MedicoLegal issues in Upper GI and Bariatric Surgery

Medico-Legal issues in Upper GI and Bariatric Surgery Royal College of Physicians 11 St Andrews Place, Regent’s Park Mr Sakhawat (Zak) Rahman MD FRCS Consultant Surgeon HPB – Upper GI – Bariatric – General Surgery

Common Instructions - BOD • The vast proportion of instructions received (Upper GI) are related to benign disease (>90%) • And over 90% of such instructions fall into: – Bariatric Surgery – Anti-reflux and Hiatal Hernia Surgery – Bile duct injuries (Cholecystectomy) • Objectives: – Basic anatomy and pathology – Operative technique, and – Case examples (spent)
Weight Loss Surgery for Obesity Metabolic Surgery
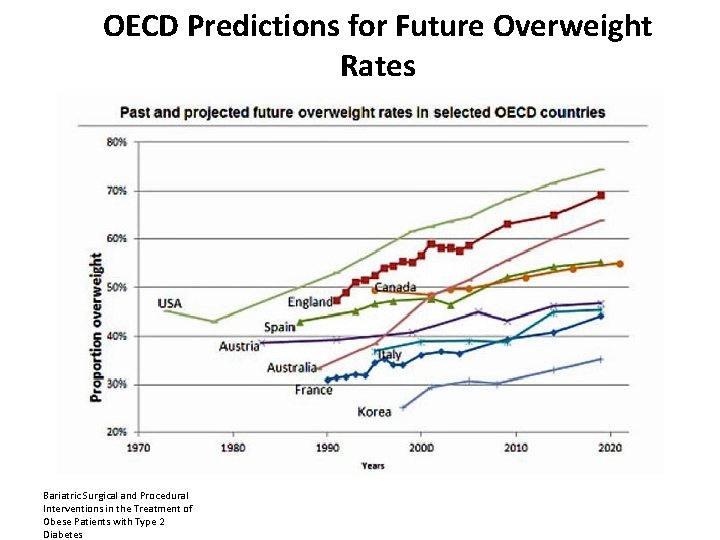
OECD Predictions for Future Overweight Rates Bariatric Surgical and Procedural Interventions in the Treatment of Obese Patients with Type 2 Diabetes

Causes of Obesity • “Thrifty” Genes – Leptin resistance – Abnormal Ghrelin • Obesogenic intrauterine environment – Maternal starvation – Maternal obesity • Environment (lifestyle) – lack of sleep – lack of physical activity • Marketing (willpower) – Larger portion sizes – Poor diet • Hormonal imbalance – Low levels of Incretins (GIP, GLP-1) – High levels of anti-Incretins Egger G, Swinburn B. An ‘ecological’ approach to the obesity pandemic. BMJ 1997; 315: 477– 80.
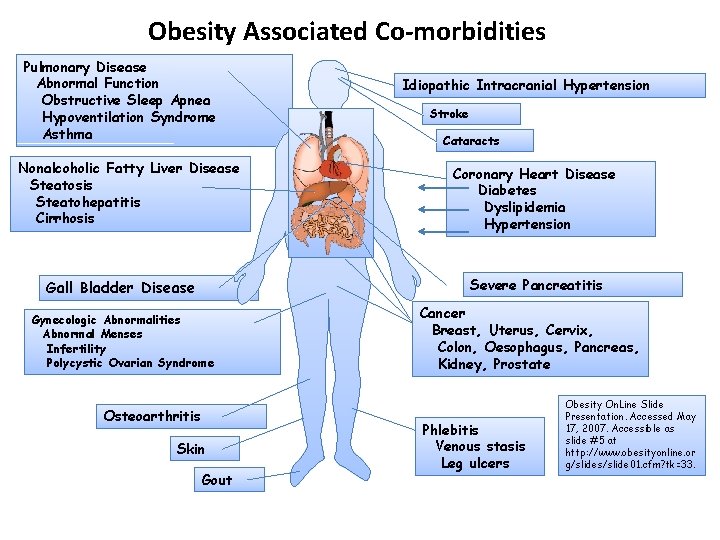
Obesity Associated Co-morbidities Pulmonary Disease Abnormal Function Obstructive Sleep Apnea Hypoventilation Syndrome Asthma Nonalcoholic Fatty Liver Disease Steatosis Steatohepatitis Cirrhosis Idiopathic Intracranial Hypertension Stroke Cataracts Coronary Heart Disease Diabetes Dyslipidemia Hypertension Severe Pancreatitis Gall Bladder Disease Gynecologic Abnormalities Abnormal Menses Infertility Polycystic Ovarian Syndrome Osteoarthritis Skin Gout Cancer Breast, Uterus, Cervix, Colon, Oesophagus, Pancreas, Kidney, Prostate Phlebitis Venous stasis Leg ulcers Obesity On. Line Slide Presentation. Accessed May 17, 2007. Accessible as slide #5 at http: //www. obesityonline. or g/slides/slide 01. cfm? tk=33.

NICE: Assessment and offering surgery BMI of 40 kg/m 2 or more, or between 35 kg/m 2 and 40 kg/m 2 and other significant disease (for example, type 2 diabetes or high blood pressure) that could be improved if they lost weight. All appropriate non-surgical measures have been tried but the person has not achieved or maintained adequate, clinically beneficial weight loss. The person has been receiving or will receive intensive management in a tier 3 service. The person commits to the need for long-term follow-up. In addition to the criteria listed above, bariatric surgery is the option of choice (instead of lifestyle interventions or drug treatment) for adults with a BMI of more than 50 kg/m 2 when other interventions have not been effective. Obesity: identification, assessment and management Clinical guideline [CG 189] Published date: November 2014

Bariatric surgery: Which obese type 2 diabetes should be considered? • Surgery should also be considered as an alternative treatment option in persons with BMI 30 to 35 when diabetes cannot be adequately controlled by optimal medical regimen, especially in the presence of other major cardiovascular disease risk factors • In Asian, and some other ethnicities of increased risk, BMI action points may be lower e. g. BMI 27. 5 to 32. 5 International Diabetes Federation (IDF) Position Statement Bariatric Surgical and Procedural Interventions in the Treatment of Obese Patients with Type 2 Diabetes Taskforce on Epidemiology and Prevention

NICE: Person with recent-onset type 2 diabetes Offer an expedited assessment for bariatric surgery to people with a BMI of 35 and over who have recent-onset type 2 diabetes as long as they are also receiving or will receive assessment in a tier 3 service (or equivalent). Consider an assessment for bariatric surgery for people with a BMI of 30– 34. 9 who have recent-onset type 2 diabetes Consider an assessment for bariatric surgery for people of Asian family origin who have recent-onset type 2 diabetes at a lower BMI than other populations Obesity: identification, assessment and management Clinical guideline [CG 189] Published date: November 2014
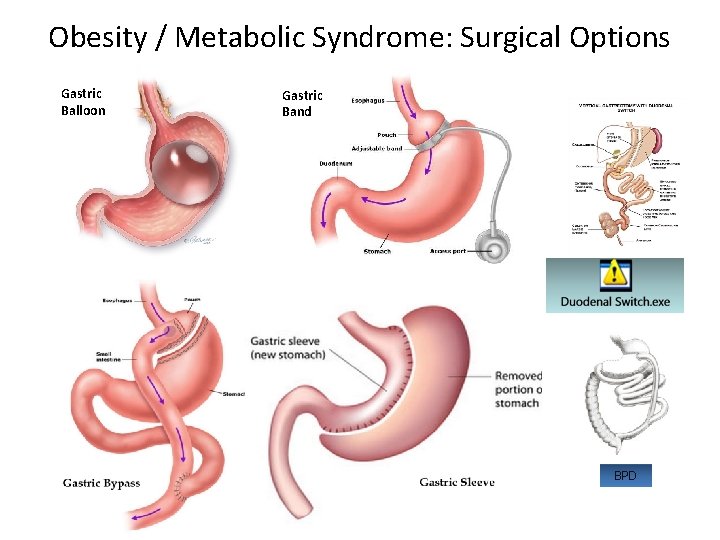
Obesity / Metabolic Syndrome: Surgical Options Gastric Balloon Gastric Band BPD
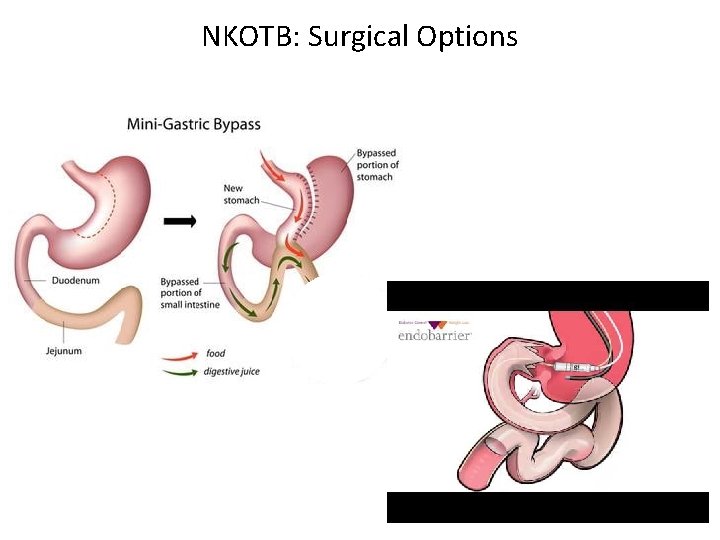
NKOTB: Surgical Options
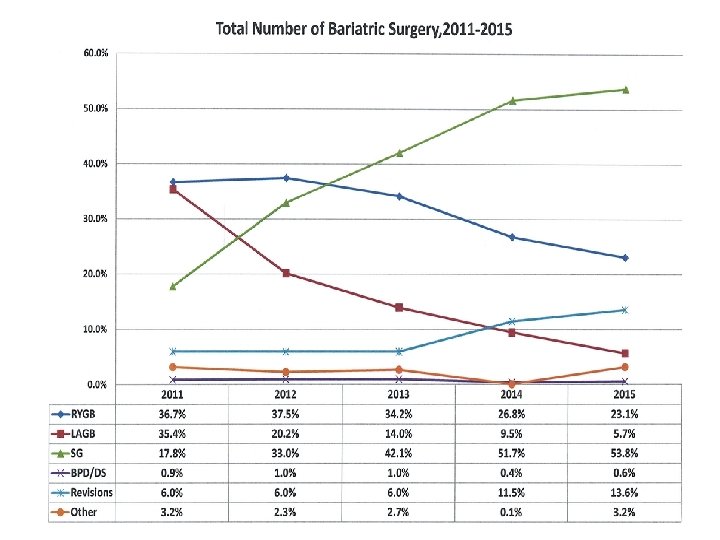
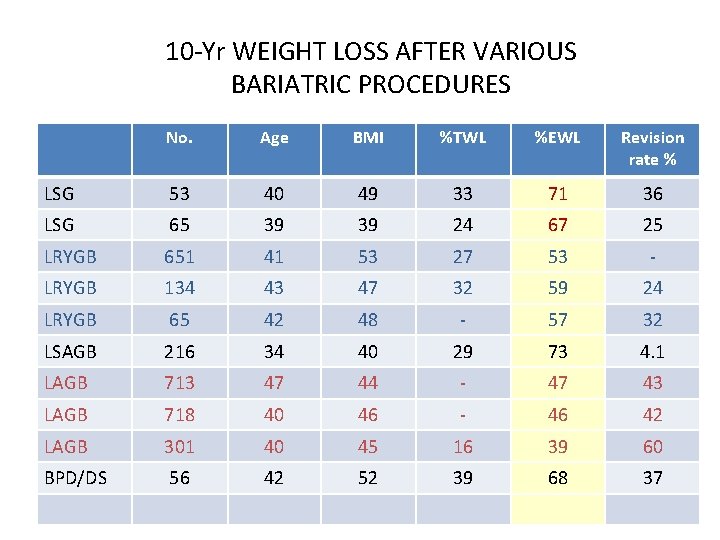
10 -Yr WEIGHT LOSS AFTER VARIOUS BARIATRIC PROCEDURES No. Age BMI %TWL %EWL Revision rate % LSG 53 40 49 33 71 36 LSG 65 39 39 24 67 25 LRYGB 651 41 53 27 53 - LRYGB 134 43 47 32 59 24 LRYGB 65 42 48 - 57 32 LSAGB 216 34 40 29 73 4. 1 LAGB 713 47 44 - 47 43 LAGB 718 40 46 - 46 42 LAGB 301 40 45 16 39 60 BPD/DS 56 42 52 39 68 37
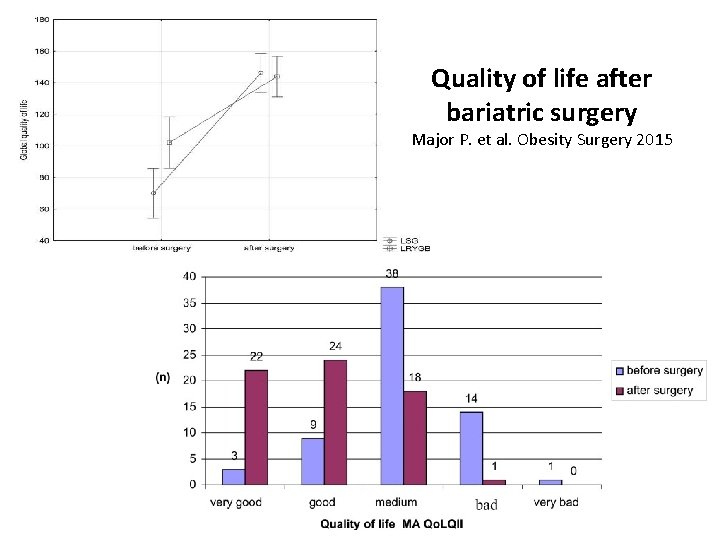
Quality of life after bariatric surgery Major P. et al. Obesity Surgery 2015

Gastric Banding (LAGB) • Day case laparoscopic procedure • Perceived as the least invasive of the “surgical” procedures • Reversible (the band can be removed) • Costs: Initial band placement & “Package” which includes 1 or 2 year followup varies from £ 3500 - £ 6000 [Private] • Disadvantages Often over the phone consultation and booking (huge private market) Requires compliance with diet and regular attendance for band fills About 10% of patient do not lose any weight. Average EWL 40% at 2 years Weight regain is common – lack of compliance with diet and follow-up Band fills after the “package” and dietary advice come at a cost (approx. £ 250 -£ 300 per band fill • Complications are relatively common • • •
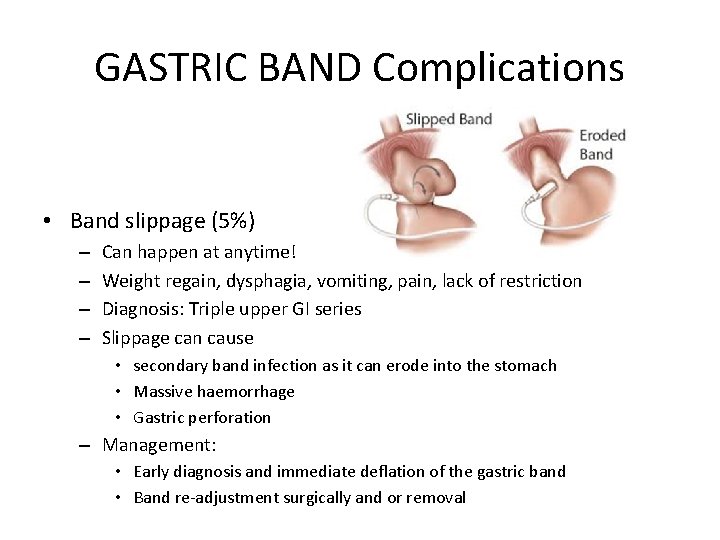
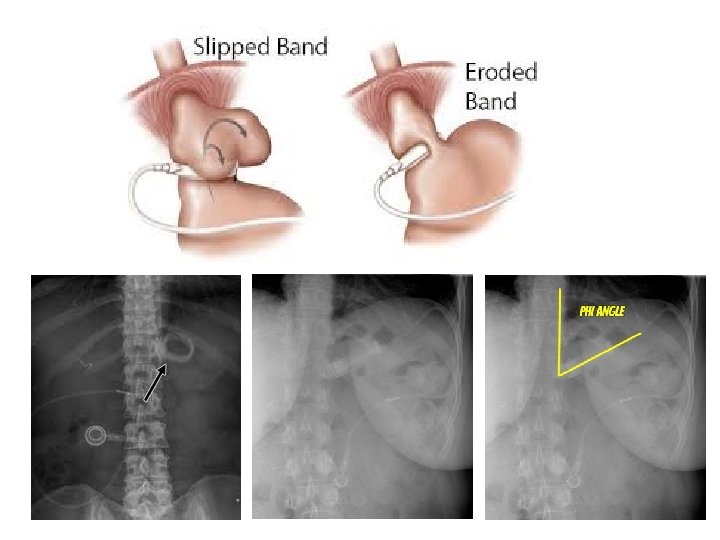
GASTRIC BAND Complications • Band slippage (5%) – – Can happen at anytime! Weight regain, dysphagia, vomiting, pain, lack of restriction Diagnosis: Triple upper GI series Slippage can cause • secondary band infection as it can erode into the stomach • Massive haemorrhage • Gastric perforation – Management: • Early diagnosis and immediate deflation of the gastric band • Band re-adjustment surgically and or removal

GASTRIC BAND Complications • Port site flippage and tubing injury – Can happen at anytime! – Difficult access to the gastric band fill port during band fill – The port is fixed to the rectus sheath, however, the sutures can give way or the port may get displaced with weight loss – Requires re-operative surgery to fix the port – cost implications! – – – Tubing injury occurs when accessing the port for band fill Often occurs if multiple attempts are made The failure to fill band or remove fluid suggests a leak. Investigated by fluoroscopic imaging Tubing may need cutting back – cost implications

GASTRIC BAND Complications • Port site infection Common complication (5%) Pain, swelling, and redness around the access port Due to band fills ? Technique ? Infected fluid ? Bad luck Antibiotics vs removal of the port (urgent) Can lead to infection of the band if left untreated or delayed management – Several cases of how the tubing is managed after the port is removed! – – – • Laparoscopic approach versus open approach • Returning the cut end of the tubing back into the abdomen • • • Both acceptable as long as all necessary and reasonable steps have been taken Advise patient of risk of ascending infection Discuss band removal in entirety and consequences Ensure that the tubing left behind is not infected – Samples for Microbiology Chase up Microbiology and act accordingly

The Gastric Band is removed – Hooray! Persistent abdominal pain after band removal…. . Fragments of tubing may be left behind Sepsis can lead to fragmentation of the tube The tubing can snap as you pull it out Issues: - Was it a recognisable component of the gastric band apparatus - Did the Surgeon check the port site and band components removed - If a section of the tubing fractures off, this may not be seen or easily accounted for Often such fragments are seen on X-rays and cross-sectional imaging.

Typical Client • Pt X 36 yr old female, BMI 36 with mild back pain • Considered a gastric band contacted a well advertised national private service to have a band fitted • Contacted by “advisor” who decided she was suitable for a band • Requested to pay the fee to secure date for surgery. Information to be sent through the post • Attended for surgery and consented on the day • Had a gastric band placement. Uncomplicated procedure and discharged February 2013 • Attended the first two follow-ups and then DNA’d further appointments

Patient X • March 2016 (3 years) later developed heartburn and upper abdominal pain • GP prescribed antacid medication • June 2016 she continues to have epigastric pain and occasional vomiting. GP referred to A&E • A&E assessment: Mild abdo pain, likely band related. AXRay and CXRay normal. No perforation. Bloods normal. Discharged with advice • August 2016 A&E attendance with upper GI bleeding and sepsis • Underwent urgent laparotomy after a CT confirmed a perforated stomach • Laparotomy: Total gastrectomy and splenectomy

Issues • Advice provided – Who, What and How? • Discussion of alternative procedures • Consent – Risks of surgery – Expectations – Expected weight loss. No weight loss – Medium & long term complications • Band slippage, erosion, infection • Port flippage, port infection, needling injury to band tubing • Weight regain Often patients are not informed that if a band has been placed in the private sector, revisional surgery or follow-up will not be accepted in the NHS The NHS will however manage patients as an emergency – band or port removal, but not replacement.

Issues – Pt X • Was the laparotomy avoidable? – Did the GP make the right call in March 2016 – Was she appropriately managed by A&E in July 2016 The GP should have considered a gastric band related complication and referred her to an NHS Bariatric Unit – referral to A&E was however appropriate in July 2016. [I would ofcourse naturally defer any such opinion to an Expert in A&E Medicine!] A&E attendance: - The clinical history suggested a band related problem: Vomiting, weight regain, epigastric pain - The abdominal X-ray showed a classical sign pathognomic of band slippage - There was a failure of the patient to be referred for a General Surgical review - The band would have been deflated and the patient referred to a Bariatric or Upper GI Surgeon - The band would have been removed within 2 to 4 weeks On the balance of probability the emergency attendance and the need for laparotomy would not have occurred.
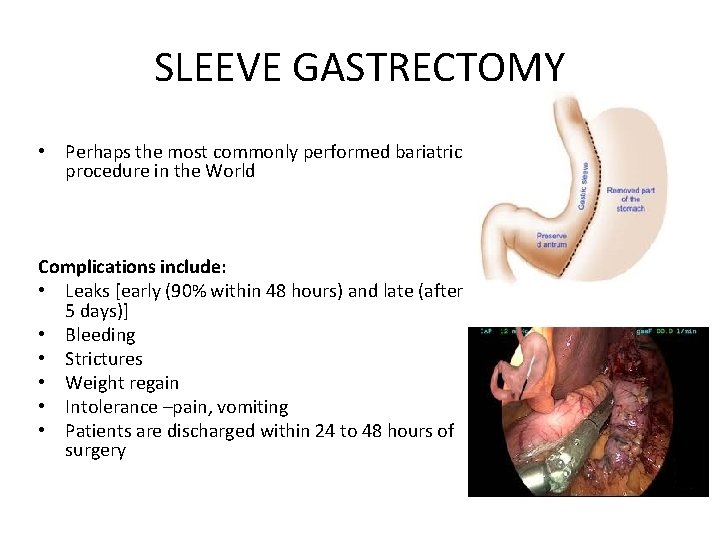
SLEEVE GASTRECTOMY • Perhaps the most commonly performed bariatric procedure in the World Complications include: • Leaks [early (90% within 48 hours) and late (after 5 days)] • Bleeding • Strictures • Weight regain • Intolerance –pain, vomiting • Patients are discharged within 24 to 48 hours of surgery

Issues on BOD - LSG • Informed Consent – Increased risk of reflux – pre-existing GERD? – Failure to lose weight – sleeve too wide? – Inability to swallow – sleeve too narrow or stricture? – Strictures – more common after leaks – Splenic injury / splenectomy – Bleeding • Operative technique – Revision surgery higher risk of complications – Was the sleeve calibrated – Bougie used? – Was a leak test undertaken – Methylene blue / air insufflation Failure to detect leak • • Early discharge – NPSA guidelines – common symptoms vs atypia – Tachycardia, high opiate usage, inability to swallow liquids, pyrexia Delayed management – weak evidence base, complex issues

Gastroesophageal reflux disease (GERD) Antireflux surgery

Issues of BOD – antireflux surgery • Did I need the operation? • Was the surgery performed to a reasonable standard? • Did I have something else wrong with me, as the operation has made we worse? – I cant swallow: the wrap was too tight – I still have reflux: the wrap was too loose – Vagal Nerve Injury, Post-vagotomy syndrome, Vagal Nerve entrapment

Definition of GERD • Montreal consensus panel (44 experts): “a condition which develops when the reflux of stomach contents causes troublesome symptoms and/or complications” • Troublesome—patient gets to decide when reflux interferes with lifestyle Vakil N, et al. Am J Gastroenterol 2006; 101: 1900

Clinical presentation • Heartburn – 1 -2 hours after eating, often at night, antacid relief • Regurgitation – Spontaneous return of gastric contents proximal to GE jxn; less well relieved with antacids • Dysphagia (40%)—difficulty with swallowing should prompt search for pathologic condition • Atypical symptoms (20 -25%) – Cough – Asthma – Hoarseness – Non-cardiac chest pain

What causes reflux? • Normal mechanisms preventing reflux – Upright posture – Anatomical: Intact crura / LES, Angulation of distal oesophagus, intraabdominal oesophagus – Intra-thoracic pressure > abdominal pressure – Normal oesophageal motility (food pushed down) – Normal stomach emptying • LES dysfunction / laxity – – – Hiatus hernia Weakness in the crura Short oesophagus Obesity Hyper acidity Gastric dysmotility

Epidemiology Hiatal Hernias • Herniation of the stomach through the oesophageal hiatus: 30% of the adult population • Asymptomatic in the vast majority • 70% of patients with GERD have a hiatus hernia • The presence of a hiatal hernia is not an indication in itself for surgery
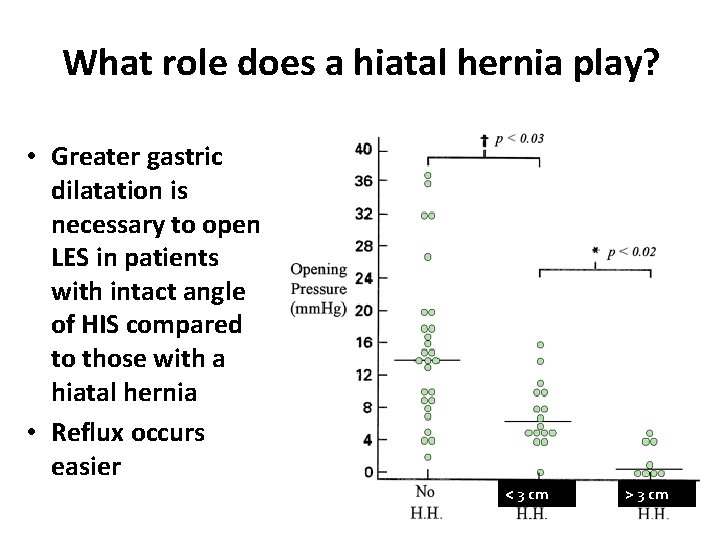
What role does a hiatal hernia play? • Greater gastric dilatation is necessary to open LES in patients with intact angle of HIS compared to those with a hiatal hernia • Reflux occurs easier < 3 cm > 3 cm
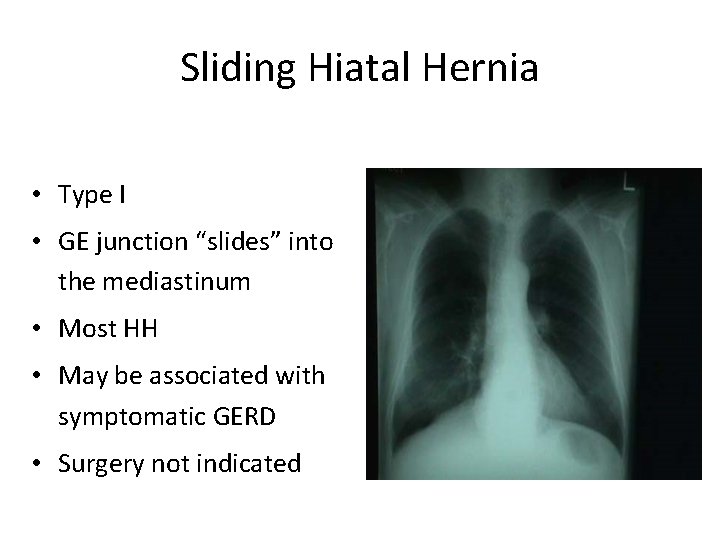
Sliding Hiatal Hernia • Type I • GE junction “slides” into the mediastinum • Most HH • May be associated with symptomatic GERD • Surgery not indicated

What does my body do to compensate for reflux esophagitis? • Compensation: – Increased swallowing saliva bathes injured mucosa, alleviating discomfort • Results in aerophagia, bloating, and belching • Distention leads to further repetitive injury to the terminal squamous epithelium in distal esophagus

Diagnosis • Diagnosis based on symptoms alone is correct in only 2/3 patients • Differential – Achalasia – Diffuse esophageal spasm – Other esophageal motility disorder – Cancer – Ulcer disease – Coronary artery disease

Who needs an operation? • Mainstay of treatment is proton pump inhibitors and lifestyle changes • Need for continuous drug treatment or escalating dose of PPI • Relatively young • Financial burden • Non-compliance with PPI • Patient choice

How do you know I’m a candidate for surgery? • Establish GERD as underlying cause of symptoms • Estimate risk of progressive disease • Determine presence or absence of esophageal shortening • Evaluate esophageal body function

What specific studies do I need preoperatively? • Endoscopy – Tumours, oesophagitis, hiatus hernia, short oesophagus etc • 24 -hour ambulatory p. H monitoring – Measures the amount of time the oesophagus is exposed to acid – Correlates acid exposure to symptoms • Fluoroscopy – contrast study – Assess oeosphageal motility, volume reflux, regurgitation • Esophageal body and gastric function – Oesophageal motility, gastric motility / emptying (pump) • Not all necessary! • Depends on pathology, symptoms and response to Rx

Am I a candidate for surgery? • Factors predictive of successful outcome following antireflux surgery (n = 199) – Abnormal score on 24 -hour esophageal p. H monitoring (p < 0. 001) – Presence of typical symptoms of GERD (heartburn and regurgitation) (p< 0. 001) – Symptomatic improvement in response to acid suppressive therapy (p = 0. 02) J Gastrointest Surg 1999; 3: 292 -300
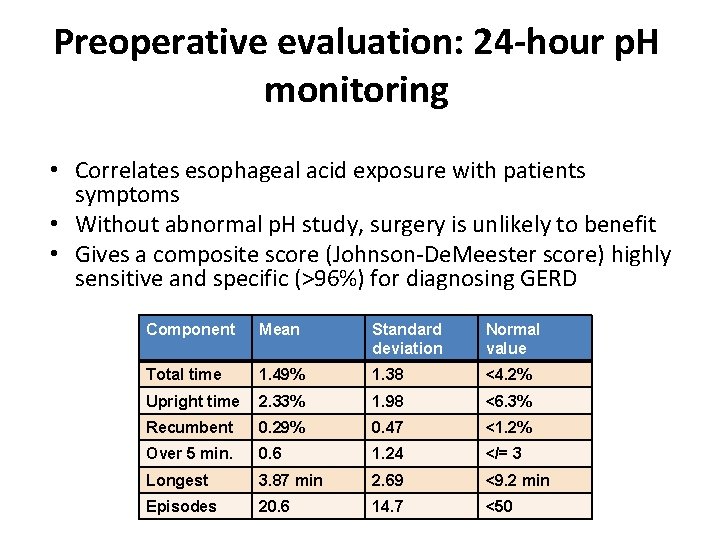
Preoperative evaluation: 24 -hour p. H monitoring • Correlates esophageal acid exposure with patients symptoms • Without abnormal p. H study, surgery is unlikely to benefit • Gives a composite score (Johnson-De. Meester score) highly sensitive and specific (>96%) for diagnosing GERD Component Mean Standard deviation Normal value Total time 1. 49% 1. 38 <4. 2% Upright time 2. 33% 1. 98 <6. 3% Recumbent 0. 29% 0. 47 <1. 2% Over 5 min. 0. 6 1. 24 </= 3 Longest 3. 87 min 2. 69 <9. 2 min Episodes 20. 6 14. 7 <50

Operative Technique & Principles of Surgery
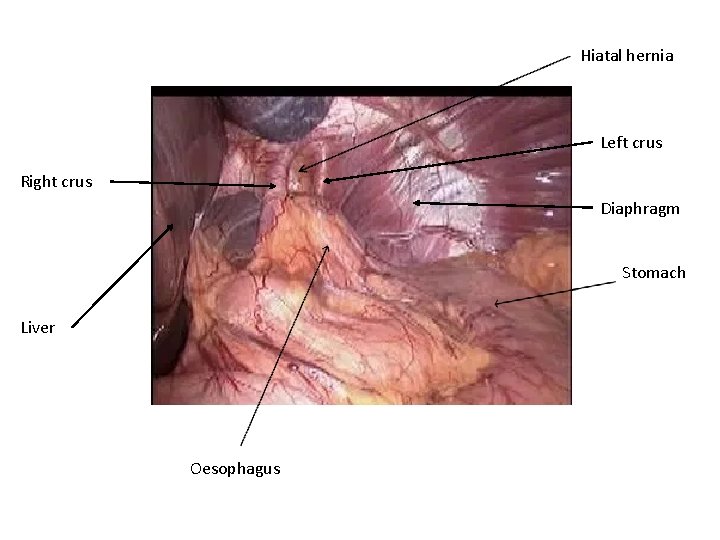
Hiatal hernia Left crus Right crus Diaphragm Stomach Liver Oesophagus

Operative procedures • The most common anti-reflux operation is the laparoscopic fundoplication – Crural dissection, – Identification and preservation of both vagi – Circumferential dissection of oesophagus and establishing a good length of intra-abdominal oesophagus • Elements of fundoplication – Crural closure (cruroplasty) – Fundic mobilization by division of short gastrics – Creation of short, loose fundoplication by enveloping anterior and posterior wall around lower esophagus
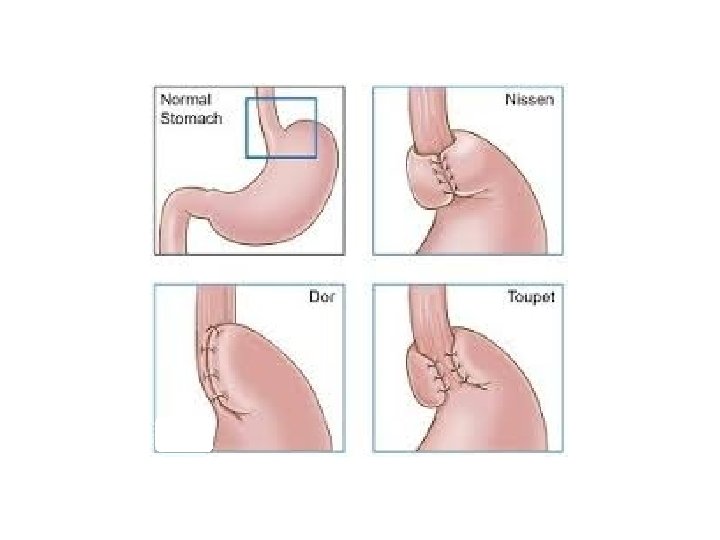
That operation looks nice, are people satisfied with it? • Patient satisfaction is high (86 -97%) • Long-term symptom relief (heartburn and regurgitation) in 84 -97% • Symptomatic failure rate 3 -13% – heartburn and regurgitation – Does not correlate with acidic reflux exposure • OPERATION DID NOTHING for 3 -13%! Surgeon, August 2009: 224.

What are the real bad things that can happen to me? • Review of 10, 489 laparoscopic antireflux procedures • Complications – Wrap herniation (early) 1. 3% – Pneumothorax 1. 0% – All others < 1% (perforation, hemorrhage, pneumonia, abscess, splenic injury, trocar hernia, effusion, PE, ulcer, atelectasis, wound infection, MI, splenectomy) JACS 2001: 193(4); 428 -39

How will I feel several months later? • Early dysphagia - usually transient (<6 weeks) • Persistent side effects (>1 month) – Bloating 9%, Reflux 4%, Dysphagia 3% Often poorly defined JACS 2001: 193(4); 428 -39 Surgeon, August 2009: 224. • Use of acid-suppressive medication after anti-reflux surgery varies (21 -62%) • But, only 20 -30% with “reflux-like” symptoms after surgery have positive p. H studies JACS 2007; 205: 570

What does all of this mean, should I have surgery or not? • Surgery wins over PPI’s if you don’t mind trading heartburn and reflux for bloating, inability to belch, and excessive flatulence RCT - Brit J Surg 2007; 94: 198. • Not in everybody, BUT IT COULD BE YOU! • Nevertheless, 86 -97% of patients are satisfied with surgery Gastroenterology 2008; 135: 1392.
![Issues – Nissen [360] • Is the wrap too tight or loose? – How Issues – Nissen [360] • Is the wrap too tight or loose? – How](http://slidetodoc.com/presentation_image_h/866a214b0ded39e57854ca05a529d643/image-51.jpg)
Issues – Nissen [360] • Is the wrap too tight or loose? – How was the problem recognised? • Revision surgery? Slipped wrap? Ongoing symptoms? • Timing of re-intervention – most problems resolve after 6 to 8 weeks – Was it calibrated with a bougie (operative note) – Was a cruroplasty done? – Was it a floppy (fundus mobilised) wrap – Was it checked for tightness • Cruroplasty – gap between oesophagus and crural repair • Between wrap and oesophagus

Para-oesophageal hernias A DIFFERENT BALL GAME!

Classification Hiatal Hernias • Classification depends on location of GEJ – Type I- “sliding” hiatal hernia – Type II- true paraesophageal hernia – Type III- “mixed” hernia- sliding hernia and true paraesophageal hernia – Type IV- intra-abdominal organ involvement
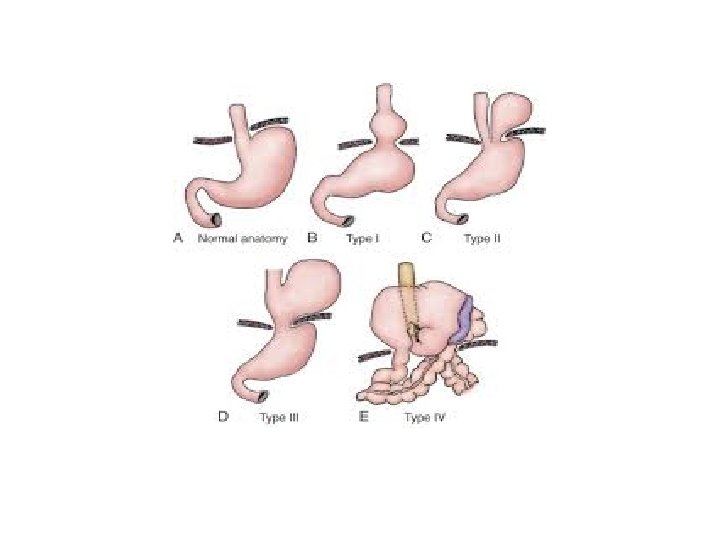
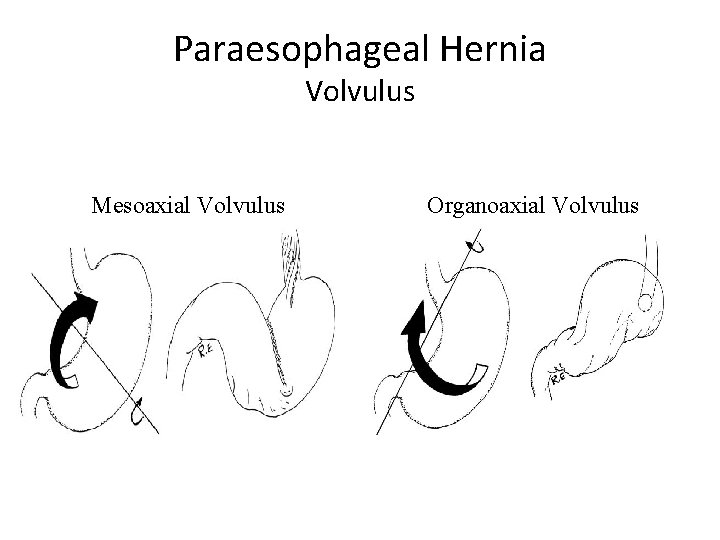
Paraesophageal Hernia Volvulus Mesoaxial Volvulus Organoaxial Volvulus

Paraesophageal Hernia Treatment Options • Observation • Medical Therapy • Surgery

Paraesophageal Hernia Observation • Assumes a low rate of gastric strangulation • Allen et al. – 23 of 147 patients followed for 12 -268 mos (median 78 mos). – Only 4 pts had progressive symptoms and 2 had elective repair – Estimate prevalence of one gastric strangulation per 245 pts J Thorac Cardiovasc Surg 1993; 105: 253

Paraesophageal Hernia Medical Therapy • Most patient are asymptomatic (incidental finding) • One-third of patients have heartburn alone – Acid inhibition – Patient clearly informed of risk of gastric strangulation, recognition of signs, and consequences – Given the age and comorbidity of such patients it is reasonable not to offer surgery unless they are symptomatic (dysphagia, chest pain, regurgitation, vomiting) Excessive (10 -50%) mortality for surgical repair of gastric strangulation
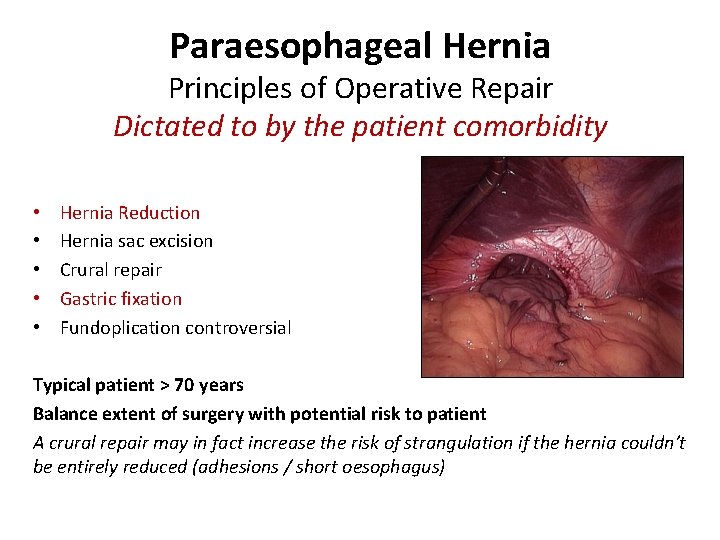
Paraesophageal Hernia Principles of Operative Repair Dictated to by the patient comorbidity • • • Hernia Reduction Hernia sac excision Crural repair Gastric fixation Fundoplication controversial Typical patient > 70 years Balance extent of surgery with potential risk to patient A crural repair may in fact increase the risk of strangulation if the hernia couldn’t be entirely reduced (adhesions / short oesophagus)

Paraesophageal Hernia Surgical Outcomes • Luketich et al. : 100 pts laparoscopic repair – 12% intra-op complications; technically demanding – 3 conversions to open procedures – 28% post-op complication rate; 0% mortality – 3% reoperation rate – 91% satisfied, 2 -day hospital stay Ann Surg 2000; 232: 608

Complications: Large Hiatal Hernia repair • • Pneumothorax - +/- chest drain (? Recognised) Intra-thoracic haemorrhage - (? over zealous dissection) Cardiac injuries (rare – ? over zealous dissection) Gastric perforation – Iatrogenic (thin friable stomach, adhesions, energy device, difficult dissection) – Left Gastric Artery injury (dissection, transection, adhesions, difficult anatomy) – Acute gastric dilatation (dysmotile stomach, pyloric oedema) Usually a combination of factors Recurrence (high risk) – most asymptomatic (20 – 50%)

VAGAL NERVE INJURY
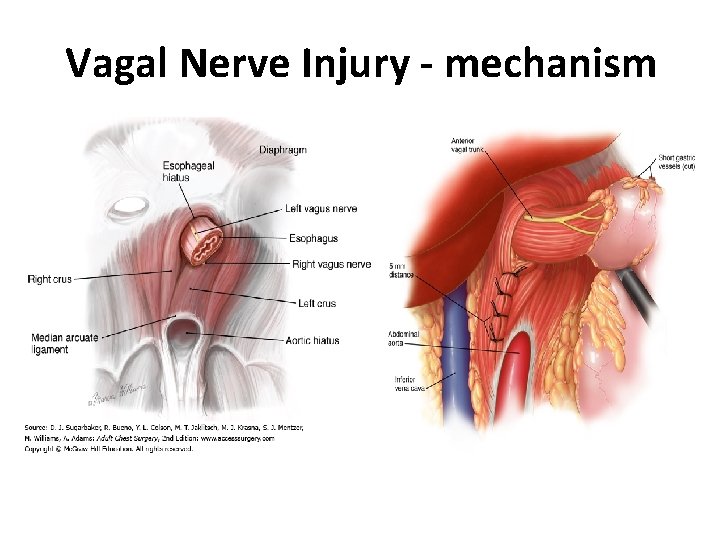
Vagal Nerve Injury - mechanism

Vagal Nerve Injury • Recognised complication of anti-reflux surgery • Increased risk in revision surgery and complex paraoesophageal hernias • The Vagus Nerves – anterior and posterior vagal nerves • Cross over function – huge overlap • Risk of injury: – Often quoted as less than 1% – Physiological testing suggests up to 30% of Vagal nerves are traumatised during surgery [unrecognised – energy device, crush injury, needle trauma] and – 10% of patients may have some associated symptoms

Vagal Nerve Injury – how? • • • Failure to identify the nerves [operative note] Difficult anatomy [revision surgery, obesity] Failure to retract out the way during cruroplasty Needle trauma (suturing) Caught by a suture (suturing wrap to oesophagus) Fibrosis / scarring

Vagal Nerve Injury What is “clinically significant” Vagal Nerve Injury Abdominal bloating Epigastric pain, Diarrhoea, Dumping syndrome Dysphagia (less common) • Such an injury can and will have a serious impact on QOL • Symptomatic management • Debilitating

Have I got a Vagal Nerve Injury? • Depends on pre-operative symptoms: Atypia, evidence of delayed gastric emptying etc. • Do they have symptoms typical of post-vagotomy syndrome? • Have they had supportive gastric emptying studies, specialised calcium stimulation tests (rare) • Is it likely a significant injury has occurred?

Surgery for Benign Disease • When there is multiplicity of operations for one condition, it proves that either none is effective, or all are effective. • The lesser the indication, the greater the complication. Mark M. Ravitch (1910– 1989) • It is difficult to make the asymptomatic patient feel better. Stanley O. Hoerr (1909– 1990)

Medico-Legal issues in Upper GI and Bariatric Surgery Royal College of Physicians 11 St Andrews Place, Regent’s Park Mr Sakhawat (Zak) Rahman MD FRCS Consultant Surgeon HPB – Upper GI – Bariatric – General Surgery
- Slides: 69