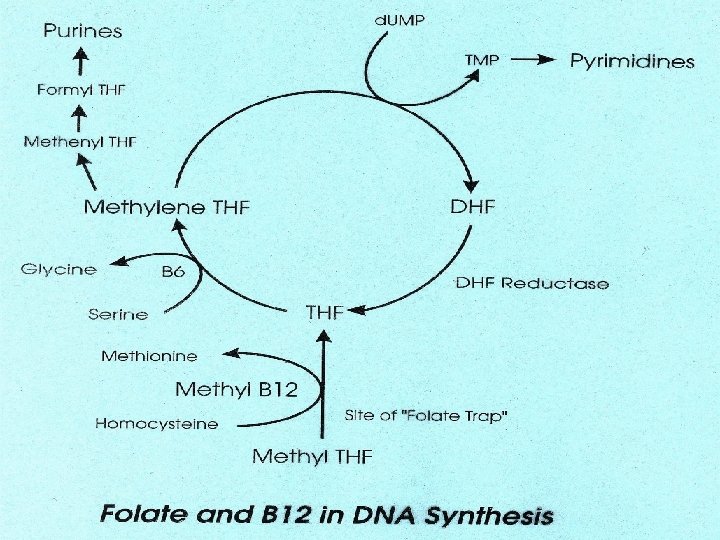

Vitamin B 12 (cobalamin)

�Sources of cobalamin a cobalt-containing vitamin, are meat, fish, and dairy products and not vegetables and fruit. �Storage : It is the only water-soluble vitamin stored in the body. About 3 mg of cobalamin are stored, of which 1 mg is stored in the liver. � Hence, it takes 3 -5 years to develop a vitamin B-12 deficiency after a total gastrectomy.
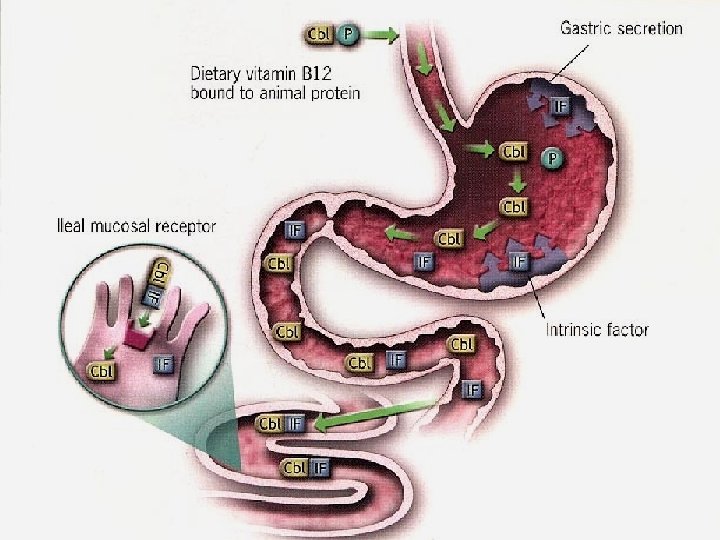

B 12 Metabolism �Bind to cobalophilin (cobalamine binding protein) in saliva and gastric secretion �Bind to IF (from parietal cell) in the duodenum �Cb 1 -IF complex bind to receptor (cubilin) at distal ileum for mucosal absorption � 1% B 12 can be absorbed without IF (mega dose of B 12 for IF deficiency )

MEGALOBLASTIC ANEMIAS Causes of Vit. B 12 deficiency(1) 1. -Inadequate intake Dietary cobalamin deficiency rarely causes megaloblastic anemia, except in vegetarians 2 -Malabsorption a) Inadequate production of intrinsic factor - pernicious anemia (autoimmune destruction of gastric parietal cells) - gastrectomy, partial or total b) Inadequate releasing vit. B 12 from food - (partial gastrectomy, atrophic gastritis and achlorhydria (mainly in elderly patients), - chronic pancreatic insufficiency (the alkaline environment in the small intestine is insufficient for release of cobalamin from R-proteins and binding to intrinsic factor) c) Terminal ileum disease (sprue, celiac disease, ileal resection, Crohn ‘s disease, lymphoma) 12

Causes of Vit. B 12 deficiency(2) d) Competition for intestinal B 12 : - bacterial overgrowth: jejunal diverticula, intestinal stasis and obstruction due to strictures, blind-loop syndrome - Fish tapeworm Diphyllobothrium latum , found in Canada, Alaska, and the Baltic Sea. 3. Inadequate utilisation Drugs: PAS, Neomycin, Colchicine, Nitrous oxide , acyclovir, hydroxyurea, metformin,

�in the Zollinger-Ellison syndrome, the acid environment also prevents binding of cobalamin to intrinsic factor. �Blind loop syndrome can result in cobalamin deficiency. Bacterial colonization can occur in intestines deformed by strictures, surgical blind loops, scleroderma, inflammatory bowel disease, or amyloidosis. Bacteria then compete with the host for cobalamin.

Pernicious Anemia �Autoantibody to Intrinsic Factor detectable in <70% �Highly specific, but insensitive � 2 types of anti-IF antibody � Blocks attachment of Cbl to IF � Blocks attachment of Cbl-IF complex to ileal receptors �Chronic atrophic gastritis �Autoantibody against parietal cells (H-K-ATPase) though pathology indicates destruction by CD 4+ T cells �Increased risk of gastric cancer (carcinoid and intestinal - type)

Folic acid

�Sources: vegetables, fruits, and animal protein �Absorption of folate and its transport is receptor mediated. Uptake occurs in the jejunum and throughout the small intestine �Storage is limited, and folate deficiency develops about 3 -4 weeks after the cessation of folate intake �The daily requirement for adults is about 0. 4 mg/d.

Causes of folate deficiency: �Low folate food content and overcooking are causes for folate deficiency, in elderly persons. �Increased demand can result in deficiency as in hemolysis, pregnancy, lactation, rapid growth, hyperalimentation, renal dialysis, psoriasis, and exfoliative dermatitis. �Intestinal disorders that impede folate absorption include tropical sprue, non-tropical sprue (celiac disease or gluten sensitivity), amyloidosis, and IBD.

Medications include: �phenytoin �metformin � phenobarbital �dihydrofolate reductase inhibitors (trimethoprim, pyrimethamine) � methotrexate � sulfonamides �valproic acid.

History findings to help identify folate deficiency are as follows �Poor nutrition, alternative diets, and excessive heating and dilution of foods �Chronic alcoholism �Conditions that interfere with folate absorption, including IBD, sprue or gluten sensitivity, and amyloidosis �Conditions that increase folate consumption, such as pregnancy, lactation, hemolytic anemia, hyperthyroidism, and exfoliative dermatitis �Hyperalimentation and hemodialysis �Medications history that interferes with folate metabolism �Hereditary disorder: A lifelong history of megaloblastosis or folate deficiency would suggest a hereditary disorder as the cause.

MEGALOBLASTIC ANEMIAS clinical features 1 - Asymptomatic for years 2 -Symptoms of anemia(weakness and cardiopulmonary impairment) 3 - Symptoms associated with vit. B 12 or Folic acid deficiency • neurologic manifestations (exclusivly in vit. B 12 deficiency) - megaloblastic madness or psychosis, - subacute, combined degeneration of the spinal cord ( proprioceptive and vibratory sensation), spinal ataxia with unsteady gait and abnormal balance. -Peripheral neuropathy (numbness, pain, tingling, and burning in a patient’s hands and feet in glove and stocking distribution). • gastrointestinal (vit. B 12 and folic acid deficiency) - loss of appetite - glossitis (red, sore, smooth tongue) - diarrhea or constipation - weight loss 21

c/p: signs: �Patients may have a lemon-yellow jaundice (combined anemia and increased indirect bilirubin from intramedullary hemolysis) �Anemia signs(tachycardia ) �Glossitis ( with loss of papilla) �Dermatologic signs include hyperpigmentation of the skin and abnormal pigmentation of hair due to increased melanin synthesis �Mental changes of psychosis �Peripheral neuropathy �SCD of cord and abnormal gait. �Blindness due to optic atrophy may occur. �signs of the cause.

Signs suggestive of the cause: �Abdominal scars may suggest a blind loop syndrome due to gastric surgery or a lack of ileal absorption of cobalamin in a patient who had an ileal resection. �Patients with nontropical and tropical sprue may have signs of malabsorption, such as weight loss, abdominal distention, diarrhea, and steatorrhea. These patients often have metabolic bone disease or bleeding resulting from to deficiencies in vitamin K–dependent factors. �Patients who have megaloblastosis as a result of HIV infection or myelodysplastic syndromes usually have signs of these disorders.

Myelodysplasia: �The myelodysplastic syndromes are all disorders of the hematopoietic stem cells in the bone marrow (only related to myeloid lineage). �In MDS, hematopoiesis (i. e. , blood production) is disorderly and ineffective �FAB classification: 1. Refractory anemia (RA) 2. Refractory anemia with ring sideroblasts (RARS) 3. Refractory anemia with excess blasts (RAEB) 4. Refractory anemia with excess blasts in transformation (RAEB-T) 5. Chronic myelomonocytic leukemia (CMML), not to be confused with chronic myelogenous leukemiaor CML
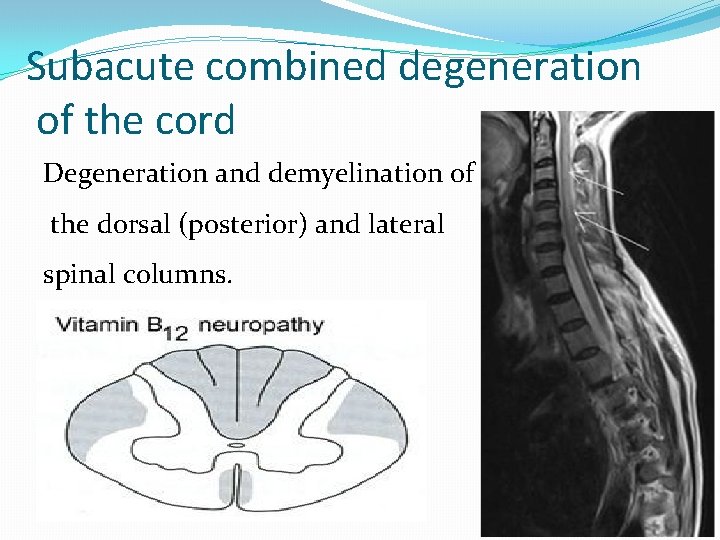
Subacute combined degeneration of the cord Degeneration and demyelination of the dorsal (posterior) and lateral spinal columns.
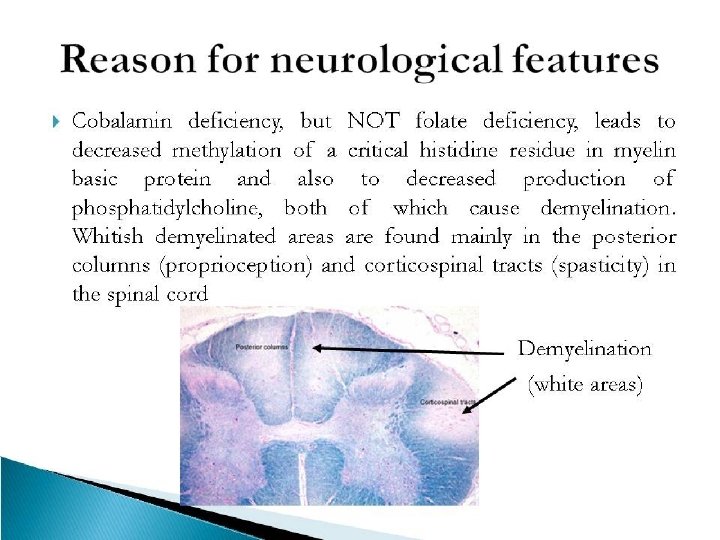

Whom should you test for B 12 or Folate deficiency? �MCV >100 with or without anemia �Hypersegmented neutrophils �Pancytopenia of uncertain cause �Unexplained neurologic s/s �Alcoholics �Malnourished, particularly the elderly �Vegans if no history of supplementation �Diabetics on metformin with new onset neuropathy

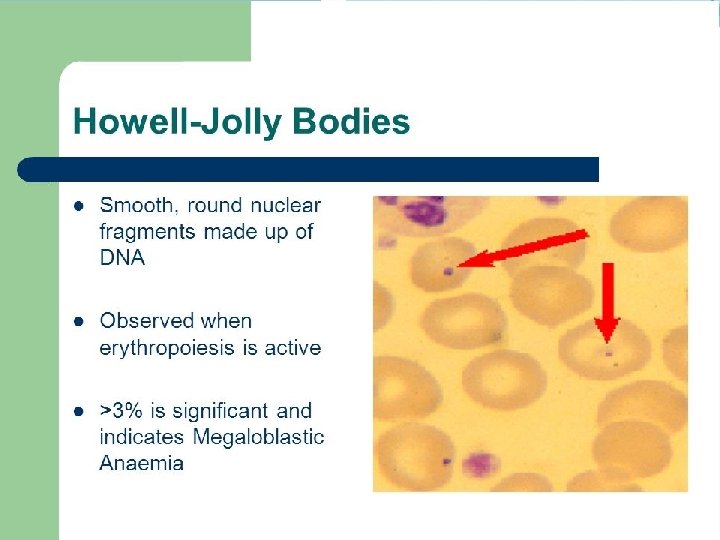
Lab work out: �Reticulocyte counts are inappropriately low, representing lack of production of RBCs due to massive intramedullary hemolysis �LDH is usually markedly increased �Peripheral smear morphology: �Macroovalocytes �Single and multiple Howell-Jolly bodies, nuclear fragment, may be seen in RBCs. Cabot rings, remnants of mitotic spindles, may also be present in RBCs. �Nucleated RBCs and megaloblasts �hypersegmented neutrophils �pancytopenia

Bone marrow aspiration �Bone marrow aspiration is usually not needed to make the diagnosis of vitamin B-12 deficiency. However, it can help rule out myelodysplasia and assess iron stores. �The bone marrow is hypercellular with erythroid hyperplasia �Giant bands, neutrophil precursors, can be present. Megakaryocytes may be large and hyperlobulated.

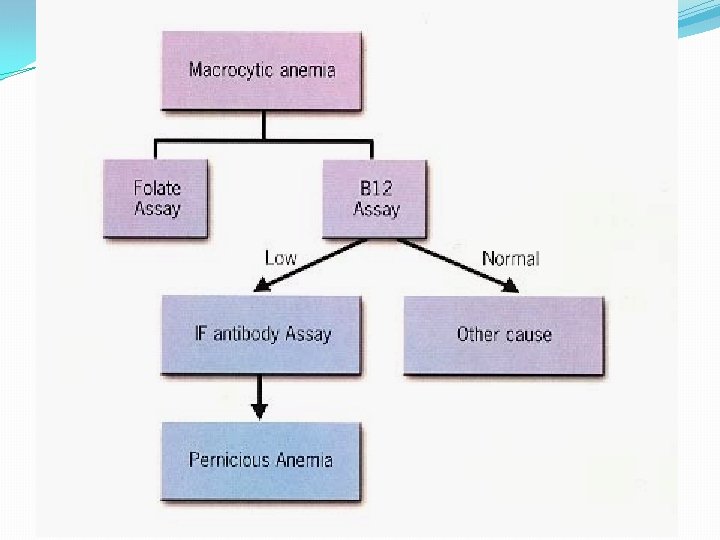
Primary Tests for B-12 and Folate Deficiencies �Serum B-12 (cobalamin) �Reference range: 200 -900 pg/m. L �Borderline: 180 -250 pg/m. L �Associated with anemia and neuropathy: < 180 mg/L �Diagnostic of B-12 deficiency: < 150 mg/L �Serum folate �Reference range: 2. 5 -20 ng/m. L � 5 ng/m. L �Folate deficiency likely (overlap with normal): < 2. 5 ng/m. L �RBC folate:
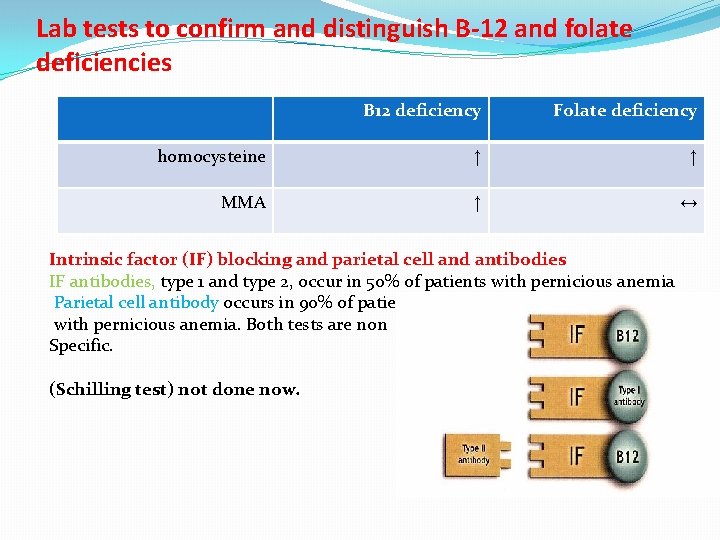
Lab tests to confirm and distinguish B-12 and folate deficiencies B 12 deficiency Folate deficiency homocysteine ↑ ↑ MMA ↑ ↔ Intrinsic factor (IF) blocking and parietal cell and antibodies IF antibodies, type 1 and type 2, occur in 50% of patients with pernicious anemia Parietal cell antibody occurs in 90% of patients. with pernicious anemia. Both tests are non Specific. (Schilling test) not done now.

Other needed tests: �Baseline iron studies and serum ferritin should be obtained since they may predict the need for iron therapy since iron stores can be consumed during cobalamin or folate therapy. �Radiographic imaging of the upper and lower GIT may be useful for detecting abnormalities that could cause a blind loop syndrome �Other tests that may be considered include : �With cobalamin deficiency, evaluate and rule out autoimmune disorders, Zollinger-Ellison syndrome, pancreatic insufficiency, fish tapeworm infestation, Crohn disease, or ileal scarring. �With folate deficiency, evaluate evidence for malnutrition and alcoholism, sprue, chronic hemolysis, and exfoliative dermatitis. �Megaloblastic anemia


THERAPY: � Transfusion therapy : restricted to patients with severe, uncompensated, and life-threatening anemia. �Cobalamin Therapy �Cobalamin (1000 µg) should be given intramuscularly daily for 2 weeks, then weekly until the hematocrit value is normal, and then monthly for life. Oral cobalamin (1000 -2000 µg) also can be administered.

Note the following: �Oral cobalamin is indicated in patients with hemophilia to avoid intramuscular injections and bleeding. �Intramuscular cobalamin and not oral cobalamin should be used to treat patients with cobalamin-related neurological disorders. �One advantage of parenteral over oral cobalamin is that all abnormalities in cobalamin absorption are bypassed. �It may be practical to initially administer parenteral cobalamin and then to continue treatment with oral cobalamin. Oral cobalamin is less expensive and is better tolerated by patients. �Patients who have undergone either a total or partial gastrectomy should be started on replacement therapy after the surgery to prevent the development of megaloblastosis

Folate Therapy �Folate (3 -5 mg) should be administered orally. daily for 4 months or until hematologic recovery �Folate should be administered prophylactically 1. during pregnancy, lactation, and the perinatal period 2. in chronic hemolytic anemias, psoriasis and exfoliative dermatitis, and during extensive renal dialysis. 3. in patients with hyperhomocystenemia who are at risk for thromboembolic complication �Fortification of foods and folic acid supplements have been recommended to reduce the risk of pancreatic, cervical, and colon cancers.

Warning �Folate therapy should not be instituted in a patient with megaloblastic anemia if cobalamin deficiency has not been definitively ruled out ( folic acid will improve the anemia but not the neurological complications of cobalamin deficiency, and the neurological disorder will worsen). � Both cobalamin and folate should be initiated if cobalamin deficiency has not been ruled out �Repeat testing for B 12 deficiency may be reasonable for those on long-term folic acid therapy if hematologic (macrocytosis or ↑LDH) or neurologic symptoms persist

Treatment of Other Related Conditions �Blind loop syndrome --- antibiotics. �Patients with transcobalamin II (TCII) deficiency --- higher doses of cobalamin. �Tropical sprue --- both cobalamin and folate. �Acute megaloblastic anemias due to nitrous oxide exposure ----- folate and cobalamin. �Fish tapeworm infection, pancreatitis, Zollinger. Ellison syndrome, and inborn errors should be treated with appropriate measures.


diet �Patients should have diets rich with folic acid. Examples of such foods include asparagus, broccoli, spinach, lettuce, lemons, bananas, melons, liver, and mushrooms. �To prevent loss of folate, foods should not be cooked excessively and should not be diluted in large amounts of water. �To prevent cobalamin deficiency, vegetarians should include dairy products and eggs in their meals

Prognosis �The prognosis is favorable if the etiology of megaloblastosis has been identified and appropriate treatment has been instituted �Folate deficiency during pregnancy can lead to neural tube defects and other developmental disorders in the fetus. However, folate in prenatal vitamins given during pregnancy has reduced these morbidities

- Slides: 45