MEDICAL GRANDROUNDS JYN A CABAL M D March

MEDICAL GRANDROUNDS JYN A. CABAL M. D. March 15, 2007

OBJECTIVES: • To present a case of invasive ductal carcinoma • To give new updates regarding breast cancer diagnosis and management

General Data • • • L. H. 54 year-old Female Single Nulliparous

First Cycle of Chemotherapy

History of Present Illness 8 weeks PTA (+) mass on right outer upper quadrant R breast on routine x-ray mammography Consult done, on P. E. : (+) 6. 5 cm mass on right outer upper & lower quadrant in largest diameter, no skin lesions, dimpling, nipple discharge or inversion
6 weeks PTA 4 weeks PTA MR mammography breast core needle biopsy: Invasive Ductal Ca Grade III R modified radical mastectomy

MR MAMMOGRAPHY Scanty fibroglandular tissue, both breasts 2. 4 x 3. 6 x 3. 7 cm enhancing lobulated mass on upper outer quadrant of R breast, highly suspicious of malignancy 0. 6 cm x 0. 6 cm enhancing nodule in 6 o’ clock position of L breast

CORE NEEDLE BIOPSY • INVASIVE DUCTAL CA, GRADE III • IMMUNOHISTOCHEMISTRY (IHC) ER 1+, PR 2+, HER-2/neu 3+

Histopathology Invasive Ductal Ca Nuclear Grade III Histologic Grade III 3. 9 cm in widest diameter Axillary LN Negative (19 LN)

Histopathology - Stanford • Estrogen receptor 3+, 95% • Progesterone Receptor 3+, 30% • HER-2/neu (-) for FISH (Fluorescence In Situ Hybridization)
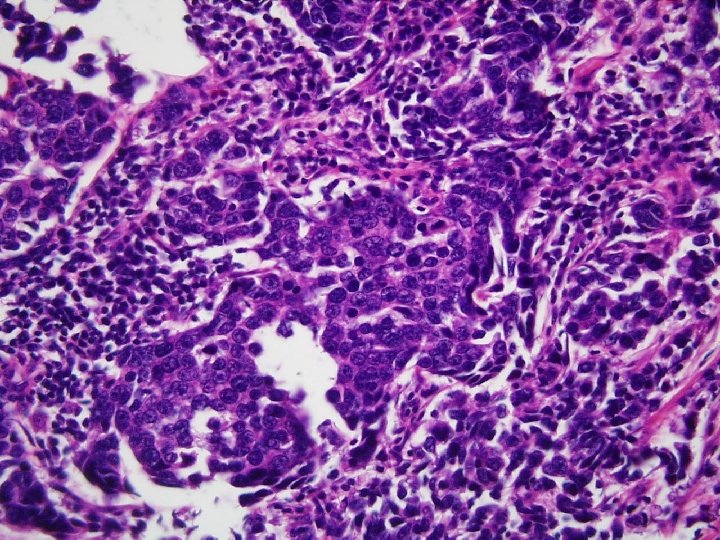
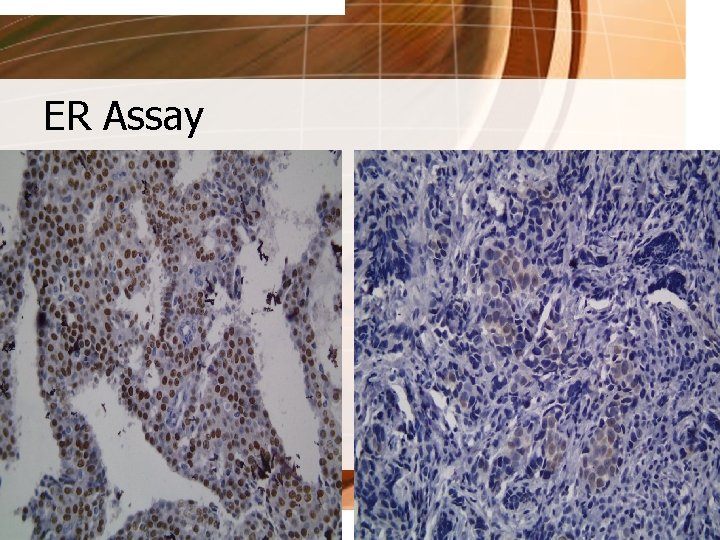
ER Assay
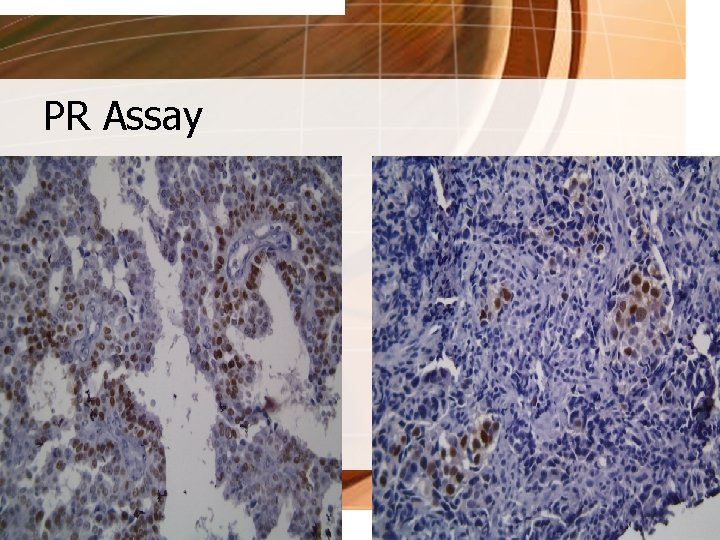
PR Assay
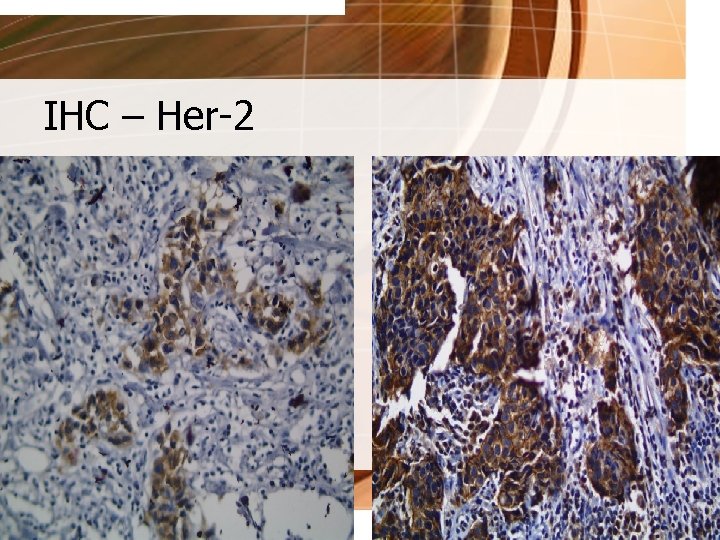
IHC – Her-2

DIAGNOSTICS • CT Scan of whole abdomen – fatty infiltrating changes in the liver • Bone Scan – no evidence of metastatic disease to the bone

DIAGNOSTICS • CBC Hgb – 12. 8 Hct – 37 WBC – 5300 Segmenters - 53 Lymphocytes - 35 PC – 297 T

Past Medical History • (+) Hypertension for 4 years on Irbesartan 150 mg OD • 1993 -- (+) L ovarian cyst excision borderline serous papillary tumor -- (+) TAH-BSO given Premarin as hormone replacement therapy x 2 years

Personal/Social History • • Single Nulliparous Non-smoker Non-alcoholic beverage drinker

Menstrual History • Menarche at age 17 • Surgical menopause at age 41

Family History • • • (+) Colon Cancer, RCC – mother, 90 y/o (+) Gastric Cancer – father, deceased (-) Breast Cancer (+) HPN – maternal side (-) Diabetes Mellitus (-) Asthma

Review Of Systems (-) weight loss (-) anorexia (-) headache (-) fever (-) dyspnea (-) cough (-) chest pain (-) palpitations (-) orthopnea (-) dysphagia (-) constipation (-) diarrhea (-) dysuria

Physical Examination • General awake, conscious, coherent, not in cardiopulmonary distress • BP- 120/70 HR- 70 RR- 36. 2 T- 36. 5 • Wt- 68 kilos Ht- 167 cms. BSA- 1. 77 • BMI- 24. 4 (overweight)

Neck trachea midline, freely movable, thyroid not palpable; no lymphadenopathy Breast (+) 15 cm incisional scar on R ant chest wall, no lymphadenopathy, no skin lesions; L breast: no mass, skin dimpling, nipple discharge Chest and Lungs symmetric chest expansion, tactile fremitus symmetric, resonant percussion throughout, no crackles, no wheezes

Heart Apex beat and PMI at 5 th intercostal space, LMCL; S 1 heard best at apex, S 2 heard best at base, no murmurs; regular rhythm Abdomen full, soft, nontender; liver, spleen, and kidney not palpable

Lymphatic no palpable lymph nodes in neck, supraclavicular, axillary, epitrochlear, or inguinal areas Musculoskeletal muscles appear symmetric with appropriate and equal strength bilaterally, full range of active and passive motion

Salient Features • • • 54 year old Female Single Nulliparous History of HRT use History of family cancer

Admitting Impression

Doxorubicin (Adriamycin) 60 mg/m IV Cyclophosphamide 600 mg/m IV

INVASIVE DUCTAL CARCINOMA

RISK FACTORS • Age • Current or prior hormone replacement therapy • Ethnicity/race • Family history of breast cancer • Early menarche • Late menopause • Older age at first live childbirth • Atypical Hyperplasia/LCIS • Genetic mutations such as BRCA ½ genes • Prior thoracic RT • BMI • Alcohol consumption

Risk Factor – HRT Use • Women 50 -64 years of age showed an association between current use of estrogen-only HRT and increased risk of breast cancer (Beral V. Lancet. 2003; 362: 419 -427) • Nurses’ Health Study demonstrated a significantly increased breast cancer risk after long term use (20 years or longer) of estrogen alone (Chen WY, Manson JE, Hankinson SE, et al. Arch Intern Med. 2006; 166: 1027 -1032)

Breast Cancer Work Up History and P. E. Breast Imaging: Mammogram Breast ultrasound Magnetic Resonance Imaging

Breast Cancer Work Up Breast Biopsy Tumor tests: Estrogen receptors Progesterone receptors HER-2/neu/cerb-b 2 Other tests: CBC, platelet count, CXR, liver function tests, CT Scan, PET Scan

MRI in Patients with Breast Cancer: Current Applications • Detects cancer that is occult on conventional imaging such as mammography and sonography • In preoperative evaluation, it can detect multifocal and multicentric disease that was previously unsuspected which facilitates accurate staging

• For patients who have undergone lumpectomy, it can be helpful in assessment of residual tumor load • Can be helpful to diagnose recurrence when conventional imaging and P. E. are nonconfirmatory

• Can assess response to neoadjuvant chemotherapy for locally advanced breast ca
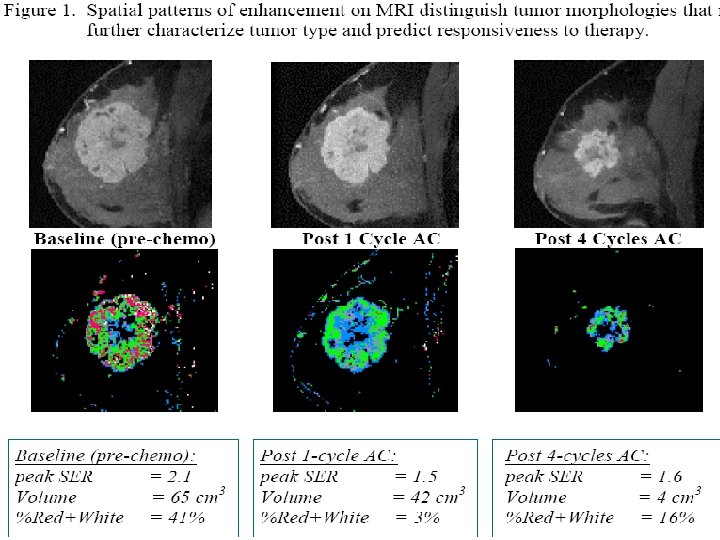
• Patient selection for preoperative breast MRI: • Young patient • Patient with dense or moderately dense breasts • Patients with difficult tumor histologic findings such as infiltrating lobular carcinoma and tumors with extensive intraductal component in which tumor size assessment is difficult

Tumor Tests • ESTROGEN and PROGESTERONE RECEPTORS - are parts of cells that attach to hormones estrogen and progesterone; serve as “welcome mats” - Hormone Receptor Assay: ER (+) and PR (+) – response rate of 70% ER (+) and PR (-) – response rate of 30% ER (-) and PR (-) – response rate of 10% - tumors that lack either or both of these receptors are more likely to recur than tumors that have them

Tumor Tests • HER-2/neu/cerb-B 2 oncogene - codes for a surface membrane receptor that interacts with an unidentified growth factor and is frequently amplified in human breast carcinoma - mapped to chromosome 17
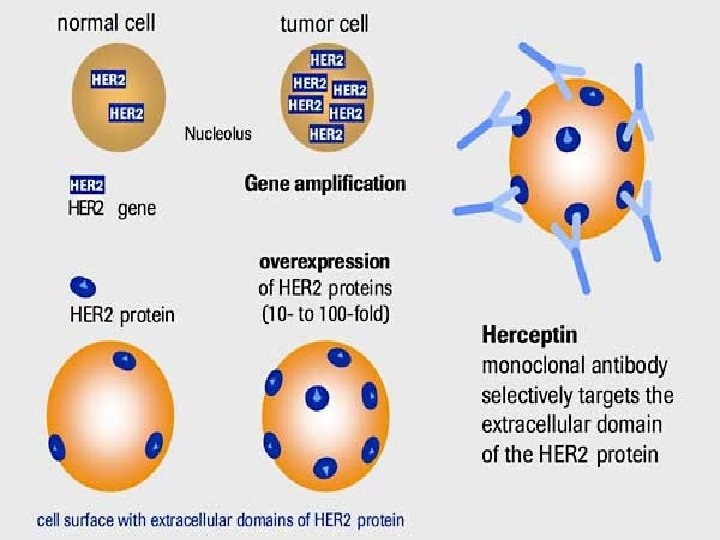

TESTS for HER-2/neu • IMMUNOHISTOCHEMISTRY - test that detects HER-2/neu protein on the surface of the cell by staining the cell with antibodies - can be 0, 1+ (negative), 2+ (borderline), 3+ (positive) - if IHC 2+, have the tissue tested with FISH test

Tests for HER-2/neu • FLOURESCENCE IN SITU HYBRIDIZATION (FISH) - gold standard for confirmatory testing - measures HER-2 gene abnormality - “paints” the HER-2 genes inside the cell so they may be accurately counted - may be (+) or (-) ** All in all, IHC has been shown to miss 15 -20% of positive specimens compared with less than 5% with FISH

• Only tests IHC 3+ or FISH (+) respond well to therapy that work against HER-2


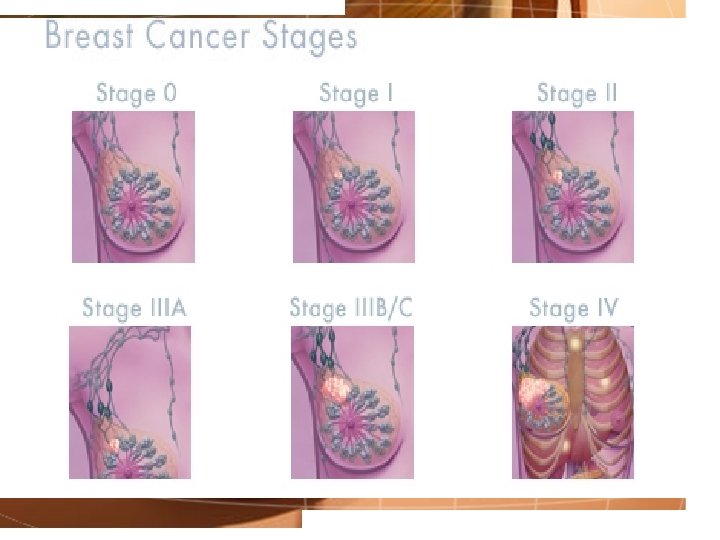

Risk Categories for Node Negative Breast Cancer (Alberta Breast Cancer Program 2006) Risk Category Risk Factors Low - < 1 cm, no negative risk factors - 1 - 2 cm, grade 1, no negative risk factors High - 1 - 2 cm with any 2 or more negative risk factors, - 2 - 3 cm with any one negative risk factor, - any > 3 cm (regardless of other risk factors) Intermediate all other combinations of factors that do not fit into either the low or high risk criteria above NEGATIVE RISK FACTORS - histologic grade 3 - estrogen receptor negative - cerb. B 2 overexpression - presence of lymph/vascular invasion - age < 35 years

Surgical Procedures of Breast Ca • Lumpectomy/Breast Conservation Therapy • Simple Mastectomy • Modified Radical Mastectomy • Radical Mastectomy
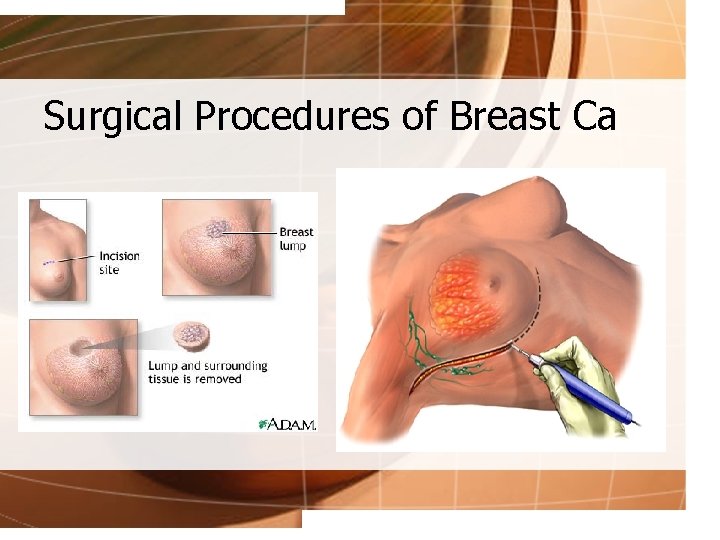
Surgical Procedures of Breast Ca

Lumpectomy vs Mastectomy • Mastectomy with axillary LN dissection or breast-conserving therapy with lumpectomy, axillary dissection, & whole breast irradiation are medically equivalent primary treatment options in the majority of women with Stage I and Stage II breast cancers. (Fisher B, et al. . N Engl J Med October 17, 2002; 347: 1233 -41. )

• Survival outcomes for young women with breast cancer receiving either breastconserving therapy or mastectomy are similar (Kroman N, Holtveg H, Wohlhart J, et al. Effect of breast conserving therapy vs redical mastectomy on prognosis for young women with breast ca. Cancer 2004; 100: 688 -693)

Lumpectomy or breast conservation therapy is usually not recommended for: • women who have already had radiation therapy to the affected breast • women with 2 or more areas of cancer in the same breast that are too far apart to be removed through 1 surgical incision, while keeping the appearance of the breast satisfactory • women whose initial lumpectomy along with (one or more) re-excision has not completely removed the cancer

• women with certain serious connective tissue diseases such as scleroderma, which make them especially sensitive to the side effects of radiation therapy • pregnant women who would require radiation while still pregnant (risking harm to the fetus) • women with a tumor larger than 5 cm (2 inches) that doesn't shrink very much with neoadjuvant chemotherapy • women with a cancer that is large relative to her breast size

Neodjuvant Therapy • Chemotherapy given before surgery • Can shrink large cancers so that they are small enough to be removed by lumpectomy instead of mastectomy • Not indicated unless invasive breast cancer is confirmed

• Indication: Ø women with large clinical stage IIA, stage IIB, and T 3 N 1 M 0 tumors who meet the criteria for breast conserving therapy except for tumor size and who wish to undergo breast conservation therapy

• Several randomized trials have assessed the value of neodjuvant chemotherapy in postmenopausal women with estrogen receptor positive breast cancer. • Neodjuvant therapy with an aromatase inhibitor is an option in the treatment of postmenopausal women with hormone receptor-positive disease

• The use of either Anastrozole or Letrozole provides superior rates of breast conserving surgery and usually objective response. (Smith IE. Dowsett M, Ebbs SR, et al. J Clin Oncol. 2005; 23: 5108 -5116)

Adjuvant Therapy • A form of therapy added to the primary treatment to keep cancer from returning Ø Radiation Ø Chemotherapy Ø Hormone Therapy Ø Biologic Therapy

Hormonal Therapy • Indication: Ø Patients with invasive breast cancers that are estrogen and progesterone receptor positive ØException: LN (-) cancer < 0. 5 cm or 0. 6 cm to 1 cm with favorable prognostic factors

TAMOXIFEN – selective estrogen receptor modulator - 1986: received FDA approval as adjuvant therapy in node-positive postmenopausal women with breast cancer - 1990: tamoxifen was approved for women of any age with node-negative disease, as long as hormone receptors were positive or unknown

AROMATASE INHIBITOR (AI) - suppresses estrogen production indirectly via inhibition of the aromatase enzyme ØAnastrozole ØLetrozole

• Switching to Anastrozole after the first 2 to 3 years of Tamoxifen is well tolerated and significantly improves event-free and recurrence-free survival in postmenopausal patients with early breast cancer J Clin Oncol. 2005 Aug 1; 23(22): 5138 -47.

• Risk of breast cancer recurrence was lower in women in the letrozole arm relative to the tamoxifen arm. (Thurlimann B, et al. N Engl J Med. 2005; 353: 2747 -2757. )

Chemotherapy • Recommended based on: Ø tumor size (> 1 cm) Ø tumor grade Ø presence or absence of LN involvement Ø tumor hormone receptor status

• NCCN Recommendation < 70 y/o Ø AC x 4 (doxorubicin/cyclophosphamide) + sequential paclitaxel x 4, every 2 weekly regimen Ø Doxorubicin, followed by CMF Ø Cyclophosphamide/epirubicin, and fluorouracil with or without docetaxel
![Ø Cyclophosphamide, methotrexate and fluorouracil [CMF] ØDoxorubicin and cyclophosphamide [AC] ØDoxorubicin and cyclophosphamide followed Ø Cyclophosphamide, methotrexate and fluorouracil [CMF] ØDoxorubicin and cyclophosphamide [AC] ØDoxorubicin and cyclophosphamide followed](http://slidetodoc.com/presentation_image_h2/89a345982542760e50d83bdee6d98dcb/image-68.jpg)
Ø Cyclophosphamide, methotrexate and fluorouracil [CMF] ØDoxorubicin and cyclophosphamide [AC] ØDoxorubicin and cyclophosphamide followed by paclitaxel or docetaxel [AC ->T] or docetaxel concurrent with AC [TAC]

Ø Cyclophosphamide/Docetaxel (TC) Ø Gemcitabine/paclitaxel (GT) Ø Epirubicin/cyclophosphamide (EC) Ø Cyclophosphamide, doxorubicin, and fluorouracil [CAF]

Biologic Therapy • TRASTUZUMAB (Herceptin) - is a monoclonal antibody with specificity for the extracellular domain of HER-2/neu receptor, preventing breast cancer cells to grow - can shrink some breast cancer metastases that return after chemotherapy or continue to grow during chemotherapy

• Adverse Ø Ø Ø Ø Effects: Fever and chills Weakness Nausea/Vomiting Cough Diarrhea Headache Heart problems

• HERA Trial The use of trastuzumab resulted in a 46% reduction in the risk of recurrence in patients following all local therapy & a variety of standard chemotherapy regimens. ( Piccart-Gebhart MJ Procter M, Leyland-Jones B, et al. N Engl J Med. 2005; 353: 1659 -1672)

• There is a 52 % reduction in risk of recurrence and a 33% reduction in the risk of death in patients with HER-2 (+), node (+) breast cancer & node (-) with primary tumors >1 cm if ER/PR (-) or >2 cm if ER/PR (+). (Joint Analysis of NSABP B-31 & NCCTG N 9831 Trial, 2005)

Key Points • The accuracy of HER-2 assays used in clinical practice is a major concern since this could affect patient’s treatment. • Breast MRI is an adjunct to other breast imaging and should not be used in lieu of standard breast imaging.

THANK YOU !
- Slides: 75