Medical Surgical Nursing II SUBARACHNOID HEMORRHAGE WITH ANEURYSYM

Medical Surgical Nursing II SUBARACHNOID HEMORRHAGE WITH ANEURYSYM
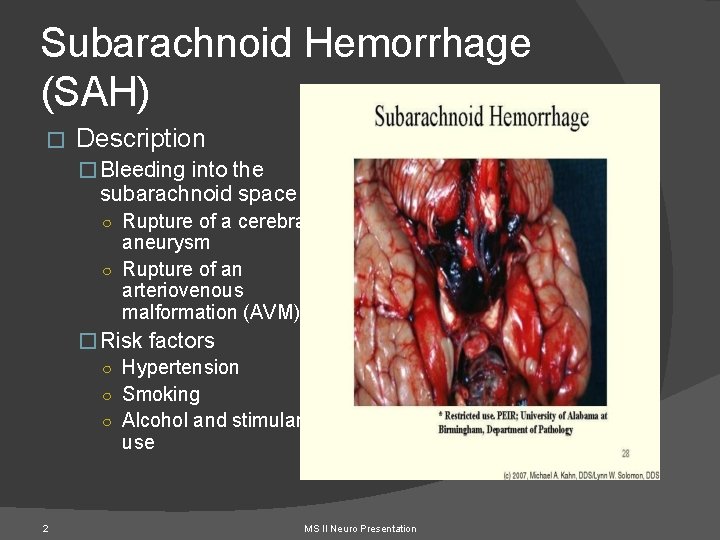
Subarachnoid Hemorrhage (SAH) � Description � Bleeding into the subarachnoid space ○ Rupture of a cerebral aneurysm ○ Rupture of an arteriovenous malformation (AVM) � Risk factors ○ Hypertension ○ Smoking ○ Alcohol and stimulant use 2 MS II Neuro Presentation

Discuss the clinical presentation of SAH as described in this case study � Assessment and Diagnosis � Clinical presentation ○ Abrupt onset of Sarah’s presentation � Sarah, a 42 year old white woman was seen in the emergency department after collapsing at work. Initially while at work Sarah was � Confused � Incontinent of urine � headache / nausea / vomiting / syncope / neurological deficit ○ May cause loss of consciousness / coma or death MS II Neuro Presentation 3

Discuss the clinical presentation of SAH as described in this case study � ER assessment � Cooperative � Pupils equal/reactive � Mildly disoriented � Subjective: Headache unlike any she had experienced before � Duration 3 to 4 weeks prior to today � Nausea – photophobia – nuchal stiffness

How is SAH diagnosed? � Clinical presentation � Non Contrast CT scan – cornerstone of SAH diagnosis � (95% of the cases CT can demonstrate blood in the subarachnoid space if performed within 48 hours of the hemorrhage) � LP is done if the initial CT finding is negative

LP (Lumbar Puncture) CSF fluid appears bloody � RBC count is greater than 1000 cells/mm# � If the LP is done five days after the SAH the fluid looks xanthochromic �

Cerebral angiography Follows to identify the exact cause of the hemorrhage � Aneurysm if this is the cause is located � It is then classified �

Pathophysiology of SAH � Cerebral Aneurysm �As cerebral aneurysm matures ○ Blood pressure rises ○ Stress placed on poorly developed and thin blood vessel wall �Most are saccular or berry-like �Often occur in the circle of Willis at the bifurcation of blood vessels �Rupture of aneurysm sends blood into the subarachnoid space (continued)
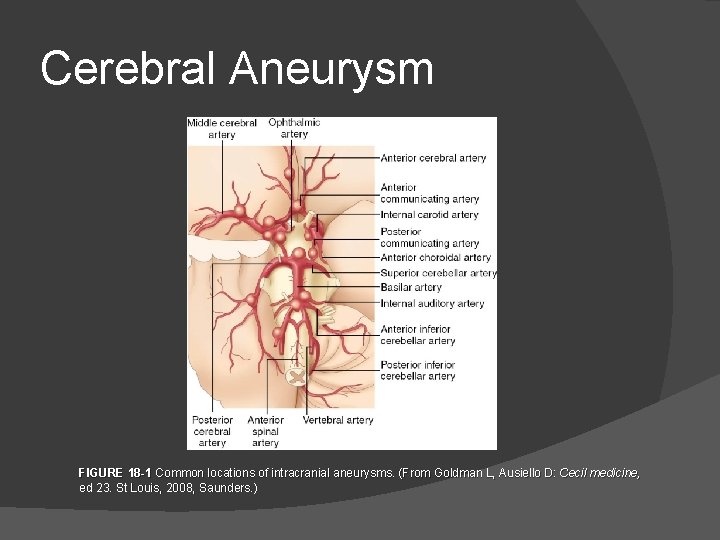
Cerebral Aneurysm FIGURE 18 -1 Common locations of intracranial aneurysms. (From Goldman L, Ausiello D: Cecil medicine, ed 23. St Louis, 2008, Saunders. )

Describe the consequences of blood in the SA space � Blood is an irritant to the tissues � Initiates an inflammatory response � Cerebral edema � Blood has decreased space in the cranial vault � Increases ICP � Decreases CPP

What therapeutic modalities are instituted after SAH � Sarah was admitted for the night. What would her priority assessments be? � Neurological check � Pupils � LOC � GCS � Vital Signs

What caused the differences in Sarah’s GCS numbers � � � On arrival her score was 14 Lethargic Arouses to name Cooperative Oriented to person only
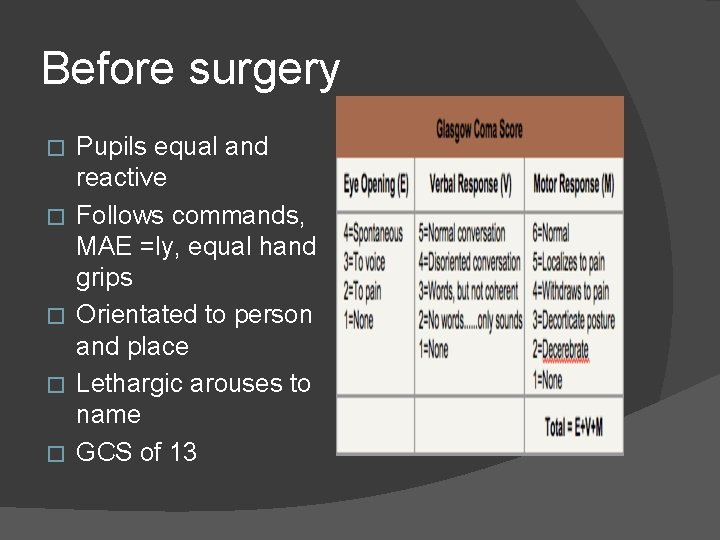

Before surgery � � � Pupils equal and reactive Follows commands, MAE =ly, equal hand grips Orientated to person and place Lethargic arouses to name GCS of 13

Apply the five major components of neurological function to Sarah � � � LOC Motor Pupillary Function Respiratory function Vitals � � � Oriented to person only day one day 2 oriented to person and place. Motor – moves all extremities =ly Pupils – equal/reactive Respiratory function 22 and 24

Vitals � � � Blood pressure day one 152/78 What is the pulse pressure? Is her pulse pressure elevated Heart rate is 102 which is significant for what stage of ICP? Day two � 142/80 � Heart rate 84 �

Medical Management of SAH Early diagnosis—SAH is medical emergency � Goal is preservation of neurological therapy � �Initial treatment ○ Support vital functions ○ Ventriculostomy to control intracranial pressure (ICP) if the patient has decreased LOC � Rebleeding (continued)

Rebleeding � Occurrence of a second SAH in an unsecured aneurysm � Less commonly AVM � Rebleeding is most common within the first _____hours but continues to be a low risk for the following month � Mortality 70% if it occurs � Again – blood pressure control individualized, avoid extremes
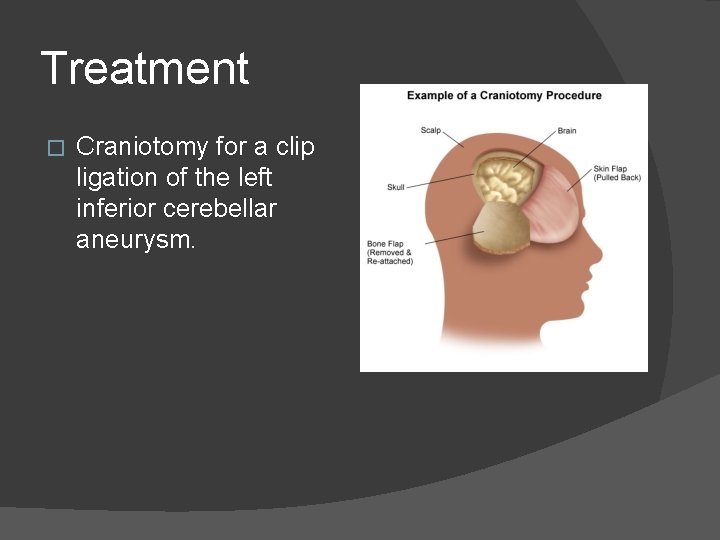
Treatment � Craniotomy for a clip ligation of the left inferior cerebellar aneurysm.
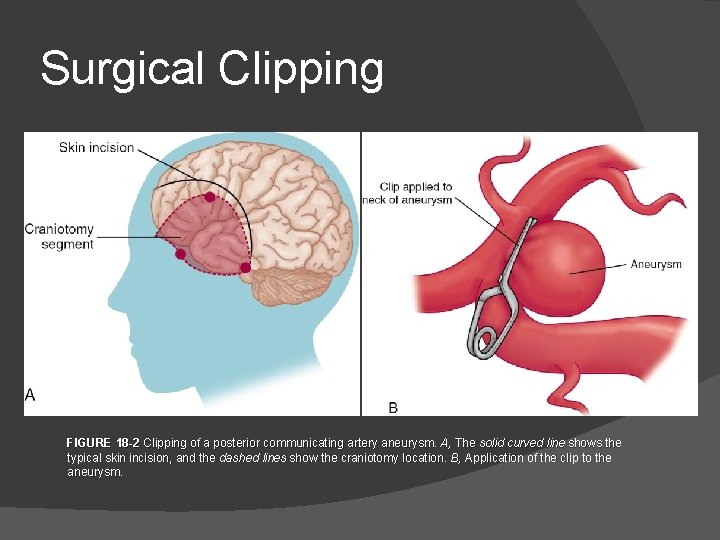
Surgical Clipping FIGURE 18 -2 Clipping of a posterior communicating artery aneurysm. A, The solid curved line shows the typical skin incision, and the dashed lines show the craniotomy location. B, Application of the clip to the aneurysm.
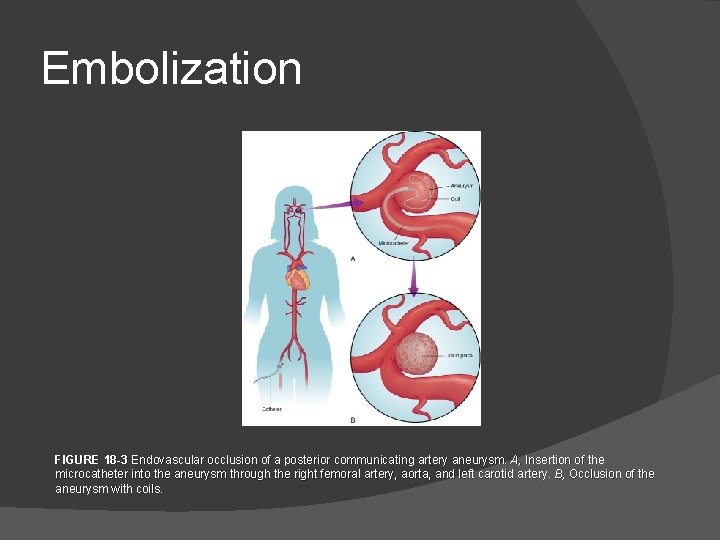
Embolization FIGURE 18 -3 Endovascular occlusion of a posterior communicating artery aneurysm. A, Insertion of the microcatheter into the aneurysm through the right femoral artery, aorta, and left carotid artery. B, Occlusion of the aneurysm with coils.

Medical Management of SAH (continued) � Surgical aneurysm clipping/surgical AVM excision � Embolization � Cerebral vasospasm: Triple H Therapy �Hypertensive/hypervolemic/hemodilution �Oral nimodipine �Transluminal cerebral angioplasty � Prevent complications �Hyponatremia �Hydrocephalus of SAH

Hypertensive/Hypervolemic/ hemodilution therapy � Used to treat cerebral vasospasm which develops in 70% of patients with SAH. � Diagnosed with cerebral antiography � Onset is ____ to 12 days after SAH � Sarah experiences this several hours after surgery. What symptoms were described?

Sarah’s Diagnosis of vasospasm � Was found with a CT scan of the head which showed no rebleeding. � This was followed with an arteriogram which demonstrated narrowing of the arteries. � What was used to assess Sarah’s response to the HHH therapy?

What is HHH therapy � Increasing the patient’s bp with vasoactive medications and fluids � Goal maintain bp between 150 and 160 systolic � Rationale: � Hemodilution: � Rationale:

What vasoactive medications are used to maintain blood pressure in this scenario � Dopamine 3 to 10 ug/kg/min � Dobutrex 2. 5 to 10 ug/kg/min � Neo-synephrine � To block vagal bradycardia which drug would be used?

Complications of HHH therapy � Cerebral edema � Increased ICP � Cardiac failure � Electrolyte imbalance

Nimodopine Therapy � Reduces poor outcomes associated with vasospasm � Dose 60 mg q 4 hours for 14 to 21 days � May produce hypotension � Bp must be maintained in spite of this drugs effects.

Hyponatremia � On arrival to the ER Sarah’s sodium was 130 mmol/L � Develops in 10 to 43% of patients with SAH – cerebral salt wasting syndrome � Onset – Several days after the initial hemorrhage � Treatment – Isotonic fluids NS

Hydrocephalus � Late complication of SAH � Blood that has circulated in the subarachnoid space and has been absorbed by the arachnoid villi may obstruct the villi and reduce the rate of CSF absorption � Temporary solution – ventriculostomy � Ventriculoperitoneal shunt.

Seizure Prophylaxis � Recommended for the SAH post operatively � Difference from stroke care � What drug IV can be given for seizure prophylaxis? � Look this medication up. � Know generic vs trade � Possible side effects 30 MS II Neuro Presentation
- Slides: 30