Medicina utemeljena na dokazima Kolegij Istraivanja u biomedicini

Medicina utemeljena na dokazima Kolegij: Istraživanja u biomedicini i zdravstvu III Seminar 4: Kritička procjena dokaza

Što je EBM u praksi? Koraci u medicini utemeljenoj na dokazima ◦ Korak 1: Postavljanje pitanja na koje se MOŽE odgovoriti ◦ Korak 2: Pronalaženje najboljeg dokaza ◦ Korak 3: Brza kritička procjena dokaza ◦ Korak 4: Primjena dokaza ◦ Korak 5: Procjena efektivnosti i efikasnosti procesa

3. Kritička prosudba dokaza 1. Jesu li rezultati istraživanja valjani? 2. Kakvi su rezultati? 3. Mogu li se rezultati primijeniti na konkretnog bolesnika?

Primjer: RCT Valjanost istraživanja: § Je li kliničko pitanje jasno definirano? § Je li raspodjela ispitanika u skupine bila slučajna (randomizacija)? § Je li randomizacijski slijed bio poznat liječniku koji prima ispitanike? § Jesu li analizirani svi ispitanici ili je analiza bila prema prethodnom planu (eng. intention to treat)? § Jesu li ispitanici u kontrolnoj i pokusnoj skupini podudarni u odnosu na poznate prognostičke čimbenike? § Jesu li ispitanici/liječnici/ispitivači svjesni kojoj skupini pripadaju? § Je li praćenje ispitanika bilo potpuno? § Jesu li podatci primjereno statistički obrađeni?

Primjer: ”Susjeda Vas pita hoće li pastile s cinkom pomoći njezinoj 10 -godišnjoj kćeri da lakše preboli prehladu? ” § Istraživači navode da je istraživanje randomizirano i na koji je način randomizacija provedena; § Od 124 djece u ispitivanoj skupini, 7 (6%) ih je prekinulo istraživanje, a od 125 djece u kontrolnoj skupini istraživanje je prekinulo troje (2%). § Tijekom analize, obrađeni su svi ispitanici, bez obzira na odustajanje (engl. , intention to treat analysis); § Autori navode i podrobno prikazuju parametre koji upućuju na sličnost ispitanika u kontrolnoj i pokusnoj skupini; § Autori također navode da ni djeca niti istraživači koji su davali lijek, nisu znali koji ispitanik što dobiva; § Na kraju, uvjereni ste da je dokazna snaga toga istraživanja dovoljno visoka, i da je mogućnost iskrivljenja rezultata (bias), mala.

Primjer: RCT Rezultat istraživanja: Mjere učinka liječenja § Relativno smanjenje rizika (RRR=relative risk reduction) § Apsolutno smanjenje rizika (ARR=absolute risk reduction) § Broj ispitanika koji je potreban za liječenje (NNT=1/ARR) § 95% raspon pouzdanosti (95%CI)
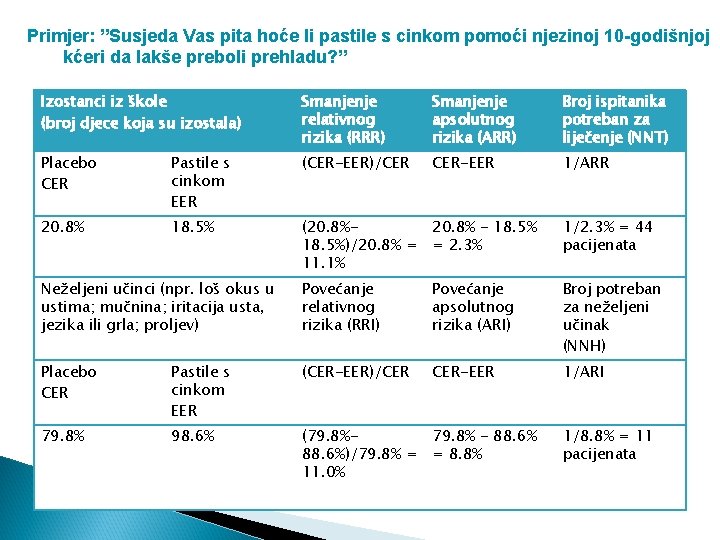
Primjer: ”Susjeda Vas pita hoće li pastile s cinkom pomoći njezinoj 10 -godišnjoj kćeri da lakše preboli prehladu? ” Izostanci iz škole (broj djece koja su izostala) Smanjenje relativnog rizika (RRR) Smanjenje apsolutnog rizika (ARR) Broj ispitanika potreban za liječenje (NNT) Placebo CER Pastile s cinkom EER (CER-EER)/CER CER-EER 1/ARR 20. 8% 18. 5% (20. 8% - 18. 5%)/20. 8% = = 2. 3% 11. 1% 1/2. 3% = 44 pacijenata Neželjeni učinci (npr. loš okus u ustima; mučnina; iritacija usta, jezika ili grla; proljev) Povećanje relativnog rizika (RRI) Povećanje apsolutnog rizika (ARI) Broj potreban za neželjeni učinak (NNH) Placebo CER Pastile s cinkom EER (CER-EER)/CER CER-EER 1/ARI 79. 8% 98. 6% (79. 8% - 88. 6%)/79. 8% = = 8. 8% 11. 0% 1/8. 8% = 11 pacijenata

Primjer: RCT Primjenjivost rezultata na konkretnog bolesnika § Jesu li ispitanici u istraživanju slični bolesniku na kojeg želimo primijeniti ispitivani postupak? § Jesu li ispitani svi klinički važni ishodi? § Može li se liječenje provesti u okruženju (engl. setting) u kojemu se bolesnik nalazi? § Postoje li drugi oblici liječenja? § Je li dobit liječenja vrijedna u odnosu na mogući rizik i cijenu?

4. Klinička primjena dokaza • Upute za kliničku praksu • Analiza odlučivanja: vjerojatnost (probability) x subjektivna ocjena stanja (utility) 5. Vrjednovanje

Što sve treba biti u članku koji opisuje RCT • CONSORT statement http: //www. consort-statement. org/ Popis za provjeru Dijagram toka

CONSORT: checklist (25 items)
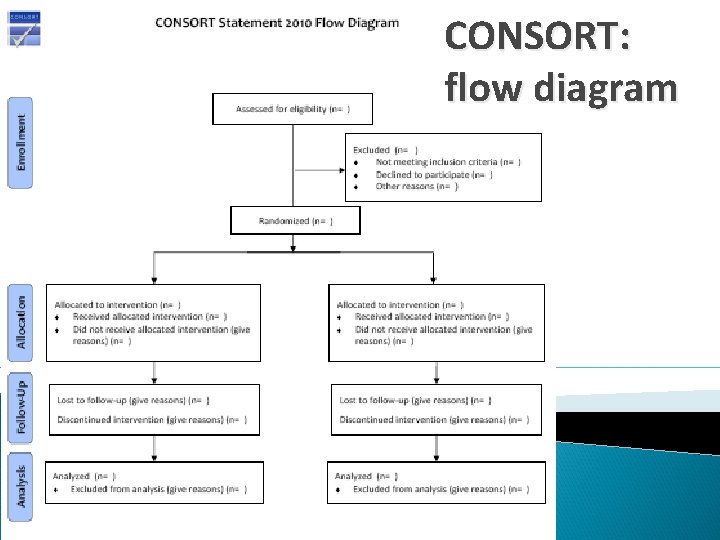
CONSORT: flow diagram

CONSORT items and examples Title and abstract 1 a Identification as a randomised trial in the title 1 b Structured summary of trial design, methods, results, and conclusions (for specific guidance see CONSORT for abstracts) 13

CONSORT items and examples Introduction Background and objectives 2 a 2 b Scientific background and explanation of rationale Specific objectives or hypotheses 14

CONSORT items and examples Introduction 15

CONSORT items and examples Methods Trial design 3 a Description of trial design (such as parallel, factorial) including allocation ratio 3 b Important changes to methods after trial commencement (such as eligibility criteria), with reasons Participants 4 a Eligibility criteria for participants 4 b Settings and locations where the data were collected 16

CONSORT items and examples Methods 17

CONSORT items and examples Methods 18

CONSORT items and examples Methods Interventions 5 The interventions for each group with sufficient details to allow replication, including how and when they were actually administered Outcomes 6 a Completely defined pre-specified primary and secondary outcome measures, including how and when they were assessed 6 b Any changes to trial outcomes after the trial commenced, with reasons 19

CONSORT items and examples Methods 20

CONSORT items and examples Methods 21

CONSORT items and examples Methods Sample size 7 a 7 b How sample size was determined When applicable, explanation of any interim analyses and stopping guidelines 22

CONSORT items and examples Methods 23

CONSORT items and examples Methods Randomisation Sequence generation 8 a Method used to generate the random allocation sequence 8 b Type of randomisation; details of any restriction (such as blocking and block size) Allocation concealment mechanism 9 Mechanism used to implement the random allocation sequence (such as sequentially numbered containers), describing any steps taken to conceal the sequence until interventions were assigned 24

CONSORT items and examples Methods 25

CONSORT items and examples Methods 26

CONSORT items and examples Methods Randomisation Implementation 10 Who generated the random allocation sequence, who enrolled participants, and who assigned participants to interventions Blinding 11 a If done, who was blinded after assignment to interventions (for example, participants, care providers, those assessing outcomes) and how 11 b If relevant, description of the similarity of interventions 27

CONSORT items and examples Methods 28

CONSORT items and examples Methods 29

CONSORT items and examples Methods Statistical methods 12 a 12 b Statistical methods used to compare groups for primary and secondary outcomes Methods for additional analyses, such as subgroup analyses and adjusted analyses 30

CONSORT items and examples Methods 31

CONSORT items and examples Methods 32

CONSORT items and examples Results Participant flow (a diagram is strongly recommended) 13 a For each group, the numbers of participants who were randomly assigned, received intended treatment, and were analysed for the primary outcome 13 b For each group, losses and exclusions after randomisation, together with reasons Recruitment 14 a Dates defining the periods of recruitment and follow-up 14 b Why the trial ended or was stopped 33
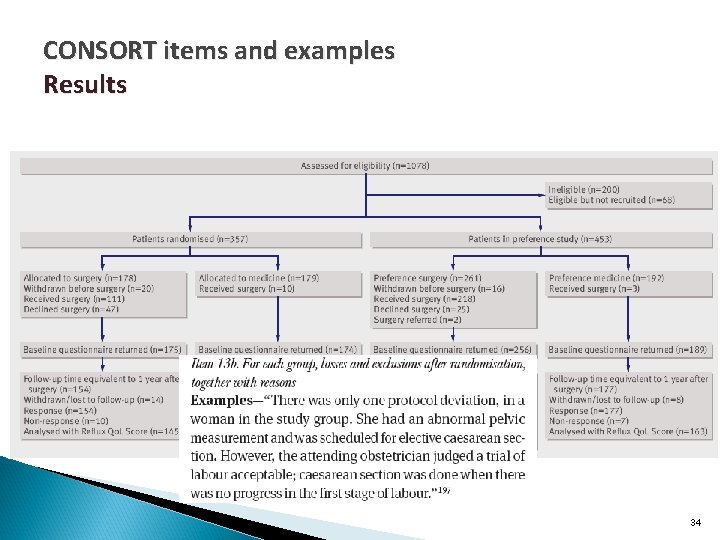
CONSORT items and examples Results 34

CONSORT items and examples Results 35

CONSORT items and examples Results Baseline data 15 A table showing baseline demographic and clinical characteristics for each group Numbers analysed 16 For each group, number of participants (denominator) included in each analysis and whether the analysis was by original assigned groups 36
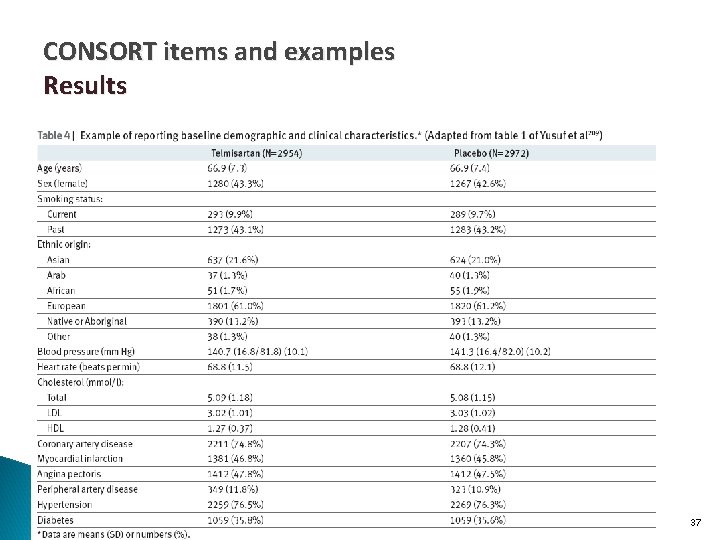
CONSORT items and examples Results 37

CONSORT items and examples Results 38

CONSORT items and examples Results Outcomes and estimation 17 a For each primary and secondary outcome, results for each group, and the estimated effect size and its precision (such as 95% confidence interval) 17 b For binary outcomes, presentation of both absolute and relative effect sizes is recommended 39
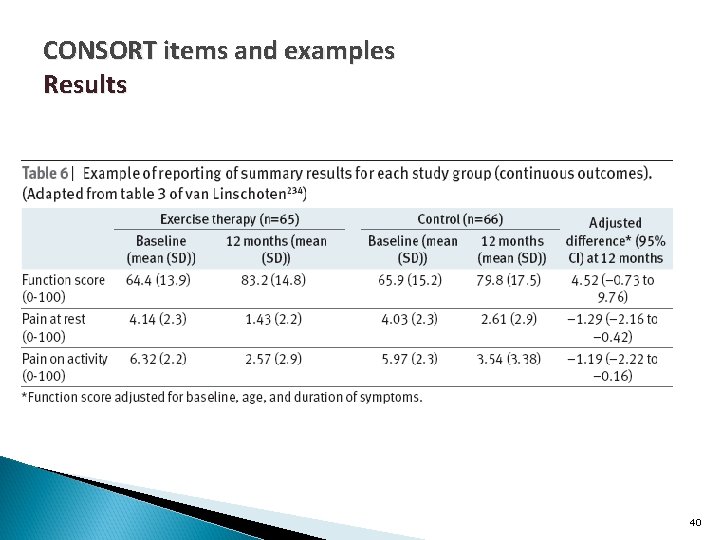
CONSORT items and examples Results 40

CONSORT items and examples Results 41

CONSORT items and examples Results Ancillary analyses 18 Results of any other analyses performed, including subgroup analyses and adjusted analyses, distinguishing pre-specified from exploratory Harms 19 All important harms or unintended effects in each group (for specific guidance see CONSORT for harms 42

CONSORT items and examples Results 43

CONSORT items and examples Results 44

CONSORT items and examples Discussion Limitations 20 Trial limitations, addressing sources of potential bias, imprecision, and, if relevant, multiplicity of analyses Generalisability 21 Generalisability (external validity, applicability) of the trial findings Interpretation 22 Interpretation consistent with results, balancing benefits and harms, and considering other relevant evidence 45

CONSORT items and examples Discussion 46

CONSORT items and examples Discussion 47

CONSORT items and examples Discussion 48

CONSORT items and examples Other information Registration 23 Registration number and name of trial registry Protocol 24 Where the full trial protocol can be accessed, if available Funding 25 Sources of funding and other support (such as supply of drugs), role of funders 49

CONSORT items and examples Other information 50

- Slides: 51