Mechanical Ventilation Presented by Jacob Riegelsberger BS LP

Mechanical Ventilation Presented by: Jacob Riegelsberger BS, LP, CCEMT-P, FP-C

Mechanical Ventilation Ø The use of external equipment and supplies to assess, assist and/or artificially control a patient’s ventilatory cycle (Inhalation and Exhalation). Ø Can be invasive (IVPP) or non-invasive (NIPPV) and employ the following accouterments: q Ventilator Machine (e. g. LTV 1200) q Ventilator circuit/tubing q ETT/Trach. q Pressure cuff monitors q HME q Waveform capnography

Indications for & Benefits of Mechanical Ventilation Ø Frees up healthcare providers for other tasks Ø Grants complete or partial control of Airway & Breathing with ability to assess and regulate the overall process. q Oxygenation q Off-gassing (Et. CO 2) q Measure Pressures and Volumes q Strict Metabolic requirements q Hypoxic & Hypercapneic Respiratory failure q Post PAI w/ extended transport times (> 10 min) Ø Real time assessment, measurement and calculation of ventilation status (PIP, PEEP, Pplat, Ve, Vte, etc…) w/ consideration to trending and interventions!!!

Cautions & Considerations w/ Mechanical Ventilation Ø Age and severity of patient – older or sicker leads to greater challenge when weaning from ventilator q Muscle atrophy and loss of drive to breathe. q Severe pathologies require more time on the vent, can lead to other pathologies (e. g. VAP) Ø Decreases Cardiac Output (CO) by INCREASING intrathoracic pressure. Ø Hypovolemia (i. e. dehydration through respiratory cycle) q HME (Heat & Moisture Exchanger) q Adequate Fluid admin / Fluid Resuscitation Ø ***PPV is NOT intrinsic*** q Does not reflect the natural breathing process (e. g. neg pressure ventilation). q Harmful to Anatomy (barotrauma and volutrauma, shearing force) q Alters physiology (Oxgen Free Radicals/breakdown of tissues)

~Not All Ventilators are Created Equal~ Ø The principles of Mechanical Ventilation are the same regardless of the device used, but consider the limitations of each device respectively: q Rescue Ventilators – small/lightweight, very limited capabilities, used in remote or pre-hospital settings. Usually only offer Vt, f and I time settings. No alarms available. Dynamic airway pressures and other information (Vte, PIP, Pplat, Flow (LPM)), etc. . . not obtainable. q Hospital Ventilators – reliable and capable, controlled by RRT with MD order, not always compatible w/ prehospital equipment or vent. circuits. Values can be additive or absolute. q Pre-hospital Ventilators – Specific for transport arena. Must be rated for aviation use by manufacturer. Must be mounted/secured per FAA regulations.

Mechanical Ventilation: Common Terms and Variables Ø PIP – Peak Inspiratory Pressure - a measure of airway resistance during inspiration. q Normal is <30 cm. H 20 Ø Pplat – Plateau Pressure – a measure of static pressure in the lungs at the level of the alveoli at end-inspiration. q Better predictor of alveolar/Paw and is BEST for monitoring lung compliance and prevention of Barotrauma. q Normal is <30 cm. H 20

Terms and Variables cont… Ø PIPs and Pplats: v An elevated PIP with normal Pplat = an airway issue (mucous plug/secretions, obstructed ETT, bronchospasm, aspiration etc…) v An elevated Pplat with normal PIP = a lung parenchyma issue (Pulmonary Embolism) v If BOTH are elevated consider: Pleural effusion, abd. Distention/diaphragmatic rupture, pneumothorax, pulmonary edema, severe infection

More on Airway Resistance & PIP u. Causes of Increased Airway Resistance (i. e. High PIP) Type Condition COPD Emphysema Bronchitis Bronchiectasis/Atelectasis Mechanical Obstruction Mucous plug ETT clamping/pt. biting ETT Gen. Obstruction (fluid or foreign body Infection Pneumonia Sepsis w/ ARDS Reactive/Restrictive Asthma Cystic Fibrosis Bronchospasm (Allergic Rxn)

Terms and Variables cont… Ø PEEP – Positive End Expiratory Pressure – q The minimal pressure maintained during exhalation. Best for oxygenation and gas exchange & “Recruitment” q Prevents patient from completely exhaling which keeps alveoli open, while increasing surface area for continued gas exchange and maintaining Mean Airway Pressure (MAP). q Important for understanding Henry’s Law and Graham’s Laws and the solubility of gases!!! Intrinsic PEEP = 3 -5 cm. H 20 [FOR PTs OF ANY AGE] Extrinsic PEEP = > 5 cm. H 20 PEEP > 8 cm. H 20 REQUIRES ETT clamping or loss of recruitment WILL occur IMMEDIATELY!

PEEP continued… q “Auto PEEP-ing” – generated by patient with pursed lips, cough or other expiratory reflex. Aimed at increasing intrinsic PEEP in presence of pathological state. (e. g. COPD = pursed lips, exacerbated cough reflex, to splint open dynamic airways (e. g. bronchi/bronchioles) and alveoli for better gas exchange **BALLOON EXERCISE** q Excellent for: q Asthma, COPD, Emphysema, Bronchitis, CHF, Pulmonary Edema or ANY patient who requires increased gas exchange.

PEEP Continued… q Great for: q Asthma q COPD q Emphysema q Bronchitis q CHF q Pulmonary Edema q or ANY patient who requires increased gas exchange. q Caution with: q Pneumothorax q Late stage/severe Asthma or COPD q Diaphragmatic rupture q Traumatic asphyxiation or crush injuries.

Terms and Variables continued… Ø PS – Pressure Support – augments the flow of gas to help patient overcome the negative pressure of the vent. circuit when taking a spontaneously generated breath q Can be used in NIPPV (Bi. PAP) or IPPV (SIMV mode only) q Normal is 5 -15 Cm. H 20 (Typical is 10 cm. H 20) Ø Ve – Minute Volume – total volume of gas moved in and out of the pulmonary system each minute. [ f x Vt = Ve ] q Normal 4 -8 LPM Ø Vt – Tidal Volume – the total volume of gas inhaled with each breath (patient generated or ventilator) q Normal 6 -10 ml/kg q *Based on IBW*

Terms and Variables continued…. again Ø Bias Flow – the basal flow rate ALWAYS flowing through the vent. circuit to assist with patient triggering. q Normal 0 -40 lpm (LTV manuf. setting of 10 lpm) q Ensures MAP and that CO 2 doesn't accumulate in the inspiratory limb upon patient exhalation. q A lower bias flow is the reason PS must be used. That way patients can more easily inhale and overcome the negative pressure of the vent. circuit. Ø I: E Ratio – Inspiratory and Expiratory phase. q Ex. 1: 6 = 1 part inhalation to 6 parts exhalation. q “Inverted I: E ratios” increase MAP and oxygenation q Is considered a last ditch maneuver - can have deleterious effects!!!

Continued…. aaaaagain Ø Sensitivity – a provider controlled setting that determines the difficulty level for a patient to generate a spontaneous breath. q Ranges from 1 to 9 (1 = Easier, 9 = Near Impossible) q Typical = 3 q Important for rough transports or patients in AC mode. Ø Oxygen Concentration (expressed as. or %) q Room air Fi. O 2. 21 = 21% q Low Pressure Source (E Cylinder) = 100% q High Pressure Source 21% to 100% and everything in between (e. g. . 50 or. 40 or. 60 = 50%, 40%, 60% resp. )

Terms and Variables cont… Ø I-Time – Inspiratory Time – q The duration of time it takes for a target to deliver a breath. Longer I-Times contribute to recruitment and mean Mean Airway Pressure(Paw) Patient Duration in Seconds Adult 0. 8 – 1. 5 Pedi 0. 6 – 0. 8 Infant 0. 4 – 0. 5 Neonate 0. 3 – 0. 4 �Example – VLV – takes 0. 8 seconds to deliver 500 Vt (adult) �Example – PVL – takes 0. 4 seconds to deliver 20 cm. H 20 PIP (infant)

Special Notes & Considerations cont… Ø Lung Compliance Vs. Lung/Chest Wall Elastic Resistance q Compliance – a measure of the lung/chest wall’s ability to expand = “distensibility” � (High vs. Low) Based on airway resistance, lung parenchyma, alveolar surface tension, presence (or absence of) of pulmonary surfactant � {High} = Easier to ventilate | {Low} = more difficult to ventilate q Elastic Resistance “Elasticity or Elastance” – lung and chest wall recoil – a measure of the ease with which lung and chest wall return to their normal resting position/size. � Based on chest wall, alveolar surface tension, and integrity of lung connective tissue/fibers/proteins. � {High} = more difficult to ventilate | {Low} = Easier to ventilate

Compliance vs. Elasticity cont… Compliance and Elasticity are reciprocal forces (i. e. there is a certain pressure change required for a unit volume change.

Compliance and Elasticity cont… Ø Compliance DECREASES as Elasticity INCREASES � Obesity � Emphysema (lack of pulmonary Surfactant) � Chest Wall Restriction (e. g. Circumferential burns, traumatic asphyxiation/crush injuries) Ø Compliance INCREASES as Elasticity DECREASES � � Bronchitis, Asthma Allergic Rxn Infection (e. g. Pneumonia) Cystic Fibrosis � SPECIAL CONSIDERATIONS – Pulmonary Edema/Pneumothorax/ARDS/Toxic Exposure, Electrical Injuries/burns, severe COPD, or only one lung…. q Example: Asthma patient = distended lungs and chest wall = High compliance as lungs expand easily, but low elasticity due to inability to return to resting position from air trapping. ** Late cases we see both low compliance and low elasticity w/ TLC reached = inability to expand lungs further, or recoil lung/chest** q Example: Circumferential thermal burns to torso = low compliance as lungs don’t easily due to high elastic forces from: internal swelling, fluid shifts, increased alveolar surface tension and burned integument (skin) restricting chest excursion.

Final Notes & Considerations cont… Ø Oxygenation -Fi. O 2 and PEEP q Exercise Henry's Law (solubility of gases). � Surface Area � Pressure on top of the gas � Gas concentration q Utilizing PEEP increases surface area of the alveoli and encourages gas exchange at the alveolar/capillary interface q By providing an Fi. O 2 >. 21 (> 21%) we increase the concentration of the gas being infused. q Graham's Law - the law of diffusion states: � 1. ) the larger the gradient the faster molecules diffuse and � 2. ) the shorter the distance the faster the molecules diffuse. � Larger molecules diffuse more slowly, and ALL molecules will diffuse slower if being placed into a viscous solution (e. g. water VS. oil, honey or maple syrup, or BLOOD

Three Main Principles of Mechanical Ventilation Ø Trigger - A Trigger is what initiates a breath based on a set schedule per minute (i. e. Modes: CMV, AC, IMV, SIMV, PSV, Oscillation, etc. ) Ø “Dictates the pattern of mechanical and patient generated breaths” Ø Target - A Target is what each ventilation is aiming to achieve (i. e. deliver a breath to a preset volume or preset pressure or total flow ‘lpm’). Ø “How the breath is given” Ø Cycle - A cycle is what stops the ventilation cycle (i. e. when the preset volume or pressure is achieved) Ø “How the breath stops”

Mechanical Ventilation: Target A Target is what each ventilation cycle is aiming to achieve (i. e. deliver a breath to a preset volume or preset pressure) Ø Comes in two flavors: q Volume – � “Volume Limited Ventilation / Volume Targeted Ventilation / Volume Cycled Ventilation”…. . all mean the same thing! � Ventilator breath delivers gas until a present tidal volume has been achieved. Example: Vt of 500 ml q Pressure – � “Pressure Limited Ventilation / Pressure Targeted Ventilation / Pressure Cycled Ventilation”…. . all mean the same thing! � Ventilator breath delivers gas until a preset pressure has been achieved. Volume varies due to airway resistance and lung compliance. Example: PIP of 20 cm. H 2 o

Targets continued… Ø Volume Targeted Ventilation – q Mechanical breath administered is in the form of a preset tidal volume (Vt) q Pressure becomes the DEPENDENT variable as the total pressure experienced (PIP and Pplat) depends on the total volume administered, airway/lung compliance and chest wall elasticity. Check vent for relative pressures. q Considerations: q ALI and Volutrauma, Hx of Pulmonary bleps or spontaneous pneumothorax, ARDS, History of Lobectomy, known or suspected tension pneumothorax MUST watch pressure(s) in volume target setting!!!!

Targets continued… Ø Pressure Targeted Ventilation – q Mechanical breath administered in the form of a preset pressure (PIP) q Has added benefit of “decreasing –or- decrescendo” flow type. q Volume becomes DEPENDENT variable as any volume could be infused as long as the preset pressures are being reached. q Best for Lung Protective Strategy: Cystic Fibrosis, Asthma, COPD pathologies, Pneumonia. ARDS, Upper airway, neck, or anterior/posterior or circumferential thoracic burns leading to tissue swelling or restricted chest excursion. q Must be cautious with pressure as it can lead to under ventilating the patient if preset/desired airway pressures are achieved too early and thus not allowing for enough volume to be administered (e. g. asthma) Leads to a Low Minute Ventilation MUST watch volumes in Pressure Target setting!!!

Mechanical Ventilation: Trigger Ø A Trigger is what initiates a breath based on a set schedule per minute. Ø Breaths initiated by: q Ventilator Time (e. g. setting f and Vt) v Example: Rate (f) of 10 BPM = 1 breath ~ q 6 seconds v Example: Rate (f) of 12 BPM = 1 breath ~ q 5 seconds q Spontaneous Patient-Generated Breaths v In the spontaneously breathing patient, a patient-generated breath may/may not trigger the ventilator v SIMV – Pressure Support (PS) is used v AC – full volume breath is administered v Comes in different Modes: v CMV, AC, IMV, SIMV, PSV, CPAP, Bi. PAP, Oscillation

Mechanical Ventilation Modes Ø Controlled Mandatory Ventilation (CMV) q Trigger - Time q Target - VTV or PTV q Provides a present tidal volume (Vt) or Pressure (PIP) at a preset rate (f) q Patient is UNABLE to exhibit effort or spontaneously breathe around ventilator breaths. Leads to “air hunger” in the under -sedated patient. q Requires generous use of analgesia, sedation & NMBA! q Common w/ older model vents. and Rescue Ventilators q Ideal for: pts who require strict physiologic monitoring (ICP, TBI, SAH) and lower metabolic demand.

Mechanical Ventilation Modes Ø A/C – Assist Control q Trigger – Time or Patient q Target – VTV or PTV q Provides a present tidal volume (Vt) or Pressure (PIP) at a preset rate (f) and allows the pt. to take a breath BUT the breath will be ASSISTED and ultimately provided by the ventilator (e. g. the pt starts to breath they get a fullon ventilator breath at preset volume or pressure setting) q Requires analgesia, sedatives and possibly NMBA q Can lead to respiratory alkalosis, gas retention and breath stacking if pt. not allowed to exhale.
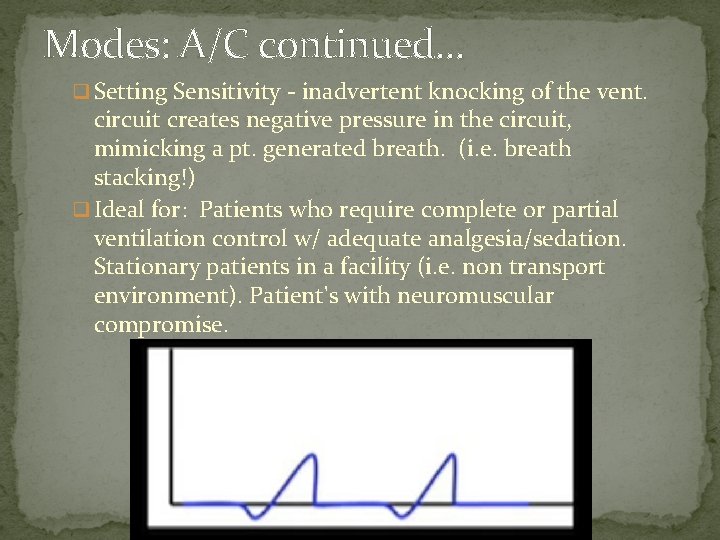
Modes: A/C continued… q Setting Sensitivity - inadvertent knocking of the vent. circuit creates negative pressure in the circuit, mimicking a pt. generated breath. (i. e. breath stacking!) q Ideal for: Patients who require complete or partial ventilation control w/ adequate analgesia/sedation. Stationary patients in a facility (i. e. non transport environment). Patient's with neuromuscular compromise.

Mechanical Ventilation Modes Ø IMV – Intermittent Mechanical Ventilation q Trigger – Time or Patient q Target – VTV or PTV q Provides a present tidal volume (Vt) or Pressure (PIP) at a preset rate (f) and allows the pt. to take a spontaneously generated breath in between ventilator breaths. **Is an Asyncrhonous Mode ** q Pt. generated breaths are un-assisted, and therefore may vary in Vt (e. g. 50 ml or 400 ml) q Leads to variable Vt delivery and WOB. q MUST have PS set!!! We want to help them breathe when taking breaths on their own! Can lead to “air hunger” and "bucking of the tube” if PS not set or analgesia/sedatives not used. q IMV may lead to air trapping, breath stacking and gas retention.
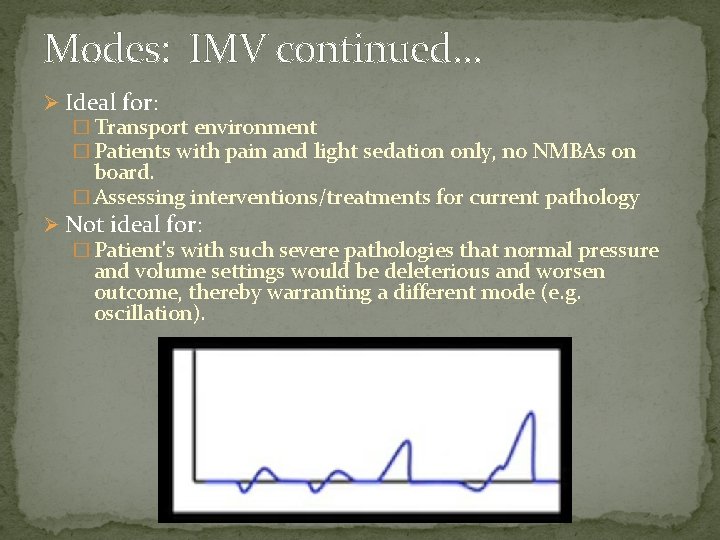
Modes: IMV continued… Ø Ideal for: � Transport environment � Patients with pain and light sedation only, no NMBAs on board. � Assessing interventions/treatments for current pathology Ø Not ideal for: � Patient's with such severe pathologies that normal pressure and volume settings would be deleterious and worsen outcome, thereby warranting a different mode (e. g. oscillation).

Mechanical Ventilation Modes Ø SIMV – Synchronized Intermittent Mechanical Ventilation q **BEST for the critically ill and injured** q Trigger – Time or Patient q Target – VTV or PTV q Provides a present tidal volume (Vt) or Pressure (PIP) at a preset rate (f) and allows the pt. to take a spontaneously generated breath in between ventilator breaths. q Pt. generated breaths are un-assisted, and therefore may vary in Vt (e. g. 50 ml or 400 ml) q MUST have PS set!!! We want to help them breathe. Can lead to “air hunger” and "bucking of the tube” if not. q Can lead to air trapping, breath stacking and gas retention. q Same benefits and cautions as IMV mode.
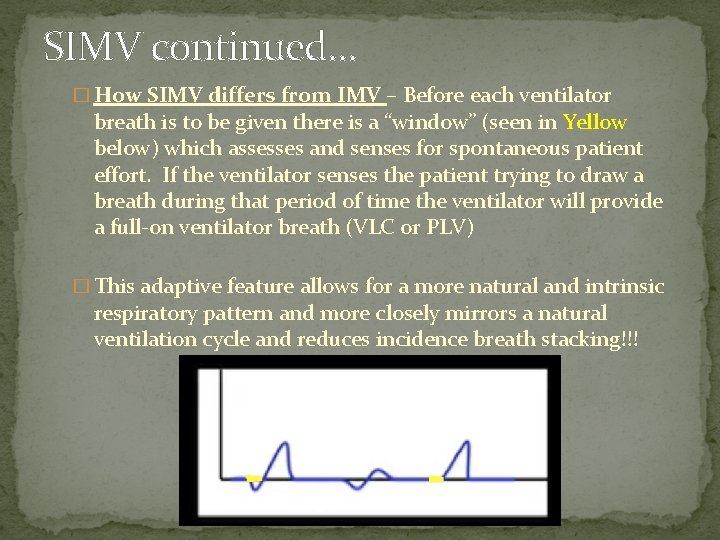
SIMV continued… � How SIMV differs from IMV – Before each ventilator breath is to be given there is a “window” (seen in Yellow below) which assesses and senses for spontaneous patient effort. If the ventilator senses the patient trying to draw a breath during that period of time the ventilator will provide a full-on ventilator breath (VLC or PLV) � This adaptive feature allows for a more natural and intrinsic respiratory pattern and more closely mirrors a natural ventilation cycle and reduces incidence breath stacking!!!
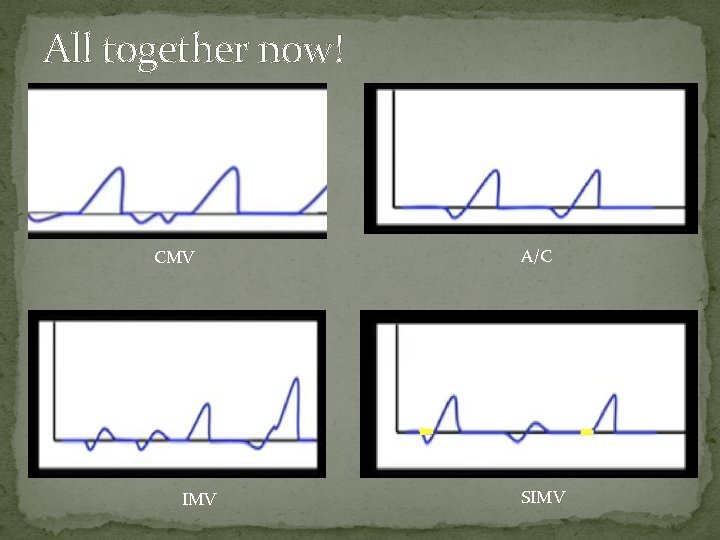
All together now! CMV IMV A/C SIMV

Modes Continued… Ø PSV – Pressure Support Ventilation – q A mode that utilizes the pt’s intrinsic rate and ventilatory effort. q Pt still intubated but breathing at sufficient rate and volume which does NOT warrant a more aggressive mode (A/C, SIMV, etc…) q Used to wean patient’s off ventilator. q Requires judicious use of analgesia for comfort, sedatives used mildly or withheld. q **Can be unreliable in patients experiencing apnea or incrased WOB** q Begs the question of why not extubate and use NIPPV? !

PSV Continued… Ø If PS set TOO LOW Ø the pt may not get a large enough Vt. Can also lead to a shorter inspiratory drive time causing the patient to double trigger spont. Breaths and auto-PEEP. Ø If PS set TOO HIGH Ø the pt. may feel overinflated and actively exhale to terminate the breath which increases WOB. MUST watch Ve (Minute Ventilation) in PSV
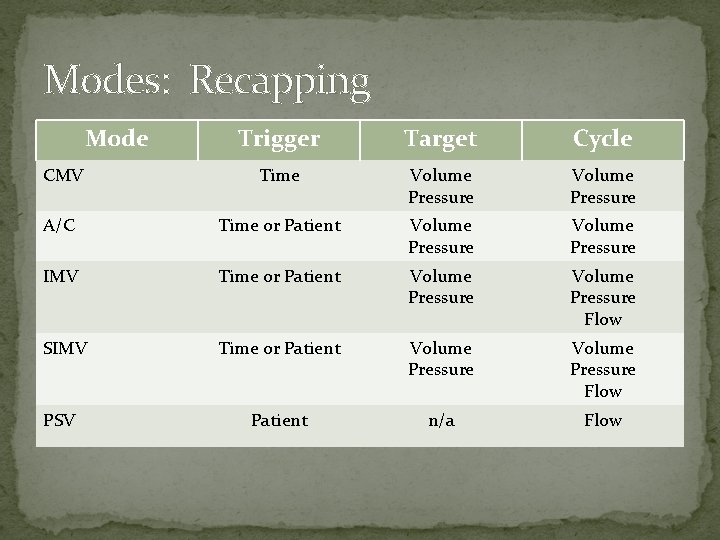

Modes: Recapping Mode Trigger Target Cycle CMV Time Volume Pressure A/C Time or Patient Volume Pressure IMV Time or Patient Volume Pressure Flow SIMV Time or Patient Volume Pressure Flow Patient n/a Flow PSV
![Modes Continued… NIPPV – Non-Invasive Positive Pressure Ventilation [CPAP & Bi. PAP] Ø CPAP Modes Continued… NIPPV – Non-Invasive Positive Pressure Ventilation [CPAP & Bi. PAP] Ø CPAP](http://slidetodoc.com/presentation_image_h/e54f5c4586c3194ded4bb013941da8b0/image-36.jpg)
Modes Continued… NIPPV – Non-Invasive Positive Pressure Ventilation [CPAP & Bi. PAP] Ø CPAP – Continuous Positive Airway Pressure q Sometimes termed “PEEP” q CPAP is an expiratory maneuver where PEEP is the RESULT of that maneuver. Encourages gas exchange and oxygenation. �Requirements for use: q Spontaneously breathing pt. w/ ability to clear airway secretions q Awake and able to follow commands. . NOT obtunded/depressed. q Ability to be coached! q Mask seal is PARAMOUNT!!!!!!!!

Modes Continued… Ø Bi. PAP – Bi-Level Positive Airway Pressure q “PEEP w/ Pressure Support” q Is BOTH an inspiratory maneuver (PS) and expiratory maneuver (CPAP). q Allows for expiratory support in the form of PEEP (splinting airways and alveoli open) while also providing an inspiratory augmentation (a little extra kick when the patient takes a breath). q Perfect for the spontaneously breathing patient who requires both aggressive oxygenation and ventilation with consideration to underlying pathology (e. g. Emphysema). q Requirements for use: q Spontaneously breathing pt. w/ ability to clear airway secretions q Awake and able to follow commands. . NOT obtunded/depressed. q Ability to be coached! q Mask seal is PARAMOUNT!!!!!!!!!

Mechanical Ventilation: Cycle A cycle is what stops the ventilation cycle: Ø Four Flavors: q Volume Cycle – ventilation stops when a preset tidal volume is achieved within lungs. q Pressure Cycle – ventilation stops when a preset pressure is achieved within lungs q Time Cycle – ventilation stops when a preset inspiratory time has elapsed. q Flow Cycle – ventilation stops when a preset flow rate has been achieved. � Cycle = internal system of checks/balances to ensure we achieve our ‘target’ goal. If we set PIP of 20, we should be getting a PIP of 20!!! Go hand-hand w/ alarms!!!

Troubleshooting the Ventilator Ø Any time a problem is encountered with the Ventilator your FIRST action is to: Remove the patient from the ventilator and ventilate manually with BVT w/ PEEP valve in place!!!! Ø Troubleshooting Mnemonics (SCOPE & DOPE) q SCOPE - Assesses High Pressure Alarms �S- Suction �C- Connections �O- Obstruction �P- Pneumothorax �E- ETT migration to L/R main stem

Troubleshooting the Ventilator cont �Mnemonics continued… q DOPE �D- Dislodgement �O- Obstruction �P- Pneumothorax �E- Equipment q Other Considerations: �Low O 2 Saturation Check settings (f and Vt / PIP, Plat, PEEP) Inspiratory time ETT location/migration Sxn Pneumothorax Pulmonary Embolism & Pulmonary Edema

Scenario #1 � 54 y/o (80 kg) male transported to hospital ED by EMS for acute exacerbation of COPD. Family states symptoms worsening over last 2 hours. � Hx of COPD/Emphysema, daily smoker (2 packs/day)+ intoxicating elixirs. � EMS Assessment & Tx � Assessment: � Patient found sitting in living room chair appears to be in distress and grabbing chest. BP unobtainable, RA Sp. O 2 87% Intercostal and supraclavicular retractions. Transport time of 8 min to ED. � Treatment: � 12 -lead with “Inferior STEMI” � NRB 15 1 pm @ [100%] = Sp. O 2 90% � ASA 324 mg / Nitro SL 0. 4 x 1 � Lungs – CEBTA � 18 g IV RAC w/ SL � Solumedrol 125 mg IV + Albuterol

Scenario #1 cont… �Hospital Assessment & Treatment: � Assessment: �Patient presenting with tachycardia, respiratory fatigue and slowing resp. rate, decreased chest excursion and low Sp. O 2. � Respiratory failure? ? Absolutely!!! � Tx: �PAI with fentanyl, versed and Succinylcholine �Mechanical Ventilation �Serial 12 -leads revealed pt NOT having a STEMI and VS Obtained �ABGs �Chest X-Ray �NS bolus at 20 ml/kg for hypotension post PAI (SBP 90)

Scenario #1 cont… �ABGs: � p. H = 7. 3 � HCO 3 - = 22 � PCO 2 = 50 � Pa. O 2 = 65 Metabolic Panel and CBC unavailable. HEMS Transport team activated.

Scenario #1 cont… �Hospital Ventilator Settings: � A/C w/ no spontaneous effort � Rate 12 � VLV - Vt of 500 ml � I-Time = 1 sec. � PEEP 5 Cm. H 20 �Sp. O 2 at 94% � TT arrives and finds: �Patient ventilating well, pain/sedation not indicated, good chest excursion, confirms ETT placement and patency verified. Lungs are diminished in apex and bases. Report obtained from ED RN. Bilateral AC Ivs with NS at TKO.

Scenario #1 cont… � At time of Transport TT elects to change vent settings � Mode/Trigger =SIMV � Rate = 12 � Target = PLV 15/5 (PIP = 20 cm. H 2 o) � I time = 1 sec. � PEEP 5 cm. H 2 o � Sp. O 2 increases to 97% and maintains � Switched sedative to Ketamine for continued low SBP and diminishing lung sounds. Albuterol MDI. NS bolus 20 ml/kg prn for SBP then TKO. � Patient improvement noted. TOC at receiving ED. Follow up revealed high BUN/Cr and relative hypernatremia. Patient discharged 5 days later. � What went wrong with this patient? ? ?

Scenario #2 �HEMS TT responds to scene call for 2 vehicle MVC rollover, multiple patients with injuries. �Patient is 24 y/o male, restrained driver of SUV involved in 2 car MVC. Fellow occupants were unrestrained and ejected at time of rollover + DOS. �EMS finds patient inside vehicle w/ GCS of 3, patent airway, breathing at 10/min and shallow w/ unilateral chest wall excursion and bleeding scalp lac. Patient extricated, backboarded, moved to ambulance and PAI w/ secondary injuries addressed. Patient is progressively becoming hypotensive with lung sounds absent L side.

Scenario #2 � TT arrives to find patient intubated w/ BVT and PEEP valve in place. Unilateral chest wall movement observed to R side only, flail chest confirmed to L side. Lung sounds present R, Absent L. � Flail chest splinted. Left side needle decompression w/ + air return. VS normalize TT packages patient and moves to Aircraft. � Transport time to level 1 Trauma Center 35 min. � En route patient Sp. O 2 drops and high pressure alarms sound. � What is your immediate action? ? What are your follow up actions? What is the problem? ?
- Slides: 47