MEDIAL TIBIAL STRESS SYNDROME SHIN SPLINTS Dr Vernon

MEDIAL TIBIAL STRESS SYNDROME “SHIN SPLINTS” Dr. Vernon Morkel 1996482590

TABLE OF CONTENTS Introduction History Clinical Evaluation Special Investigations Three stage assessment Problem list formulation Plan and Progression Discussion

INTRODUCTION 26 y. o. male, rugby player – backline Plays rugby for fun, not very fit Bank clerk Smoker & social drinker No chronic medical conditions

HISTORY Came of rugby field during pre-season practice Intense pain – over both lower legs Started gradually during running exercise Has to stop running for relieve Flared up with increased exercise intensity Previous h/o ‘shin-splints’
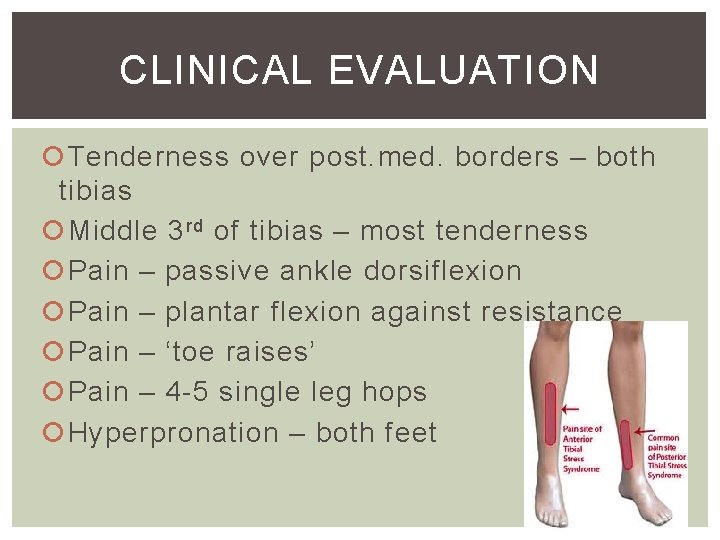
CLINICAL EVALUATION Tenderness over post. med. borders – both tibias Middle 3 rd of tibias – most tenderness Pain – passive ankle dorsiflexion Pain – plantar flexion against resistance Pain – ‘toe raises’ Pain – 4 -5 single leg hops Hyperpronation – both feet

SPECIAL INVESTIGATIONS None indicated None done

THREE STAGE SUMMARY 1. Clinical Medial Tibial Stress Syndrome (Shin Splints) Brought on – intense & repetitive running exercises 2. Personal Concerned – he frequently has to stop running or exercise – severe leg pain

THREE STAGE SUMMARY 3. Social Afraid – miss out on team selection Friends – ‘sissy’, for quitting exercise

PROBLEM LIST FORMULATION 1. Active Painful lower legs – Medial Tibial Stress Syndrome (Shin Splints) 2. Passive Preventing him from completing training sessions & matches General fitness deteriated

PLAN AND PROGRESSION Iced lower legs – initially Analgesia Recommended – 10 days rest from running Refer – innersoles to improve hyperpronation Physiotherapy Still in rest period & awaiting innersoles

DISCUSSION Definition Medial Tibial Stress Syndrome (MTSS) is defined as pain along the posteromedial border of the tibia that occurs during exercise, excluding pain from ischaemic origin or signs of stress fracture (Newman and Adams 2012).

DISCUSSION MTSS – one of the most common causes of exercise-related leg pain Running & walking activities – most frequently 16. 8% long distance runners 35% - military academies USA Females twice the risk then men Middle third mostly, then lower third of tibia
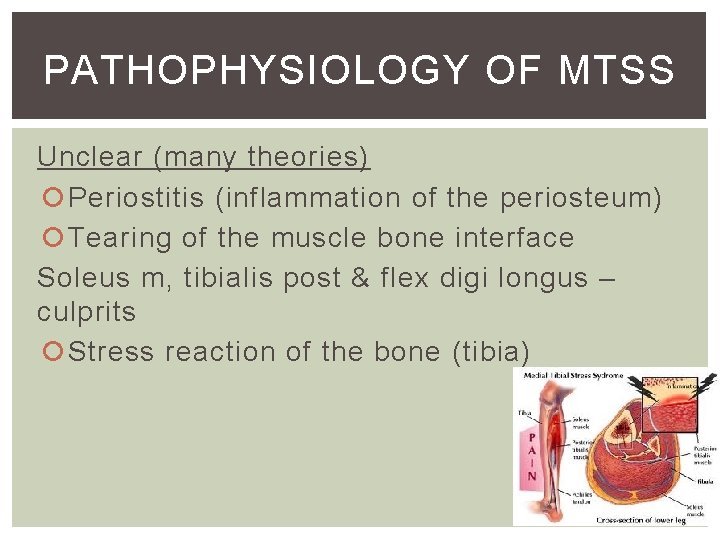
PATHOPHYSIOLOGY OF MTSS Unclear (many theories) Periostitis (inflammation of the periosteum) Tearing of the muscle bone interface Soleus m, tibialis post & flex digi longus – culprits Stress reaction of the bone (tibia)
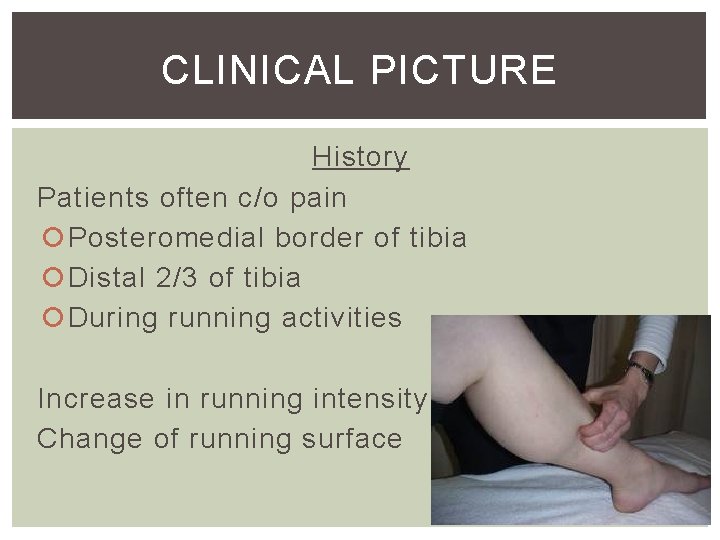
CLINICAL PICTURE History Patients often c/o pain Posteromedial border of tibia Distal 2/3 of tibia During running activities Increase in running intensity Change of running surface
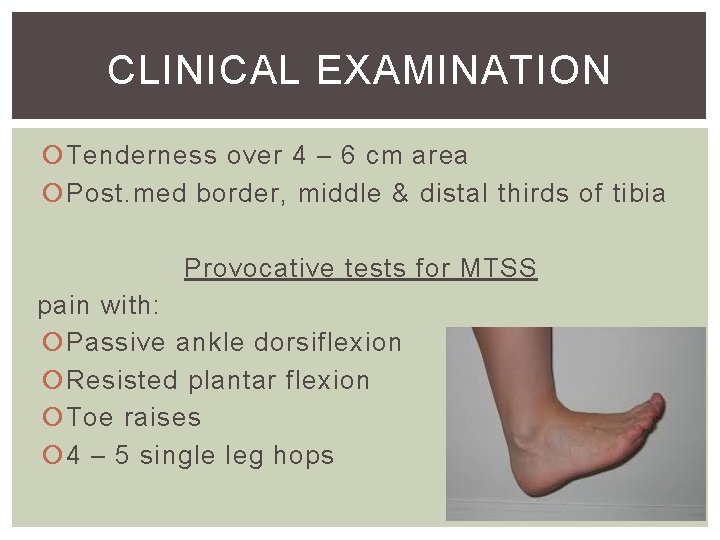
CLINICAL EXAMINATION Tenderness over 4 – 6 cm area Post. med border, middle & distal thirds of tibia Provocative tests for MTSS pain with: Passive ankle dorsiflexion Resisted plantar flexion Toe raises 4 – 5 single leg hops

RISK FACTORS FOR MTSS abrupt increase in training activities inadequate shoes hard or inclined running surfaces previous MTSS female gender increased BMI

RISK FACTORS FOR MTSS (2) increased foot pronation increased varus tendency of the forefoot and/or hind foot hip internal or external rotation increased muscular strength of plantar flexors

DIFFERENTIAL DIAGNOSIS Stress fractures of the tibia – caused by repetitive loading with resulting microfracture Chronic exertional Compartment syndrome – is a condition of increased pressure in the fascial compartments of the leg

DIFFERENTIAL DIAGNOSIS (2) Peripheral Nerve entrapment – most often caused by trauma, the common peroneal, superficial peroneal and saphenous nerves are most commonly at risk for entrapment Popliteal artery entrapment syndrome – is an uncommon overuse injury, frequently caused by compression of the popliteal artery by surrounding musculotendinous structures as it exits the popliteal fossa (Brewer and Gregory 2012 )

SPECIAL INVESTIGATIONS X-rays – rarely positive early on. X-rays performed 2 to 3 weeks after onset of pain may reveal periosteal reaction or a radiolucent line (stress fracture) Radio isotopic bone scan – can confirm the presence of MTSS or a stress fracture MRI scan – is the investigation of choice for lower leg pain MRI arteriograph – can confirm popliteal artery syndrome
TREATMENT OPTIONS Rest for 7 to 10 days from painful activities Icing Analgesia for pain relieve Stretching of calf musculature Strengthening of calf musculature Activity modification Orthotics or inner soles to correct foot hyperpronation

TREATMENT MODALITIES (2) Extracorporeal Shock Wave Therapy (ESWT) – is a new treatment modality for MTSS. Rompe et al (2010) used low-energy ESWT to treat MTSS. After 15 months 76% of the treatment group were able to return to their sport symptom free, compared to only 37% of the control group. This study showed that low-energy ESWT is safe and effective to treat MTSS

TREATMENT MODALITIES (3) Bisphonates (currently used for treatment of osteoporosis) – Moen at el (2011) administered bisphonates to two athletes diagnosed with chronic MTSS. Both athletes returned to their sport in a much shorter time. These case reports raise the possibility that bisphonates could decrease the time to return to sport in MTSS patients. Surgery – only for very severe cases of shin splints that do not respond to conservative treatment. However the effectiveness of surgery remains unclear.
PREVENTION MEASURES Shock-absorbent insoles Pronation control insoles (specifically controlling navicular drop) Graduated running programs Correcting training errors: – like an abrupt increase in training activity -Changing to a harder training surface

LEARNING EXPERIENCE Abruptly increasing training activities, changing running surfaces and inadequate shoes – ‘shin splints’, correcting these factors and rest are important to manage the condition.

REFERENCES 1. Brewer, RB. , et al, 2012. Chronic lower leg pain in athletes: A guide for the differential diagnosis, evaluation and treatment. Sports Health, 4(2), 121 -127 2. Brukner & Khan, 2012. Clinical Sports Medicine, 4 th ed, NSW, Australia, Mc. Graw - Hill 3. Craig, DI. , 2008. Medial Tibial Stress Syndrome: Evidence-Based Prevention. Journal of Athletic Training, 43(3), 316 -318 4. Loudon, JK. , 2010. Use of foot Orthoses and Calf Stretching for individuals with Medial Tibial Stress Syndrome. Foot & Ankle Specialist, 3(1), 15 -20 5. Moen, MH. , 2011. The treatment of medial tibial stress syndrome with bisphonates. Sport & Geneeskunde, 1, 22 -25 6. Newman, P. , 2012. Two simple clinical tests for predicting onset of medial tibial stress syndrome: shin palpation test and shin oedema test. British Journal of Sports Medicine, 1 -5 7. Rompe, JD. , et al, 2010. Low-Energy Extracorporeal Shock Wave Therapy as a treatment for Medial Tibial Stress Syndrome. The American Journal of Sports Medicine, 38(1), 125 -132 8. Yates, B. , 2004. The Incidence and Risk Factors in the development of Medial Tibial Stress Syndrome among Naval Recruits. The American Journal of Sports Medicine, 32(3), 772 -780

THANK YOU Dr. VERNON MORKEL vmorkel@iway. na
- Slides: 27