Medical Nutrition Therapy for Diabetes Mellitus and Hypoglycemia

Medical Nutrition Therapy for Diabetes Mellitus and Hypoglycemia of Nondiabetic Origin Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Diabetes Mellitus n A group of diseases characterized by high blood glucose concentrations resulting from defects in insulin secretion, insulin action, or both Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Diabetes and Prediabetes: Types n Type 1 (formerly IDDM, type I) n Type 2 (formerly NIDDM, type II) n Gestational diabetes mellitus (GDM) n Prediabetes (impaired glucose homeostasis) n Other specific types Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.
Prediabetes (Impaired Glucose Homeostasis) n Two forms; may have either or both – Impaired fasting glucose (IFG): fasting plasma glucose(FPG) above normal – Impaired glucose tolerance (IGT): plasma glucose elevated after 75 g glucose load Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Type 1 Diabetes n Two forms – Immune mediated: beta cells destroyed by autoimmune process – Idiopathic: cause of beta cell function loss unknown n Symptoms: hyperglycemia, polyuria, polydipsia, weight loss, dehydration, electrolyte disturbance, and ketoacidosis Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Type 2 Diabetes n Most common form of diabetes accounting for 90% to 95% of diagnosed cases n Combination of insulin resistance and beta cell failure (insulin deficiency) n Progressive disease: hyperglycemia develops gradually and may not cause the classic symptoms of type 1 diabetes Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Gestational Diabetes Mellitus (GDM) n Glucose intolerance with onset or first recognition during pregnancy n Occurs in about 7% of pregnancies Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Risk Factors for Type 2 Diabetes n BMI >25 n Physical inactivity n High-risk ethnic groups (African American, Latino, Native American, Asian America, Pacific Islander) n Previous delivery of baby >9 lbs or GDM n Hypertension n HDL <35 mg/dl or triglycerides >250 mg/dl n IGT or IFG n History of vascular disease Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Methods of Diagnosis n Fasting plasma glucose (FPG) n Casual plasma glucose (any time of day) n Oral glucose tolerance test (OGTT) Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.
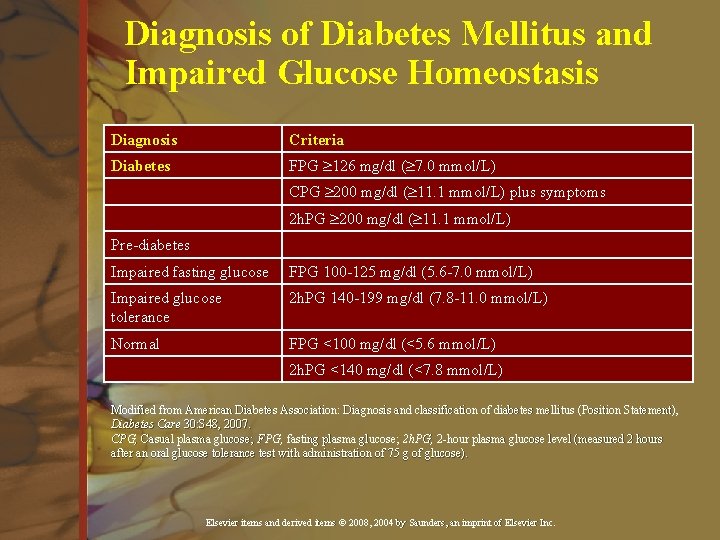
Diagnosis of Diabetes Mellitus and Impaired Glucose Homeostasis Diagnosis Criteria Diabetes FPG ³ 126 mg/dl (³ 7. 0 mmol/L) CPG ³ 200 mg/dl (³ 11. 1 mmol/L) plus symptoms 2 h. PG ³ 200 mg/dl (³ 11. 1 mmol/L) Pre-diabetes Impaired fasting glucose FPG 100 -125 mg/dl (5. 6 -7. 0 mmol/L) Impaired glucose tolerance 2 h. PG 140 -199 mg/dl (7. 8 -11. 0 mmol/L) Normal FPG <100 mg/dl (<5. 6 mmol/L) 2 h. PG <140 mg/dl (<7. 8 mmol/L) Modified from American Diabetes Association: Diagnosis and classification of diabetes mellitus (Position Statement), Diabetes Care 30: S 48, 2007. CPG, Casual plasma glucose; FPG, fasting plasma glucose; 2 h. PG, 2 -hour plasma glucose level (measured 2 hours CPG, Casual plasma glucose; FPG, after an oral glucose tolerance test with administration of 75 g of glucose). Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Algorithm for Type 1 Diabetes Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.
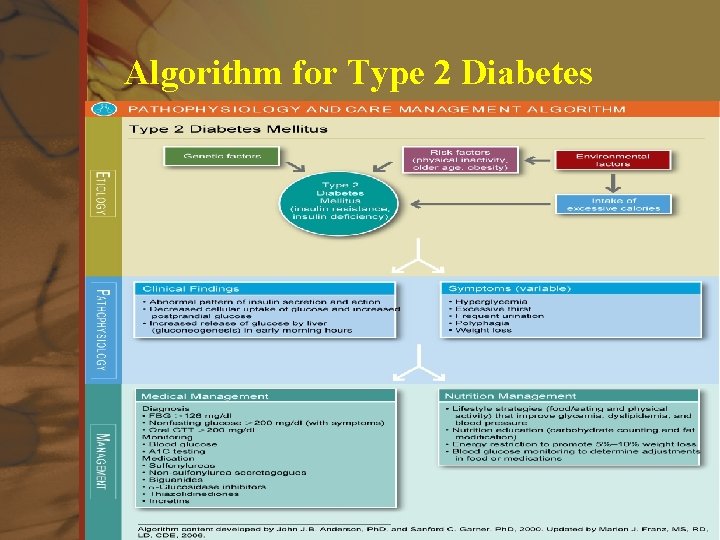
Algorithm for Type 2 Diabetes Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Management of Pre-Diabetes n Diabetes prevention trials n Lifestyle change –Increase physical activity –Moderate weight loss –Education –Reduced fat and energy intake –Regular participant follow-up –Whole grains and dietary fiber Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Management of Diabetes n Trials – Diabetes and Control and Complications Trial (DCCT) – United Kingdom Prospective Diabetes Study (UKPDS) n Management – Medical nutrition therapy – Physical activity – Monitoring – Medications – Self-management education Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Insulin Counter-regulatory Hormones n Glucagon: a hormone secreted by the A cells of the pancreatic islets of Langerhans in response to hyperglycemia; it has an opposite balancing effect to that of insulin, raising the blood sugar, and thus is used as a quick acting antidote for a low blood sugar reaction of insulin. n Epinephrine (adrenaline): Epinephrine is a chemical that narrows blood vessels and opens airways in the lungs. These effects can reverse severe low blood pressure, wheezing, severe skin itching, hives, and other symptoms of an allergic reaction. Epinephrine injection is used to treat severe allergic reactions. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Insulin Counter-regulatory Hormones n Norepinephrine: Norepinephrine /nor·epi·neph·rine/ (-ep-ĭ- nef´rin) a catecholamine, which is the principal neurotransmitter of postganglionic adrenergic neurons, having predominant α-adrenergic activity; also secreted by the adrenal medulla in response to splanchnic stimulation, being released n Cortisol: Cortisol is a steroid hormone, more specifically a glucocorticoid, which is produced by the zona fasciculata of the adrenal cortex. It is released in response to stress and a low level of blood glucose. Its functions are to increase blood sugar through gluconeogenesis. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Insulin Counter-regulatory Hormones n Growth hormone: Growth hormone (GH or HGH), also known as somatotropin or somatropin, is a peptide hormone that stimulates growth, cell reproduction and regeneration in humans and other animals. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Diabetes: Treatment Goals Recommendations for Glycemic Control for Adults With Diabetes Glycemic Control A 1 C <7. 0%* Preprandial capillary plasma glucose 90 -130 mg/dl (5. 0 -7. 2 mmol/l) Peak postprandial capillary plasma glucose† <180 mg/dl (<10. 0 mmol/l) Modified from American Diabetes Association: Standards of medical care in diabetes— 2007, Diabetes Care 30: 54, 2007. *Referenced to a nondiabetic range of 4%-6% using a DCCT-based assay. †Peak levels in patients with diabetes. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.
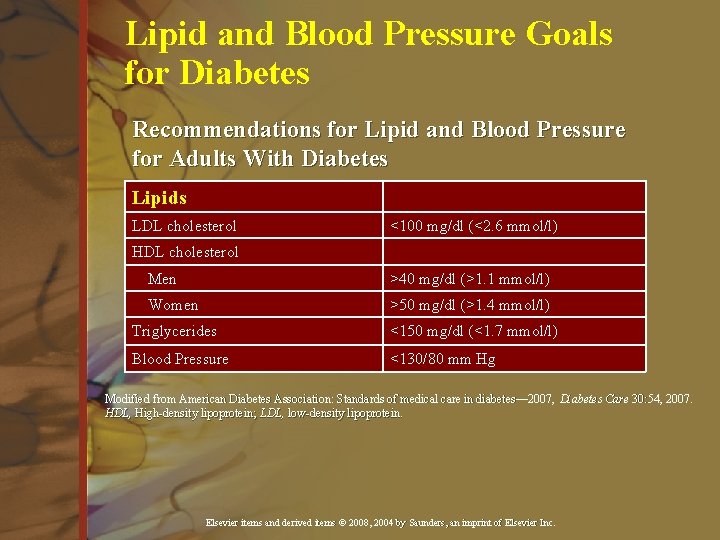
Lipid and Blood Pressure Goals for Diabetes Recommendations for Lipid and Blood Pressure for Adults With Diabetes Lipids LDL cholesterol <100 mg/dl (<2. 6 mmol/l) HDL cholesterol Men >40 mg/dl (>1. 1 mmol/l) Women >50 mg/dl (>1. 4 mmol/l) Triglycerides <150 mg/dl (<1. 7 mmol/l) Blood Pressure <130/80 mm Hg Modified from American Diabetes Association: Standards of medical care in diabetes— 2007, Diabetes Care 30: 54, 2007. HDL, High-density lipoprotein; LDL, low-density lipoprotein. High-density lipoprotein; LDL, low-density lipoprotein. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Medical Nutrition Therapy for Diabetes n Individualize energy needs and nutrition care based on metabolic profile, treatment goals, changes person is willing and able to make Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Goals of MNT for Diabetes Mellitus n Pre-diabetes – Decrease risk of diabetes and CVD by promoting healthy food choices and physical activity leading to moderate weight loss n Diabetes – Achieve and maintain BG levels in or near normal range, low-risk lipid and lipoprotein profile, low-risk blood pressure – Prevent or delay chronic complications – Address individual nutrition needs Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Goals of MNT for Diabetes Mellitus– cont’d n Specific situations – Meet unique needs to youth with type 1 or type 2 diabetes, pregnant and lactating women and older adults with diabetes – Self-management training for individuals treated with insulin or insulin secretagogues for safe exercise, prevention and treatment of hypoglycemia, and treatment of acute illness Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Carbohydrate n Low-carbohydrate diets are not recommended n Sugars do not increase glycemia more than isocaloric amounts of starch n Factors influencing glycemic response to foods: glycemic index (GI) and glycemic load (GL) n Carbohydrate counting; portions of food containing 15 g carbohydrate n Exchange lists Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Fiber n Research results are mixed n Recommend same as general public: variety of fiber-containing foods such as legumes, fiber-rich cereals (>5 g/serving), fruits, vegetables, and whole grains Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Sweeteners n Sucrose in food plan should be substituted for other carbohydrate sources or covered with insulin or glucose-lowering medications n Reduces intake of healthy foods or increases calorie intake n Fructose has no benefit over sucrose n Reduced calorie sweeteners: sugar alcohols and tagatose n Nonnutritive sweeteners: saccharin, aspartame, neotame, acesulfame potassium, and sucralose Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Protein n Does not affect blood glucose levels in well-controlled diabetes n Does not slow absorption of carbohydrate n Recommend usual protein intake (15% to 20% of kcals) Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Dietary Fat n People with diabetes have similar risk to those with past history of CVD n Recommend: – Total fat 25% to 35% of total kcals – Saturated fatty acids <7% – Minimized or eliminate trans fat – Very long omega-3 polyunsaturated fatty acids – Plant sterol and stanol esters; 2 to 3 g/day Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Alcohol n Abstain if history of abuse, pregnancy, medical problems; moderation for others n Moderate amounts of alcohol with food have minimal effect on glucose and insulin n Excessive alcohol (3+ drinks/day) contributes to hyperglycemia Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Micronutrients n No clear evidence of benefits of supplements n High-risk groups n Chromium probably not beneficial Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Physical Activity/Exercise n Integral part of treatment plan for diabetes n Improve insulin sensitivity n Reduces cardiovascular risk factors n Weight control n Improves well-being n May prevent type 2 diabetes in high-risk individuals n Glycemic responses to exercise in type 1 and type 2 diabetes Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Potential Problems with Exercise n Hypoglycemia if using insulin or insulin secretagogues – Due to increased insulin sensitivity n Hyperglycemia – Due to greater than normal increase in counterregulatory hormones n Exercise guidelines – Frequent blood glucose monitoring before, during and after exercise – Reduce insulin or ingest carbohydrate Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Insulin Guidelines for Exercise n Moderate to strenuous activity >45 to 60 minutes: decrease rapid- or short-acting insulin (1 to 2 U) n Prolonged vigorous exercise: may need 15% to 20% decrease in total daily insulin dose Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Exercise Prescription n At least 150 min/week of moderateintensity aerobic physical activity; or at least 90 min/week of vigorous aerobic exercise n Distribute over at least 3 days/week with no more than 2 consecutive days without activity n Resistance exercise 3×/week Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Oral Glucose-Lowering Medications n Newer glucose-lowering medications used alone or in combination to achieve euglycemia in type 2 diabetes n Four classes – Insulin secretagogues: sulfonylureas (first and second generation) and meglitinides (repaglinide and nateglinide) – Biguanides: metformin – Thiazolidinediones: TZDs (pioglitazone, rosiglitazone) – a-glucosidase inhibitors: acarbose, miglitol Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Glucose-Lowering Medications–cont’d n Insulin secretagogues – Sulfonylureas and meglitinides – Promote insulin secretion by b-cells n Insulin sensitizers – Enhance insulin action – Biguanides (metformin) and TZDs – Require presence of exogenous or endogenous insulin n Enzyme inhibitors (a-glucosidase inhibitors) – Inhibit enzymes that digest carbohydrates in small intestine; delay carbohydrate absorption and lower postprandial glycemia – Acarbose (Precose) and miglitol (Glyset) Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Insulin n Essential to survive in type 1 diabetes n May be needed to restore glycemia in type 2 diabetes n Onset, peak, and duration n Inhaled insulin n Individualize type and timing of insulin regimen based on eating and exercise habits and blood glucose levels n Insulin pump Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.
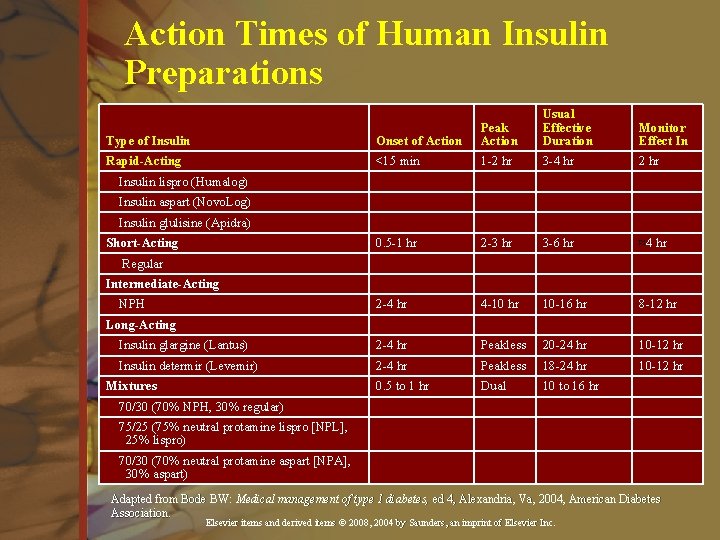
Action Times of Human Insulin Preparations Usual Effective Duration Monitor Effect In Type of Insulin Onset of Action Peak Action Rapid-Acting <15 min 1 -2 hr 3 -4 hr 2 hr Insulin lispro (Humalog) Insulin aspart (Novo. Log) Insulin glulisine (Apidra) Short-Acting 0. 5 -1 hr 2 -3 hr 3 -6 hr ≈4 hr Regular Intermediate-Acting NPH 2 -4 hr 4 -10 hr 10 -16 hr 8 -12 hr Long-Acting Insulin glargine (Lantus) 2 -4 hr Peakless 20 -24 hr 10 -12 hr Insulin determir (Levemir) 2 -4 hr Peakless 18 -24 hr 10 -12 hr Mixtures 0. 5 to 1 hr Dual 10 to 16 hr 70/30 (70% NPH, 30% regular) 75/25 (75% neutral protamine lispro [NPL], 25% lispro) 70/30 (70% neutral protamine aspart [NPA], 30% aspart) Adapted from Bode BW: Medical management of type 1 diabetes, ed 4, Alexandria, Va, 2004, American Diabetes Association. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Monitoring n Self-monitoring of blood glucose (SMBG) up to 8 times per day n Training and record-keeping n Used to adjust insulin doses and food n Continuous ambulatory blood glucose monitoring n Urine and blood ketones Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

MNT for Type 1 Diabetes n Integrate insulin regimen into usual eating habits and physical activity schedule n Multiple injections (3+/day) of insulin pump n Half insulin as basal or background; other half before meals n Total energy intake and CHO intake to avoid weight gain Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

MNT for Type 2 Diabetes n Lifestyle interventions to improve metabolic abnormalities (glycemia, dyslipidemia, hypertension) n Progressive: usually need to add medication to MNT n Blood glucose control, improve food choices, increase physical activity, moderate energy restriction to promote weight loss n Teaching: carbohydrate sources, serving sizes, number of servings, meal planning, limiting fats n SMBG Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

MNT for Type 1 Diabetes in Youth n Maintain normal growth and development n Nutrition prescription based on nutrition assessment n Use typical food and nutrition history n Adjust with age, physical activity, and growth rate n Individualize food plans and insulin regimens n Realistic blood glucose goals n Reduce risk of CVD n Meal planning approaches: CHO counting etc. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

MNT for Type 2 Diabetes in Youth n Accompanies childhood obesity n Cessation of excessive weight gain, promote normal growth and development, achieve blood glucose and A 1 C goals n Address comorbidities: hypertension and dyslipidemia n Behavior modification strategies n Metformin Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

MNT for Preexisting Diabetes and Pregnancy n Preconception counseling n Hormonal changes in first trimester lead to erratic BG levels; adjust meal plan n Increased need for insulin in second and third trimesters n Adjust meal plan to provide additional kcals n Avoid hypoglycemia and ketosis Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

MNT for Gestational Diabetes Mellitus n About 7% of pregnancies n High risk for type 2 diabetes later in life n Screening and testing n Carbohydrate-controlled meal plan, adequate energy, normoglycemia, and absence of ketosis n Individualize and adjust meal plan throughout pregnancy n Use of insulin n Carbohydrate distribution n Exercise Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

MNT for Older Adults n Increased prevalence of diabetes and IGT with age n Similar recommendations to younger population n Concern for malnutrition n Hyperglycemia and dehydration can lead to hyperglycemic hyperosmolar state (HHS) Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Nutrition Care Process n Nutrition assessment n Nutrition diagnosis n Nutrition intervention – Developing a food/meal plan – Self-management training – Facilitating behavioral changes and goal setting n Nutrition monitoring and evaluation n Follow-up Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Acute Complications n Hypoglycemia – Autonomic/adrenergic symptoms: shakiness, sweating, palpitations, anxiety, hunger – Neuroglycopenic symptoms: slow performance, difficulty concentrating, confusion and disorientation, slurred speech, irrational behavior, extreme fatigue, seizures, unconsciousness – Treatment n Hyperglycemia and diabetic ketoacidosis – DKA is life-threatening but reversible – Dawn phenomenon – Somogyi effect Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Common Causes of Hypoglycemia Inadvertent or deliberate errors in insulin doses Excessive insulin or oral secretagogue medications Improper timing of insulin in relation to food intake Intensive insulin therapy Inadequate food intake Omitted or inadequate meals or snacks Delayed meals or snacks Unplanned or increased physical activities or exercise Prolonged duration or increased intensity of exercise Alcohol intake without food Modified from American Diabetes Association: Medical management of type 1 diabetes, ed 4, Alexandria, Va, 2004, American Diabetes Association. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.
Long-Term Complications n Macrovascular diseases – Dyslipidemia – Hypertension n Microvascular diseases – Nephropathy – Retinopathy – Neuropathy Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Hypoglycemia of Nondiabetic Origin n Symptoms usually with BG <65 mg/dl n Postprandial (reactive) hypoglycemia n Alimentary hyperinsulinemia n Idiopathic reactive hypoglycemia n Fasting (food-deprived) hypoglycemia n Factitious hypoglycemia n Management: 5 or 6 small meals/day Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.

Focal Points n Nutrition therapy is a challenging but essential aspect of the management of diabetes and hypoglycemia of nondiabetic origin. n Attention to nutrition and food and meal-planning principles is essential for metabolic (glucose, lipids, and blood pressure) control and overall good health. n An RD who is knowledgeable and skilled in implementing current nutrition principles and making recommendations for diabetes or hypoglycemia of nondiabetic origin is the medical team member who should plan, implement, and evaluate MNT and the nutrition care process. n Effective education and counseling of the person with diabetes will lead to his or her becoming a team player in management of his or her blood glucose. n The effectiveness of nutrition interventions need to be continually monitored and documented to promote the best possible outcomes. Elsevier items and derived items © 2008, 2004 by Saunders, an imprint of Elsevier Inc.
- Slides: 51