Medical microbiology is a branch of medicine concerned


Medical microbiology is a branch of medicine concerned with the prevention, diagnosis and treatment of infectious diseases. There are four kinds of microorganisms that cause infectious disease; bacteria, fungi, parasites and viruses. A medical microbiologist studies the characteristics of pathogens, their modes of transmission, mechanisms of infection and growth, Using this information a treatment can be devised. Not all medical microbiologists study microbial pathology; some study common, non-pathogenic species to determine whether their properties can be used to develop antibiotics or other treatment methods.

Medical microbiological terms Pathogen : An organism that causes disease Infection: The invasion and multiplication of microorganisms such as bacteria, viruses, and parasites that are not normally present within the body. Symptoms : subjective evidence of disease or physical disturbance Antibiotic : A chemical that kills or inhibits the growth of bacteria and is used to treat bacterial infections. Vaccine : A special type of medicine that is given to both people and animals to artificially increase immunity to a particular disease and to prevent an infectious disease from developing's .
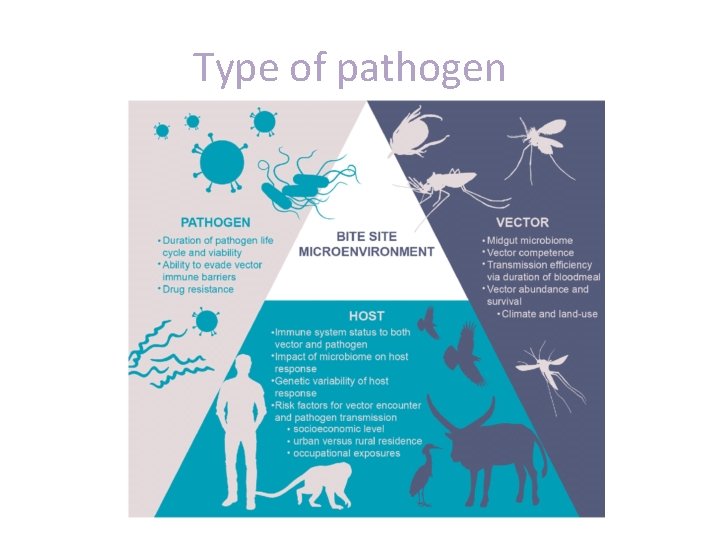
Type of pathogen

Types of pathogen Obligate pathogens (primary) These organisms have to cause disease in human being in order to continue to survive and propagate. for example Mycobacterium tuberculosis , viruses Which Capable of establishing infection and causing disease (symptomatic infections) in previously healthy individuals with intact immunological defences (immunocompetent). Immunocompetent are Able to develop an immune response. An immunocompetent body is able to recognize antigens and act against them. Immunocompetent is the opposite of immunodeficient

Types of pathogen Accidental or incidental pathogens (conditional) Causing disease confers no obvious biological advantage on the organism ex : Many bacterial pathogens Their natural habitat in humans but cause disease in only small minority Have a habitat (or reservoir) in nature but if they encounter a susceptible host in a particular way, infection may occur. The reservoir typically harbors the infectious agent without injury to itself and serves as a source from which other individuals can be infected

Types of pathogen Opportunistic pathogens Rarely cause disease in individuals with intact immunological defences (cause infection when the host defences are impaired or compromised - immunocompromised host). Ex: normal flora immunocompromised are Having a weakened immune system. Patients who are immunocompromised have a reduced ability to fight infections and other diseases. This may be caused by certain diseases or conditions, such as AIDS, cancer, diabetes, malnutrition, and certain genetic disorders. It may also be caused by certain medicines or treatments, such as anticancer drugs, radiation therapy, and stem cell or organ transplant. Also called immunosuppressed
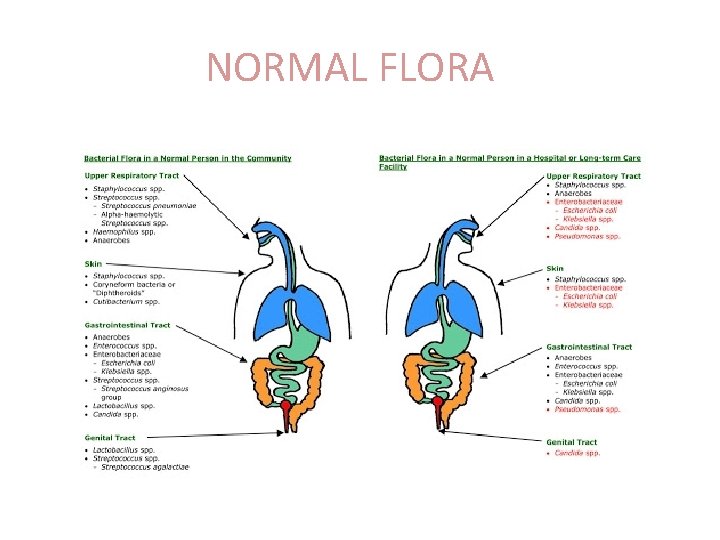
NORMAL FLORA

Normal flora Normal body flora Microbes that have adapted to living on the body, are usually present and rarely cause home, The human body harbor near 1014 bacteria. The normal flora of humans consists of a few fungi, but bacteria are the most numerous They are frequently found on or within body of healthy individuals that inhabit in our body but do not harm the host
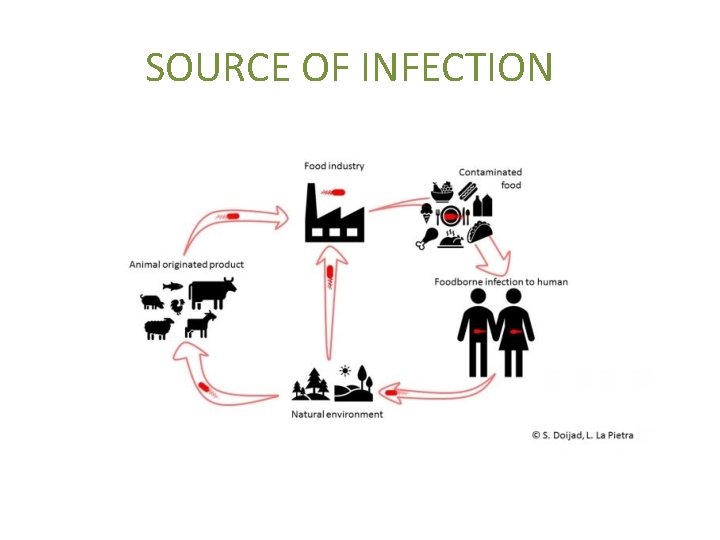
SOURCE OF INFECTION

Source of infection Organisms from the host’s normal flora cause endogenous infection , ex: Staphylococcus aureus that are normally found in the nose may cause wound infection if inoculated into surgical wound. or Organisms transmitted from another source exogenous infection whereas human is the most important source of infection or it could be Animal pathogens (Zoonotic pathogens) found in a variety of animals and may transferred to humans coming into contact with animals directly or indirectly or environmental source of infection That may affect the digestive system through contaminated food
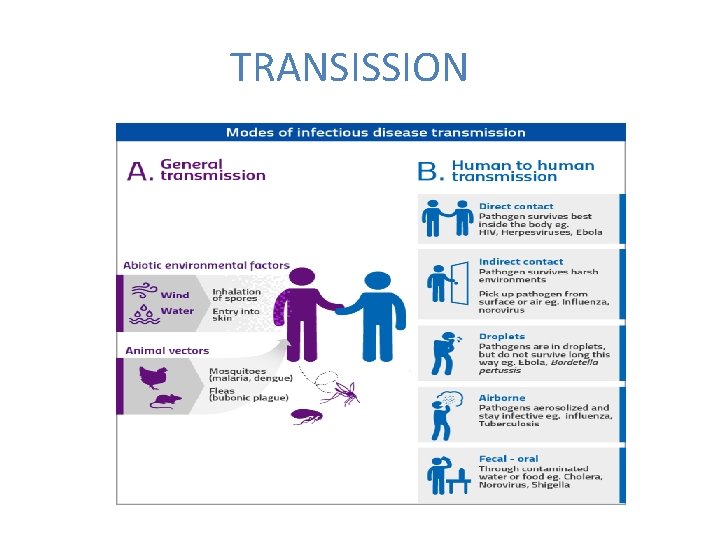
TRANSISSION

transmission Fecal-oral transmission Food and water contain pathogens that may infect the gastrointestinal tract. Organisms that cause gastrointestinal infections (diarrhoea), spread to other hosts by ingestions (faecal-oral route)

Transmission Victor-borne transmission (insect bite) Organisms with a life-cycle stage inside an insect vector that allows transmission by a biting insect Vector-borne Insects that feed on blood may transmit a wide range of pathogens: most importantly mosquitoes -transmit malaria

Transmission Air-borne transmission(respiratory) Microorganisms derived from the nose and mouth in a sneeze can remain suspended in the air on droplet nuclei (5μm). Infection may occur when these droplets are inhaled by another person Transmission of respiratory pathogens may require direct contact with infectious material- microorganisms cannot survive in the environment

Transmission Blood-borne transmission (Percutaneous/ Parenteral) Percutaneous transmission refers to exposure through any break in intact skin, whether from sharps injury (such as from needles, stylets, or surgical blades) or other types of tissue trauma. From a mother to her unborn baby Sexual transmission Sexual intercourse allows organisms with poor survival ability outside the body to be transmitted. Sexually transmitted pathogens require direct person-to-person mucosal contact for transmission
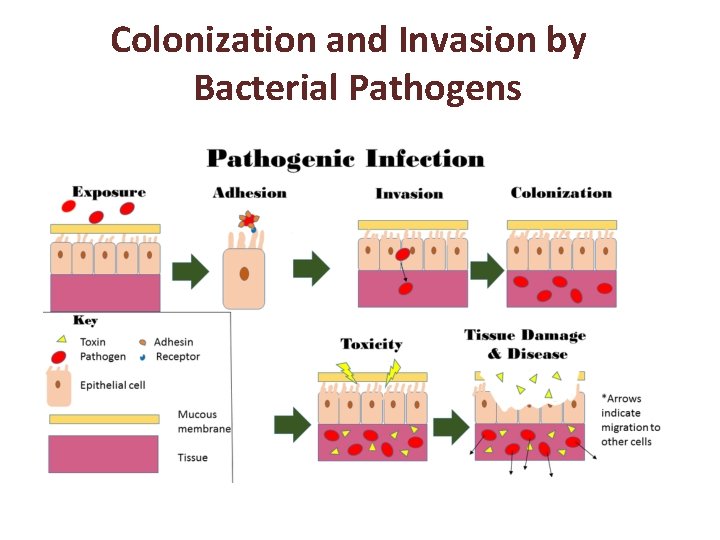
Colonization and Invasion by Bacterial Pathogens

Colonization and Invasion by Bacterial Pathogens Adherence A surface structure or macromolecule that binds a bacterium to a specific surface In its simplest form, bacterial adherence or attachment to a eucaryotic cell or tissue surface requires the participation of two factors: a receptor and a ligand. The receptors so far defined are usually specific carbohydrate or peptide residues on the eucaryotic cell surface. The bacterial ligand, called an adhesin, is typically a macromolecular component of the bacterial cell surface which interacts with the host cell receptor. Adhesins and receptors usually interact in a complementary and specific fashion with specificity comparable to enzyme-substrate relationships and antigen-antibody reactions.

Colonization and Invasion by Bacterial Pathogens COLONIZATION The first stage of microbial infection is colonization: the establishment of the pathogen at the appropriate portal of entry. Pathogens usually colonize host tissues that are in contact with the external environment. Sites of entry in human hosts include the urogenital tract, the digestive tract, the respiratory tract and the conjunctiva. Organisms that infect these regions have usually developed tissue adherence mechanisms and some ability to overcome or withstand the constant pressure of the host defenses at the surface.

Invasiveness is the ability of a pathogen to invade tissues. Invasiveness encompasses (1) mechanisms for colonization (adherence and initial multiplication), (2) production of extracellular substances ("invasins"), that promote the immediate invasion of tissues and (3) ability to bypass or overcome host defense mechanisms which facilitate the actual invasive process. This chapter deals with the first two aspects of of invasiveness: colonization and invasion.

Microbial pathogenicity has been defined as the structural and biochemical mechanisms whereby microorganisms cause disease. Pathogenicity in bacteria may be associated with unique structural components of the cells (e. g. capsules, fimbriae, LPS or other cell wall components) or active secretion of substances that either damage host tissues or protect the bacteria against host defenses. Hence, there are two broad qualities of pathogenic bacteria that underlie the means by which they cause disease: invasiveness and toxigenesis.
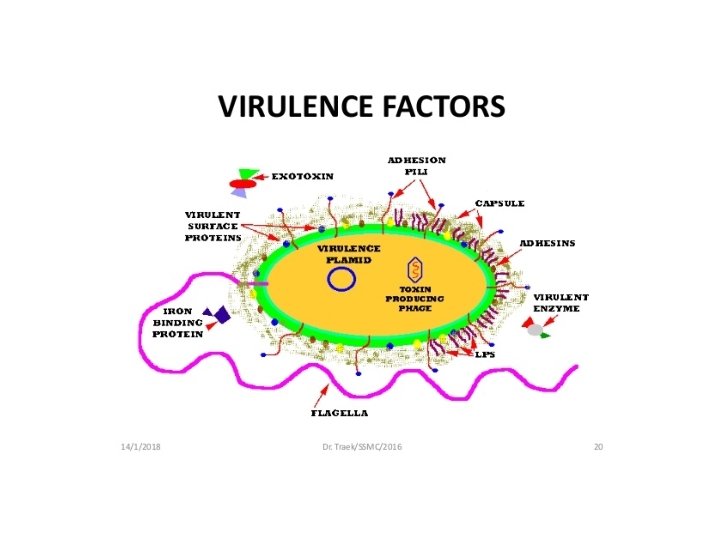

Virulence factors are molecules produced by bacteria, viruses, fungi, and protozoa that add to their effectiveness and enable them to achieve the following: colonization of a niche in the host (this includes attachment to cells) immunoevasion , evasion of the host's immune response. Toxigenesis is the ability to produce toxins. Toxic substances produced by bacteria, both soluble and cellassociated, may be transported by blood and lymph and cause cytotoxic effects at tissue sites remote from the original point of invasion or growth.

Virulence factor Cell walls cell wall is a layer located outside the cell membrane found in plants, fungi, bacteria, algae, and archaea. A peptidoglycan cell wall composed of disaccharides and amino acids gives bacteria structural support. The bacterial cell wall is either + or , bacterial cell wall often a target for antibiotic treatment Gram-positive: have a thick peptidoglycan layer and a cell membrane Gram-negative: have three layers: inner and outer membranes, and a thinner peptidoglycan layer.

Virulence factor Capsules are a fully hydrated polysaccharide layer resolvable by light microscopy. A narrower layer only detectable by indirect serological method or by electron microscopy, termed microcapsule biofilm: it protects the organism against eradication by antibiotics specially in patient on an inserted medical device.

Virulence factor Spores Highly resistant resting phase, whereby the organism can survive in a dormant state through long period of starvation or other adverse environmental conditions Fimbriae and pili Specialized thin projections that aid adhesion (attachment) to Host cells Toxic shock syndrome toxin (TSST) is a superantigen with a size of 22 k. Da produced by 5 to 25% of Staphylococcus aureus isolates. It causes toxic shock syndrome (TSS) by stimulating the release of large amounts of interleukin-1, interleukin-2 and tumour necrosis factor
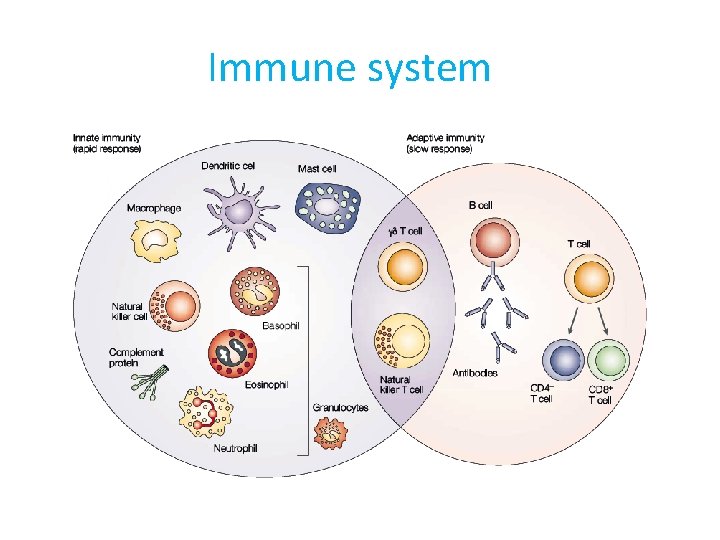
Immune system

The immune system is a complex system of structures and processes that has evolved to protect us from disease. Molecular and cellular components make up the immune system. The function of these components is divided up into nonspecific mechanisms, those which are innate to an organism, and responsive responses, which are adaptive to specific pathogens. Fundamental or classical immunology involves studying the components that make up the innate and adaptive immune system.

The immune system Innate immunity : is the first line of defense and is non-specific. That is, the responses are the same for all potential pathogens, no matter how different they may be. Innate immunity includes physical barriers (e. g. skin, saliva) and cells (e. g. macrophages, neutrophils, basophils, mast cells). These components ‘are ready to go’ and protect an organism for the first few days of infection. In some cases, this is enough to clear the pathogen, but in other instances the first defense becomes overwhelmed and a second line of defense kicks in.

The immune system Adaptive immunity : is the second line of defence which involves building up memory of encountered infections so can mount an enhanced response specific to the pathogen or foreign substance. Adaptive immunity involves antibodies, which generally target foreign pathogens roaming free in the bloodstream. Also involved are T cells, which are directed especially towards pathogens that have colonised cells and can directly kill infected cells or help control the antibody response.
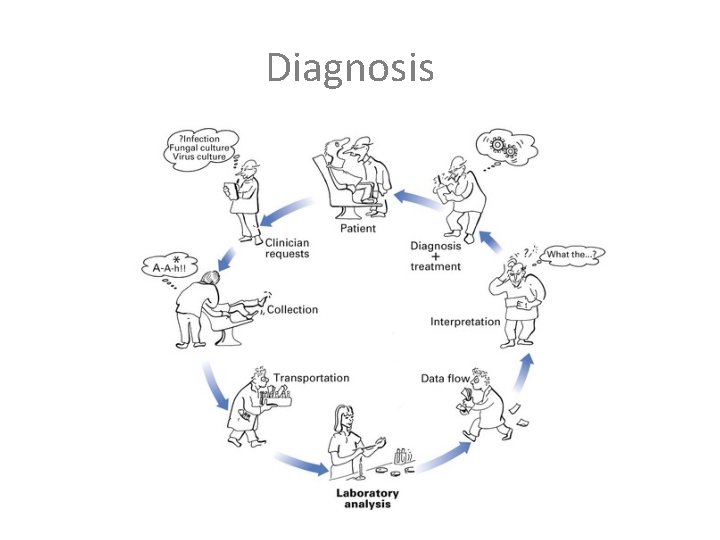
Diagnosis

Diagnosis The cycle of important events in diagnostic microbiology, depicting the interaction between the clinician and the microbiology laboratory. 1. clinical request and provision of clinical information 2. collection and transport of appropriate specimen(s) 3. laboratory analysis 4. interpretation of the microbiology report and use of the information.

REFRENCE MEDICAL MICROBIOLOGY SLIDES https: //microbiologyonline. org/about-us/glossary https: //www. immunology. org/public-information/what-is-immunology https: //www. merriam-webster. com/dictionary/symptom https: //www. cancer. gov/publications/dictionaries/cancer-terms/def/immunocompromised http: //textbookofbacteriology. net/colonization. html https: //www. medicinenet. com/script/main/art. asp? articlekey=3934 Done by : Eithar Essam Faden NO: 1707969 Section : DAR Supervisor: Nisreen Tashkandi
- Slides: 33