Medication Management A Caregivers Guide Presented by Amy

Medication Management: A Caregiver’s Guide Presented by Amy Pope, Pharm. D, BCPS, RPh Pharmacy Director| Harnett Health System

Objectives �Identify different types of medications �Learn important things about medication safety �Understand the components of a prescription �Learn about medication reconciliation �Explore common medication problems �Learn questions to ask about medication management �Explore programs that provide medication assistance

Types of Medications � Prescription Medications: Ordered by a provider and filled at a pharmacy or by mail order Prescription medications can be either “generic” or “brand-name” These medications types are nearly the same, but generic medications often cost less � Doctors may want patients to use brand-name medications for certain conditions � � Over-the-counter medications (OTC): Sold without a prescription � Examples include aspirin, laxatives, cold medicine, and others � Herbal medications: vitamins, dietary supplements, and herbal teas that are sold at pharmacies, health food stores, or botanicals
Medications come in many forms: Pills Capsules Liquids Patches Medicated creams Inhalers Injectable solutions Suppositories Ointments Eye drops Ear drops

Medication Management �As a caregiver, you may be giving one or more medications. Doing so includes these tasks: Order prescriptions and pick up refills Read medication labels and follow all instructions Give the right medication at the right time and in the right amount � You may be the one doing this, or you may need to teach others to do it right

Important Things to Know About Meds Common Side Effects: nausea, vomiting, confusion, dizziness Expiration Date: Medications may not be safe after this date. Throw away any medication past the “use by” date Medication Safety Don’t Share Medications: Make sure no one else takes your family member’s medication Keep All Medications in a Safe Place: Some need to be in the refrigerator. All medications must be kept away from children.

Understanding the Prescription �Prescriptions can be confusing �Often written in Latin �Says how much and how often the medications need to be taken �You should always ask the pharmacist or doctor for clear instruction �Common codes: Sig = write BID = twice daily TID = three times daily QID = four times daily Q 3 H = every 3 hours QD = daily PRN = as needed PO = by mouth

Medication Reconciliation

Medication Reconciliation �Medication reconciliation is a way to check that all of the over the counter and prescription medications are correct. The best way to do this is with a list, making sure that no medications are extra or missing. It can be hard to keep an up-to-date list as medications often change. This happens a lot when people have a new diagnosis or move from one place to another.

Ways to help - Medication Reconciliation Keep a current (up-to-date) medication list. Add all new medications, and remove medications no longer prescribed Put the medication list where you can quickly find it, even during an emergency Bring this medication list to every doctor appointment or if admitted to the hospital or nursing home Discuss all the medications with the doctor. Ask whethere any side effects or other problems to watch for. Let the doctor know if your family member also takes other medications.

Common Medication Problems

Common Medication Problems � Problem related to the name of the medication: The name of the medication you get from the pharmacy is not always the same as the name the doctor wrote on the prescription. Doctor wrote for a “brand” name while the pharmacy gave you the same medication in its “generic” name. This can happen when insurance will only pay for the generic form. � What You Can Do Ask the doctor if the name on the prescription is brand or generic Ask the doctor if it matters whether taking the brandname or generic version of this medication

Common Medication Problems �Problem reading the prescription You should compare the written prescription with the medication you get from the pharmacy �What You Can Do Tell the doctor or nurse if you cannot read the prescription Ask the doctor to tell you what the prescription is for Health care providers and caregivers can read the information for patients with vision impairments

Common Medication Problems �Problems getting prescriptions filled Insurance may not pay for certain prescriptions The pharmacy may not accept your family member’s insurance as payment The pharmacy may not have the medication �What You Can Do Talk with the doctor or nurse to see if they may have a solution Call the insurance company to see if they can help you Call other pharmacies to see if the medication is in stock, or ask when to expect if ordered

Common Medication Problems �Problems hearing what the doctor, nurse, or pharmacist is saying This can happen when the other person is rushed or you are talking in a noisy place. �What You Can Do Tell people you cannot hear, and ask them to speak louder Ask people to write what they are saying so you can read it later Make sure you understand everything before leaving the doctor, nurse, or pharmacist. It will be more difficult to get answers later

Common Medication Problems � Problems remembering to take medications It is easy to forget to take medications on time, even more so when your family member needs to take two or more medications. � What You Can Do Use special pill boxes that have sections to put pills for each meal and for bedtime Ask about special bottles with caps that count how many times the bottle has been opened Try a medication reminder app on your smart phone to remind you when to take your meds Find out from your pharmacist what to do if a dose is missed

Common Medication Problems �Problems opening pill bottles or giving medications the correct way �What You Can Do Ask the doctor or pharmacist to make a medication plan that fits your schedule Use special pill boxes that have sections to put medication for different days and different times of the day Ask about automatic pill boxes that can be set to open at specific times Easy open bottle tops Pre-split tablets if needed

Common Medication Problems �Problems swallowing tablets or capsules �Ask the doctor or pharmacist if the medication is available in other forms �Other forms: liquid, skin patch, suppository and meds that dissolve in the mouth which reduce difficulty associated with swallowing
Common Medication Problems �Scheduling logistics: Scheduling many different medications throughout the day �Work medication schedule into the daily routine �For example, meal times or bedtimes can be used as cues for scheduling medication if mealtimes and bedtimes are regularly scheduled

Common Medication Problems � Too many medicines � Common problem among � Is this medication really older adults and many people with disabilities, also referred to as “polypharmacy” � More meds a person takes, the greater risk of experiencing a medication related problem � Obtain all prescription medications from one pharmacy if possible needed? � Will the medication be a problem with other medical conditions? � Any interactions with other meds? � Right dose? � Can it be taken correctly based on the patient?

Questions to Ask about Medication Management �What is the name of the medication? �What is it being used for? �What time of day it is taken? �Should it be taken with food? �If it is to be taken “on an empty stomach”, how many hours before or after meals? �Are there any foods, drinks, or activities (such as driving) to avoid? �If the medication is prescribed “as needed”, how do you know when to give it?

Questions to Ask about Medication Management �Should I expect any problems such as side effects or allergic reactions? �What are expected side effects? Do we need to do anything if experiencing side effects? �Is the prescription for the brand name or generic form? �If a generic version is available, is that OK? �How much does the medication cost? Will insurance pay for it? �What can I do if it is not covered by insurance? �When should we stop taking this medication?

Pain Management

Pain Management �Most pain can be controlled, through a combination of drug and nondrug strategies �Caring for someone in pain or at risk for pain is often an ongoing process �Pain is whatever the person says it is and exists whenever the patient states that it does �Your job as caregiver is to make sure that good pain control is provided. Tell health professionals if pain does not improve with treatment. Your goal is to help evaluate and relieve pain.
Pain Management �Drug Strategies Prescribed pain meds Ask about also using: � Acetaminophen � Ibuprofen � Ointments/rubs Think about � Bowel regimens (stomach pain) � Others: dry eye, mouth sores �Nondrug strategies Heating pads Ice packs Dimming lights Repositioning (pillows/blankets for support) White music (ocean, birds) Back rub, massage, or warm bath

Pain Management �What you can do to help evaluate pain Ask about the pain: The best way to find out if a person is in pain is to ask. Listen for words other than “pain”: Some older people may use different words to describe their pain, such as “discomfort”, or “soreness”, or “ache”. Look for behavior or body language that could be a response to pain. Patients may be unwilling to report pain or unable to communicate about pain in words. Behaviors to look for include facial expressions or groaning when moved.

Pain Management �Improve chances for obtaining good pain relief Use pain medicines as prescribed: if the prescription says to take the pain medicine at certain times or certain time intervals, do so. Do not wait until the pain comes back to give the medicine. This will cause needless suffering. Insist on good pain control: Pain tends to be undertreated. Make sure the doctor knows there is a pain problem. Ask about pain clinics: if your doctor cannot control the pain, ask for a referral to a pain clinic. Universities and large hospitals often have clinics to evaluate and treat pain.

Traveling with Medications

Traveling with Medications �Before you go: Discuss your travel plans with your prescriber and pharmacist to properly adjust your dosing schedule by time zones Visit your prescriber to obtain all necessary prescriptions for your medications and supplies Pack enough medication to last the trip, plus at least 2 days extra Don’t pack your medications in your checked bag to avoid temperature issues and delays

Traveling with Medications �Pill/Solid You are allowed to bring all prescription and OTC medications as long as they undergo screening �Liquid/cream/gel/aerosol These are exempt from the 3 -1 -1 liquids rule, so you’re allowed to bring all prescription and OTC medications > 3. 4 oz (100 m. L) in your carry-on Medically-required liquids like baby formula, breast milk, and liquids/gels that treat hypoglycemia are allowed You don’t have to include them in the re-sealable bag along with other liquids �Insulin This is exempt from the 3 -1 -1 liquids rule It can safely pass through x-ray machines, but you can request hand inspection if needed

Obtaining Medications

Mail Order Many insurers and some pharmacies have mail order. This is helpful if medication is prescribed for a long time. Most plans allow 90 days instead of 30. May be cheaper Refill every 3 months Delivery to your house

Financial Assistance �If your family member cannot afford to pay for a medication, be sure to tell the doctor. They may have alternative medications that cost less, or can refer you to a program that specializes in medication assistance �Options: Sample meds from the doctor Free prescription trial cards Contact insurance company for alternate medication in a different “Tier” Medication assistance programs

Financial Assistance Prescription Assistance Programs � Medication Management of Harnett County (910 -8921000 ext 4092) � Cumberland County Mediation Access Program (CCMAP) (910 -433 -3602) � Project Access of Johnston County (919 -553 -4202) Websites � www. needymeds. com � http: //www. ncdhhs. gov/as sistance/low-incomeservices/medicationassistance-program � http: //www. co. cumberland. nc. us/health/services/medi cation_access. aspx � http: //johnstonhealth. org/ patients-andvisitors/resources/financial -services/project-access/
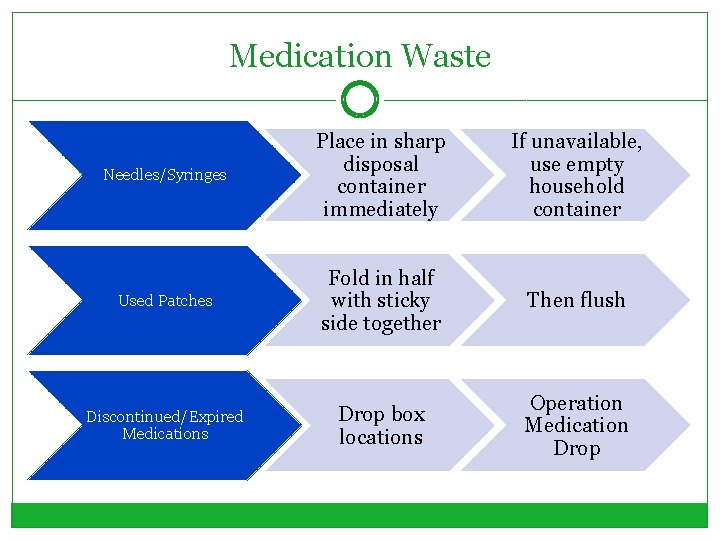
Medication Waste Needles/Syringes Place in sharp disposal container immediately If unavailable, use empty household container Used Patches Fold in half with sticky side together Then flush Discontinued/Expired Medications Drop box locations Operation Medication Drop

Medication Waste

FDA Sharps Container Recommendation

Operation Medicine Drop Prescription drug takeback events across the state can help you safely destroy old drugs to keep them from falling into the wrong hands. Safely disposing of old medications instead of flushing them down the drain prevents chemicals from ending up in the water supply. Medication Drop Box Locations in Harnett County �Lillington: Harnett Co. Sheriff’s Department – Front Lobby �Dunn: Dunn Police Department

Remember! �If you do not understand, ask! �Medication safety and adherence starts with understanding why medications are needed and when they are to be administered �Your doctor, nurse, and pharmacist are resources to help

Questions?
- Slides: 40