MEDICARE MEDICAID AND MARKETPLACE 2019 Linda Chamberlain Board

MEDICARE, MEDICAID, AND MARKETPLACE 2019 Linda Chamberlain Board Certified in Elder Law Special Needs Lawyers, PA

MEDICARE OCTOBER 15 – DECEMBER 7, 2018

THERE ARE MANY DECISIONS AND CHOICES

WHERE DO YOU START? MEDICARE. GOV

NEED HELP MAKING A DECISION? MEDICARE. GOV

MEDICARE PART A “INPATIENT” 2019 COSTS Part A Premium most people don’t pay monthly premium (you’ve paid for it through your Medicare taxes while working) (can buy Part A, premium $240 - $437 based on # of quarters Medicare taxes paid) Part A Hospital (including Mental Health) Inpatient Deductible and Co-Insurance $1, 364 deductible for each benefit period (60 days of no services) Days 1 -60: no co-insurance for each benefit period Days 61 -09: $341 co-insurance per day Days 91 and beyond: $682 co-insurance per each “lifetime reserve day” after day 90 for each benefit period (up to 60 days over your lifetime) Beyond lifetime reserve days: all costs

MEDICARE PART A “HOSPICE” 2019 COSTS No deductible for Hospice care May have no more than $5 copayment for prescription drugs for pain relief and symptom control while at home You may need to pay 5% of the Medicare-approved amount for inpatient respite care Medicare does not cover room and board while receiving hospice care in your home or another facility

MEDICARE PART A “SKILLED NURSING STAY” 2019 COST Days 1 -20: $0 for each benefit period (benefit period ends when you have gone 60 days in a row without an inpatient hospital stay or a skilled nursing stay) Days 21 -100: $170. 50 co-insurance per day of each benefit period Days 101 and beyond: All costs

MEDICARE PART B 2019 COSTS Part B Premium $135. 50 per month (or higher depending upon your income) Part B Deductible and Co-Insurance $185/year deductible and you typically pay 20% of the Medicare approved amount for most doctor services (including doctor services while an inpatient), home health services, outpatient therapy, outpatient hospital setting services (Observation status) and durable medical equipment (DME)

MEDICARE PART B 2019 COSTS Most people will pay the standard Part B premium amount, however if their modified adjusted gross income from 2 years ago is above a certain limit they will pay the standard premium and an Income Related Monthly Adjustment Amount (IRMAA). For example: if your 2017 AGI was above $85, 000 up to $107, 000 (single) or above $170, 000 up to $214, 000 (married) you would pay $189. 60/month for Part B For example: if your 2017 AGI was above $160, 000 and less than $500, 000 (single) or above $320, 000 and less than $750, 000 (married) you would pay $433. 40/month for Part B

MEDICARE PART C 2019 COSTS Part C – Medicare Advantage Plans Monthly premium varies by plan Medicare. gov has a Medicare Plan Finder online that helps you view Medicare Advantage plans (like an HMO or PPO, or Medicare Prescription Drug Plans Part D) CMS projects 36% (22. 6 million) of Medicare beneficiaries will enroll in Medicare Advantage Plans in 2019 On average premiums are decreasing 6% to $28/month, however 46% of the Medicare Advantage enrollees will pay NO monthly premium Approximately 3, 700 Medicare Advantage plans available nationwide, with most Medicare beneficiaries having 10 or more plans to change from.

MEDICARE PART C UPDATES Medicare Advantage Part C plans are required to provide Medicare Part A and B insurance coverage. Part C plans generally offer additional benefits, such as vision, dental, hearing, and many provide prescription drug coverage. Part C plans often have networks, which mean you may have to see certain doctors, go to certain hospitals, go to certain skilled rehabilitation facilities in the plan’s network to get care. You can typically choose a Part C plan if you have original Part A and B coverage You live in the service are of the plan you want to join You don’t have end-stage renal disease (requiring dialysis)

MEDICARE PART C UPDATES New types of supplemental benefits are available in 2019: Adult daycare services In-home support services and assistance for people with disabilities or medical conditions Home-based palliative care Therapeutic massage Over the counter items Meals Modifications to help keep seniors safe in their homes, like wheelchair ramps, stair rails or grab bars Nursing hotlines Transportation for medical services Tele-health services ***Medicare Disenrollment Period runs from 1/1 – 2/14/19 allowing Medicare Part C enrollees to disenroll and return to Original Medicare Coverage

MORE MEDICARE PART C UPDATES Seniors can now access cutting edge technology that delivers continuous insulin based on individual settings. Medicare will now pay for devices that will allow seniors — and their families — to use their smartphones to continuously monitor blood sugar levels. Patients can now have their doctor check in on them and receive treatment and guidance through an electronic portal instead of going to the office. (Now reimbursable) Patients can connect with their doctor by phone or video chat to see if their condition warrants them going into the office. (Now reimbursable)

BAYCARE E-WOUND CARE

BAYCARE @HOME

TYPICAL CLIENT

ALL IT TAKES IS YOUR ZIP CODE

A FEW BASIC QUESTIONS TO ANSWER
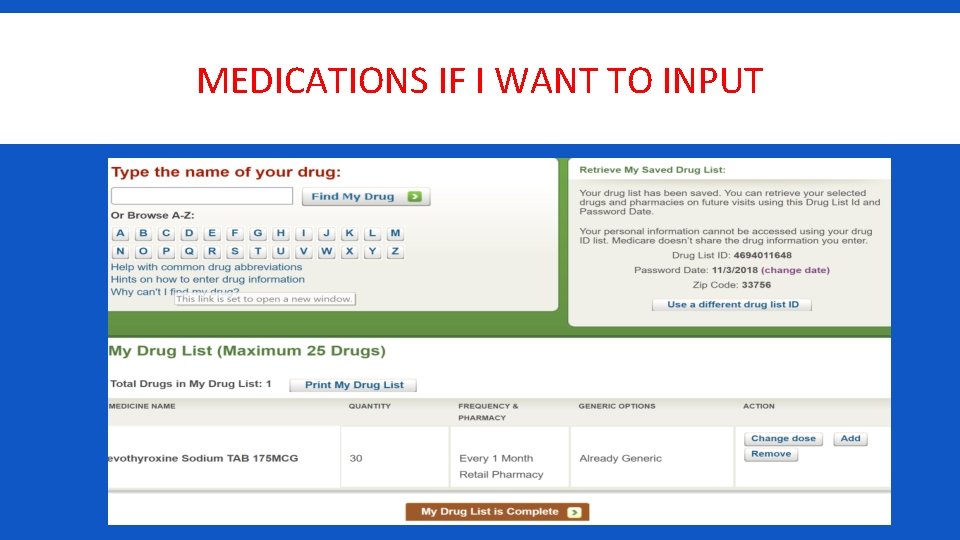
MEDICATIONS IF I WANT TO INPUT
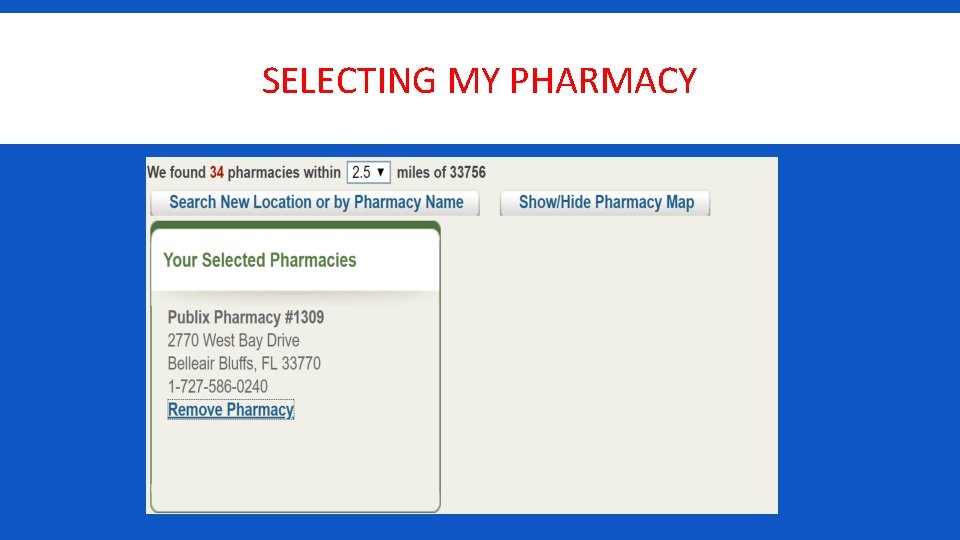
SELECTING MY PHARMACY
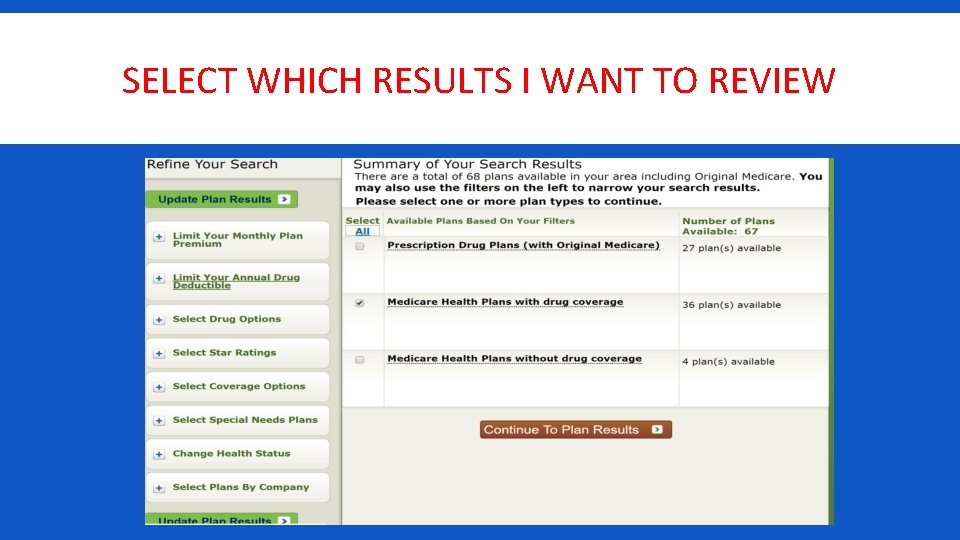
SELECT WHICH RESULTS I WANT TO REVIEW
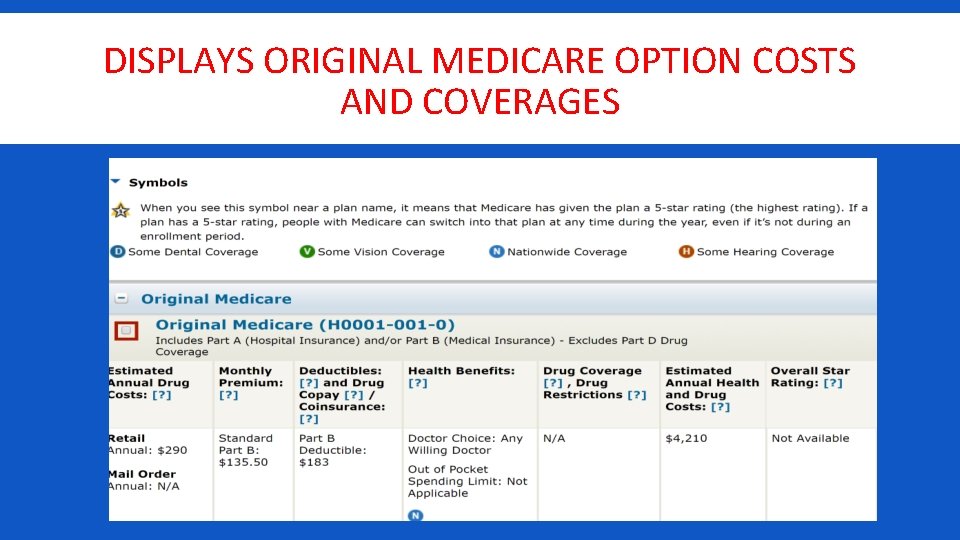

DISPLAYS ORIGINAL MEDICARE OPTION COSTS AND COVERAGES
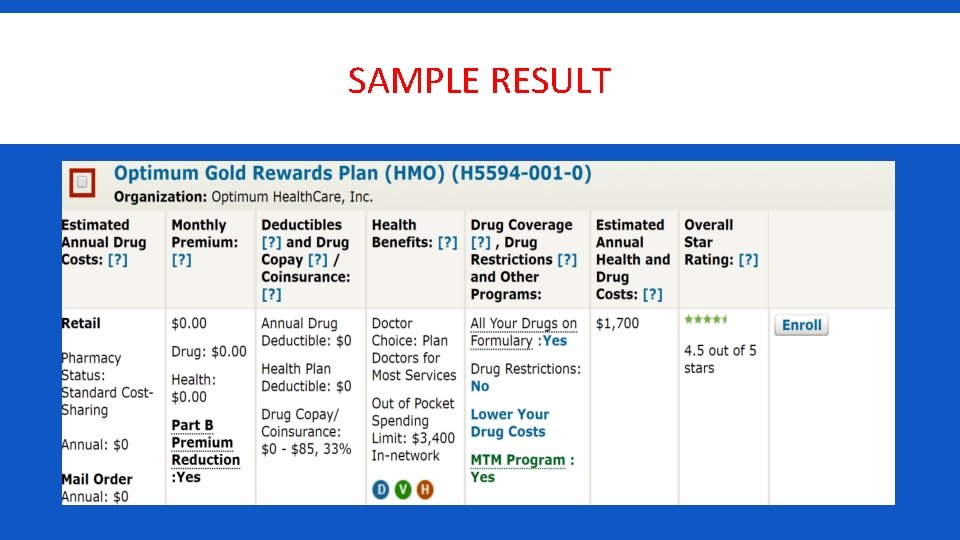
SAMPLE RESULT

SAMPLE COSTS OF PART C COVERAGE

MEDICARE PART D “PRESCRIPTION DRUG COVERAGE” 2019 COSTS Part D Premium Monthly premium varies by plan (higher-income consumers may pay more) Part D Deductible - $415 After the deductible is met, Beneficiary pays 25% of covered cost up to total prescription costs meeting the Initial Coverage Limit – Donut hole begins at $3, 820 The beneficiary pays 100% of their prescription costs up to the Out of Pocket Threshold, $5, 100. Total Part D Out of pocket spending, including the donut hole is $7, 653. 75. Catastrophic Coverage starts after this point. Total estimated spent $8, 139. 54.

FLORIDA PRESCRIPTION DRUG PRICE COMPARE TOOL

AMAZON PILL PACK

HB 21 AND F. S. 456. 44 NEW LAW ON CONTROLLED SUBSTANCE PRESCRIBING Requires all medical prescribers, Drs. , Dentists, ARNP’s, etc. . To review a patient’s controlled substance dispensing history – using statewide system E-FORCSE – Electronic-Florida Online Reporting of Controlled Substances Evaluation Program New definition of “Acute Pain. ” Acute pain is defined as “the normal, predicted, physiological, and time-limited response to an adverse chemical, thermal, or mechanical stimulus associated with surgery, trauma, or acute illness. Exempted from this definition: Cancer Terminal Condition or surgical condition that causes significant functional impairment and is not considered by the treating physician as nonmalignant pain – the physician must indicate on the prescription “NONACUTE PAIN. ” Palliative care Traumatic Injury with Severity Score of 9 or greater

HB 21 AND F. S. 456. 44 NEW LAW ON CONTROLLED SUBSTANCE PRESCRIBING If the prescriber prescribes a Schedule II controlled substance related to a traumatic injury with a severity score of 9 or greater, they must also prescribe an emergency opioid antagonist. Prescriber is limited to providing a 3 -day supply for treatment of acute pain (exceptions for up to 7 days allowed if criteria met) Prescribers are still looking for guidance re: refills via phone, in-person visit, etc… Prescribers must put on script – for Non-Acute paid if for one of the exceptions listed above.

MEDIGAP/SUPPLEMENTAL INSURANCE POLICIES Medicare Supplement Insurance (Medigap) policy helps pay some of the health care costs that Original Medicare doesn't cover, like: Co-insurance and Deductibles Medigap policies are sold by private companies. Some Medigap policies also cover services that Original Medicare doesn't cover, like medical care when you travel outside the U. S. If you have Original Medicare and you buy a Medigap policy, here's what happens: Medicare will pay its share of the Medicare-approved amount for covered health care costs. Then, your Medigap policy pays its share.

8 THINGS TO KNOW ABOUT MEDIGAP POLICIES You must have Medicare Part A and Part B. A Medigap policy is different from a Medicare Advantage Plan. Those plans are ways to get Medicare benefits, while a Medigap policy only supplements your Original Medicare benefits. You pay the private insurance company a monthly premium for your Medigap policy. You pay this monthly premium in addition to the monthly Part B premium that you pay to Medicare. A Medigap policy only covers one person. If you and your spouse both want Medigap coverage, you'll each have to buy separate policies.

8 THINGS TO KNOW ABOUT MEDIGAP POLICIES You can buy a Medigap policy from any insurance company that's licensed in your state to sell one. Any standardized Medigap policy is guaranteed renewable even if you have health problems. This means the insurance company can't cancel your Medigap policy as long as you pay the premium. Some Medigap policies sold in the past cover prescription drugs. But, Medigap policies sold after January 1, 2006 aren't allowed to include prescription drug coverage. If you want prescription drug coverage, you can join a Medicare Prescription Drug Plan (Part D). It's illegal for anyone to sell you a Medigap policy if you have a Medicare Advantage Plan, unless you're switching back to Original Medicare.

FINDING A MEDIGAP PLAN

MEDIGAP PLAN F CHANGES IN 2020 On or after January 1, 2020, a Medicare Supplement policy that provides coverage of the Part B deductible may not be sold or issued to a newly eligible Medicare beneficiary. Eliminating any new Medicare beneficiaries from being able to purchase a Plan F After January 1, 2020, you will not be able to enroll in Medicare Supplement Plan C, one of the closest alternatives to Plan F, either, since it also covers the Part B deductible. If you already have Plan F, you can keep it. The law only affects new enrollees.

MEDICARE BLUE BUTTON MEDICARE. GOV Through the Blue Button 2. 0 program, Medicare beneficiaries are able to obtain and control their Medicare claims data in a digital format, and share it with caregivers and doctors to provide better care – this will organize medication lists, etc. Blue Button 2. 0 gives you a wide range of options to manage and improve your health. Options include things like: Using an app to keep track of the regular tests and services you need based on your personal health information. The app can send you reminders when it’s time to schedule your next appointment. Using an app or other computer program to track your health over long periods of time. This can help you and your doctor make better decisions about your health. Using an app to organize your health information in an easy-to-read format, like charts and graphs. This can help you keep track of important information, like your medicines, allergies, or results of lab tests. Connecting your data to research projects. Researchers can use your data to expand their knowledge about a range of health issues.
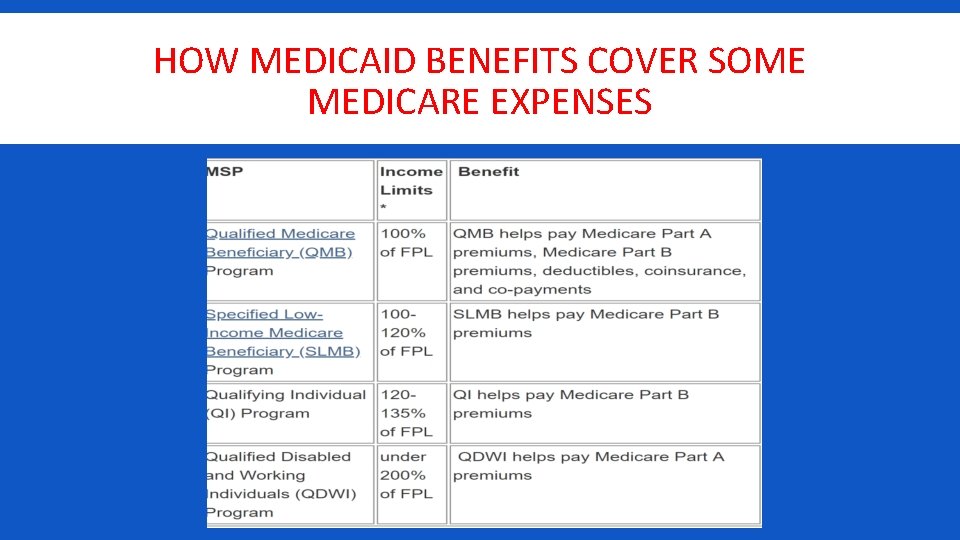
HOW MEDICAID BENEFITS COVER SOME MEDICARE EXPENSES

SMMC LONG TERM CARE
MEDICAID’S COVERED SERVICES AND HCBS WAIVERS

MEDICAID PROVIDER REGION 5 (PINELLAS/PASCO) AND REGION 6 (HARDEE, HIGHLANDS, HILLSBOROUGH, MANATEE, AND POLK)
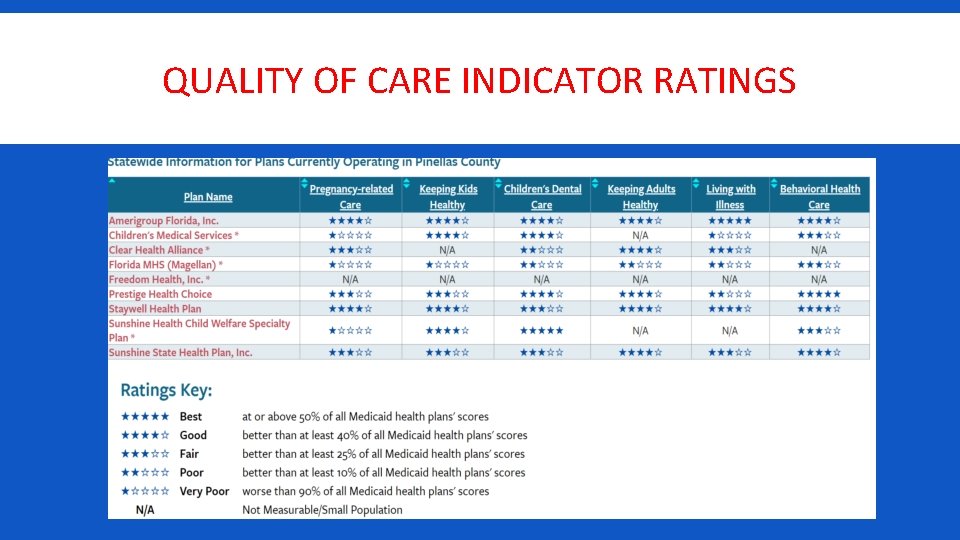
QUALITY OF CARE INDICATOR RATINGS

SMMC TRANSITIONING January 1, 2019 is when the transition will take place for Medicaid beneficiaries receiving SMMC benefits. The managed care plan must be responsible for continuity of care for new enrollees transitioning into the managed care plan. In the event a new enrollee is receiving prior authorized ongoing course of treatment with any provider, including those services previously authorized under the fee-for-service delivery system or by the enrollee’s immediate former managed care plan, the managed care plan must be responsible for the costs of continuation of such course of treatment, without any form of authorization and without regard to whether such services are being provided by participating or nonparticipating providers for up to sixty (60) days after the effective date of enrollment.

STANDARD LTC BENEFITS

SERVICES ONLY FOR LTC ENROLLEES

SMMC REPORT GUIDE

EXAMPLE OF COVERAGES DURABLE MEDICAL EQUIPMENT AND SUPPLIES

HOME HEALTH SERVICES COVERAGE

HEALTH INSURANCE MARKETPLACE OPEN ENROLLMENT Open enrollment begins November 1, 2018 – December 15, 2018 Your choice of coverage begins January 1, 2019 Cannot get coverage in 2019 if you miss open enrollment unless you qualify for a Special Enrollment Period includes certain life events: Loss of health insurance coverage (lost job, lost Medicaid) Got divorced or legally separated and lost health insurance Someone died and you lost your health insurance coverage due to their death You are moving to a new zip code or county You are getting married You are having a baby You are adopting a child

DEDUCTIBLES AND COPAYS DO YOU UNDERSTAND YOUR OWN POLICY?

SOCIAL SECURITY 2019 Social Security recipients will get a 2. 8% increase effective January 2019. Supplemental Security Income (SSI) payment amount increases to $771 for an eligible individual.

GOOGLE IS YOUR FRIEND!
- Slides: 51