Medicaid Transformation A Changing System NCAPSE Spring 2019














- Slides: 23

Medicaid Transformation: A Changing System. NCAPSE Spring 2019 Conference Julia Adams Scheurich Pag e 1

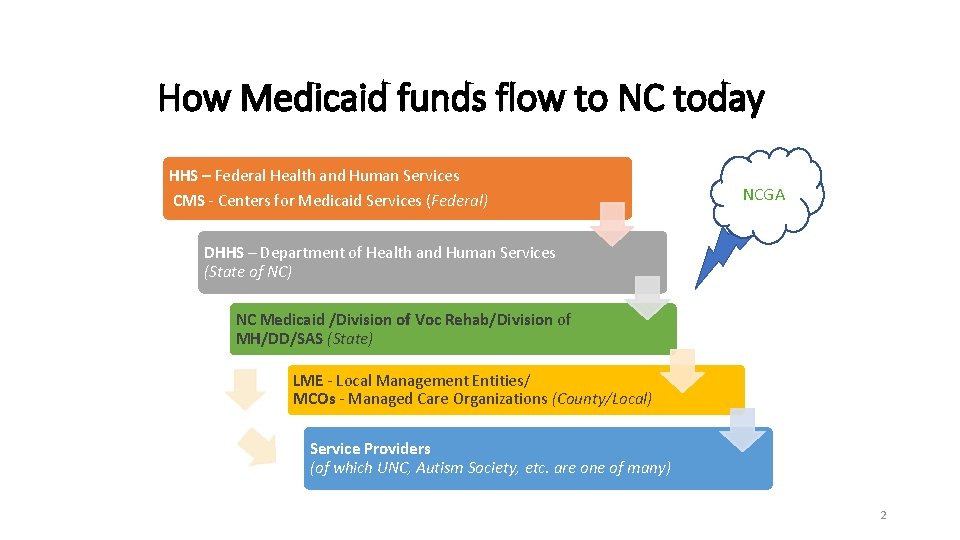
How Medicaid funds flow to NC today HHS – Federal Health and Human Services CMS - Centers for Medicaid Services (Federal) NCGA DHHS – Department of Health and Human Services (State of NC) NC Medicaid /Division of Voc Rehab/Division of MH/DD/SAS (State) LME - Local Management Entities/ MCOs - Managed Care Organizations (County/Local) Service Providers (of which UNC, Autism Society, etc. are one of many) 2

• “Improving the health and well-being of North Carolinians through an innovative, whole-person centered and well- coordinated system of care that addresses both medical and non-medical drivers of health. ” Vision for Medicaid Managed Care - DHHS 3

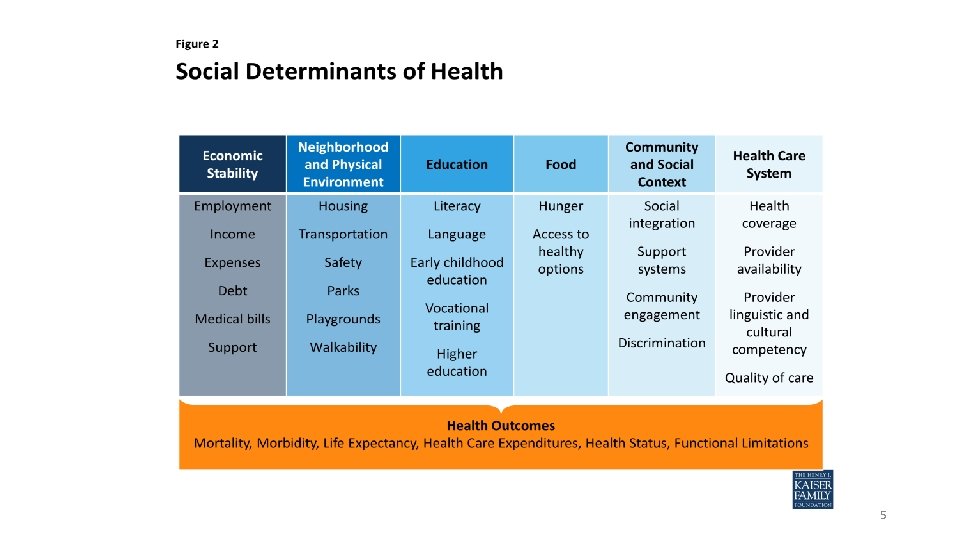
4 Medicaid Transformation = Change is coming • Requires Medicaid to move to an at risk, capitated, managed care 1115 waiver • 1115 waiver is the federal authority used to accomplish the foundations set forth in the state law • We currently operate under the 1915 b/c waiver • Moves away from a fee for service model for services outside of the LME/MCO. • Vision of reform is to deliver whole-person care through coordinated physical health, behavioral health, intellectual/developmental disabilities and pharmacy products and care models. • Includes Social Determinants of Health. • Address the full set of factors that impact health, uniting communities and health care systems • https: //www. ncdhhs. gov/assistance/medicaid-transformation

5

2015: Session Law 2015 -245 directs the Department to transition to managed care 2015 -2018: Extensive collaboration with and feedback from stakeholders How did we get here? Aug 2018: RFP released Oct 2018: CMS approves 1115 waiver Feb 2019: Contracts Awarded to PHP. 6

PHPs for NC Medicaid Managed Care for Standard Plans • Statewide contracts • Ameri. Health Caritas North Carolina, Inc. • Blue Cross and Blue Shield of North Carolina, Inc. • United. Healthcare of North Carolina, Inc. • Well. Care of North Carolina, Inc. • Regional contract – Regions 3 & 5 • Carolina Complete Health, Inc.

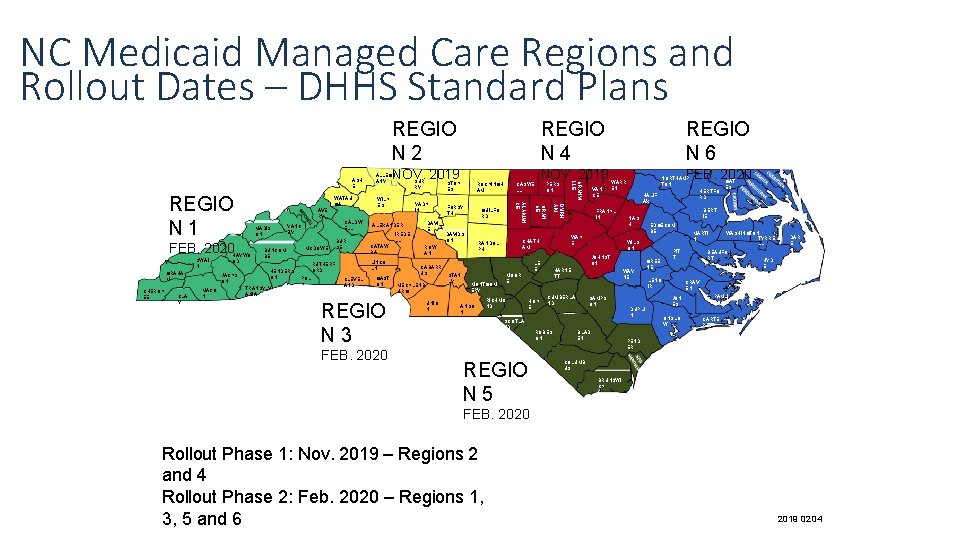
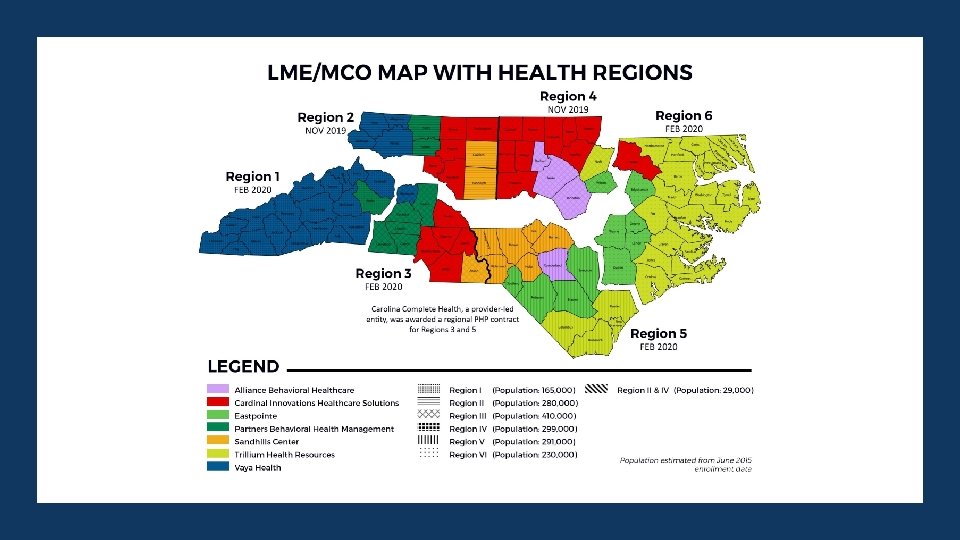
NC Medicaid Managed Care Regions and Rollout Dates – DHHS Standard Plans REGIO N 2 GRAHA M CHEROK EE CLA Y HAYWO OD JACKS ON MACO N MADIS ON YANC EY BUNCOM BE HENDERS ON TRANSYLV ANIA MCDOWE LL CALDW ELL BUR KE POL K CLEVEL AND DAVI E ALEXANDER IREDE LL CATAW BA LINCO LN RUTHERF ORD YADK IN GAST ON REGIO N 3 FEB. 2020 ROCKINGH AM FORSY TH GUILFO RD DAVIDS ON CABARR US MECKLENB URG UNIO N PERS ON MONTGOM ERY ANSO N HOK E SCOTLA ND REGIO N 5 FRANKL IN NAS H WAY NE CUMBERLA ND ROBES ON SAMPS ON BLAD EN HERTFO RD HALIF AX DUPLI N GAT ES BERT IE EDGECOM BE WILS ON HARNE TT MOOR E RICHMO ND FEB. 2020 NORTHAMP TON WARR EN JOHNST ON LE E STAN LY VAN CE REGIO N 6 WAK E CHATH AM RANDOL PH ROW AN NOV. 2019 CASWE LL DURH AM SWAI N AVE RY WILK ES STOK ES ORAN GE FEB. 2020 WATAU GA SUR RY ALAMAN CE REGIO N 1 NOV. 2019 ALLEGH ANY GRANVI LLE ASH E REGIO N 4 GREE NE WASHINGTON TYRRE LL MARTI N PIT T LENO IR BEAUFO RT DAR E HYD E CRAV EN JON ES ONSLO W PAMLI CO CARTE RET PEND ER COLUMB US BRUNSWI CK FEB. 2020 Rollout Phase 1: Nov. 2019 – Regions 2 and 4 Rollout Phase 2: Feb. 2020 – Regions 1, 3, 5 and 6 8 2019 02 04


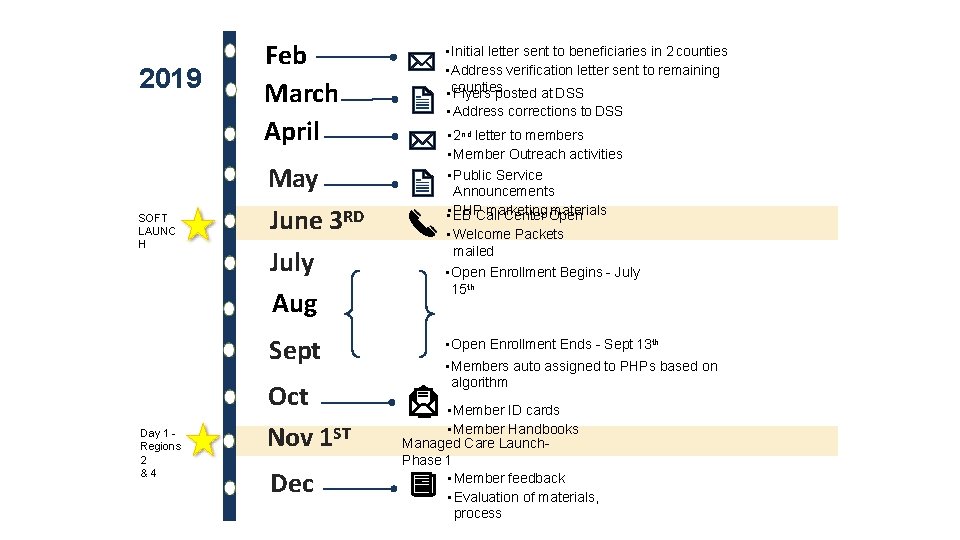
2019 SOFT LAUNC H Feb March April May June 3 RD July Aug Sept Day 1 Regions 2 &4 Oct Nov 1 ST Dec • Initial letter sent to beneficiaries in 2 counties • Address verification letter sent to remaining • counties Flyers posted at DSS • Address corrections to DSS • 2 nd letter to members • Member Outreach activities • Public Service Announcements PHPCall marketing materials • • EB Center Open • Welcome Packets mailed • Open Enrollment Begins - July 15 th • Open Enrollment Ends - Sept 13 th • Members auto assigned to PHPs based on algorithm • Member ID cards • Member Handbooks Managed Care Launch. Phase 1 • Member feedback • Evaluation of materials, process

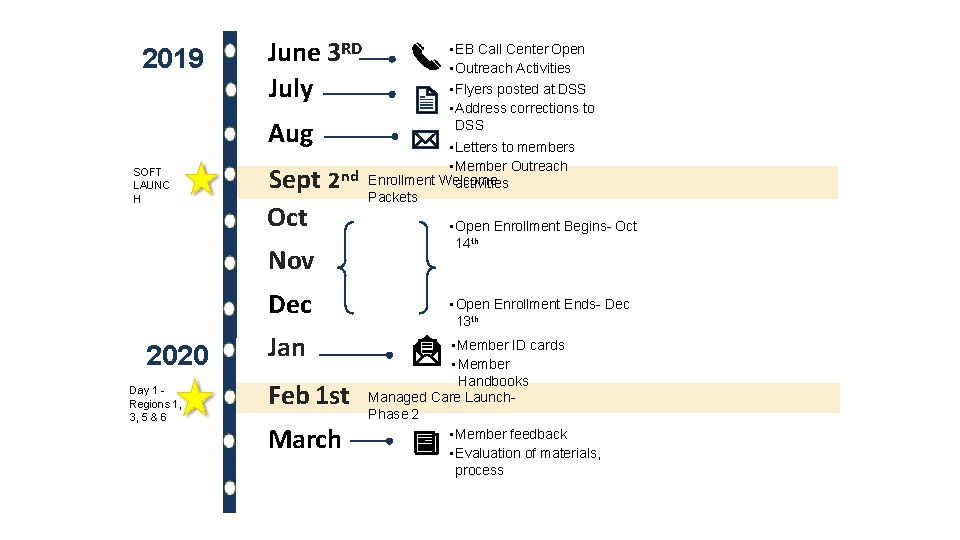
2019 June 3 RD July Aug SOFT LAUNC H Sept 2 Oct • Letters to members • Member Outreach nd Enrollment Welcome activities Packets Nov Dec 2020 Day 1 Regions 1, 3, 5 & 6 • EB Call Center Open • Outreach Activities • Flyers posted at DSS • Address corrections to DSS Jan Feb 1 st March • Open Enrollment Begins- Oct 14 th • Open Enrollment Ends- Dec 13 th • Member ID cards • Member Handbooks Managed Care Launch. Phase 2 • Member feedback • Evaluation of materials, process

How will people know which plan we are in? This Photo by Unknown Author is licensed under CC BY-NC-ND

Independent of the PHPs. Maximus: The Role of the Enrollment Broker Will help people decide which plan they should be in. There is an auto assignment into the plans but there is choice. Won an RFP to do this work in NC.

Beneficiary Experience – Auto Assignment Beneficiaries who don’t choose a health plan will be assigned one automatically, consistent with the following components in this order: 1. Where the beneficiary lives. 2. Whether the beneficiary is a member of a special population (e. g. member of federally recognized tribes or BH I/DD Tailored Plan eligible). 3. If the beneficiary has a historic relationship with a particular PCP/AMH. 4. Plan assignments of other family members. 5. If the beneficiary has a historic relationship with a particular PHP in the previous twelve (12) months (e. g. , “churned” off/into Medicaid Managed Care). 9

The Prepaid Health Plans: Benefits Both Standard Plans and BH I/DD Tailored Plans will be integrated managed care products and will provide a robust set of physical health, behavioral health, long-term services and supports, and pharmacy benefits. Create single point of accountability for care and outcomes for Medicaid. Standard Plans Beneficiaries benefit from integrated physical & behavioral health services “Primary care” behavioral health spend included in PHP capitation rate Phased implementation – Nov. 2019 & Feb. 2020 Tailored Plans Specialized managed care plans targeted toward populations with significant BH and I/DD needs Access to expanded service array Behavioral Health Homes Projected for July 2021 3

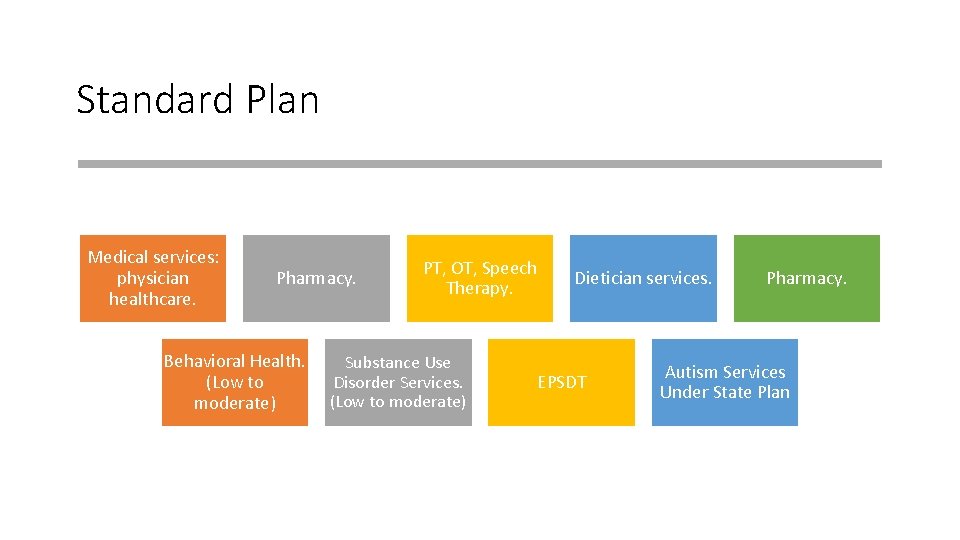
Standard Plan Medical services: physician healthcare. Pharmacy. Behavioral Health. (Low to moderate) PT, OT, Speech Therapy. Substance Use Disorder Services. (Low to moderate) Dietician services. EPSDT Pharmacy. Autism Services Under State Plan

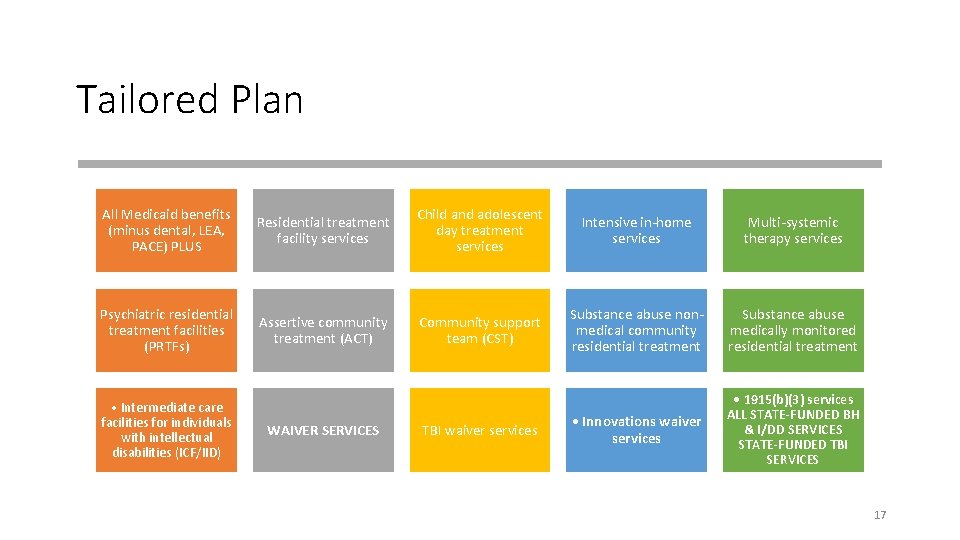
Tailored Plan All Medicaid benefits (minus dental, LEA, PACE) PLUS Residential treatment facility services Child and adolescent day treatment services Intensive in-home services Multi-systemic therapy services Psychiatric residential treatment facilities (PRTFs) Assertive community treatment (ACT) Community support team (CST) Substance abuse nonmedical community residential treatment Substance abuse medically monitored residential treatment • Innovations waiver services • 1915(b)(3) services ALL STATE-FUNDED BH & I/DD SERVICES STATE-FUNDED TBI SERVICES • Intermediate care facilities for individuals with intellectual disabilities (ICF/IID) WAIVER SERVICES TBI waiver services 17

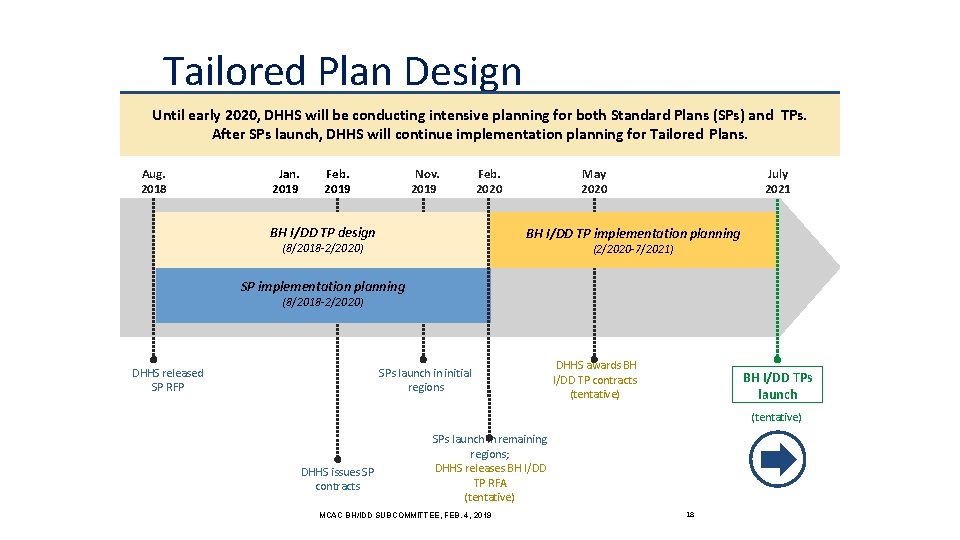
Tailored Plan Design and Launch Timeline Until early 2020, DHHS will be conducting intensive planning for both Standard Plans (SPs) and TPs. After SPs launch, DHHS will continue implementation planning for Tailored Plans. Aug. 2018 Jan. 2019 Feb. 2019 Nov. 2019 Feb. 2020 BH I/DD TP design May 2020 July 2021 BH I/DD TP implementation planning (8/2018 -2/2020) (2/2020 -7/2021) SP implementation planning (8/2018 -2/2020) DHHS released SP RFP SPs launch in initial regions DHHS awards BH I/DD TP contracts (tentative) BH I/DD TPs launch (tentative) DHHS issues SP contracts SPs launch in remaining regions; DHHS releases BH I/DD TP RFA (tentative) MCAC BH/IDD SUBCOMMITTEE, FEB. 4, 2019 18

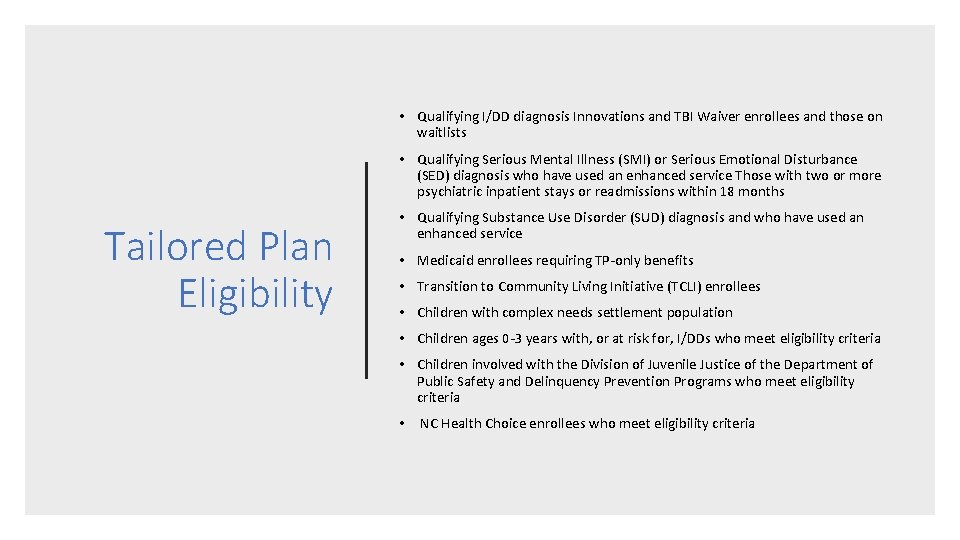
• Qualifying I/DD diagnosis Innovations and TBI Waiver enrollees and those on waitlists • Qualifying Serious Mental Illness (SMI) or Serious Emotional Disturbance (SED) diagnosis who have used an enhanced service Those with two or more psychiatric inpatient stays or readmissions within 18 months Tailored Plan Eligibility • Qualifying Substance Use Disorder (SUD) diagnosis and who have used an enhanced service • Medicaid enrollees requiring TP-only benefits • Transition to Community Living Initiative (TCLI) enrollees • Children with complex needs settlement population • Children ages 0 -3 years with, or at risk for, I/DDs who meet eligibility criteria • Children involved with the Division of Juvenile Justice of the Department of Public Safety and Delinquency Prevention Programs who meet eligibility criteria • NC Health Choice enrollees who meet eligibility criteria

What services are in the standard plan for people with I/DD, MH or SUD? Tailored Plan Simplified • Behavioral Health Urgent Care • Outpatient Plus • Rapid Care Services • Behavioral Health Crisis Assessment and Intervention • Child First Outpatient • EPSDT (both plans) • RBBHT –State Plan Services for children and young adults with Autism. Age 0 -21. This is ABA. (both plans) • Care management. • SDOH through NCCARES 360, Healthy Opportunities Pilots, and what the PHPs have internally that they will bring to NC.

What services will remain in the tailored plan? Tailored Plan Simplified • Innovations waiver. • B 3. • ILOS (except for ones that are specifically for the standard plan) • Behavioral Health Urgent Care • Outpatient Plus • Rapid Care Services • Behavioral Health Crisis Assessment and Intervention • Child First Outpatient • State dollar services. • ICF/IDD • Intensive services for mental health, substance use disorders, PRTF, residential.

Tailored Plan Simplified Is there choice in which plan a person can enroll in? • Yes and No Can I go to the standard plan and stay on the Innovations waitlist? • Yes. You will not loose your place on the waitlist. Can I go to the standard plan and keep my Innovation waiver, B 3, ILOS, or Single Stream Services? • No. You would loose your tailored plan services.

How can I learn more about the tailored plans? • DHHS has a lot of information: • Behavioral Health/IDD Tailored Plan: https: //medicaid. ncdhhs. gov/behavioral-healthidd-tailored-plans • Has link to all the previous webinars including the slides and a transcript of the presentations. • Link to the Eligibility and Enrollment Paper: https: //files. nc. gov/ncdhhs/BH-IDD-TPFinal. Policy. Guidance-Final-20190318. pdf • Next white paper from DHHS will be on care/case management.