Mechanisms of intervention to reduce proteinuria Biomarkers beyond

Mechanisms of intervention to reduce proteinuria & Biomarkers: beyond proteinuria Jeffrey Kopp, MD Kidney Disease Section NIDDK, NIH
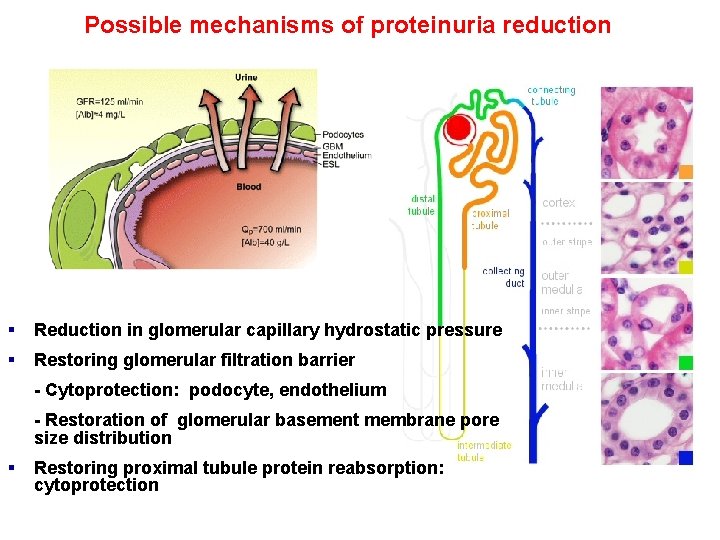
Possible mechanisms of proteinuria reduction § Reduction in glomerular capillary hydrostatic pressure § Restoring glomerular filtration barrier - Cytoprotection: podocyte, endothelium - Restoration of glomerular basement membrane pore size distribution § Restoring proximal tubule protein reabsorption: cytoprotection
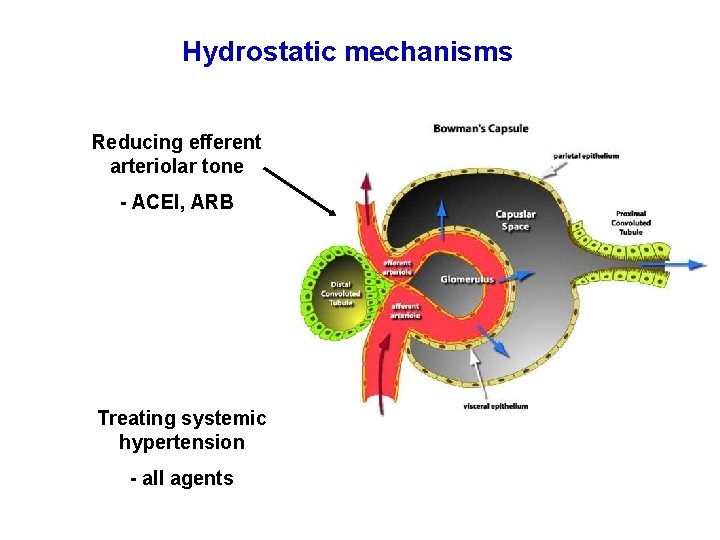
Hydrostatic mechanisms Reducing efferent arteriolar tone - ACEI, ARB Treating systemic hypertension - all agents
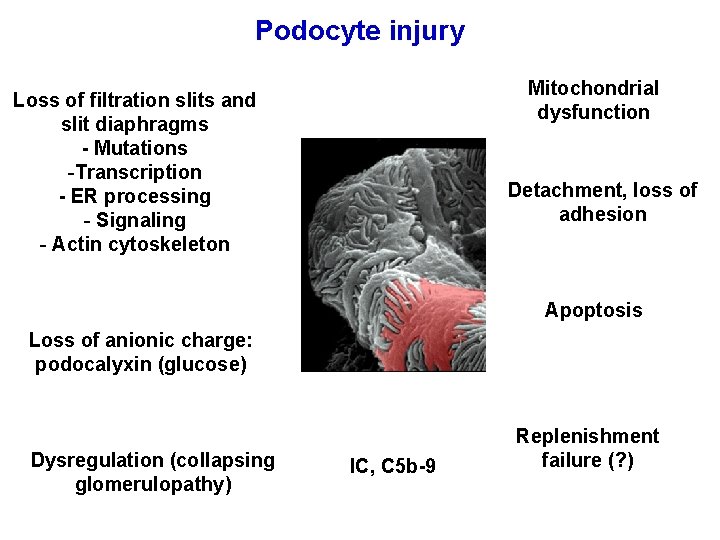
Podocyte injury Mitochondrial dysfunction Loss of filtration slits and slit diaphragms - Mutations -Transcription - ER processing - Signaling - Actin cytoskeleton Detachment, loss of adhesion Apoptosis Loss of anionic charge: podocalyxin (glucose) Dysregulation (collapsing glomerulopathy) IC, C 5 b-9 Replenishment failure (? )

Protecting and restoring podocyte phenotype Glucocorticoids -Transcription - Actin stabilization Ransom KI 2005 - Anti-apoptotic Preventing IC deposition Mizoribine - Transport from ER via energetics Nakajo JASN 2007 Wada JASN 2005 - Transport from ER Fuji KI 2006 Cyclosporine Retinoids -reverse FPE - nephrin, podocin Vaughan KI 2005
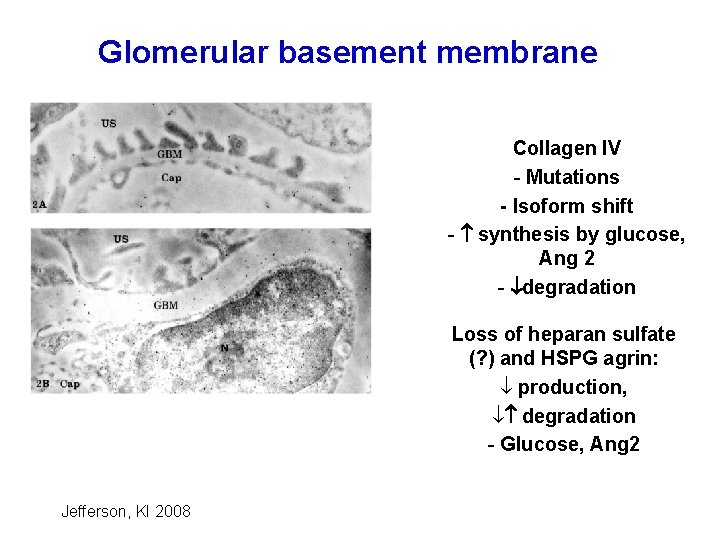
Glomerular basement membrane Collagen IV - Mutations - Isoform shift - synthesis by glucose, Ang 2 - degradation Loss of heparan sulfate (? ) and HSPG agrin: ¯ production, ¯ degradation - Glucose, Ang 2 Jefferson, KI 2008
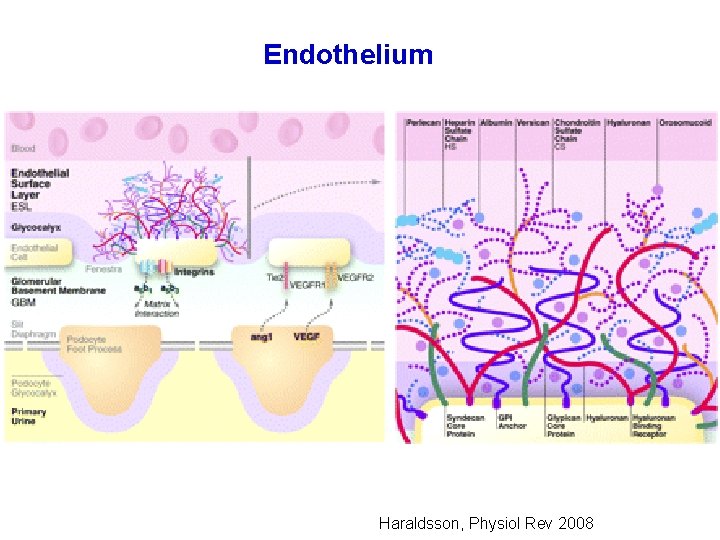
Endothelium Haraldsson, Physiol Rev 2008
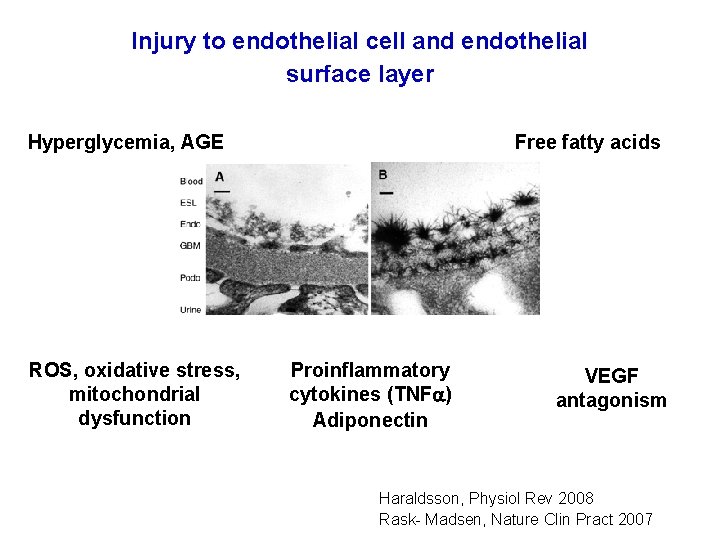
Injury to endothelial cell and endothelial surface layer Hyperglycemia, AGE ROS, oxidative stress, mitochondrial dysfunction Free fatty acids Proinflammatory cytokines (TNF ) Adiponectin VEGF antagonism Haraldsson, Physiol Rev 2008 Rask- Madsen, Nature Clin Pract 2007

Pima diabetics: Macroproteinuria but not microproteinuria is associated with shunt Macro Micro § Shunt magnitude correlates with FPE Lemley, JASN 2000
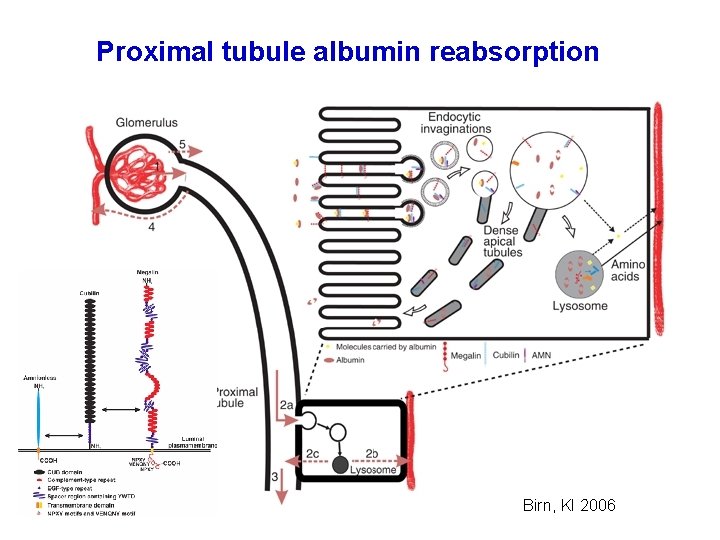
Proximal tubule albumin reabsorption Birn, KI 2006

Impaired albumin reabsorption by proximal tubule in PAN nephrosis 0 40 s 14 min CON PAN Russo, KI 2007
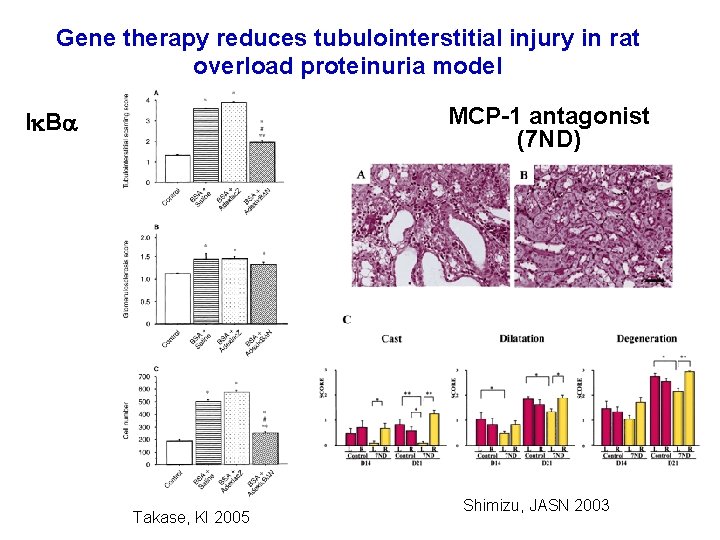
Gene therapy reduces tubulointerstitial injury in rat overload proteinuria model MCP-1 antagonist (7 ND) I B Takase, KI 2005 Shimizu, JASN 2003

Does macroalbuminuria cause tubulointerstitial damage? Pro § Overload albuminuria models § Exposure to albumin (or cytokines of FA on albumin) induces RANTES, MCP-1, IL 8, fractalkine, TNF- , ET, TGF- ; alters integrins, may induce apoptosis § Other proteins: iron carriers, complement, Ig, growth factors § Gene therapy to PTC (MCP-1 reduction, I B) protects Con § Minimal change nephropathy: proteinuria for years without progression § Role of selectivity
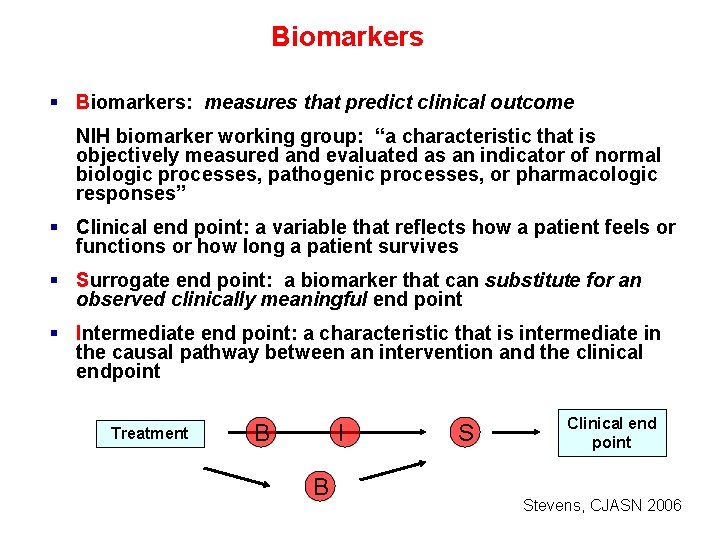
Biomarkers § Biomarkers: measures that predict clinical outcome NIH biomarker working group: “a characteristic that is objectively measured and evaluated as an indicator of normal biologic processes, pathogenic processes, or pharmacologic responses” § Clinical end point: a variable that reflects how a patient feels or functions or how long a patient survives § Surrogate end point: a biomarker that can substitute for an observed clinically meaningful end point § Intermediate end point: a characteristic that is intermediate in the causal pathway between an intervention and the clinical endpoint Treatment B I B S Clinical end point Stevens, CJASN 2006

Biomarkers in drug development and use § Pre-clinical/animal Clinical studies: identify pathways Animal studies: screening for leads, rank candidates § Clinical studies Identify pathways Early detection Differential diagnosis, identify subpopulations Prognosis § Surrogate end point for trials Assess drug effect, dose-ranging, more efficient trial design § Clinical therapy: drug dosing Hewitt, JASN 2004
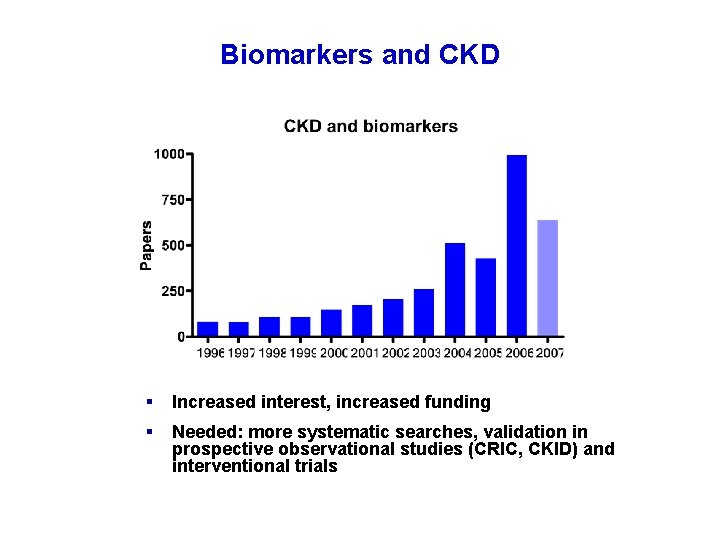
Biomarkers and CKD § Increased interest, increased funding § Needed: more systematic searches, validation in prospective observational studies (CRIC, CKID) and interventional trials
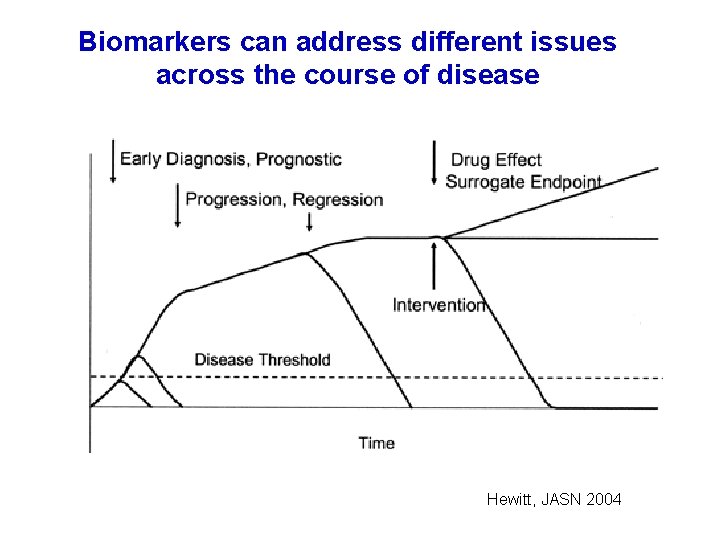
Biomarkers can address different issues across the course of disease Hewitt, JASN 2004
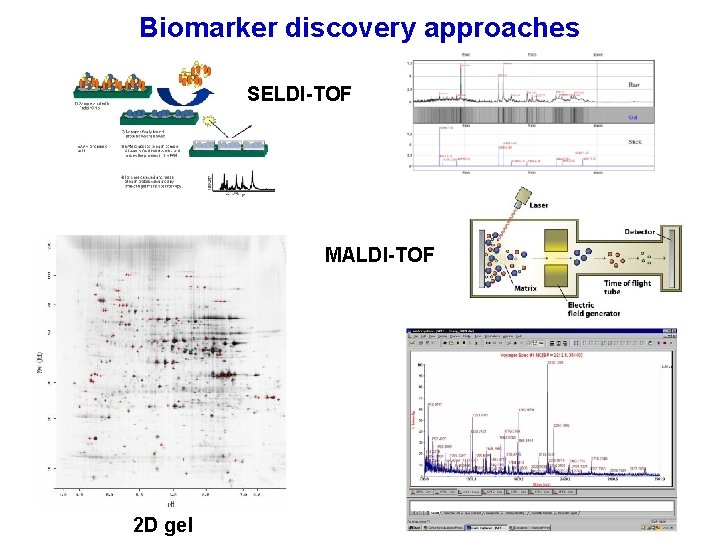
Biomarker discovery approaches SELDI-TOF MALDI-TOF 2 D gel
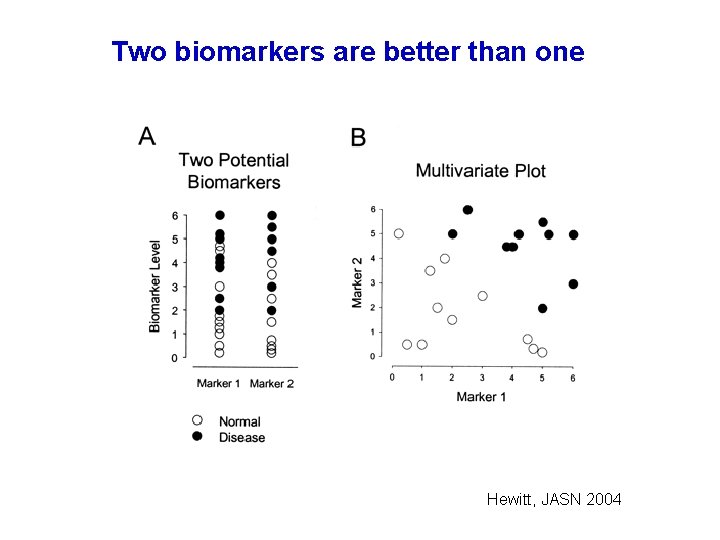
Two biomarkers are better than one Hewitt, JASN 2004
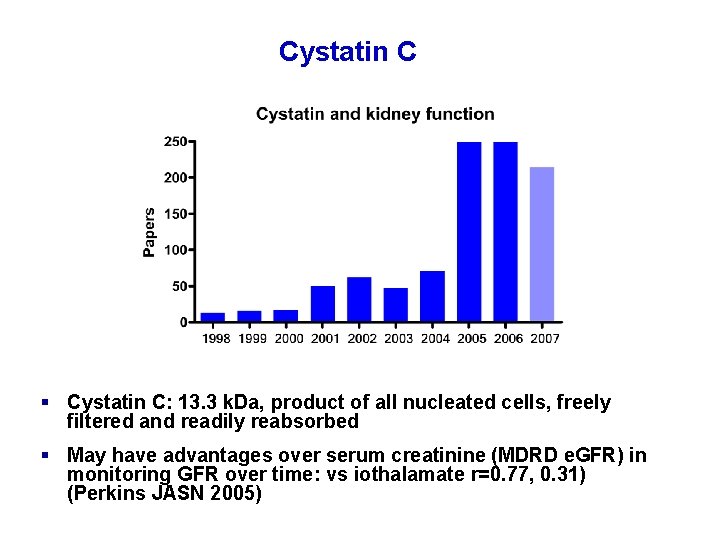
Cystatin C § Cystatin C: 13. 3 k. Da, product of all nucleated cells, freely filtered and readily reabsorbed § May have advantages over serum creatinine (MDRD e. GFR) in monitoring GFR over time: vs iothalamate r=0. 77, 0. 31) (Perkins JASN 2005)
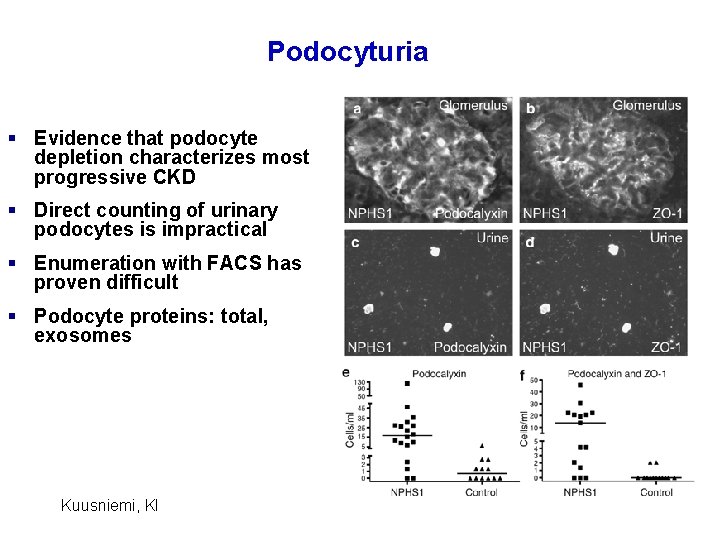
Podocyturia § Evidence that podocyte depletion characterizes most progressive CKD § Direct counting of urinary podocytes is impractical § Enumeration with FACS has proven difficult § Podocyte proteins: total, exosomes Kuusniemi, KI
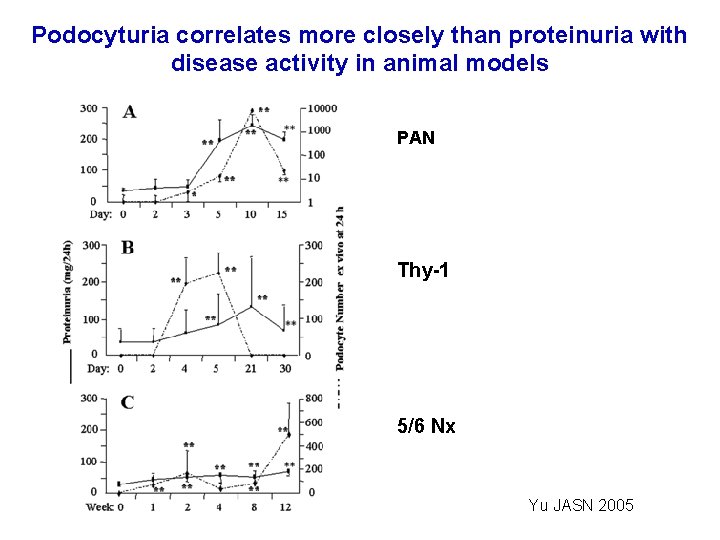
Podocyturia correlates more closely than proteinuria with disease activity in animal models PAN Thy-1 5/6 Nx Yu JASN 2005
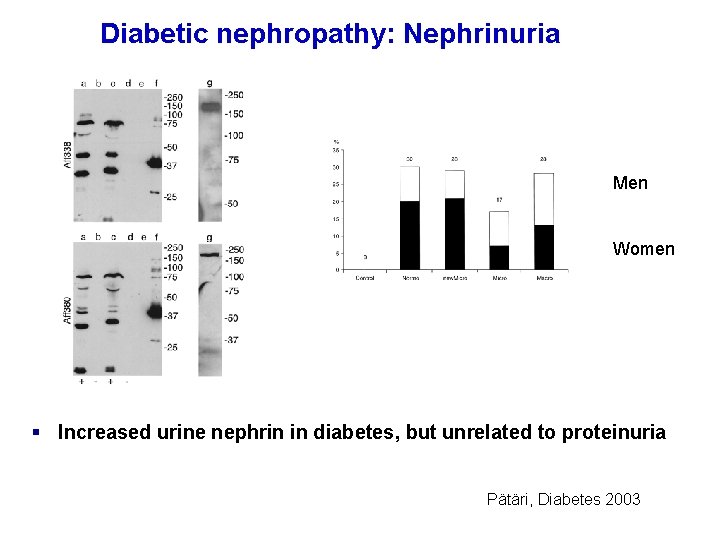
Diabetic nephropathy: Nephrinuria Men Women § Increased urine nephrin in diabetes, but unrelated to proteinuria Pätäri, Diabetes 2003
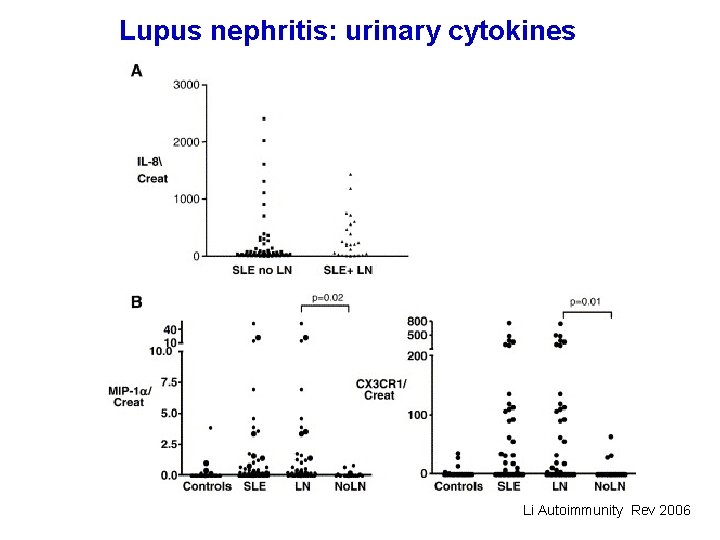
Lupus nephritis: urinary cytokines Li Autoimmunity Rev 2006
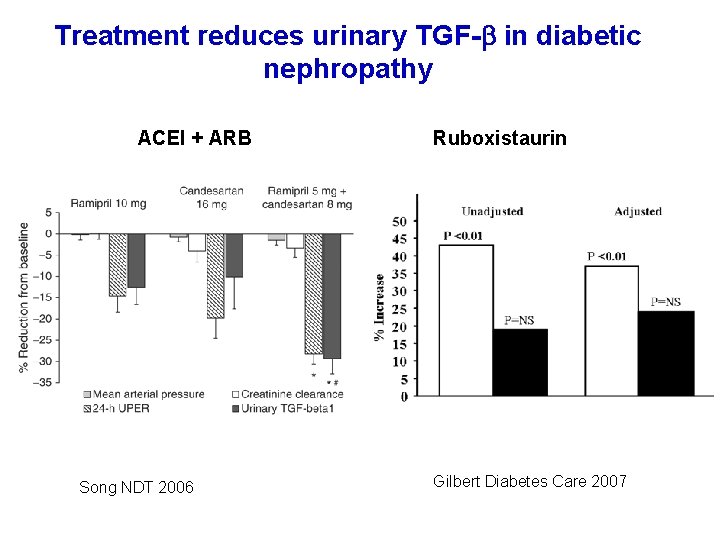
Treatment reduces urinary TGF- in diabetic nephropathy ACEI + ARB Song NDT 2006 Ruboxistaurin Gilbert Diabetes Care 2007
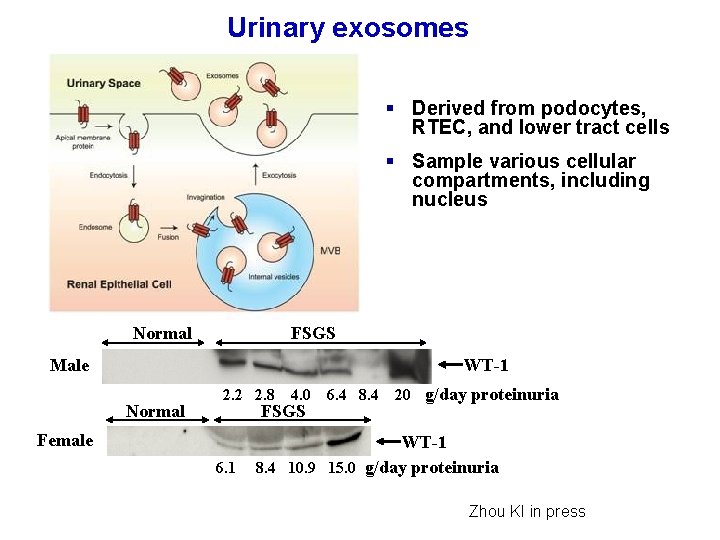
Urinary exosomes § Derived from podocytes, RTEC, and lower tract cells § Sample various cellular compartments, including nucleus Normal FSGS WT-1 Male Normal 2. 2 2. 8 4. 0 FSGS Female 6. 1 6. 4 8. 4 20 g/day proteinuria WT-1 8. 4 10. 9 15. 0 g/day proteinuria Zhou KI in press
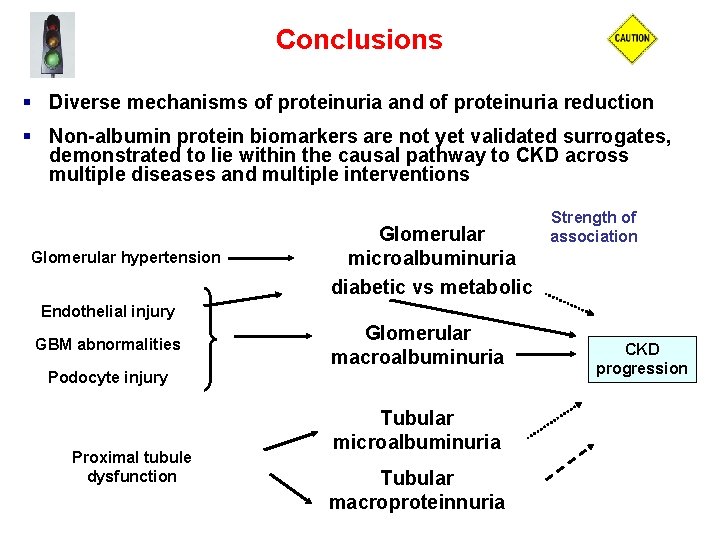
Conclusions § Diverse mechanisms of proteinuria and of proteinuria reduction § Non-albumin protein biomarkers are not yet validated surrogates, demonstrated to lie within the causal pathway to CKD across multiple diseases and multiple interventions Glomerular hypertension Glomerular microalbuminuria diabetic vs metabolic Strength of association Endothelial injury GBM abnormalities Glomerular macroalbuminuria Podocyte injury Proximal tubule dysfunction Tubular microalbuminuria Tubular macroproteinnuria CKD progression

- Slides: 28