Medicaid Part II July 10 2019 By Ashley

Medicaid Part II July 10, 2019 By: Ashley M. Valla, Esq. Haley Weinblatt & Calcagni, LLP 1601 Veterans Memorial Highway, Suite 425 Islandia, New York 11749 (631) 582 -5151; Fax (631) 234 -7108 e-mail: amv@hwclaw. com 1

Types of Applications • • • Community Medicaid* Immediate Need Community Medicaid Conversion (Community Chronic or vice versa) Chronic Care* Renewal / Recertification 2

Terms • Pick-Up Date • Date applicant is looking for coverage • Pend • Document request issued by the DSS caseworker • NAMI • Net Available Monthly Income payable to the nursing home every month • Spenddown/Overage (Community Medicaid) • Amount over the income or resource level that needs to be spent -down before an applicant is considered eligible for Medicaid benefits • A/R • Applicant / Recipient 3

Medicaid Application Timeline 1. Initial Meeting with Client 2. Review of documentation and request additional documentation as necessary 3. Optional follow-up meeting with client 4. Preparation of application 5. Submission of Medicaid application 6. Acknowledgment of application by DSS 7. Document Request(s) (Pends) 8. Decision 9. Post-Decision appeal (if necessary) • Depending on the type of application, this process can take several months to complete. 4

Initial Client Meeting • Prior to meeting, send out questionnaire and/or checklist if client already knows what type of application • Ask client to bring current assets, income and most recent tax returns with 1099 s to the meeting • Determine client’s needs and long term plan (ex: prognosis, financial situation, estate planning, etc. ) • Review financial snapshot of assets and income and create a plan for eligibility • Define and set expectations (ex: application time, time until care is in place, NAMI payments, etc. ) 5

Application Forms • Medicaid Application (DOH-4220) • Supplement A (DOH-5178 A) • Authorized Representative form (DOH-5427) • Submission on Behalf of Applicant (DOH-5147) • Authorization for Verification of Resources forms (DOH-5148 & DOH-5149) • Spousal Refusal 6

7

Community Medicaid Application Procedures • This is a two (2) prong application: • Financial Eligibility and Medical Eligibility • Prepare and file application • Submit and process application • After receiving the acceptance, evaluations to be done • 1 st evaluation – MAXIMUS Conflict Free Assessment • 2 nd evaluation – MLTC to determine hours • If using a pooled trust, submit first overage payment and supply DSS with a verification of deposit to have coverage changed in the system 8

9

Additional Forms for Community Medicaid • Immediate Need forms (16 ADM-02) • Expedited process to get home care in place. DSS has 7 days to process a Medicaid application when it is complete and DSS must conduct an evaluation for services no later than 12 days after the receipt of a completed application. • HIPAA release • State Disability Review forms • Accepted Pooled Trust Joinder Agreement 10

11

Preparing the Application • Keep separate folders for different documents (ex: vitals, residency, income, resources (can even break this down further) • Have your client continue to send updated bank statements during the entire process • Fill out application forms and start to draft the cover letter to DSS • Remember that coverage can be dated back three months from date of application, not including the month the application is filed, so long as the A/R is eligible. 12

Reviewing Financial Statements • Make sure you have all of the statements for the five (5) year look-back period • Practice Tip: If you are filing a conversion application, the lookback period starts on the 1 st day of the month that the applicant enters the facility, not when the application is filed. 13

Reviewing Financial Statements • You should be tracking the statements before submitting the application to Medicaid. Track all deposits and track all withdrawals (threshold amount is $2, 000. 00) and patterned withdrawals • If you find deposits and withdrawals, ask client for back-up documentation (withdrawal slips, deposit slips, canceled checks, etc. ) 14

Reviewing Financial Statements • You should also be cognizant for transfers from other bank accounts. Medicaid will ask who these belong to! 15
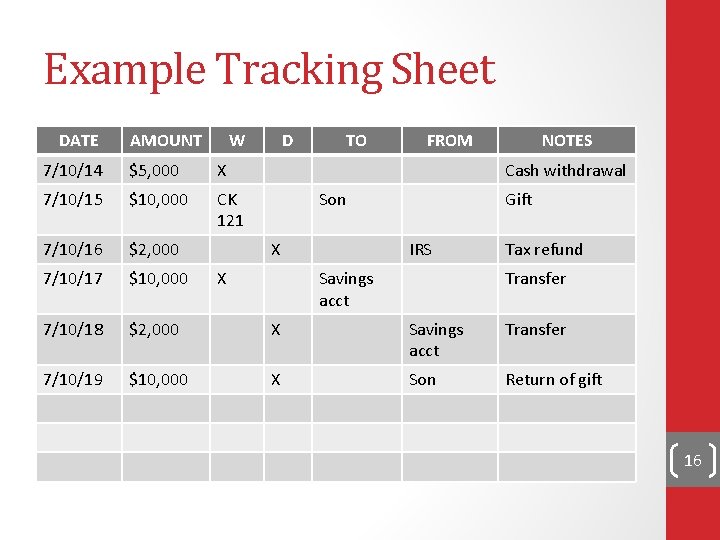
Example Tracking Sheet DATE AMOUNT W D TO FROM NOTES 7/10/14 $5, 000 X Cash withdrawal 7/10/15 $10, 000 CK 121 7/10/16 $2, 000 7/10/17 $10, 000 7/10/18 $2, 000 X Savings acct Transfer 7/10/19 $10, 000 X Son Return of gift Son X X Gift IRS Savings acct Tax refund Transfer 16

Filing the Application • Make sure you keep your own copy of the application you are submitting to Medicaid. • File the application with the appropriate county. These can be mailed, couriered or hand-delivered. • Have the county acknowledge that the application was received. If hand delivered, you will bring your own copy of the cover letter and have the county mark it “RECEIVED” with the date. If mailing, use certified return receipt or a delivery confirmation for courier delivery. • DSS is obligated to render a decision within forty-five (45) days. If you have not heard from a caseworker within that time frame, call DSS and ask for an update. 17

Processing of the Application (Pends) • You will most likely receive a Document Request from the assigned caseworker asking for updated or further documentation. Make sure you diary the due date because the documents are usually due back within ten (10) days! • You may request an extension of time from the caseworker. The first request for an extension should always be granted. Further requests will have to be supported with proof of your attempts to secure the documentation. You can always ask for more than 10 days, just explain why you need more time. • You also have the option to request a Collateral Investigation from DSS to help try to obtain documentation, however, you must prove to Medicaid that you cannot get the documentation (letter from bank, etc. ) 18

Notice of Decision • When your case has been processed, DSS will issue a Notice of Decision. It will either ACCEPT or DENY the application. • This Notice of Decision will also have an effective date, the CIN number and the budget. You should review the notice for accuracy. • If you have questions about the Notice of Decision or need a revision made, you can contact the caseworker. It is always best practice to send a request in writing. • The Notice of Decision will also include appeal rights. If a post -decision appeal is necessary, you have 60 days to request it from the notice date. 19

Post-Decision Appeals • Reconsideration • Must be made within 30 days of the notice date • Re-application • This will affect the pick-up date • Fair Hearing • Administrative Hearing • Article 78 • Special Proceeding through the courts • Must exhaust Fair Hearing remedy first 20

Practice Tips • Create a checklist of documentation required for filing an application that you can share with the client • Create a questionnaire that the client completes • Create a template detailing all of client accounts (open and closed), income details • Have the client sign an authorization for 3 rd parties so that you may contact them on the client’s behalf • Have the client sign the application forms at one of the first meetings • Diary deadlines (ex: application to be filed by, etc. ) • Memorialize conversations with clients, 3 rd parties (financial institutions, DSS, etc. ) • Keep in contact with the nursing home. Some nursing homes have hired collection agencies – do not disclose financial information to them. 21

Resources • GIS (General Information System) & ADM (Administrative Directives) available on New York State Department of Health Website • Medicaid Reference Guide • Fair Hearing Archive database • NYLAG (New York Legal Assistance Group) • NYSBA Elder Law listserv • Colleagues • Department of Social Services / Caseworker 22
- Slides: 22