MEDICAL GRANDROUNDS July 3 2008 Abigail CruzZaraspe M

MEDICAL GRANDROUNDS July 3, 2008 Abigail Cruz-Zaraspe M. D.

OBJECTIVES o o o To present a case of bacteremia in aplastic anemia To discuss salmonella nontyphi bacteremia and myositis manifestations, diagnosis and treatment To discuss briefly the treatment of aplastic anemia



IDENTIFYING DATA o o A. R. 42/M Married Real-estate broker

CHIEF COMPLAINT o Right thigh pain
HISTORY OF PRESENT ILLNESS o 5 weeks PTA o 4 weeks PTA Easy fatigability, SOB, (+) melena, (+) abdominal pain, (+)palpitations sought consult, CBC Pancytopenia admitted for the first time for transfusion

HISTORY OF PRESENT ILLNESS o First admission blood transfusions BMA-hypocellular BM Dx: Aplastic anemia treatment options were discussed (discharged-platelet ct 44 k)

HISTORY OF PRESENT ILLNESS o 3 weeks PTA intermittent fever (390 C), body malaise, nose bleeding Consult: WBC 1860, PLT 10 k Tx: Co-amoxyclav 625 mg TID x 7 d, tranexamic acid 500 mg TID GCSF 300 mcg
HISTORY OF PRESENT ILLNESS o 3 weeks PTA o 2 nd admission generalized petechial rashes & gum bleeding and was admitted CBC- pancytopenia Tx: blood & PC transfusions
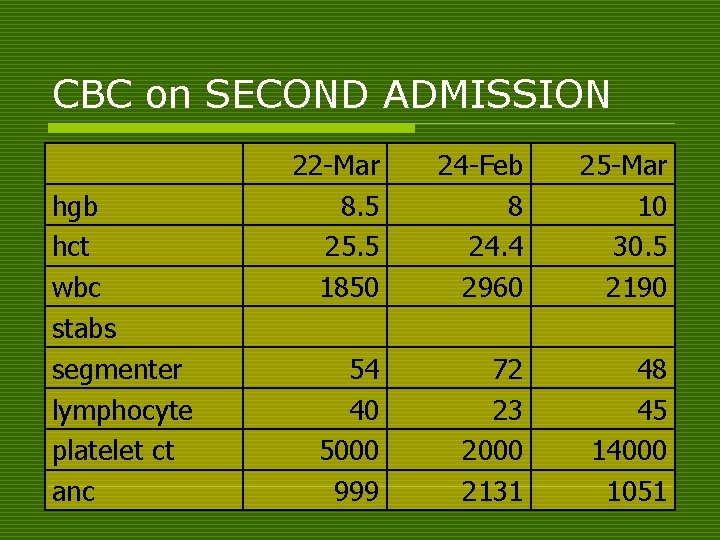
CBC on SECOND ADMISSION hgb hct wbc stabs segmenter lymphocyte platelet ct anc 22 -Mar 8. 5 25. 5 1850 24 -Feb 8 24. 4 2960 25 -Mar 10 30. 5 2190 54 40 5000 999 72 23 2000 2131 48 45 14000 1051

HISTORY OF PRESENT ILLNESS o 2 nd admission Initially given Cefepime 1 gm Q 12

HISTORY OF PRESENT ILLNESS o 2 nd admission + right thigh & hip pain 5/10 (dull, aching constant) +direct tenderness no swelling no limitation in ROM no paresthesia
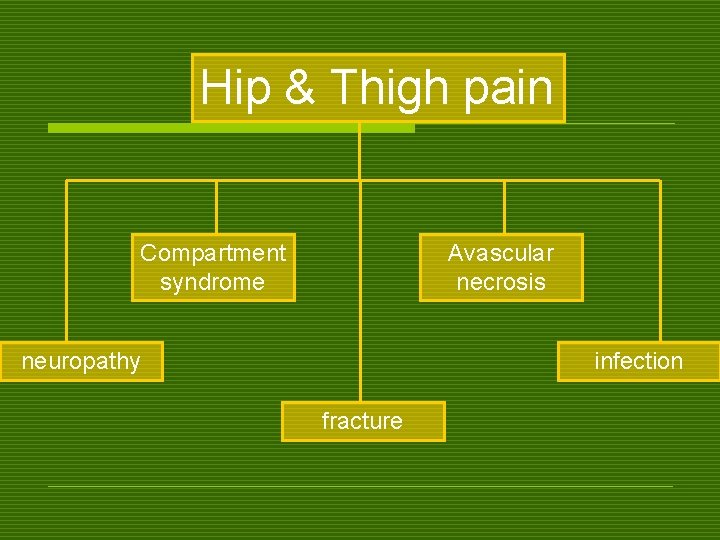
Hip & Thigh pain Compartment syndrome Avascular necrosis neuropathy infection fracture
NEUROPATHY o o Severe intractable pain Unusual burning, tingling or shocklike quality Triggered by light touch Sensory deficit on area of pain
Hip & Thigh pain Compartment syndrome Avascular necrosis neuropathy infection fracture

COMPARTMENT SYNDROME o o o Pain Parasthesia Pulselessness Pallor pressure
Hip & Thigh pain Compartment syndrome Avascular necrosis neuropathy infection fracture

HISTORY OF PRESENT ILLNESS o 2 nd admission Pelvis and Right hip xray: no pathologic finding
Hip & Thigh pain Compartment syndrome Avascular necrosis neuropathy infection fracture

HISTORY OF PRESENT ILLNESS o 2 nd admission Blood CS: Salmonella enteritidis Grp C Sensitive: Ceftriaxone Chloramphenicol Ciprofloxacin shifted to Ciprofloxacin 500 mg/tab, 1 tab BID
HISTORY OF PRESENT ILLNESS o 2 nd admission Dx: Aplastic anemia Salmonella nontyphi bacteremia Advised treatment w/ Anti-thymocyte globulin / cyclosporine

HISTORY OF PRESENT ILLNESS o 2 nd admission THM: Ciprofloxacin 500 mg/tab, 1 tab BID to complete 7 days Prednisone 30 mg BID, Tranexamic acid & Omeprazole

HISTORY OF PRESENT ILLNESS o Since discharge episodes of fever & progression R hip & thigh pain on movement & palpation unable to stand admitted 3 rd time

REVIEW OF SYSTEMS o o o o (-) headache (-) loss of consciousness (-) cough or colds (-) weight loss (-) chest pain (-) dyspnea (-) palpitations (-) abdominal pain o o o (-) nausea or vomiting (-) LBM/ constipation (+) melena (-) hematochezia (-) dysuria (-) hematuria

PAST MEDICAL HISTORY o o o Non-hypertensive Non-diabetic No known allergies

FAMILY HISTORY o o o No No No hypertension diabetes asthma blood dyscrasias cancer

PERSONAL AND SOCIAL HISTORY o o o Previous smoker, stopped in late ‘ 90 s Occasional beer drinker Lived near an electroplating factory Previously worked as a cashier in a gasoline station Real estate broker

PHYSICAL EXAMINATION o o o General: conscious, coherent, bed-bound Vital signs: BP 130/80, HR = 103 bpm, reg, RR = 22/min, T = 390 C HEENT: Pale conjunctivae, icteric sclerae, no tonsillopharyngeal congestion, no cervical lymphadenopathy

PHYSICAL EXAMINATION o Chest/Lungs: Symmetrical chest expansion, no retractions, clear breath sounds Adynamic precordium, tachycardic with regular rhythm, no murmurs

PHYSICAL EXAMINATION o Abdomen: Flabby, normoactive bowel sounds, soft, non-tender, no hepatomegaly no splenomegaly

PHYSICAL EXAMINATION o Extremities: (+) erythema and hyperemia, right thigh extending to mid-leg area No discharge, no open wounds no sensory deficit Left leg was grossly normal pulses: full and equal

SALIENT FEATURES o o o o 42/M Known case of aplastic anemia Known case of non-typhi salmonella bacteremia Treated with ciprofloxacin 500 mg BID x 1 week Still febrile Right thigh and hip pain Erythema and swelling of right lower extremity
Hip & Thigh pain Compartment syndrome Avascular necrosis neuropathy infection fracture
AVASCULAR NECROSIS o o o results from infarction of bone trabeculae and marrow cells equal frequency in the femoral and humeral heads The femoral heads more commonly undergo progressive joint destruction as a result of chronic weight bearing. The changes are best detected by MRI

AVASCULAR NECROSIS o o Most studies have found that the risk is low (< 3 percent) in patients treated with doses of prednisone less than 15 to 20 mg/day In one series, the prednisone dose in the highest month of therapy exceeded 40 mg/day in 93 percent, and 20 mg/day in 100 percent of patients with osteonecrosis.
Hip & Thigh pain Compartment syndrome Avascular necrosis neuropathy infection fracture

o 150 patients with aplastic anemia treated at Clinical Hematology Branch of the National Heart, Lung and Blood Institute (NHLBI) between 1978 and 1990 n Infection was documented in 47% of cases o respiratory tract (32 percent) o soft tissues (24 percent) o blood (22 percent) o gastrointestinal tract (17 percent) o urinary tract (6 percent).

IMPRESSION o Aplastic anemia Salmonella non-typhi bacteremia with secondary myositis o r/o Avascular necrosis, osteomyelitis o

COURSE IN THE WARDS o On admission n CBC, PTT, UA, CXR, crea, BUN, K, Na were requested. He was placed on a neutropenic diet. n He was started on Piperacillintazobactam 4. 5 mg/IV x 1 dose then 2. 25 mg q 8 hours
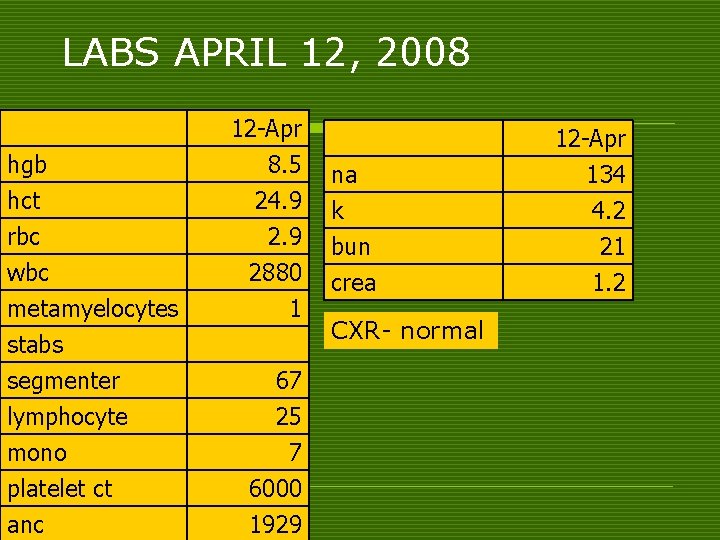
LABS APRIL 12, 2008 hgb hct rbc 12 -Apr 8. 5 24. 9 2. 9 wbc metamyelocytes stabs segmenter lymphocyte mono platelet ct 2880 1 anc 1929 67 25 7 6000 na k bun 12 -Apr 134 4. 2 21 crea 1. 2 CXR- normal
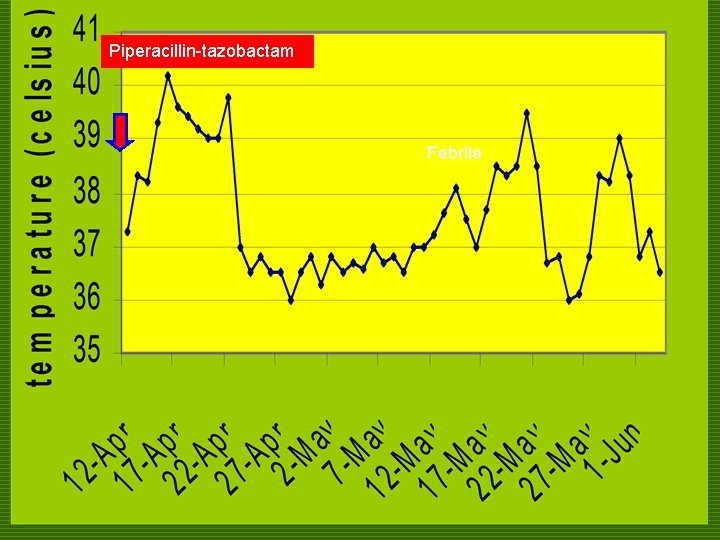
Piperacillin-tazobactam Febrile

COURSE IN THE WARDS o 2 nd hospital day n + severe leg pain, unrelieved by Tramadol. n referred to Orthopedic service o Impression: t/c pathologic fracture vs. avascular necrosis, R hip; aplastic anemia. o Tx: Ketorolac and Morphine.

COURSE IN THE WARDS o 2 nd hospital day o Pelvic MRI was requested n Myositis with fasciitis involving the right gluteal and right thigh muscle and the right obturator internus muscle. n Avascular necrosis of the right femoral head considered

COURSE IN THE WARDS o 2 nd hospital day n still with fever and leg pain o Blood CS: n Salmonella Enteritidis Group C n sensitive to Ceftriaxone and Ciprofloxacin n resistant to Co-trimoxazole and Ampicillin.

COURSE IN THE WARDS o 5 th HD n referred to Infectious Disease service. o o Impression: Salmonella nontyphi bacteremia with secondary myositis. Tx: shift Piperacillin-tazobactam to Ciprofloxacin 500 mg/tab 2 x a day & ceftriaxone 2 g/IV OD
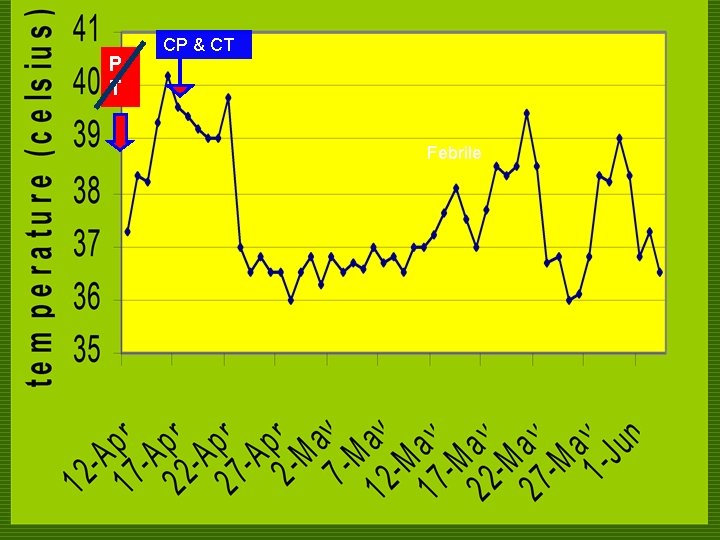
P T CP & CT Febrile

COURSE IN THE WARDS o 11 th HD n patient was still febrile (Tmax 400 C) o n n n endovascular Salmonella was considered Ceftriaxone was discontinued Piperacilin-Tazobactam was resumed & increased to 4. 5 IV Q 8 dexamethasone 4 mg/tab 12 hrs
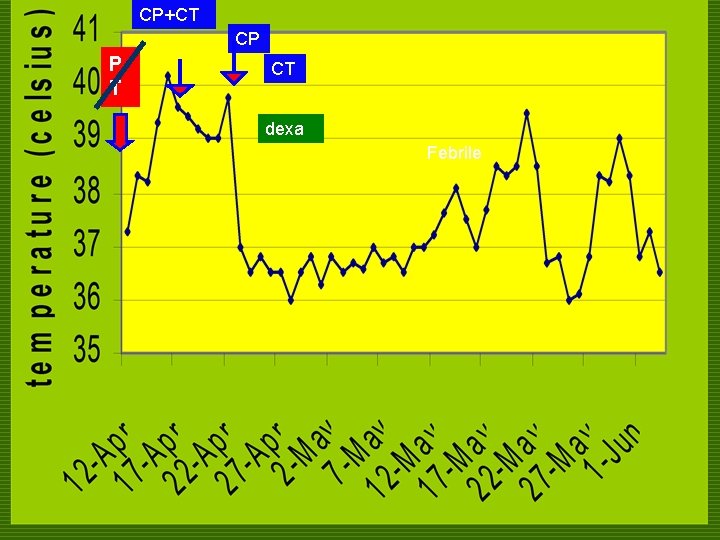
CP+CT CP P T CT dexa Febrile

COURSE IN THE WARDS o 13 th HD n Afebrile n pain decreased n Dexamethasone was tapered to 4 mg/tab bid.

COURSE IN THE WARDS o 18 th HD n Cyclosporine (Neoral)100 mg/cap BID n ATG 1000 mg in PNSS x 4 hrs, once daily until D 11 ( 5/9/08)
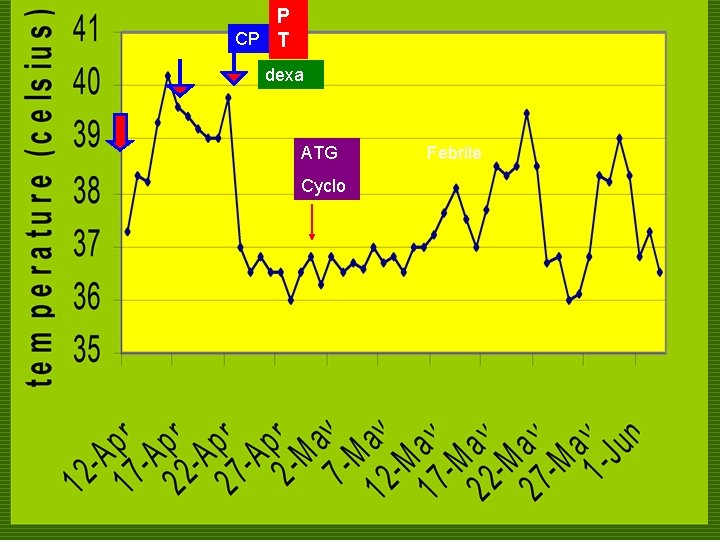
P CP T dexa ATG Cyclo Febrile

COURSE IN THE WARDS o 21 st HD n patient was afebrile, Piperacillin -tazobactam was discontinued
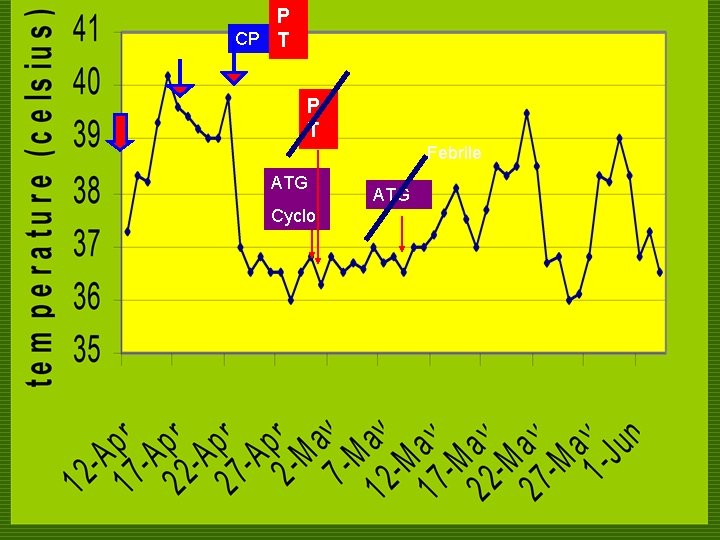
P CP T Febrile ATG Cyclo ATG

COURSE IN THE WARDS o 38 th HD n n fever recurred Increased severity of R thigh pain Blood CS: negative after 5 days CBC still showed pancytopenia.
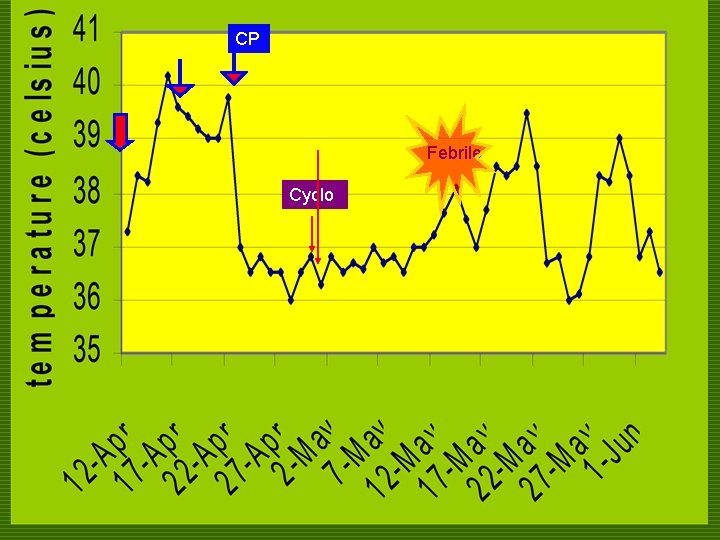
CP Febrile Cyclo

COURSE IN THE WARDS o 41 st HD n persistence of fever n CXR, urinalysis, CBC were requested o CXR & urinalysis were normal o CBC still showed pancytopenia. n Piperacillin-tazobactam 4. 5 g/IV q 8 was resumed
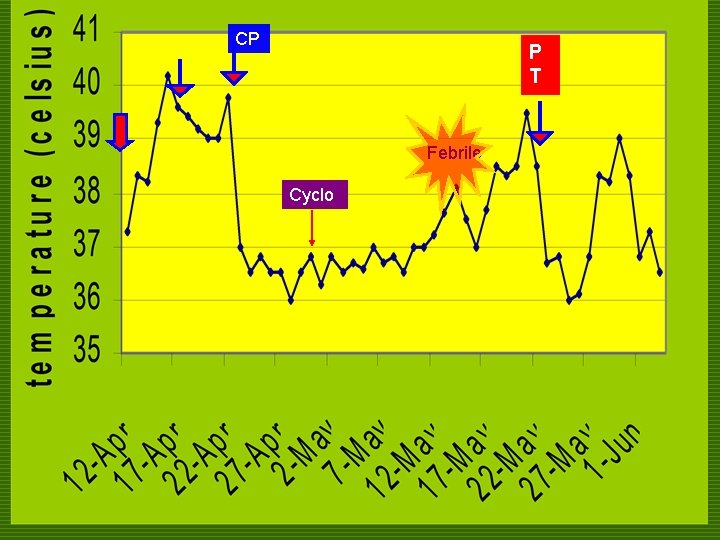
CP P T Febrile Cyclo

COURSE IN THE WARDS o 46 th HD n BMA: beginning bone marrow recovery. Some section shows good cellularity with myeloid and erythroid precursors, although megakaryocytes are still decreased but present
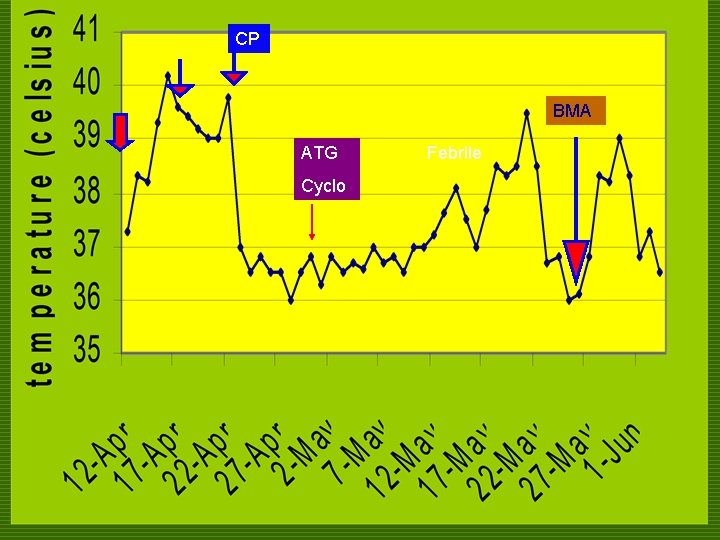
CP BMA ATG Cyclo Febrile
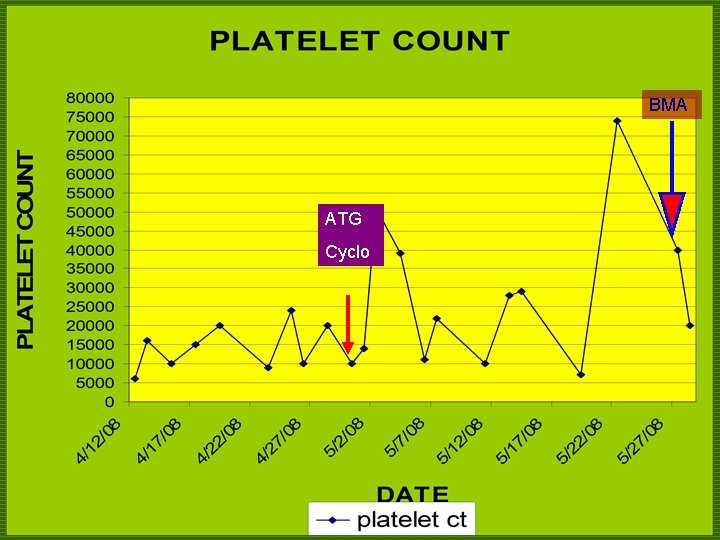
BMA ATG Cyclo
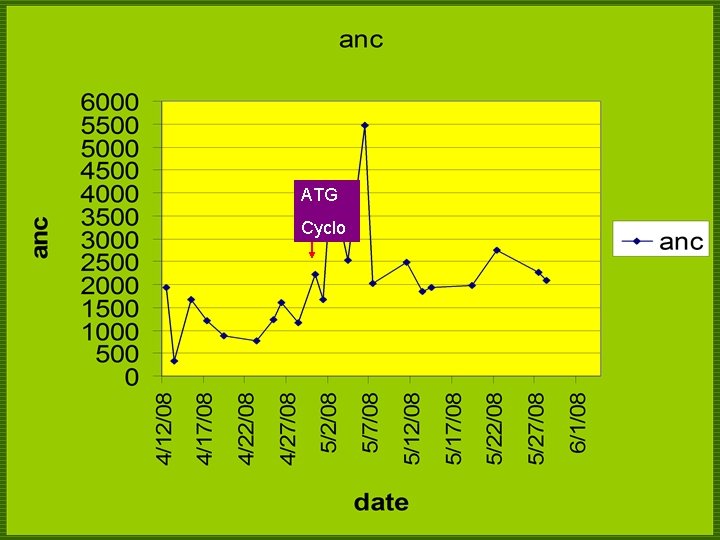
ATG Cyclo

COURSE IN THE WARDS o 47 th HD n again had febrile episodes n Blood culture: negative n MRI of R leg: myositis, fasciitis & avascular necrosis of the R thigh
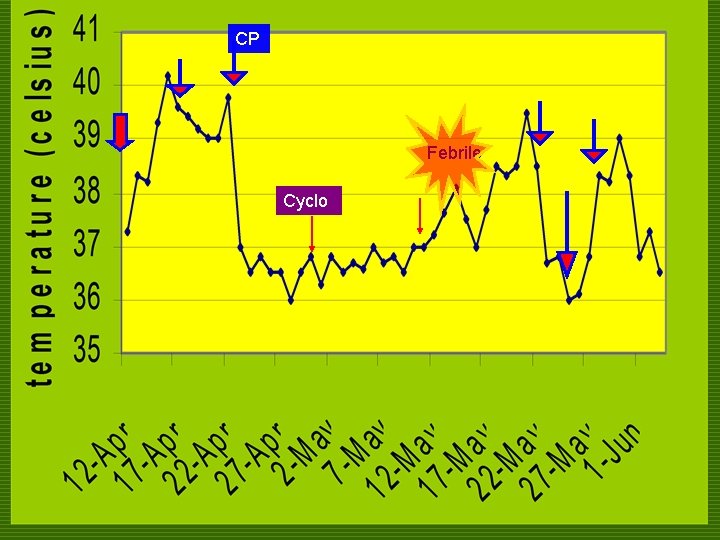
CP Febrile Cyclo

COURSE IN THE WARDS o 53 rd HD n sent home n afebrile o medications: n Tranexamic acid, Cyclosporine 100 mg BID, ciprofloxacin 500 mg BID

FINAL DIAGNOSIS o Aplastic anemia o Salmonella enteritides myositis o Avascular necrosis, femoral head

DISCUSSION

SALMONELLA: MICROBIOLOGY o o o o Gram-negative non-spore forming Facultatively anaerobic bacilli Produce acid on glucose fermentation Motile Do not ferment lactose (99%) Differential metabolism of sugars is used to distinguish serotypes S. typhi does not produce gas on sugar fermentation

NON-TYPHOIDAL SALMONELLA: EPIDEMIOLOGY o o 1996 -1999 estimated 1. 4 M cases of NTS in US 2004 – 14. 7/100, 000 persons n n n Typhimurium – 20% Enteritidis – 15% Newport – 10%

NON-TYPHOIDAL SALMONELLA: EPIDEMIOLOGY - HOST FACTORS o o o o Impaired cell-mediated immunity AIDS Corticosteroid use Malignancy Impaired phagocytic function Hemoglobinopathies Chronic granulomatous disease Schistosomiasis Histoplasmosis Malaria

NON-TYPHOIDAL SALMONELLA: EPIDEMIOLOGY - HOST FACTORS o o Neonates Elderly Extremes of ages Decreased gastric acidity achlorhydria Antacids or suppression of gastric acidity Altered intestinal function o o IBD Prior antibiotic therapy

NON-TYPHOIDAL SALMONELLA: EPIDEMIOLOGY o o Small but significant number Associated with food products (meat, poultry, eggs or dairy products) Associated with shell eggs Associated with exotic pets, especially reptiles

NON-TYPHOIDAL SALMONELLA: EPIDEMIOLOGY

NON-TYPHOIDAL SALMONELLA: PATHOGENESIS o Ingestion from contaminated food/water n o o Infectious dose: 103 -106 CFU Gastric acidity is the initial barrier Bacteria mediated endocytosis

NON-TYPHOIDAL SALMONELLA: PATHOGENESIS o o o Innate immune system n May be determining factor for severity n Depressed PMN function increases incidence Cell-mediated immunity n Role in clearing infection and protecting against subsequent Salmonella infection Humoral immune responses n Protective immunity

NON-TYPHI SALMONELLA CLINICAL MANIFESTATIONS • • o Gastroenteritis Bacteremia and vascular infection Localized infection Chronic carrier state Clinically useful, have no pathogenic nor prognostic significance

NON-TYPHI SALMONELLA BACTEREMIA AND VASCULAR INFECTIONS o 5% of patients with NTS o Infants, elderly and immunocompromised o Salmonella has high propensity for infection of vascular sites n n n 10 -25% in persons > 50 Aorta Venous septic thrombophlebitis

NON-TYPHI SALMONELLA : LOCALIZED INFECTION o Occurs in 5 -10% of patients with NTS bacteremia
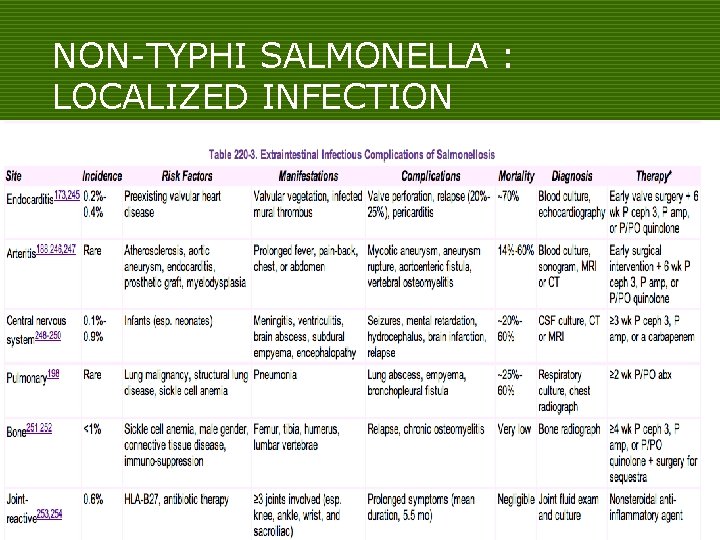
NON-TYPHI SALMONELLA : LOCALIZED INFECTION
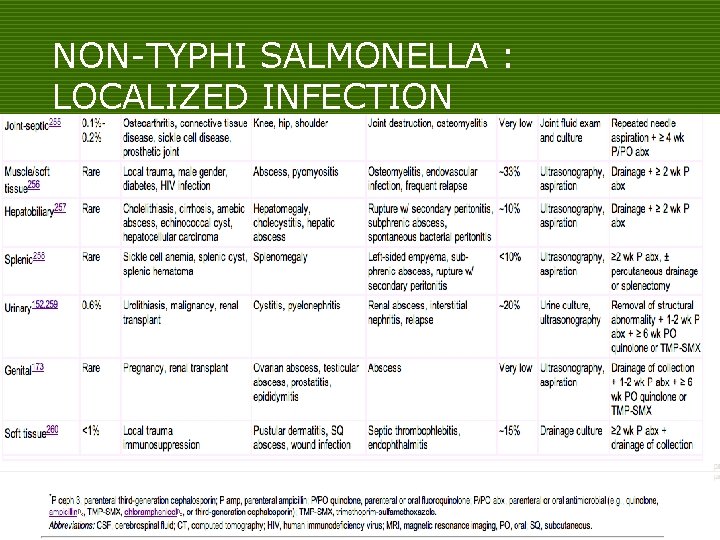
NON-TYPHI SALMONELLA : LOCALIZED INFECTION





NON-TYPHI SALMONELLA SPECIAL POPULATIONS o o o o Immunosuppression Biliary and urinary tract abnormalities Hemoglobinopathies Malaria Schistosomiasis Histoplasmosis AIDS

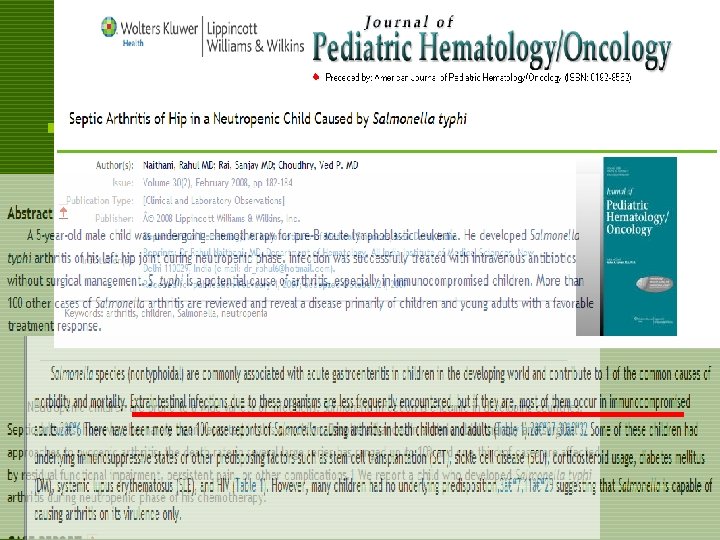

NON-TYPHI SALMONELLOSIS TREATMENT o Neonates, >50 years of age and in patients with immunosuppresion or valvular/endovascular abnormalities ® Oral or IV antimicrobial for 48 to 72 hours or until patient is afebrile

SALMONELLA NON-TYPHI BACTEREMIA TREATMENT o o Empiric: 3 rd generation cephalosporin and a fluoroquinolone Low-grade: 7 -14 days of Tx High-grade: 6 weeks IV therapy with ßlactam (ampicillin or ceftriaxone) is recommended to treat documented or suspected endovascular infection IV Ciprofloxacin, followed by prolonged oral therapy

SALMONELLA NON-TYPHI LOCALIZED INFECTION TREATMENT o o o Ceftriaxone 2 g/d or Cefotaxime 2 g q 8 h Ciprofloxacin 500 mg/tab BID or 400 mg/IV BID Ampicillin 2 g/IV q 6 h

SALMONELLA: ANTIMICROBIAL RESISTANCE o o Widespread use of “over-the-counter” antibiotics Plasmid-encoded resistance Empirical treatment of febrile syndromes and as growth promoters in animal production DT 104: n resistant to ACSSu. T: ampicillin, chloramphenicol, streptomycin, sulfonamides and tetracyclines n Acquired from plasmids in Pseudomonas species

SALMONELLA: ANTIMICROBIAL RESISTANCE o Increase in ceftriaxone and fluoroquinolone resistant nontyphoidal Salmonella



SALMONELLA: PREVENTION AND CONTROL o o o Hand washing Safe drinking water and effective sewage treatment Improved food safety practices Good personal hygiene Prudent antimicrobial use

TREATMENT OF APLASTIC ANEMIA o Hematopoietic stem cell transplantation o Immunosuppression n Anti-thymocyte globulin – induces hematologic recovery Addition of cyclosporine increases response rate up to 70% esp. in children Improvement in leukocyte count apparent within 2 months

TREATMENT OF APLASTIC ANEMIA (IMMUNOSUPPRESSIVE THERAPY) o o o improvement in blood counts occurred in 60 percent of patients after three months The actuarial risk of relapse was 35 percent at five years. Most of the relapsing patients responded to additional courses of immunosuppression, and relapse was not associated with a significant survival disadvantage. . Rosenfeld, SJ, Kimball, et. al Intensive immunosuppression with antithymocyte globulin and cyclosporine as treatment forsevere acquired aplastic anemia. Blood 1995; 85: 3058.

Treatment of aplastic anemia with antilymphocyte globulin and methylprednisolone with or without cyclosporine. The German Aplastic Anemia Study Group o o antilymphocyte globulin, methylprednisolone, and cyclosporine appears to be more effective than a regimen of antilymphocyte globulin and methylprednisolone without cyclosporine may thus represent a treatment of choice for patients who are not eligible for bone marrow transplantation Frickhofen N, Kaltwasser JP, Schrezenmeier H, Raghavachar A, Vogt HG, Herrmann F, Freund M, Meusers P, Salama A, Heimpel H

THANK YOU!

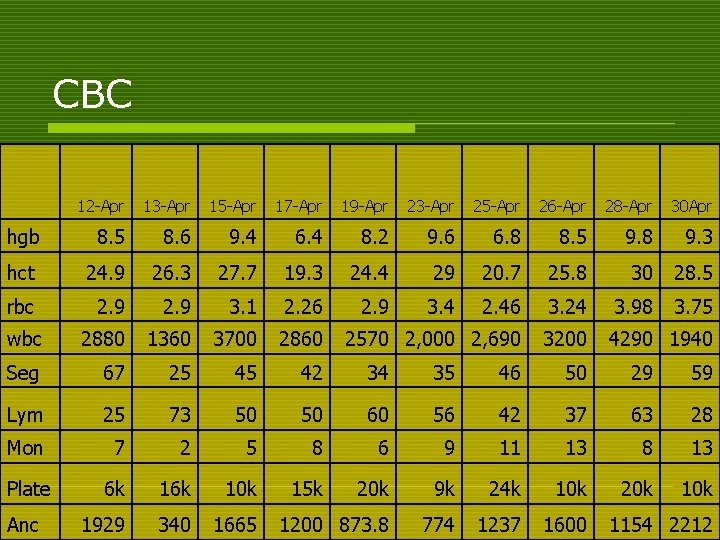
CBC 12 -Apr 13 -Apr 15 -Apr 17 -Apr 19 -Apr 23 -Apr 25 -Apr 26 -Apr 28 -Apr 30 Apr hgb 8. 5 8. 6 9. 4 6. 4 8. 2 9. 6 6. 8 8. 5 9. 8 9. 3 hct 24. 9 26. 3 27. 7 19. 3 24. 4 29 20. 7 25. 8 30 28. 5 rbc 2. 9 3. 1 2. 26 2. 9 3. 4 2. 46 3. 24 3. 98 3. 75 wbc 2880 1360 3700 2860 2570 2, 000 2, 690 3200 4290 1940 Seg 67 25 45 42 34 35 46 50 29 59 Lym 25 73 50 50 60 56 42 37 63 28 Mon 7 2 5 8 6 9 11 13 8 13 Plate 6 k 10 k 15 k 20 k 9 k 24 k 10 k 20 k 1929 340 1665 1200 873. 8 774 1237 1600 Anc 1154 2212
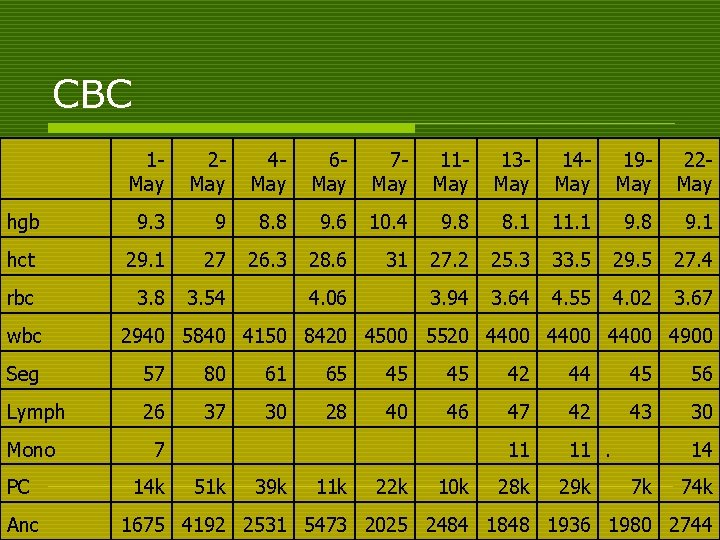
CBC 1 May 2 May 4 May 6 May 7 May 11 May 13 May 14 May 19 May 22 May hgb 9. 3 9 8. 8 9. 6 10. 4 9. 8 8. 1 11. 1 9. 8 9. 1 hct 29. 1 27 26. 3 28. 6 31 27. 2 25. 3 33. 5 29. 5 27. 4 rbc 3. 8 3. 54 3. 94 3. 64 4. 55 4. 02 3. 67 wbc 4. 06 2940 5840 4150 8420 4500 5520 4400 4900 Seg 57 80 61 65 45 45 42 44 45 56 Lymph 26 37 30 28 40 46 47 42 43 30 Mono 7 11 11. PC Anc 14 k 51 k 39 k 11 k 22 k 10 k 28 k 29 k 14 7 k 74 k 1675 4192 2531 5473 2025 2484 1848 1936 1980 2744

TREATMENT OF APLASTIC ANEMIA (IMMUNOSUPPRESSIVE THERAPY) o Horse ATG at a dose 40 mg/kg per day in 500 m. L of saline given over four to six hours for four consecutive days. Rosenfeld, SJ, Kimball, et. al Intensive immunosuppression with antithymocyte globulin and cyclosporine as treatment forsevere acquired aplastic anemia. Blood 1995; 85: 3058.

TREATMENT OF APLASTIC ANEMIA (IMMUNOSUPPRESSIVE THERAPY) o Prednisone or methylprednisolone in divided doses of 1 mg/kg per day. Steroids were given for two weeks, with the dose tapered so that the corticosteroids were discontinued by day 30. Rosenfeld, SJ, Kimball, et. al Intensive immunosuppression with antithymocyte globulin and cyclosporine as treatment forsevere acquired aplastic anemia. Blood 1995; 85: 3058.

TREATMENT OF APLASTIC ANEMIA (IMMUNOSUPPRESSIVE THERAPY) o Cyclosporine, 10 -12 mkd, in two equally divided doses, n n aiming for trough levels of 100 to 200 ng/m. L of serum or 500 to 800 ng/m. L in whole blood. Cyclosporine is generally continued for about six months, although the dose may be tapered after one month to trough whole blood levels of 200 to 500 ng/m. L. Rosenfeld, SJ, Kimball, et. al Intensive immunosuppression with antithymocyte globulin and cyclosporine as treatment forsevere acquired aplastic anemia. Blood 1995; 85: 3058.
- Slides: 105