MedSurg I Emergency Care First Aid Lisa Osborne

Med/Surg I Emergency Care & First Aid Lisa Osborne, RN BSN

Learning Objectives 1. Discuss the importance of assessing the safety of an emergency scene. 2. Describe the medical identification tag and its purpose. 3. Describe, in order, the steps for assessing an ill or injured person in an emergency. 4. Identify early, common, and progressive signs of shock.

Learning Objectives, cont. 9. Describe general emergency actions for chest, neck, back, and head injuries. 10. Demonstrate in the lab, emergency actions for a puncture wound of the chest. 11. Describe at least three signs of increasing intracranial pressure. 12. Explain symptoms and first aid for injuries caused by exposure to cold, including frostbite and hypothermia.

Learning Objectives, cont. 5. Describe at least five common types of shock, including hypovolemic shock, identifying nursing actions in emergency induced shock. 6. Define sudden death. 7. Differentiate between clinical and biological death. 8. State and demonstrate the procedure for calling a code in your healthcare facility or agency.

Learning Objectives, cont. 13. Describe symptoms and immediate first aid for heat related illnesses and injuries, including heat exhaustion and severe burns. 14. List at least three signs of an inhalation injury following a fire. 15. Discuss first aid for musculoskeletal injuries, including a fracture, demonstrating the ability to safely splint an ulnar or radial fracture using common household materials.

Learning Objectives 16. Describe the immediate actions of a rescuer in suspected heart attack 17. Describe emergency care for at least three different types of hemorrhage. 18. Define the term anaphylaxis and describe causes, symptoms, and treatment of anaphylaxis.

Learning Objectives, cont. 19. Identify at least three precautions to take when a client has been exposed to hazardous materials. 20. List at least five immediate actions to take when a person is suspected of being poisoned. 21. Define the term triage, and describe how it applies to emergency care. 22. List at least four factors that identify a psychiatric emergency or the potential for suicide.

New Terminology • • AMBU bag anaphylaxis antidote avulsion injury bandage biological death café coronary caustic • • clinical death code debride dislocation epistaxis extrication fracture frostbite

New Terminology, cont. • • heat cramps heat exhaustion heat stroke hemorrhage hypothermia intrusion injury intubation mediastinal shift • • near drowning pneumothorax poison rabies shock splint sprain strain

New Terminology, cont. • • • stridor sudden death syncope thrombolytic tourniquet • • toxin trauma triage wind chill factor

Acronyms • • • ABCDE ACLS AED AVPU BCLS BLS • • • CMS CPR DNI DNR EMS EMT

Acronyms, cont. • • • HAZMAT ICP LOC MAST MI MVA • • • PERRLA+C PTSD RICE SIRES SIRS

Identify Problems • • • When reporting an MVA, note the vehicle's condition. Is the vehicle upside down, on its side, or in a ditch? Is the vehicle in the water? Is there a gasoline spill? Note areas of intrusion: the driver's side, passenger's side, roof, front end, or back end. Were victims wearing seatbelts? Were the airbags deployed? Was anyone thrown from the vehicle, and if so, how many feet or yards? If the victim was riding a bicycle or motorcycle, was the victim wearing a helmet and protective clothing? This information can help emergency personnel anticipate certain types of injuries. Medic Alert Tag signifies any specific medical problem (eg, diabetes, epilepsy) to be considered when administering first aid. If you do not consider such information and treat accordingly, the person may die.

S/S of Hypovolemic Shock • If a person is experiencing absolute hypovolemic shock, look for the following: – Hypotension (lowered blood pressure, after a slight increase) – Weak, thready pulse – Cool, clammy skin – Tachycardia (increased pulse) – Tachypnea (increased respiratory rate) – Hyperpnea (very deep breathing, gasping) – Restlessness, anxiety (caused by decreased blood flow to the brain) – Weakness – Decreased urinary output

Introduction • Trauma refers to a wound or injury that is caused by an outside force. Thousands of people die from the effects of trauma and sudden illness every year. Traumatic injuries are caused by events such as motor vehicle accidents (MVAs), poisonings, burns, responses to temperature extremes, obstructed airways, and gunshot wounds.

Trauma • Wound or injury that is caused by an outside force • Includes – Motor vehicle accidents (MVAs) – Poisonings – Burns – Responses to temperature extremes – Obstructed airways – Gunshot wounds

Trauma • Wound or injury that is caused by an outside force • Includes – Motor vehicle accidents (MVAs) – Poisonings – Burns – Responses to temperature extremes – Obstructed airways – Gunshot wounds

Introduction • Cardiopulmonary resuscitation (CPR) and basic life support are not described in detail in this chapter. To learn the detailed methods used in CPR and removal of airway obstruction, the nurse must take a specific course. Healthcare facilities and organizations require CPR certification for all employees. It is up to each healthcare provider to take the responsibility for obtaining this training and to keep certification current.

PRINCIPLES OF EMERGENCY CARE • Simply because you are a nurse, people will expect you to be able to deal with emergencies. • In an emergency, the first responder must decide quickly what to do. • Without an adequate oxygen supply due to blood loss or airway obstruction—a person's brain cells begin to die within 4 to 6 minutes. Therefore, you must give care in an emergency quickly.

Good Samaritan Laws

Assess Safety • Is there any danger of fire, explosion, or building collapse? Is there danger of being caught in traffic or hit by a car? Are there electrical hazards, live wires, or other hazardous materials? Is the person in danger of drowning? • If the scene is unsafe, the first responder may need to call for additional help before assist ing injured persons. • It may also be necessary to move victims away from danger before starting first aid care. Do not move any injured person, however, if the area is safe. Rationale: Unnecessary movement can compound or cause additional problems.

Identify Problems • Are containers lying about that suggest attempted suicide, poisoning, or drug abuse? • Do medications give a clue to a medical problem (eg, diabetes, epilepsy)? • Are there signs of alcohol or drug abuse? • Is there any indication of foul play? If there is any indication of foul play, treat the victim without disturbing what has now become a crime scene.

Perform Triage • Triage is the process of sorting and classifying to determine priority of needs. Triage involves determining life threatening situations and assisting those clients first. • The triage nurse and rescue personnel must determine whom to assist first, when and how to call for help, and how untrained bystanders can assist. • If there are numerous victims, the local hospital must be notified so that they can activate their disaster plan.

Organ Donors • If a card is found indicating that a person wishes to donate tissues or organs after death, inform emergency personnel at the scene of the accident. In many states, the fact that the victim wishes to be a donor is indicated on his or her driver's license. (Remember that the next of kin is required to give permission for organ or tissue donation if a person dies, even if the person has a donor card. )

Medic. Alert Tag

Summon Assistance • The fastest way to summon the emergency medical service (EMS) is by telephoning 911. • If possible, send someone to call, but make sure the person has all necessary information, including the exact location and the nature of the emergency.

Shock • Many types of shock • Body attempts to compensate – Some types of shock try to maintain an adequate blood supply to vital organs. • Categories of shock – Primary: nervous system’s response immediately after severe injury – Secondary (delayed or deferred): 1 to 24 hours after injury

Assess and Treat for Shock • Shock is often the first phase of the body's "alarm reaction" to trauma or severe tissue damage. After an accident, many conditions can lead to shock; however, shock usually results from problems in the cardio vascular system. • The central nervous system (CNS) controls all body functions, it monitors changes and immediately implements compensatory circulation to maintain an adequate blood supply to vital organs (eg, the brain and the heart) in an emergency. • This compensatory action can quickly adjust the rate and strength of the heart's contractions and the tone of blood vessels in all body parts. It actually shuts down the flow of blood to the skin, digestive system, and kidneys, and shunts (transfers) the blood that would normally go to these areas to the heart and brain instead. (The symptoms of shock are largely related to this compensatory mechanism. ) Compensatory circulation is a survival mechanism that ensures that the body's most vital organs are adequately perfused with blood until the last possible moment.

Shock (cont’d) • However, in some cases the body cannot compensate. In this case, shock develops. • Shock may develop rapidly following trauma (or more slowly in other situations). • Consequently, every injured person should receive preventive and precautionary treatment for shock. • Anything that could cause increased blood loss or otherwise contribute to shock should be avoided. • For this reason, never handle or move injured persons roughly or cause them undue anxiety.

Shock (cont’d) • Shock may fall into three major categories: – primary—the nervous system's response immediately after a severe injury; – secondary—one or more hours after an injury, perhaps up to 24 hours later (delayed or deferred shock); – hemorrhagic—due to blood loss, and may be categorized as primary or secondary

Shock Related to Fluid Loss • Hypovolemic shock related to – Hemorrhage, ie, blood loss – Loss of plasma fluid in intravascular spaces (but not necessarily loss of blood from intravascular spaces) • Severe diaphoresis, diarrhea, or vomiting; burns – Severe infection and/or inflammatory process • Intestinal obstruction, peritonitis, acute pancreatitis

Types of Shock • Hemorrhagic shock reduced blood volume caused by either external or internal bleeding. • Plasma loss shock reduced blood volume results from loss of plasma into the interstitial spaces and greatly increased blood viscosity. • Intestinal obstruction results in the movement of large amount of plasma from the blood into the intestine. • Severe burns loss of large amounts of plasma from the burned surface. • Dehydration results from severe and prolonged shortage of water intake. • Severe diarrhea or vomiting loss of plasma through the intestinal wall. • Neurogenic shock rapid loss of vasomotor tone that leads to vasodilation to the extent that a severe decrease in blood pressure results. • Anesthesia deep general anesthesia or spinal anesthesia that decreases the activity of the medullary vasomotor center or the sympathetic nerve fibers.

Types of Shock • Brain damage leads to an ineffective medullary vasomotor function. • Emotional shock (vasovagal syncope) results from emotions that cause strong parasympathetic stimulation of the heart and results in vasodilation in skeletal muscles and in the viscera. • Anaphylactic shock results from an allergic response that causes the release of inflammatory substances that increase vasodilation and capillary permeability. • Septic shock or "blood poisoning" results from peritoneal, systemic, and gangrenous infections that cause the release of toxic substances into the circulatory system, depressing the activity of the heart, leading to vasodilation, and increasing capillary permeability. • Cardiogenic shock occurs when the heart stops pumping in response to conditions such as heart attack or electrocution.

Types of Shock • • • There are several methods to group the types of shock. One method uses the physiological basis: Distributive Shock (same volume, increased space) Hypovolemic Shock (same space, decreased volume)Hypovolemic inadequate volume Cardiogenic inadequate pump Distributive increased vascular space » Anaphylactic » Septic » Neurogenic Others have included diabetic shock and adrenal crisis as forms of shock. Distributive Hypovolemi Shock c Shock (same volume, space, increased decreased space) volume)

Hypovolemic Shock • Early signs and symptoms Hypotension (after a short term rise in BP) Tachycardia (increased heart rate) Weak, thready pulse Tachypnea (increased respiratory rate) Restlessness Decreased urinary output

Hypovolemic Shock, cont. • Late signs of hypovolemic shock Lowered body temperature Decreasing BP extreme hypotension Increasing pulse followed by decreasing pulse Shallow respirations Narrowed pulse pressure • Decompensated shock irreversible shock death
Treatment of Hypovolemic Shock • • • Maintain and/or increase blood supply to brain. Identify bleeding sites; control bleeding. Replace fluid loss. Replace blood and blood components. Maintain BP tissue perfusion Treat cause, eg, infection, burn

Key Concept • Look for all signs of shock. A falling blood pressure is a late sign of shock, and is ominous. Remember, shock is not always caused by blood loss. Nursing Alert • The most common airway obstruction in an unconscious person is caused by the tongue falling back and occluding the airway

Assessing the Person in an Emergency • ABCDE A = Airway and cervical spine B = Breathing C = Circulation and bleeding D = Disability E = Expose and examine

Life Threatening Chest Injuries Pain at the site of injury and on breathing Shortness of breath, gasping Failure of the chest to expand Coughing up blood

Life Threatening Chest Injuries, cont. Rapid, weak pulse and low blood pressure Cyanotic lips, gums, fingernails, or fingertips Panic, agitation, nasal flaring Abnormal breathing sounds, such as wheezing or stridor Abnormal chest movements on breathing
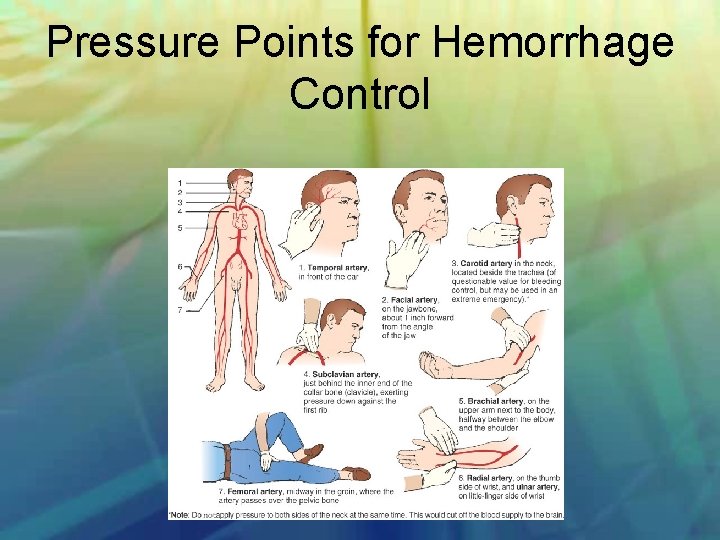
Pressure Points for Hemorrhage Control

Nursing Alert • Use a one way filtered breathing mask for cardiopulmonary resuscitation (CPR) whenever possible, to protect the rescuer. Key Concept • Follow Standard Precautions whenever possible in administering first aid.

Measures To Stop Bleeding • • • Apply direct pressure. Elevate a bleeding limb. Apply ice or cold pack. Apply indirect pressure. In severe bleeding, try to grasp the bleeding vessel. • Last resort: apply tourniquet

Neurologic Assessment: AVPU • • A = Alert V = Verbal stimuli only P = Painful stimuli only U = Unresponsive

Neurologic Assessment: Eye Signs • PERRLA+C PE = Pupils equal R = Round RL = React to light A = Accommodation OK C = Coordinated

Cardiopulmonary Arrest: Sudden Death • Breathing and heartbeat stop abruptly/unexpectedly • CPR: BLS and ACLS needed • Causes – Electrocution – Adverse reaction to general anesthesia – Drowning – Myocardial infarction – Anaphylaxis – Cerebrovascular accident – Drug overdose – Severe trauma – Poisoning – Total airway obstruction; suffocation – Shock – Smoke inhalation

Definitions of Death • Clinical death – Breathing and heartbeat stop – May be reversible • Biological death – Permanent damage of brain cells due to lack of oxygen – Irreversible

Basic (Cardiac) Life Support • Basic life support (BLS) – Rapid entry into EMS – CPR – Techniques to clear an obstructed airway – Automated external defibrillator (AED) • Initial treatment of victims in cardiac arrest

Advanced Cardiac Life Support • Emergency medical technicians (EMTs), (ACLS) paramedics, nurses • Includes – Starting intravenous (IV) lines – Administering fluids and emergency medications – Using defibrillation and cardiac monitoring – Administering oxygen, maintaining airway, intubation

Advance Directives • DNR – Do not resuscitate • DNI – Do not intubate

• • Family With Client Emergency at Home Pocket mask and gloves Family taught CPR (unless specified as DNR) Call 911 Person designated to watch for the ambulance Clear a pathway Reassure family after the event Document event and outcome

Code in a Healthcare Facility • Emergency; activate code using facility’s code system • Assisting with a code – Obtain emergency equipment – Pediatric emergencies use color coded tape that gives equipment sizes, drug doses, and defibrillation settings based on height and body build • Code team usually assigned daily; assist code team • Primary healthcare provider determines disposition and care

Key Concept • Remember: You are expected to perform first aid only to the level of your training and experience.

Chest, Back, Neck, and Head Injuries • Do not move except in unusual situations • Extrication = emergency removal of a victim • Common causes of chest injuries – Blows – Stabbings – Shootings – MVAs

Pneumothorax, cont. • Tension pneumothorax – Air leaks out of the lung or bronchus into the chest cavity and cannot escape – Breath sounds greatly diminished or absent on affected side; mediastinal shift possible • Treatment – Seal wound using aluminum foil, petroleum jelly (Vaseline) gauze, plastic wrap, or rolled up dressing

Chest Injuries RIB FRACTURES: The most common type of chest trauma usually involving the fifth through the ninth ribs. Fractures of the first three ribs are rare but deadly due to laceration of the subclavian artery. Fractures of the lower ribs are associated with injury to the spleen and liver. The patient will experience severe pain, tenderness, and muscle spasm over the site of the fracture. There may be bruising around the fracture site. A crackling grating sound in the thorax may be detected. Occurs in over 60% of patients admitted with chest trauma. Most rib fractures are benign and are treated conservatively. The goals of treatment are to control pain and detect and treat the injury. Sedation is used to allow for deep breathing and coughing. Intercostal nerve block, ice to the area, and a chest binder may also be used to abate the pain which usually subsides in 5 to 7 days. Most fractures heal within 3 to 6 weeks.

Chest Injuries FLAIL CHEST: Flail chest occurs when two or more adjacent ribs are fractured at two or more sites, resulting in a free floating rib segment. As a result the chest wall loses stability, with subsequent respiratory impairment and severe respiratory distress. During inspiration, as the chest expands, the detached part of the rib segment (flail segment) will move in a paradoxical manner in that it is pulled inward during inspiration reducing the amount of air that can be taken into the lungs. On expiration, the flail segment will bulge outward impairing the patient’s ability to exhale. Lung contusion and atelectasis often accompany flail chest. Associated with blunt trauma to the chest and fracture of the ribs in two or more locations. Management includes providing ventilatory support, clearing secretions from the lungs, and controlling pain. The underlying pulmonary contusion is treated by restricting fluid intake and prescribing diuretics, etc. while relieving chest pain. In severe flail chest, ET intubation and mechanical ventilation are performed. The patient will be monitored by serial chest x rays, ABGs, pulse oximetry, and pulmonary function study.

Chest Injuries HEMOTHORAX: A collection of blood in the space between the chest wall and the lung (the pleural cavity). Symptoms of this disorder include chest pain, shortness of breath, breathing absent temporarily, rapid heart rate, anxiety, restlessness. A physical examination reveals decreased or absent breath sounds on the affected side. Signs of hemothorax may show on chest x ray, thoracentesis, or pleural fluid analysis. The most common cause of hemothorax is chest injury. Other causes include cancer, a defect of the blood clotting mechanism, thoracic surgery, or pulmonary (lung) infarction (tissue death). In a chest injury, a rib may lacerate lung tissue or an artery, causing blood to collect in the pleural space. The incidence is 6 out of 100, 000 people. Use safety measures (such as seat belts) to avoid injury. Depending on the cause, a hemothorax may not be preventable. The objective of treatment is to stabilize the condition of the affected person, stop the bleeding, and remove the blood in the pleural space. A chest tube is inserted through the chest wall to drain the blood, and it is left in place for several days to reexpand the lung. The cause of the hemothorax should be treated. Frequently surgery is indicated because of the nature of injury sustained by trauma.

Chest Injuries PNEUMOTHORAX: A collection of air or gas in the chest causing the lung to collapse. Symptoms associated with this disorder include sudden chest pain, shortness of breath, chest tightness, easy fatigue, rapid heart rate, bluish color of the skin caused by lack of oxygen Symptoms may begin during rest or sleep. Additional symptoms that may be associated with this disease include nasal flaring, breathing absent temporarily, anxiety, stress, and tension, abdominal pain. Stethoscope examination of the chest reveals decreased breath sounds on the affected side. Diagnostic tests include chest X ray (to determine the presence of air outside the lung) and arterial bllod gases. There are several types of pneumothorax, which are classified by cause. Spontaneous pneumothorax is thought to be caused by the rupture of a bleb or bullae (a small air filled sac in the lung). The disease affects tall, thin men between 20 and 40 years old most frequently. Cigarette smoking and family history are contributing factors. Pneumothorax may also be a complication of underlying pulmonary (lung) disease (COPD, asthma, cystic fibrosis, tuberculosis, and whooping cough). Other types of pneumothorax include traumatic pneumothorax and tension pneumothorax, which are discussed below. Pneumothorax affects 9 out of 100, 000 people a year. The objective of treatment is to remove the air from the pleural space, allowing the lung to re expand. Small pneumothoraces may resolve spontaneously. The placement of a chest tube (chest tube insertion) between the ribs into the pleural space allows the evacuation of air from the pleural space. With the chest tube left in place, the lung may take several days to reexpand. Hospitalization is required for chest tube management. Surgery may be indicated to prevent recurrent episodes. To prevent the recurrence of pneumothorax, patients should discontinue smoking and avoid high altitudes, scuba diving, or flying in unpressurized aircraft.

Chest Injuries TENSION PNEUMOTHORAX: A complete collapse of the lung that occurs when air enters, but does not leave, the pleural space. A mediastinal shift occurs. In tension pneumothorax, air enters the pleural space with each breath, is not expelled by exhaling, and becomes trapped. The trapped air builds up pressure in the chest, as the amount of trapped air accumulates. If untreated, the lung collapses on the affected side and may cause a mediastinal shift in which the heart, trachea, esophagus, and great vessels are pushed towards the unaffected side of the chest. The shift may cause compression of the opposite lung and may affect the flow of blood returning to the heart. Symptoms of this disorder include, sudden chest pain, shortness of breath, chest tightness, easy fatigue, bluish color of the skin due to lack of oxygen, rapid heart rate, low blood pressure, decreased mental alertness, wheezing, consciousness, decreased breathing, distended neck veins. Physical examination may show decreased breath sounds when listening to the chest with a stethoscope. There may be evidence of mediastinal shift (heart, trachea, esophagus and great vessels shifted towards unaffected lung). Subcutaneous emphysema may be present, causing a spongy feeling when the chest is palpated. Tests used in the diagnosis of tension pneumothorax include a chest x ray and arterial blood gases. Causes include penetrating trauma to the chest, lung infection, mechanical ventilation with high pressures, and as a complication of cardio pulmonary resuscitation. Tension pneumothorax is a life threatening emergency. The objective of treatment is to remove the air from the pleural space, allowing the lung to re expand. A chest tube is inserted which slowly and continuously removes air from the chest cavity. This allows the lung to re expand. As the lung heals and stops leaking air, the vacuum is turned down and then the chest tube is removed. Hospitalization is usually required since it may take several days to fully re expand the lung. Surgery may be indicated if there are recurrent episodes or if the lung does not re expand after a chest tube has been in place for 5 days.

Chest Injuries OPEN (TRAUMATIC) PNEUMOTHORAX: A collection of air or gas in the chest causing the lung to collapse usually caused by an open injury to the chest. The incidence is 3 out of 1, 000 people. Clinical manifestations of this disorder include sudden chest pain, shortness of breath, breathing, rapid, chest tightness, easy fatigue Listening to the chest with a stethoscope reveals decreased breath sounds. There may be a bluish coloration of the skin caused by lack of oxygen. The affected person may have a rapid heart rate. Tests to diagnose and evaluate an open pneumothorax include: • arterial blood gases • chest X ray. Traumatic pneumothorax occurs when a physical injury causes the lung to collapse. It can be the result of an injury or accident (gunshot or knife wounds to the chest, automobile accidents, scuba diving accidents), or can occur following medical procedures which accidentally allows air into the pleural space. High risk medical procedures include transbronchial biopsy, pleural biopsy, thoracentesis, chest tube placement, intracostal needle anesthesia, and esophagoscopy. The goal of treatment is to remove the air from the pleural space, allowing the lung to reexpand. Small pneumothoraces may resolve spontaneously. Aspiration of air through a Teflon catheter to a vacuum bottle may re expand the lung. The placement of a chest tube between the ribs into the pleural space allows the evacuation of air from the pleural space when simple aspiration is not successful, or the pneumothorax is large. Re expansion of the lung may take several days with the chest tube left in place. Hospitalization is required for chest tube management.

Chest Injuries PULMONARY CONTUSION: Pulmonary contusion is damage to the lung tissues resulting in hemorrhage and localized edema. Pulmonary contusion may be mild, moderate, or severe. The clinical manifestations vary from tachypnea, tachycardia, pleuritic chest pain, hypoxemia, and blood tinged secretions to even more severe frank bleeding, crackles, severe hypoxemia, and respiratory acidosis. It is associated with chest trauma when there is rapid compression and decompression to the chest wall (blunt trauma). The goal of treatment includes maintaining the airway, providing adequate oxygenation, and controlling pain. In mild pulmonary contusion, ultrasonic mist nebulization is used to keep the secretions fluids. Pain is managed by intercostal nerve blocks or opiods. In moderate pulmonary contusion, the individual is intubated and placed on the ventilator with low O 2 concentrations. A patient with sever pulmonary contusion has symptoms of ARDS and is treated aggressively with intubation and mechanical ventilation.

Chest Injuries SUBCUTANEOUS EMPHYSEMA: The presence of gas within the tissue beneath the skin. Subcutaneous emphysema is a rare finding and generally related to the inadvertent introduction of air into tissues (such as through a pneumomediastinum). It can also occur from the production of gas within a tissue by infection such as in gas gangrene. Subcutaneous emphysema can often be seen as a smooth bulging of the skin. Palpation produces an unusual crackling sensation as the gas is pushed through the tissue. Common causes of subcutnaeous emphysema include pneumomediastinum, gas gangrene, necrotizing enterocolitis Note: There may be other causes of subcutaneous emphysema. This list is not all inclusive, and the causes are not presented in order of likelihood. Explore the possible explanations for subcutaneous emphysema, occurring alone or in combination with other problems. Giving the patient inhalations of high concentrations of oxygen will promote the reabsorption of subcutaneous air by washing nitrogen from the blood and improving its diffusion from the subcutaneous tissues back into the circulation. In severe cases, where there is widespread subcutaneous emphysema, a tracheotomy is indicated to ensure patency of the airway.

Pneumothorax • Collapse of a lung due to air or gas in the chest cavity • Signs/symptoms Difficult breathing Weak and rapid pulse Restlessness Distended neck veins Hypotension Chest and shoulder pain Cyanosis

Nursing Alert • In an emergency, do not remove an article puncturing the chest if it is still in place. – Rationale: The article will help to seal the hole; its removal may cause added damage. Surgical removal is necessary under controlled conditions. • Any person who has a head injury, no matter how minor, should be observed carefully for at least 24 hours. Late complications can occur.

Back and Neck Injuries • • • Immobilize Keep warm Check for signs of increasing intracranial pressure (ICP) Ice pack to swollen area Watch for signs of complications every 2 hours for the first 24 hours. Advise client to see a physician after any head injury

Head Injuries • Observe for – – Blood or fluid draining from the nose or ears Bruising behind the ears or under the eyes Persistent bleeding Change in behavior since the accident • Have person lie flat • Do not lower the person’s head!
Signs/Symptoms of ICP Confusion, disorientation, or agitation Loss of memory Any change in vision, such as blurred vision or double vision Decreased level of consciousness (LOC) or difficulty arousing; extreme lethargy Numbness, tingling, or weakness in an arm or leg Persistent vomiting Severe headache Speech problems Seizures

Glasgow Coma Scale Eye Opening Response Verbal Response Motor Response Spontaneous open with blinking at baseline 4 points Opens to verbal command, speech, or shout 3 points Opens to pain, not applied to face 2 points None 1 point Oriented 5 points Confused conversation, but able to answer questions 4 points Inappropriate responses, words discernible 3 points Incomprehensible speech 2 points None 1 point Obeys commands for movement 6 points Purposeful movement to painful stimulus 5 points Withdraws from pain 4 points Abnormal (spastic) flexion, decorticate posture 3 points Extensor (rigid) response, decerebrate posture 2 points None 1 point
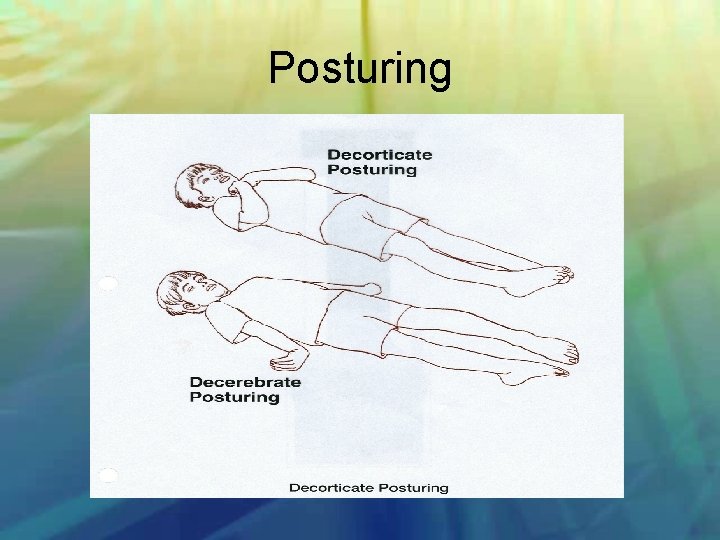
Posturing

Cold Related Injuries • Frostbite – Freezing of body tissues that results from exposure to cold temperatures • Factors influencing cold related injuries – Temperature of the exposure – Wind chill factor – Wetness – Length of exposure time

Cold Related Injuries, cont. • Factors influencing cold related injuries, cont. – Part of the body exposed – Other injury or irritation – Person’s age and mental status – Circulatory status – Nutritional and hydration status – General physical condition – Drug or alcohol use

Nursing Alert • If you work in a public healthcare facility in a cold climate, you will likely see frostbite among homeless people, especially those who are mentally ill, inebriated, elderly, or physically debilitated.

Degrees of Frostbite

Hypothermia • Loss of total body heat, core temperature drops • Types – Accidental hypothermia due to external forces – Induced or surgical hypothermia – Local hypothermia • Confined to one body part

Hypothermia, cont. • Signs/symptoms Sleepiness Slow and clumsy movements Shaking Cardiac dysrhythmia Loss of reflexes and slowed reaction times Impaired judgment Confusion Respiratory failure

Treatment of Hypothermia • • Gradual versus rapid rewarming Transfer to healthcare facility Monitor vital signs and IV infusion Close observation

Key Concepts • Preventing hypothermia is important, especially for individuals engaged in outdoor activities. • Because major heat loss occurs via the uncovered head (which acts like a chimney), wearing a hat is very important. • Wearing wool and layered clothing helps. • Adequate food and fluid intake is important. • Warn campers and hikers to remain dry and to avoid sitting on wet, cold ground or cold metal surfaces.

Nursing Alert • Hypothermia that accompanies frostbite is a medical emergency. • Give immediate emergency care in any case of hypothermia. • A person with severe hypothermia is not considered dead until he or she has been rewarmed and still shows no signs of life. • Because of the increased risk for cardiac standstill, CPR is not usually recommended for this person until he or she is in the Emergency Department. • Remember that air temperature does not have to be cold for hypothermia to occur.

Heat Related Injuries • Occur on days of high humidity – 95° to 100° F (35° to 37. 8° C) with no breeze • Heat cramps – Severe muscle spasms that usually occur after hard exertion – Relieved by drinking very dilute salt solutions

Key Concept • Persons in cooler climates, such as mountain climbers, may experience heat cramps because they are dressed too warmly, causing excessive sweating. • Massaging cramped muscles will not cure heat cramps; in fact, it may increase the pain.
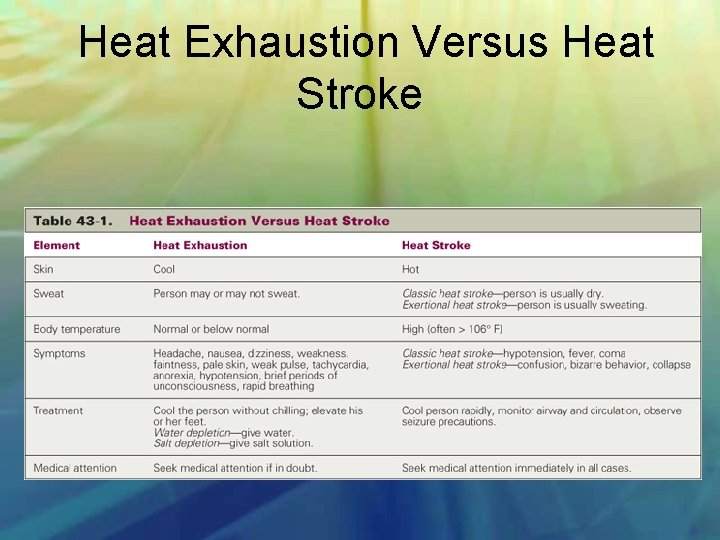
Heat Exhaustion Versus Heat Stroke

Nursing Alert • Certain illnesses, such as cystic fibrosis and scleroderma, restrict the client’s ability to sweat. These individuals are more susceptible to heat stroke.

Nursing Alert • If the person suffering from any type of heat related illness vomits, stop giving fluids. • The person needs IV fluid replacement. – This is usually the only time a person with heat exhaustion needs to be hospitalized. • Any person with heat stroke needs immediate medical attention.

Burns • Most common sources of burns – Thermal – Electrical – Chemical – Radiation

Burns, cont. • Seriousness estimated by – Depth – Percentage of the body burned – Location – Age of victim – Underlying complications

Burns, cont. • Special considerations – Involvement of > 10% of body surface extremely serious – Second or third degree burn serious – Burns to hands, feet, mouth, throat, and perineum are serious. – Full thickness circumferential burns to limbs or chest restrict circulation, breathing – Diabetic persons – Underlying injury – Compromised immune system

Burns: Associated Problems • Inhalation injuries and breathing problems Burned or singed nasal hairs Burns around mouth Flecks of soot in saliva Smell of smoke on breath Hoarse voice

Nursing Alert • If a burned person was trapped in a confined space and exposed to chemicals or smoke, suspect smoke or heat inhalation injury.
Drowning • Drowning – Suffocation from submersion in liquid • Near drowning – Recovery has occurred after submersion – Lifesaving measures until evaluation with instruments, eg, electroencephalogram – Treat hypothermia and shock – Maintain respirations and blood pressure until person cleared medically

Fractures, Sprains, and Dislocations • Fracture: broken bone • Sprain: twisting of a joint with rupture of ligaments and other possible damage • Strain: twisting or stretching that damages a muscle or tendon • Dislocation: displacement of a bone from a joint
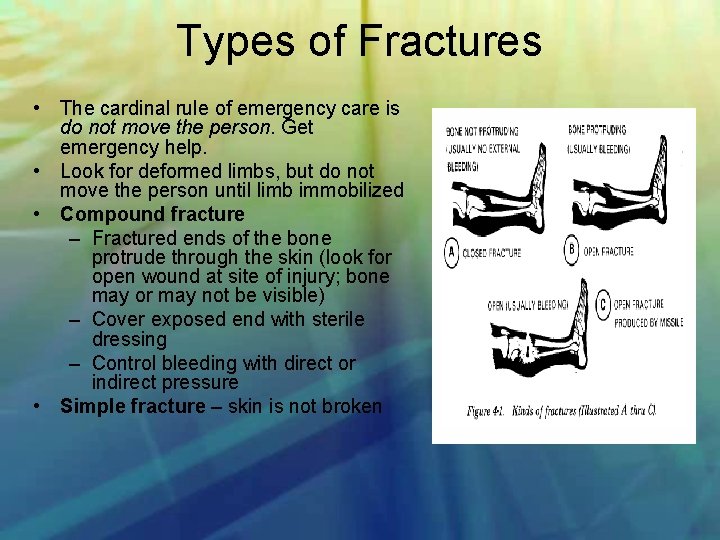
Types of Fractures • The cardinal rule of emergency care is do not move the person. Get emergency help. • Look for deformed limbs, but do not move the person until limb immobilized • Compound fracture – Fractured ends of the bone protrude through the skin (look for open wound at site of injury; bone may or may not be visible) – Cover exposed end with sterile dressing – Control bleeding with direct or indirect pressure • Simple fracture – skin is not broken

Treatment: Sprains and Strains • RICE R = Rest I = Ice C = Compression (such as with a roller bandage) E = Elevation (above the level of the heart, if possible) • Splint = device applied to immobilize a fracture or sprain • Splint wound area – Splint suspected fracture in its existing position – Do not attempt to straighten out limb

Nursing Alert • When splinting a fracture, check the person’s distal pulse before and after splinting. • An absent pulse is a medical emergency. • Obtain medical attention immediately.

Dressing a Wound • Use sterile dressing or cleanest available material • Use bandage and sling to give support or to apply pressure • Do CMS checks: color, motion, and sensitivity or sensation

Dressing a Wound, cont. • Bandage application guidelines Use gloves whenever possible (Standard Precautions) Apply firmly and monitor circulation (can become restricted if swelling/bleeding occurs) Use square knot Keep tips of toes and fingers exposed

Dental Injuries and Missing Teeth • Require immediate dental care • Intrusion injury: tooth pushed up into socket • Avulsion injury: tooth knocked out

In Practice: Giving First Aid for an Evulsed Tooth

Key Concept • If the person can cooperate, have him or her hold an evulsed tooth under the tongue en route to the dentist. • Otherwise, place the evulsed tooth in milk. – Rationale: The client’s own saliva or the milk will help to preserve the integrity and viability of the tooth’s root system.

Foreign Objects in Eyes • Irritating to cornea, especially when the eyelid opens and closes • Scratchy effect and cause tears to flow • Caustic substances burn or destroy eyes. – FLUSH EYES IMMEDIATELY • Contact lenses – scratches or ulceration of corneas • Never attempt to remove foreign object • Seek medical assistance!

Foreign Objects in the Nose or Ears • Have child blow nose gently with both nostrils open • Do not attempt to remove it with finger or instrument • Seek medical assistance if lodged in ear

Airway Obstruction • Foreign objects often lodged in throat – If able to talk, encourage coughing – Seek medical assistance; do not leave person • If no air exchange, call 911 – Use appropriate obstructed airway techniques • Suspect obstructed airway if – Client becomes cyanotic, stops breathing, and collapses

Fainting (Syncope) • Signs/symptoms Dizziness Blackness or spots before the eyes Pallor Excessive perspiration Loss of consciousness, weak pulse, shallow breathing

In Practice: Assisting the Client Who Is Fainting

Suspected Heart Attack • Myocardial infarction (MI) also called heart attack • Symptoms – call for help immediately – Chest pain, may radiate to the left (or right) arm • Pain not relieved by rest – Pain radiating to back, neck, jaw, or teeth – Mistaken for heartburn or indigestion – Restlessness – Panic

Suspected Heart Attack, cont. • Symptoms, cont. – Feeling of impending doom – Difficulty breathing and other signs of respiratory distress – Change in pulse quality and rate – Skin is cold and clammy – Cyanosis

Treatment of Myocardial Infarctions • Thrombolytic medications – Dissolve clot and clear the blocked blood vessel – Best and most effective if given within 1 hour of onset of pain

In Practice: Giving First Aid in Suspected Heart Attack

Nursing Alerts • Myocardial infarction: The most frequent common denominator in heart attack is denial. The person cannot believe that he or she is having a heart attack. • Foreign objects: Be aware that an object such as a bean or a dried pea will swell when moistened. This makes these objects very difficult to remove, especially from the nose.

Nursing Alert • If the person with a nosebleed has a fractured skull, do not attempt to stop the bleeding. – Doing so could increase intracranial pressure. • In severe hypertension, a nosebleed may be the body’s safety valve against a cerebrovascular accident (stroke).

Wounds • Minor injuries – Cover with sterile pad, clean handkerchief, or cloth • Hemorrhage = bleeding that is abundant or uncontrollable • Assess type of bleeding – Capillary bleeding – Arterial bleeding – Venous bleeding

Hemorrhage • Treatment – Stop bleeding – Treat for shock – Apply direct pressure (over wound) – Apply indirect pressure (over pressure points) if direct pressure does not control hemorrhage • Tourniquet – use ONLY as last option – Tie around an extremity over a pressure point to stop hemorrhage – Loss of O 2 to area can cause damage to tissue

Nursing Alert • Never wipe a blood clot from a wound. – The clot acts as a plug for ruptured blood vessels. – If the clot breaks loose, death may result from external hemorrhage or from embolism.

Military Antishock Trousers (MAST) • Massive internal hemorrhage or hypovolemia • Used rarely and only by trained personnel • Careful application necessary • Careful deflation necessary

MAST Trousers

Internal Bleeding • Trauma? Consider internal bleeding. • Signs/symptoms Large or unexplained bruises and contusions Bleeding from the mouth, rectum, ears, or other body opening Dizziness when rising from a lying to a standing position, without a known cause

Internal Bleeding, cont. • Signs/symptoms, cont. Cold, clammy skin Profuse sweating Restlessness, anxiety, unexplained combative behavior Confusion, without other known causes Weak, rapid pulse Shallow, rapid breathing

Internal Bleeding, cont. • Signs/symptoms, cont. Extreme thirst Unexplained weakness Falling blood pressure Altered LOC • Treatment – Stop bleeding – Replace blood and fluids

Anaphylaxis • Hypersensitivity to allergen; also called anaphylactic effect • Triggers – Bee stings – Certain foods (eg, peanuts and chocolate) – Food additives or preservatives (eg, sulfite, MSG) – Medications (eg, antibiotics, aspirin) – Chemicals – Inhaled substances

Nursing Alert • Anaphylaxis is a true medical emergency. Time is crucial.

In Practice: Signs/Symptoms of Anaphylaxis

In Practice: Important Medications to Treat Anaphylaxis

Allergic or Anaphylactic Situation • SIRES S = Stabilize I = Identify the toxin R = Reverse the effect of the toxin E = Eliminate the toxin S = Support Open airway Activate EMS Medication

Animal Bites • Animal is almost always a household pet • Need treatment to prevent infection – Cat scratch disease/fever – Cat bite disease more serious • Rabies almost always fatal if untreated – Check immunizations given to animal – Needs antidote, given as a series of injections

Animal Bites, cont. • To help prevent infection – Cleanse area – Obtain medical care – Debride wound – Tetanus immunization – Antibiotics

Key Concepts • Capture and observe animal whenever possible. • If it cannot be located or captured, obtain an accurate description of the animal and the circumstances. • Do not destroy the animal; sometimes a length of time in quarantine is needed to determine if it is diseased or not. • In the case of a household pet, a fine may be assessed if the animal has bitten someone previously. • The law requires reporting any animal bite to the Public Health Department and the police immediately.

Exposure to Hazardous Materials • Hazardous materials (HAZMATs) in many common products – Fuel – Medications – Plastics – Home cleaning agents

Exposure to Hazardous Materials, cont. • Primary exposure: direct exposure to a hazardous substance • Secondary exposure: exposure of rescuer or healthcare provider to the contaminated person – Use personal protective equipment (PPE). – Decontaminate victim. – Special area for decontamination located in facilities

Poisoning • Treatment • Determine type: food, medication, accidental ingestion, other – Emetic medication may be ordered, causing the person to vomit (do not use with caustic substances) – Gastric lavage (“pumping the stomach”) seldom used • Follow the instructions from the Poison Control Center. • Never make the person who has ingested poison vomit unless specifically instructed to do so by the Poison Control Center or physician.

In Practice: Giving First Aid in Poisoning or Overdose

In Practice: Important Medications for Poisoning and Drug Overdose

Nursing Alert • Warn clients to never use a home canned or commercially canned item if the top is bulging, if there is dark leakage around the seams, or if there is any discoloration in the contents of jarred foods. • If there is any doubt, throw it out!

Botulism Poisoning • Severe form of food poisoning • Caused by the organism Clostridium botulinum • Signs/symptoms Weakness Headache Paralysis of eye and throat muscles Respiratory paralysis • Treatment – Antitoxins – Rescue breathing – Maintenance on ventilator

Psychiatric Emergencies • Signs/symptoms Threat to self or others Suicidal thoughts Refusal to talk History of suicide attempts Severe depression Intoxication or drug abuse, combined with suicidal or violent thoughts or actions

Psychiatric Emergencies, cont. • Signs/symptoms, cont. Self injurious behavior Out of control or bizarre behavior Evidence of self harm Evidence of no self care Reports by family or friends

Key Concepts • When dealing with an emotionally disturbed person, remain calm and speak softly, slowly, and clearly. • Maintain a non threatening posture and tone of voice. • Do not allow the person to get between yourself and the door—maintain an “escape route” for yourself. • Prevent the person from injuring him or herself or anyone else. • Seek assistance as soon as possible.

STUDENT SYNTHESIS Key Points 1. Nurses are with clients much of the time in the healthcare facility. Therefore, the nurse may be in the position to recognize and alert the appropriate staff to deal with cardiopulmonary arrest and other emergencies. 2. Nurses must use Standard Precautions when administering first aid (to whatever extent possible). 3. In emergencies, nurses and nursing students function only at their level of first aid training. Quick evaluation of the scene and planning for action are crucial.

STUDENT SYNTHESIS, cont. 4. Calling 911 will summon the EMS system in almost all areas of the United States and Canada. The nurse must know how to summon assistance in an emergency. 5. When assessing an emergency, the most important consideration is to make sure the person is breathing and that his or heart is beating. 6. Be sure to treat the injured person for shock.

STUDENT SYNTHESIS, cont. 7. Do not move an injured person, unless the situation is life threatening. Take precautions to prevent further injury. 8. All healthcare workers, including nurses, should know how to perform CPR in an emergency. Maintain current CPR certification. 9. The nurse may be called on to provide first aid assistance in a community. Each nurse has the responsibility to be knowledgeable in basic first aid techniques.

STUDENT SYNTHESIS, cont. 10. Chest injuries can result in inadequate air exchange and are immediately life threatening. Ensure that the chest wall is intact. Plug any open wound of the chest. Do not remove any penetrating objects. 11. Be aware of the possibility of injury from excessive heat or cold. Take prompt action in life threatening situations. 12. A person who is having a heart attack is often in denial. EMS personnel may need to be very persuasive to get the victim to appropriate medical care.

STUDENT SYNTHESIS, cont. 13. The first aid person must be knowledgeable in methods used to stop bleeding. 14. Anaphylaxis is a medical emergency that requires immediate treatment. 15. Follow the instructions of the Poison Control Center in the event of poisoning or overdose. 16. Remain calm when dealing with an emotionally upset client. Be alert for the possibility of suicide.
- Slides: 142