Medical Care In Diabetes Bijan Iraj MD Assistant

Medical Care In Diabetes �Bijan Iraj, MD Assistant Professor of Internal Medicine and Endocrinology Department of Endocrinology and Metabolism Isfahan Medical School.

Management of Type 2 Diabetes Mellitus DX HIS PE LAB + ECG REFFERAL TARGET HBA 1 C

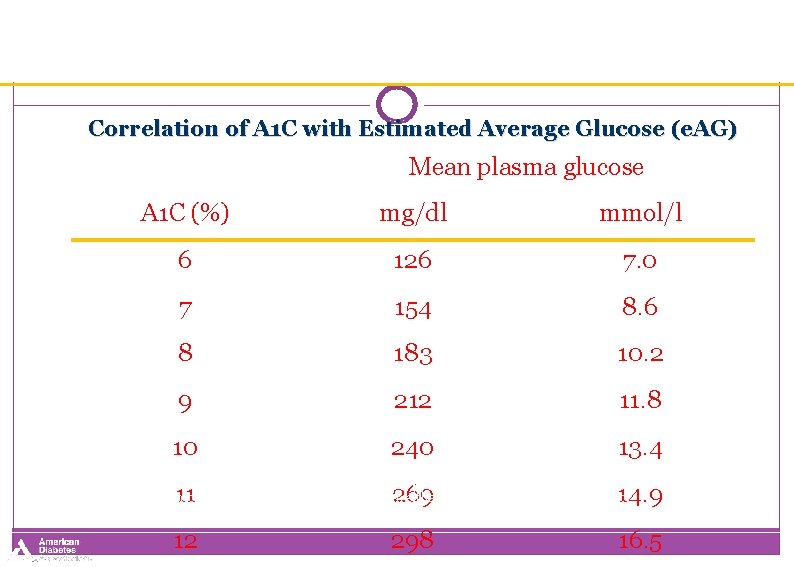
Correlation of A 1 C with Estimated Average Glucose (e. AG) Mean plasma glucose A 1 C (%) mg/dl mmol/l 6 126 7. 0 7 154 8. 6 8 183 10. 2 9 212 11. 8 10 240 13. 4 11 269 14. 9 12 298 16. 5 These estimates are based on ADAG data of ~2, 700 glucose measurements over 3 months per A 1 C measurement in 507 adults with type 1, type 2, and no diabetes. The correlation between A 1 C and average glucose was 0. 92. A calculator for converting A 1 C results into estimated average glucose (e. AG), in either mg/dl or mmol/l, is available at http: //professional. diabetes. org/Glucose. Calculator. aspx.

Treat the patient, not the blood sugar.

�Lifestyle modification �Lipid treatment �BP control �ASA+/�Cigarette cessation �Glucose control
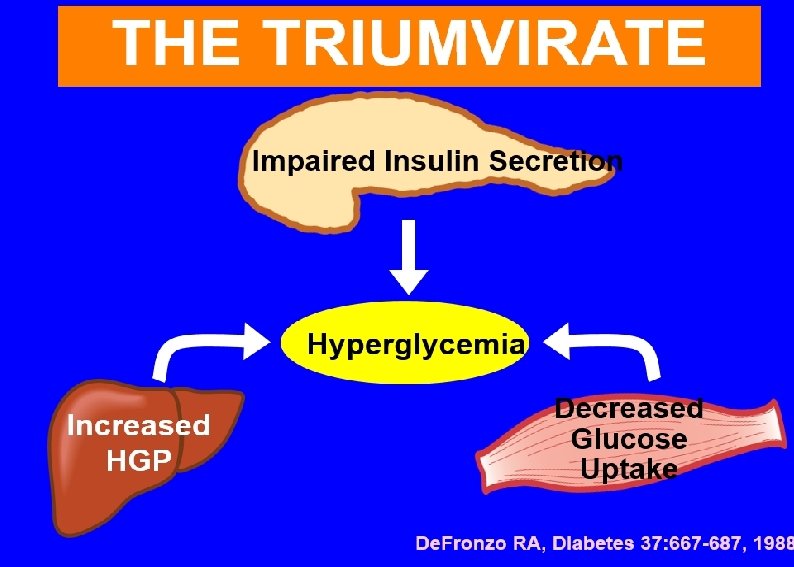
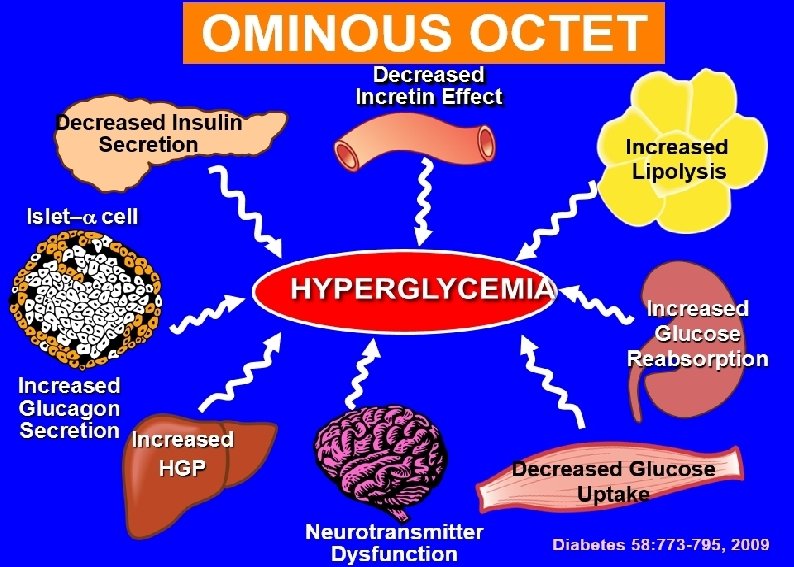




Lifestyle intervention

Lifestyle Therapy § medical nutrition therapy § regular physical activity § sufficient amounts of sleep § behavioral support § smoking cessation and avoidance of all tobacco products. � Lifestyle therapy begins with nutrition counseling and education. � All patients should strive to attain and maintain an optimal weight through a primarily plant-based diet high in polyunsaturated and monounsaturated fatty acids, with limited intake of saturated fatty acids and avoidance of trans fats.

Pharmacotherapy of DM 2 �Efficacy: Hb. A 1 c �Hypoglycemia �Weight �Side effects �Durability �Cardiovascular/CNS outcome �CKD �NAFLD/NASH �Cost
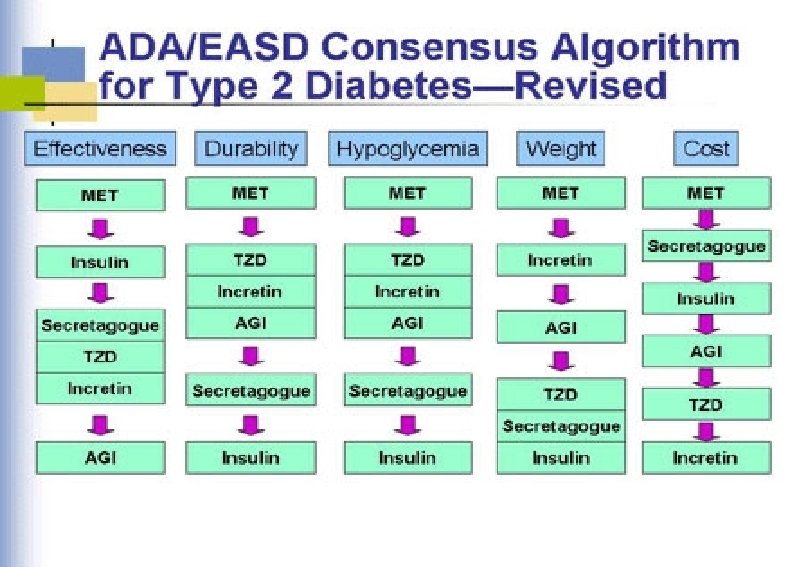
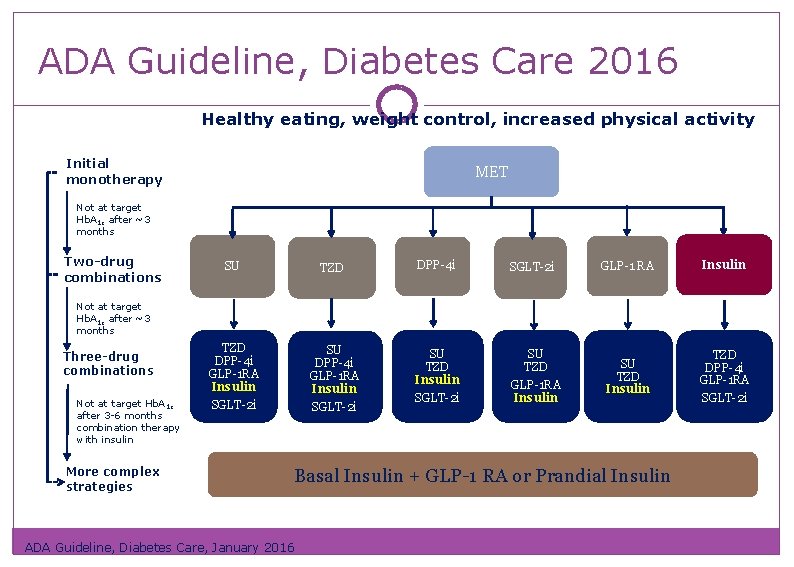
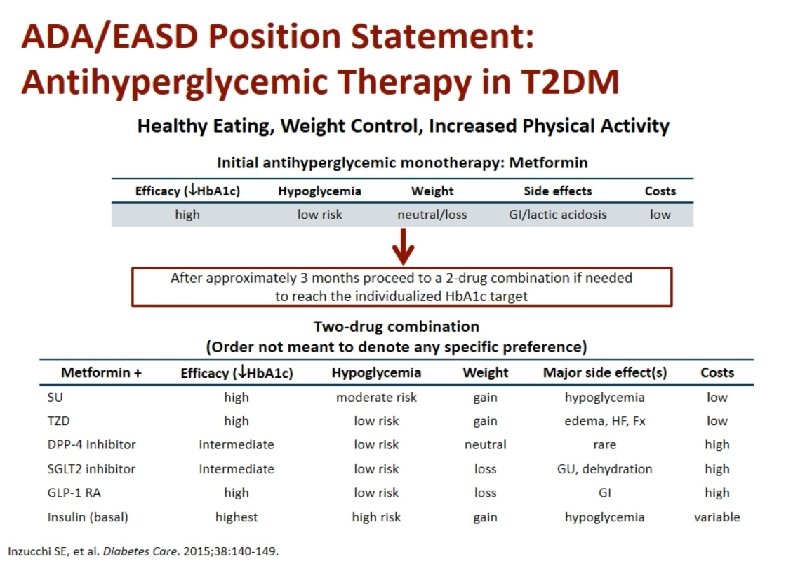
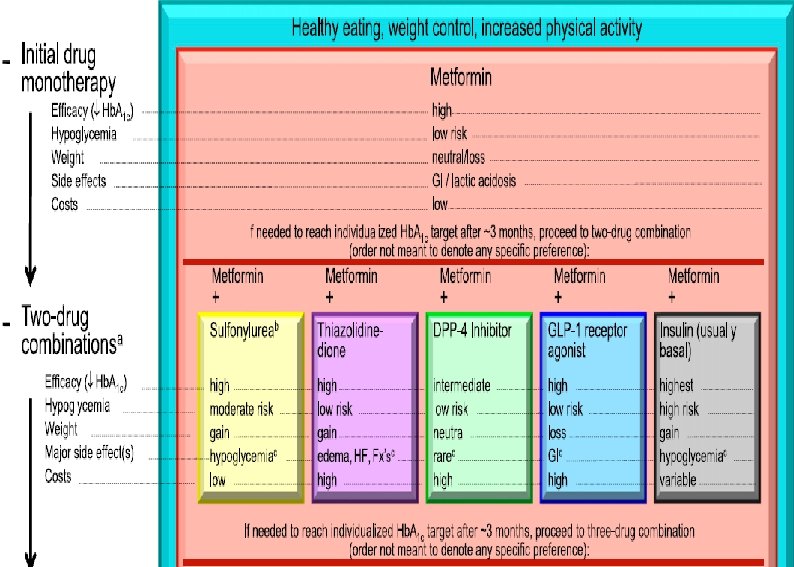
ADA Guideline, Diabetes Care 2016 Healthy eating, weight control, increased physical activity Initial monotherapy MET Not at target Hb. A 1 c after ~3 months Two-drug combinations SU TZD DPP-4 i SGLT-2 i TZD DPP-4 i GLP-1 RA Insulin SGLT-2 i SU TZD GLP-1 RA Insulin GLP-1 RA Insulin SU TZD Insulin TZD DPP-4 i GLP-1 RA SGLT-2 i Not at target Hb. A 1 c after ~3 months Three-drug combinations Not at target Hb. A 1 c after 3 -6 months combination therapy with insulin More complex strategies Basal Insulin + GLP-1 RA or Prandial Insulin ADA Guideline, Diabetes Care, January 2016
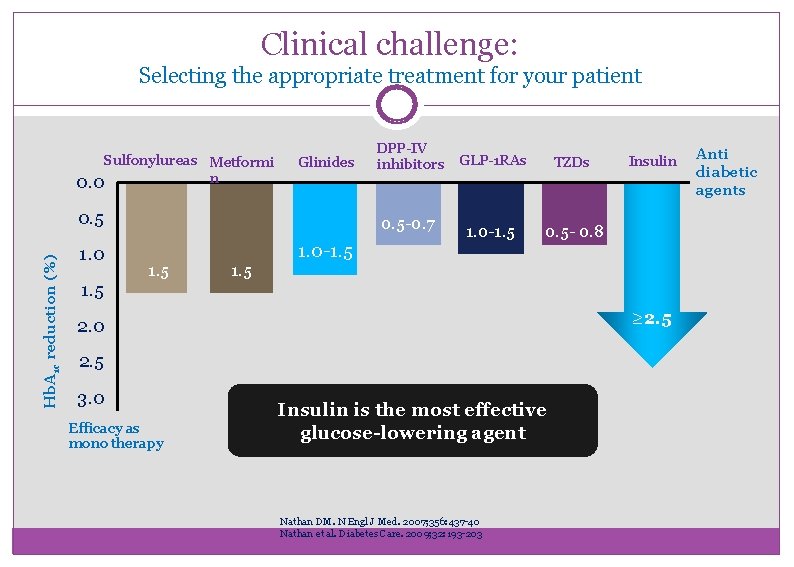
Clinical challenge: Selecting the appropriate treatment for your patient Sulfonylureas Metformi n 0. 0 Glinides Hb. A 1 c reduction (%) 0. 5 1. 0 1. 5 DPP-IV inhibitors 0. 5 -0. 7 1. 5 1. 0 -1. 5 GLP-1 RAs TZDs 1. 0 -1. 5 0. 5 - 0. 8 ≥ 2. 5 2. 0 2. 5 3. 0 Efficacy as mono therapy Insulin is the most effective glucose-lowering agent Nathan DM. N Engl J Med. 2007; 356: 437 -40 Nathan et al. Diabetes Care. 2009; 32: 193 -203 Anti diabetic agents

Insulin sensitizer with predominant action in the liver: Metformin: v. Dose v. Adverse events v. Titration

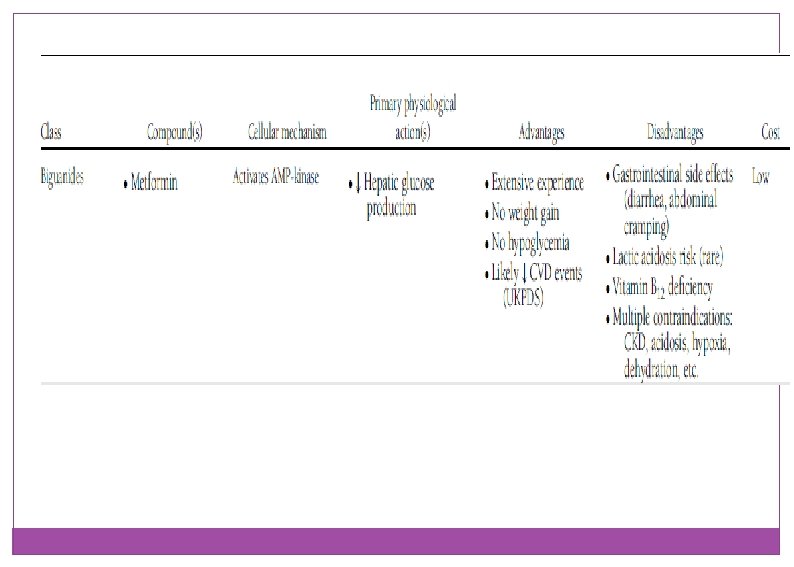
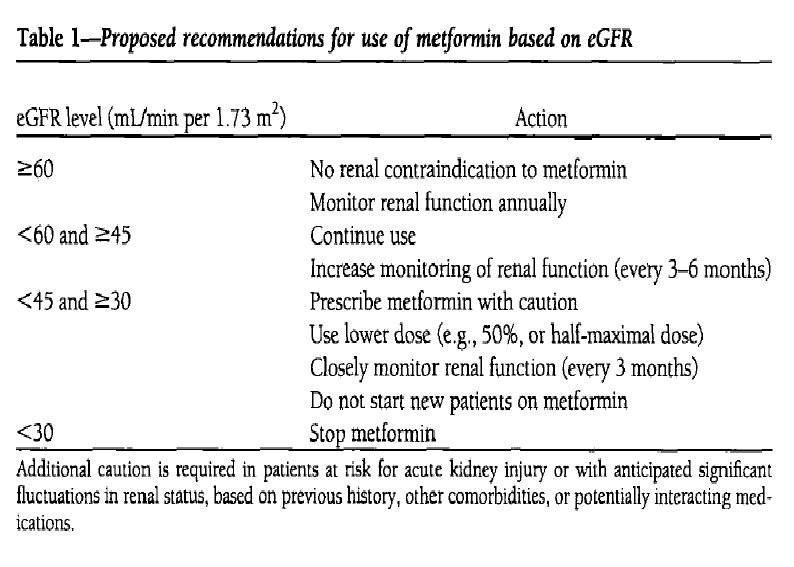

Insulin sensitizer with predominant action in Peripheral: TZD Pioglitazon: v. Dose v. Advers events
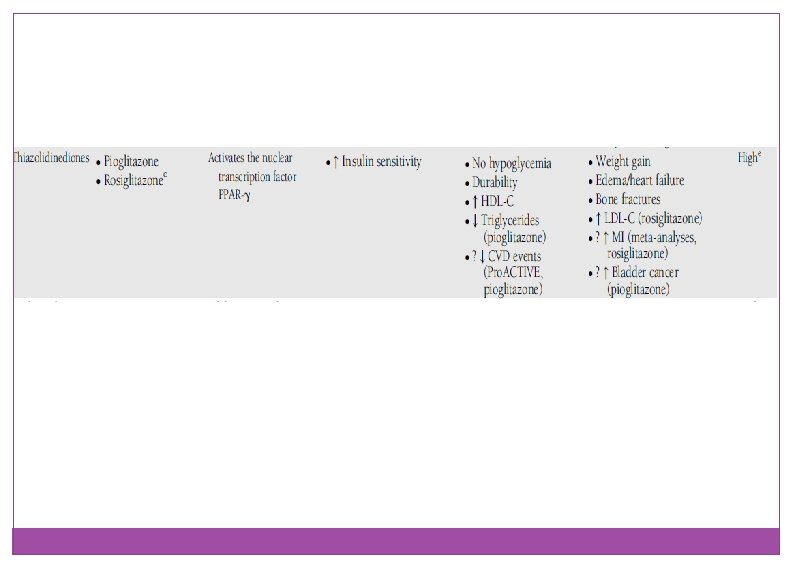
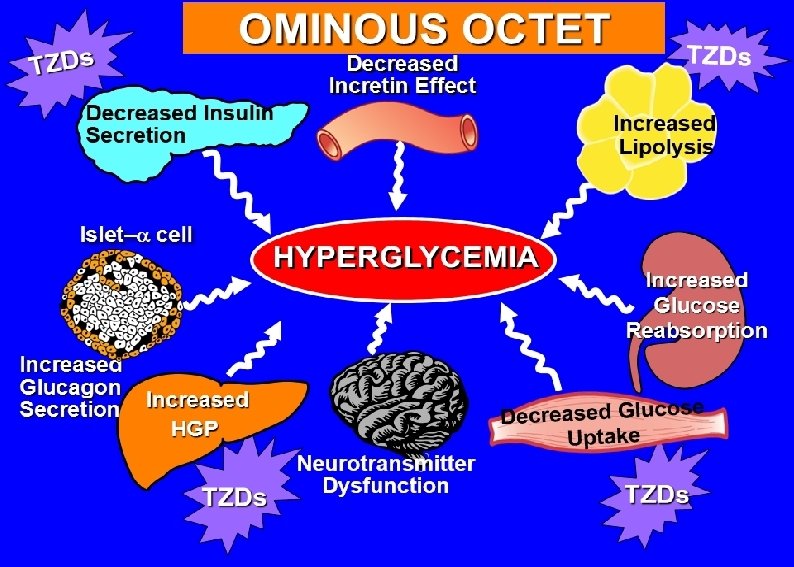

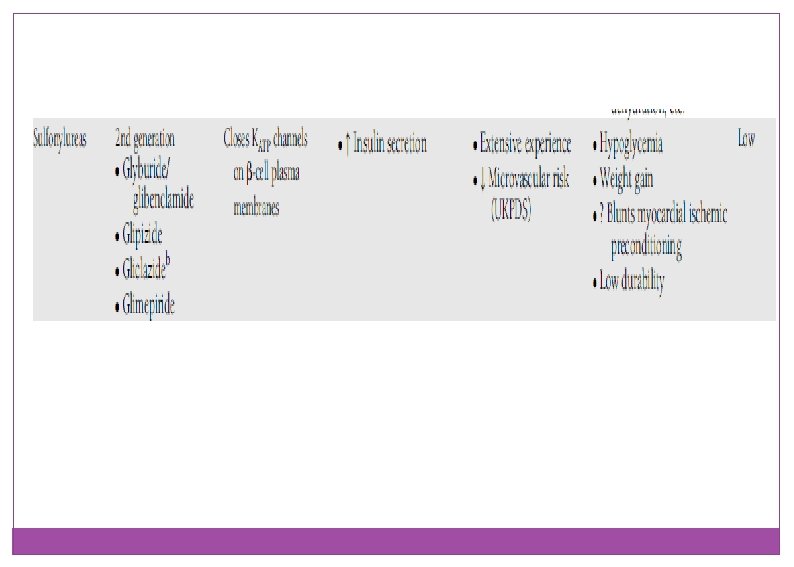
Insulin secretagogues: sulfonylureas Meal plane and Regularity: v. Dose v. Potency v. Age v. Drug interaction v. Indications
Hypoglycemia due to SUR Glibenclamid �Glimiprid �Glicloasid Repaglinid/nateglinid SR Glipizid � MR Gliclazid



Carbohydrate absorption inhibitors α-glucosidose inhibitors Acarbose: v. Dose v. Adverse events

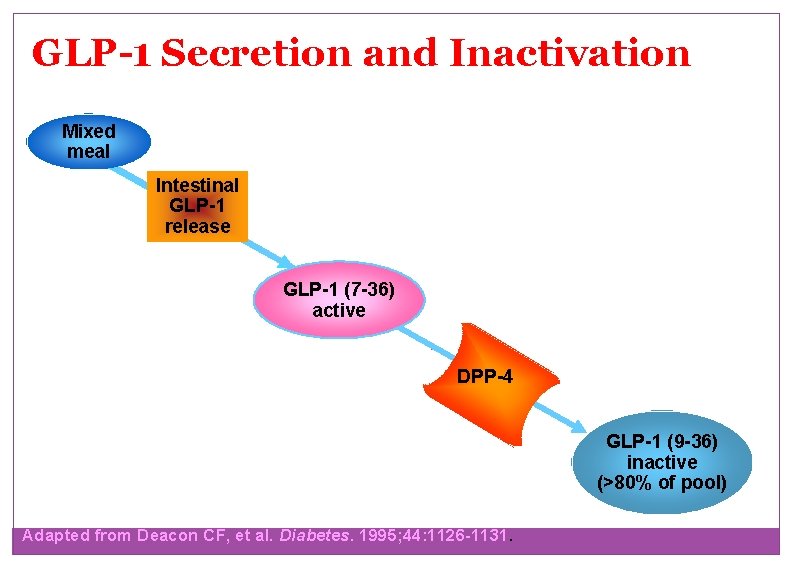
GLP-1 Secretion and Inactivation Mixed meal Intestinal GLP-1 release T 1/2 = 1 to 2 min GLP-1 (7 -36) active DPP-4 GLP-1 (9 -36) inactive (>80% of pool) Adapted from Deacon CF, et al. Diabetes. 1995; 44: 1126 -1131.

Inhibition of DPP-4 Increases Active GLP-1 Mixed meal Intestinal GLP-1 release GLP-1 (7 -36) GLP-1 active DPP-4 inhibitor Adapted from Rothenberg P, et al. Diabetes. 2000; 49(suppl 1): A 39. GLP-1 (9 -36) inactive

Incretin – Based therapies DPP-4 Inhibitors: v Sitagliptin v Linagliptin v Saxagliptin v Alogliptin

Incretin – Based Therapies GLP 1 agonists: v Exenetide v Liraglutide v Exenetide QW

Sodium Glucose Co-Transports 2 inhibitors SGLT 2 IS
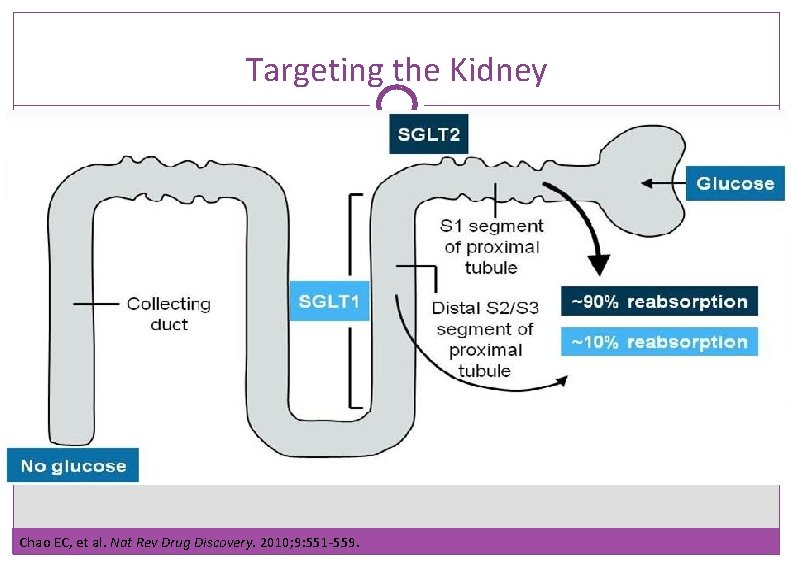
Targeting the Kidney Chao EC, et al. Nat Rev Drug Discovery. 2010; 9: 551 -559.

The Kidneys Play an Important Role in Glucose Control Normal Renal Glucose Physiology • 180 g of glucose is filtered each day • Virtually all glucose reabsorbed in the proximal tubules & reenters the circulation • SGLT 2 reabsorbs about 90% of the glucose • SGLT 1 reabsorbs about 10% of the glucose • Virtually no glucose excreted in urine Mather, A & Pollock, C. Kidney International. 2011; 79: S 1 -S 6.

SGLT 2 Inhibitors in Phase 3 Development • Empagliflozin • Canagliflozin • Dapagliflozin • Ipragliflozin

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • • Age Weight Sex / racial / ethnic / genetic differences Comorbidities - Coronary artery disease Heart Failure Chronic kidney disease Liver dysfunction Hypoglycemia Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of print

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Age: Older adults - Reduced life expectancy Higher CVD burden Reduced GFR At risk for adverse events from polypharmacy More likely to be compromised from hypoglycemia üLess ambitious targets üHb. A 1 c <7. 5– 8. 0% if tighter targets not easily achieved üFocus on drug safety Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Weight - Majority of T 2 DM patients overweight / obese Intensive lifestyle program Metformin GLP-1 receptor agonists ? Bariatric surgery Consider LADA in lean patients Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of print

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction - Hypoglycemia Ø Metformin: CVD benefit (UKPDS) Ø Avoid hypoglycemia Ø ? SUs & ischemic preconditioning Ø ? Pioglitazone & CVD events Ø ? Effects of incretin-based therapies Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of print

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction Ø Metformin: May use unless condition is unstable or severe Ø Avoid TZDs Ø ? Effects of incretin-based therapies - Hypoglycemia Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of print
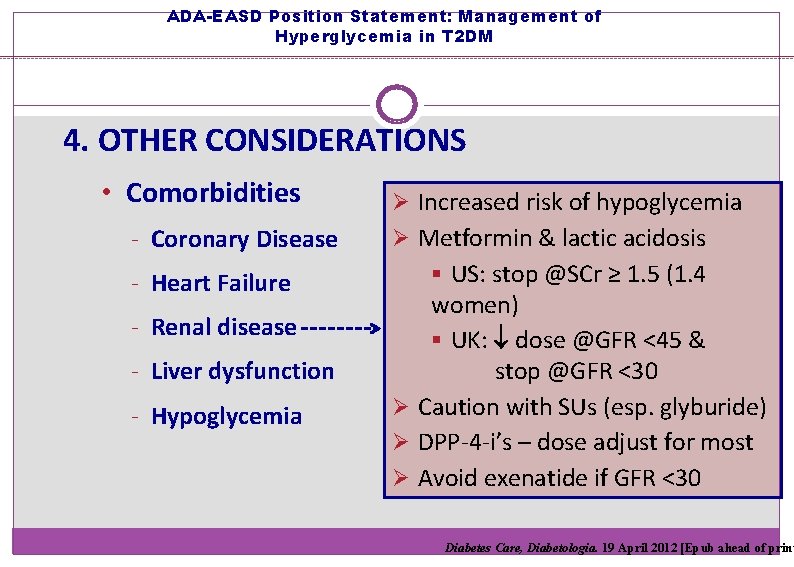

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction - Hypoglycemia Ø Increased risk of hypoglycemia Ø Metformin & lactic acidosis § US: stop @SCr ≥ 1. 5 (1. 4 women) § UK: dose @GFR <45 & stop @GFR <30 Ø Caution with SUs (esp. glyburide) Ø DPP-4 -i’s – dose adjust for most Ø Avoid exenatide if GFR <30 Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of print

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction - Hypoglycemia Ø Most drugs not tested in advanced liver disease Ø Pioglitazone may help steatosis Ø Insulin best option if disease severe Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of print

ADA-EASD Position Statement: Management of Hyperglycemia in T 2 DM 4. OTHER CONSIDERATIONS • Comorbidities - Coronary Disease - Heart Failure - Renal disease - Liver dysfunction - Hypoglycemia Ø Emerging concerns regarding association with increased mortality Ø Proper drug selection in the hypoglycemia prone Diabetes Care, Diabetologia. 19 April 2012 [Epub ahead of print
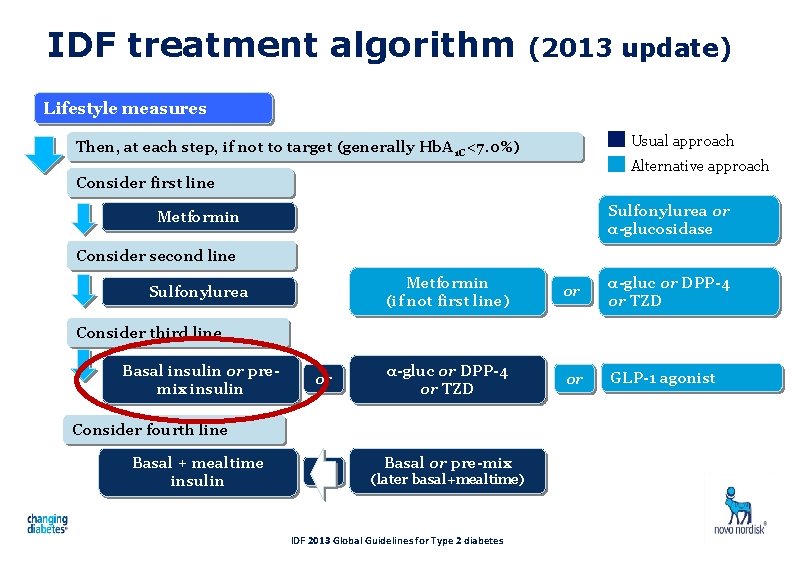
IDF treatment algorithm (2013 update) Lifestyle measures Usual approach Then, at each step, if not to target (generally Hb. A 1 C<7. 0%) Alternative approach Consider first line Sulfonylurea or α-glucosidase Metformin Consider second line Sulfonylurea Metformin (if not first line) or α-gluc or DPP-4 or TZD or GLP-1 agonist Consider third line Basal insulin or premix insulin or Consider fourth line Basal + mealtime insulin Basal or pre-mix (later basal+mealtime) IDF 2013 Global Guidelines for Type 2 diabetes

Recommended standards of care for patients with type 2 Diabetes Mellitus v Weight at each visit v Bp at each visit v Blood glucose monitoring individualized v Hb. A 1 C at 3 -mo intervals v at diagnosis and then yearly v Dilated v v eye exam Lipid profile Urine micro albumin

- Slides: 57