Medical Management of Vestibular Disorders Dr W WATAD

Medical Management of Vestibular Disorders Dr. W. WATAD 1

Introduction l Basic inputs – l Vision - ocular stability Proprioception - gait control l Vestibular system - balance l l Disorders of vestibular system are major disruptors causing spatial disorientation l Vestibular DD has remained stable over the past several decades, but the management strategies continue to 2 improve

The Goal l To review and discuss the medical management of vestibular disorders 3
Pathophysiology l Vestibular labyrinth - detects linear and angular head movements l Semicircular canals - angular l Hair cells - cupula l Otolithic organs (utricle, sacule) - linear l Hair cells - macula 4
l Vestibular nerve - superior, inferior l Afferent nerve fibers are bipolar l cell bodies lie within Scarpa’s ganglion 5
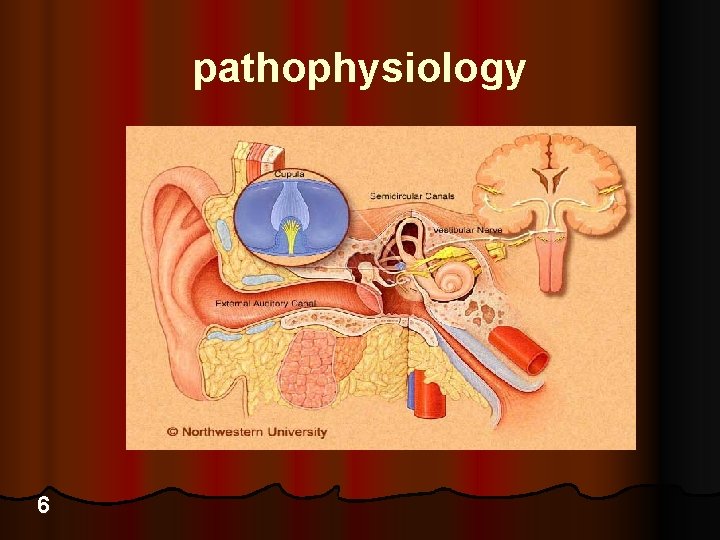
pathophysiology 6
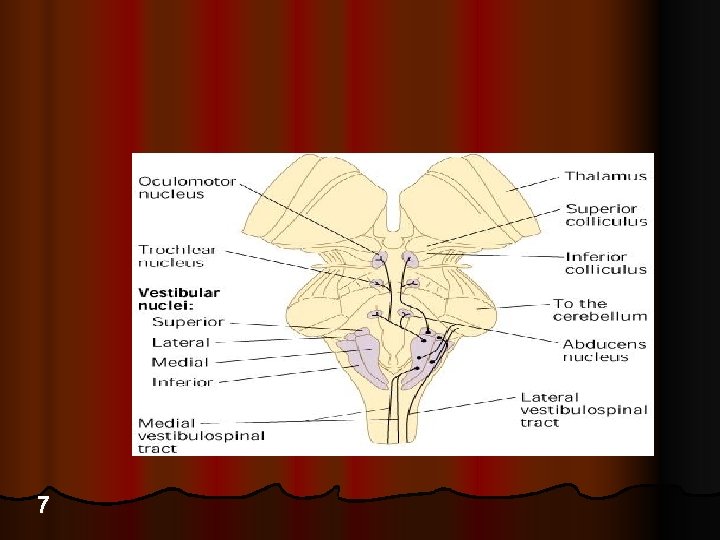
7

Pathophysiology l Balance requires – l Normal functioning vestibular system l Input from visual system (vestibulo-ocular) l Input from proprioceptive system (vestibulo- spinal) l Disruption of balance between inputs results in : l vertigo (acute) l disequilibrium (chronic) 8
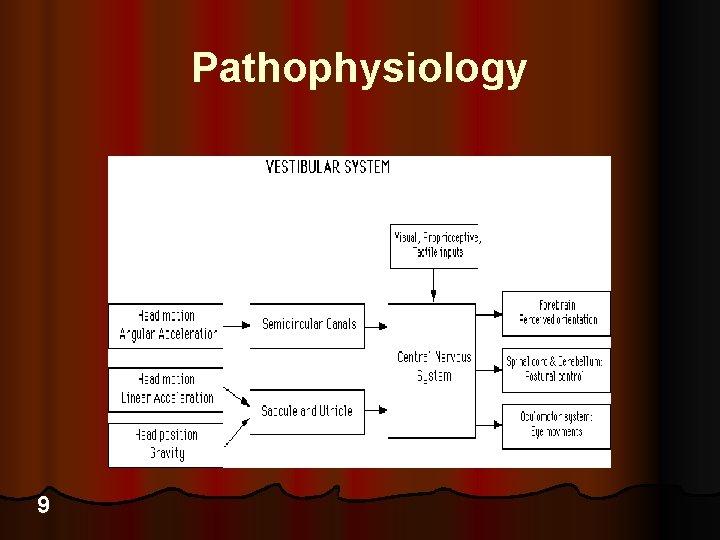
Pathophysiology 9
l Central causes of vestibular dysfunction compromise central circuits that mediate vestibular influences on posture, gaze control, and autonomic function : nausea, vomiting l Pallor l Respiratory/circulatory changes l l 10 Goal of treatment: restore balance between different inputs

Medical Treatment l Symptomatic : l Relieve acute symptoms , autonomic complaints l Specific therapy : l Targeting the underlying cause of vertigo 11

Symptomatic Pharmacotherapy l Predominant targeted vestibular neurotransmitters: Cholinergic l Histaminergic l GABA neurotransmitters - negative inhibition l l Vomiting center transmitters: Dopaminergic (D 2) l Histaminergic (H 1) l Serotonergic (5 -HT 3) l l 12 Multiple classes of drugs effective

Symptomatic Pharmacotherapy l Main classes : l Antihistaminergic - dimenhydrinate l Anticholinergics - scopolamine, meclizine l Anti-dopaminergic - droperidol l (gamma)-aminobutyric acid enhancing (GABA -ergic) agents - lorazepam, valium l Reduce the severity of vestibular symptoms 13
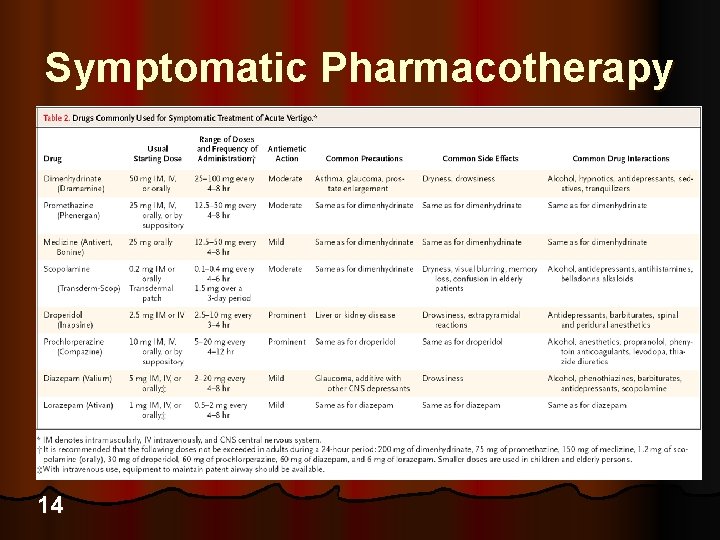
Symptomatic Pharmacotherapy 14

l Suppressant agents : l Anticholinergics l Antihistamines l Benzodiazepines l Anti-emetic drugs 15

anticholinergics l Inhibit stimulation ( exessive impulses ) from peripheral organs – vestibular n. l Inhibit transmission in LVN ( lat. Vestibular Nucleus ) l Non-specific muscarine receptor antagonist l Reversible overcompensation 16

l Agents not cross BBB are ineffective l Ineffective after symptoms have appeared l Scopalamine / atropine l SE : l Dry mouth l Urinary retention l Constipation dilated pupils sedation confusion l C/I : BPH , closed angle glaucoma 17

antihistamines l l l l 18 Uncertain mechanism Central effect ( block H 1 -R) Inhibiton synaptic transmission on MVN ( medial vestibular nucleus ) Anticholinergic and sedative effects Effective also after symptomes have appeared Cinnarazine promethazine / diphenhydramine - sedative prochlorperazine / miclizine - antiemetic

benzodiazepines l GABA modulators l Central suppression of vestibular response l Sedative , hypnotic, muscle relaxant , reduce anxiety l Clonazepam / lorazepam / alprazolam l SE : l Impaired vestibular compensation l Impaired memory l addiction 19

Anti emetics l Dopamine block activity l Not ideal for emesis from vestibular imbalance l Antihistamine effect – promethazine ( H 1 R block) l Metoclopramide – potent central antiemetic, speed gastric emptying is not effective antivertigo drug 20

l Sulpiride : l Selective dopamine (D 2) antagonist l Low incidence of extrapyramidal l Antiemetic action l Improve blood flow, mucosal secretion in GI l Antivertigo , anti-migraine headache l Antidepressant activity ( low doses ) l Antipsychotic activity ( high doses ) 21

l New antiemetic – 5 -HT 3 antagonist serotonin ( 5 hydroxytryptamine subtype 3 receptor ) antagonist l Ondensetron / granisetron l Nausea and vomiting associated with chemotherapy , post. Operation l Less effective for vestibular emesis l High cost 22

Other options l Ca channel blockers : l Vestibular suppression on Ca channel in hair cells l Flurnarazine / cinnarazine l Antihistamines and anticholinergic activity l Effective in menier’s and migrane l SE : sedation , weight gain , parkinsonism 23

l Na channel blocker : l Affect GABA NT , glutamate antagonist l Phenytoin / nerontin / tegretol l Central nystagmus l Anticonvulsants are promising agents for treatment vertigo ( uncertain mechanism ) 24

l Histamine agonist : l Betahistine – H 1/H 3 – R agonist l Increase circulation to inner ear l Suppress veastibular function l Facilitation of compensation l SE : nausea , headache l Caution ; peptic dis , pheochromocytoma 25

l Steroids l Reduce duration of vertigo episodes l Effective in meniere’s , vestibular neuritis l Sypmpathomimetics l Counterbalance sedative effect of vestibular suppressant - increase compensation l Ephedrine / amphetamine – limitted use 26
l Acetyl- leucine l Vestibular suppresant l Rapid antivertigo effect ( IV) l Ginkgo-Biloba l Vestibular suppresant l Effective in tinnitus , improve memory 27

l Selective Ach antagonist l M 2 -R antagonist l Vestibular suppressant without SE l Little reaserch 28

l Alternative medicine agents l Ambra grisea D 6 l Anamirta cocculus D 4 l Conium maculatum D 3 l Petroleum rectificatum D 8 29

30

Specific Pharmacotherapy l Vestibular Neuritis * l Meniere’s Disease * l Benign Paroxysmal Positional Vertigo * l Otosyphilis l Vertebrobasilar Insufficiency l Migraine (with vertigo) * more common 31

Vestibular Neuritis l Sudden onset of peripheral vertigo l Inflammation of vestibular nerve - presumably of viral origin l Spontaneous, complete symptomatic recovery with supportive treatment l Treatment aimed at stopping inflammation 32

Vestibular Neuritis l Ariyasu et al. (1990) l 20 patients: double-blinded, crossover l Methylprednisolone vs. placebo l 90% decrease in vertigo within 24 hours vs. 30% of placebo group l Placebo switched to steroid after 24 hours with decrease in vertigo over next 24 hours l 16 patients receiving steroid with resolution had normal ENG within one month 33

Meniere’s Disease l Hallpike and Cairns - 1938 found endolymphatic hydrops by histology l Precise etiology is unknown 34

Meniere’s Disease l Widely accepted medical treatment l Dietary salt restriction l Diuretics l Thiazide diuretics l Decrease Na absorption is distal tubule l Side effects - hypokalemia, hypotension, hyperuricemia, hyperlipoproteinemia l Combination potassium sparing agents spironolactone , thiazide + amiloride 35

Meniere’s Disease l At least 3 months of diuretic therapy recommended before discontinuing l Sulfa allergies - can try loop diuretics or alternate therapies 36

Meniere’s Disease l Carbonic anhydrase inhibitors (acetazolamide) l “inner ear glaucoma” l Decreased Na-H exchange in tubule l Decreased CSF production l Diuretic effect not as long-lasting l Side effects - nephrocalcinosis, mild metabolic acidosis, GI disturbances 37

Meniere’s Disease l Vasodilators l Based on hypothesis - pathogenesis results from ischemia of stria vascularis l Rationale - improve metabolic function l IV histamine, ISDN, cinnarizine (CA antagonist), betahistine (oral histamine analogue) l Anecdotal success l No demonstrated beneficial effects in studies 38

Meniere’s Disease l Newer theories l Multifactorial inheritance l Immune-mediated phenomena l Association of allergies l Study by Gottschlich et al. l 50% meeting criteria have antibodies to 70 -k. D heat-shock protein l 70 -k. D HSP implicated in AI-SNHL 39

Meniere’s Disease l Immunosuppressive agents gaining favor l Systemic and intra-tympanic glucocorticoids l Cyclophosphamide l Methotrexate l Shea study - intractable Meniere’s l 48 patients IT dexamethasone l 66. 7% elimination of vertigo l 35. 4% improvement in hearing (>10 d. B and/or 15% change in word recognition score) 40

Meniere’s Disease l Chemical labyrinthectomy l Disabling vertigo l After trial of adequate medical therapy l Intratympanic aminoglycoside (ITAG) l Allows treatment of unilateral disease l Gentamicin l Primarily vestibulotoxic l may impair vestibular dark cells (endolymph) l Inherent hearing loss risk - 30% 41

ITAG l Stock solution - 40 mg/m. L gentamicin l 10 to 20 mg injected over round window l Patient supine, ear up for 30 minutes l Instructed not to swallow l Bolus injections - weekly or bi-weekly l End point variable - vestibular hypofunction l Audiometry monitoring between injections l Total vestibular ablation not necessary 42

ITAG l Minor l 91% control of vertigo l 3% rate of profound SNHL (usually sudden) l 22% recurrence rate l Continuous delivery l Microwick l Round Window Microcatheter l Direct injection (labyrinthotomy) l Significant hearing loss 43 l Out of favor
BPPV Most common cause l Dysfunction of posterior SCC l Cupulolithiasis vs. Canalithiasis l 44
BPPV l Treatment approaches Liberatory maneuvers l Particle repositioning l Habituation exercises l 45
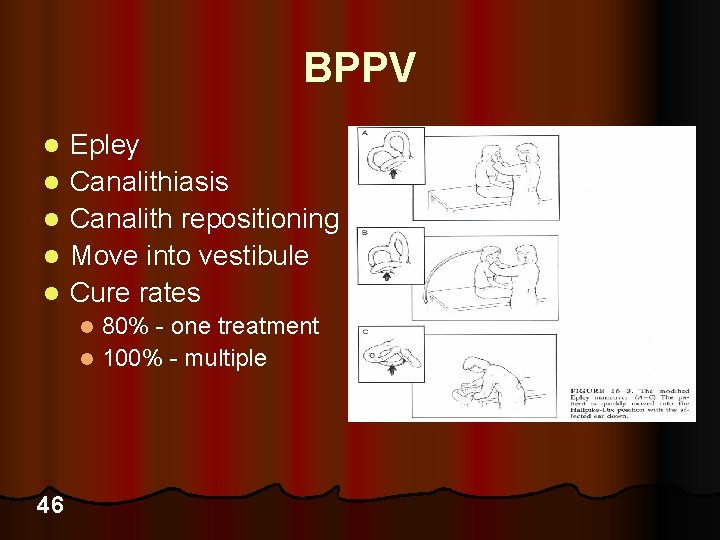
BPPV l l l Epley Canalithiasis Canalith repositioning Move into vestibule Cure rates 80% - one treatment l 100% - multiple l 46

Otosyphilis l Penicillin established treatment l IM and IV routes acceptable l IM - 2. 4 million units benzathine PCN weekly x 3 consecutive weeks is minimal treatment (some advocate up to 1 year) l IV - 10 million units PCN G q. D in divided doses x 10 days, followed by 2. 4 million units benzathine PCN x 2 weeks 47

Vertebrobasilar insufficiency l Vertigo, diplopia, dysarthria, gait ataxia and bilateral sensory & motor disturbance l Transient ischemia - low stroke risk l Antiplatelet therapy - aspirin 325 mg q. D l Ticlid l Platelet aggregate inhibitor l Risk of life-threatening neutropenia l Only in patients unable to tolerate aspirin 48

Migraine l Concomitant vertigo and disequilibrium l Headache control improves vertigo l Diagnostic criteria l Personal/family history l Motion intolerance l Vestibular symptoms - do not fit other causes l Theories - vascular origin, abnormal neural activity (brainstem), abnormal voltagegated calcium channel genes 49

Migraine l Treatment l Modifying risk factors l Exercise and diet l Avoid nicotine, caffeine, red wine and chocolate l Abortive medical therapy l Ergots l Sumatriptin l Midrin 50 l Prophylactic medical therapy l B blockers, Ca channel blockers, NSAIDs, amitryptiline, and lithium
Vestibular Rehabilitation l Promoting vestibular compensation l Habituation l Enhancing adaptation of VOR & VSR l May have initial exacerbation 51
Vestibular Rehabilitation l Cawthorne - Cooksey l Developed in 1940 s l Head movements l Balance tasks l Coordination of eyes with head l Total body movements l Eyes open & closed l Noisy environments 52
Vestibular Rehabilitation l Habituation of pathologic responses l Postural control exercises l Visual-vestibular interaction l Conditioning activities l B. I. D. , most improve after 4 -6 weeks 53

VRT - Elderly l Multifactorial causes of balance difficulty l Need 2 of 3 systems functional l vestibular, visual, proprioceptive l Good outcome measures with longer time l Impact on complications of falls 54

Conclusions l Vestibular complaints common to ENT l Thorough evaluation and understanding l Dx and treat acute symptoms l Wean vestibular suppressants l Specific pharmacotherapy instituted l Chronic, uncompensated disease benefits from early VRT 55
- Slides: 55