MEDICAL HISTORY Prof Mohammad Abduljabbar Bledsoe et al

MEDICAL HISTORY Prof. Mohammad Abduljabbar Bledsoe et al. , Essentials of Paramedic Care: Division 1 I © 2006 by Pearson Education, Inc. Upper Saddle River, NJ

Components of a Patient History Establishing rapport Chief complaint History of the present illness Past medical history Current health status – Family history – Psychosocial history Review of systems

The Interview Differential field diagnosis Helps establish a bond Bledsoe et al. , Essentials of Paramedic Care: Division 1 I © 2006 by Pearson Education, Inc. Upper Saddle River, NJ

Patient Rapport

Patient Rapport – Setting the Stage If a patient’s chart is available, review it before interviewing the patient. Use this information to gain clues about the patient.

Patient Rapport – The First Impression Present yourself as a caring, competent, and confident health care professional.

Patient Rapport – Building Trust When you introduce yourself to the patient, shaking hands or offering a comforting touch will help build trust.

Patient Rapport – Asking Questions Use a combination of open-ended and closed-ended questions.

Patient Rapport – Language and Communication Use appropriate language. Use an appropriate level of questioning, but do not appear condescending. When encountering communication barriers, try to enlist someone to help. Actively listen.

Patient Rapport – Active Listening Facilitation Reflection Clarification Empathy Confrontation Interpretation Asking about feelings

Patient Rapport – Sensitive Topics A paramedic must learn to become comfortable dealing with sensitive topics. It is important to earn a patient’s trust.

The Comprehensive Patient History

Preliminary Data Date and time Age Sex Race Birthplace Occupation

The Chief Complaint This is the pain, discomfort, dysfunction that caused the patient to request help.

The Present Illness OPQRST-ASPN Onset of the problem Provocative/ Palliative factors Quality Region/Radiation Severity Time Associated Symptoms Pertinent Negatives

Past History General state of health Childhood diseases Adult diseases Psychiatric illnesses Accidents or injuries Surgeries or hospitalizations

Current Health Status (1 of 3) Current medications Allergies Tobacco Alcohol, drugs, and related substances Diet Screening tests Immunizations

Current Health Status (2 of 3) Sleep patterns Exercise and leisure activities Environmental hazards Use of safety measures Family history Home situation and significant others Daily life

Current Health Status (3 of 3) Important exercises Religious beliefs The patient’s outlook
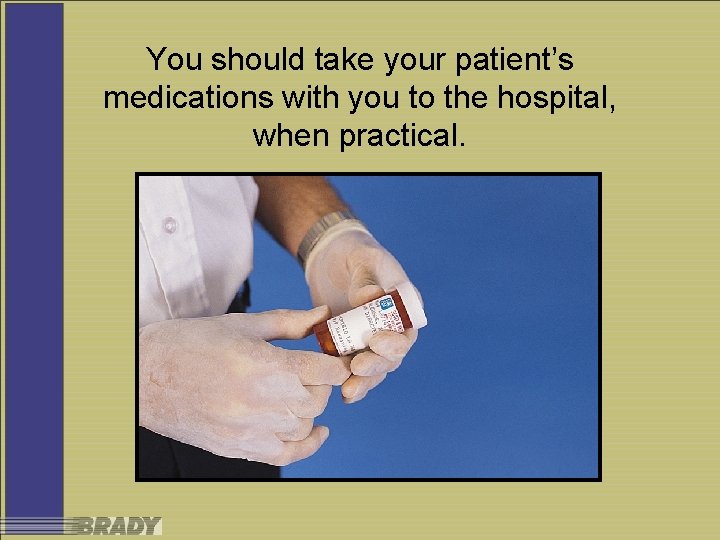
You should take your patient’s medications with you to the hospital, when practical.

Review of Systems A system-by-system series of questions designed to identify problems your patient has not already identified: Skin Head Eyes Ears Nose Mouth/Throat Respiratory Cardiovascular Gastrointestinal Genitourinary Musculoskeletal Neurologic Psychologic Endocrine Hematologic

Psychosocial History Chronic health conditions Job – Work schedule – Stress Family dynamics Support Safety issues – Car seat usage – Smoke and CO alarms
Special Challenges (1 of 2) Silence Overly talkative patients Multiple symptoms Anxiety Depression Sexually attractive or seductive patients Confusing behaviors or symptoms

Special Challenges (2 of 2) Patients needing reassurance Anger and hostility Intoxication Crying Limited intelligence Language barriers Hearing problems Blindness Talking with families or friends

If the patient cannot provide useful information, gather it from family or bystanders.

Summary History-Taking Techniques Active Listening The Comprehensive Health History
- Slides: 26