Mediastinal Syndromes Barkum Hadi Zafira 01141113 Mukoro D

Mediastinal Syndromes Barkum Hadi Zafira 01141113 Mukoro D. Ese 01141011 Oyebode P. Ifeoluwa 01120580 Sobo A. Motunrayo 01130558

Definition The mediastinum is a broad central compartment of the thoracic cavity. It separates the two laterally placed pleural cavities, and is enclosed on each side by the mediastinal pleura. The mediastinum contains all of the thoracic viscera and structures except for the lungs. It also serves as a pathway for the esophagus, thoracic duct, and several components of the nervous system, allowing them to traverse through the thorax on their way to the abdomen.

Anatomy It is divided into superior and inferior mediastinum, the latter is further subdivided into anterior, middle and inferior mediastinum. Ø Superior: Begins at the level of the first rib and descends to the horizontal plane of T 4. It contains the lower ends of the sternohyoid, sternothyroid and longus colli muscles, thymus remnants, great vessels and veins, the trachea, the esophagus, related nerves and the thoracic duct, in addition to the paratracheal, brachiocephalic and tracheobronchial lymph nodes. Ø Anterior inferior: Starts from T 4 and continues to the diaphragm at the level of the T 9. It extends posteriorly from the body of the sternum and transversus thoracis muscle to the fibrous pericardium. It consists of loose connective tissue, fat, sternopericardial ligaments, a few lymph nodes, SVC, brachiocephalic veins and aortic arch. In some cases it may partially contain the thymus gland, or its degenerated remains.

Anatomy Ø Middle Inferior: It also begins at T 4 and ends between T 9 and T 10, It extends posteriorly from the body of the sternum and transversus thoracis muscle to the fibrous pericardium. it contains the pericardium, the heart, the tracheal bifurcation, both main bronchi, SVC, ascending aorta, pulmonary trunk, pericardiacoophrenic artery, right and left phrenic nerves, the deep part of the cardiac plexus, and the tracheobronchial lymph nodes. Ø Posterior Inferior: Originates from the same place as the others and ends at T 12. It runs from the posterior aspect of the fibrous pericardium to the vertebral column. Its major contents include the esophagus, the right and left vagi, the thoracic duct, the thoracic aorta, the azygos system of veins, the sympathetic trunk, the thoracic splanchnic nerves, and the posterior mediastinal lymph nodes.
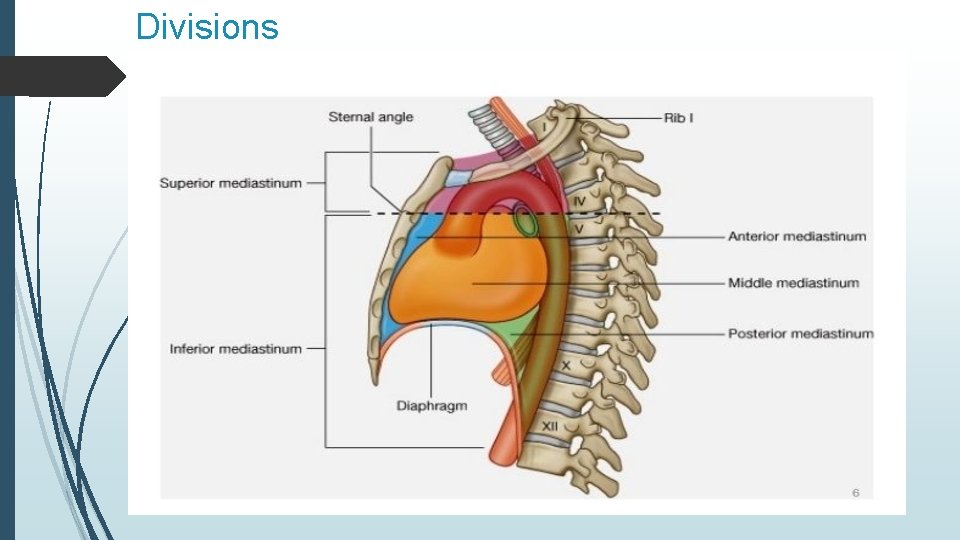
Divisions
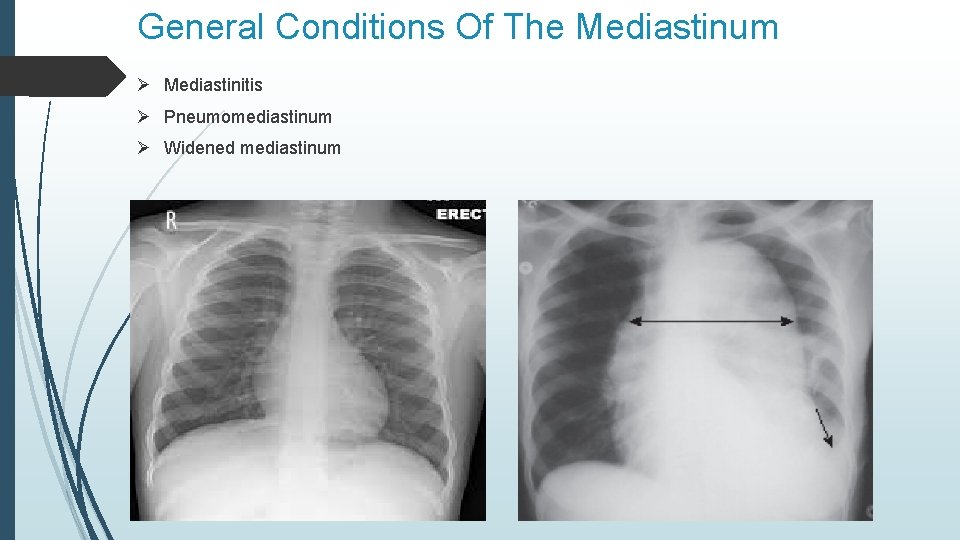
General Conditions Of The Mediastinum Ø Mediastinitis Ø Pneumomediastinum Ø Widened mediastinum

Mediastinitis Inflammation of the tissues in the midchest, may be acute or chronic. It usually occurs after cardiovascular surgery. • ACUTE: pre development of modern cardiovascular surgery this was usually caused by perforation of the esophagus or from the contiguous spread of odontogenic or retropharyngeal infections. Treated by aggressive IV antibiotic regimen and hydration. Collections of fluids (abscesses) have to be surgically drained or debrided. • Chronic: this is usually diagnosed by radiologic findings of diffuse fibrosis of the soft tissue of the mediastinum. This may be due to the presence of prior granulomatous disease e. g. histoplasmosis may also be due to TB and radiation therapy. This condition constricts the blood vessels and airways and results in conditions such as superior vena cava syndrome or pulmonary edema. Treatment is controversial and may include steroid use or surgical decompression of the affected vessels

Pneumomediastinum Abnormal presence of air or other gases in the mediastinum. May be as a result of physical trauma or other conditions that lead to air escaping from the airways or bowels into the chest cavity Symptoms include severe central chest pain, labored breathing, voice distortion, subcutaneous emphysema(face, neck and chest). It is recognized on auscultation by a crunching sound timed with the cardiac cycle (Hamman’s crunch) Diagnosis: is confirmed via chest x-ray showing radiolucent outline around the heart and mediastinum or via CT scanning of the thorax. Treatment: The tissues in the mediastinum will slowly reabsorb the air in the cavity so treatment is mainly conservative. Inhalation of high flow oxygen will increases the air absorption. In cases where the heart is under pressure needle decompression is indicated. If its due to a rupture in the esophagus or trachea, esophagus or bowel needs surgical repair

Widened Mediastinum • This diagnosis is made when the mediastinum has a width greater than 6 cm on an upright PA chest x-ray or 8 cm on a supine chest film. This may be as a result of: • Aortic aneurism • Aortic dissection • Aortic unfolding • Aortic rupture • Hilar lymphadenopathy • Esophageal rupture • Pericardial effusion • Thoracic vertebrae fractures • Anthrax inhalation

ANTERIOR INFERIOR MEDIASTINUM

Mediastinal teratomas • Mediastinal teratomas are germ cell tumors arising from ectopic pluripotent stem cells that failed to migrate from yolk endoderm to the gonad. By definition they should contain elements from all three embryological layers: endoderm, mesoderm and ectoderm. It located in the anterior mediastinum. It Usually occurs within or near the thymus gland. • It is associated with • Mature teratomas (well differentiated) have been associated with Klinefelter syndrome (47, XXY) • Immature teratomas (poorly differentiated) can be associated with • non-lymphocytic leukemia • pleomorphic undifferentiated sarcoma

Clinical presentation The majority of patients are asymptomatic, with the mediastinal mass discovered incidentally when the thorax is imaged for another reason Masses that become symptomatic can do so in a variety of ways: • Mass effect respiratory distress (infants), respiratory failure, superior mediastinal syndrome, neck mass, Horner syndrome • Endocrine function hormone production, e. g. beta-HCG, insulin • Rupture chest pain, hemoptysis, respiratory distress, cardiac tamponade, pleural effusions

Diagnosis and treatment • Mature teratomas and most immature teratomas are benign tumors, but still carry a risk of malignancy despite being indolent initially and require close clinical, serological, and radiological follow-up, or surgical excision. There is also a low incidence of malignant transformation of somatic cells (i. e. non germ cell components) within these tumors, e. g. carcinoma, sarcoma, leukemia. • Mature teratomas of the mediastinum should be completely surgically resected. The tumors may be adherent to surrounding structures. Necessitating resection of the pericardium, pleura or lung. When complete resection is achieved, we get long term cure with low rates of recurrence. When complete resection is impossible, partial resection often leads to symptom relief, frequently without relapse

Thymoma A thymoma is a tumor originating from the epithelial cells of the thymus that may be benign or malignant. It is the most common neoplasm of the anterior mediastinum, accounting for 20 -25% of all mediastinal tumors and 50% of anterior mediastinal masses. Its peak incidence occurs in the fourth and fifth decades of life; the mean age of patients is 52 years. No sexual predilection exists. Associations: As many as 30 -40% of patients who have a thymoma experience symptoms suggestive of Myasthenia Gravis. An additional 5% of patients who have a thymoma have other systemic syndromes, including red cell aplasia, dermatomyositis, systemic lupus erythematosus (SLE), Cushing syndrome, and syndrome of inappropriate antidiuretic hormone secretion (SIADH).

Pathology Thymoma originates from the epithelial cell population in the thymus, and several microscopic subtypes are now recognized. There are three principal histological types of thymoma, depending on the appearance of the cells by microscopy: Type A if the epithelial cells have an oval or fusiform shape (less lymphocyte count); Type B if they have an epithelioid shape (Type B has three subtypes: B 1 (lymphocyte-rich), B 2 (cortical) and B 3 (epithelial). ); Type AB if the tumor contains a combination of both cell types. Type C: thymic carcinoma Thymic cortical epithelial cells have abundant cytoplasm, vesicular nucleus with finely divided chromatin and small nucleoli and cytoplasmic filaments contact adjacent cells. Thymic medullary epithelial cells in contrast are spindle shaped with oval dense nucleus and scant cytoplasm thymoma if recapitulates cortical cell features more, is thought to be less benign.
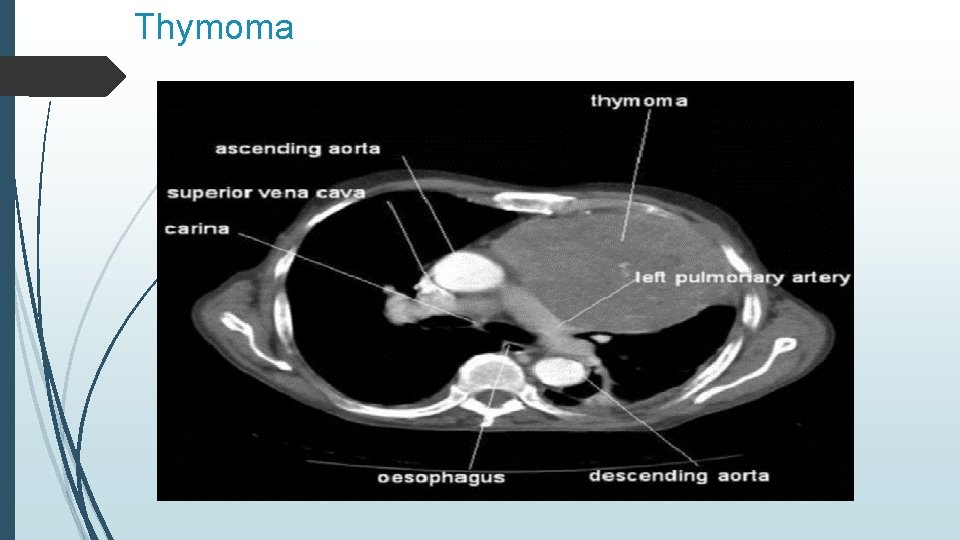
Thymoma

Clinical presentation and diagnosis
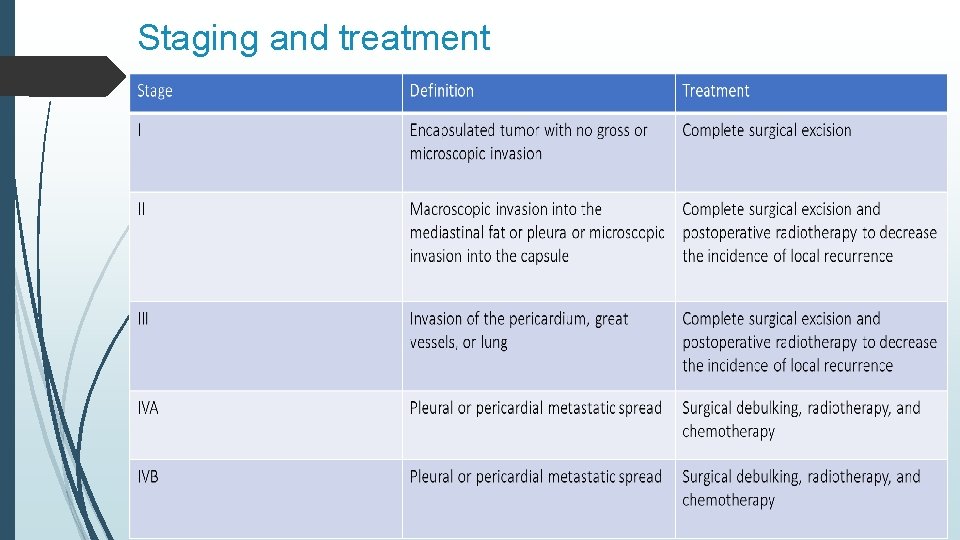
Staging and treatment

Parathyroid carcinoma is a rare malignancy of the parathyroid glands. These tumors usually secrete parathyroid hormone, thereby producing hyperparathyroidism, which is usually severe. Parathyroid carcinoma may be suspected, but it usually cannot be confirmed prior to operation It causes hyperparathyroidism in all but a few rare cases of nonfunctional parathyroid carcinoma. Hyperparathyroidism is caused by overproduction of parathyroid hormone. It is usually severe, with high serum calcium levels, severe bone disease, and renal stones. Rarely, parathyroid cancer can be nonfunctional, that is, it may cause a tumor but not produce parathyroid hormone and the sequelae of hyperparathyroidism. A large mass in the neck is often seen.

Diagnosis and Treatment
Superior vena cava syndrome are symptoms that occur when the blood flow through the superior vena cava is blocked or compressed. These symptoms include breathing problems, lightheadedness, and swelling in the upper part of the body It most often occurs as a complication of another medical issue, such a tumor or a swollen lymph node obstructing the flow of blood through the vein. Common causes include non Hodgkin lymphomas and lung cancer

Diagnosis and treatment

MEDIAL INFERIOR MEDIASTINUM

MIDDLE MEDIASTINAL 30% of mediastina masses are from the middle of the mediastinum Adenopathy: infection (bacterial, granulomatous), neoplasm (leukemia/lymphoma, metastasis) Bronchopulponary or foregut malformations: e. g. bronchogenic cysts and the likes

Bronchogenic cyst Bronchogenic cysts are the most common cystic lesions of the mediastinum. They are small, solitary cysts or sinuses, most typically located in the region of the suprasternal notch or over the manubrium q PATHOLOGY They are formed in the 6 th week of gestation from the abnormal budding of tracheal diverticulum. . They are lined by respiratory type (ciliated) epithelium which is characterized by cilia. . Histologically, these are composed of cartilage, smooth muscle, fibrous tissue and mucous glands. . The cysts originate from the ventral fore gut that forms the respiratory system. They are located in the trachea or main stem branch. . There is rarely communication of the cysts with the trachea bronchial tree

Cont CLINICAL PRESENTATION. they are found mostly in young adults and are rare in infancy. . usually symptoms are s a result of compression of the cyst e. g difficulty breathing, difficulty swallowing, cough, chest pain, recurrent infections, pneumothorax, esophageal compression. malignant degeneration has been recorded on rare occasions Ø INVESTIGATION. chest x-ray. CT scan q TREATMENT. excision biopsy-provides definitive diagnosis and has less surgical risk. observation-it provides minimal risk from the intervention but carries risk of bleeding or infection of the cyst and at a later time, it makes excision more difficult if it occurs
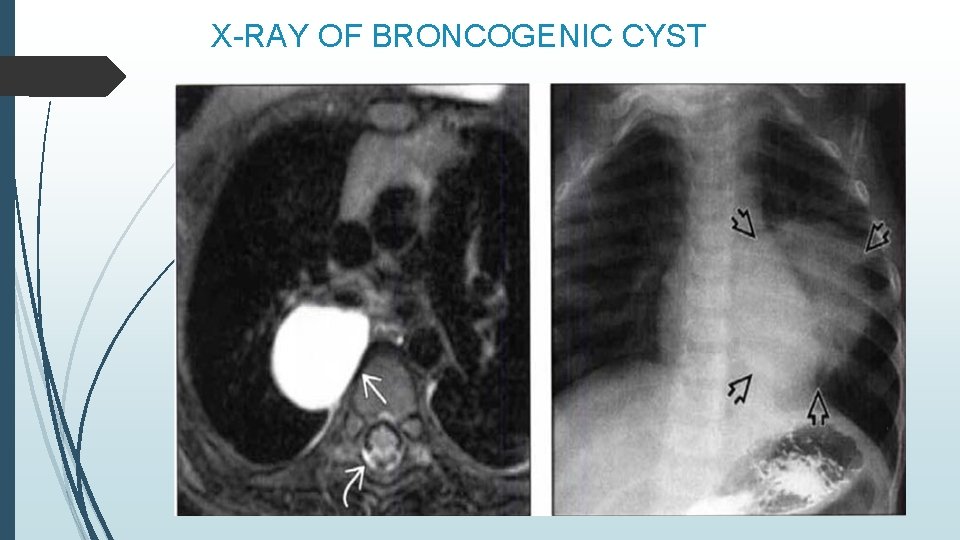
X-RAY OF BRONCOGENIC CYST

Pericardial cyst Cystic lesions within the pericardial space are very rare and are usually found in the 3 rd or 4 th decade of life and males and females are affected equally The are commonly congenital in origin and they arise from failure of fusion of one of the mesenchyme lacunae that form the pericardial sac. Inflammatory: rheumatic pericarditis, bacterial infections mostly particularly TB. Traumatic Post cardiac surgery CLINICAL PRESENTATION They are usually asymptomatic and the diagnosis is usually an incidental findings in chest x-ray. Symptoms may appear when the cyst compresses on a nearby structure. chronic cough Chest pain. dyspnea. Feeling of retrosternal pressure. palpitations. Recurring lower respiratory tract infections have also been described. Recurrent syncope

Cont. DIAGNOSIS. chest x-ray. CT scan is considered best for diagnosis. MRI. echocardiography. USS TREATMENT. conservative management is done with follow ups. Percutaneous aspiration and surgery. Thoracotomy and surgical resection this is a second line treatment.

MORGAGNI HERNIA It is a congenital diaphragmatic hernia and it is characterized by herniation through the foramen of morgagni. They are anterior and more right sided, they are small and rare. It is usually associated with. congenital heart diseases. trisomy 21 (down syndrome) They most often contain omental fat, but the transverse colon (60%) or stomach (12%) may be included within the hernia v CLINICAL PRESENTATION. only about 30% of patients are symptomatic. newborns may present with respiratory distress at birth. re-current chest infections and GI symptoms § TREATMENT . laparoscopic surgical repair even in asymptotic patients to reduce the risk of strangulation of the hernia contents.

NODULAR SCLEROSIS It is know as nodular sclerosis classical Hodgkin's lymphoma (NSCHL) and it is generally seen in teens and young adults q ETIOLOGY. the cause is usually unknown but in most cases, mutation of B lymphocytes is reported. This leads to enlargement of said lymphocytes causing them to block the lymphatic system. (genetic mutation) o CLINICAL FEATURES Pain in lymph nodes. loss of appetite. loss of weight. fatigue. itching. fever. excessive sweating

Cont DIAGNOSIS. physical exam. biopsy. Blood tests(FBC, blood chemistry). Imaging studies (chest x-ray, CT scan, MRI) ü TREATMENT. Radiation therapy. Chemo therapy

LYMPHOBLASTIC LEUKEMIA/LYMPHOMA It usually develops from the T lymphocytes but occasionally from B lymphocytes. These abnormal lymphocytes are present in the lymph nodes or thymus gland. affects adults under 35 but affects kids and teens mostly The cause is unknown ü CLINICAL FEATURES. patients usually present with painless swelling in the neck, armpit or groin this is cause by the enlarged lymph nodes. . a central chest lump may occur which can cause dyspnea or chest pain. . other body parts may be affected e. g thymus gland, liver, spleen, skin, testis and brain. . fatigue, loss of appetite and weight loss often occur. . in addition, drenching night sweats and unexplained fevers § TREATMENT . chemotherapy: it is done in 3 stages (induction, consolidation, maintenance)

POSTERIOR INFERIOR MEDIASTINUM

DISEASES AFFECTING THE POSTERIOR MEDIASTINUM • NEUROGENIC TUMORS • MEDIASTINAL (ENTERIC) CYSTS • BOCHDALEK HERNIA
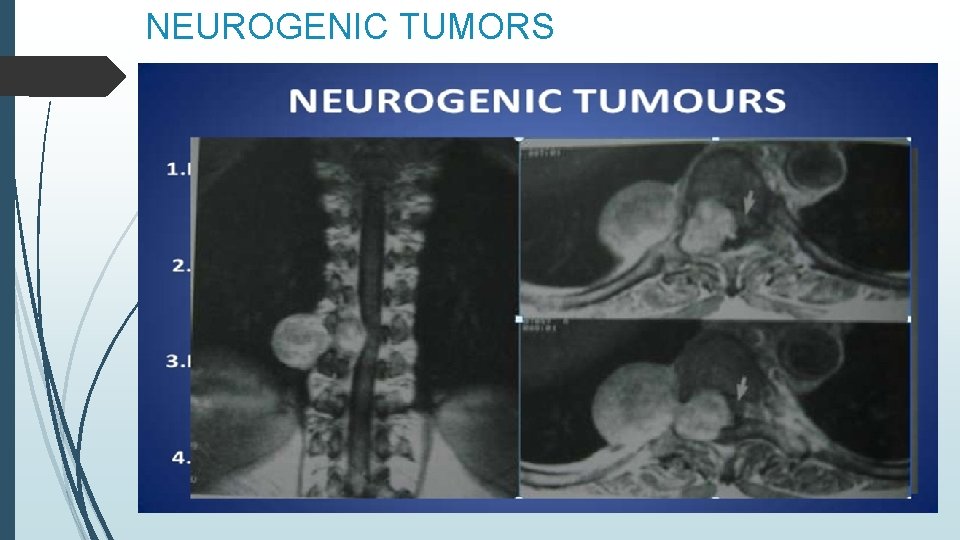
NEUROGENIC TUMORS

Clinical Presentation • Many mediastinal tumors and cysts produce no symptoms and are found incidentally during chest radiography or other imaging studies of the thorax performed for another reason. • Despite the rarity of symptoms, the following respiratory symptoms are bound to occur: • Cough • Dyspnea • Stridor • Chest pain and Weight loss (Malignancy)

Investigations and Treatment • INVESTIGATIONS: • Chest X-ray • Serum Assays • TREATMENT: • Surgical Resection

MEDIASTINAL (ENTERIC) CYSTS

Clinical Presentation • Cough • Dyspnea • Stridor • Fever • Malaise • Vague Chest Pain • DYSPHAGIA • SEPSIS

Investigation and Treatment • INVESTIGATIONS: • Chest X-ray • Chest CT • TREATMENT • Surgical resection • Aspiration
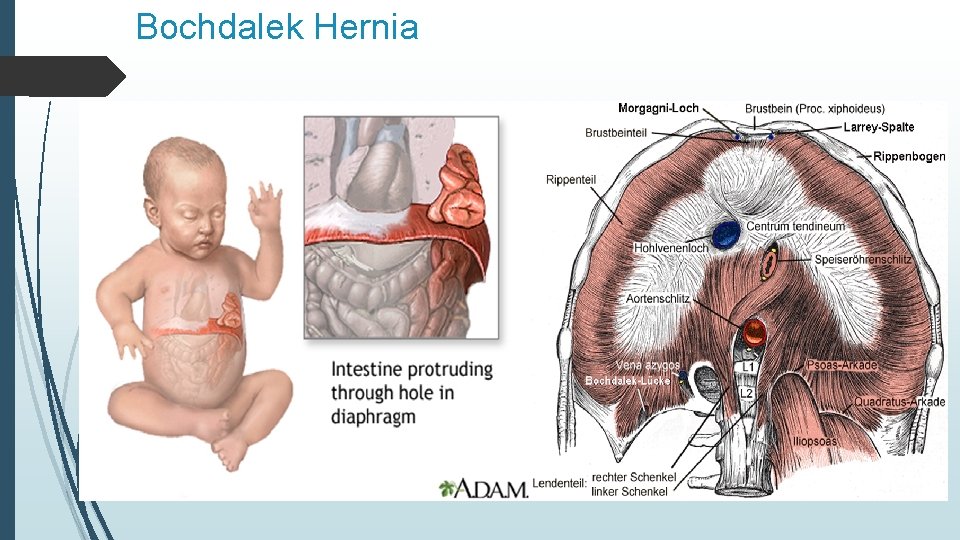
Bochdalek Hernia

Clinical Presentation • The symptoms are often observable simultaneously with the baby's birth. • They include difficulty breathing, fast respiration and increased heart rate. • Also, if the baby appears to have cyanosis, this can also be a sign. • Another way to differentiate a healthy baby from a baby with Bochdalek Hernia, is to look at the chest immediately after birth. If the baby has a Bochdalek Hernia it may appear that one side of the chest cavity is larger than the other and or the abdomen appears scaphoid.

Investigation and Treatment • INVESTIGATIONS: • Chest X-ray • PCR • TREATMENT: • Surgery

Other Notable Mentions • MEDIATINAL GERM CELL TUMOR: • Germ cell tumors occur most frequently in the gonad, but in rare cases, they occur in extragonadal locations, usually in or near the midline. • A variety of extragonadal germ cell tumors are known. • The mediastinum is the most common extragonadal location.

References • Mediastinum dictionary definition • Thoracic Wall, Pleura, and Pericardium – Dissector Answers Archived 2012 -09 -01 at the Wayback Machine. • Geusens; Pans, S. ; Prinsloo, J. ; Fourneau, I. (2005). "The widened mediastinum in trauma patients". European Journal of Emergency Medicine. 12 (4): 179– 184. doi: 10. 1097/00063110 -200508000 -00006. PMID 16034263. • Jump up ^ Richardson; Wilson, M. E. ; Miller, F. B. (1990). "The widened mediastinum. Diagnostic and therapeutic priorities". Annals of Surgery. 211 (6): 731– 736; discussion 736– 7. doi: 10. 1097/00000658 -19900600000012. PMC 1358125 reely accessible. PMID 2357135. • Jump up ^ Chandra S, Laor YG (April 1975). "Lung scan and wide mediastinum". J. Nucl. Med. 16 (4): 324– 5. PMID 1113190.
- Slides: 46