Medicaid Managed Care Initiatives December 2011 Medicaid Service

Medicaid Managed Care Initiatives December 2011

Medicaid Service Delivery Models • STAR • Capitated, Health Maintenance Organization (HMO) model for non-disabled pregnant women and children. • Provides acute care services. • STAR+PLUS • Capitated HMO model for disabled Medicaid clients and dual eligibles (Medicaid and Medicare). • Provides acute and long term services and supports (LTSS). 2

Medicaid Service Delivery Models • STAR Health • Capitated HMO model for foster care children. • Provides acute care services with emphasis on behavioral health and medication management. • Primary Care Case Management (PCCM) • Non-capitated service delivery model. • Includes non-disabled pregnant women, children and disabled adults. • Acute care services only. 3

Medicaid Managed Care Initiatives • Expand STAR+PLUS to South Texas. • Expand STAR+PLUS to El Paso and Lubbock service areas. • Convert PCCM Areas to the STAR Program model. • Include In-patient Hospital Services in STAR+PLUS. • Include pharmacy benefits in managed care. • Expand Dental Managed Care Model for children in Medicaid. Page 4
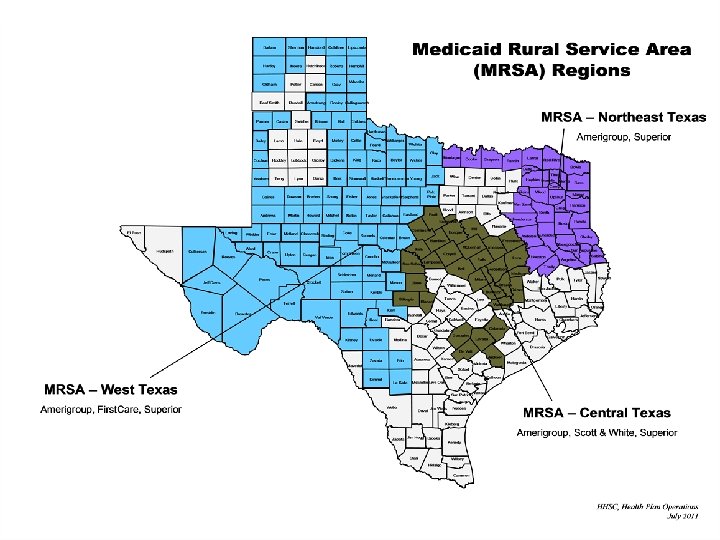
STAR+PLUS Managed Care Service Areas 5
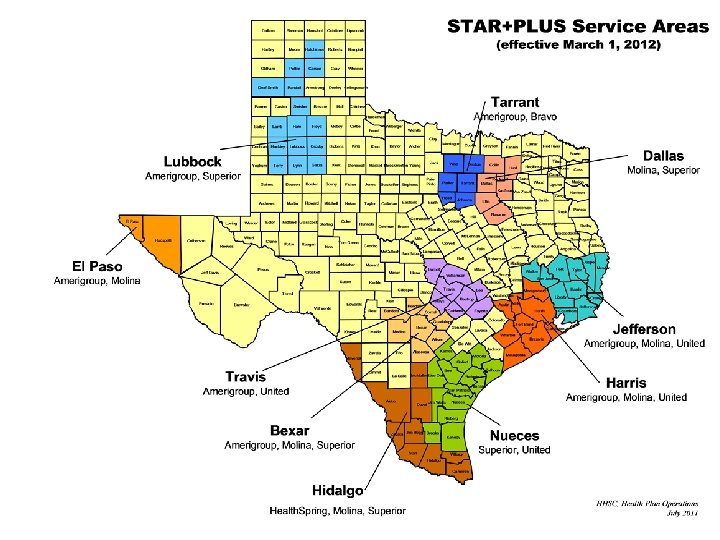
STAR+PLUS Managed Care Service Areas 6
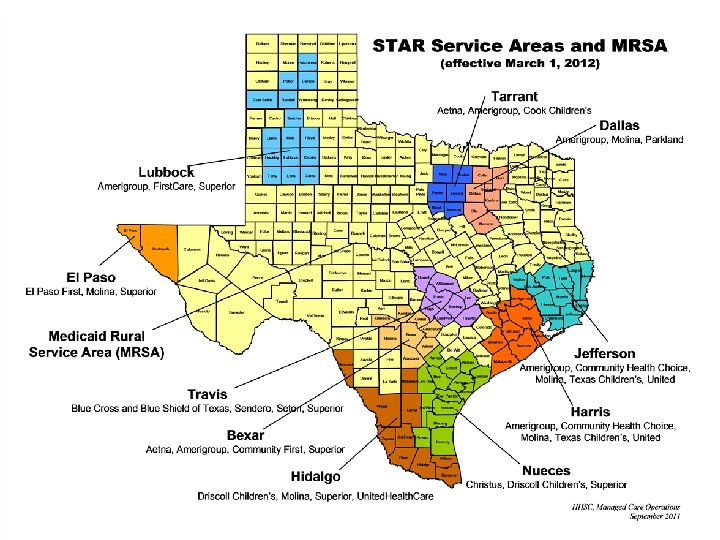
Geographic Distribution of Managed Care Delivery Models Page 7

HMO Member Benefits • Traditional Medicaid benefit package. • Provider directories – physicians, specialists, and LTSS. • PCP to coordinate health care of patient (Medicaid only). • Member services helpline (through their health plan). • Member handbooks and health education. • Service Coordination. • Value Added Services – vary by health plan.

STAR Members • Populations mandatory for STAR include: Ø Temporary Assistance to Needy Families (TANF) recipients Ø Pregnant Women Ø Children receiving Medicaid assistance only • Populations excluded from STAR include: Ø Medicaid recipients who reside in institutions Ø Medicaid recipients receiving Supplemental Social Security (SSI) Ø Dual-eligible Medicaid recipients (clients with both Medicaid and Medicare) Ø Medically needy Ø Foster children Ø Refugees • Medicaid Rural Service Area: Ø Children age 20 and younger can choose to join STAR if they receive SSI but do not receive Medicare. Page 9

STAR+PLUS Members • Medicaid recipients who must participate in STAR+PLUS: Ø SSI adults who are not: • Residing in a Nursing Facility or other institution. • Being served through a Home and Community Based Waiver program other than Community Based Alternatives (CBA). Ø Non-SSI adults who qualify for 1915(c) Nursing Facility Waiver services must enroll in STAR+PLUS to receive those services. • Medicaid recipients who can choose to participate in STAR+PLUS: Ø SSI children, under age 21, may voluntarily enroll in STAR+PLUS. SSI children that do not volunteer will be in traditional Medicaid effective March 1, 2012. 10

Managed Care vs. FFS Ø State operated plan. Ø Providers are contracted directly with state. Ø Providers paid fee-for-service (FFS) rates. Managed care Ø Providers must contract and be credentialed with the health plan to provide services. Ø Rates are negotiated between the provider and the MCO or DMO. Page 11

PCCM vs. Managed Care Organizations Primary Care Case Management (PCCM) Ø State operated plan. Ø Providers are contracted directly with state. Ø Members assigned PCP, but can see any Medicaid specialist. Ø Providers paid fee-for-service (FFS) rates. Medicaid Managed Care Organizations Ø Providers must contract and be credentialed with the MCO to provide STAR services. Ø Rates are negotiated between the provider and the MCO. Page 12

Significant Traditional Providers • Significant Traditional Provider (STP) requirements relate to providers that have been providing services to Medicaid clients in some service areas. • MCOs are obligated to offer STP contractors the opportunity to be a part of the contracted MCO provider network. • MCOs will reach out to contact STPs; however, STPs may initiate the contact. • STP providers must accept MCO conditions for contracting and pass credentialing.

Public Health Coordination • The MCO must make good faith effort to enter into a subcontract for covered services with public health entities. • Services covered by public health entities may include: Ø Ø Sexually transmitted diseases Confidential HIV testing Immunizations Tuberculosis care

MCO Contract Requirements: Immunizations • MCOs must educate providers on the following: Ø Standard requirements in • • Chapter 161 of the Health and Safety Code ACIP Immunization Schedule AAP Periodicity schedule for CHIP members Texas Health Steps Periodicity schedule for Medicaid members. Ø The screening provider is responsible for administration of immunizations and should not refer children to local health departments for immunizations. Ø Compliance with Imm. Trac requirements, including parental consent on the Vaccine Information Statement.

Enrollment Broker • Client Welcome letters/FAQs: • Dental – September 2011 • Medical – November 2011 • Client Enrollment packets: • Dental – November 2011 • Medical – December 2011 through January 2012 • Clients must enroll by February 10, 2012 or the state will assign a plan and main doctor. Page 16

Enrollment Broker • Enrollment Options • Fill out the forms and mail them back. • Call the Help Line and sign up by phone. Ø 1 -800 -964 -2777 • Attend a client outreach and enrollment event. • Client outreach and enrollment events – November 2011 through February 2012 • www. txmedicaidevents. com Page 17

Managed Care Operations HHSC Managed Care Operations monitors the HMO performance quarterly for these key indicators: Ø Network Adequacy Ø Claims Processing time Ø Hotline Performance Ø Complaint processing Additional contract requirements and performance is also monitored on ongoing basis. Page 18

Provider Complaints • Initial point of contact is MCO or dental plan • May submit written complaint to HHSC at hpm_complaints@hhsc. state. tx. us • HHSC will intervene in issues when MCO is not complying with HHSC contract Page 19

Resources • HHSC Managed Care Proposals Webpage: http: //www. hhsc. state. tx. us/medicaid/mmc. shtml • TMHP Website: http: //www. tmhp/Pages/PCCM_Home. aspx • Email: Ø managedcare_exp 2012@hhsc. state. tx. us Ø managedcaredental@hhsc. state. tx. us 20

Questions?
- Slides: 21