Mechanical Ventilation Objectives List the indications for mechanical

Mechanical Ventilation

Objectives • List the indications for mechanical ventilation (MV) • Describe benefits and risks of MV • Review how resistance and compliance contribute to patient-ventilator interactions • Recognize common modes of MV and ventilator terminology • Recognize appropriate evaluation for weaning from mechanical ventilation

Indications for Mechanical Ventilation • Respiratory Failure - Hypoxemic (Type I) - Hypercapnic/ventilatory (Type II) - Shock (Type IV) • Unsustainable increased work of breathing • Airway obstruction or impending airway obstruction • Altered mental status - Obtunded or agitated (with or without Type I or II)

Benefits of Mechanical Ventilation Airway protection Medication delivery Facilitations of procedures Improved gas exchange: can supply high levels of oxygen and control minute ventilation • Reduction in work of breathing • Beneficial Cardiopulmonary/hemodynamic interactions • • v. The ventilator is a TOOL we have to provide supportive care, but it is infrequently the solution to the underlying problem

Toxicities of Mechanical Ventilation • Lip/palate/laryngeal/ tracheal injury • ETT issues • Oxygen toxicity • Volutrauma/barotrauma • Cardiopulmonary interactions • Ventilator associated pneumonia (VAP) • Sinusitis • Disuse muscle atrophy • Self-extubation • Need for sedation • Iatrogenesis
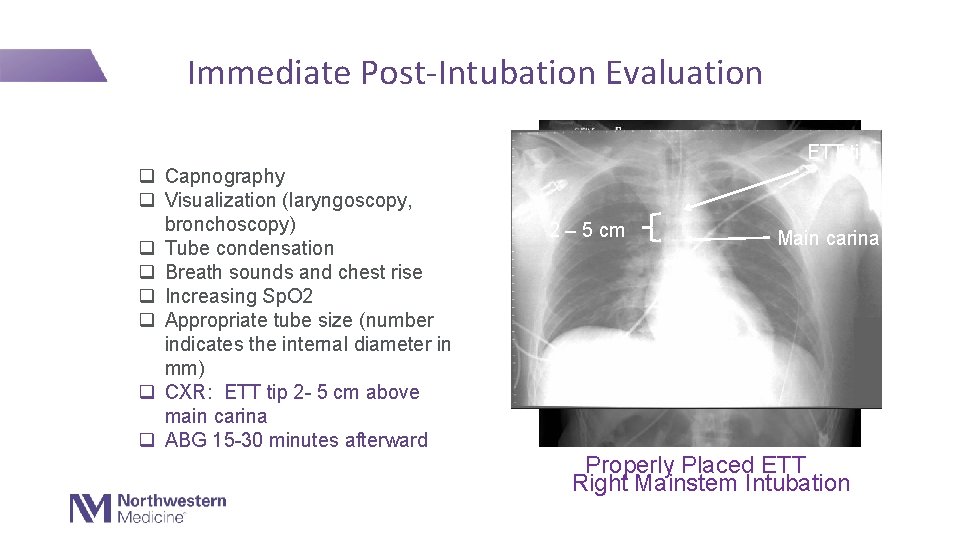
Immediate Post-Intubation Evaluation ETT tip q Capnography q Visualization (laryngoscopy, bronchoscopy) q Tube condensation q Breath sounds and chest rise q Increasing Sp. O 2 q Appropriate tube size (number indicates the internal diameter in mm) q CXR: ETT tip 2 - 5 cm above main carina q ABG 15 -30 minutes afterward 2 – 5 cm Main carina Properly Placed ETT Right Mainstem Intubation

Setting up the Ventilator

Common Initial Default Ventilator Settings Mode RR VT Fi. O 2 PEEP. Vi AC/VC 14 -20 RR and TV will affect Pa. CO 2 550 ml 0. 40 - 1. 0 Fi. O 2 and PEEP will affect Pa. O 2 5 cm. H 2 O (flow) 60 -70 L/min, decelerating (ramp) ABGs, airway pressures, clinical management, and synchrony will guide subsequent changes. * The tidal volume should be appropriate for the size (height) of the patient – a good starting point is 8 cc/kg based on their predicted body weight (PBW)

Most Common Initial Mode in the MICU Assist/Control (AC) - Both spontaneously triggered breaths and timed (controlled) breaths get “assisted” by the ventilator to deliver the same set volume or pressure • AC/VC = assist control, volume control • Set a tidal volume (Vt) and flow (V) • Pressures and inspiratory time are the dependent variables (outcomes, cannot be directly controlled) • AC/PC = assist control, pressure control • Set an inspiratory pressure (Pi) and inspiratory time (Ti) • Volume and flows are the dependent variables (outcomes, cannot be directly controlled)
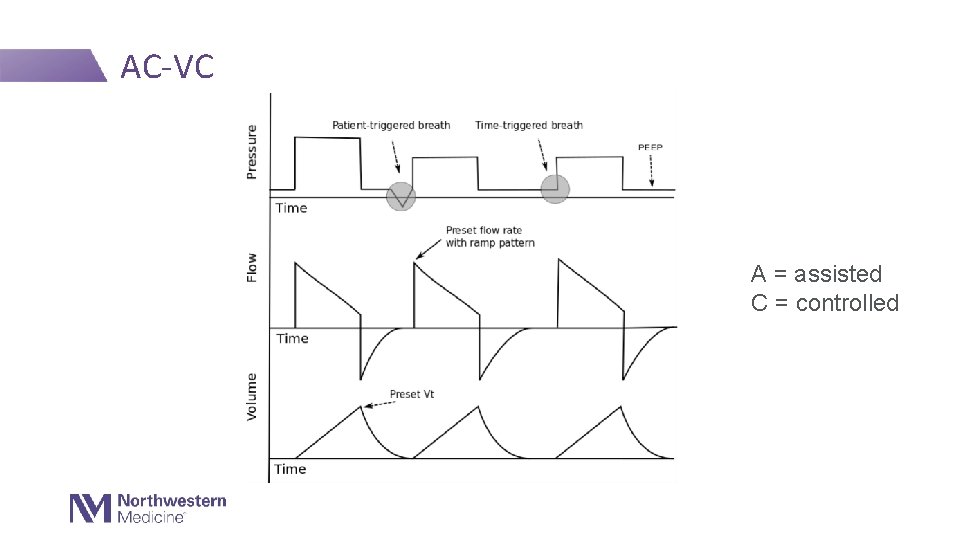
AC-VC A = assisted C = controlled
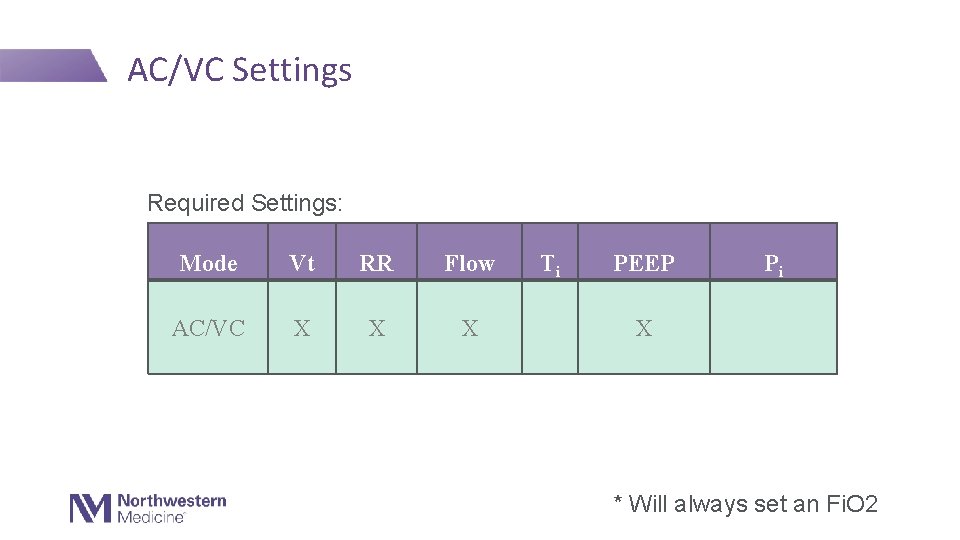
AC/VC Settings Required Settings: Mode Vt RR Flow AC/VC X X X Ti PEEP Pi X * Will always set an Fi. O 2
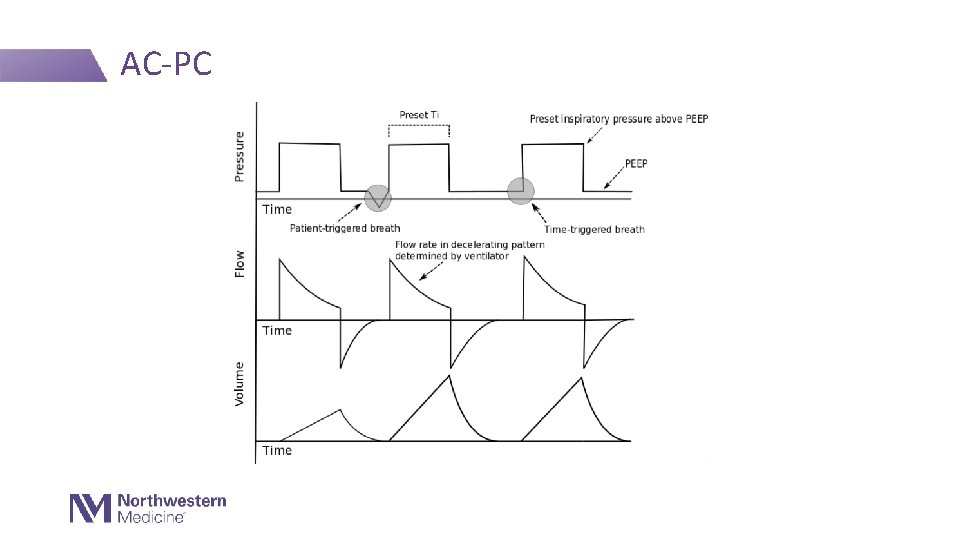
AC-PC
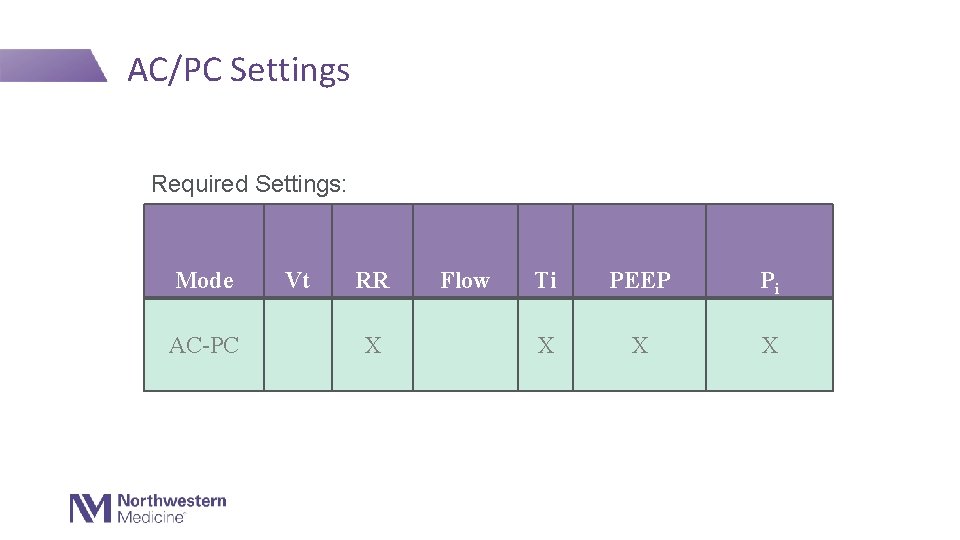
AC/PC Settings Required Settings: Mode AC-PC Vt RR Flow Ti PEEP Pi X X ✔� ✔�

Other Available Modes - Spontaneous mode - aka “pressure support” (PS) • Patient triggered breaths are supported by a set inspiratory pressure - Synchronized Intermittent Mandatory Ventilation (SIMV) • Spontaneous breaths triggered by the patient over the set rate get supported with pressure support • The ventilator attempts to synchronize some of these spontaneous breaths with the controlled breaths that are determined by the set rate
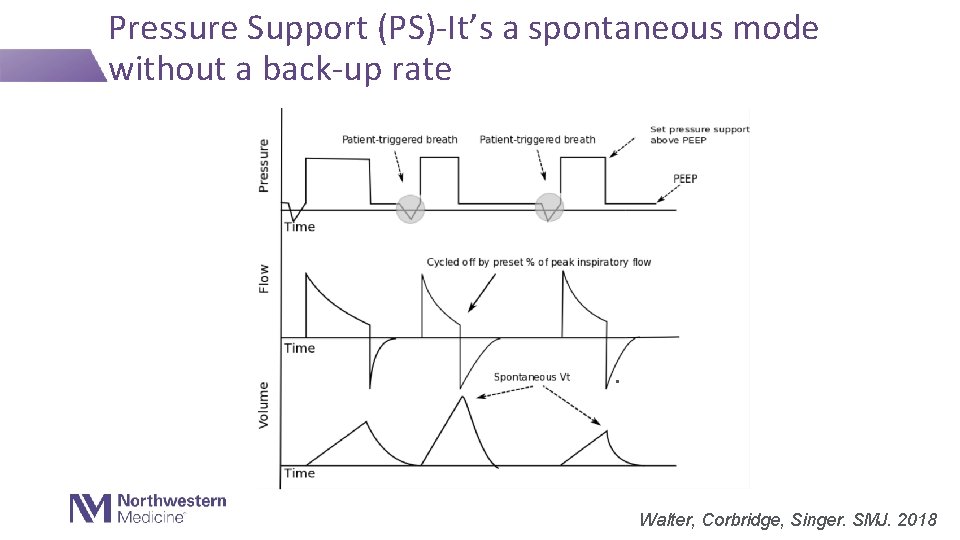
Pressure Support (PS)-It’s a spontaneous mode without a back-up rate . Walter, Corbridge, Singer. SMJ. 2018
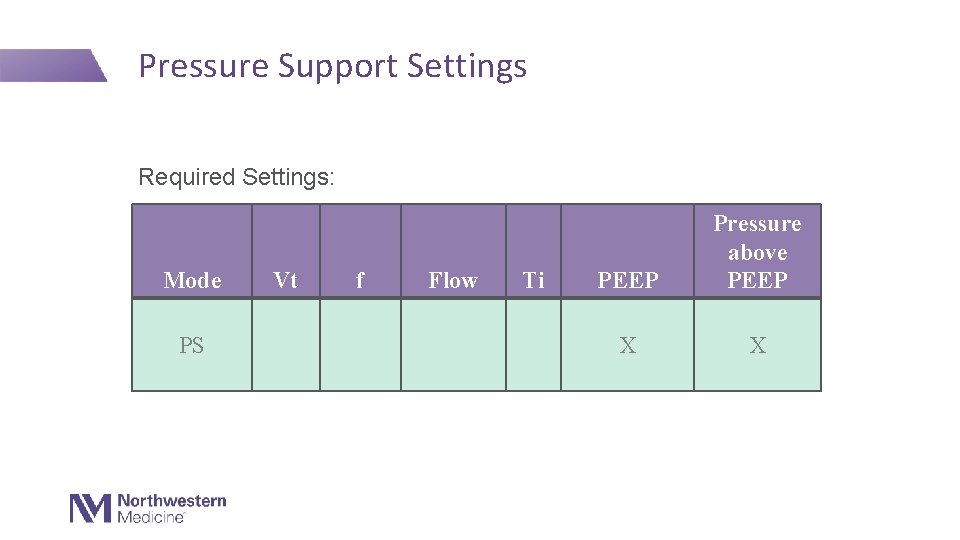

Pressure Support Settings Required Settings: Mode PS Vt f Flow Ti PEEP Pressure above PEEP X X ✔�

Synchronized Intermittent Mandatory Ventilation (SIMV)

SIMV- VC + Pressure Support • Triggers: Mandatory/timed (based on set rate) or patient (if initiated before next timed breath) • Target: - Mandatory or synchronous breath: volume (flow also set) • Dependent: PIP, inspiratory time - Spontaneous breath: pressure • Dependent: volume .
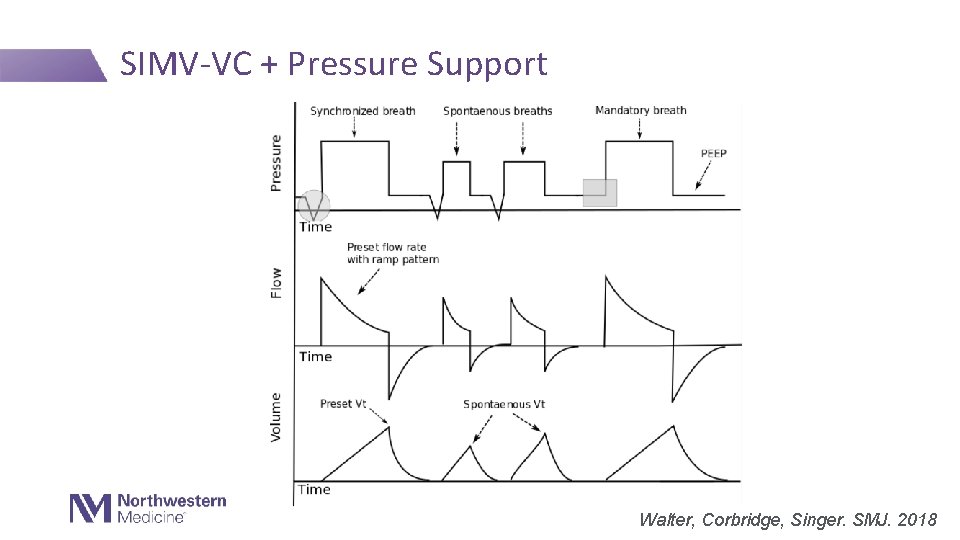
SIMV-VC + Pressure Support A C Walter, Corbridge, Singer. SMJ. 2018
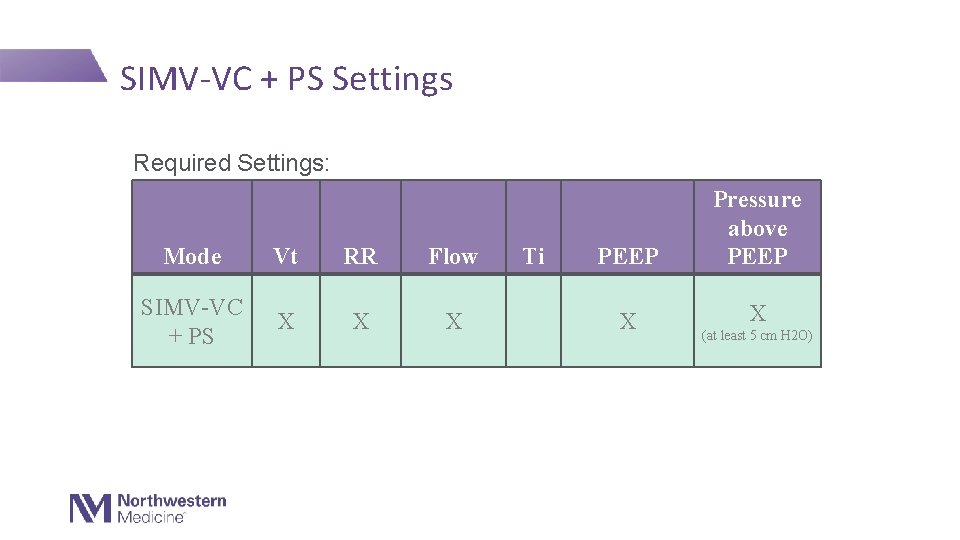

SIMV-VC + PS Settings Required Settings: Mode Vt RR Flow SIMV-VC + PS X X X Ti PEEP Pressure above PEEP X X (at least 5 cm H 2 O)

AC vs. SIMV • As long as you know what you’re doing, it doesn’t matter (much) • AC and SIMV are identical in a patients not spontaneously breathing • AC VC = assured volume with each breath (assisted or controlled) • SIMV - VC = varying volume with spontaneous breaths

Ventilators are “simple” machines • “Everything about mechanical ventilation can be discussed in terms of flow, pressure, time, resistance, and compliance. ” • “The ventilator is just a slightly more complex leaf blower. ”
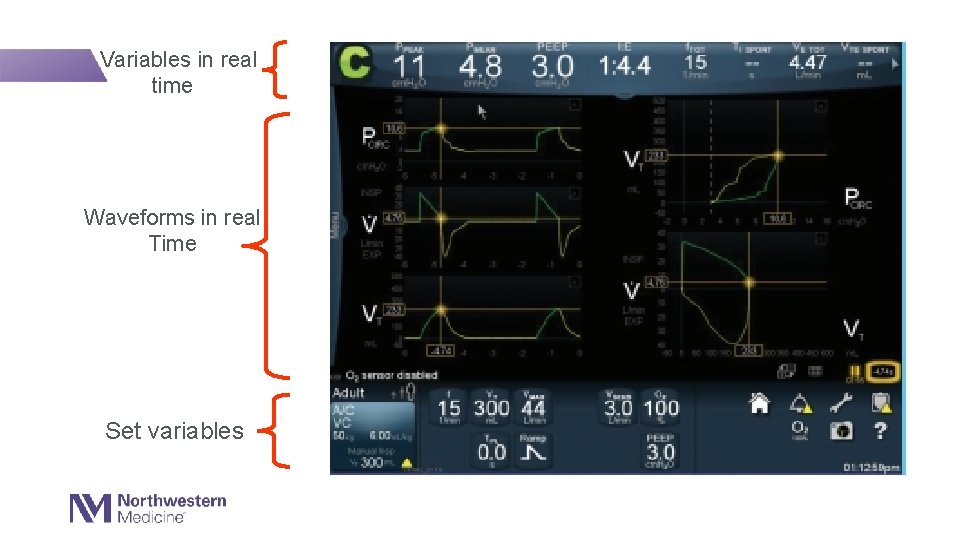
Variables in real time Waveforms in real Time Set variables
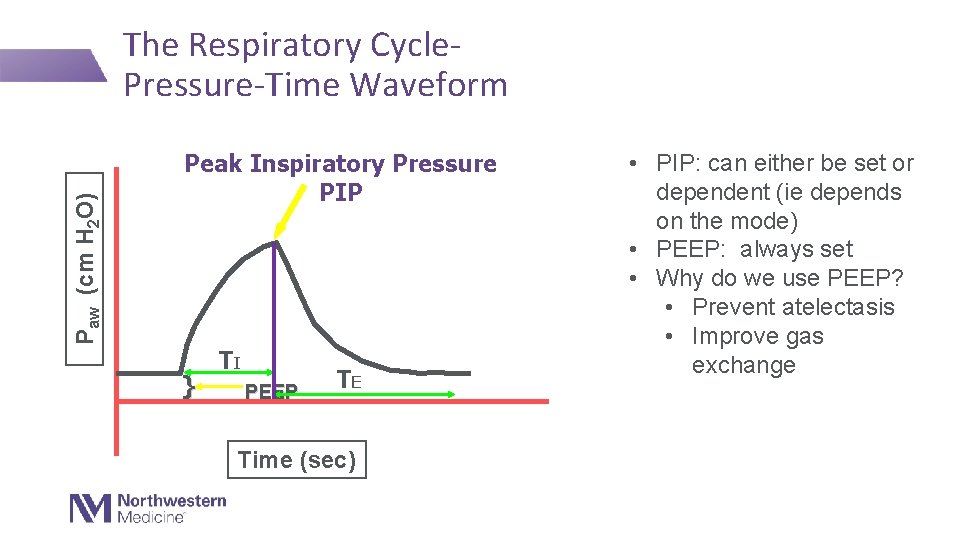
Paw (cm H 2 O) The Respiratory Cycle. Pressure-Time Waveform Peak Inspiratory Pressure PIP } TI PEEP TE Time (sec) • PIP: can either be set or dependent (ie depends on the mode) • PEEP: always set • Why do we use PEEP? • Prevent atelectasis • Improve gas exchange
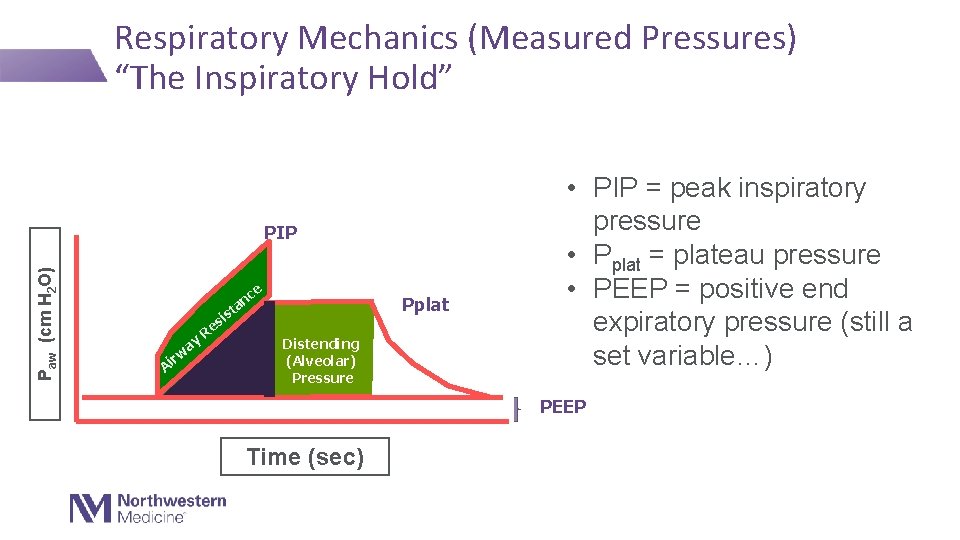
Respiratory Mechanics (Measured Pressures) “The Inspiratory Hold” Paw (cm H 2 O) PIP e nc a t Pplat s si A irw ay Re Distending (Alveolar) Pressure • PIP = peak inspiratory pressure • Pplat = plateau pressure • PEEP = positive end expiratory pressure (still a set variable…) PEEP Time (sec)

Resistance (R) and Compliance (C) Resistance-is the tube/airway tight/kinked? Compliance-how easy is it to expand the lungs? • R= ΔP/flow (liters/sec) • If flow = 60 L/min 1 L/sec • ΔP = PIP - Pplat • Normal < 15 cm. H 2 O/L/sec • C = ΔV/ ΔP • ΔV = Vt = tidal volume • ΔP = Pplat - PEEP • Normal >60 ml/cm. H 2 O - If less than 60, stiff lungs-think ARDS
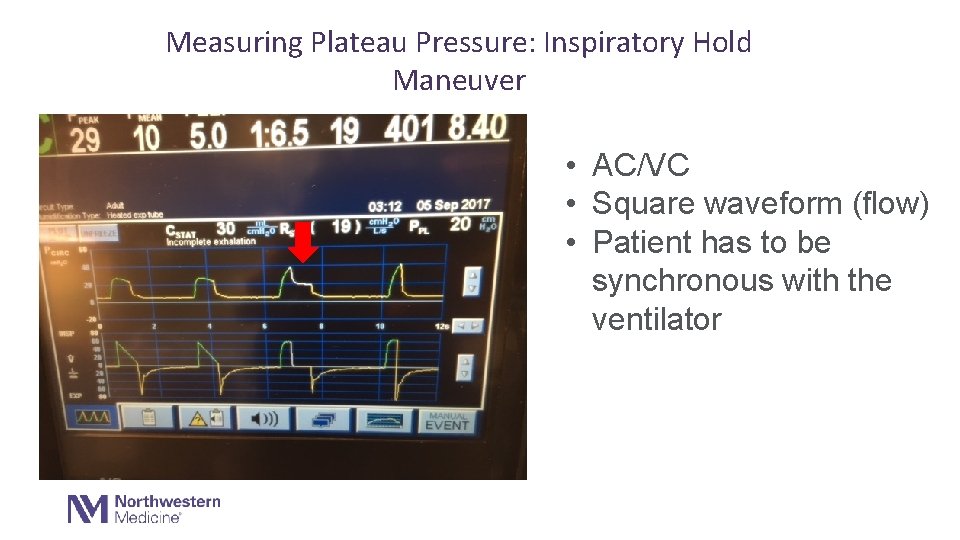
Measuring Plateau Pressure: Inspiratory Hold Maneuver • AC/VC • Square waveform (flow) • Patient has to be synchronous with the ventilator

Problems with Lung Mechanics What causes decreased compliance? What causes increased resistance? • Kinked tubing • Biting on the endotracheal tube • Secretions • Bronchospasm (ie asthma and COPD) • Airway tumors • Foreign bodies Alveolar filling: blood/pus/water Pleural filling: air/blood/pus/water Interstitial lung disease Decreased lung size: PTX, Right mainstem intubation • Abdominal issues: ascites, distended bowel, pregnancy • Chest wall issues: obesity • •

When there’s an alarm… • When there are high peak pressures on the ventilator: 1. Check the tubing, suction, listen 2. Check the plateau pressure 3. If high peak and plateau compliance problem 4. If high peak, unchanged plateau resistance problem
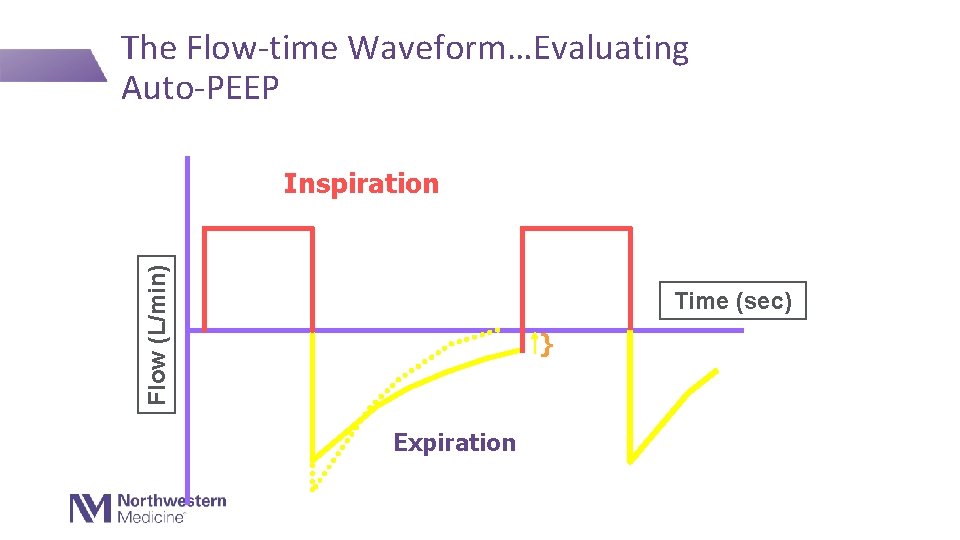
The Flow-time Waveform…Evaluating Auto-PEEP Flow (L/min) Inspiration Time (sec) } Expiration
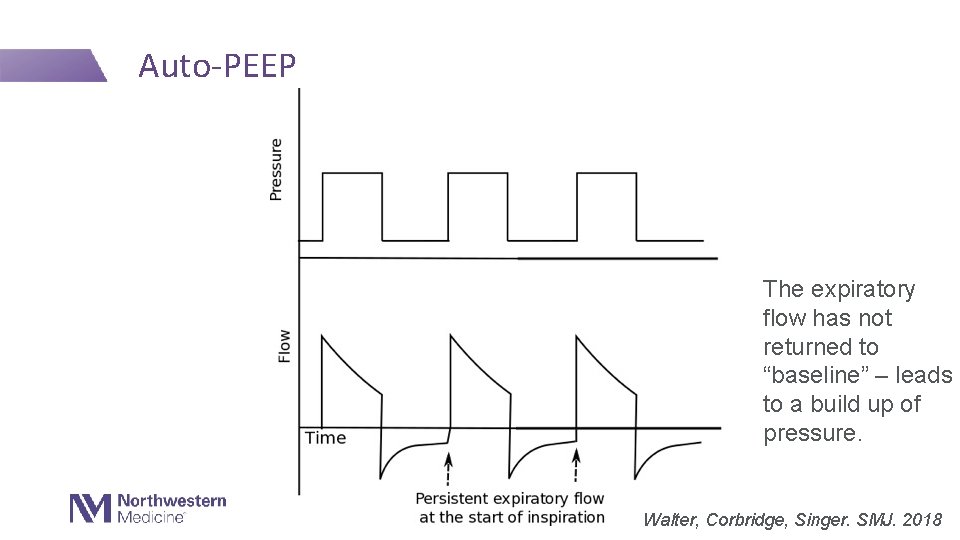
Auto-PEEP The expiratory flow has not returned to “baseline” – leads to a build up of pressure. Walter, Corbridge, Singer. SMJ. 2018

Causes of Auto. PEEP • A resistance and/or “I/E” problem: • How can we reduce auto. PEEP? Asthma COPD Hyperdynamic airway collapse Tachypnea Iatrogenesis (High Vt or low flows) Small ETT - Increase the expiratory time by: • • • Increase flow Decrease respiratory rate Decrease tidal volume Treat the underlying problem *if the patient is breathing quickly, decreasing the RR will not help – may need heavy sedation to suppress the respiratory drive.

Spontaneous Breathing Trials (SBT)

What is an SBT? • Spontaneous breathing trial • Supporting patient with only enough ventilator support to overcome resistance from the ETT or allowing them to breath on their own - Most often done using pressure support (PS): • NMH: inspiratory pressure of 5, PEEP 5 - Also can use a T-piece, CPAP • Who gets SBTs?

Candidates for SBT • Adequate mental status - Can tolerate an SAT: spontaneous awakening trial • No immediate plan for procedures • Hemodynamic stability • Sustainable minute ventilation • Adequate oxygenation • Low levels of PEEP
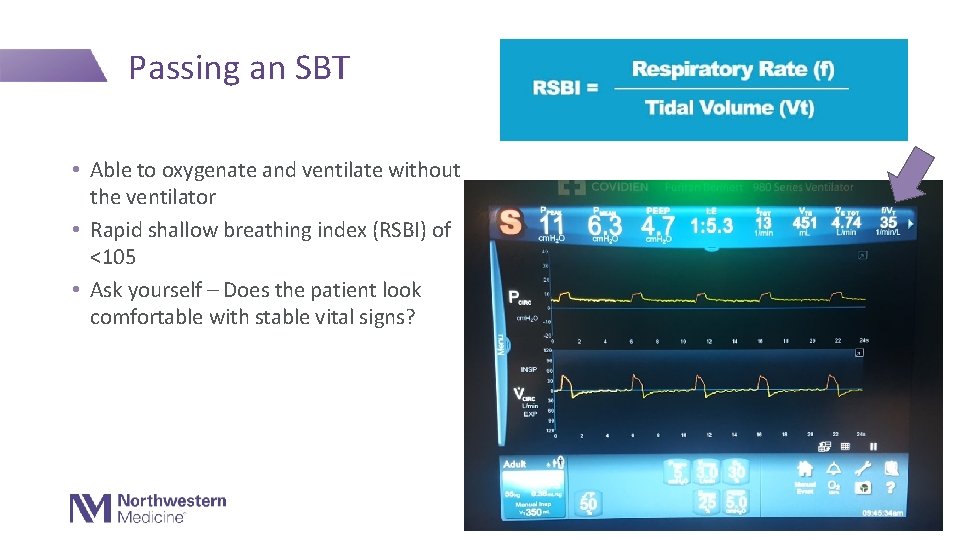
Passing an SBT • Able to oxygenate and ventilate without the ventilator • Rapid shallow breathing index (RSBI) of <105 • Ask yourself – Does the patient look comfortable with stable vital signs?

When to extubate? • Requirements for extubation: - Hemodynamic stability - No planned procedures - No need for frequent suctioning - Able to protect airway, good mental status - Cuff leak (ask an RT) - Able to ventilate and oxygenate without the ventilator • Passed an SBT
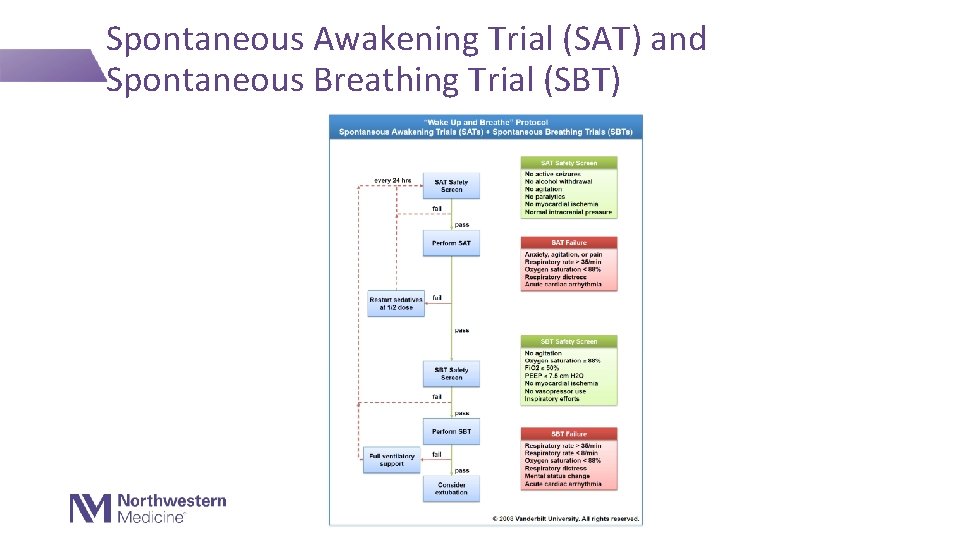
Spontaneous Awakening Trial (SAT) and Spontaneous Breathing Trial (SBT)

Conclusions • The most common mode of ventilation in the MICU at NM is AC/VC - Set volume, monitor pressures • Other modes can achieve similar outcomes and are acceptable alternatives although the nuisances are beyond the scope of this primer • Assessing efficacy and safety of the ventilator should occur daily • Daily consideration for SBT and possible extubation

Special Thanks To: • • Khalilah Gates, MD Elizabeth Malsin, MD Clara Schroedl, MD James Walter, MD
- Slides: 40